Introduction
At the forefront of cardiovascular care, Amavita Heart and Vascular Health provides a comprehensive suite of treatments aimed at addressing heart disease directly. As our population ages, more individuals are facing cardiovascular challenges, making innovative and effective therapies more crucial than ever. This article explores ten essential treatments available at Amavita, showcasing their unique benefits and the profound impact they can have on patients’ lives.
As heart health becomes an increasing concern, it’s natural to wonder: what are the most effective strategies to combat these challenges and enhance your quality of life? We understand that navigating health issues can be daunting, but rest assured, you’re not alone in this journey. Our dedicated team is here to support you every step of the way.
Amavita Heart and Vascular Health: Comprehensive Cardiovascular Treatments
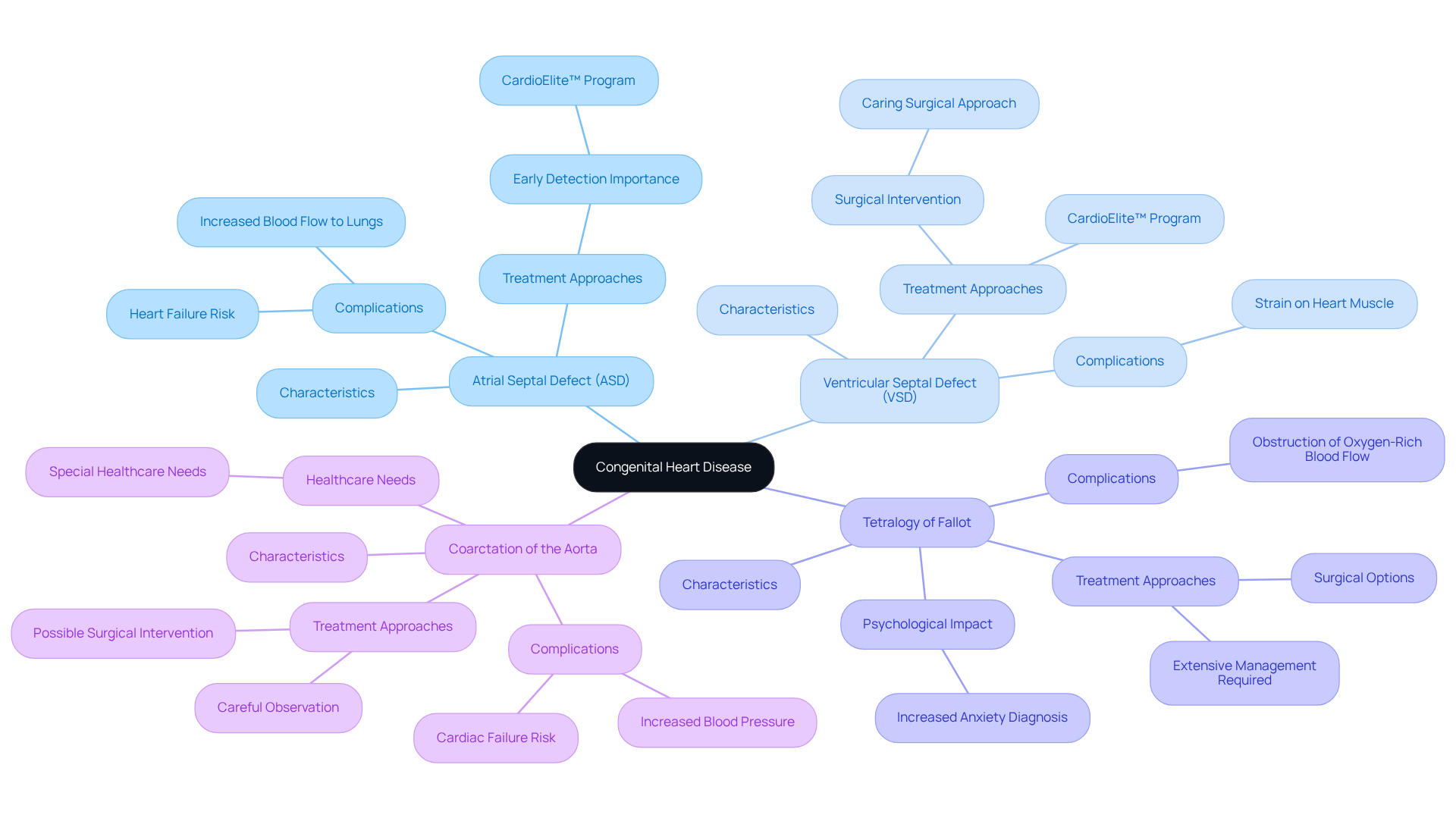
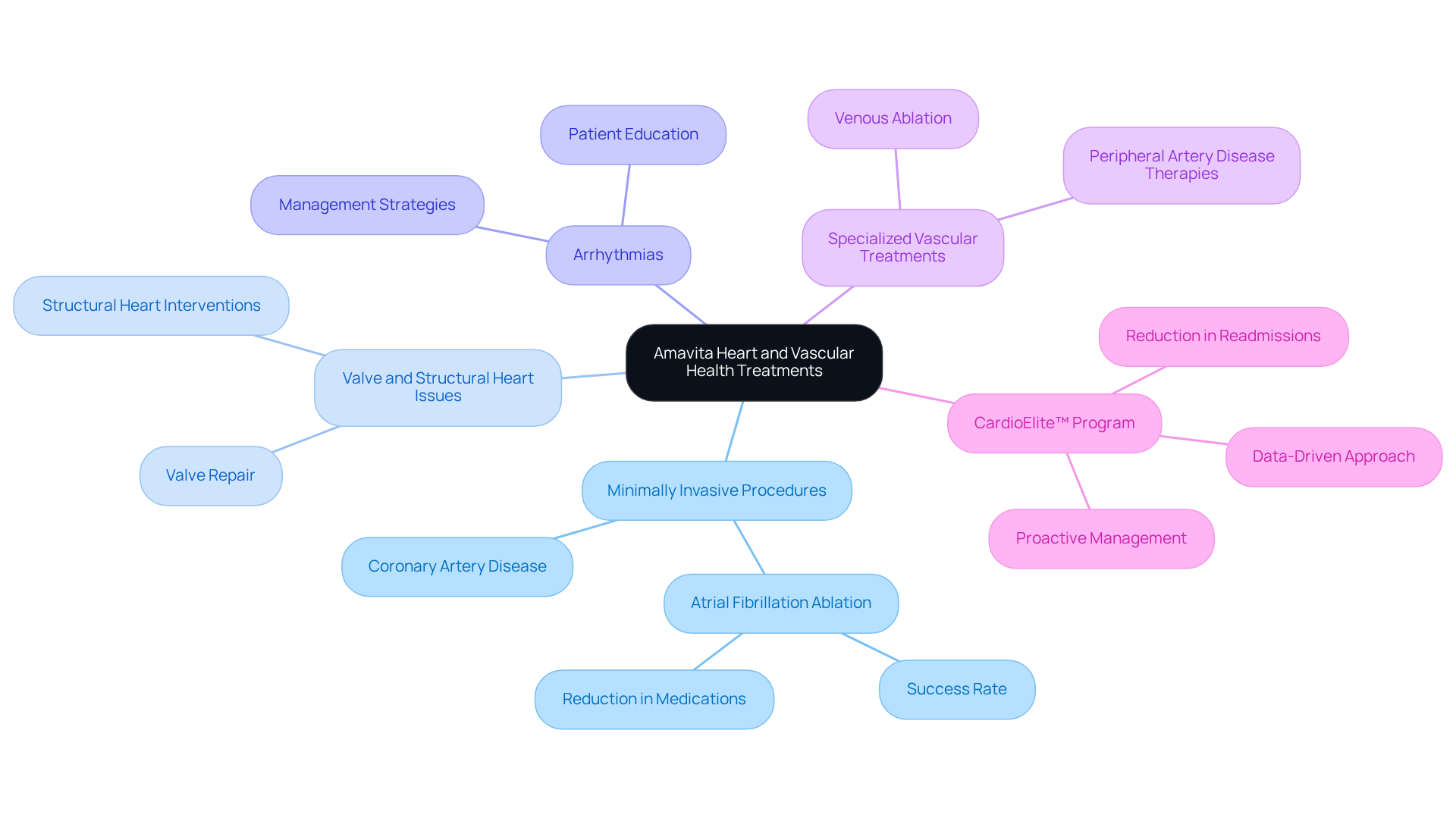
