Introduction
Have you ever felt your heart racing unexpectedly, leaving you anxious and unsure? Understanding the distinction between tachycardia and atrial fibrillation is important for anyone who has experienced this unsettling sensation. While both conditions involve an abnormal heart rate, they come with unique symptoms and health implications that can significantly affect your well-being. Millions of people are affected by these heart rhythm disorders, and recognizing the symptoms is vital.
What happens when the signs of these two conditions blur together? It can be confusing, but knowing how to navigate your health journey is essential for your peace of mind. Seeking appropriate care is crucial, and understanding these differences can empower you to take charge of your heart health and seek the care you deserve.
Define Tachycardia and Atrial Fibrillation
Have you ever felt your heart racing unexpectedly? It can be a frightening experience, especially when you don’t know what it means. Tachycardia, or a racing heart, occurs when your pulse exceeds 100 beats per minute while you’re at rest, and it can be concerning to experience. While it might be a normal response to stress or physical activity, it can also indicate underlying health issues that deserve attention.
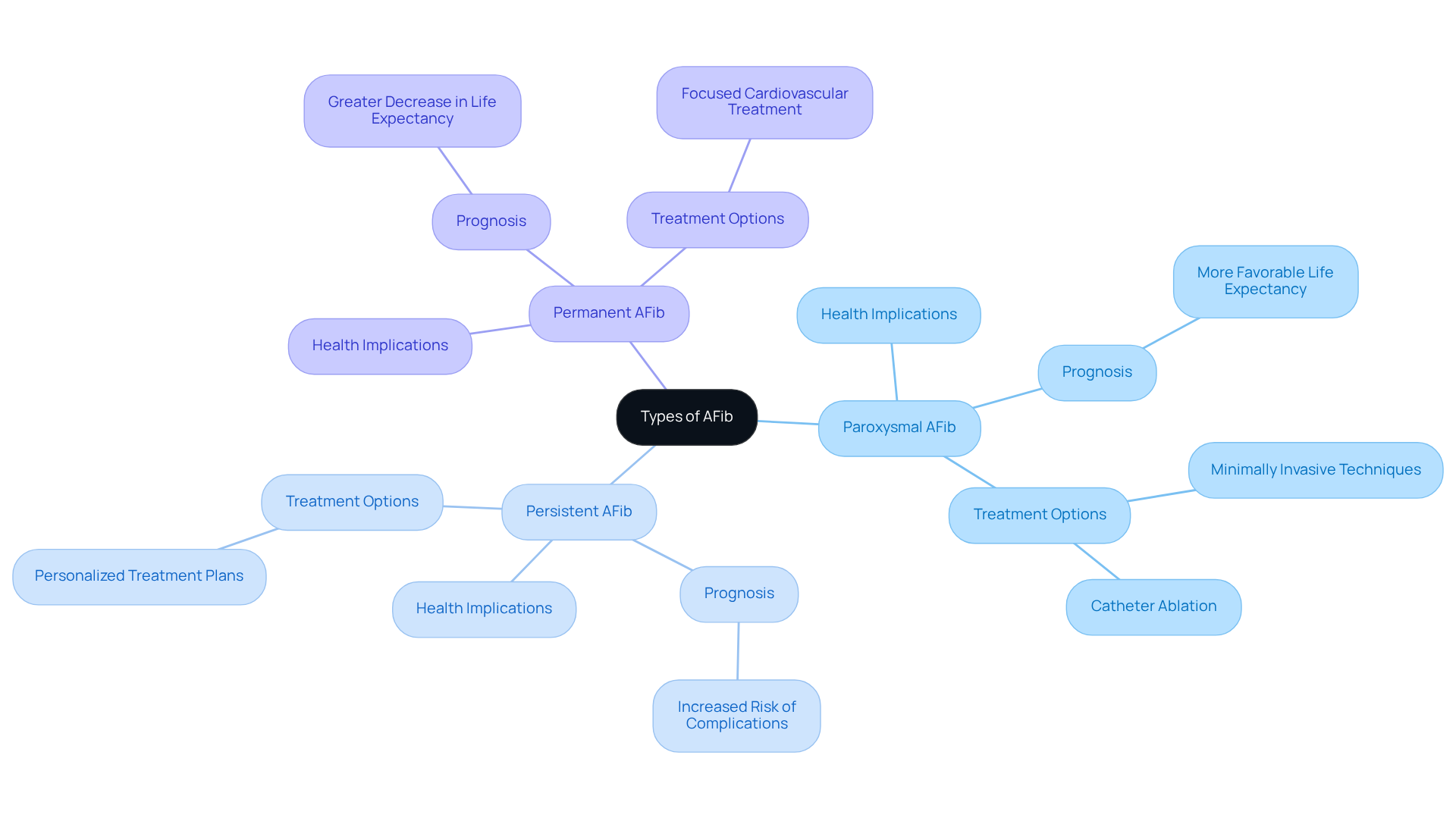
One specific type of tachycardia is atrial fibrillation, raising the question of is tachycardia the same as afib, which many people experience. This condition is marked by an irregular and often rapid heartbeat that can feel unsettling. A common question is whether is tachycardia the same as afib, as atrial fibrillation is the most common sustained arrhythmia, affecting millions and significantly increasing the risk of stroke. In fact, research suggests that the risk of stroke can rise fivefold when standard factors are considered.
Understanding these terms can help you recognize symptoms and know when to seek help, which is so important for your health. Many individuals with atrial fibrillation may have episodes that go unnoticed, both symptomatic and asymptomatic. This knowledge is vital for ensuring you receive timely and appropriate medical care. Remember, you’re not alone in this, and there are resources available to support you.
