Introduction
A nuclear stress test is an important diagnostic tool that assesses blood flow to the heart. This is especially crucial for elderly patients, who may face higher risks of heart disease. Understanding this procedure can greatly improve health outcomes and help patients prepare effectively for the test.
You might be wondering: what steps can elderly patients take to ensure accurate results and a smooth experience? This article provides essential instructions and insights designed to empower elderly individuals, allowing them to navigate the nuclear stress test with confidence and clarity.
By taking the time to learn about the process, patients can feel more at ease and supported. Remember, you’re not alone in this journey; there are resources and people ready to help you every step of the way.
Understand the Nuclear Stress Test: Key Concepts and Purpose
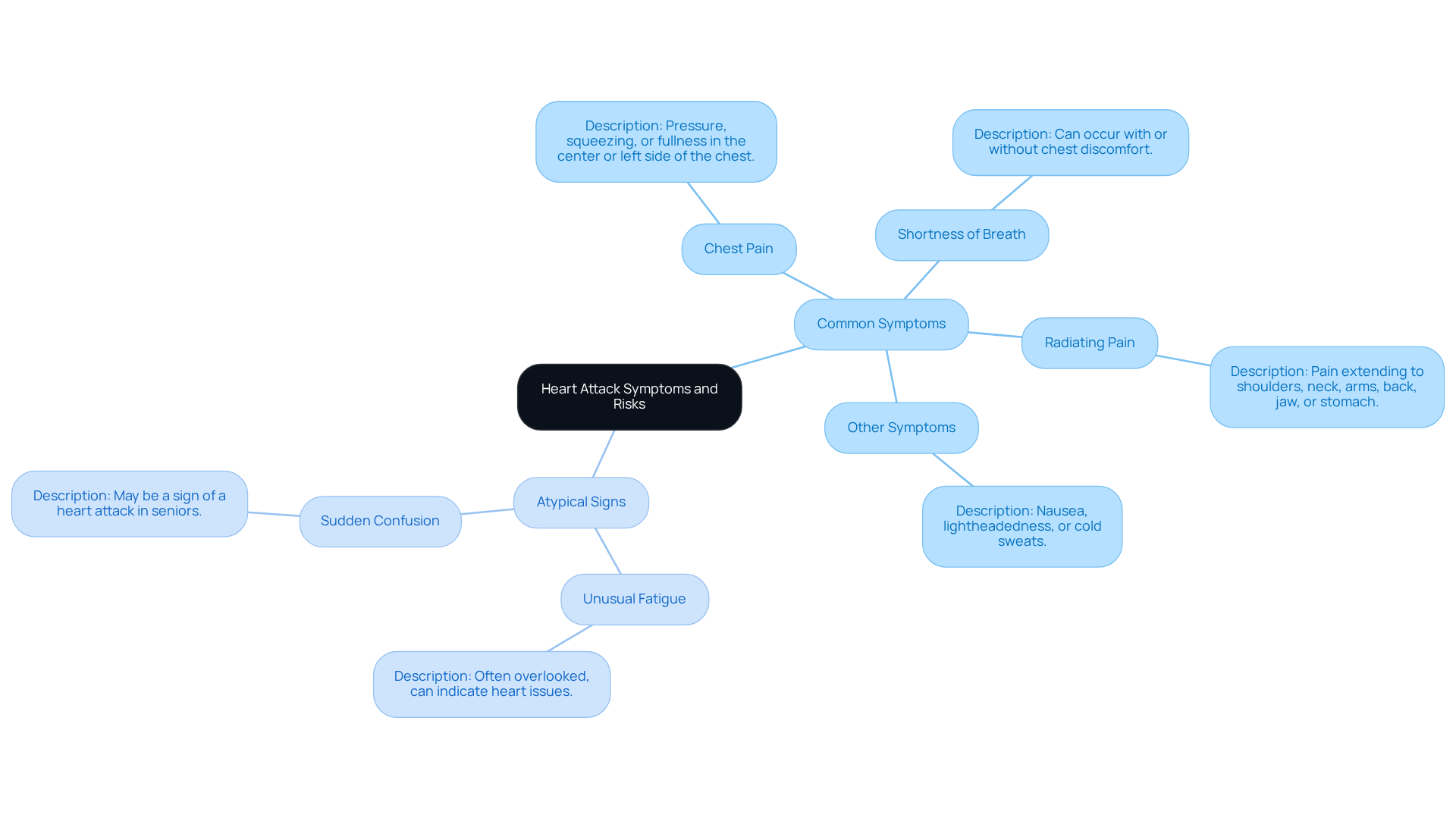
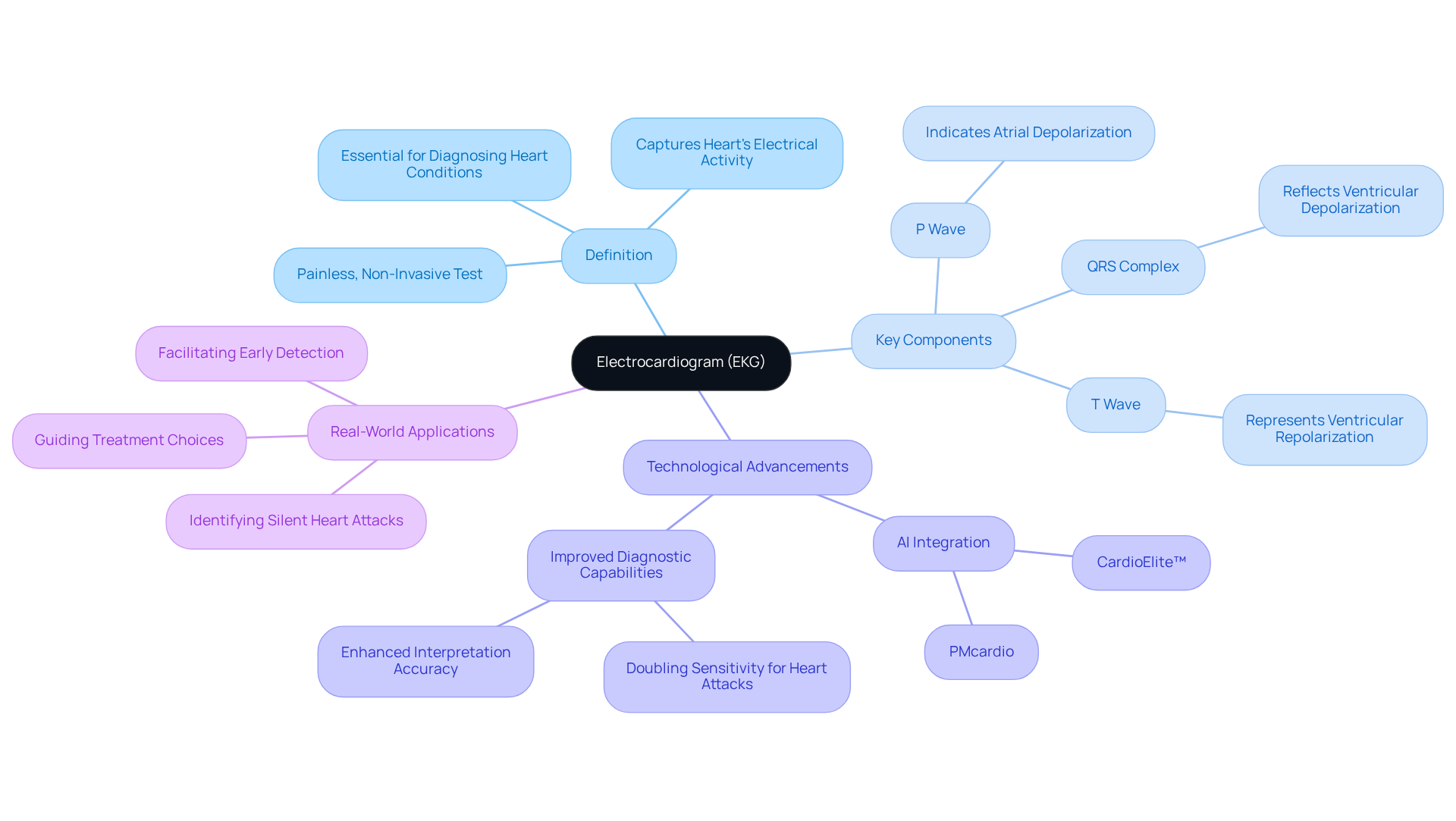
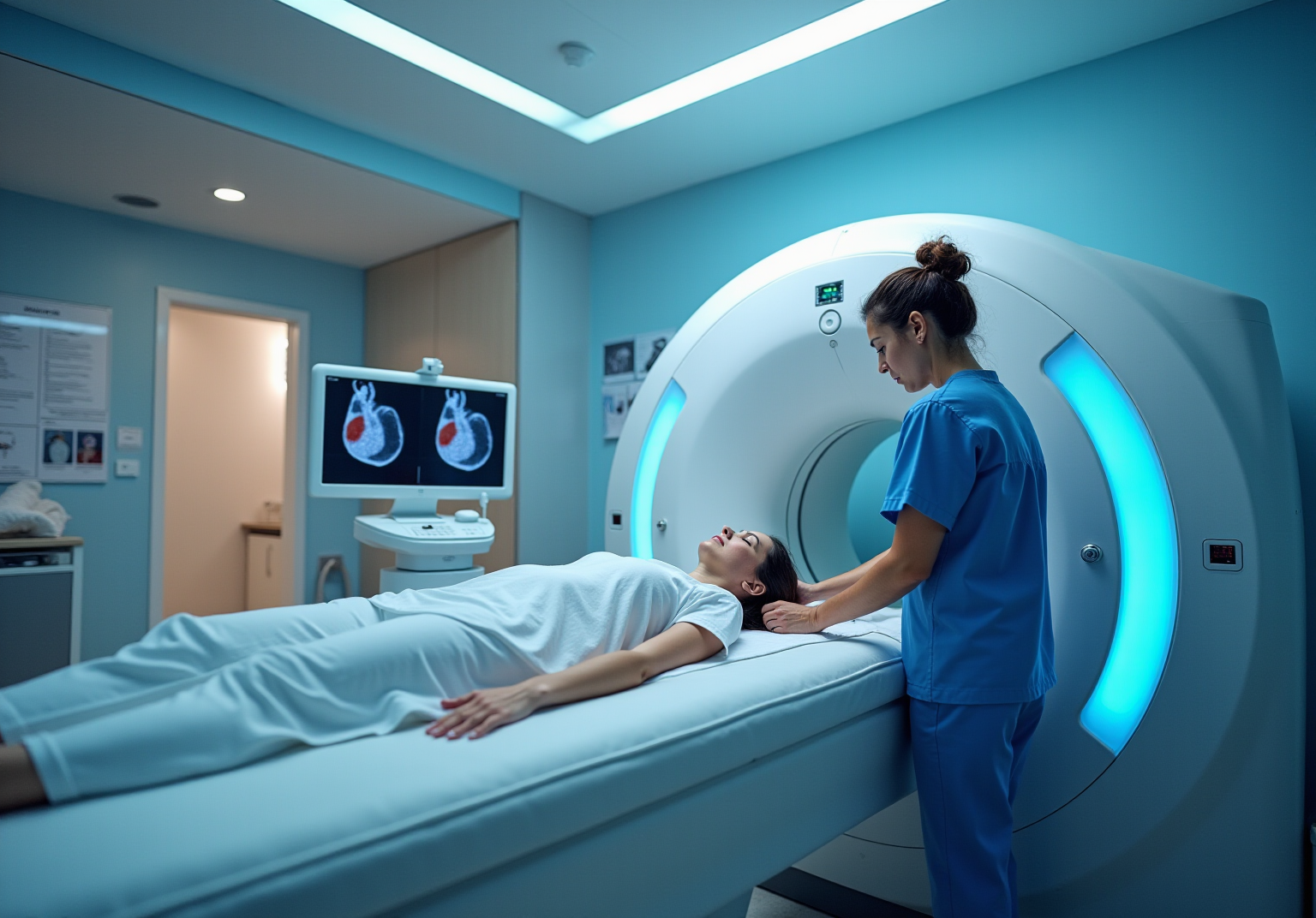
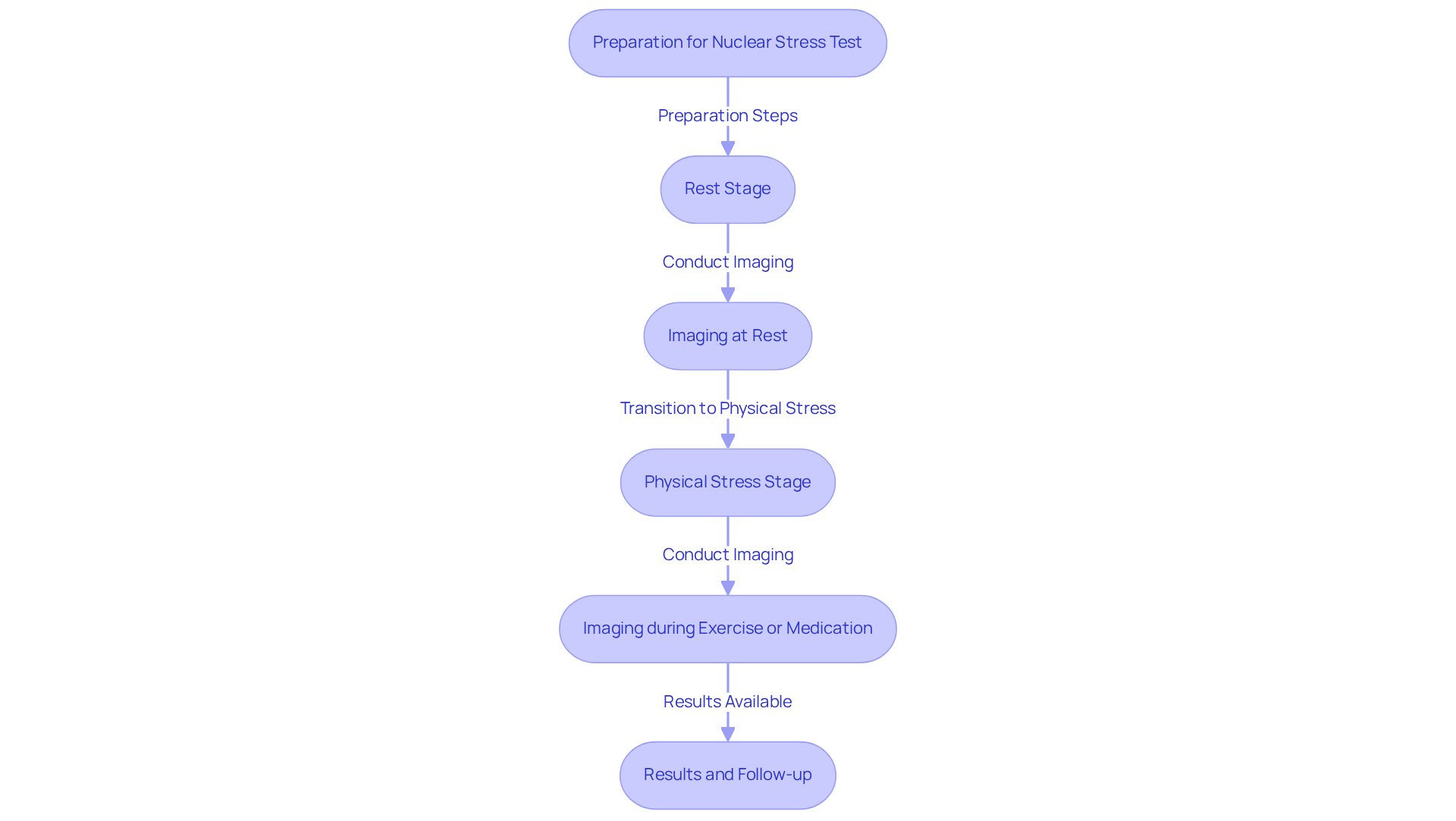
A nuclear stress test is a vital diagnostic procedure that examines blood circulation to the heart muscle during both rest and physical activity. By using a small amount of radioactive material, this test creates detailed images of the heart, helping to identify areas with reduced blood flow that may signal blockages or other heart issues. For our elderly patients, this evaluation is crucial, as it can greatly affect treatment decisions and improve overall health outcomes.
At Amavita Heart and Vascular Health®, we take a comprehensive approach to patient care. We combine advanced risk assessment tools and lifestyle changes with personalized care. The nuclear stress tests are a key part of our preventive cardiology strategy, helping us spot potential heart problems early and tailor treatment plans to fit individual needs.
The procedure typically happens in two stages: one while at rest and another during physical stress, which can be induced by exercise or medication. This thorough method allows healthcare providers to assess heart function accurately. Notably, research indicates that nuclear evaluations are particularly beneficial for individuals aged 85 and older, especially before heart surgery, as they help predict the risk of serious complications like heart failure or arrhythmias.
With the increasing prevalence of heart disease among older adults, the nuclear stress test instructions serve as an essential tool for healthcare providers. It not only helps identify existing problems but also plays a crucial role in assessing the heart’s readiness for non-heart surgeries, ensuring that older patients receive the most appropriate care tailored to their specific health needs. Additionally, through our comprehensive care programs, we enhance cardiac care by offering management strategies that reduce hospital readmissions and improve health outcomes.
