Introduction
Facing heart health challenges can be overwhelming, especially when considering aortic valve replacement (AVR) options that could greatly affect your well-being. With choices ranging from traditional surgical methods to innovative minimally invasive techniques, you have the opportunity to select a path that aligns with your health needs and lifestyle. Many patients feel uncertain about which option is right for them, leading to anxiety about their health decisions.
How can you find the best approach considering your unique circumstances? In this article, we’ll explore the different types of AVR together, helping you feel more empowered to make choices that can enhance your heart health and quality of life.
Define Aortic Valve Replacement: Key Concepts and Importance
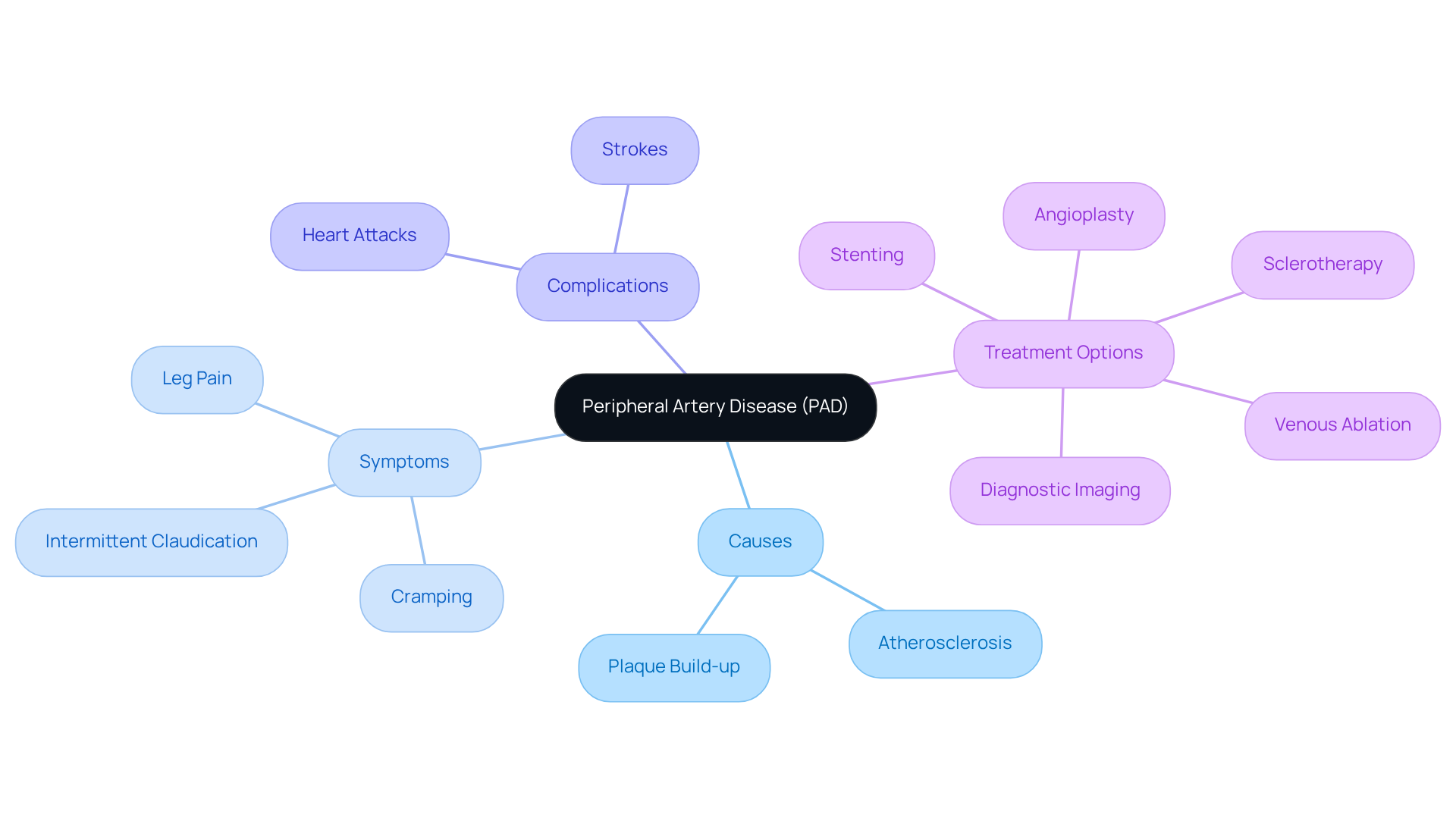
If you or a loved one is facing heart issues, understanding aortic valve replacement (AVR) can feel daunting, but it’s a vital step towards better health. AVR is an essential surgical operation designed to replace a faulty heart valve, which plays a crucial role in controlling blood flow from the heart to the rest of the body. Conditions like aortic stenosis, where the valve opening narrows, or aortic regurgitation, where it allows backflow, can lead to serious health problems, including heart failure. Understanding AVR is important, especially for older adults who may feel more vulnerable to heart issues. This procedure not only restores normal heart function but also significantly enhances the quality of life for these individuals.