At Amavita Heart and Vascular Health, we understand that facing heart and vascular issues can be daunting, especially for our elderly patients. That’s why we offer a comprehensive range of advanced therapies tailored to meet various cardiac conditions. Our services include:
We prioritize a patient-centered approach, ensuring that each treatment plan, particularly the cardiac rehabilitation program, is customized to enhance your quality of life. We recognize the unique challenges that older adults often face in managing heart disease, and we’re here to support you every step of the way in your health journey. Our commitment to innovative care means we incorporate the latest medical technologies alongside compassionate support into our practice.
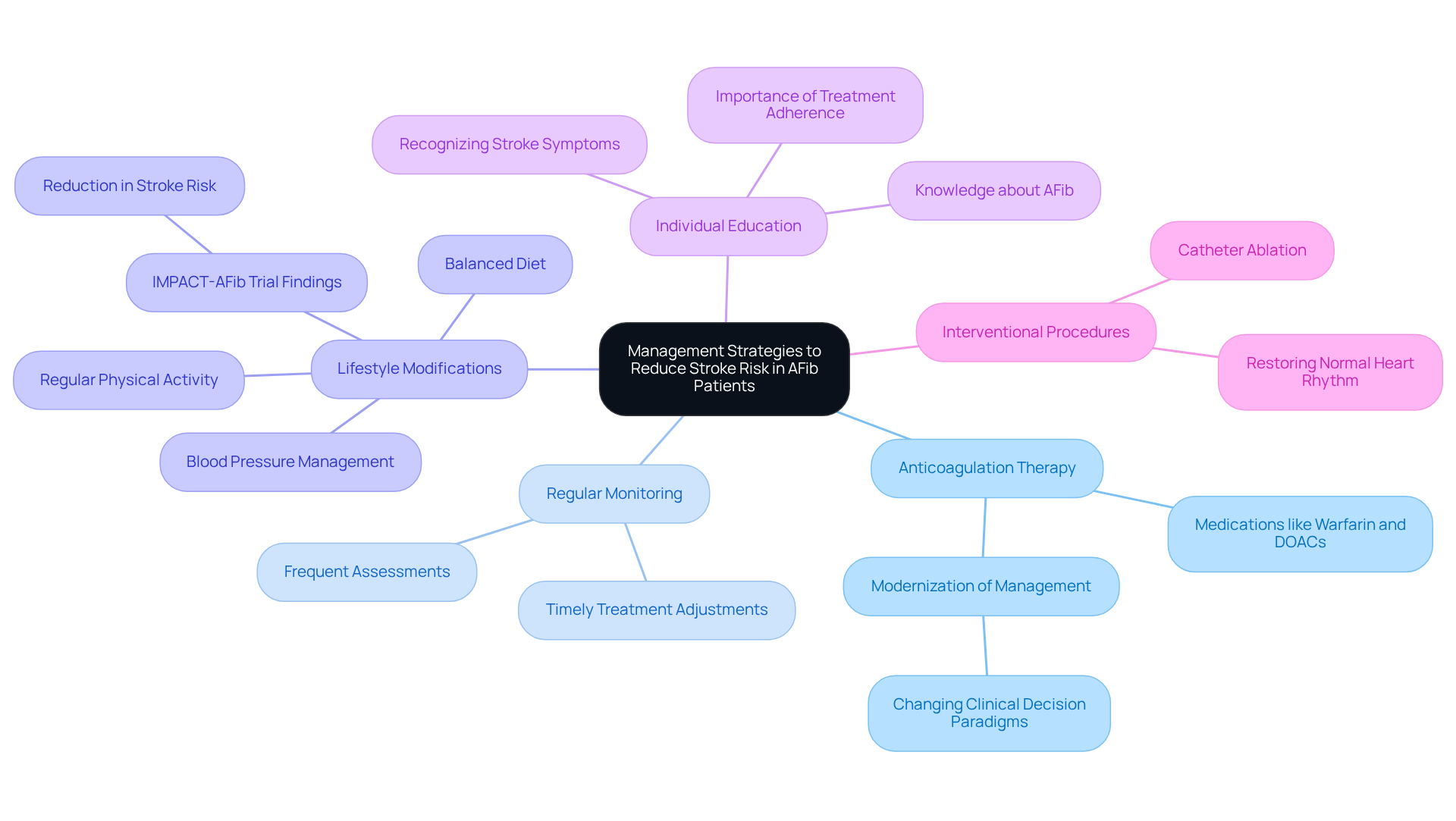
One of our standout offerings is the AFib ablation program, which focuses on proactive, data-driven cardiovascular management. This program has been shown to significantly reduce hospitalizations by up to 70%. As our Amavita Heart and Vascular Health® Content Team emphasizes, “Understanding the intricacies of AFib ablation empowers individuals to make informed decisions about their treatment options.”
