Introduction
Recognizing the visual indicators of Peripheral Artery Disease (PAD) is crucial. This common circulatory condition can significantly impact your quality of life. By exploring the stark contrasts between healthy legs and those affected by PAD, you can gain valuable insights into your vascular health and the potential risks associated with this often-overlooked disease.
But what happens when these visual signs go unnoticed? How can early detection change outcomes for those at risk? Understanding these dynamics is essential for proactive health management. It empowers you to seek timely intervention, ensuring you receive the care you deserve.
In addition to this, being aware of your body’s signals can lead to a more informed approach to your health. Remember, you’re not alone in this journey. Many individuals share similar concerns, and reaching out for support can make all the difference. Together, we can navigate these challenges and work towards a healthier future.
Define Peripheral Artery Disease and Its Visual Indicators
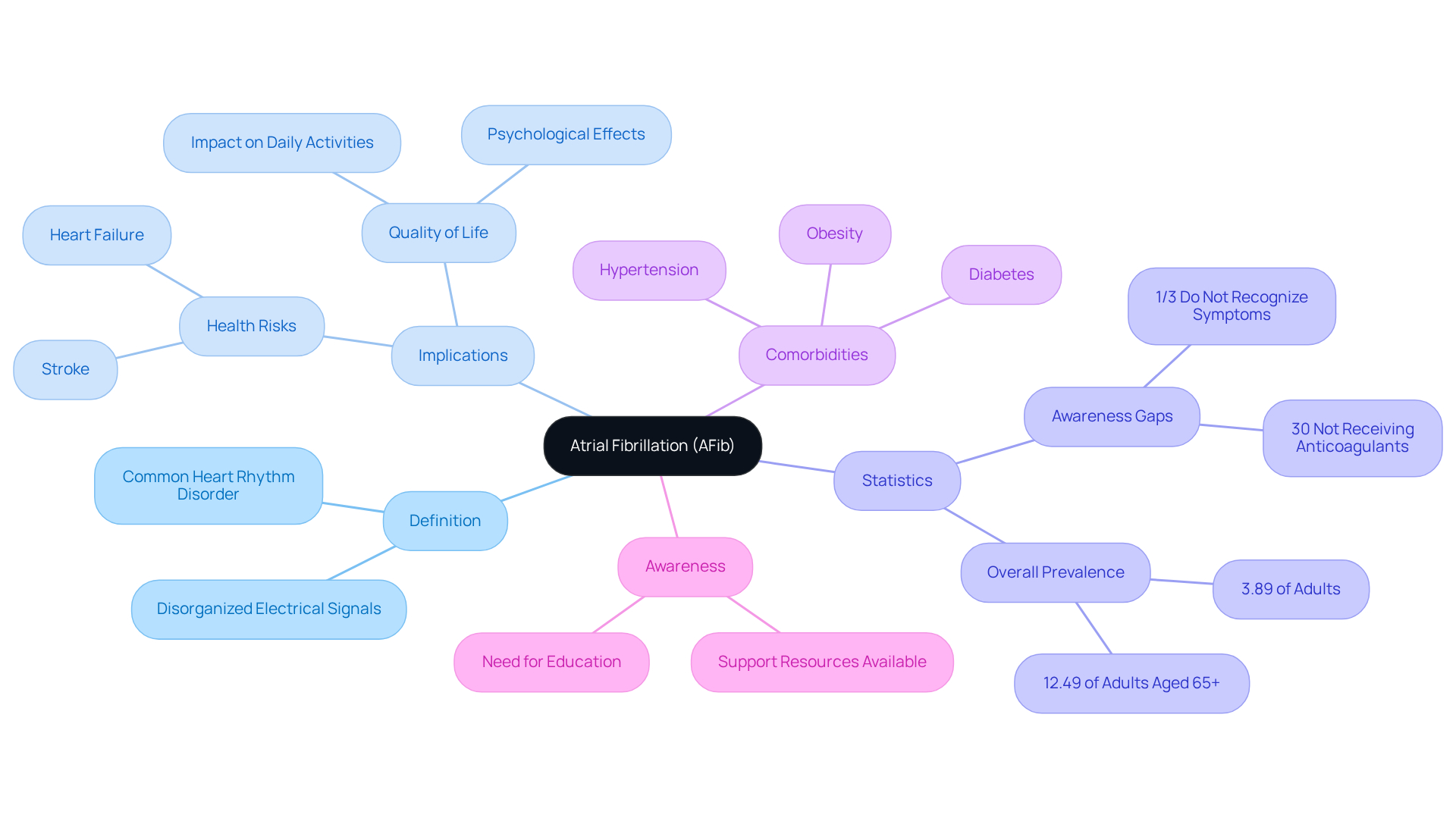
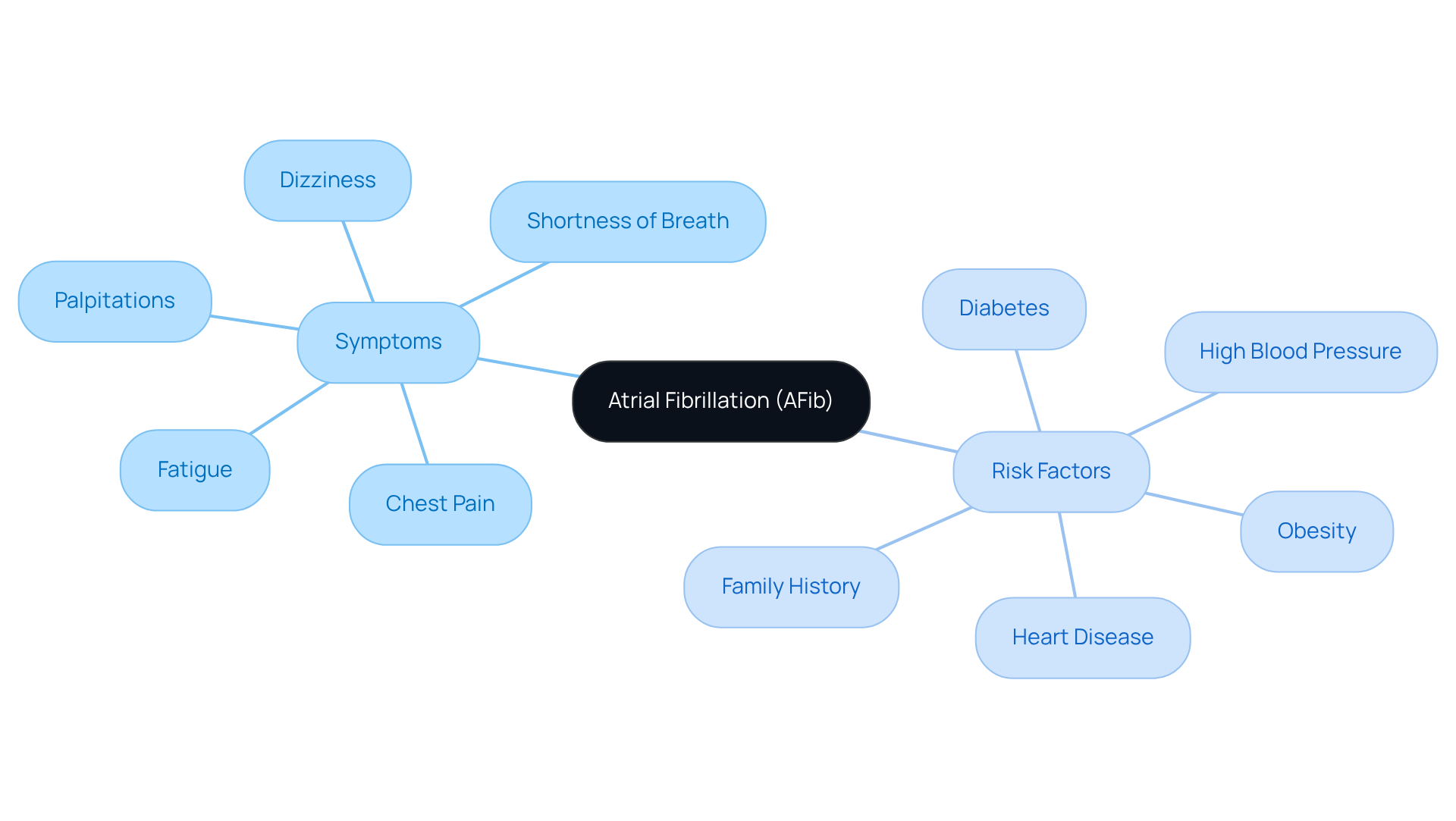
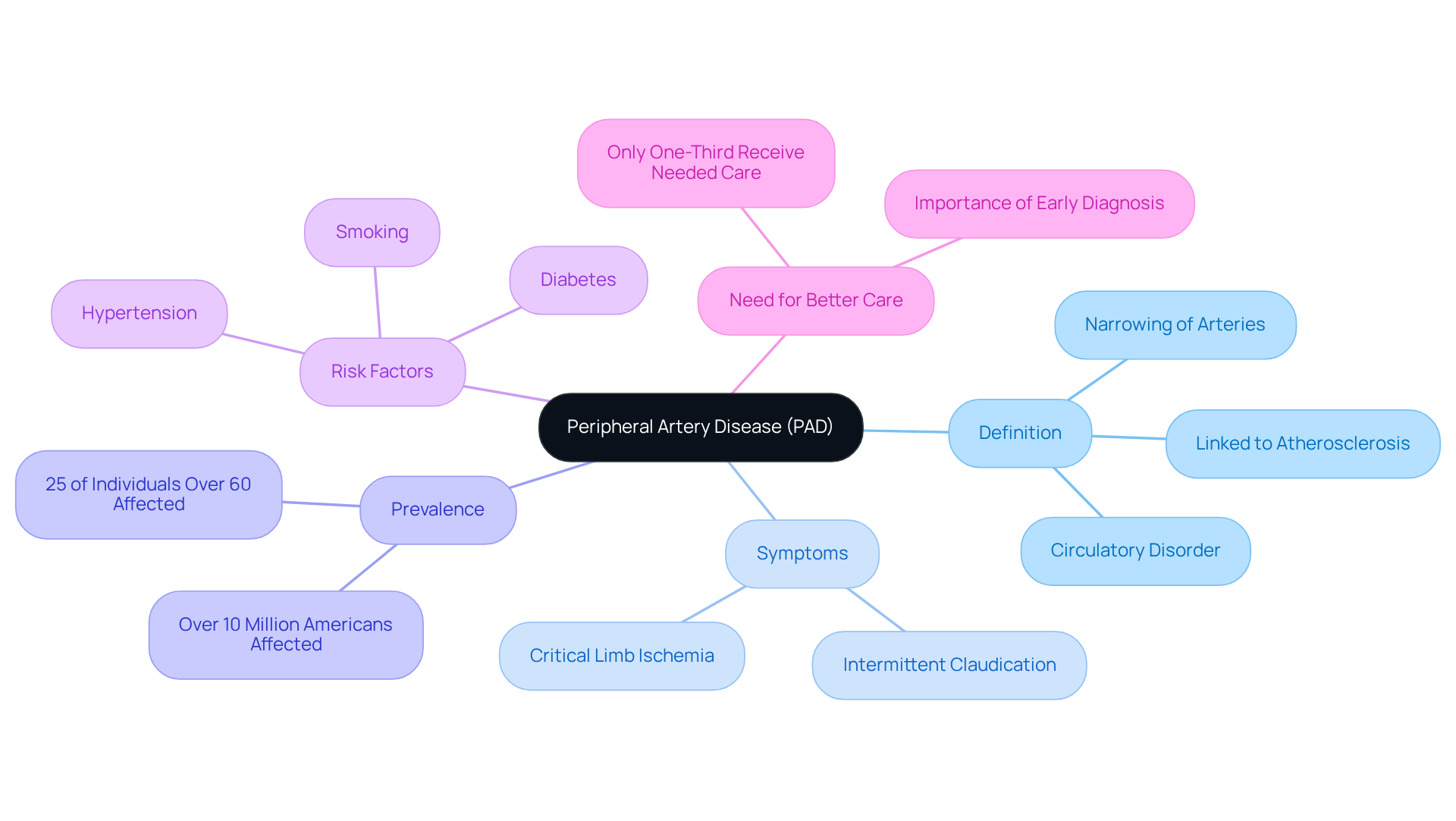
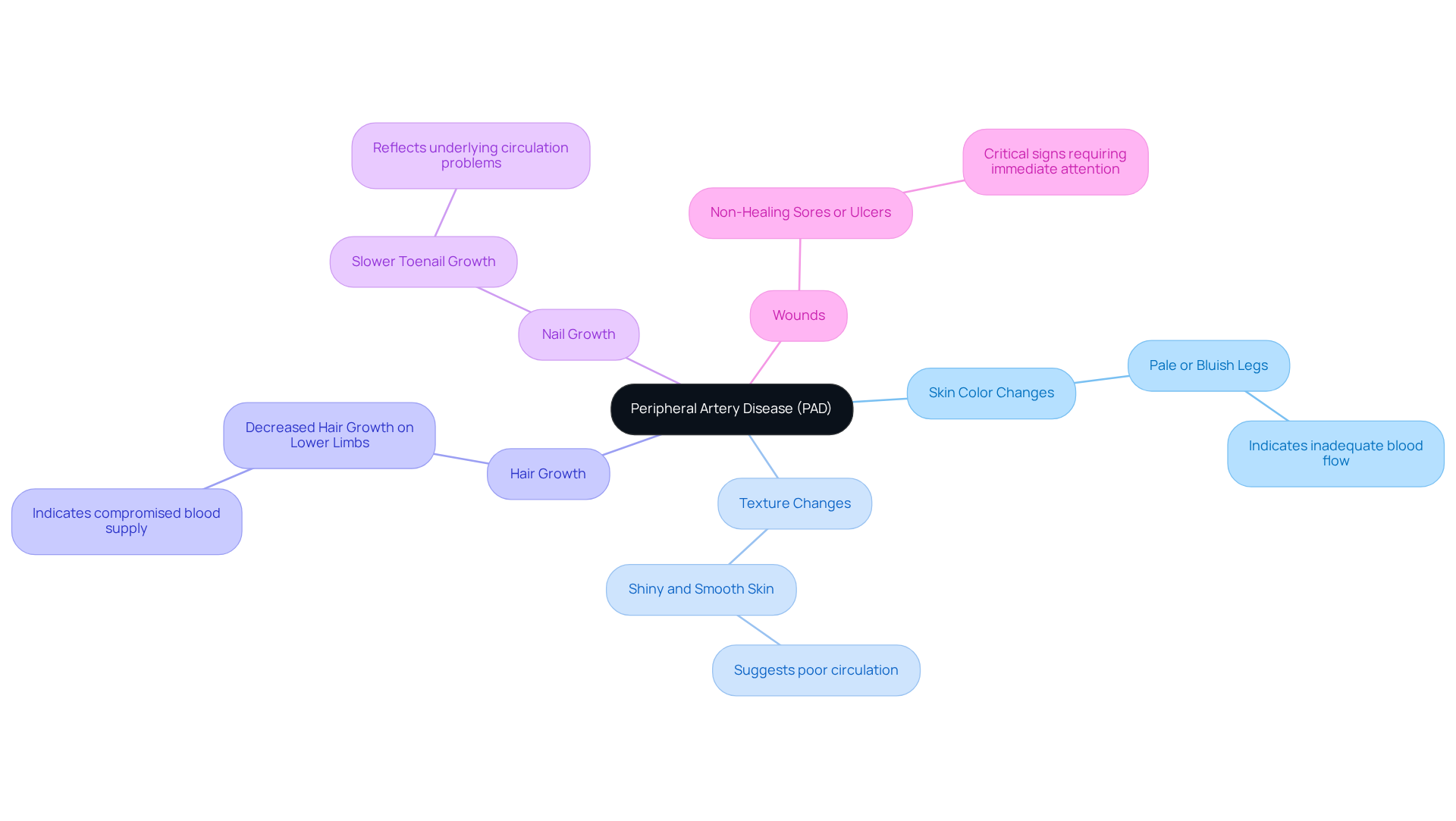
(PAD) is a common circulatory condition that can significantly impact your quality of life. It occurs when narrowed arteries reduce blood flow to your extremities, particularly your legs. Often, this is due to atherosclerosis, where fatty deposits build up in the artery walls. Understanding the visual indicators is crucial for your health, as illustrated by various symptoms. Here are some key visual indicators to watch for:
- Color Changes: If your legs appear pale or bluish, it may signal inadequate blood flow.
- Texture Changes: Shiny, smooth skin can indicate poor circulation, as seen in pictures of affected legs.