To prepare for the test, individuals should avoid caffeine for at least 24 hours beforehand, as it can affect the results. The entire nuclear assessment process may take 3 to 4 hours, so it’s important for individuals to plan accordingly. At Amavita, we are dedicated to providing care that aligns with your lifestyle and health goals, ensuring that every step of your evaluation and treatment is designed around your needs.
Prepare Effectively: Essential Instructions for Patients
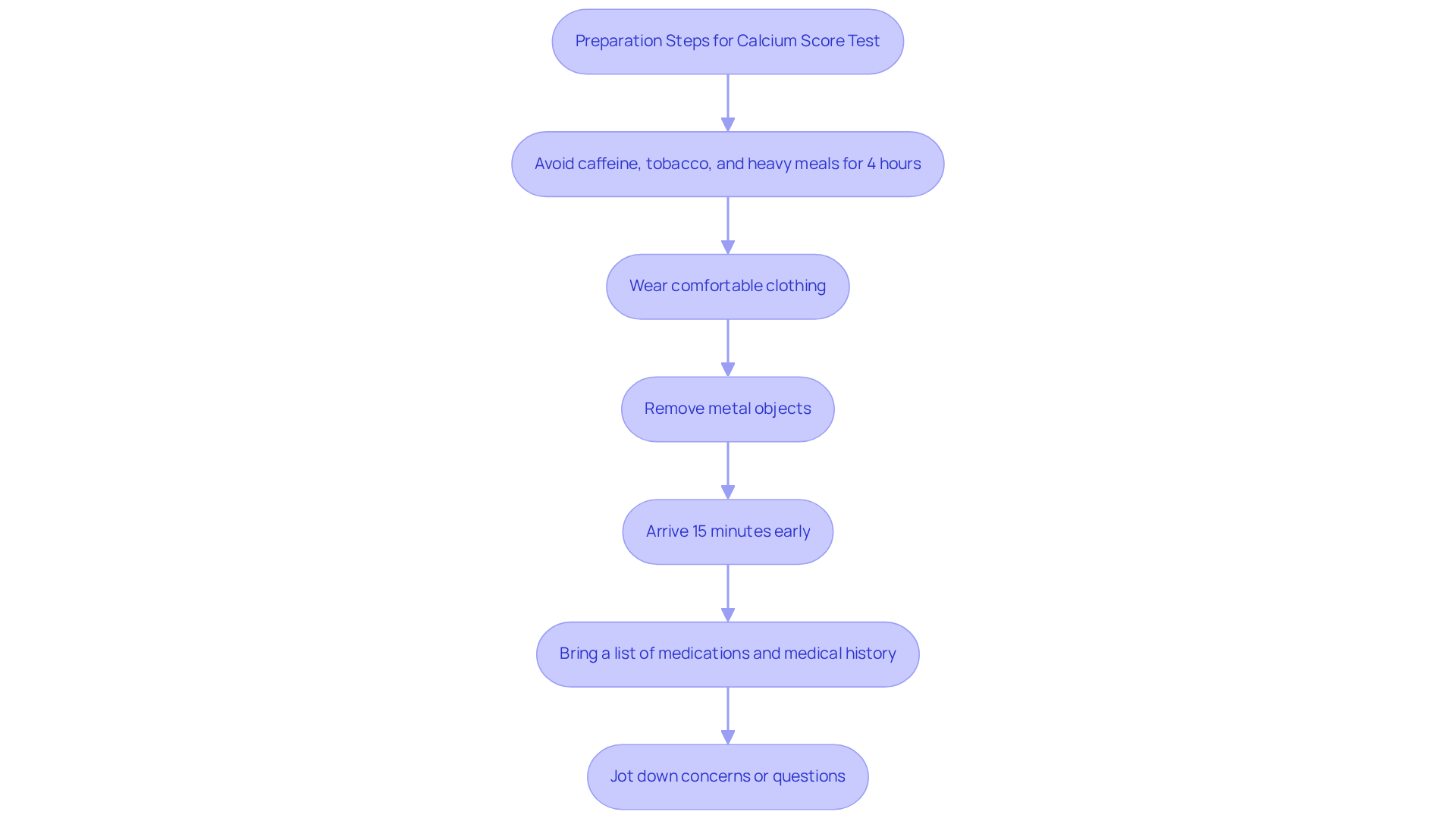
Preparing for a nuclear stress test can feel daunting, especially for elderly patients. But don’t worry; following these instructions can help ensure a successful experience.
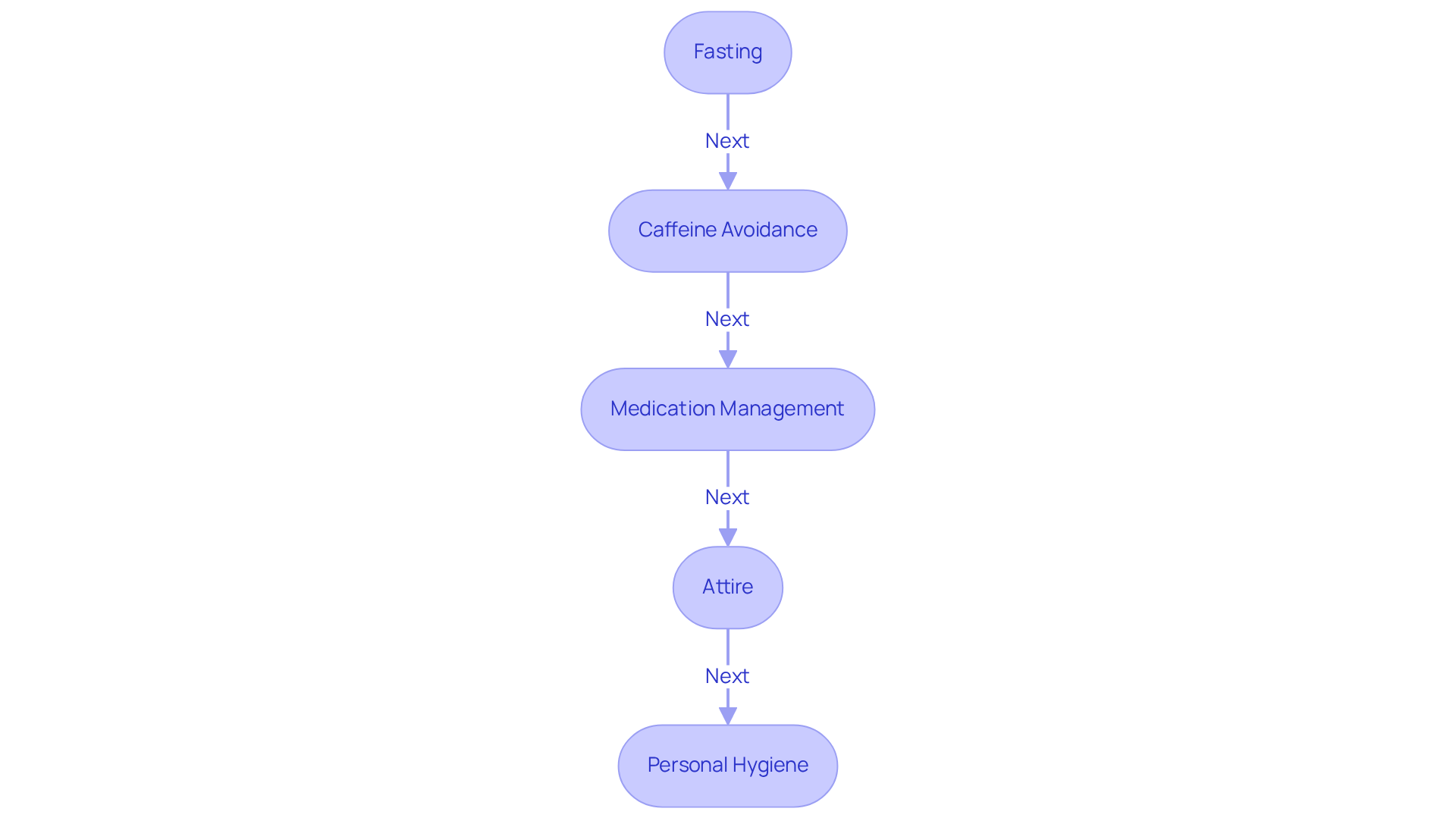
- Fasting is the first step. It’s important to fast for at least 4 hours before your test. If you have diabetes, please follow the specific instructions from your healthcare team. You can drink water during this time. Research shows that proper fasting can significantly improve the accuracy of your results, which is crucial for diagnosing conditions like heart disease.