This dedication to individualized care shines through in the successful outcomes of our patients. Many patients report substantial decreases in AFib episodes and improved cardiac function. We invite you to reach out and learn more about how we can help you navigate your heart health with understanding and care. Your well-being is our priority, and we’re here to provide the support you need.
Coronary Angioplasty: Minimally Invasive Procedure for Blocked Arteries
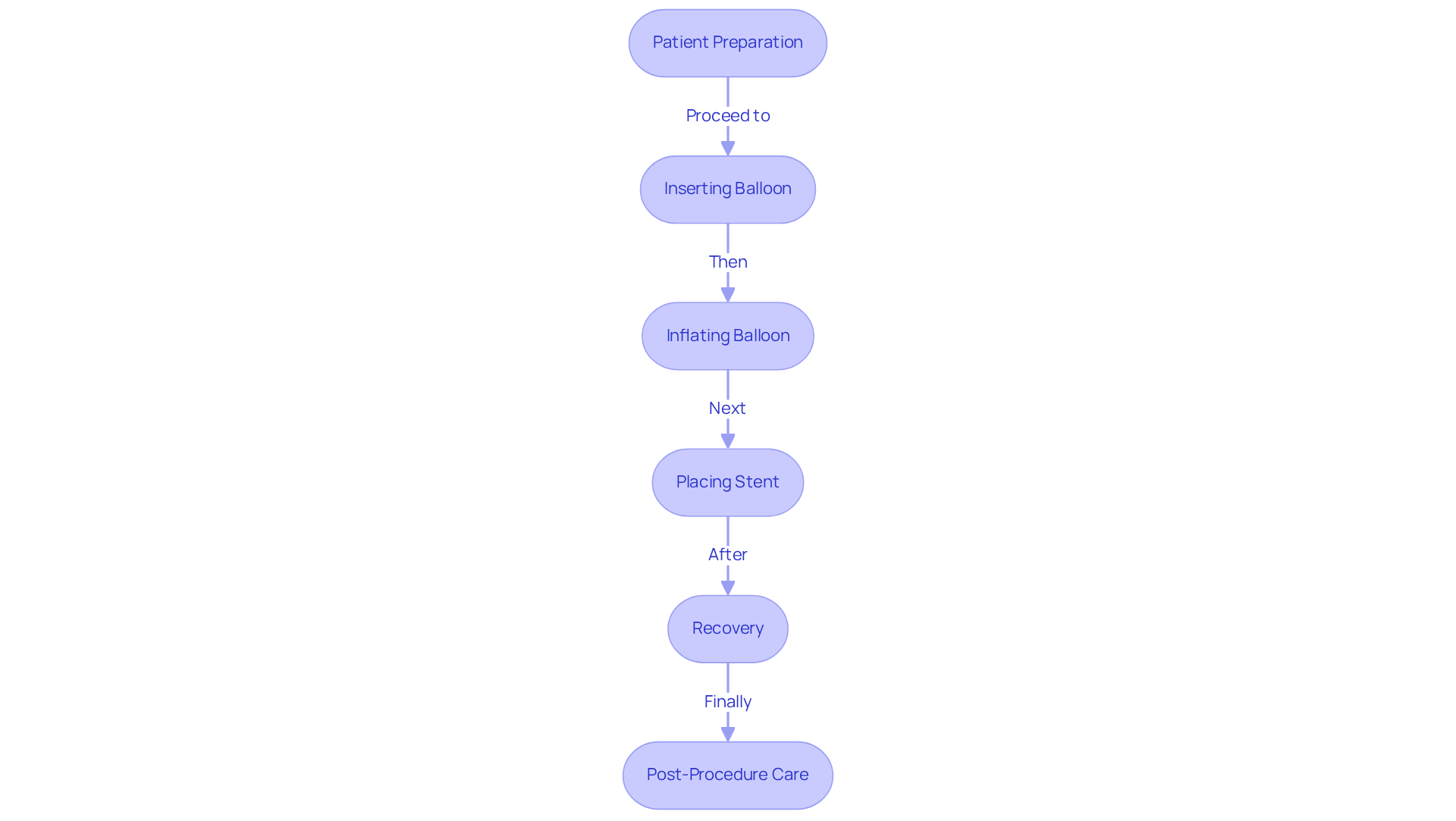
Coronary angioplasty is a procedure designed to open blocked coronary arteries. This technique involves inserting a small balloon at the blockage site, which is then inflated to widen the artery. Often, a stent is placed to maintain the artery’s openness. This method is especially beneficial for individuals who may not meet the criteria for conventional surgery, as it typically results in less recovery time and less discomfort.
At Amavita, our skilled team utilizes advanced techniques to ensure precision during the procedure, which is vital for improving outcomes. Our specialists employ state-of-the-art diagnostic imaging to accurately identify blockages, allowing for effective treatment planning. Patients typically experience a swift recovery, with most resuming normal activities within just 2 to 3 days. Many individuals report feeling considerably better after the procedure, enjoying enhanced energy levels and reduced symptoms of cardiovascular disease.
Success stories abound, showcasing individuals who have regained their quality of life after undergoing angioplasty. For instance, one patient noticed a significant improvement in their ability to engage in everyday tasks without the earlier restrictions caused by cardiovascular issues. Such outcomes highlight the effectiveness of this procedure and the comprehensive care approach at Amavita.
Moreover, the benefits of minimally invasive coronary procedures extend beyond immediate recovery. They include shorter hospital stays and a more comfortable overall experience. It’s important for patients to be aware of warning signs of complications, such as:
- Redness
- Warmth
- Pus
- Fever
- Increasing pain or swelling
If an incision starts to bleed and does not stop with pressure, contacting a doctor is crucial. As one cardiologist noted, “Minimally invasive methods such as angioplasty not only improve recovery but also empower individuals to take control of their heart health.” Additionally, individuals are encouraged to drink 8 to 10 glasses of water within the 24 hours following angioplasty to help flush out the contrast dye used during the procedure.
At our facility, we also emphasize same-day discharge, allowing many individuals to go home shortly after their procedure. Our CardioElite™ program further enhances comprehensive cardiovascular management, ensuring that individuals receive continuous support and monitoring post-procedure.
In summary, coronary angioplasty at our facility represents a crucial treatment for heart disease for individuals facing significant blockages. We merge expertise and compassion to achieve optimal results, ensuring you feel valued and cared for throughout your journey.