- Hair Loss: A decrease in hair growth on your lower limbs might suggest PAD, which can be visually represented in images, as healthy blood circulation is vital for hair follicles.
- Nail Growth: Slow nail growth can reflect compromised blood supply, a common issue for those with pictures of affected legs.
- Wounds: Non-healing wounds, which can be seen in images, are critical signs that require immediate medical attention.
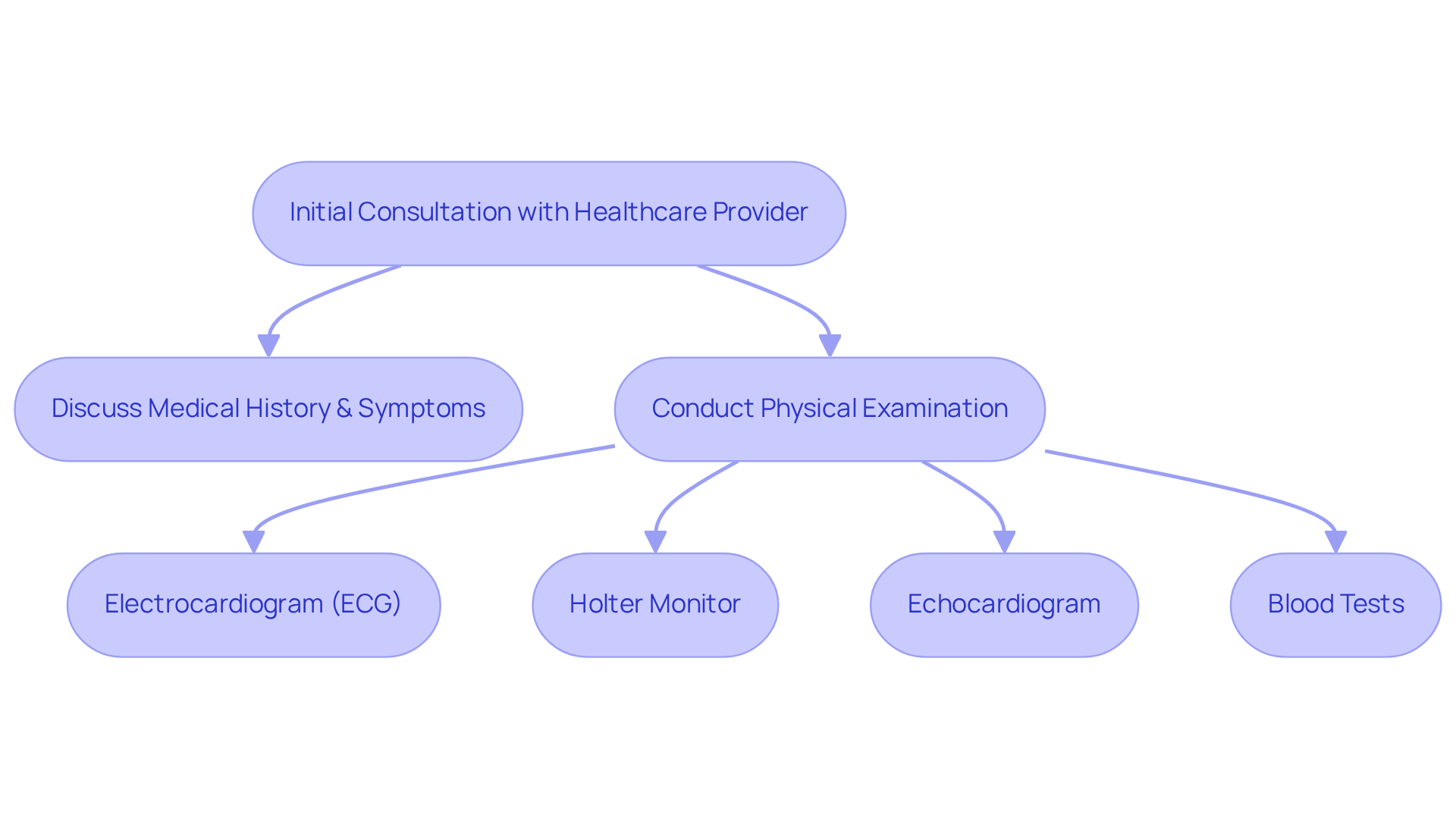
Recognizing these indicators is vital for early diagnosis and intervention, which can greatly enhance your outcomes, especially when interpreting pictures of affected legs. Recent studies show that early detection can lead to timely treatment through lifestyle changes, medication, and surgery. This proactive approach can significantly reduce the risk of severe complications, such as amputations. In fact, 85% of amputations due to severe PAD are preventable with timely intervention and appropriate care. Alarmingly, nearly 70% of individuals with PAD are unaware of their condition, highlighting the importance of awareness and education in managing this disease effectively.
