Introduction
Abnormal nuclear stress test results can understandably cause anxiety for many individuals. These results often signal potential heart issues that need immediate attention. It’s essential to grasp what these results mean, as they not only guide the next steps in your medical care but also empower you to take charge of your cardiovascular health.
What should you do when faced with such unsettling news? How can you navigate the complex landscape of follow-up care and lifestyle changes? This guide is here to help demystify the nuclear stress test process and provide you with actionable insights for managing abnormal results. We want to ensure that you feel equipped to make informed decisions about your heart health.
In addition to this, remember that you’re not alone in this journey. Many have walked this path and found ways to manage their health effectively. By understanding your results and the steps that follow, you can take proactive measures to support your heart. Let’s explore this together, ensuring you feel supported every step of the way.
Understand the Nuclear Stress Test Process
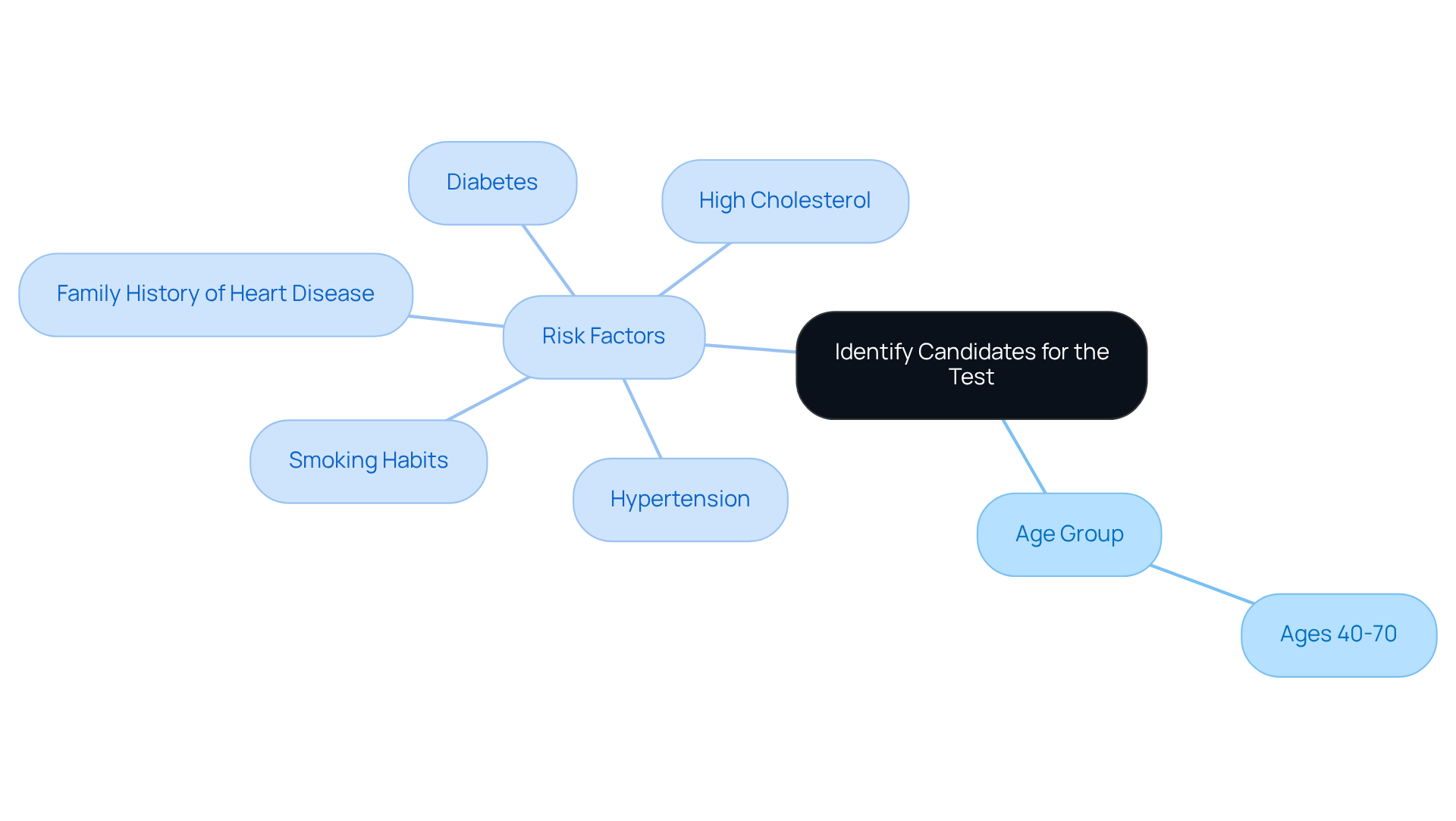
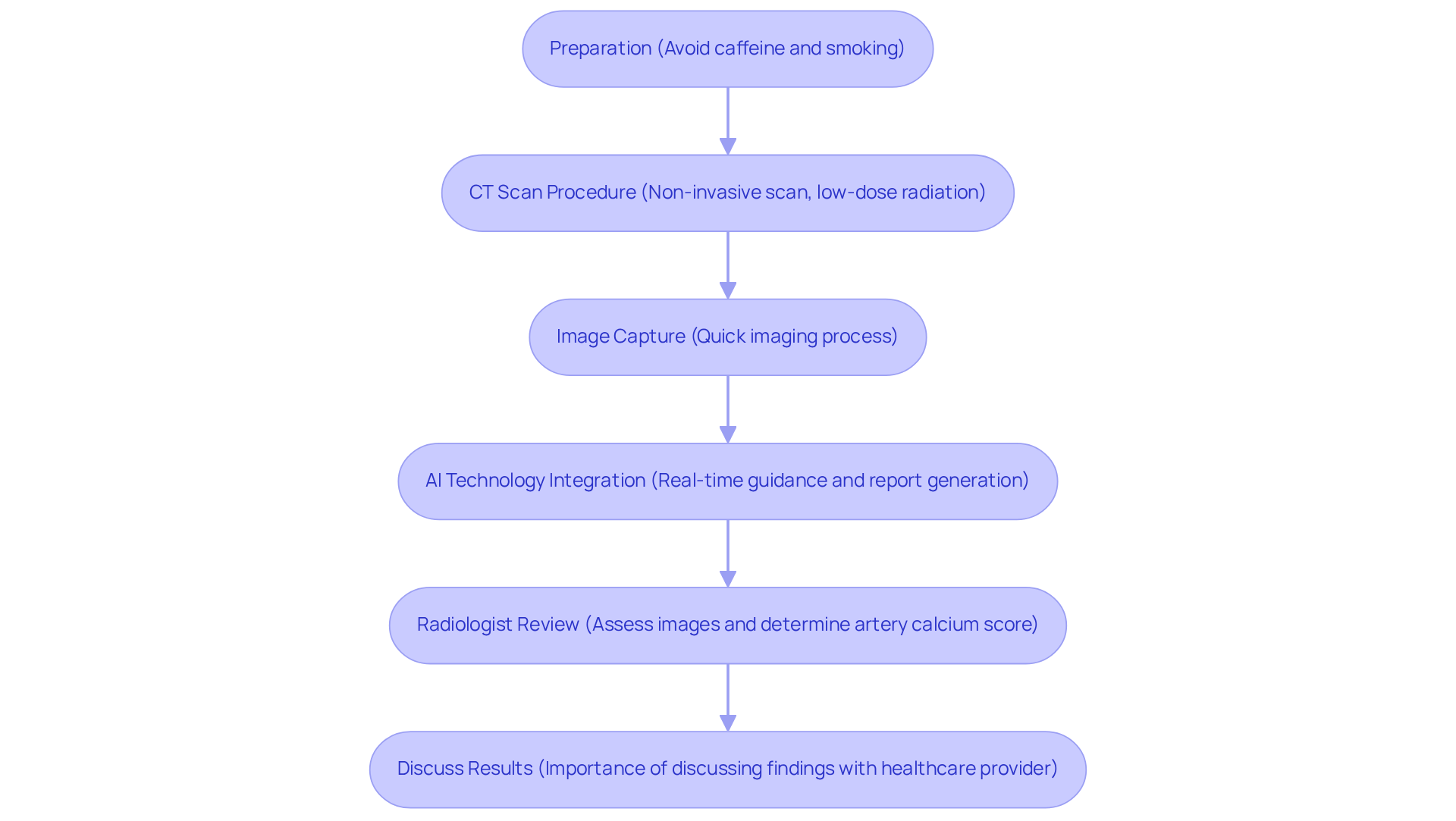
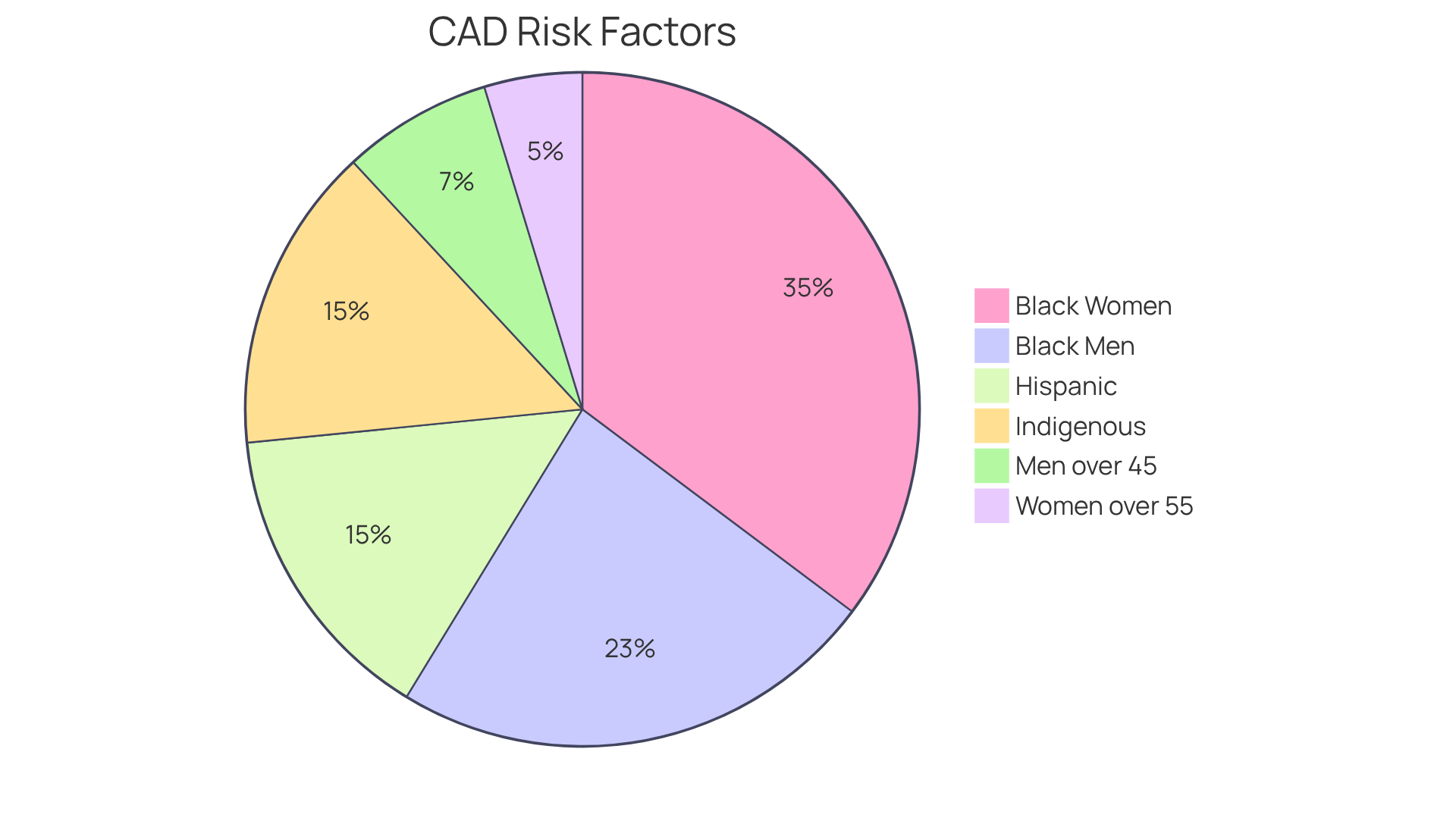
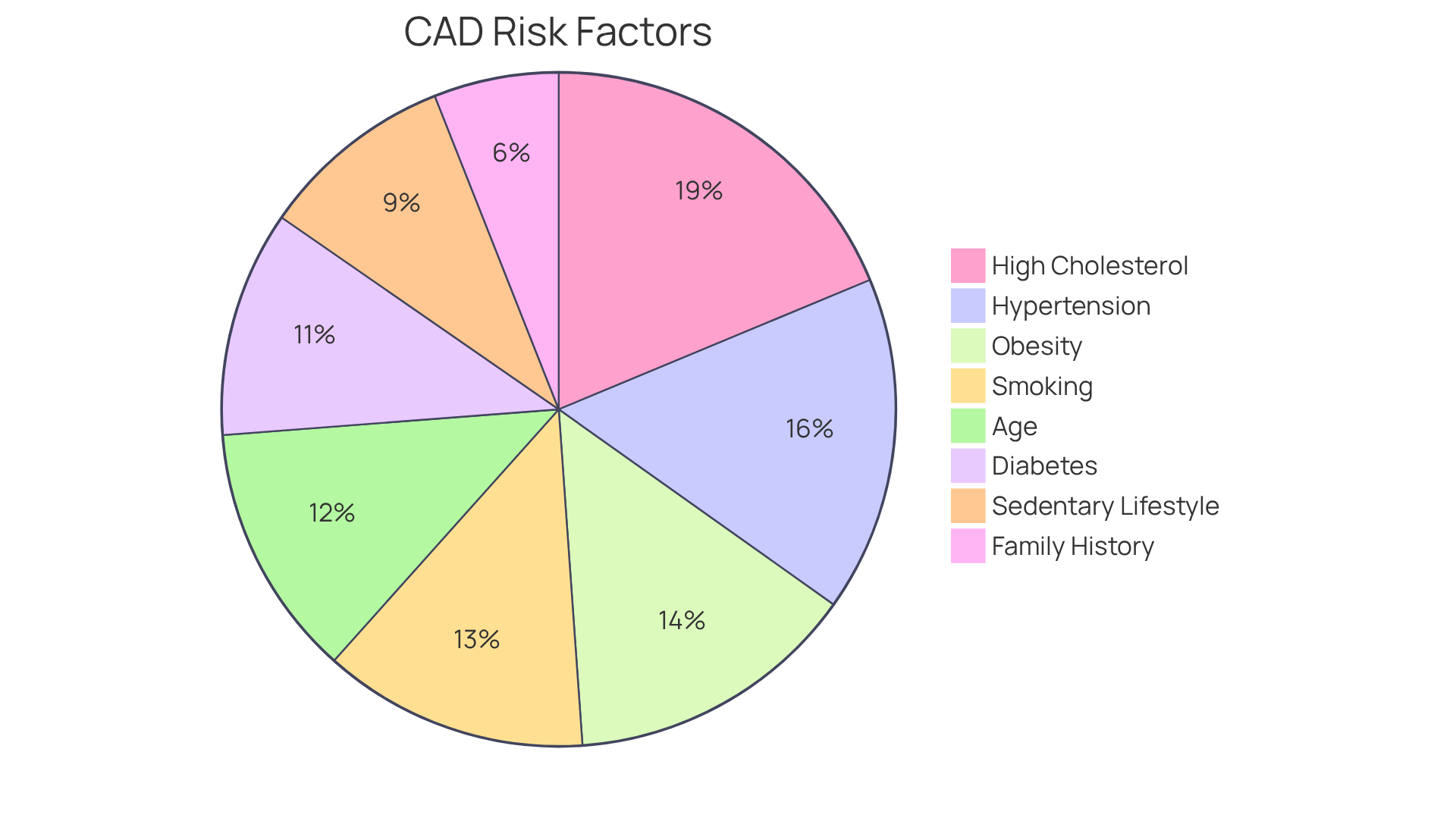
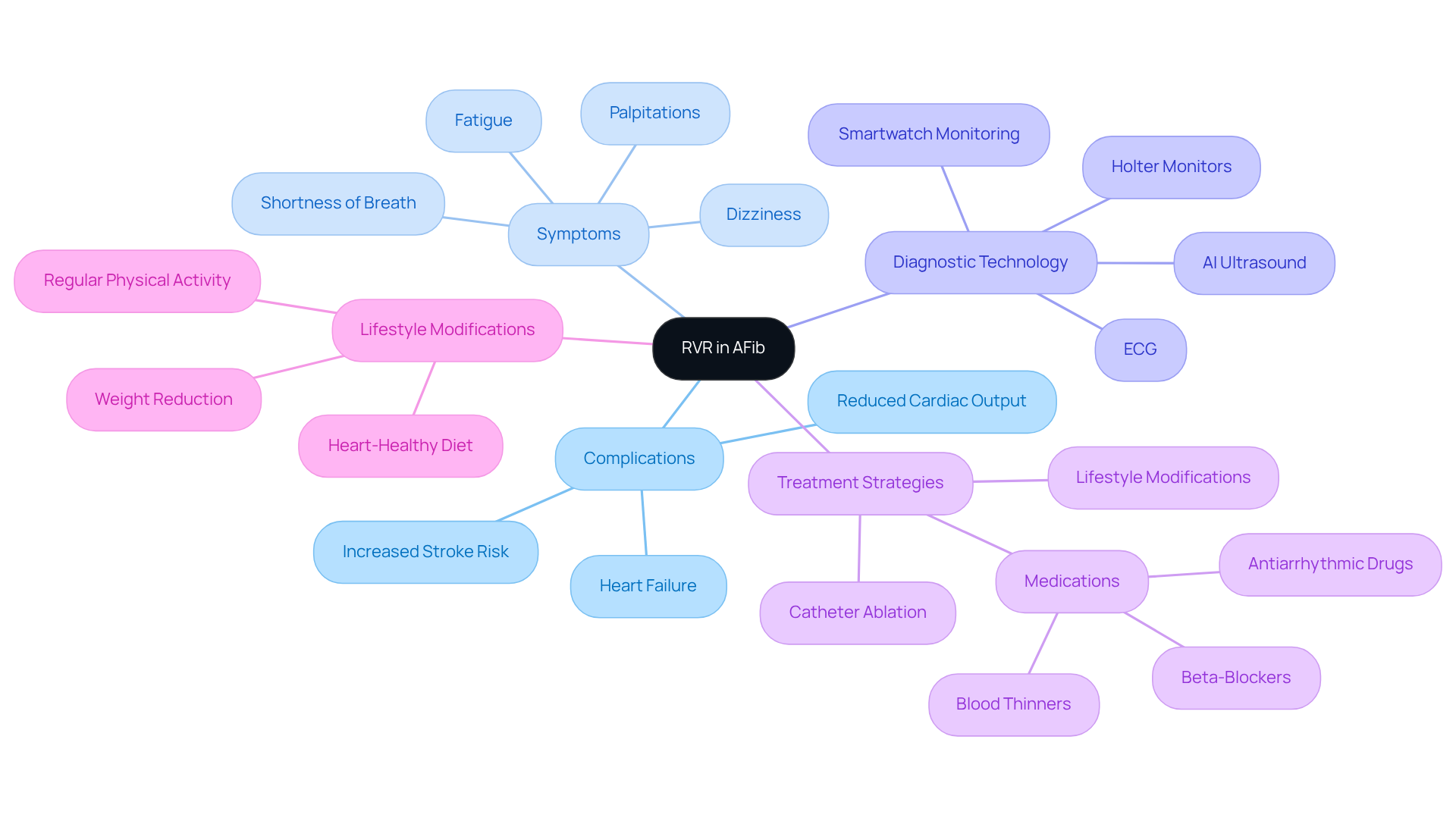
A nuclear stress test is a vital diagnostic procedure that helps assess blood circulation to your heart muscle during both rest and stress. This test is especially beneficial for those at higher risk, such as individuals with diabetes, hypertension, or a family history of heart disease. Let’s break it down into two main phases:
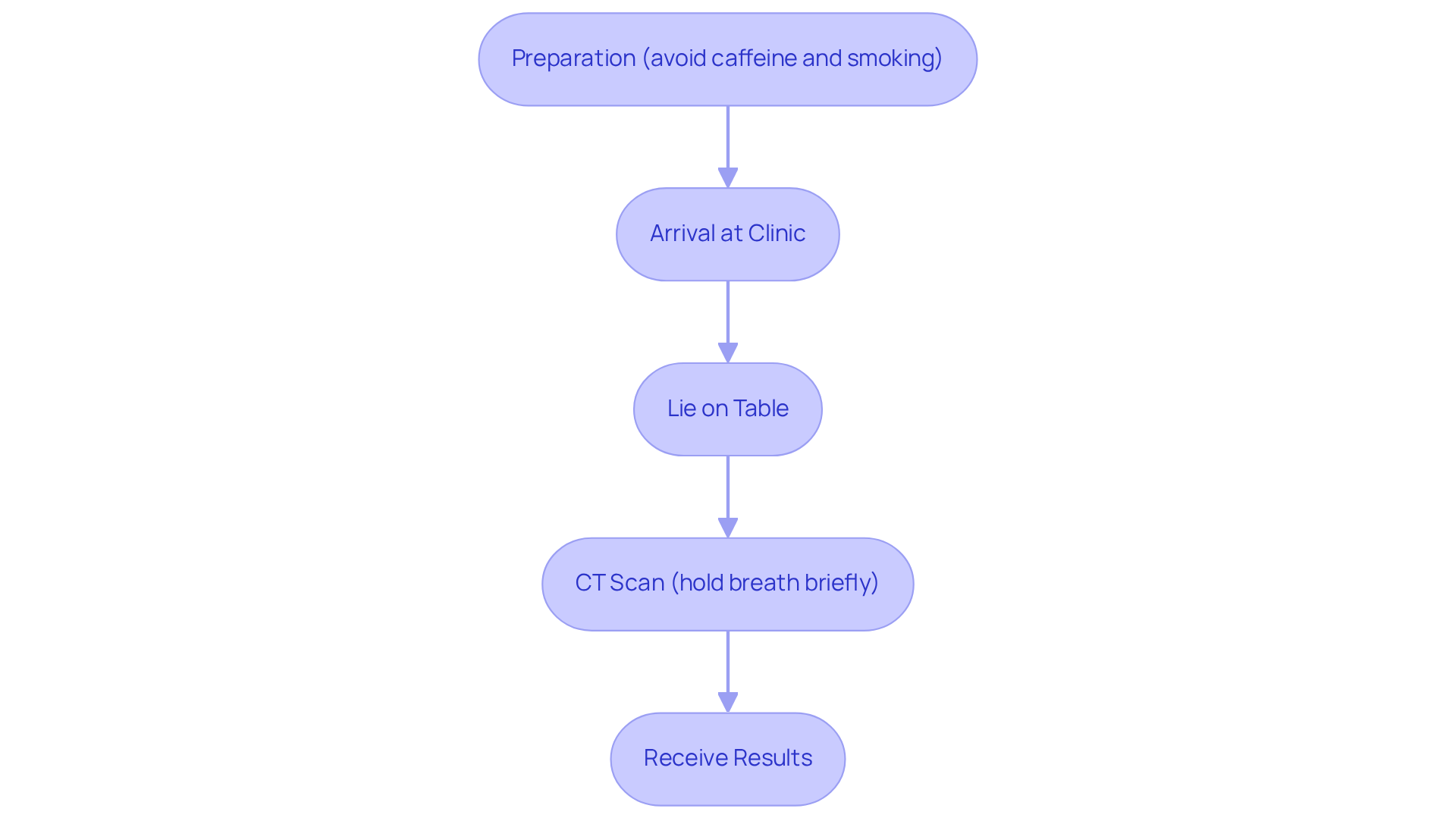
- Resting Phase: A small amount of a radioactive tracer, usually technetium-99 (Tc-99), is injected into a vein. This allows us to take images of your heart and see how blood flows while you’re at rest. Don’t worry; this tracer loses its radioactivity within one to two days.
- Stress Phase: You’ll either exercise on a treadmill or receive medication that mimics exercise effects. Afterward, we’ll take more images to observe how blood flow changes under stress.
This comparison of blood flow during rest and exertion is crucial for identifying potential heart issues, like coronary artery disease. With around 10 million tests performed each year in the U.S., understanding this procedure empowers you to take an active role in your healthcare journey.