Coronary Artery Bypass Grafting: Surgical Solution for Severe Blockages
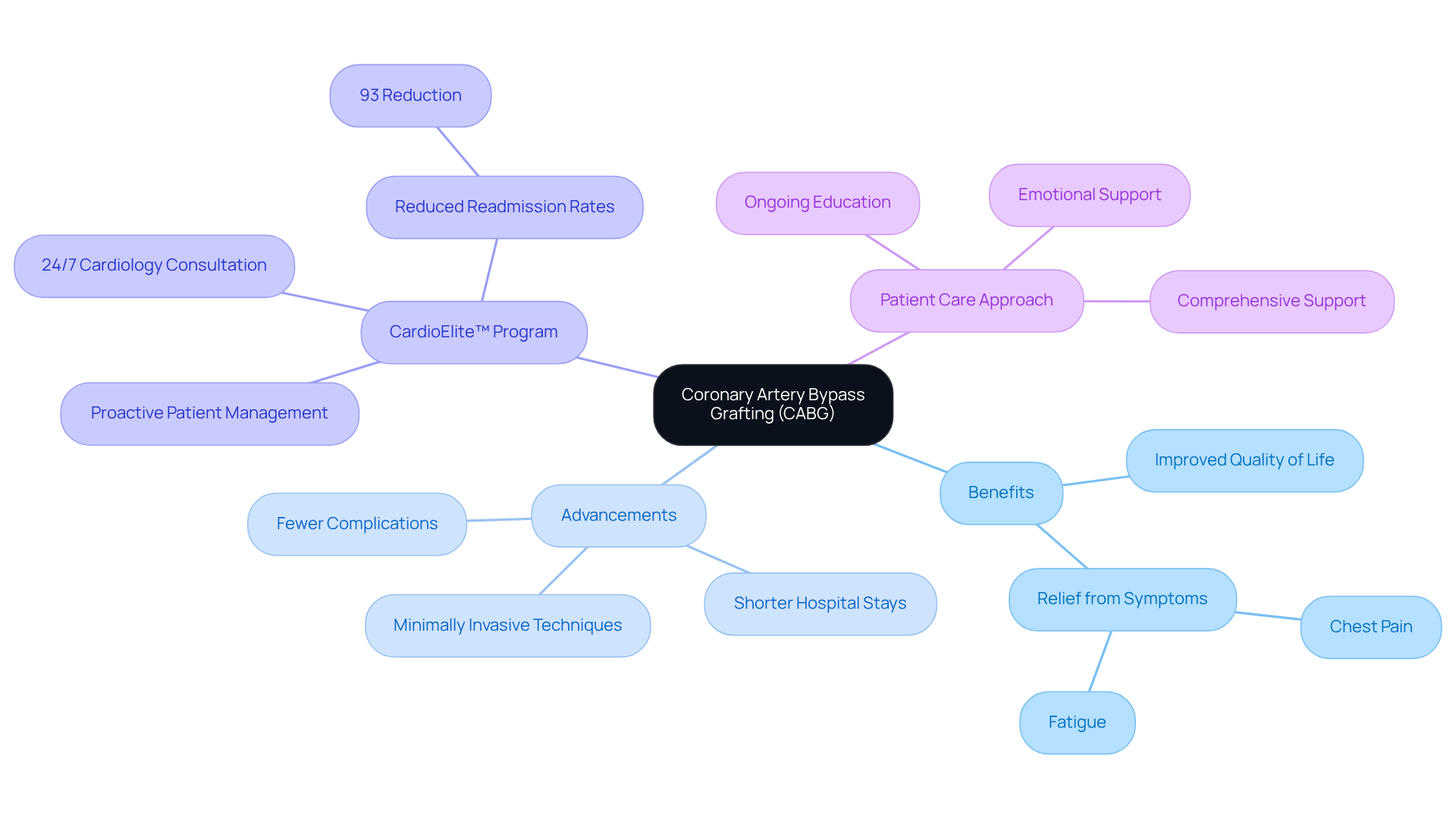
Coronary artery bypass grafting (CABG) is a vital surgical procedure that acts as a solution by addressing severe blockages in the coronary arteries. This intervention creates a new pathway for blood to reach the heart by grafting a blood vessel from another part of the body. It’s particularly beneficial for those with multiple blockages or for individuals who haven’t had success with angioplasty. At our healthcare facility, our surgical team is committed to providing comprehensive care, ensuring that patients receive the care they need during their recovery journey.
In addition to CABG, Amavita’s CardioElite program plays a crucial role in enhancing recovery in skilled nursing facilities (SNFs). This program combines advanced diagnostic tools with 24/7 cardiology consultation, allowing for proactive management of patients and significantly reducing readmission rates by 93%. Many recovery stories from patients highlight the positive changes following CABG, with numerous individuals experiencing a remarkable improvement in their quality of life, including relief from distressing symptoms like chest pain and fatigue. Surgeons emphasize that CABG is a lifesaving procedure, especially for older adults facing complex cardiovascular issues. As Dr. John H. Alexander notes, ‘Coronary artery bypass graft surgery can serve as a lifesaving option in appropriately selected individuals with coronary artery disease.’
Recent advancements in CABG techniques, including minimally invasive approaches, have further enhanced outcomes for patients. These innovative methods often lead to shorter hospital stays, quicker recovery times, and fewer complications. On average, patients can expect to stay in the hospital for about four to five days, depending on their individual circumstances and any potential complications, such as arrhythmia, bleeding, or infection.
At Amavita, our focus on patient-centered care extends well beyond the operating room. We provide ongoing education and support, helping individuals and families make informed decisions about their health. This addresses not only the physical aspects of recovery but also the emotional and social challenges that may arise after surgery. Understanding that older patients may experience cognitive or behavioral changes, our team emphasizes the importance of emotional support during recovery. We encourage patients to discuss their recovery plans with healthcare providers to ensure a comprehensive approach to their care, further enhanced by the proactive strategies of the CardioElite program.
Heart Valve Repair: Restoring Functionality to Damaged Valves
Heart valve repair is a vital procedure aimed at addressing damaged or malfunctioning heart valves. If left untreated, these issues can lead to serious complications. At Amavita, we understand how concerning this can be, which is why we utilize advanced techniques, including minimally invasive methods, to enhance recovery and comfort for our patients. This approach not only allows for faster recovery times but also reduces discomfort, making it especially beneficial for older individuals.
Techniques like valve reshaping, which helps restore the valve’s shape, and the use of clips to secure valve leaflets, play a crucial role in our repair process. Studies indicate that older individuals who undergo heart valve repair experience survival rates comparable to their age-matched peers without cardiovascular issues, underscoring the effectiveness of this procedure. Furthermore, nearly 90% of patients report significant benefits from these minimally invasive techniques, leading to improved cardiac function and overall wellness.
Cardiologists emphasize the importance of heart valve repair as a vital treatment for heart disease, as it can halt the progression of heart conditions and enhance quality of life. Have you or a loved one been feeling anxious about heart health? Success stories from those we serve highlight the profound impact of these procedures, reinforcing our commitment to providing exceptional care. We’re here to support you every step of the way.