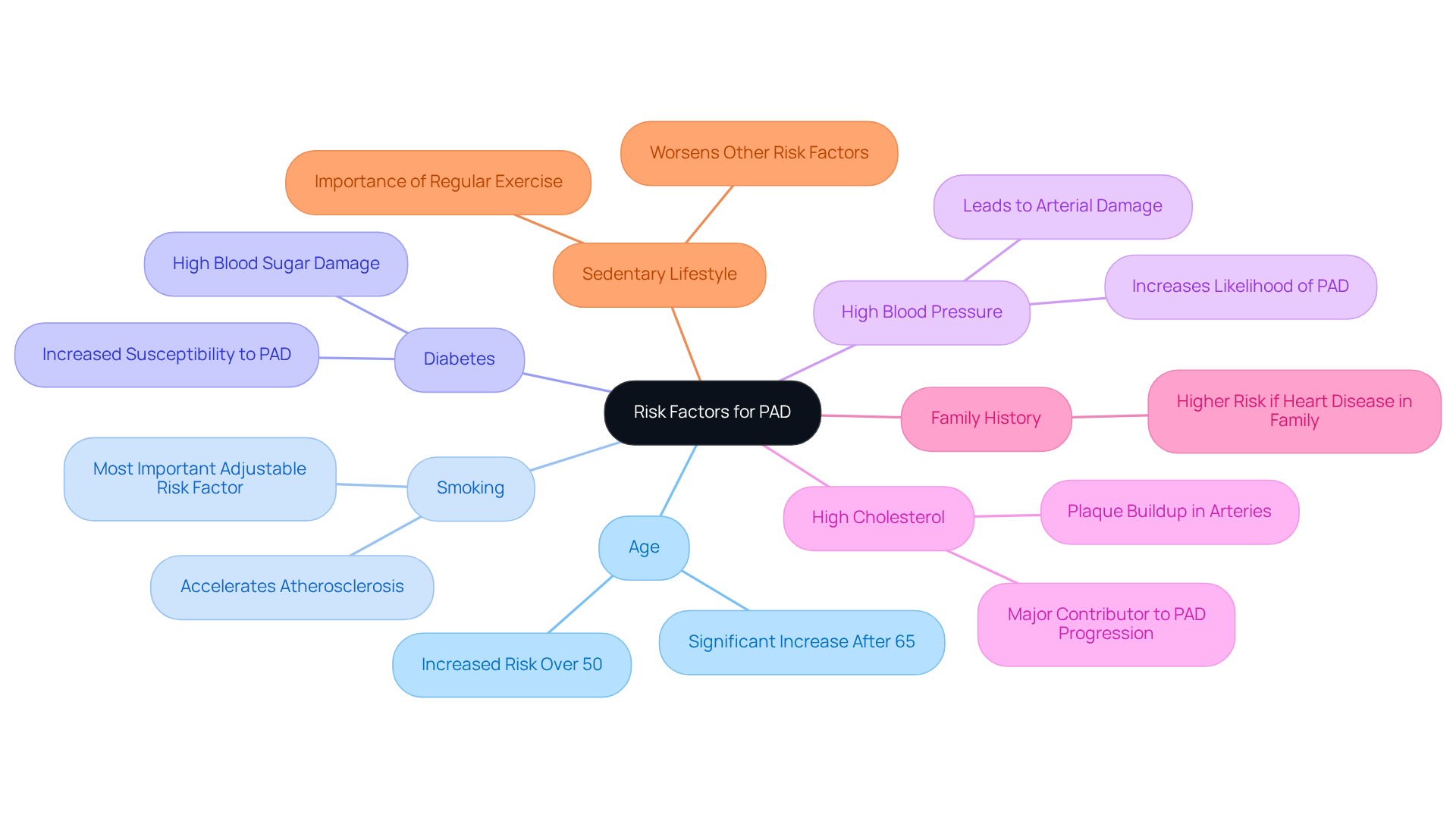
At Amavita, we understand how concerning this can be. Our program is designed to revolutionize cardiovascular care by providing advanced bedside diagnostics that facilitate early detection of conditions like PAD. Powered by the AISAP platform, our dedicated team can perform comprehensive cardiac assessments, ensuring that high-risk patients – like those with diabetes, hypertension, or a family history of heart disease – receive the targeted care they need.
Looking ahead, projections indicate a staggering 220% increase in PAD cases by 2050. This underscores the urgency of recognizing PAD symptoms and the need for proactive management. If you or a loved one are experiencing any of these symptoms, please don’t hesitate to reach out for support. We’re here to help you navigate your health journey with compassion and expertise.
Identify Characteristics of Healthy Legs
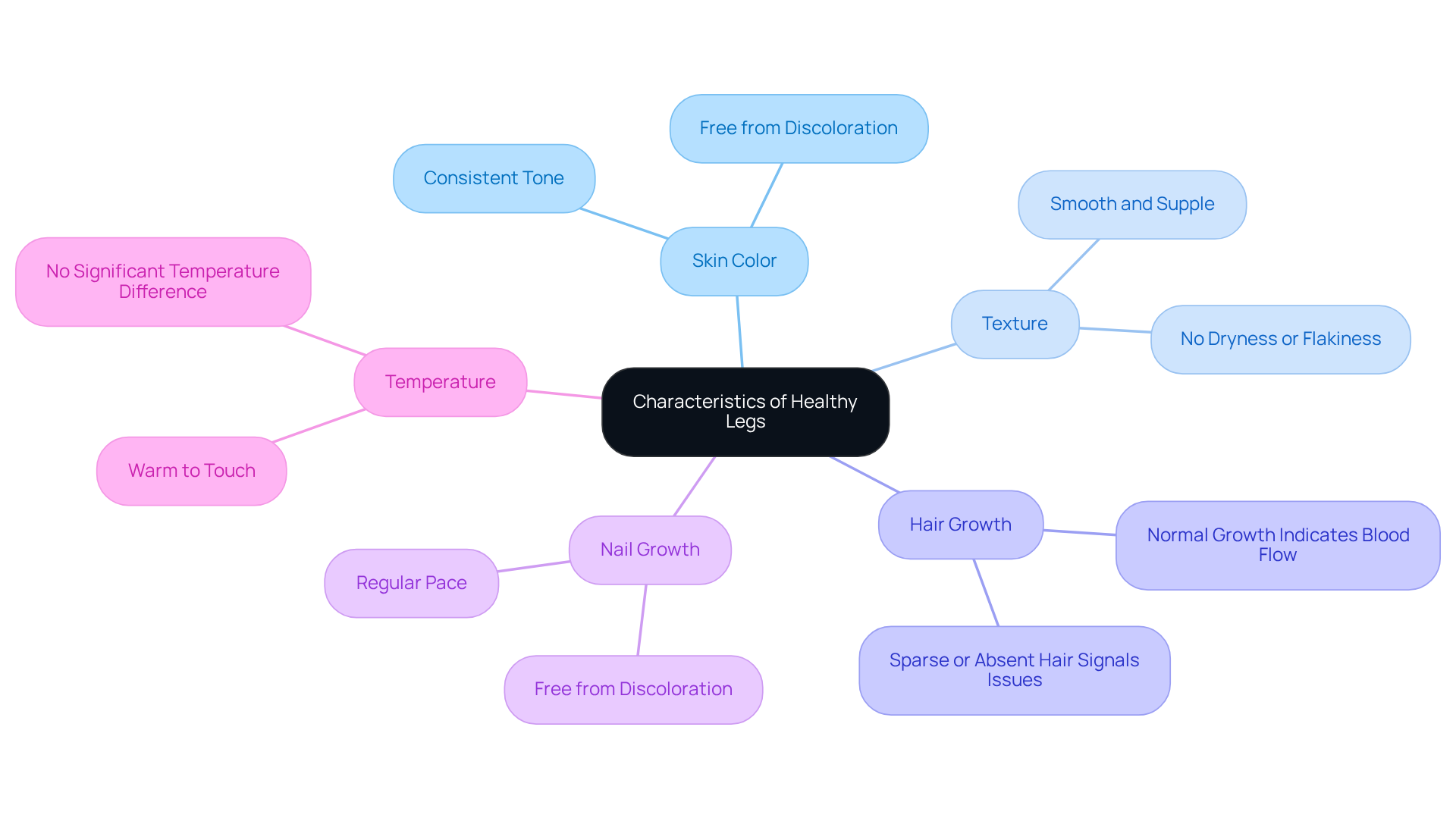
Healthy legs show several important signs that reflect good circulation and overall health.