Identify Symptoms of Tachycardia and Afib
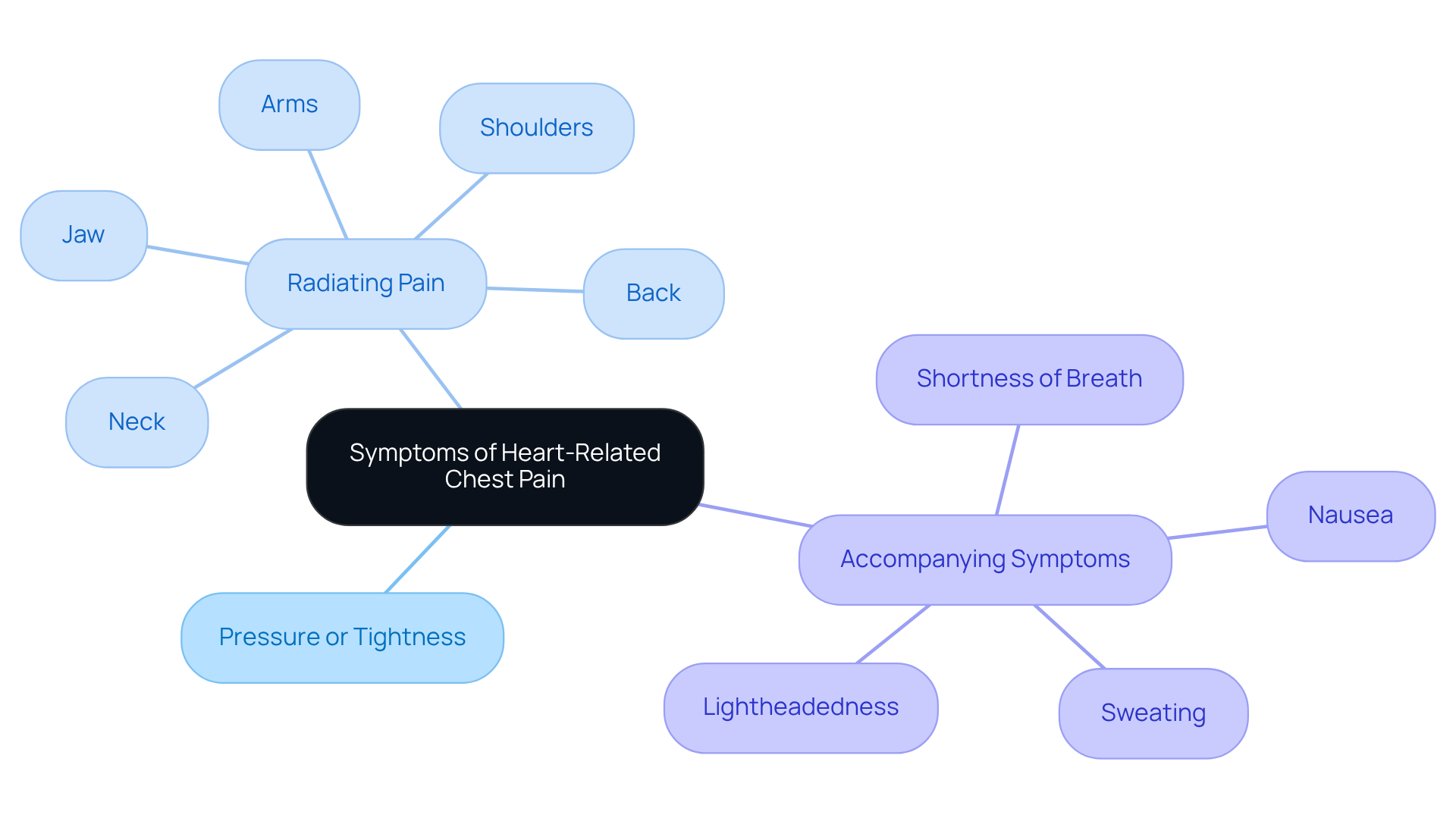
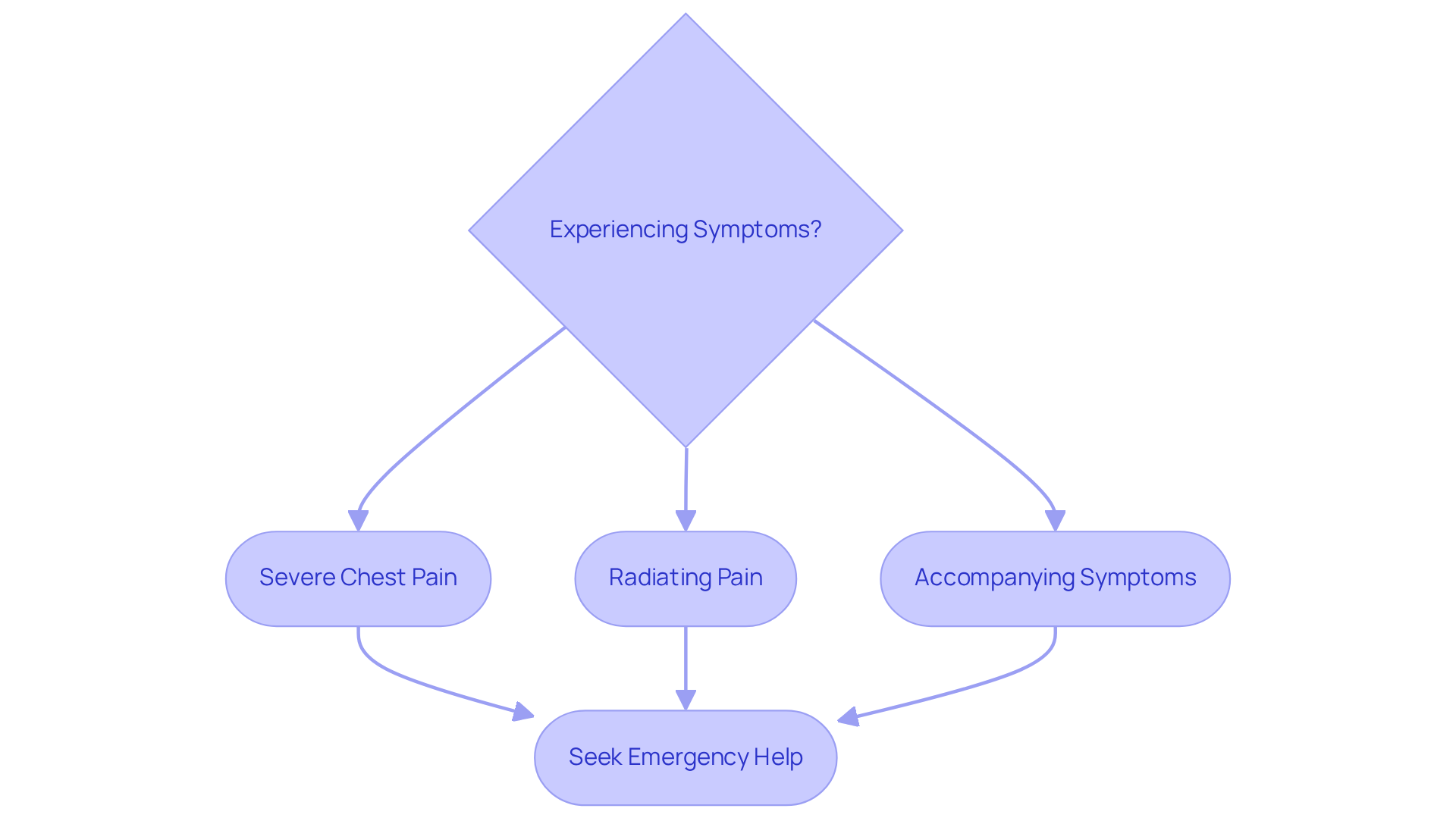
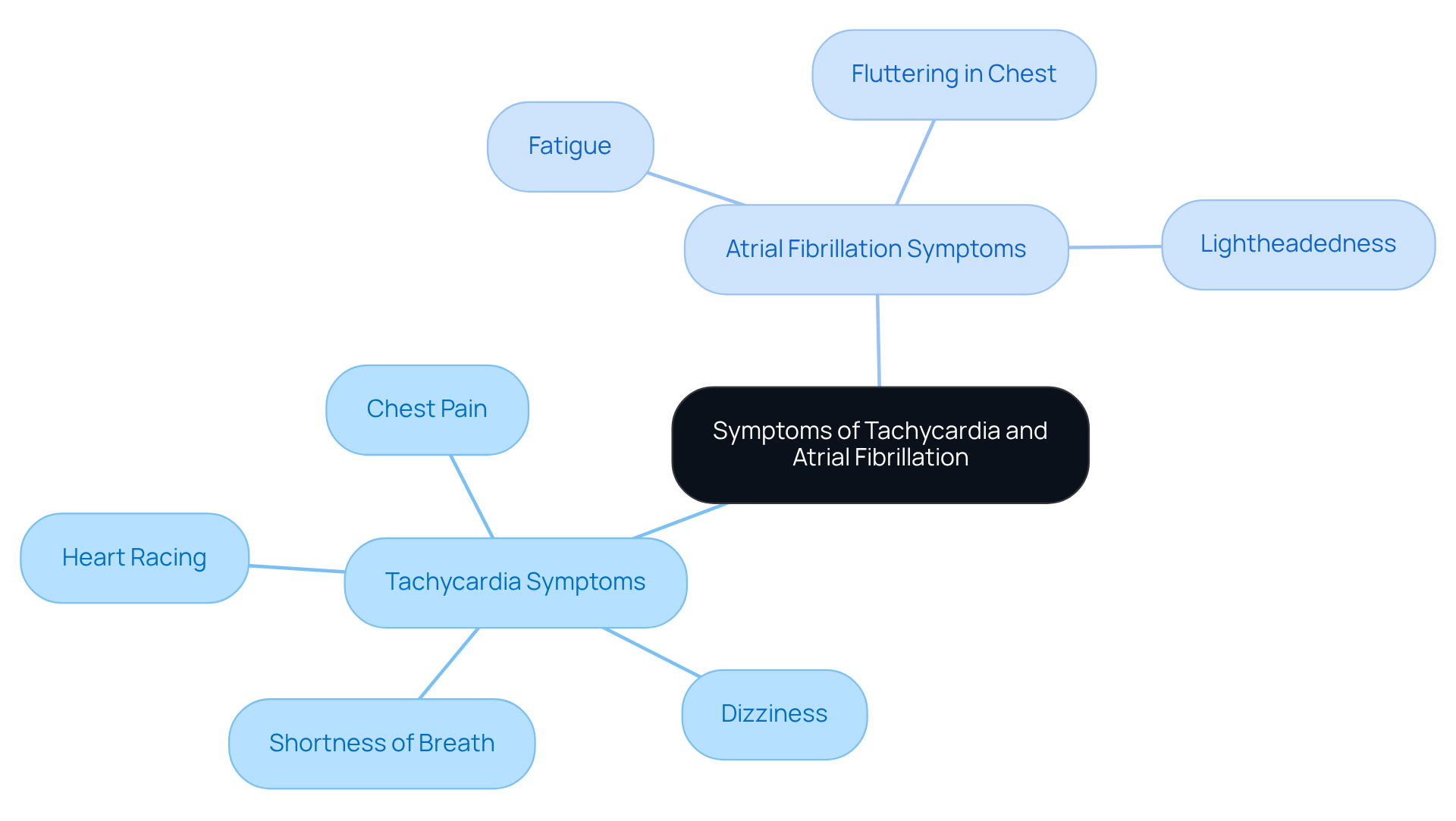
Have you ever felt your heart racing unexpectedly, leaving you worried about what it might mean for your health? Tachycardia can show up in various ways, like when you notice your heart racing, accompanied by feelings of dizziness, shortness of breath, or even chest pain. On the other hand, atrial fibrillation might bring additional sensations, such as fatigue, a fluttering feeling in your chest, or lightheadedness. It’s important to remember that some people may not experience any symptoms at all, which can make it harder to catch these issues early.