- Next, let’s talk about caffeine. It’s best to steer clear of caffeine for at least 12 hours before your exam. Caffeine can affect your test results, leading to false positives. Dr. Partha Ghosh reminds us, “Caffeine can lead to false positives in tests, making it crucial for patients to avoid it.”
- Medication management is also key. Please discuss your current medications with your healthcare provider. Some may need to be paused temporarily to ensure the test results are not affected. Remember, never change or stop your medications without consulting a healthcare professional first.
- When it comes to attire, wearing comfortable clothing and suitable footwear is a good idea, as you may need to engage in some physical activity during the assessment.
- Lastly, let’s not forget about hygiene. On the day of your test, take a shower and avoid applying lotions, powders, or fragrances on your chest. These can interfere with the imaging quality.
By adhering to the instructions, you’re taking important steps to ensure your nuclear evaluation goes smoothly and safely, leading to more accurate outcomes. A case study involving a 62-year-old woman with atypical chest pain showed that sticking to these preparation guidelines resulted in a clearer assessment of her condition. This highlights just how vital the instructions truly are. Remember, you’re not alone in this process; your health and comfort are our top priorities.
Know What to Expect: Navigating the Testing Experience
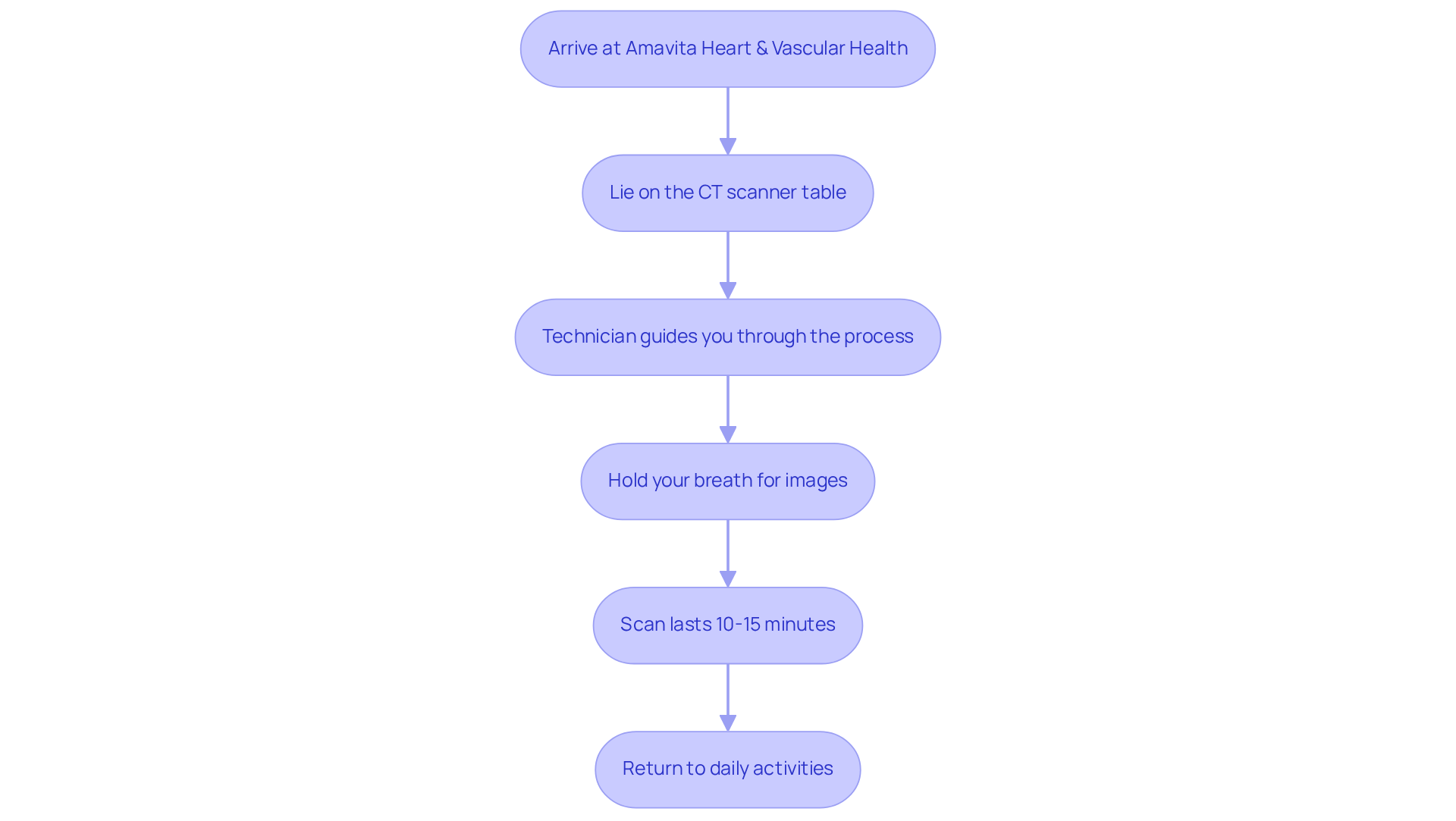
At Amavita Heart and Vascular Health, we understand that for elderly patients, following instructions can be a source of anxiety. That’s why we’ve designed a structured and supportive experience to help you feel at ease throughout the process. Here’s what you can expect:
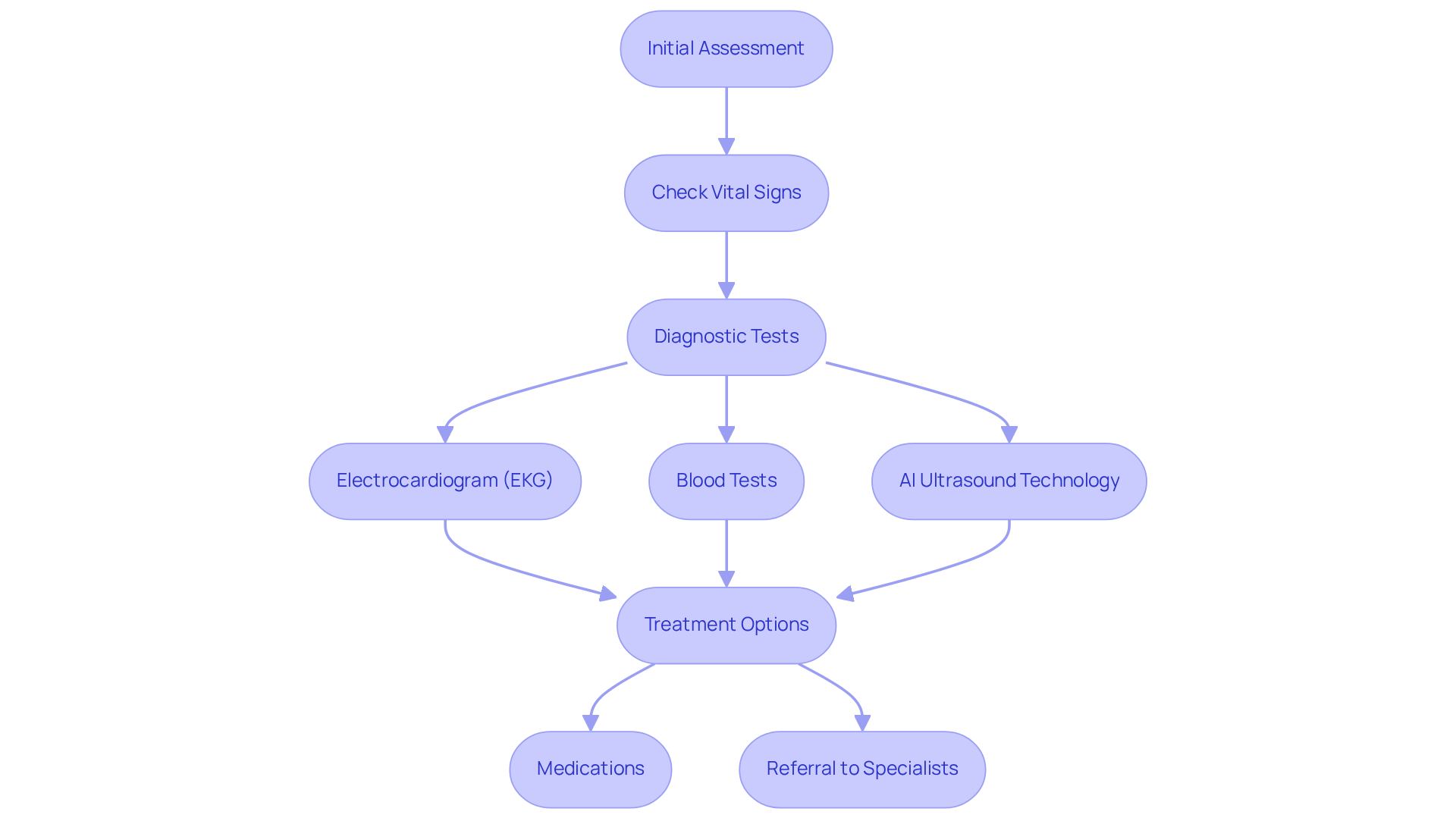
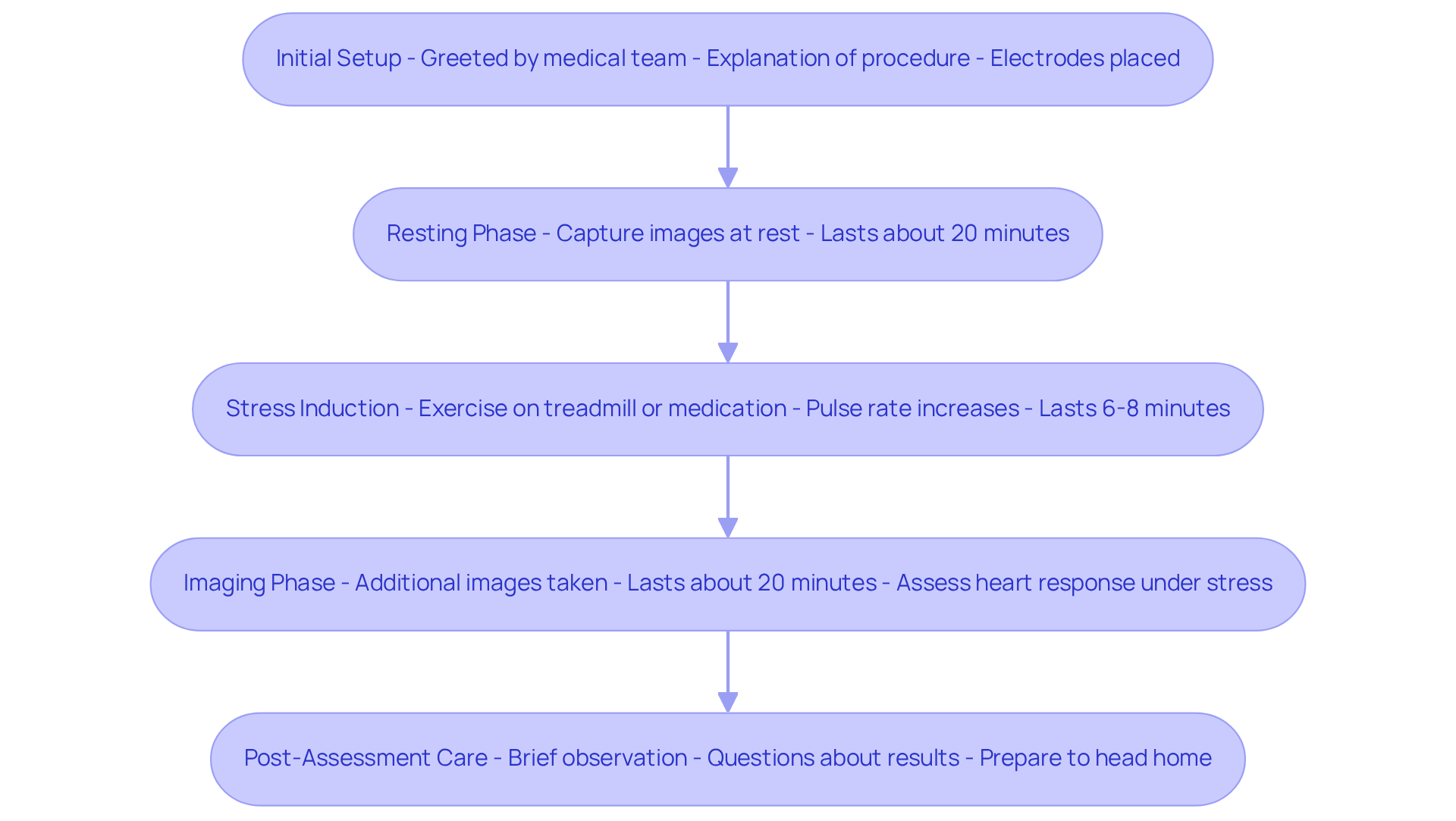
- Initial Setup: When you arrive, our friendly medical team will greet you warmly and explain the procedure in detail. We’ll place electrodes on your chest to monitor your heart activity, ensuring you feel comfortable and informed right from the start.
- Resting Phase: The test begins with a resting phase, where we capture images of your heart while you’re at rest. This phase typically lasts about 20 minutes and allows us to establish a baseline evaluation of your cardiac function.