Statins: Cholesterol Management for Heart Disease Prevention
Statins lower cholesterol levels in the bloodstream, which can significantly reduce the risk of cardiovascular disease and stroke. By blocking an enzyme that produces cholesterol in the liver, statins are particularly beneficial for older adults, who often face a higher risk of heart-related issues. At our facility, we integrate statins into treatment plans for individuals with elevated cholesterol or those identified as high-risk for heart disease. Our CardioElite™ program emphasizes proactive, data-informed support, including AI integration and 24/7 access to cardiology consultations.
Recent studies highlight the importance of statin therapy. Those not on statins are at a much greater risk of experiencing heart attacks and strokes. For instance, a longitudinal study found that over half of high-risk elderly individuals were not receiving statin therapy, revealing a significant gap in care that proactive management strategies, like those offered by Amavita Heart and Vascular Health®, can help bridge.
Real-life stories demonstrate how effective statin therapy can be. Take Mrs. Fuentes, for example. She struggled with elevated triglyceride levels but found success with a treatment plan that included statins and lifestyle changes. This combination not only improved her cholesterol profile but also empowered her to make healthier choices, showcasing how statins fit into a comprehensive heart health strategy.
Cardiologists generally agree that statins are safe and effective for most people, including the elderly. However, it’s important to monitor for potential side effects. Common issues may include headaches, muscle pain, and digestive problems. Patients should also be aware of possible interactions with other medications and foods, such as grapefruit juice, which can heighten the risk of adverse effects.
The American Heart Association notes that while there are some risks associated with statins, such as a slight increase in the likelihood of diabetes or liver problems, the benefits of statins as a treatment option far outweigh these concerns when used appropriately. Guidelines recommend that patients, especially those over 75, improve their cholesterol management. Additionally, the cost-effectiveness of statins in preventing atherosclerotic cardiovascular disease (ASCVD) makes them a valuable option for elderly patients and their caregivers. Thus, statins remain a cornerstone in heart disease management, particularly for older adults seeking effective treatments like those provided by Amavita.
Beta Blockers: Regulating Heart Rate and Blood Pressure
that help manage pulse rate and blood pressure by blocking adrenaline’s effects on the heart. They are often prescribed for conditions like hypertension, heart failure, and arrhythmias, playing a vital role in improving heart function and reducing the risk of cardiovascular issues.
At our facility, we focus on tailoring beta blocker treatment to meet the unique needs of each individual, especially seniors who may respond differently to these medications. Have you ever wondered how beta blockers work? Recent studies from 2025 show that individualized dosing can lead to significantly better outcomes. This highlights the importance of monitoring and adjustments based on each person’s health profile.
This is a key part of Amavita’s CardioElite™ program, which includes personalized treatment plans and 24/7 cardiology consultations to enhance proactive healthcare management. Our cardiologists emphasize that tailored treatment plans are crucial, as they can lead to improved health and a better quality of life for seniors.
Success stories from individuals illustrate how beta blockers can stabilize pulse rates and manage blood pressure effectively. These medications are significant in heart disease management, ultimately serving as a cornerstone and aiming to reduce hospital readmissions.
If you or a loved one are navigating heart health challenges, know that support is available. We’re here to help you every step of the way.
Angiotensin-Converting Enzyme (ACE) Inhibitors: Supporting Heart Function
Angiotensin-converting enzyme (ACE) inhibitors play a vital role in enhancing blood circulation by relaxing blood vessels. This process helps reduce the workload on your heart, which is especially important for those dealing with conditions like elevated blood pressure and heart disease. At Amavita, we often recommend these medications as part of a comprehensive treatment plan tailored to your needs.
It’s essential to understand that while ACE inhibitors can significantly improve your heart’s function, they also require careful monitoring of kidney and electrolyte levels. This is particularly crucial for older adults, who may face increased risks of side effects. Regular evaluations can help prevent complications, ensuring that these medications work effectively without compromising your kidney health.
Have you ever wondered how ACE inhibitors can make a difference? Real-world examples show that starting treatment at the right time can lead to remarkable improvements in heart health. This reinforces their importance in cardiovascular care, particularly among seniors.
We’re here to support you every step of the way. If you have concerns about your heart health or the medications you’re taking, please don’t hesitate to reach out. Your well-being is our priority, and together, we can navigate your treatment journey with care and understanding.
Nitrates: Alleviating Angina Symptoms
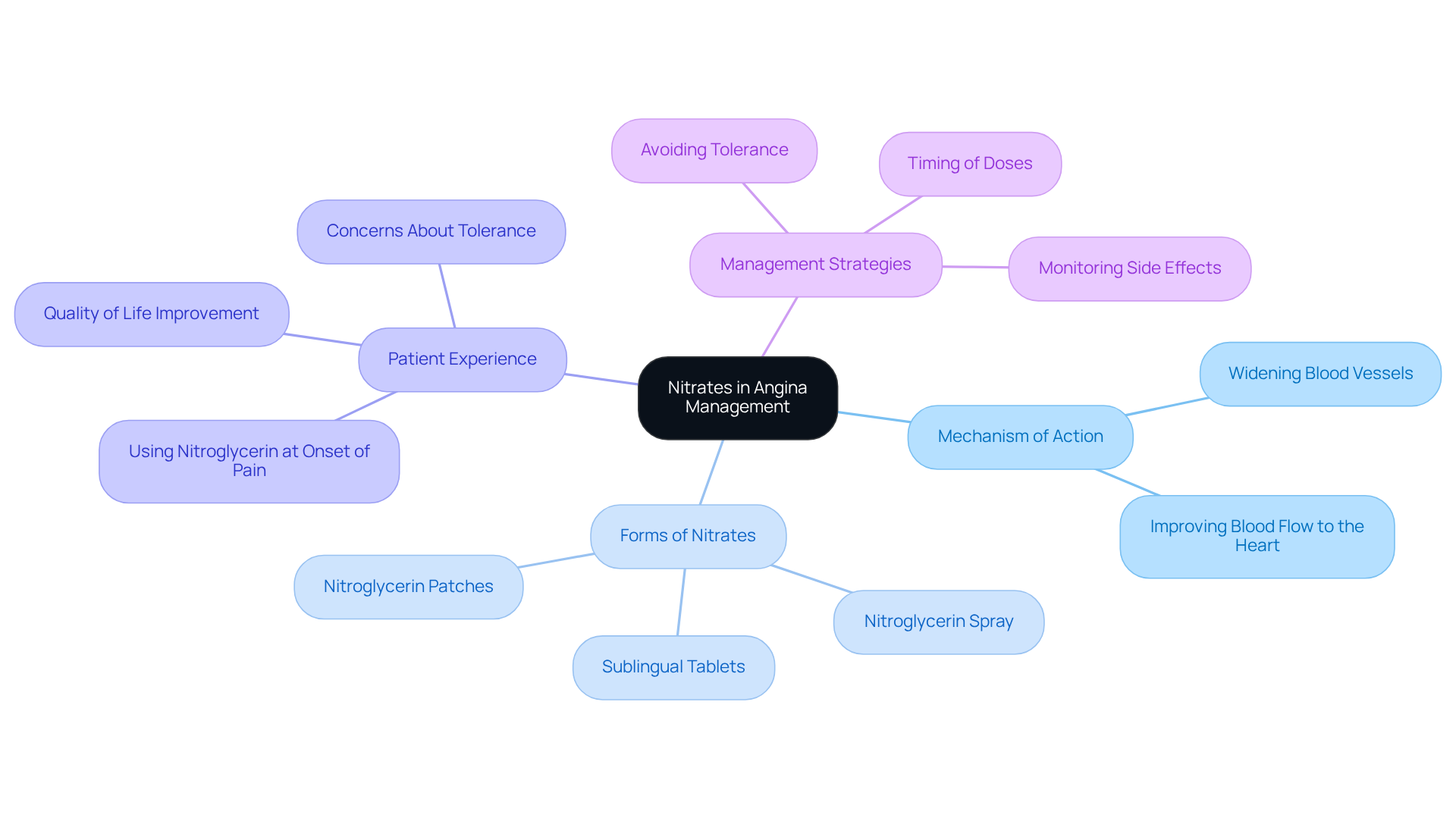
Nitrates play a vital role in easing the discomfort of angina by relaxing blood vessels, which helps improve blood flow to the heart. At Amavita Heart and Vascular Health®, we offer these medications in various forms, including sublingual tablets that provide quick relief during angina attacks.