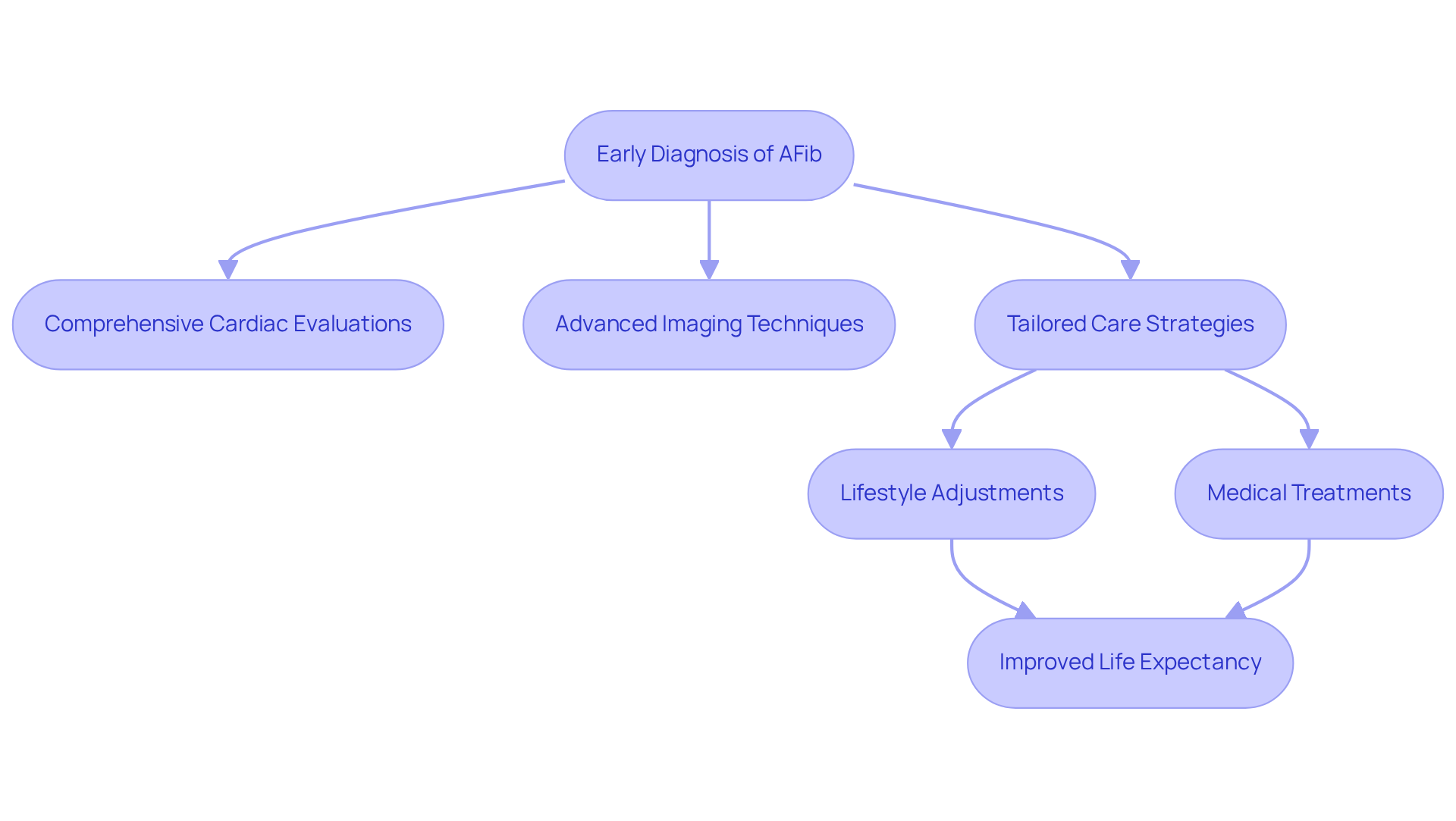
Recognizing these symptoms is crucial because it allows you to seek help sooner, which can greatly enhance your health outcomes. Early detection can lead to prompt medical evaluation and intervention, making a significant difference in your health journey. Recent studies show that if silent atrial fibrillation is found during health screenings, it can put you at a higher risk for heart failure, which is why being aware of your heart health is so important.
By staying informed and proactive, you can take important steps towards safeguarding your heart health and overall well-being.