There are various types of aortic valve replacement, such as traditional open-heart surgery and newer, less invasive methods like transcatheter heart valve replacement. TAVR, in particular, has emerged as a safer option for older adults, allowing for valve replacement without the risks associated with open-heart surgery. Did you know that over 13 percent of Americans aged 75 and older will face aortic stenosis? This makes timely intervention all the more crucial.
The benefits of AVR go beyond just physical health; many individuals report feeling more energetic and breathing easier shortly after the procedure. For example, an 83-year-old woman who underwent TAVR experienced significant improvements in her breathing and overall vitality, allowing her to engage more fully with her family. This illustrates the profound effect AVR can have on the quality of life for older individuals, enabling them to resume their daily activities with renewed energy.
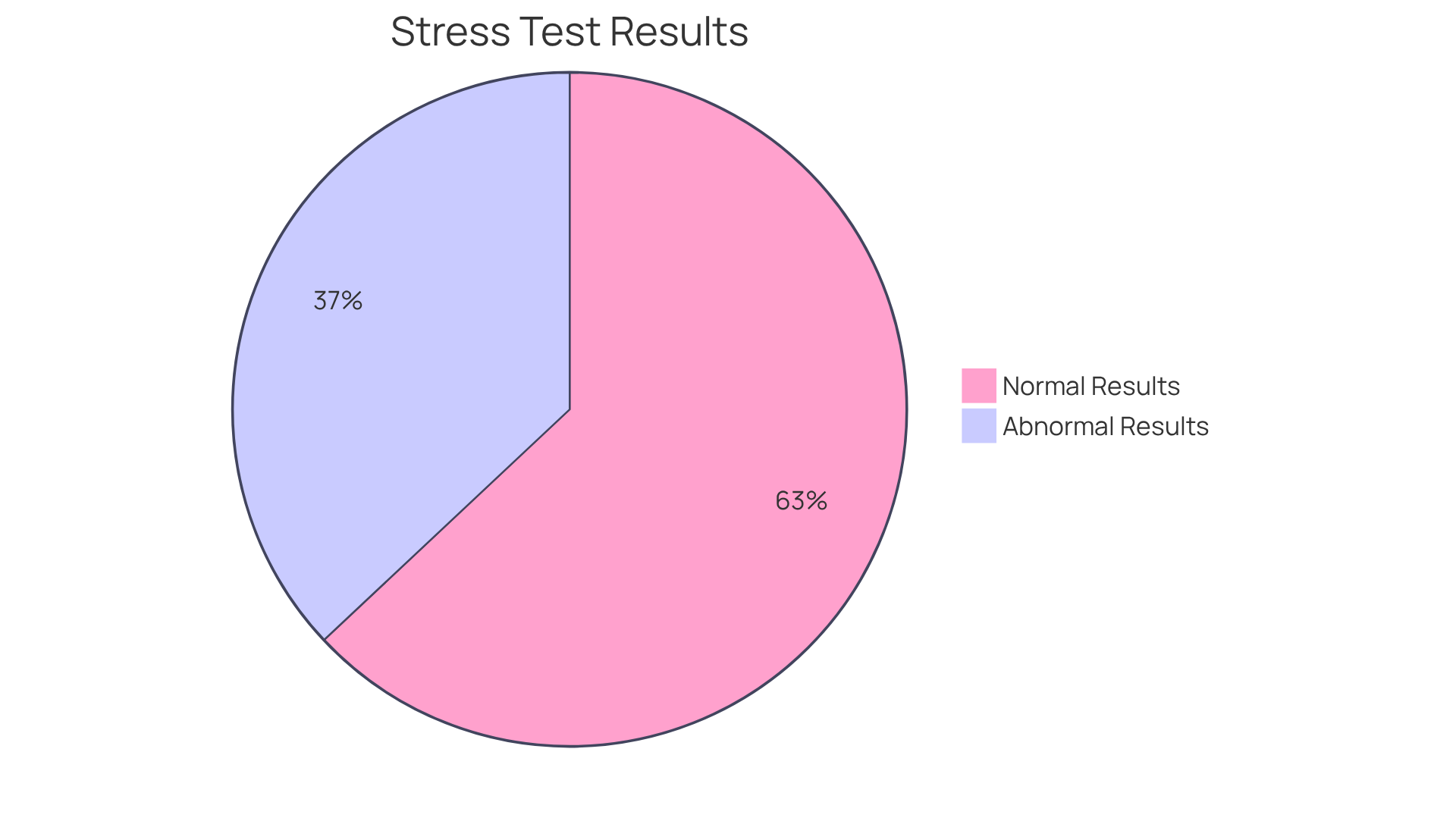
Statistics show that individuals treated with TAVR or traditional surgery have similar rates of all-cause mortality and disabling stroke at five years, underscoring the effectiveness of this intervention. As our population ages, the importance of heart surgery becomes increasingly clear, making it a vital consideration for healthcare providers and patients alike. Amavita’s commitment to comprehensive cardiovascular care, featuring advanced imaging technologies and the CardioElite™ program, ensures that individuals receive the best possible outcomes through personalized treatment strategies and innovative minimally invasive options. Choosing AVR could be the key to reclaiming your life and enjoying precious moments with loved ones once again.