- Skin Color: A healthy leg usually has a consistent skin tone, free from discoloration or unusual markings. While normal skin color can vary from light to dark shades based on ethnicity, it should remain uniform.
- Texture: The skin should feel smooth and supple, without any signs of dryness or flakiness. Healthy skin texture often indicates proper hydration and circulation.
- Hair Growth: Normal hair growth on the lower limbs suggests adequate blood flow. Sparse or absent hair might indicate underlying issues.
- Nail Growth: Healthy toenails grow at a regular pace and are free from discoloration or deformities. Consistent nail growth is a sign of good health.
- Temperature: Healthy limbs should feel warm to the touch, indicating good blood circulation. If you notice a significant temperature difference between your legs, it could signal potential circulation problems.
Recognizing these characteristics is crucial for spotting any deviations that may indicate underlying medical issues, including pictures of PAD in legs. If you experience pain, swelling that doesn’t go away overnight, skin changes, or large varicose veins, it’s important to consult a doctor. Regularly monitoring these features can aid in early detection and intervention, ultimately enhancing your quality of life.
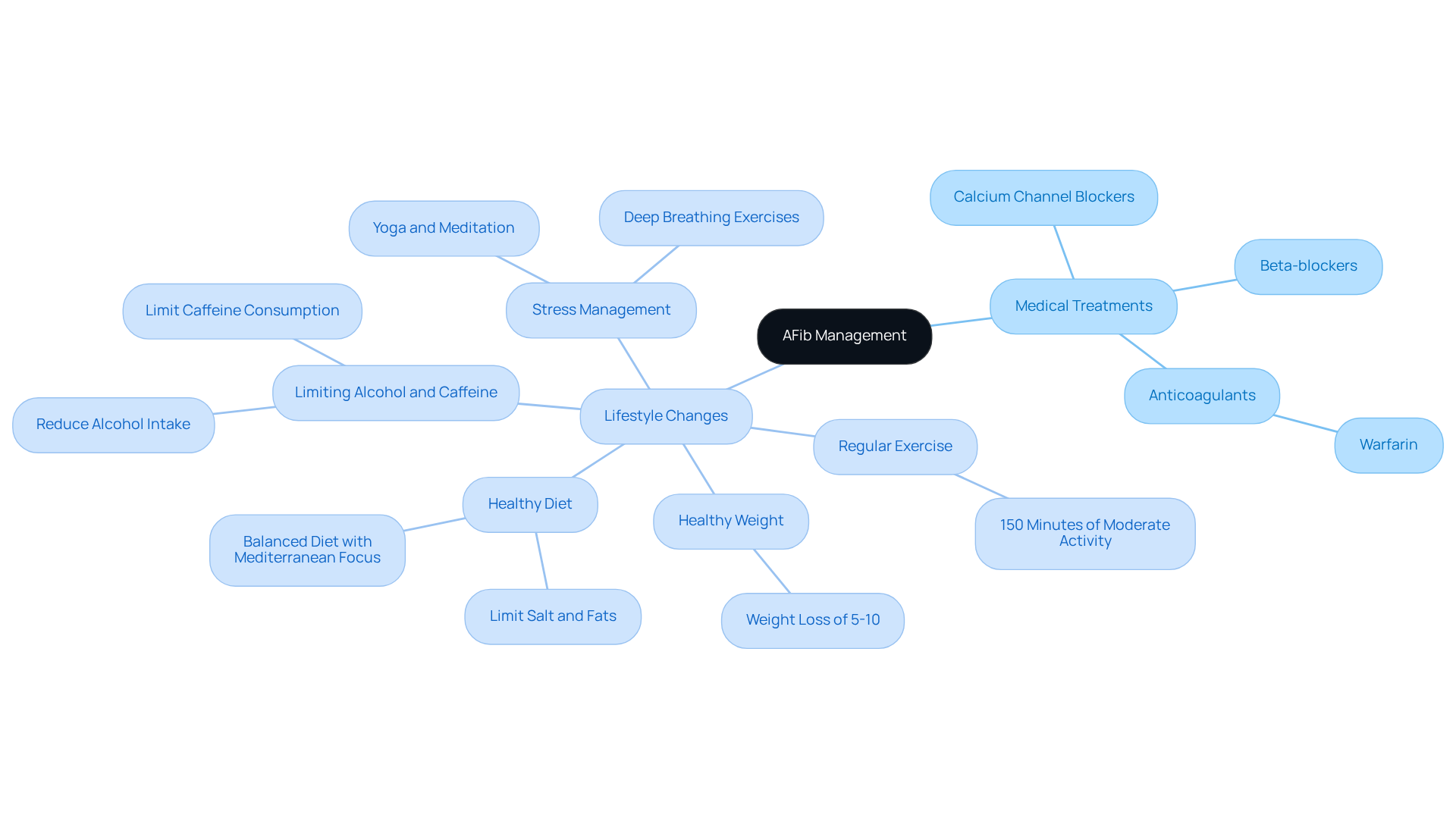
In addition to this, lifestyle factors like regular movement, staying hydrated, and maintaining a balanced diet. Including foods rich in antioxidants and anti-inflammatory nutrients can also support vascular well-being. Exercise or a wellness program are essential for proactive wellness management, especially if you’re at risk of PAD, and can help in understanding the pictures of PAD in legs. Furthermore, advanced treatment options like the clinical trial, evaluated within the PATHFINDER Registry, offer innovative solutions for effectively addressing complex cases of PAD, which can be illustrated through case studies, enhancing the overall management of PAD.
Remember, you’re not alone in this journey. Seeking help and staying informed can make a world of difference in your health.
Contrast Visual Features of PAD-Affected Legs and Healthy Legs
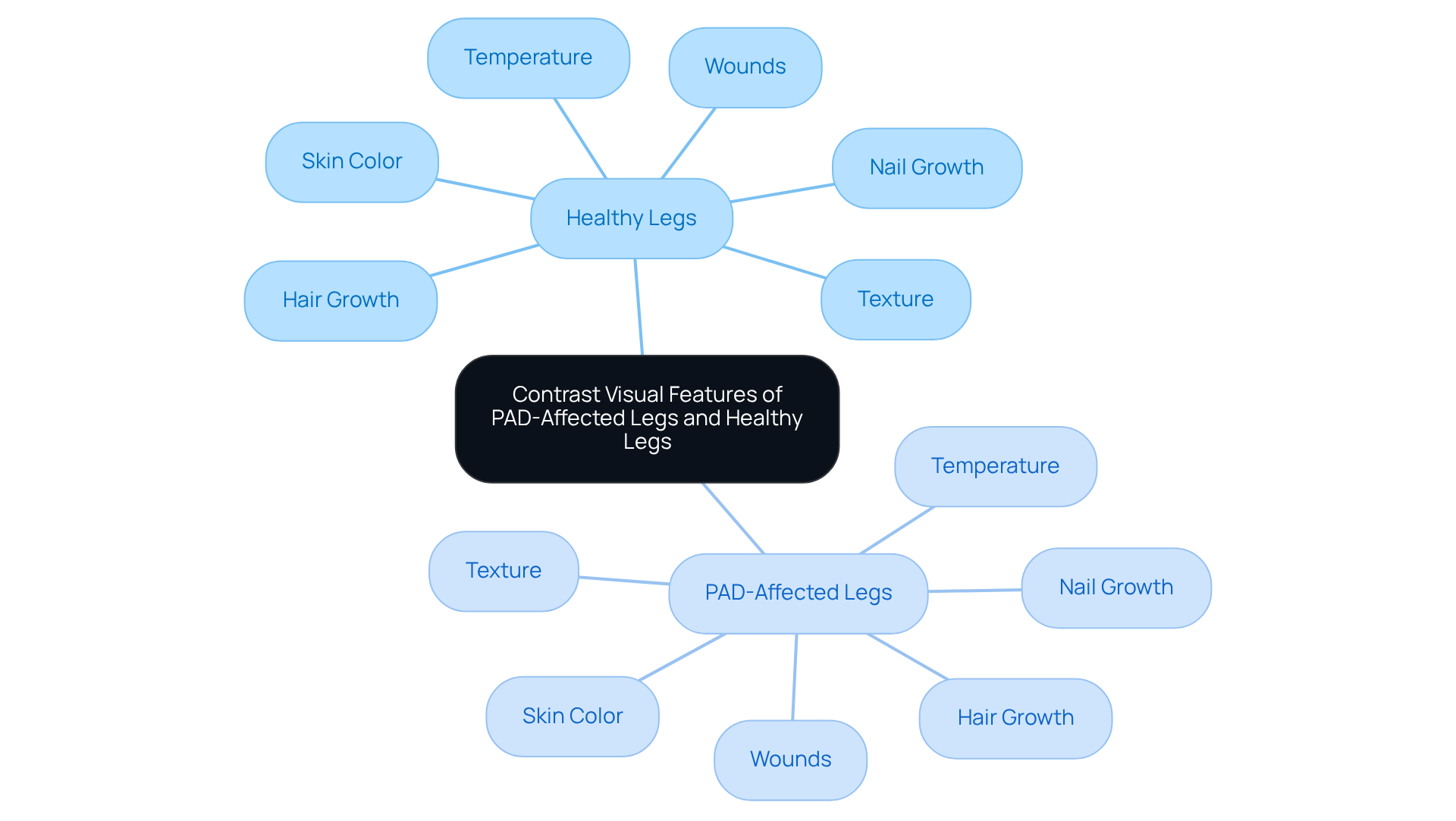
When comparing pictures of PAD-affected legs to healthy ones, several visual features stand out, especially for those at high risk who could greatly benefit from at Amavita.