We understand that managing angina can be challenging, especially for older individuals. Our cardiologists emphasize the importance of using nitrates thoughtfully to avoid tolerance and manage potential side effects. For example, one patient shared how greatly their quality of life improved.
In addition to this, our CardioElite™ program features personalized assessments and lifestyle modifications, ensuring that you receive tailored care that meets your unique needs. We are committed to providing effective treatment options that empower you to maintain your cardiovascular health.
Overall, nitrates are a cornerstone in angina management, equipping you with the necessary tools to take charge of your heart health. At Amavita, we’re here to support you every step of the way, offering guidance and innovative strategies designed with your well-being in mind.
Diuretics: Managing Fluid Retention in Heart Disease
Diuretics, often called ‘water pills,’ play a vital role in helping your body get rid of excess fluid. This can be especially important for those facing heart failure or other cardiovascular issues. By easing fluid overload, diuretics can help alleviate uncomfortable symptoms like swelling and shortness of breath, which can significantly improve your comfort and overall well-being.
At Vascular Health®, we understand the challenges you may face. That’s why we incorporate diuretics into a comprehensive management plan for heart disease. This plan includes:
- A tailored treatment plan just for you
Our dedicated team carefully evaluates how well the diuretics are working and adjusts dosages based on your unique needs, particularly for our elderly patients. This personalized attention helps minimize side effects and enhances your overall health.
But it doesn’t stop there. Our approach not only addresses your immediate symptoms but also provides a strategy to reduce hospital readmissions and improve long-term health outcomes. Through education and support, we’re here to support you every step of the way. Remember, you’re not alone in this journey; we’re committed to helping you achieve a healthier, more comfortable life.
Clinical Trials at Amavita: Accessing Tomorrow’s Heart Treatments
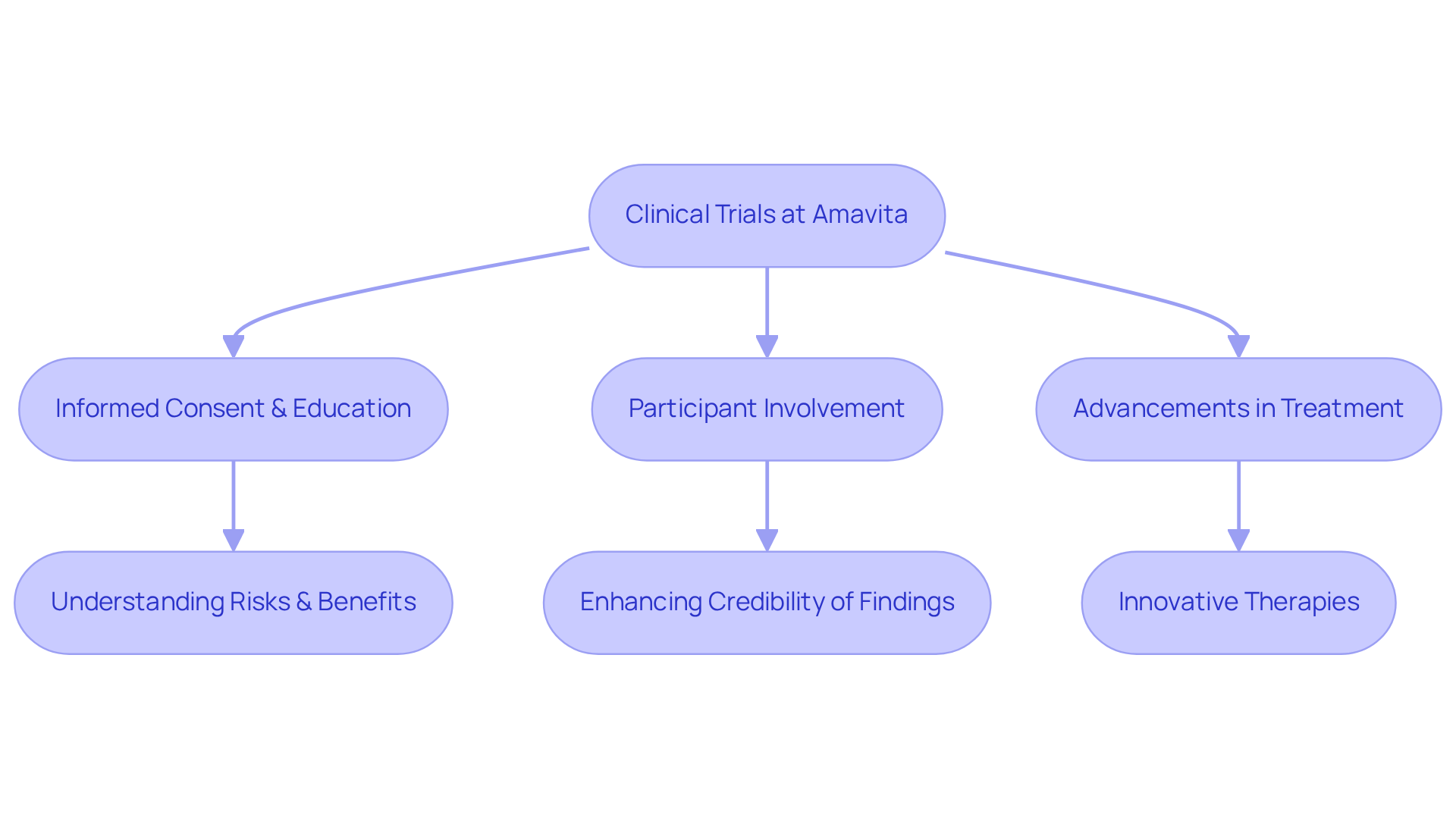
At Amavita Heart and Vascular Health, we’re dedicated to leading research that explore new treatments and therapies. These trials not only offer individuals options that might not yet be part of standard care, but they also empower them to play a vital role in advancing cardiovascular medicine. By participating in clinical research, you can help drive significant progress in the protocols, ultimately improving patient outcomes.