Explore Types of Aortic Valve Replacement: Surgical vs. Minimally Invasive
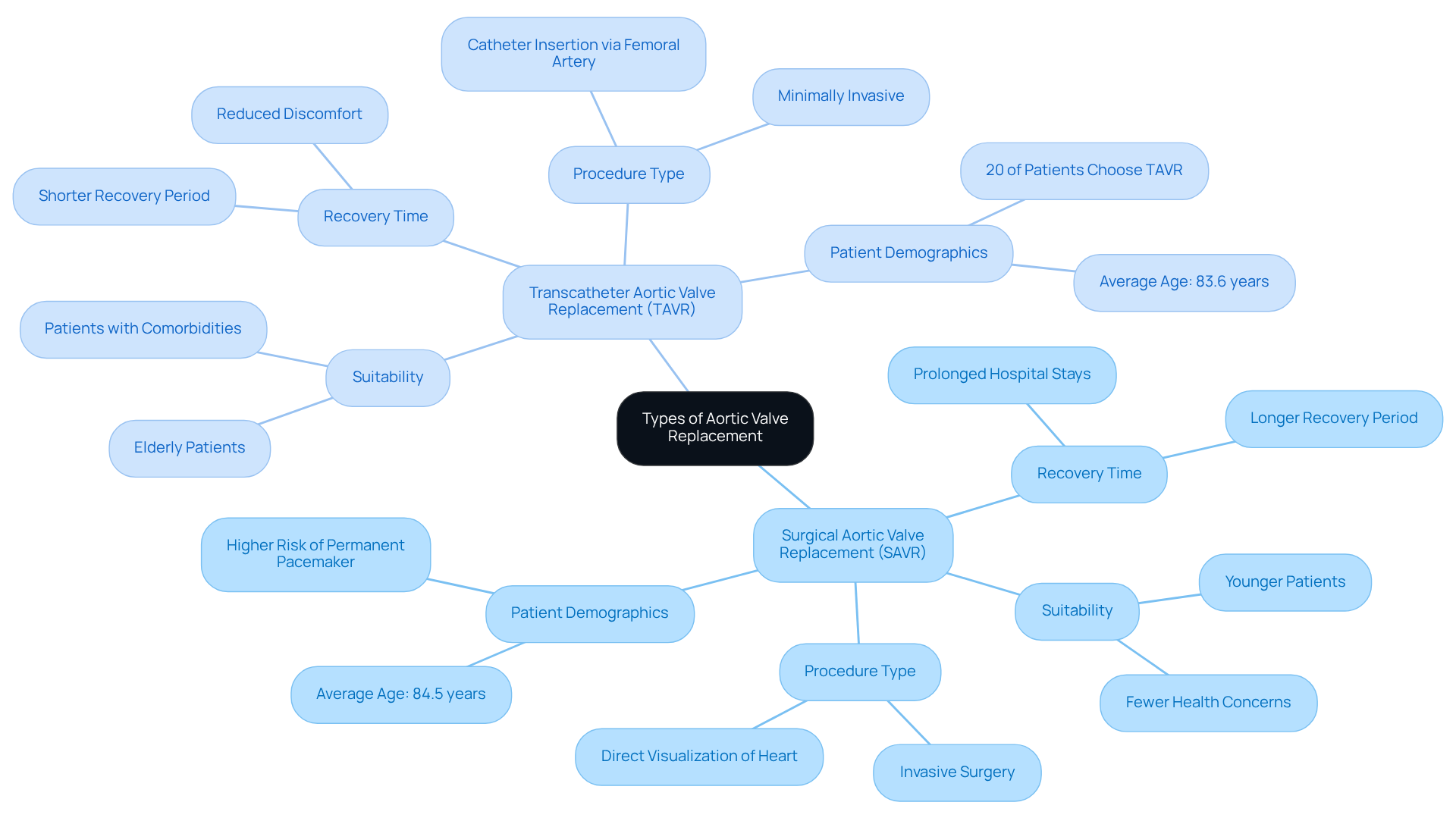
Are you feeling uncertain about your heart health options? Let’s explore the two main types of aortic valve replacement, which are surgical aortic valve replacement (SAVR) and transcatheter aortic valve replacement (TAVR).