At Amavita Heart and Vascular Health®, we believe that your healthcare should revolve around your life, not just your condition. Our preventive cardiology approach combines advanced risk evaluation tools with personalized interventions to significantly lower your risk of a cardiac event. It’s important to note that the radiation exposure from a nuclear stress test is about 11 millisieverts, which is roughly three times the yearly dose from everyday life. We also want you to be aware of preparation guidelines, including dietary restrictions and medication management, to ensure you get the most accurate results.
Real-world examples show that abnormal results might indicate previous heart damage, while normal images suggest a low likelihood of heart disease. However, it’s essential to consider potential risks associated with the examination, such as radiation exposure and allergic reactions. Engaging with this information can help you navigate your healthcare more effectively, especially when thinking about treatments tailored to your unique conditions and lifestyle.
Remember, you’re not alone in this journey. We’re here to support you every step of the way.
Identify Abnormal Results and Their Implications
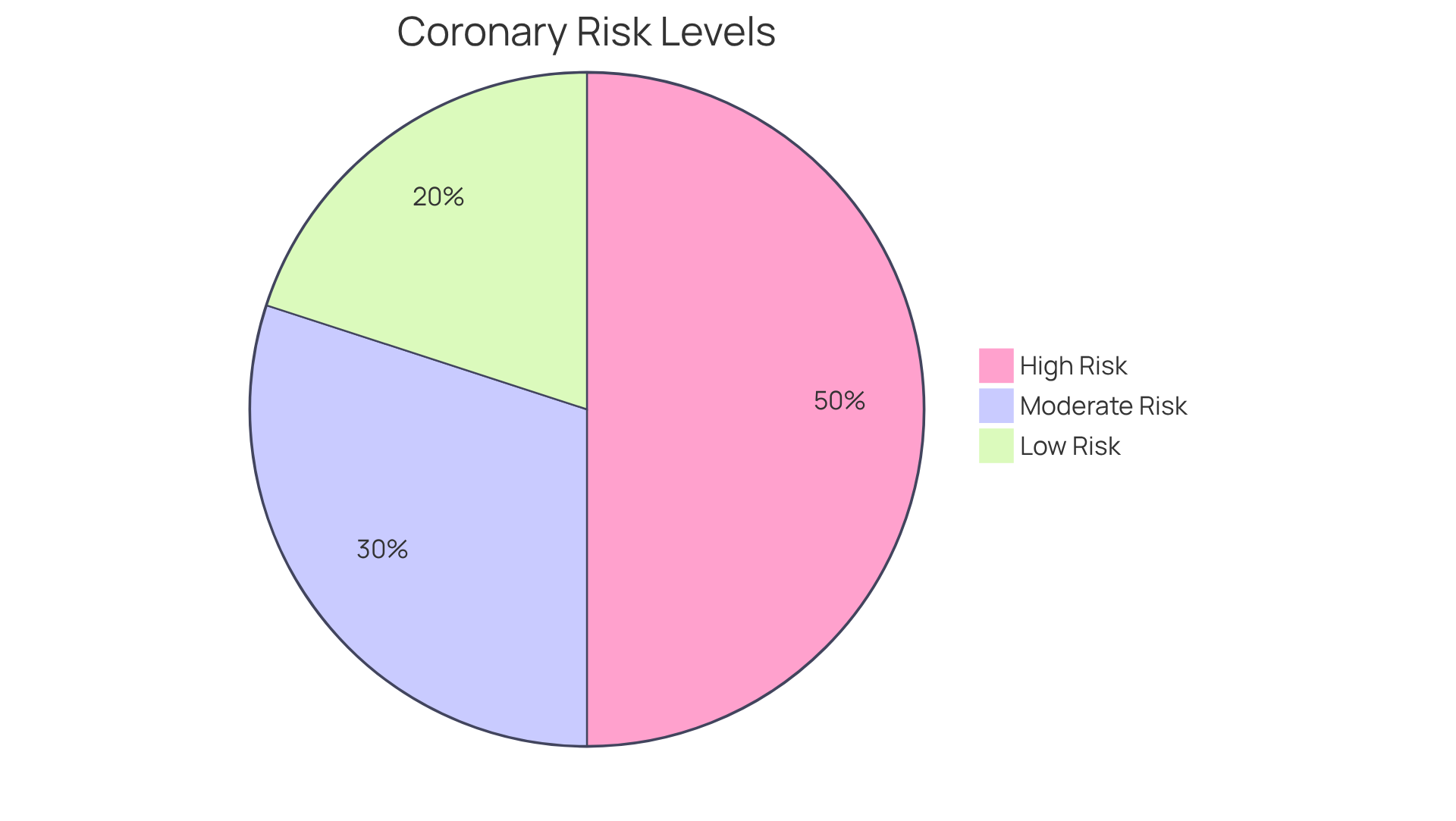
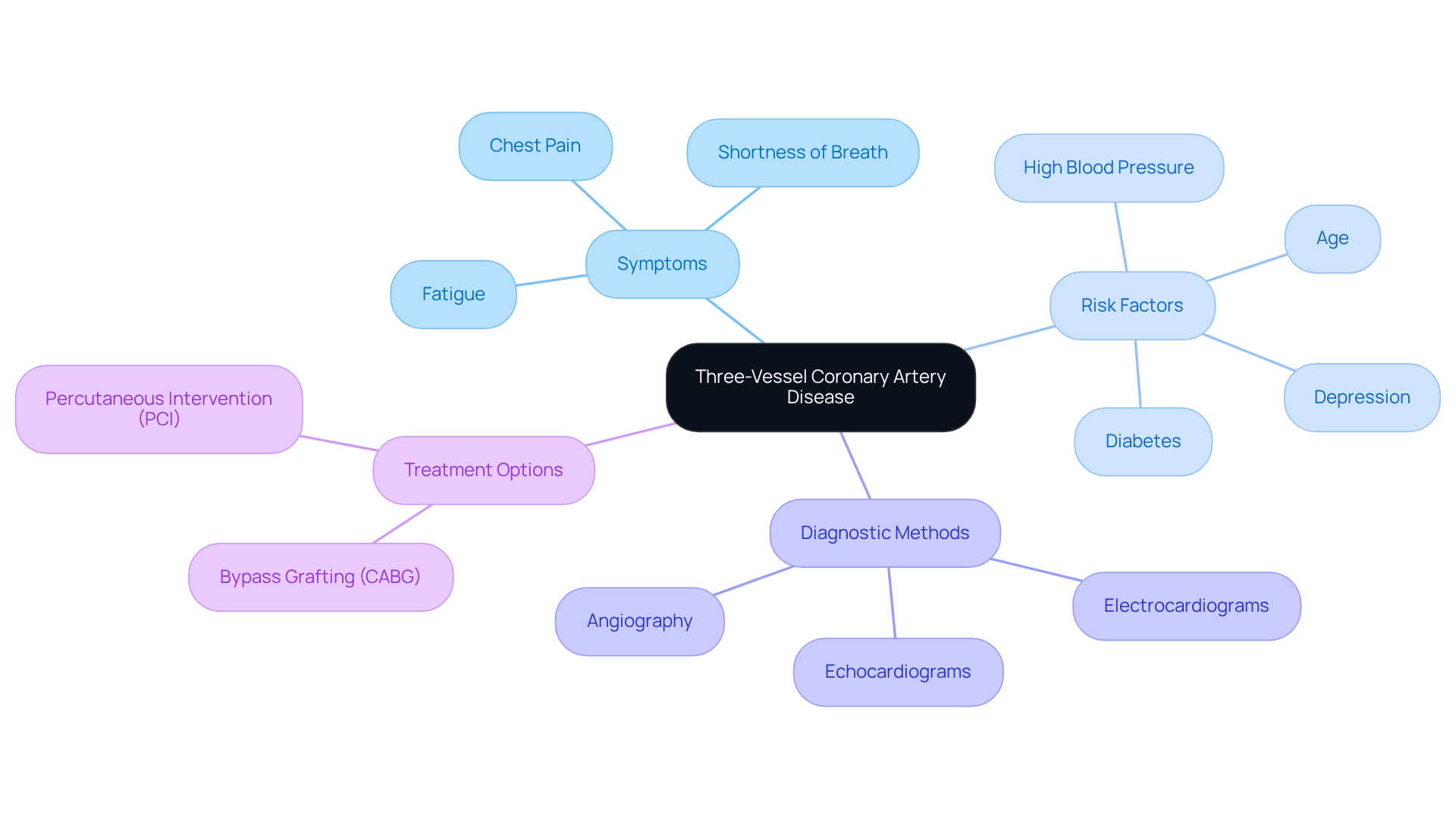
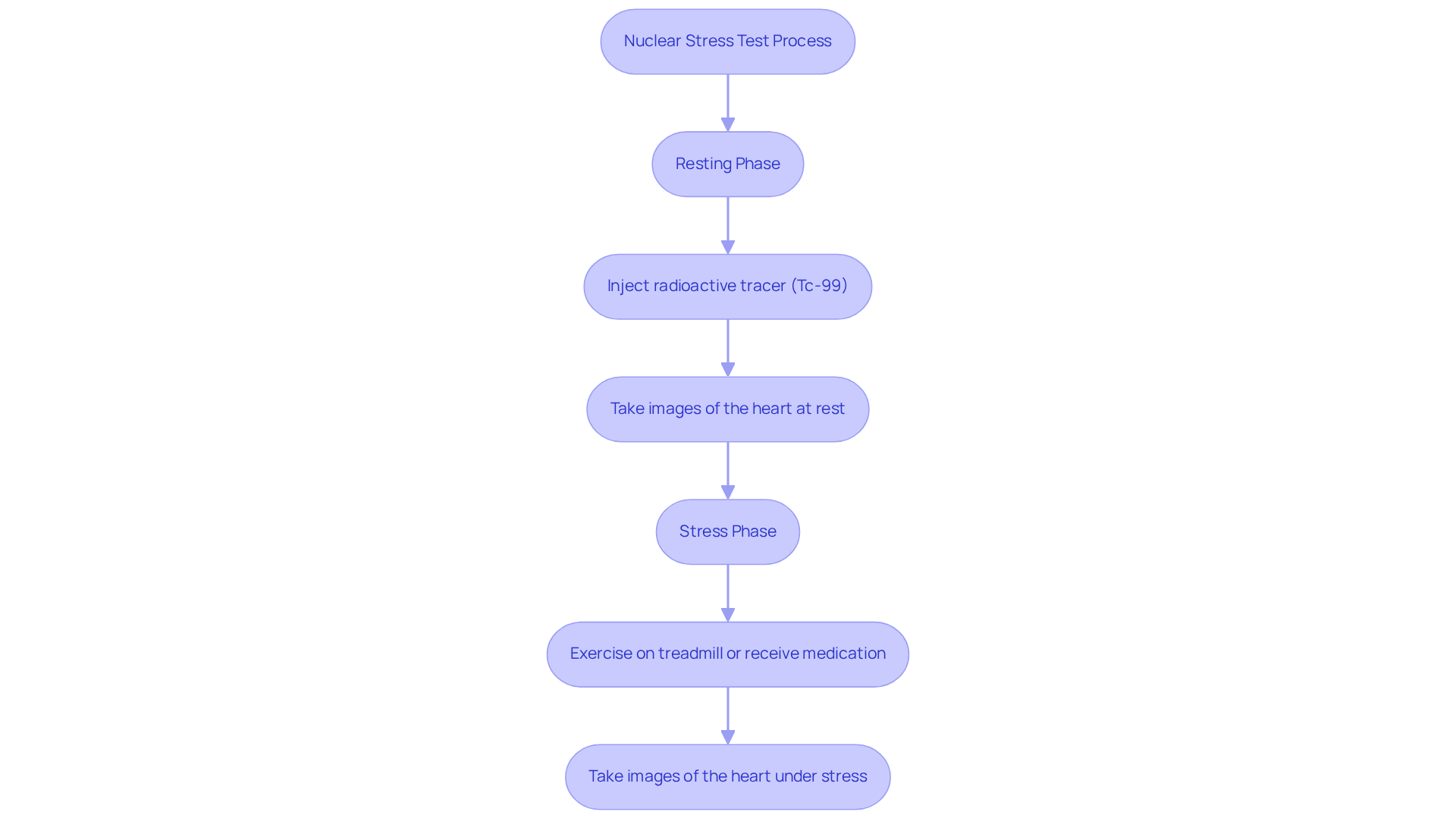
can indicate unusual outcomes from a nuclear stress evaluation, raising concerns about blood circulation to the heart muscle and often pointing to coronary artery disease. Understanding these implications is crucial for your heart health. Here are some common outcomes:
- Coronary artery disease: This condition is often the main reason for abnormal test results, indicating potential blockages in the coronary arteries. Research shows that about 37% of individuals tested may have results suggestive of CAD. This highlights the importance of vigilant monitoring and timely intervention when dealing with heart issues. Amavita’s technology provides advanced, real-time diagnostic data to help identify and manage CAD effectively, reducing the risk of readmissions. Heart failure may be indicated by abnormal results, suggesting that the heart isn’t pumping as it should, which can lead to serious complications. Unfortunately, individuals with heart failure often face a significantly reduced life expectancy, with only 50% living five years after diagnosis. At Amavita, we are dedicated to enhancing cardiac function through comprehensive cardiovascular management, aiming to improve your outcomes.
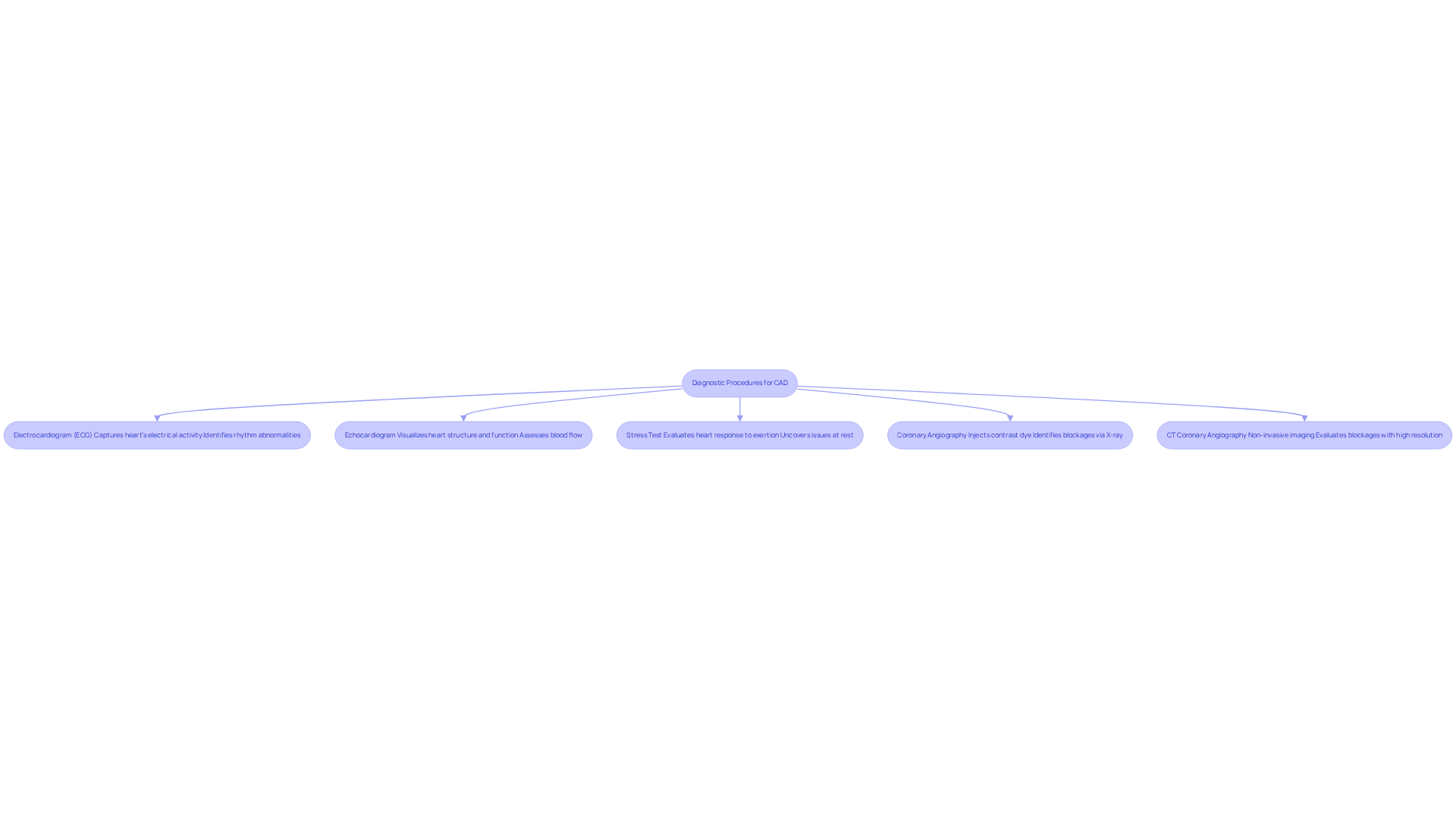
- Additional testing: Depending on the severity of the abnormalities, your doctor may recommend additional tests like angiograms or echocardiograms. It’s important to remember that abnormal results don’t rule out cardiovascular disease; they may simply indicate no significant blockage, necessitating further evaluation. Amavita’s platform integrates AI and AHA-certified staff training to ensure you receive thorough assessments and personalized care plans.