Understanding the importance of clinical trials and participant education is crucial in the clinical trial process. It’s essential that participants fully grasp the potential risks and benefits of their involvement. This commitment to transparency fosters trust and allows individuals to make informed choices about their health.
Recent advancements in cardiovascular clinical research at Amavita have yielded promising results. Our trials focus on therapies that could be effective as a treatment option and greatly enhance patient care. For example, studies have shown that anticoagulant medication can reduce stroke risk from atrial fibrillation by up to two-thirds. This highlights the potential benefits of participating in these trials. Real-life stories from individuals who have taken part in these studies illustrate the positive impact of access to novel treatments for heart disease, demonstrating how these treatments can lead to a better quality of life.
Experts emphasize that patient involvement is essential. Dr. Luke Laffin, a cardiologist at the Cleveland Clinic, noted, “Involving individuals in the research process not only enhances the credibility of the findings but also ensures that the treatments developed align with the needs and preferences of those receiving care.” This collaborative approach is paving the way for a new era in cardiovascular management, where individuals are active contributors in their journeys.
Moreover, Amavita’s CardioElite™ program exemplifies our commitment to patient care. By integrating AI and comprehensive management strategies, including lifestyle modifications and coronary revascularization, we aim to reduce cardiac readmissions and improve hospital quality scores. Our goal is to ensure that patients receive the highest standard of care throughout their treatment journey.
Conclusion
At Amavita Heart and Vascular Health, we’re dedicated to offering comprehensive and innovative treatments for heart disease, shining a light of hope for those facing cardiovascular challenges. Our article showcases a wide array of therapies available, from minimally invasive procedures like coronary angioplasty to surgical options such as coronary artery bypass grafting, along with essential medications like statins and beta blockers. Each treatment is crafted with a patient-centered approach, ensuring that you receive personalized care tailored to your unique health needs.
Key insights from our article highlight how effective these treatments can be in enhancing the quality of life for patients, especially older adults who often navigate complex health issues. The CardioElite™ program stands as a testament to our commitment, integrating advanced diagnostic tools and proactive management strategies to improve patient outcomes. Success stories and data-driven results reinforce the significance of timely and appropriate interventions in managing heart disease.
Ultimately, the message is clear: engaging proactively in your heart health through comprehensive care and innovative treatments can lead to significantly better outcomes for those living with cardiovascular conditions. If you’re looking to understand your options or need support, we encourage you to reach out to Amavita Heart and Vascular Health. By prioritizing your heart health and embracing the latest advancements in treatment, you can take meaningful steps toward a healthier future.
Frequently Asked Questions
What services does Amavita Heart and Vascular Health offer for heart disease treatment?
Amavita Heart and Vascular Health offers a comprehensive range of advanced therapies for heart disease, including minimally invasive procedures for coronary artery disease, valve and structural heart issues, arrhythmias, specialized vascular treatments like venous ablation, and therapies for peripheral artery disease.
What is the CardioElite™ program?
The CardioElite™ program is a proactive, data-driven cardiovascular management initiative that focuses on reducing cardiac readmissions. It has been shown to significantly reduce readmissions by up to 70% and emphasizes individualized care for patients.
How does coronary angioplasty work?
Coronary angioplasty is a minimally invasive procedure that opens blocked coronary arteries by inserting a small balloon at the blockage site, which is then inflated to widen the artery. A stent may also be placed to maintain the artery’s openness.
What are the recovery expectations after coronary angioplasty?
Patients typically experience a swift recovery, with most resuming normal activities within 2 to 3 days. Many individuals report feeling significantly better after the procedure, with enhanced energy levels and reduced symptoms of cardiovascular disease.
What complications should patients watch for after angioplasty?
Patients should be aware of warning signs of complications such as redness, warmth, pus, fever, increasing pain or swelling, and any bleeding from the incision that does not stop with pressure.
What is coronary artery bypass grafting (CABG)?
CABG is a surgical procedure that creates a new pathway for blood to reach the heart by grafting a blood vessel from another part of the body, addressing severe blockages in the coronary arteries. It is particularly beneficial for individuals with multiple blockages or those who have not had success with angioplasty.
How does the CardioElite™ program enhance care for CABG patients?
The CardioElite™ program combines advanced diagnostic tools with 24/7 cardiology consultation, allowing for proactive management of patients in skilled nursing facilities and significantly reducing readmission rates by 93%.
What advancements have been made in CABG techniques?
Recent advancements in CABG techniques include minimally invasive options that lead to shorter hospital stays, quicker recovery times, and fewer complications. Patients can typically expect to stay in the hospital for about four to five days.
What support does Amavita provide for patients after CABG surgery?
Amavita provides ongoing education and support for patients after CABG surgery, helping them manage their recovery and make informed decisions about their health. The approach also addresses emotional and social challenges that may arise during recovery.