- Surgical Aortic Valve Replacement (SAVR): This conventional technique requires a significant cut in the chest to reach the heart, which can feel daunting for many patients. It’s often more suitable for younger individuals or those with fewer health concerns. While SAVR allows for direct visualization and manipulation of the heart, it generally means a longer recovery period, which can feel overwhelming, with individuals often experiencing prolonged hospital stays.
- Transcatheter Aortic Valve Replacement (TAVR): This minimally invasive approach involves inserting a new valve via a catheter, usually through the femoral artery. TAVR is especially beneficial for elderly individuals or those with considerable health concerns, as it typically leads to shorter recovery periods, reduced discomfort, and a diminished risk of complications. Many older adults find that TAVR significantly improves their quality of life, making it a choice worth considering. Interestingly, only about 20 percent of patients in the U.S. choose the minimally invasive TAVR option, even though it offers so many benefits.
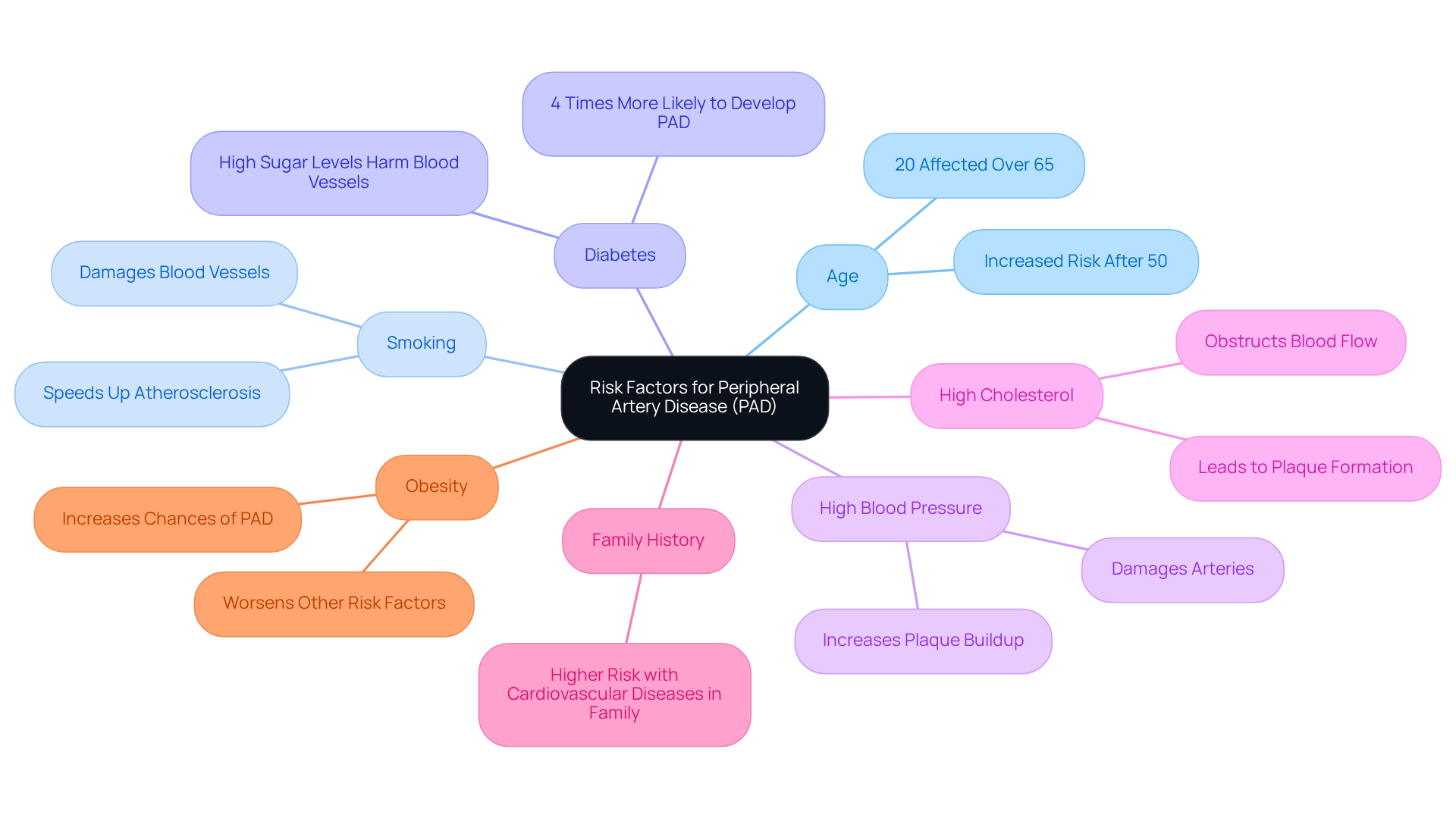
At Amavita Heart & Vascular Health, we emphasize targeted cardiovascular care for individuals at high risk, including those with diabetes, hypertension, or a family history of heart disease. Our advanced imaging capabilities and comprehensive evaluations ensure that individuals receive personalized treatment plans tailored to their specific needs. It’s important for you and your loved ones to understand these choices as you discuss treatment options with your healthcare provider. Cardiologists stress that while SAVR may be favored for younger individuals, TAVR provides significant benefits for older adults, especially those with comorbidities, as it is linked to decreased stroke risk and improved in-hospital outcomes. Furthermore, our CardioElite™ program enhances this care by offering advanced, real-time diagnostic data and 24/7 cardiology consultation, further assisting proactive management and reducing emergency workload. Understanding your options can empower you to make the best choice for your heart health journey.