Recognizing these implications is vital, as it underscores the urgency of follow-up care and the importance of proactive heart health management. Experts agree that early intervention can greatly improve outcomes for those at risk of coronary artery disease. At Amavita, we are committed to providing the comprehensive care you need to navigate these challenges with confidence and support.
Take Action: Next Steps After Abnormal Results
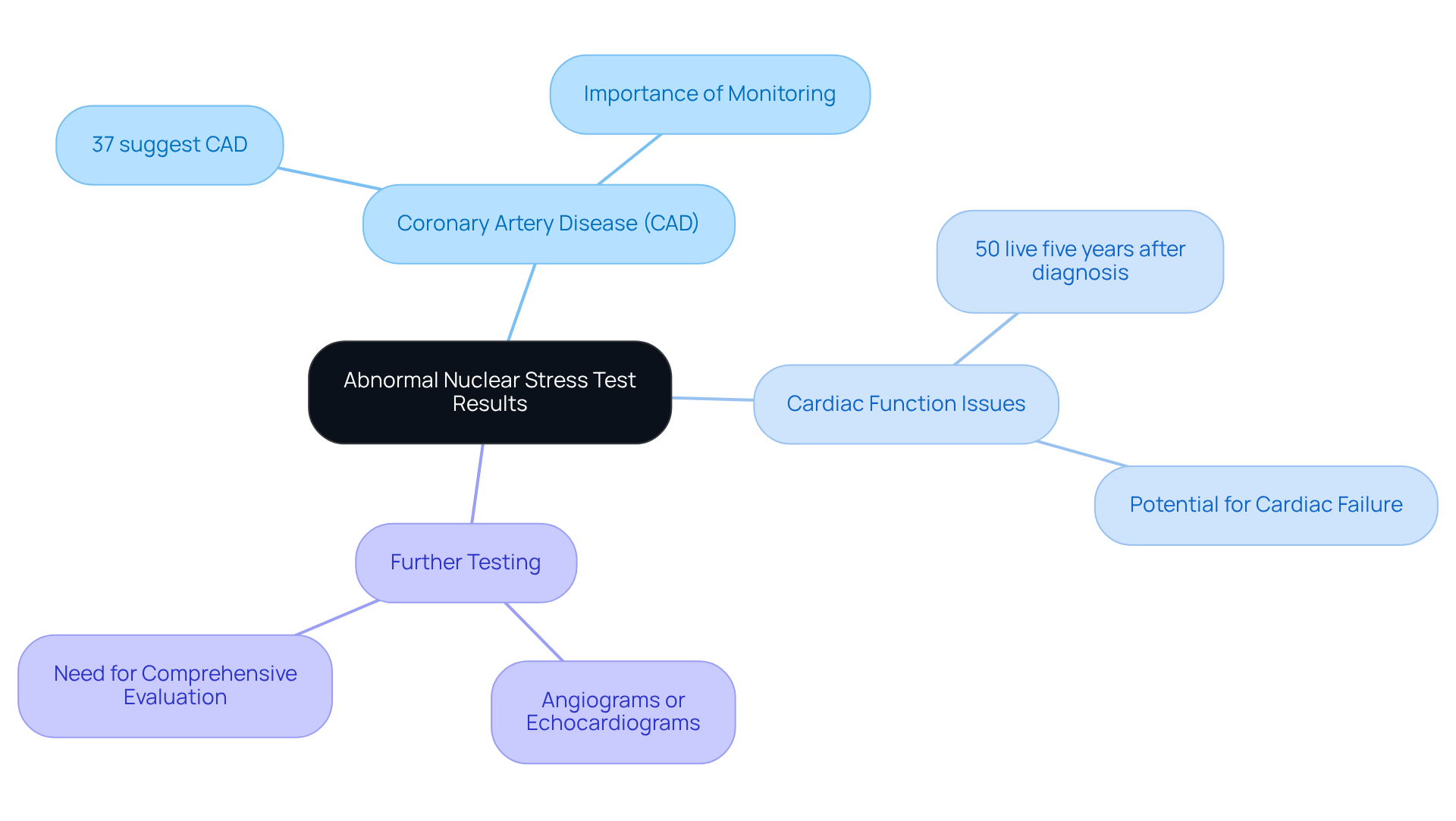
After receiving abnormal nuclear stress test results, it’s natural to feel concerned about your health. Here are some important steps you can take to ensure you’re managing your health effectively:
- Schedule an appointment: It’s crucial to schedule an appointment to discuss your results in detail. Your cardiologist will help clarify what the results indicate for you and outline potential next steps. Understanding the implications of your results is essential for making informed decisions about your care.
- Prepare for additional assessments: Be prepared for additional assessments that may be necessary to further evaluate your condition. Common follow-up procedures, like angiography, allow for direct visualization of the coronary arteries and help confirm any significant blockages. This step is vital, as it can guide your treatment options effectively.