Consult a Healthcare Professional for Diagnosis
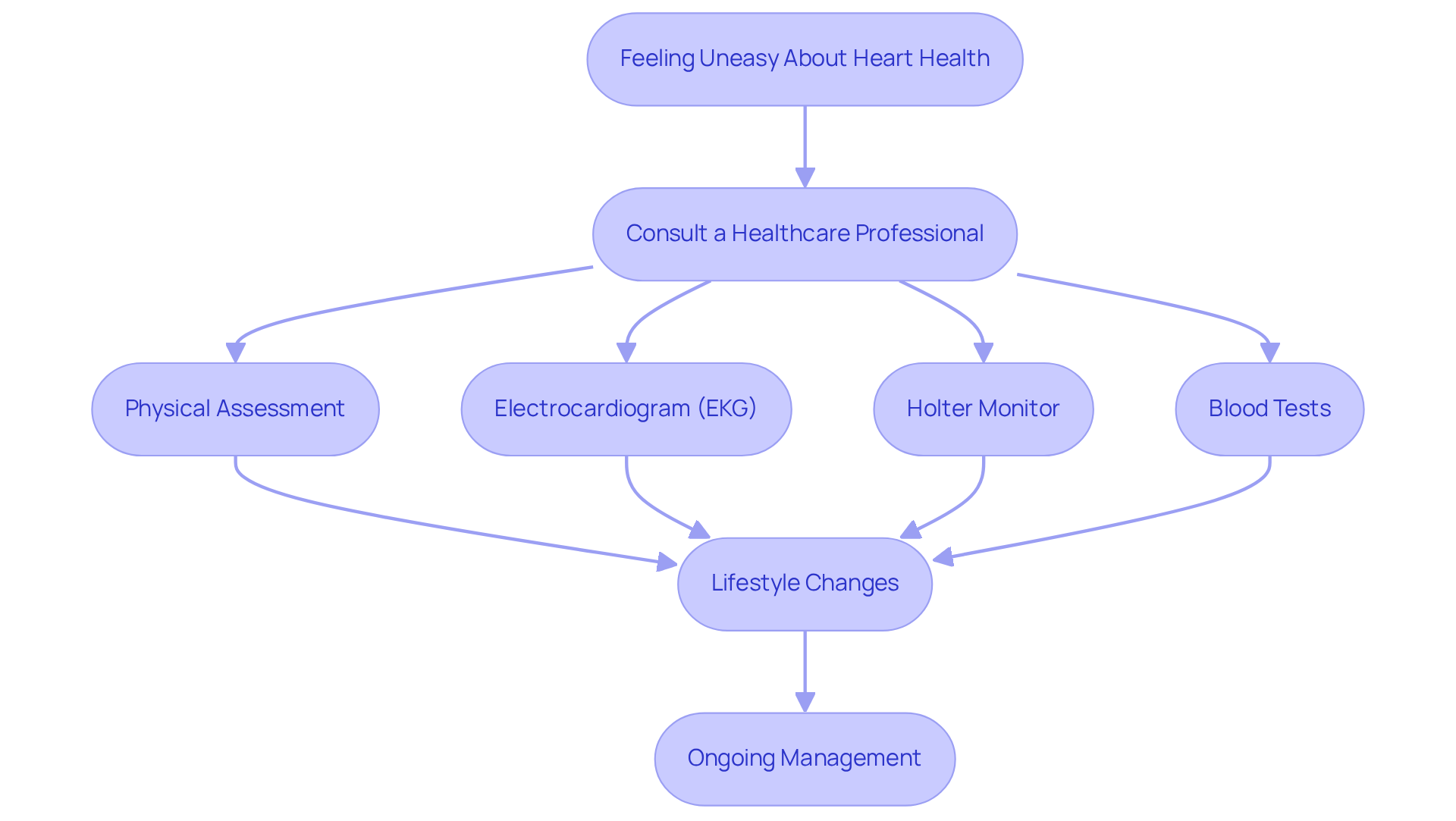
If you’re feeling uneasy about your heart health, you’re not alone. If you suspect you have tachycardia or are questioning if tachycardia is the same as afib, reaching out to a healthcare professional is a vital step. At Amavita Heart & Vascular Health, we perform a thorough physical assessment followed by advanced diagnostic tests, like an electrocardiogram (EKG), to check your heart’s rhythm. We use innovative AI-powered diagnostic technology, like a portable, FDA-cleared ultrasound, to provide accurate imaging and real-time guidance during your bedside cardiac assessments. This technology produces reports on cardiac structure and function within minutes, allowing for early detection and informed decisions.
It’s natural to feel worried when faced with heart health issues. Additional assessments may include:
- A Holter monitor, which records heart activity continuously over 24 hours
- Blood tests to identify any underlying health issues
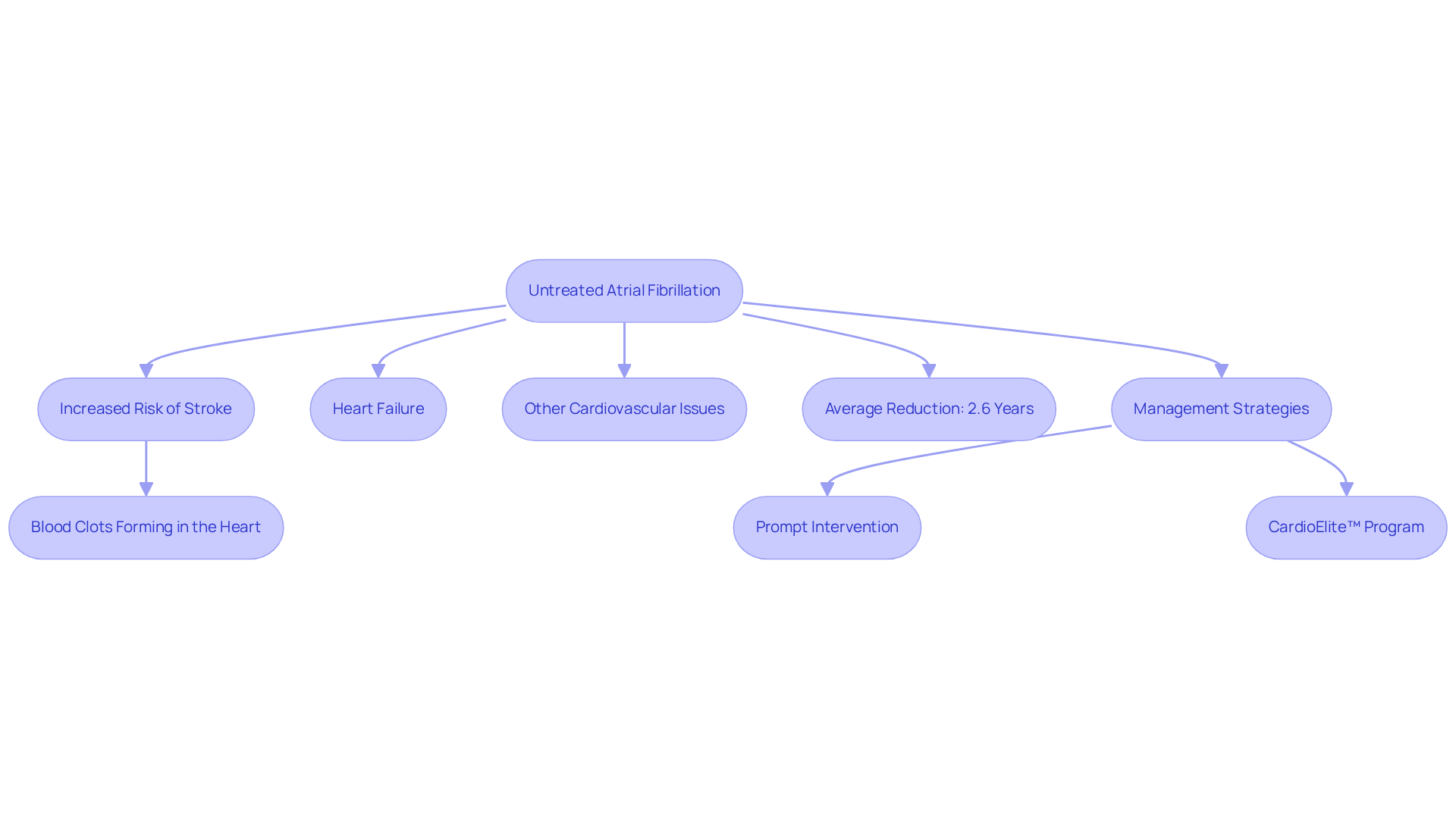
It’s important to know that getting diagnosed early can make a big difference in how we manage these conditions together. Cardiologists emphasize that prompt intervention can greatly enhance results, as untreated atrial fibrillation is linked to a fivefold heightened risk for stroke. Furthermore, atrial fibrillation is a chronic condition that requires ongoing management.