Determine Selection Criteria: Choosing the Right Aortic Valve Replacement
Choosing the right types of aortic valve replacement can feel overwhelming, especially when considering how it affects your health and future. Several key criteria can significantly impact your outcomes, and understanding them is the first step towards making an informed decision.
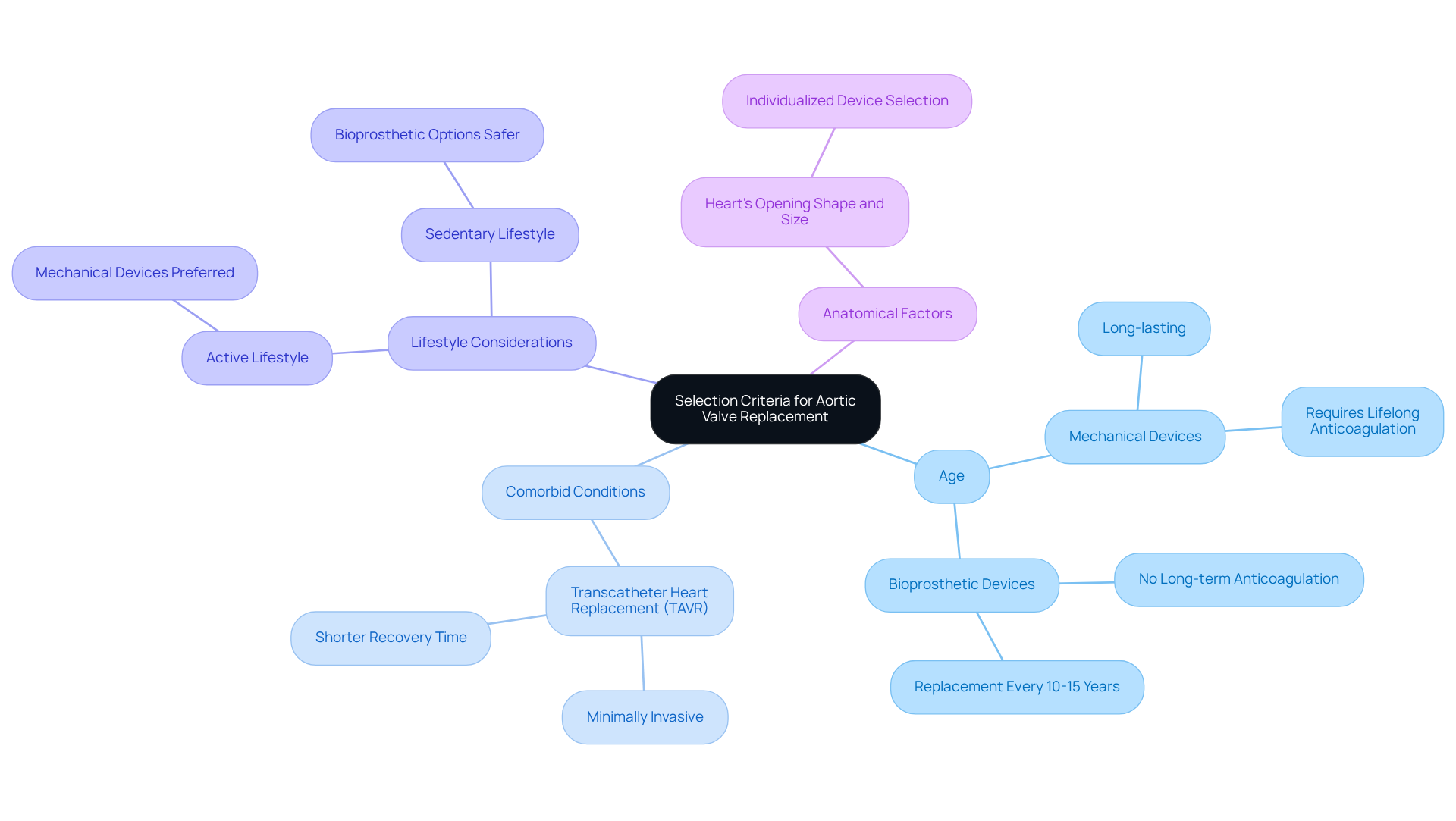
- Age of the Individual: If you’re younger, mechanical devices might be a good fit for you. They last a long time but require lifelong anticoagulation treatment. On the other hand, if you’re older, you might prefer bioprosthetic devices, which eliminate the need for long-term anticoagulation but usually need to be replaced every 10 to 15 years.