- Stress Induction: Next, we’ll induce stress, either through exercise or with medication that mimics physical activity. You might notice your pulse rate increasing, and it’s normal to feel a bit short of breath or fatigued during this time. Most older adults manage this well, and we’re here to support you every step of the way.
- Post-Stress Imaging: After the stress induction, we’ll take additional images to see how your heart responds under stress. This also lasts around 20 minutes and is crucial for assessing your cardiovascular health. At Amavita, we use advanced imaging technology to ensure accurate evaluations, guided by the expertise of Dr. Martinez-Clark, whose training at Harvard enhances our comprehensive care approach.
- Final Observation: Once the assessment is complete, we’ll observe you briefly to ensure your well-being before you head home. We encourage you to ask any questions about your results or the procedure.
Understanding these steps can significantly reduce anxiety and lead to a smoother testing experience, especially for those who may have concerns about their heart health. At Amavita, we believe that cardiac care should revolve around your life, not just your condition. Regular assessments through nuclear stress tests are essential, as they help identify potential issues like coronary artery disease, which is common among older adults. We also recommend wearing comfortable clothing and shoes to enhance your comfort during the test.
Interpret Results: Understanding Your Nuclear Stress Test Outcomes
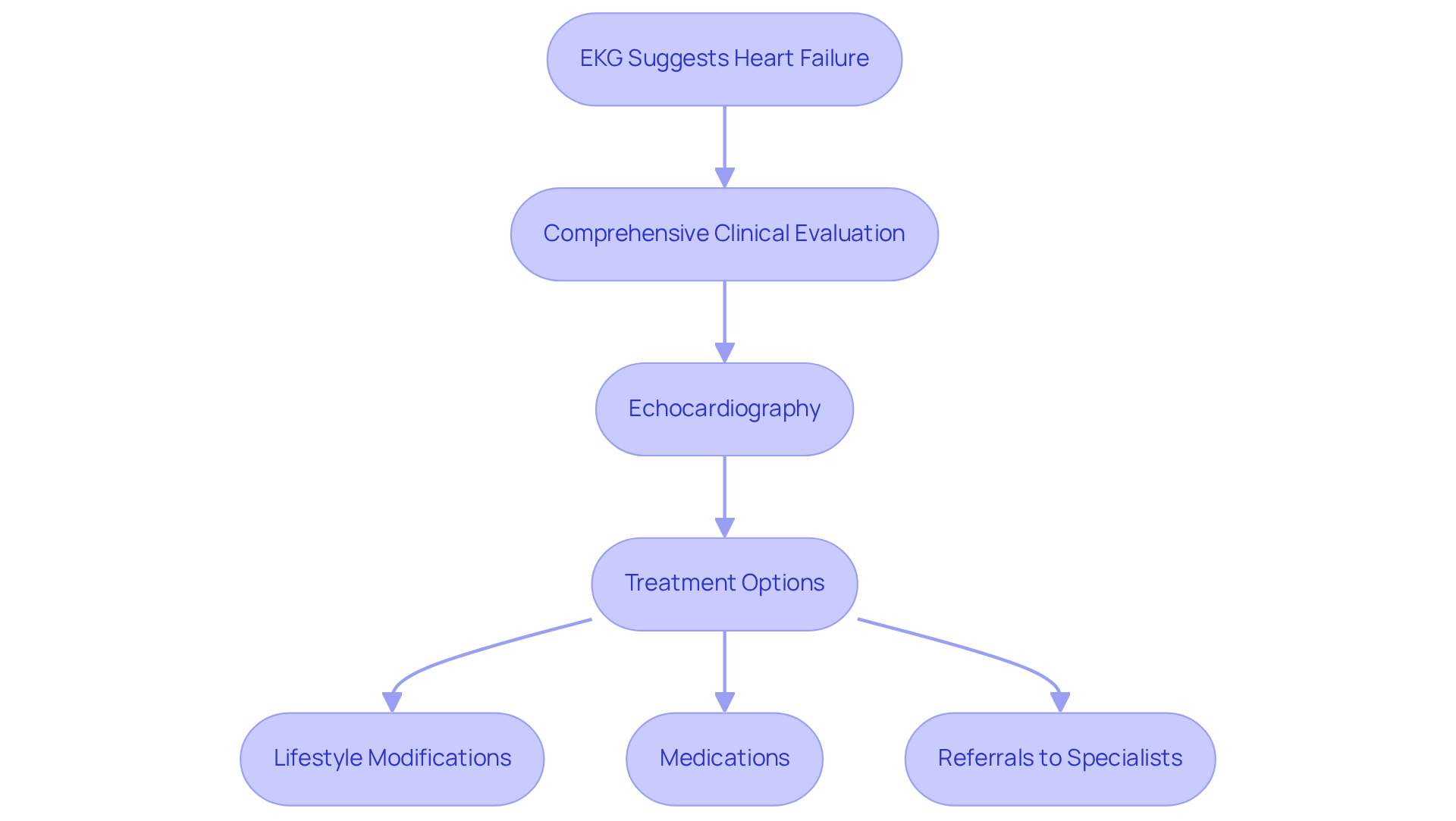
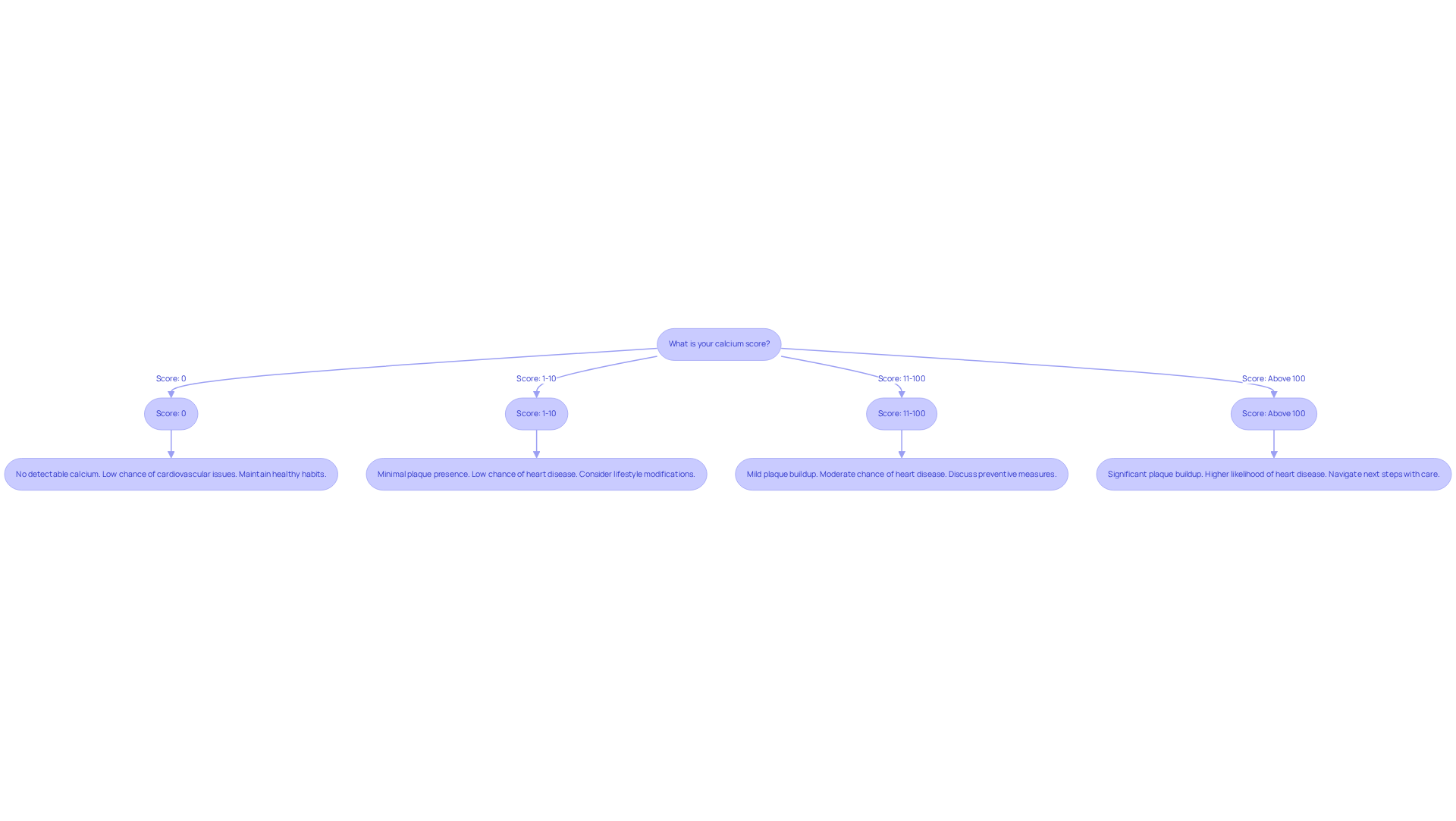
After a test, your cardiologist will carefully analyze the results, which can be understood in a few key ways:
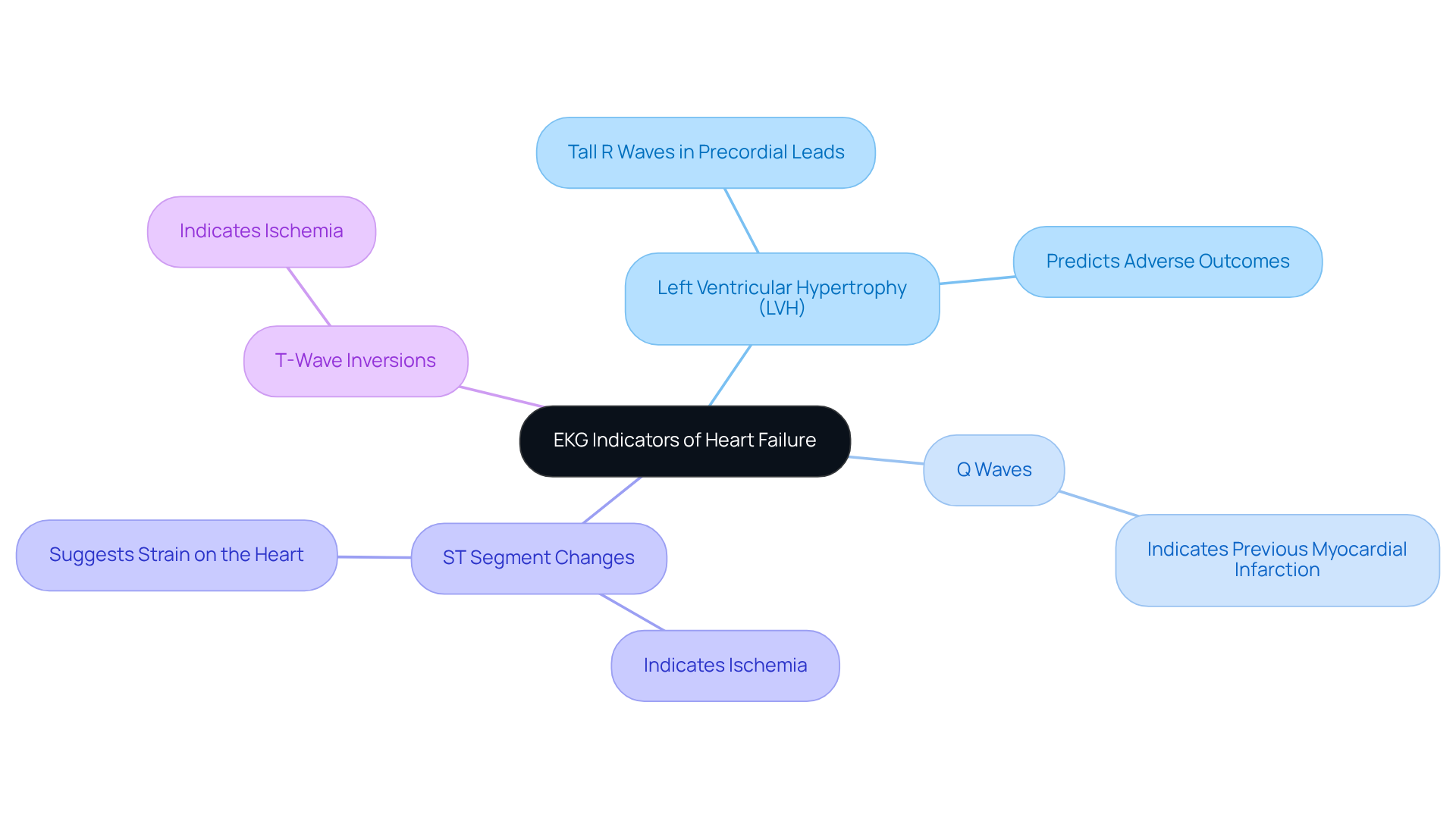
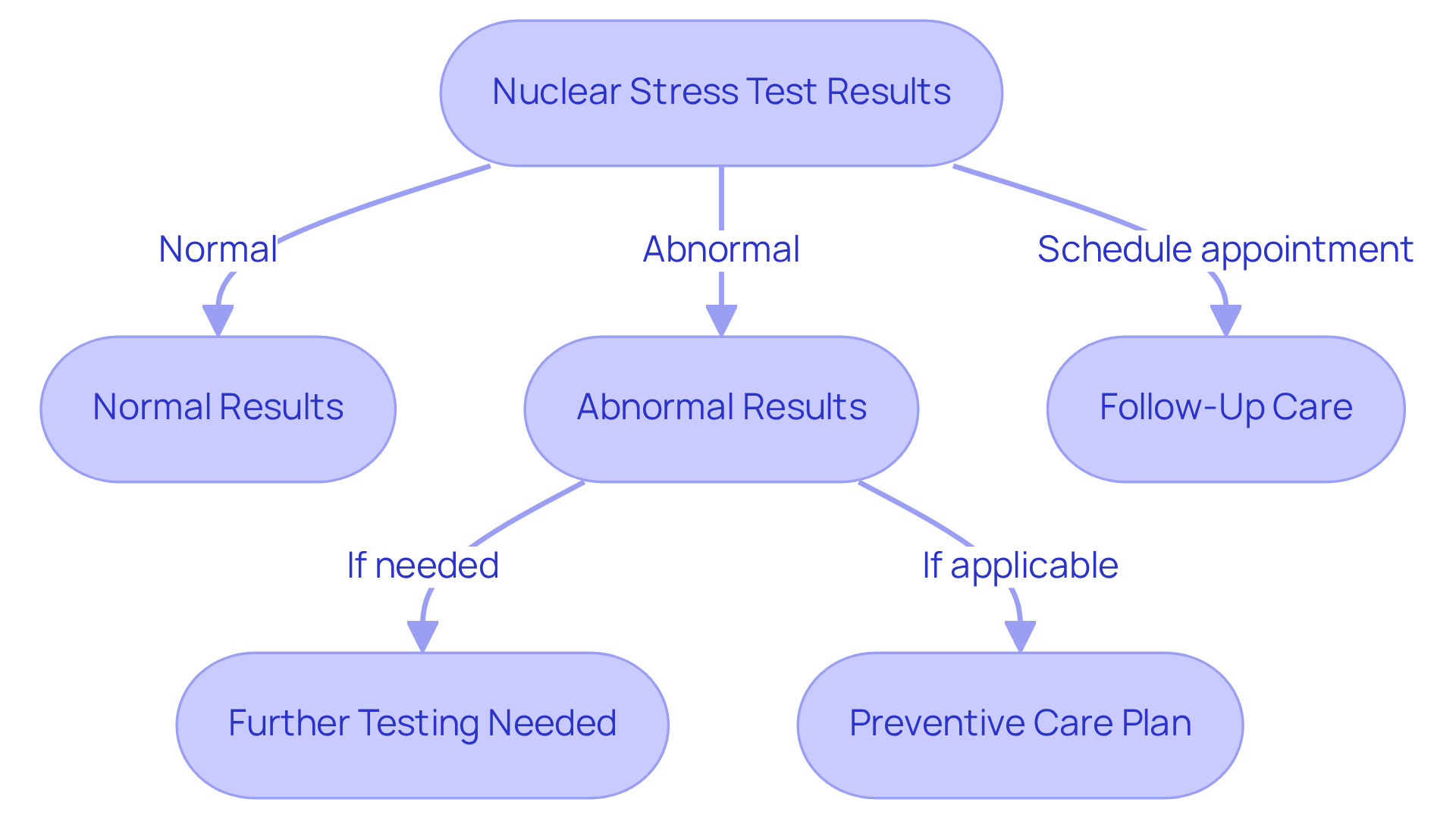
- Normal Results: If both resting and exertion images show normal blood flow, it means your heart is functioning well, without significant blockages. This is great news and a sign of good health!
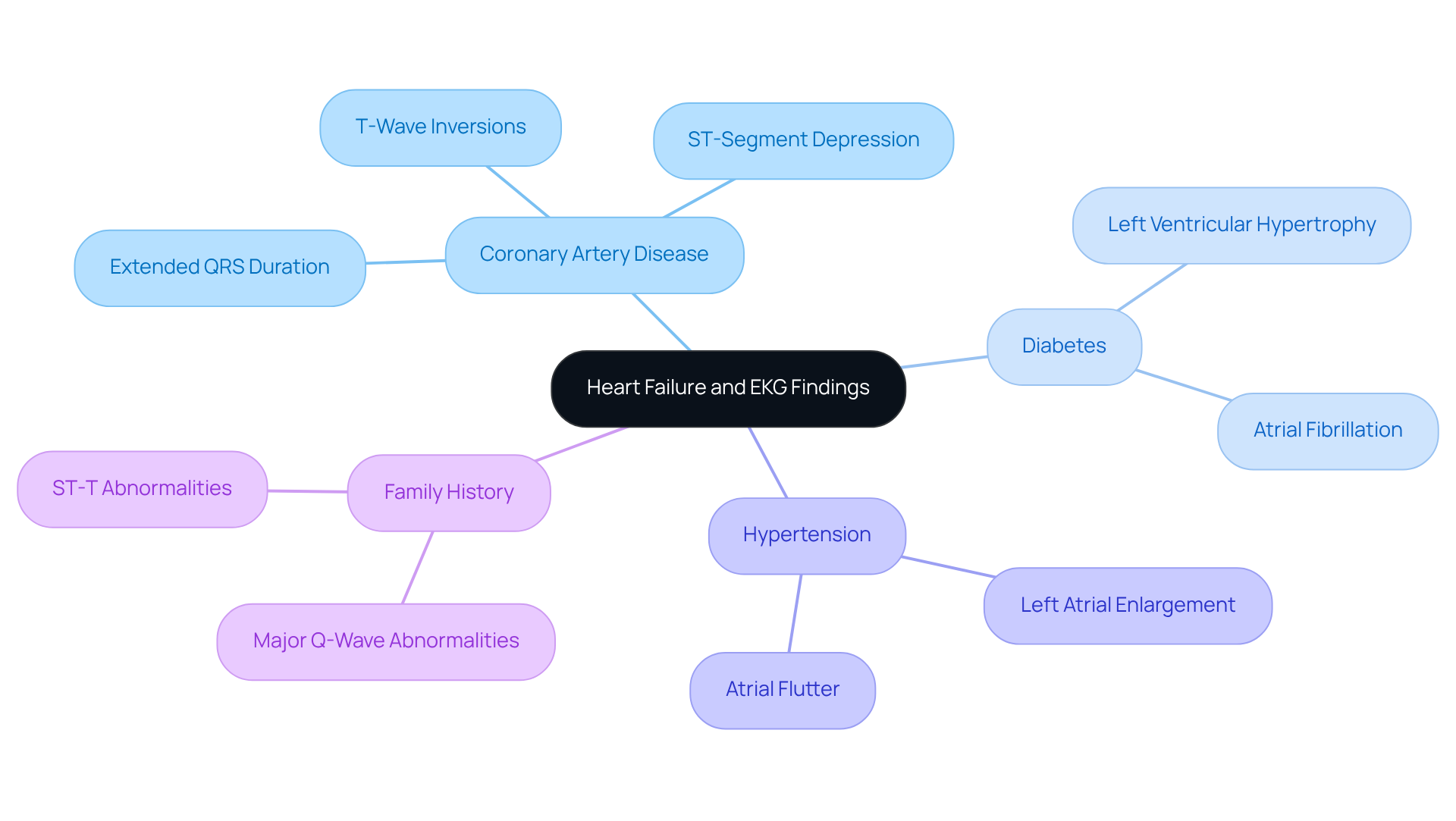
- Abnormal Results: If there are areas of reduced blood flow during stress, it may indicate ischemia or other heart conditions. This could mean that further testing or treatment options are necessary. At Amavita, our team ensures that any follow-up you need is included in your care plan, especially if you have risk factors like a family history of heart issues, high blood pressure, or diabetes.