Incorporating lifestyle changes, such as limiting alcohol consumption and maintaining a healthy lifestyle, is essential for managing atrial fibrillation effectively. The Optimal Program at Amavita includes comprehensive biomarker panels, cardiac screenings, and quarterly consultations, ensuring tailored care. Employing advanced diagnostic techniques, such as echocardiograms and event recorders, can further improve the precision of atrial fibrillation and tachycardia diagnoses, which raises the question: is tachycardia the same as afib, ensuring you receive suitable care customized to your individual requirements. Additionally, our AHA certification underscores our commitment to high evidence-based care standards. By seeking help now, you can avoid serious complications down the road.
Explore Treatment Options and Lifestyle Changes
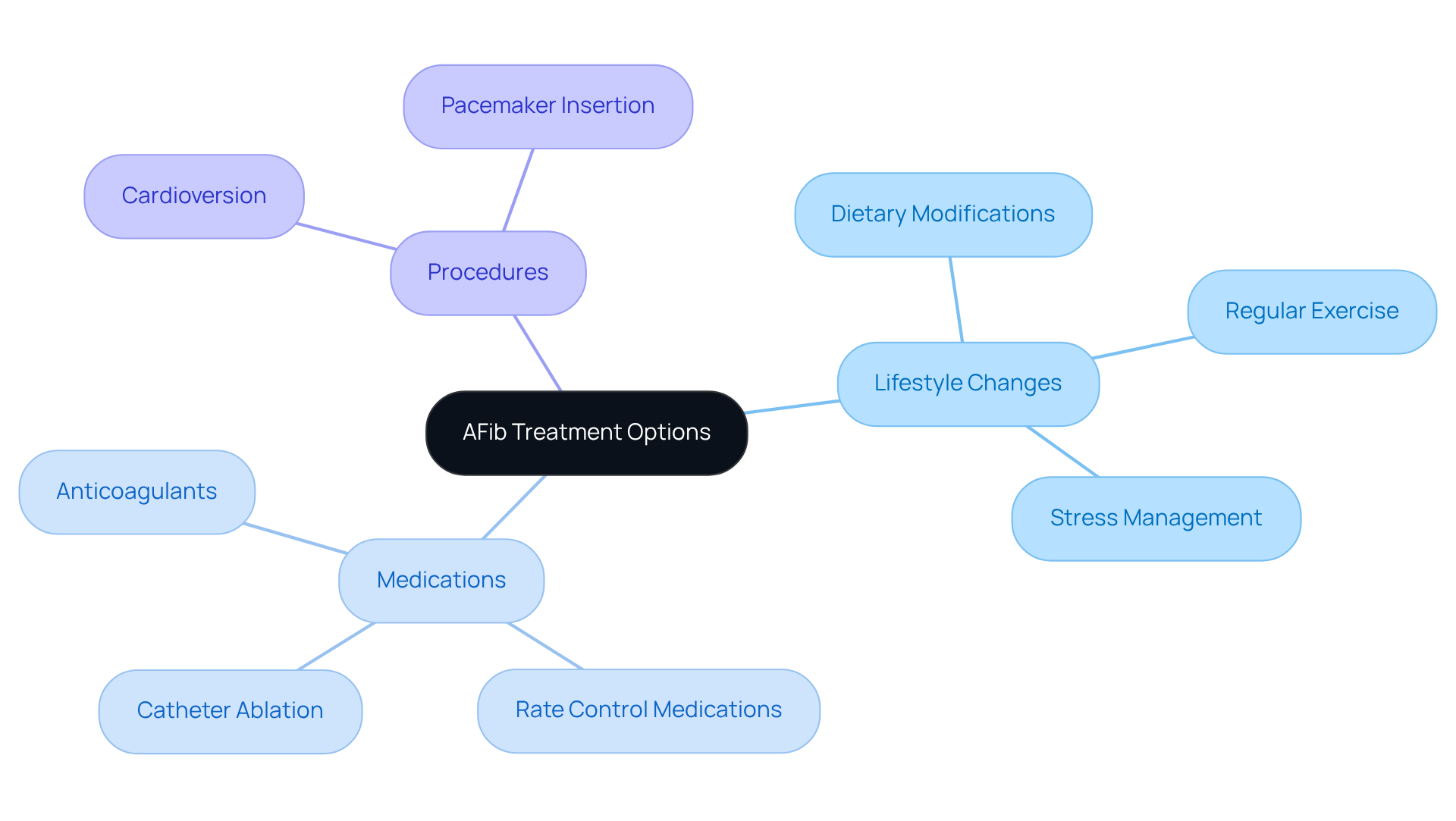
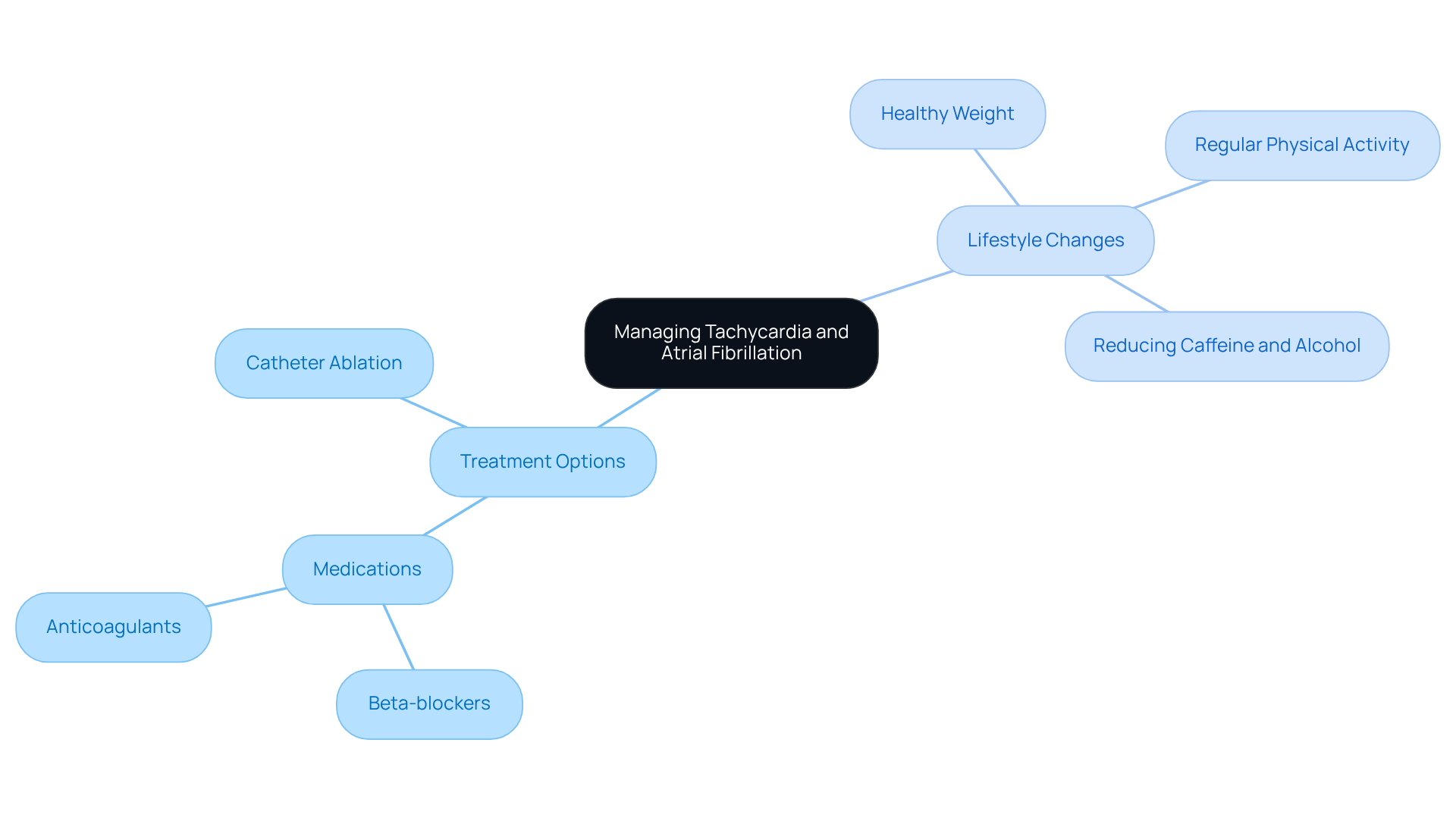
Managing tachycardia and atrial fibrillation can feel overwhelming, leading many to wonder, is tachycardia the same as afib, but you’re not alone in this journey. Effective management often means combining medications with lifestyle changes, and programs like Amavita’s CardioElite™ can help you every step of the way. Commonly recommended medications include:
- Beta-blockers, which help regulate your pulse rate
- Anticoagulants, which reduce the risk of blood clots
In some cases, catheter ablation may be suggested as a more definitive treatment option. This minimally invasive procedure has shown promising success rates, allowing many patients to experience relief from AFib symptoms and lessen their dependence on anti-arrhythmic medications.
With Amavita’s CardioElite™, you’ll have access to real-time diagnostic information and support from cardiology experts whenever you need it. This is especially important for high-risk patients, including those with diabetes, hypertension, or a family history of heart disease. It’s important to work with your healthcare provider to create a management plan that fits your unique needs and lifestyle.
Lifestyle changes are crucial in improving outcomes for those with tachycardia and atrial fibrillation, especially for those wondering if ‘is tachycardia the same as afib’. Maintaining a healthy weight is vital, as obesity is a recognized risk factor for AFib. Regular physical activity not only enhances cardiovascular health but also helps manage stress, which can trigger episodes. Additionally, cutting back on caffeine and alcohol can help ease symptoms.