- Comorbid Conditions: If you have additional health concerns, like diabetes or chronic kidney disease, transcatheter heart replacement (TAVR) could be a better option. This minimally invasive technique often leads to a shorter recovery time, which is especially important if your overall health complicates traditional surgical options.
- Lifestyle Considerations: Think about your daily activities. If you lead an active lifestyle, mechanical devices might help you avoid future surgeries. However, if you’re more sedentary, bioprosthetic options could be a safer choice with a lower risk of complications.
- Anatomical Factors: The shape and size of your heart’s opening play a crucial role in determining the right choice for you. Not every device suits every individual, so it’s important to work closely with your cardiologist to find the best types of aortic valve replacement that are tailored just for you.
Real-world examples highlight these factors: DeWayne Epley, a former heart surgery recipient, emphasized the importance of being well-prepared and asking questions about the surgical process, which can lead to improved results. Similarly, Tom Sabourin’s experience with an aneurysm underscores the need for personalized strategies based on individual patient factors. By understanding these important factors, you can take a confident step towards a healthier heart and a brighter future.
Assess Risks and Benefits: Understanding Outcomes of Aortic Valve Replacement
Navigating the decision for aortic valve replacement (AVR) can feel overwhelming, but understanding the risks and benefits can empower you to make informed choices about your health.
-
Benefits:
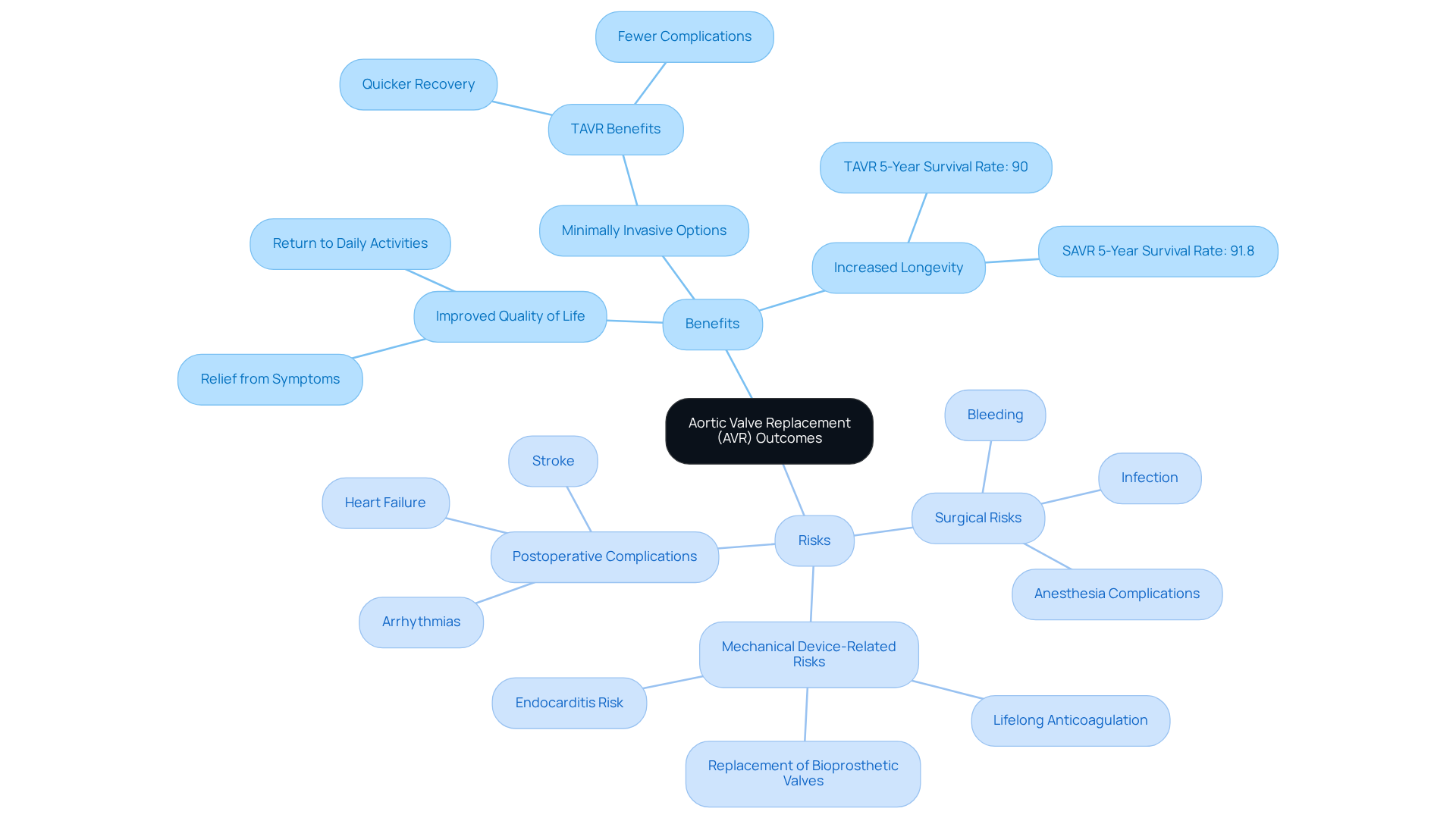
- Improved Quality of Life: Many people notice their heart works better right after getting a new valve. They often feel relief from symptoms like shortness of breath and fatigue, allowing them to return to daily activities. We focus on using the best imaging technology to help you get the most from your treatment, especially for those at higher risk.