List of Sources
- Amavita Heart and Vascular Health: Comprehensive Cardiovascular Treatments
- ENSURING PATIENT-CENTERED ACCESS TO CARDIOVASCULAR DISEASE MEDICINES IN LOW- AND MIDDLE-INCOME COUNTRIES THROUGH HEALTH-SYSTEM STRENGTHENING – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9771684)
- amavita.health (https://amavita.health/blog/understanding-a-fib-ablation-techniques-preparation-and-benefits)
- hTEE-guided Management of a Hemodynamically Unstable LVAD Patient – Hemodynamic Ultrasound for ICU | ImaCor (https://imacorinc.com/hemodynamic-ultrasound/blog/case_studies/htee-guided-management-of-a-hemodynamically-unstable-lvad-patient)
- 10 Inspiring Patient Experience Quotes | Relias (https://relias.com/blog/patient-experience-quotes)
- Coronary Angioplasty: Minimally Invasive Procedure for Blocked Arteries
- Recovery After Coronary Angioplasty: What to Expect (https://resources.healthgrades.com/right-care/angioplasty/recovery-after-coronary-angioplasty-what-to-expect)
- Coronary Artery Bypass Grafting: Surgical Solution for Severe Blockages
- Coronary Artery Bypass Graft | CABG | MedlinePlus (https://medlineplus.gov/coronaryarterybypasssurgery.html)
- Coronary Artery Bypass Grafting (CABG) – Cardiovascular Disorders – MSD Manual Professional Edition (https://msdmanuals.com/professional/cardiovascular-disorders/coronary-artery-disease/coronary-artery-bypass-grafting-cabg)
- Elderly CABG Patients Stand to Benefit From Artery-Only Strategy (https://tctmd.com/news/elderly-cabg-patients-stand-benefit-artery-only-strategy)
- Living Within Limits: Unpleasant Experiences From the Perspective of Patients After Cardiac Surgery, a Content Analysis Study (https://brieflands.com/journals/jjcdc/articles/21720)
- Humacyte Announces Planned IND Filing in 2025 to Support First-In-Human Clinical Study of Small-Diameter ATEV™ for Coronary Artery Bypass Grafting | Humacyte, Inc. (https://investors.humacyte.com/news-releases/news-release-details/humacyte-announces-planned-ind-filing-2025-support-first-human)
- Heart Valve Repair: Restoring Functionality to Damaged Valves
- 10 Essential Foods for Your Cardiac Diet Menu (https://amavita.health/blog/10-essential-foods-for-your-cardiac-diet-menu)
- Johns Hopkins Advances Treatment for Patients with Mitral Valve Disease (https://hopkinsmedicine.org/news/articles/2023/10/johns-hopkins-advances-treatment-for-patients-with-mitral-valve-disease)
- 10 Cardiac Fatigue Symptoms Every Elderly Patient Should Know (https://amavita.health/blog/10-cardiac-fatigue-symptoms-every-elderly-patient-should-know)
- Mitral valve surgery in elderly patients with mitral regurgitation: repair or replacement with tissue valve? – PubMed (https://pubmed.ncbi.nlm.nih.gov/23314759)
- Statins: Cholesterol Management for Heart Disease Prevention
- Statin utilization and cardiovascular outcomes in a real-world primary prevention cohort of older adults (https://sciencedirect.com/science/article/pii/S2666667724000321)
- Statins for cholesterol control: Benefits, risks, and more (https://medicalnewstoday.com/articles/statins-for-cholesterol-control)
- Primary Prevention With Statins in the Elderly – American College of Cardiology (https://acc.org/Latest-in-Cardiology/ten-points-to-remember/2018/01/02/17/14/Primary-Prevention-With-Statins-in-the-Elderly)
- 5.1: Appendix A – Case Studies (https://med.libretexts.org/Bookshelves/Nutrition/Culinary_Medicine_2025e_(Antonopoulos_et_al.)/05:_Appendices/5.01:Appendix_A-_Case_Studies)
- Beta Blockers: Regulating Heart Rate and Blood Pressure
- Beta-Blockers Don’t Benefit All Heart Attack Survivors — and May Raise Heart Risks for Women (https://everydayhealth.com/cardiovascular-diseases/beta-blockers-dont-benefit-everyone-after-heart-attack)
- Beta blockers linked to reduced 1-Year mortality in critically ill congestive heart failure patients with differential benefits across subgroups – Scientific Reports (https://nature.com/articles/s41598-025-17483-3)
- Beta-blockers Not Helpful After MI in Patients With Preserved EF (https://tctmd.com/news/beta-blockers-not-helpful-after-mi-patients-preserved-ef)
- Large-scale study confirms that millions of people are taking a heart attack drug unnecessarily (https://english.elpais.com/science-tech/2025-11-10/large-scale-study-confirms-that-millions-of-people-are-taking-a-heart-attack-drug-unnecessarily.html)
- Comparative Effectiveness of β-Blocker Use Beyond 3 Years After Myocardial Infarction and Long-Term Outcomes Among Elderly Patients | Circulation: Cardiovascular Quality and Outcomes (https://ahajournals.org/doi/10.1161/CIRCOUTCOMES.118.005103)
- Angiotensin-Converting Enzyme (ACE) Inhibitors: Supporting Heart Function
- Early treatment with ACE inhibitors improves cardiac outcomes of patients with Becker muscular dystrophy (https://news-medical.net/news/20210920/Early-treatment-with-ACE-inhibitors-improves-cardiac-outcomes-of-patients-with-Becker-muscular-dystrophy.aspx)
- ACE inhibitors and ARBs: Managing potassium and renal function (https://ccjm.org/content/86/9/601)
- Prescribing dilemma: angiotensin-converting enzyme inhibitors for heart failure in an older patient (https://pharmaceutical-journal.com/article/ld/prescribing-dilemma-angiotensin-converting-enzyme-inhibitors-for-heart-failure-in-an-older-patient)
- Products – Data Briefs – Number 347 – August 2019 (https://cdc.gov/nchs/products/databriefs/db347.htm)
- Nitrates: Alleviating Angina Symptoms
- A cardiologist’s advice on how to use this “wonder drug” (https://myheartsisters.org/2013/08/19/nitroglycerin)
- The role of organic nitrates in the optimal medical management of angina (https://escardio.org/Journals/E-Journal-of-Cardiology-Practice/Volume-15/The-role-of-organic-nitrates-in-the-optimal-medical-management-of-angina)
- Nitroglycerin – StatPearls – NCBI Bookshelf (https://ncbi.nlm.nih.gov/books/NBK482382)
- Researchers urge caution in co-prescribing potency drugs and nitrates (https://news.ki.se/researchers-urge-caution-in-co-prescribing-potency-drugs-and-nitrates)
- Clinical Trials at Amavita: Accessing Tomorrow’s Heart Treatments
- thehealthinnovationnetwork.co.uk (https://thehealthinnovationnetwork.co.uk/case_studies/supporting-the-detection-of-atrial-fibrillation-and-optimising-treatment)
- Underrepresentation of women in cardiovascular trials- it is time to shatter this glass ceiling – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10978176)
- statnews.com (https://statnews.com/2024/08/27/clinical-trials-payments-congress-taxes)
- Cleveland Clinic First-In-Human Trial of CRISPR Gene-Editing Therapy Shown to Safely Lower Cholesterol and Triglycerides (https://newsroom.clevelandclinic.org/2025/11/08/cleveland-clinic-first-in-human-trial-of-crispr-gene-editing-therapy-shown-to-safely-lower-cholesterol-and-triglycerides)