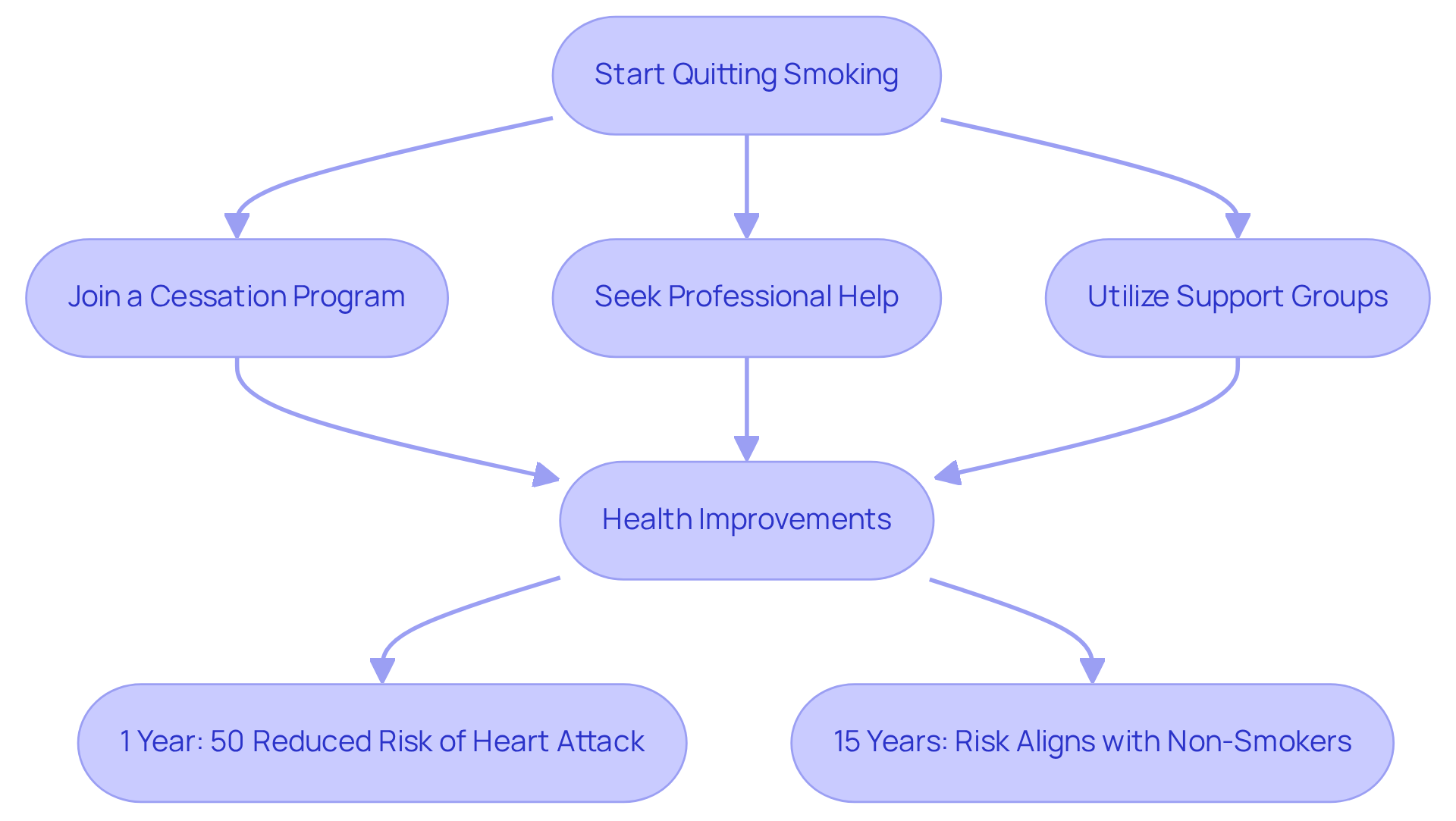
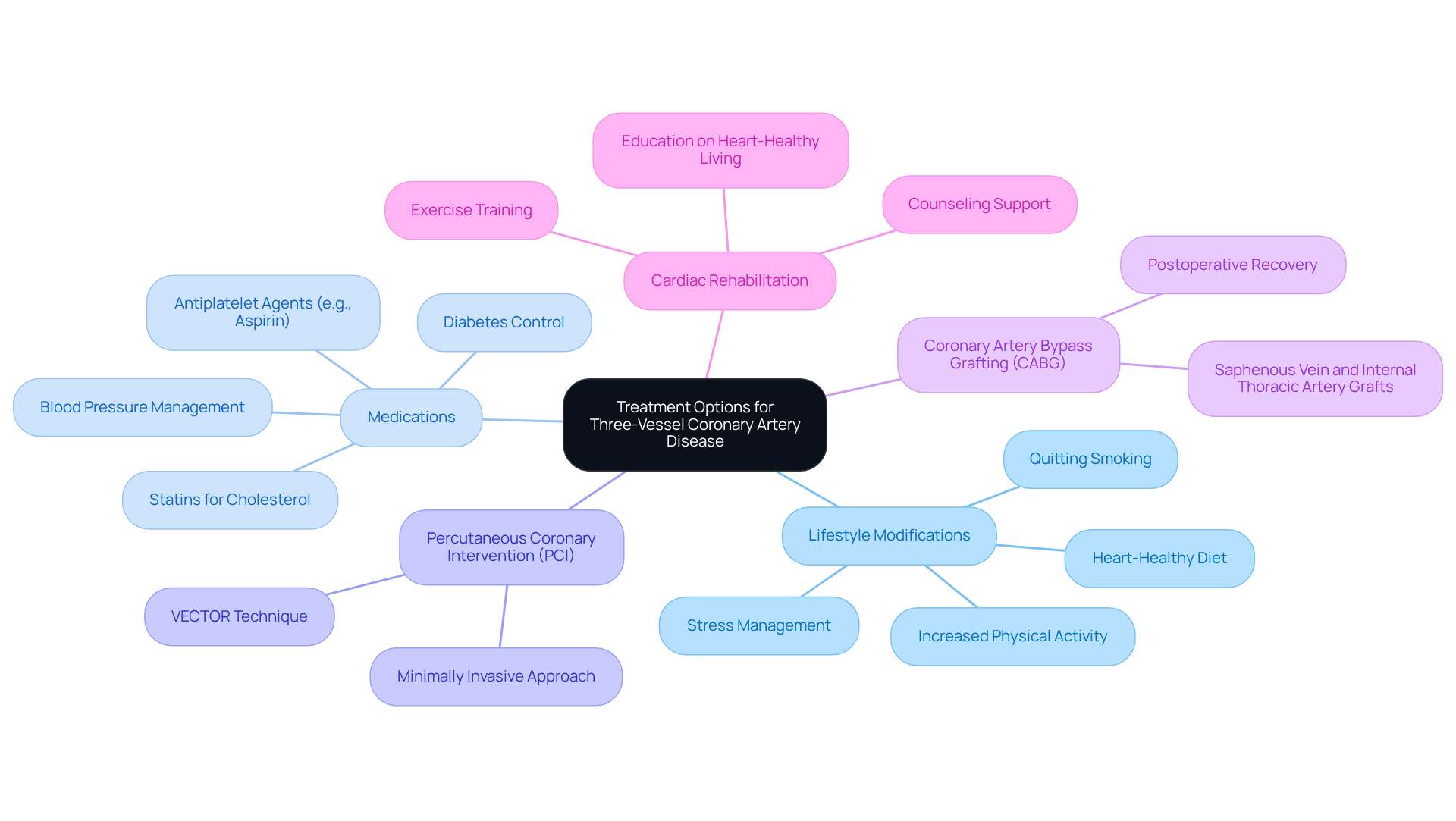
- Make lifestyle changes: Talk to your healthcare provider about making lifestyle changes that can positively impact your health. This might include adopting a heart-healthy diet, engaging in regular physical activity, quitting smoking, and managing stress. These changes can significantly lower your cardiovascular risk and improve your overall well-being.
- Consider rehabilitation: If recommended, participating in a cardiac rehabilitation program can greatly enhance your recovery. These programs offer supervised exercise and education, supporting your recovery while equipping you with the knowledge and skills to maintain a healthier lifestyle.
Support is essential for effectively managing your health. Remember, you’re not alone in this journey; reaching out for support is a sign of strength, and there are resources available to help you every step of the way.
Access Resources for Further Support and Information
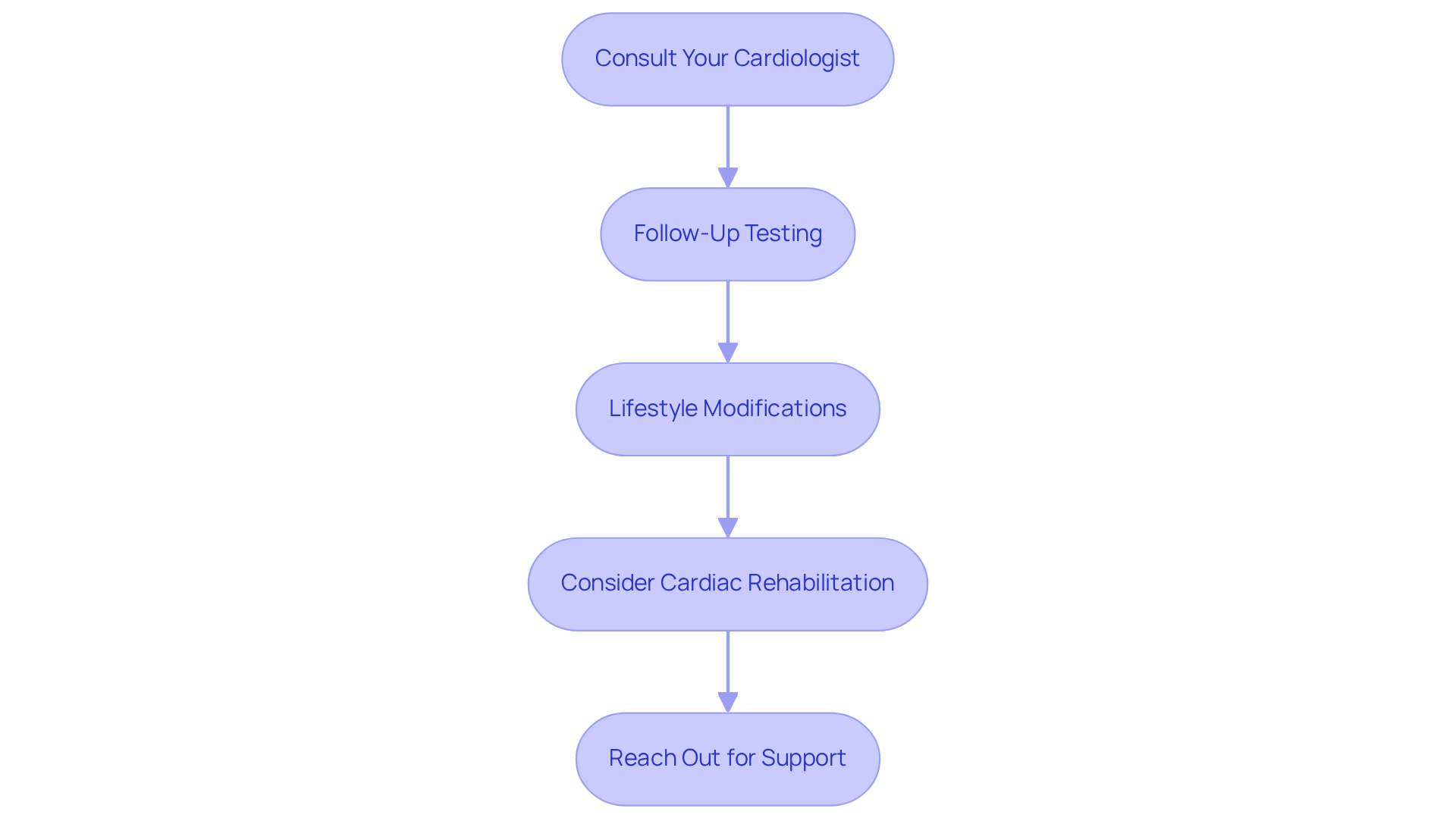
If you’re feeling uncertain about your health, remember that you’re not alone. There are various resources available to support you on your journey toward recovery:
- Local Support Groups: This organization provides a wealth of information on heart health, including support networks and resources that can help you feel more connected.