- Increased Longevity: AVR can help you live longer, particularly if you have severe aortic stenosis. Studies show that about 90% of people undergoing transcatheter valve replacement (TAVR) survive for five years, while surgical valve replacement (SAVR) has a slightly higher rate of 91.8%. Knowing these statistics can be reassuring, especially when considering your options with our targeted cardiovascular care.
- Minimally Invasive Options: TAVR offers a gentler alternative to traditional surgery, leading to quicker recoveries and fewer complications. This is particularly beneficial for older adults or those with multiple health concerns. Dr. Martinez-Clark specializes in these techniques, which can greatly enhance your experience and outcomes.
-
Risks:
- Surgical Risks: Every surgery has its risks, and knowing what they are can help you feel more at ease. Potential issues include bleeding, infection, and complications related to anesthesia.
- Mechanical Device-Related Risks: If you have artificial heart components, you’ll need lifelong anticoagulation treatment, which can increase the risk of bleeding. Bioprosthetic valves, made from animal tissue, may need replacement after about ten years due to wear. Additionally, complications like endocarditis can occur, so we emphasize personalized treatment plans to address these risks effectively.
- Postoperative Complications: Issues such as arrhythmias, stroke, or heart failure can arise, especially in older individuals with pre-existing health conditions. Being aware of these complications means we can keep a close eye on your recovery, helping you heal better. Our comprehensive care approach is designed to support you throughout your recovery journey.
By carefully weighing these risks and benefits, you can engage in meaningful discussions with your healthcare provider at Amavita Heart & Vascular Health. By discussing these factors with your healthcare provider, you can take a confident step towards a healthier heart and a better quality of life.
Conclusion
Making decisions about your heart health can feel overwhelming, but understanding your options is the first step toward feeling empowered. Knowing about the different types of aortic valve replacement is essential for making informed health choices. This article highlights how aortic valve replacement (AVR) can be a life-changing procedure for those facing heart valve issues. By exploring both traditional surgical methods and minimally invasive options like transcatheter aortic valve replacement (TAVR), you can navigate your choices and find the best intervention for your unique situation.
Key insights discussed include:
- The differences between surgical aortic valve replacement (SAVR) and TAVR
- The criteria for selecting the right type of valve replacement based on your age, health conditions, lifestyle, and anatomy
- The potential risks and benefits of each method
At places like Amavita Heart & Vascular Health, we focus on personalized care and thorough evaluations to ensure you get the best treatment for your needs.
Ultimately, the choice of aortic valve replacement can significantly impact your quality of life and longevity. When you understand your options and talk openly with your healthcare team, you can take important steps to regain your health and enjoy life more fully. Embracing this knowledge empowers you to make the best choices for your heart health journey, paving the way for a brighter future filled with cherished moments and improved well-being.
Frequently Asked Questions
What is aortic valve replacement (AVR)?
Aortic valve replacement (AVR) is a surgical operation designed to replace a faulty heart valve that controls blood flow from the heart to the rest of the body.
Why is AVR important?
AVR is important because it addresses conditions like aortic stenosis and aortic regurgitation, which can lead to serious health problems, including heart failure. It restores normal heart function and significantly enhances the quality of life, especially for older adults.
What are the types of aortic valve replacement?
There are various types of aortic valve replacement, including traditional open-heart surgery and newer, less invasive methods like transcatheter aortic valve replacement (TAVR).
What is TAVR and who is it suitable for?