Real-world examples show how these lifestyle changes can make a difference. Patients who engage in regular physical activity and follow a heart-friendly diet often report fewer AFib episodes and feel better overall. Collaborating closely with healthcare providers, especially through programs like CardioElite™, is essential for developing a comprehensive management strategy. With the right support, you can take charge of your heart health and live a fulfilling life.
Conclusion
Navigating heart health can feel daunting, especially when faced with conditions like tachycardia and atrial fibrillation. While both involve an abnormal heartbeat, they come with different symptoms and require tailored management strategies. It’s crucial to recognize symptoms like dizziness and irregular heartbeats, as they can guide you to seek the help you need. By understanding these signs and reaching out for timely medical advice, you can significantly impact your health outcomes.
Throughout this guide, we’ve explored key insights into the definitions, symptoms, and diagnostic processes for both tachycardia and atrial fibrillation. Remember, symptoms such as dizziness, chest pain, and irregular heartbeats are critical indicators that warrant professional evaluation. However, by understanding these conditions and seeking help, you can take control of your heart health and feel empowered.
Taking proactive steps to understand your heart health can truly empower you to make informed choices. Engaging with healthcare professionals, adopting lifestyle changes, and utilizing available treatment options can lead to improved management of these conditions. By taking these steps, you not only protect your heart but also embrace a healthier, more vibrant life.
Frequently Asked Questions
What is tachycardia?
Tachycardia is a condition characterized by a racing heart, occurring when your pulse exceeds 100 beats per minute while at rest. It can be a normal response to stress or physical activity but may also indicate underlying health issues.
What is atrial fibrillation?
Atrial fibrillation (afib) is a specific type of tachycardia marked by an irregular and often rapid heartbeat. It is the most common sustained arrhythmia and can feel unsettling to those who experience it.
Is tachycardia the same as atrial fibrillation?
While tachycardia refers to an elevated heart rate, atrial fibrillation is a specific type of tachycardia that involves an irregular heartbeat. Therefore, they are related but not the same.
What are the risks associated with atrial fibrillation?
Atrial fibrillation significantly increases the risk of stroke, with research suggesting that the risk can rise fivefold when standard factors are considered.
Can atrial fibrillation go unnoticed?
Yes, many individuals with atrial fibrillation may experience episodes that go unnoticed, which can be either symptomatic or asymptomatic.
Why is it important to understand tachycardia and atrial fibrillation?
Understanding these conditions helps individuals recognize symptoms and know when to seek help, which is crucial for receiving timely and appropriate medical care.
List of Sources
- Define Tachycardia and Atrial Fibrillation
- heart.org (https://heart.org/en/news/2025/09/23/new-afib-diagnosis-heres-some-help-to-clear-any-confusion)
- About Atrial Fibrillation (https://cdc.gov/heart-disease/about/atrial-fibrillation.html)
- New Developments in Atrial Fibrillation (https://uscjournal.com/articles/new-developments-atrial-fibrillation?language_content_entity=en)
- Tachycardia (https://yalemedicine.org/conditions/tachycardia)
- Identify Symptoms of Tachycardia and Afib
- About Atrial Fibrillation (https://cdc.gov/heart-disease/about/atrial-fibrillation.html)
- Tachycardia (https://yalemedicine.org/conditions/tachycardia)
- Silent Heart Rhythm Problem Might Triple Risk Of Heart Failure In Seniors (https://usnews.com/news/health-news/articles/2026-04-15/silent-heart-rhythm-problem-might-triple-risk-of-heart-failure-in-seniors)
- New research finds 62% of AFib patients were unaware of the condition before diagnosis (https://newsroom.heart.org/news/new-research-finds-62-of-afib-patients-were-unaware-of-the-condition-before-diagnosis)
- Consult a Healthcare Professional for Diagnosis
- heart.org (https://heart.org/en/news/2025/09/23/new-afib-diagnosis-heres-some-help-to-clear-any-confusion)
- Atrial fibrillation: First of its kind therapy for ‘debilitating’ heart condition (https://bbc.com/news/articles/c9wnky140dko)
- Evidence Gaps and Lessons in the Early Detection of Atrial Fibrillation: A Prospective Study in a Primary Care Setting (PREFATE Study) (https://mdpi.com/2227-9059/13/1/119)
- New research finds 62% of AFib patients were unaware of the condition before diagnosis (https://newsroom.heart.org/news/new-research-finds-62-of-afib-patients-were-unaware-of-the-condition-before-diagnosis)
- Atrial fibrillation – Diagnosis and treatment – Mayo Clinic (https://mayoclinic.org/diseases-conditions/atrial-fibrillation/diagnosis-treatment/drc-20350630)
- Explore Treatment Options and Lifestyle Changes
- Atrial Fibrillation (AF) Catheter Ablation Success Rates (https://stopafib.org/procedures-for-afib/catheter-ablation/success-rates)
- 10 Lifestyle Modifications That Can Help Manage AFib — Capital Cardiology Associates (https://capitalcardiology.com/cca-news/10-lifestyle-modifications-that-can-help-manage-afib)
- Cleveland Clinic-led Trial Shows Pulsed Field Ablation Procedure More Effective Than Medications for Persistent Atrial Fibrillation – Florida Hospital News and Healthcare Report (https://southfloridahospitalnews.com/cleveland-clinic-led-trial-shows-pulsed-field-ablation-procedure-more-effective-than-medications-for-persistent-atrial-fibrillation)
- massdevice.com (https://massdevice.com/biggest-cardiac-news-2026-af-symposium)
- Current Treatment Options in Atrial Fibrillation – A Changing Paradigm (https://uscjournal.com/articles/current-treatment-options-atrial-fibrillation-changing-paradigm?language_content_entity=en)