- Hospital Programs: Many hospitals and clinics offer specialized programs designed to assist individuals like you in managing stress and anxiety. These programs can be a vital part of your healing process.
- Online Forums and Communities: Websites such as HealthUnlocked or local community groups can offer support, allowing you to connect with others who understand what you’re going through.
- Educational Materials: Look for brochures or online articles from trusted medical organizations that explain treatment options. These resources can empower you with knowledge.
Utilizing these resources can help you feel more informed and supported. Remember, reaching out for help is a strong step toward taking charge of your health.
Conclusion
Understanding how to respond to abnormal nuclear stress test results is crucial for anyone concerned about their heart health. It’s natural to feel anxious when faced with such findings, but being proactive and informed can make a significant difference. By recognizing what these results mean and taking the right steps, you can enhance your cardiovascular care and overall well-being.
Let’s explore some key points together. The nuclear stress test process is designed to assess how well your heart functions under stress. If results come back abnormal, it may indicate conditions like coronary artery disease. This is why follow-up testing and lifestyle modifications are so important. Consulting with healthcare professionals can provide clarity and guidance, ensuring you receive comprehensive care tailored to your needs.
Engaging in cardiac rehabilitation and making informed lifestyle changes can lead to improved heart health outcomes. Have you considered how small adjustments in your daily routine could positively impact your heart? Every step you take towards better health is a step worth celebrating.
Ultimately, taking charge of your cardiovascular health is a shared journey. By understanding the significance of abnormal nuclear stress test results and seeking the right support, you empower yourself to make informed decisions about your health. Whether it’s reaching out to a cardiologist or tapping into community resources, remember that you’re not alone. Each action you take is a step toward a healthier heart and a brighter, more informed future.
Frequently Asked Questions
What is a nuclear stress test?
A nuclear stress test is a diagnostic procedure that evaluates blood circulation to the heart muscle during both rest and stress, helping identify potential heart issues like coronary artery disease.
Who should consider undergoing a nuclear stress test?
Individuals at higher risk, such as those with diabetes, hypertension, or a family history of heart disease, should consider undergoing a nuclear stress test.
What are the two main phases of a nuclear stress test?
The two main phases are the Resting Phase, where a radioactive tracer is injected to take images of the heart at rest, and the Stress Phase, where the patient either exercises or receives medication to mimic exercise effects, followed by additional imaging.
What is the purpose of comparing blood flow during rest and stress?
Comparing blood flow during rest and stress is crucial for identifying potential heart issues, as it helps determine how well blood flows to the heart under different conditions.
How many nuclear stress evaluations are performed each year in the U.S.?
Approximately 10 million nuclear stress evaluations are performed each year in the U.S.
What is the radiation exposure from a nuclear stress evaluation?
The radiation exposure from a nuclear stress evaluation is about 11 millisieverts, which is roughly three times the yearly dose from everyday life.
Are there any preparation guidelines for a nuclear stress test?
Yes, there are preparation guidelines that include dietary restrictions and medication management to ensure the most accurate results.
What do abnormal nuclear stress test results indicate?
Abnormal nuclear stress test results may indicate previous heart damage, while normal images suggest a low likelihood of coronary artery disease.
What are some potential risks associated with a nuclear stress test?
Potential risks include cardiac arrhythmias and allergic reactions.
How can understanding the nuclear stress test process help patients?
Understanding the nuclear stress test process empowers patients to take an active role in their healthcare journey and navigate their cardiac care more effectively, especially when considering personalized treatment plans.
List of Sources
- Understand the Nuclear Stress Test Process
- mayoclinic.org (https://mayoclinic.org/tests-procedures/nuclear-stress-test/about/pac-20385231)
- What You Should Know About the Nuclear Stress Test (https://verywellhealth.com/nuclear-stress-test-overview-4172096)
- Nuclear Stress Tests: What You Need to Know – ASNC (https://asnc.org/resource/nuclear-stress-tests-what-you-need-to-know)
- Survey Shows Suboptimal Practice of Nuclear Stress Testing – American College of Cardiology (https://acc.org/latest-in-cardiology/articles/2013/05/08/10/18/survey-shows-suboptimal-practice-of-nuclear-stress-testing)
- Identify Abnormal Results and Their Implications
- Memorable Cardiology Quotes – TheKnowHow.Æ (https://theknowhow.ae/memorable-cardiology-quotes-heart)
- Taylor Swift Raising Awareness of Heart Disease and Nuclear Stress Testing – ASNC (https://asnc.org/news/taylor-swift-raising-awareness-of-heart-disease-and-nuclear-stress-testing)
- parade.com (https://parade.com/1187612/michelle-parkerton/quotes-about-heart-disease)
- atlantichealth.org (https://atlantichealth.org/health-articles/heart-health/stress-tests-don-t-have-to-be-stressful)
- Columbia University Medical Center Study Shows Stress Test Saves Lives of Patients With Chest Pain | NYP (https://nyp.org/news/cumc-study-shows-stress-test-saves-lives-of-patients-with-chest)
- Take Action: Next Steps After Abnormal Results
- chinatowncardiology.com (https://chinatowncardiology.com/blog/what-happens-after-a-cardiac-stress-test)
- 6+ After Abnormal Stress Test: The Next Step (https://jitsi.cmu.edu.jm/what-is-the-next-step-after-an-abnormal-stress-test)
- What to Expect from a Nuclear Stress Test | UNC Health Talk (https://healthtalk.unchealthcare.org/what-to-expect-from-a-nuclear-stress-test)
- Your doctor has ordered a stress test: 9 common questions answered (https://novanthealth.org/healthy-headlines/your-doctor-has-ordered-a-stress-test-9-common-questions-answered)
- healthline.com (https://healthline.com/health/heart-health/what-happens-if-you-fail-a-stress-test)
- Access Resources for Further Support and Information
- crestline.com (https://crestline.com/c/slogans-for-american-heart-month)
- heart.org (https://heart.org/en/news)
- ahajournals.org (https://ahajournals.org/doi/10.1161/circoutcomes.119.005902)
- millionhearts.hhs.gov (https://millionhearts.hhs.gov/data-reports/factsheets/cardiac.html)
- Novel virtual care program enhances at-home support for people with heart failure (https://newsroom.heart.org/news/novel-virtual-care-program-enhances-at-home-support-for-people-with-heart-failure)
- Nearly 5,000 organizations nationwide recognized for high-quality cardiovascular care (https://newsroom.heart.org/news/nearly-5-000-organizations-nationwide-recognized-for-high-quality-cardiovascular-care)