TAVR is a less invasive method for replacing the aortic valve that has emerged as a safer option for older adults, allowing for valve replacement without the risks associated with open-heart surgery.
How common is aortic stenosis among older adults?
Over 13 percent of Americans aged 75 and older will face aortic stenosis, highlighting the importance of timely intervention.
What are the benefits of AVR beyond physical health?
Many individuals report feeling more energetic and breathing easier shortly after the procedure, which can significantly improve their overall quality of life and ability to engage in daily activities.
What does research indicate about the effectiveness of TAVR compared to traditional surgery?
Statistics show that individuals treated with TAVR or traditional surgery have similar rates of all-cause mortality and disabling stroke at five years, underscoring the effectiveness of both interventions.
How does Amavita support patients undergoing AVR?
Amavita is committed to comprehensive cardiovascular care, featuring advanced imaging technologies and the CardioElite™ program, ensuring patients receive the best possible outcomes through personalized treatment strategies and innovative minimally invasive options.
List of Sources
- Define Aortic Valve Replacement: Key Concepts and Importance
- Electronic Provider Notifications Increase Lifesaving Valve Replacement by More Than 50% in Elderly Patients with Severe Symptomatic Aortic Stenosis | SCAI (https://scai.org/media-center/news-and-articles/electronic-provider-notifications-increase-lifesaving-valve)
- New Heart Valve Helps 83-year-old Hometown Woman Breathe Easier and Creates a Deeper Bond Between Mother and Son (https://news.nm.org/new-heart-valve-helps-83-year-old-hometown-woman-breathe-easier-and-creates-a-deeper-bond-between-mother-and-son)
- 5-Year Outcomes After Transcatheter or Surgical Aortic Valve Replacement in Low-Risk Patients With Aortic Stenosis: (https://jacc.org/doi/10.1016/j.jacc.2025.03.004)
- UVA offers elderly patients new approach to aortic valve replacement (https://uvahealth.com/news/uva-offers-elderly-patients-new-approach-to-aortic-valve-replacement)
- Six-Year Outcomes After Transcatheter vs Surgical Aortic Valve Replacement in Low-Risk Patients With Aortic Stenosis: (https://jacc.org/doi/10.1016/j.jacc.2026.02.5063)
- Explore Types of Aortic Valve Replacement: Surgical vs. Minimally Invasive
- TAVR vs. SAVR: Real-world data highlight advantages of both techniques (https://cardiovascularbusiness.com/topics/clinical/cardiac-surgery/tavr-vs-savr-real-world-data-highlight-advantages)
- Minimally Invasive Aortic Valve Replacement Risks Are Overestimated, Miller School Study Finds – InventUM (https://news.med.miami.edu/minimally-invasive-aortic-valve-replacement-risks-are-overestimated-miller-school-study-finds)
- Surgical versus transcatheter aortic valve replacement in patients age <65 years (https://jtcvsopen.org/article/S2666-2736(25)00235-9/fulltext)
- Benefits of TAVR Remain Consistent in Patients at Low Surgical Risk at Three Years – American College of Cardiology (https://acc.org/about-acc/press-releases/2023/03/05/13/53/benefits-of-tavr-remain-consistent-in-patients)
- 5-Year Outcomes After Transcatheter or Surgical Aortic Valve Replacement in Low-Risk Patients With Aortic Stenosis: (https://jacc.org/doi/10.1016/j.jacc.2025.03.004)
- Determine Selection Criteria: Choosing the Right Aortic Valve Replacement
- Excellent Patient Quote After Heart Surgery – DeWayne Epley (https://heart-valve-surgery.com/heart-surgery-blog/2007/09/12/excellent-heart-valve-surgery-patient-quote-1-dewayne-epley-georgia)
- Assess Risks and Benefits: Understanding Outcomes of Aortic Valve Replacement
- How Serious Is Heart Valve Replacement Surgery and What Are the Risks? (https://int.livhospital.com/how-serious-is-heart-valve-replacement-surgery-and-what-are-the-risks)
- What Heart-Valve Patients Need to Know Before Treatment (https://wsj.com/health/healthcare/what-heart-valve-patients-need-to-know-before-treatment-bf562caa)
- Aortic Valve Replacement Procedures Show Similar Long-Term Survival Rates – News Center (https://news.feinberg.northwestern.edu/2023/11/27/aortic-valve-replacement-procedures-show-similar-long-term-survival-rates)
- Risk/Benefit Comparison of Mechanical and Biologic Valve Replacements – Clinical Research Forum (https://clinicalresearchforum.org/page/RiskBenefit)
- Aortic and Mitral Valve Replacement Surgery – Benefits and Risks (https://medtronic.com/en-us/l/patients/treatments-therapies/surgical-heart-valve-repair-and-replacement/aortic-and-mitral-valve-replacement/benefits-risks.html)