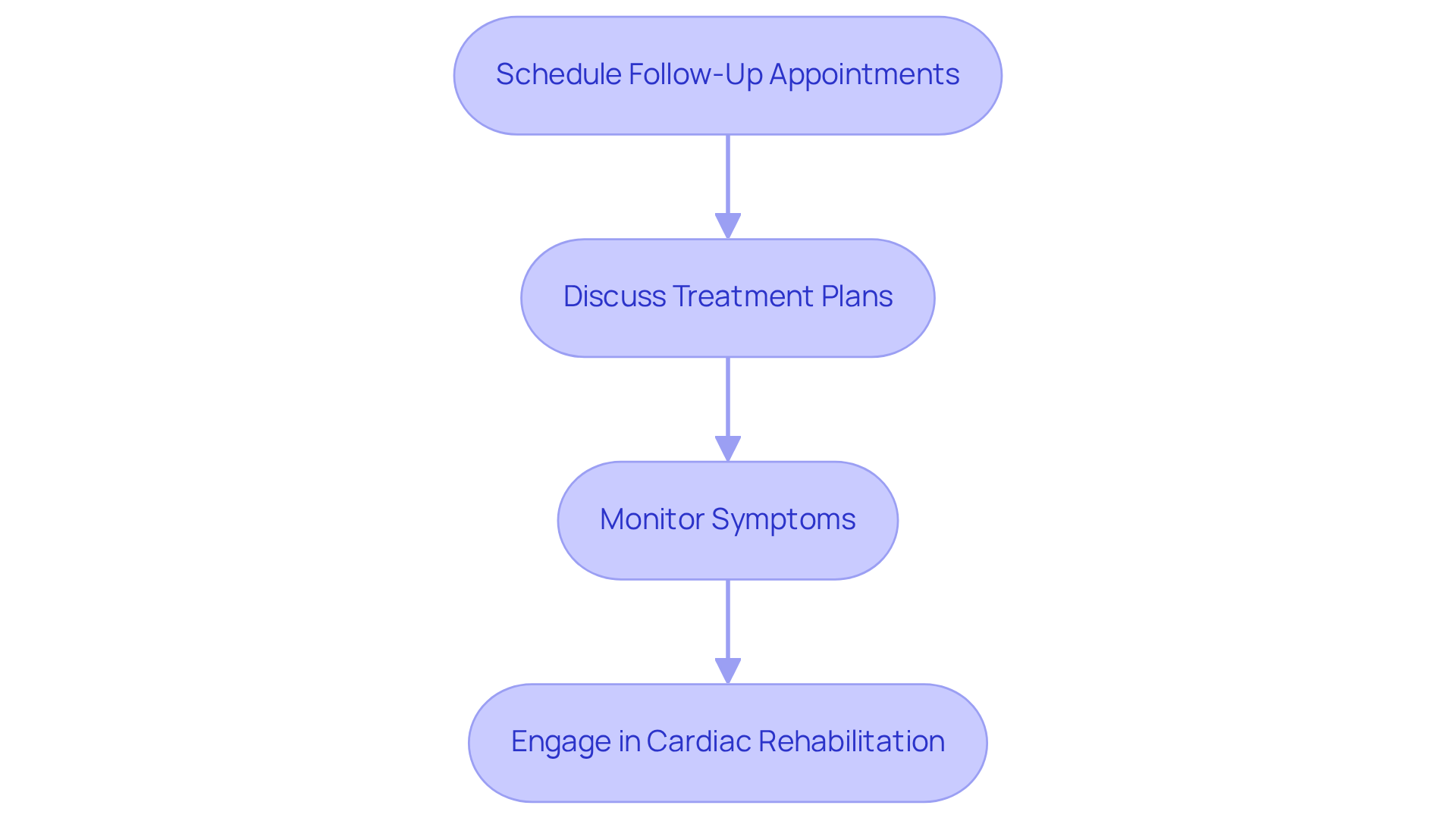
- Follow-Up Care: It’s really important for you, especially if you’re older, to schedule an appointment to discuss your results in detail. This meeting provides an opportunity for you to ask questions and understand the instructions, as well as what the results mean for your health. We want to help you create a plan that fits your specific condition and lifestyle.
Understanding these results is crucial for making decisions about your future care and lifestyle changes. We’re here to support you in enhancing your quality of life, especially as you navigate your health journey.
Conclusion
A nuclear stress test plays a vital role in assessing heart health, especially for our elderly loved ones. By grasping the details of this important diagnostic procedure, individuals can truly understand its value in spotting potential heart issues and crafting tailored treatment plans. Throughout this article, we’ve highlighted how crucial it is to follow specific preparation guidelines, ensuring accurate results and a smooth testing experience.
Key points to remember include:
- The necessity of fasting
- Steering clear of caffeine
- Managing medications before the test
Moreover, the structured process of the nuclear stress test-from the initial setup to interpreting results-showcases the comprehensive care approach that healthcare providers take. This thorough preparation not only boosts the accuracy of the evaluation but also eases anxiety for patients, making sure they feel supported every step of the way.
Ultimately, understanding and following the nuclear stress test instructions is essential for elderly patients. It opens the door to early detection and effective management of heart conditions, which can significantly enhance overall health outcomes. Embracing these guidelines is a proactive step toward maintaining heart health and improving quality of life. Engaging with healthcare professionals and asking questions about the process can empower patients to take charge of their cardiovascular health, leading to informed decisions and personalized care.
Frequently Asked Questions
What is a nuclear stress test?
A nuclear stress test is a diagnostic procedure that evaluates blood circulation to the heart muscle during rest and physical activity, using a small amount of radioactive material to create detailed images of the heart.
Why is a nuclear stress test important for elderly patients?
It is crucial for elderly patients as it can greatly affect treatment decisions and improve overall health outcomes, particularly in identifying coronary artery disease and assessing heart function before surgeries.
How is the nuclear stress test conducted?
The procedure is conducted in two stages: one while the patient is at rest and another during physical stress, which can be induced by exercise or medication.
What are the benefits of a nuclear stress test for individuals aged 85 and older?
Research indicates that nuclear evaluations are particularly beneficial for individuals aged 85 and older, as they help predict the risk of serious complications like heart failure or arrhythmias before heart surgery.
What should individuals do to prepare for a nuclear stress test?
Individuals should avoid caffeine for at least 24 hours before the test, as it can affect the results.
How long does the nuclear stress test process take?
The entire nuclear assessment process typically takes 3 to 4 hours.
What role does the CardioElite™ program play in cardiac care?
The CardioElite™ program enhances cardiac care by offering comprehensive management strategies that reduce hospital readmissions and improve health outcomes for patients.
How does Amavita Heart and Vascular Health® approach cardiac evaluations?
Amavita combines advanced risk assessment tools and lifestyle changes with personalized care as part of their preventive cardiology strategy to spot potential heart problems early and tailor treatment plans to individual needs.
List of Sources
- Understand the Nuclear Stress Test: Key Concepts and Purpose
- Is a Nuclear Stress Test Safe for Elderly People? (https://healthline.com/health/is-nuclear-stress-test-safe-for-elderly)
- Stress Nuclear: Methodology and Case Studies – Houston Methodist Hospital (https://mdvideos.houstonmethodist.org/videos/stress-nuclear-methodology-and-case-studies)
- mayoclinic.org (https://mayoclinic.org/tests-procedures/nuclear-stress-test/about/pac-20385231)
- FAQs About Cardiac Stress Tests for Elderly Patients – Advanced Heart and Vascular Institute (https://advancedhvi.com/2025/04/18/faqs-about-cardiac-stress-tests-for-elderly-patients)
- Prepare Effectively: Essential Instructions for Patients
- Clinical Case Studies (https://siemens-healthineers.com/en-us/molecular-imaging/mi-clinical-corner/clinical-case-studies)
- mayoclinic.org (https://mayoclinic.org/tests-procedures/nuclear-stress-test/about/pac-20385231)
- Know What to Expect: Navigating the Testing Experience
- Average Treadmill Time for Stress Test by Age Explained (https://getlabtest.com/news/post/average-treadmill-time-stress-test-age)
- What Is the Average Time on a Treadmill for a Stress Test by Age? (https://drsalmamazhar.com/what-is-the-average-time-on-a-treadmill-for-a-stress-test-by-age)
- FAQs About Cardiac Stress Tests for Elderly Patients – Advanced Heart and Vascular Institute (https://advancedhvi.com/2025/04/18/faqs-about-cardiac-stress-tests-for-elderly-patients)
- healthline.com (https://healthline.com/health/stress-test-results-by-age-chart)
- Nuclear Cardiology Procedure Duration: How Long Does a Stress Test Take? – Liv Hospital (https://int.livhospital.com/nuclear-cardiology-procedure-duration-stress-test-timeline)
- Interpret Results: Understanding Your Nuclear Stress Test Outcomes
- Cases from a busy nuclear cardiology laboratory – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9542470)
- theheartclinics.com (https://theheartclinics.com/post/heres-how-to-interpret-the-results-of-your-exercise-stress-test)
- tmlt.org (https://tmlt.org/case-studies/failure-to-monitor-patient-during-stress-test)
- Appeals Court Orders New Trial for Cardiologists in Stress-Test Death Case (https://thecardiologyadvisor.com/features/stress-test-death-case)