- Skin Color: Healthy legs typically have a consistent, healthy tone, while PAD-affected legs may depict pale or bluish discoloration.
- Texture: Healthy skin is smooth and supple, whereas pictures of PAD-affected legs can show skin that appears shiny and smooth or dry and flaky.
- Hair Growth: Normal hair growth is common in healthy legs, but in PAD-affected legs, those affected often experience reduced or absent hair growth.
- Nail Growth: Pictures of PAD-affected legs may show that nail growth is slower and accompanied by signs of discoloration, while healthy nails grow regularly and maintain a healthy appearance.
- Temperature: Healthy legs feel warm to the touch, whereas PAD-affected legs often depict limbs that may feel cool or cold.
- Wounds: Wounds are absent in healthy legs, while pictures of PAD-affected legs may show open sores.
This contrast highlights the critical visual differences that can indicate the presence of peripheral artery disease, emphasizing the importance of early detection. At Amavita, our team ensures that these observable indicators are integrated into a comprehensive care plan, especially for patients with diabetes, hypertension, or a family history of heart disease.
Furthermore, the sophisticated imaging features at Amavita provide a thorough assessment for patients who may have ambiguous results from standard testing, ensuring that every aspect of cardiovascular well-being is taken into account.
If you or a loved one are experiencing any of these symptoms, don’t hesitate to reach out. Early intervention can make a significant difference in your health journey, and we’re here to support you every step of the way.
Discuss Health Implications of Visual Differences in PAD
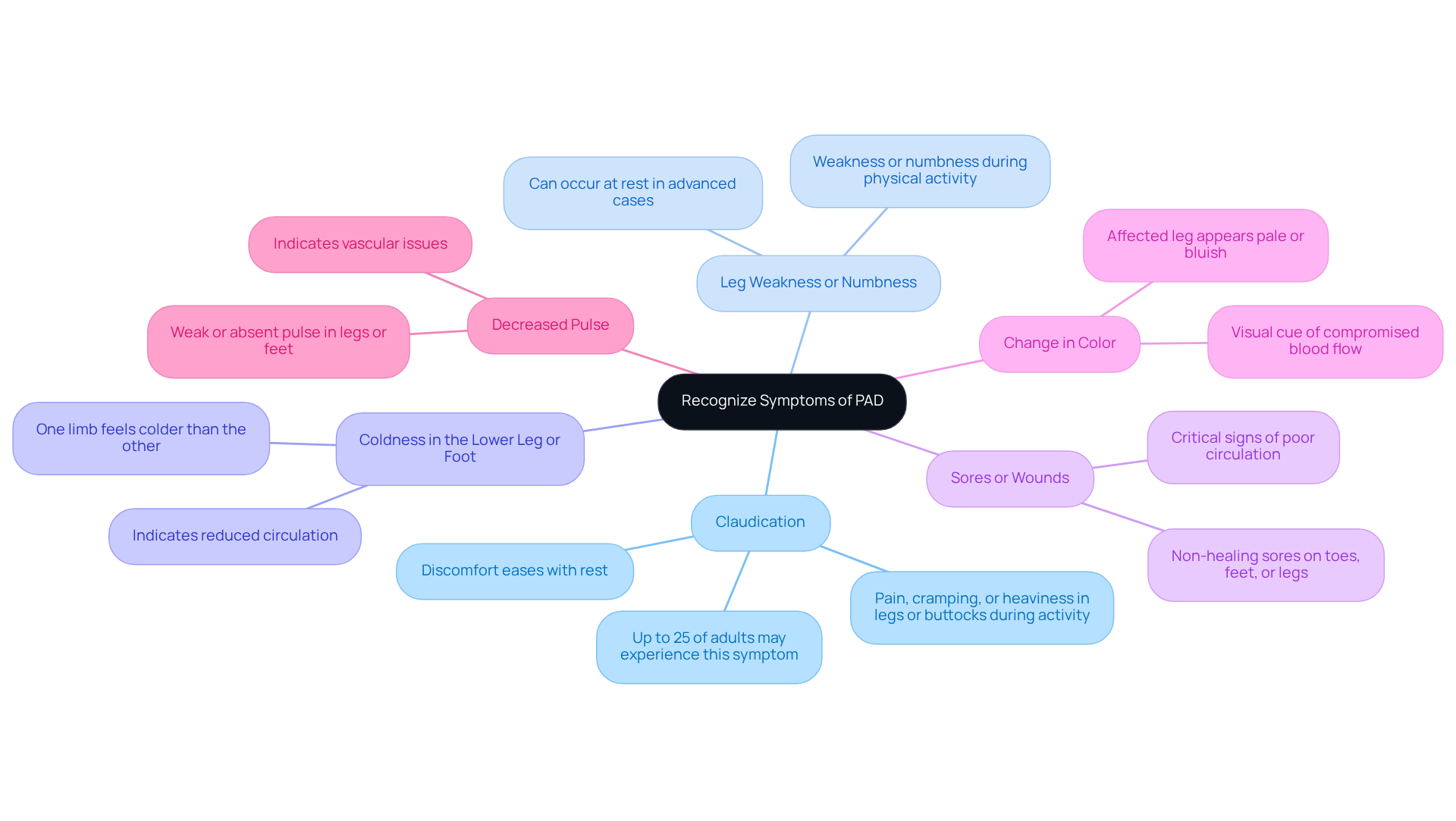
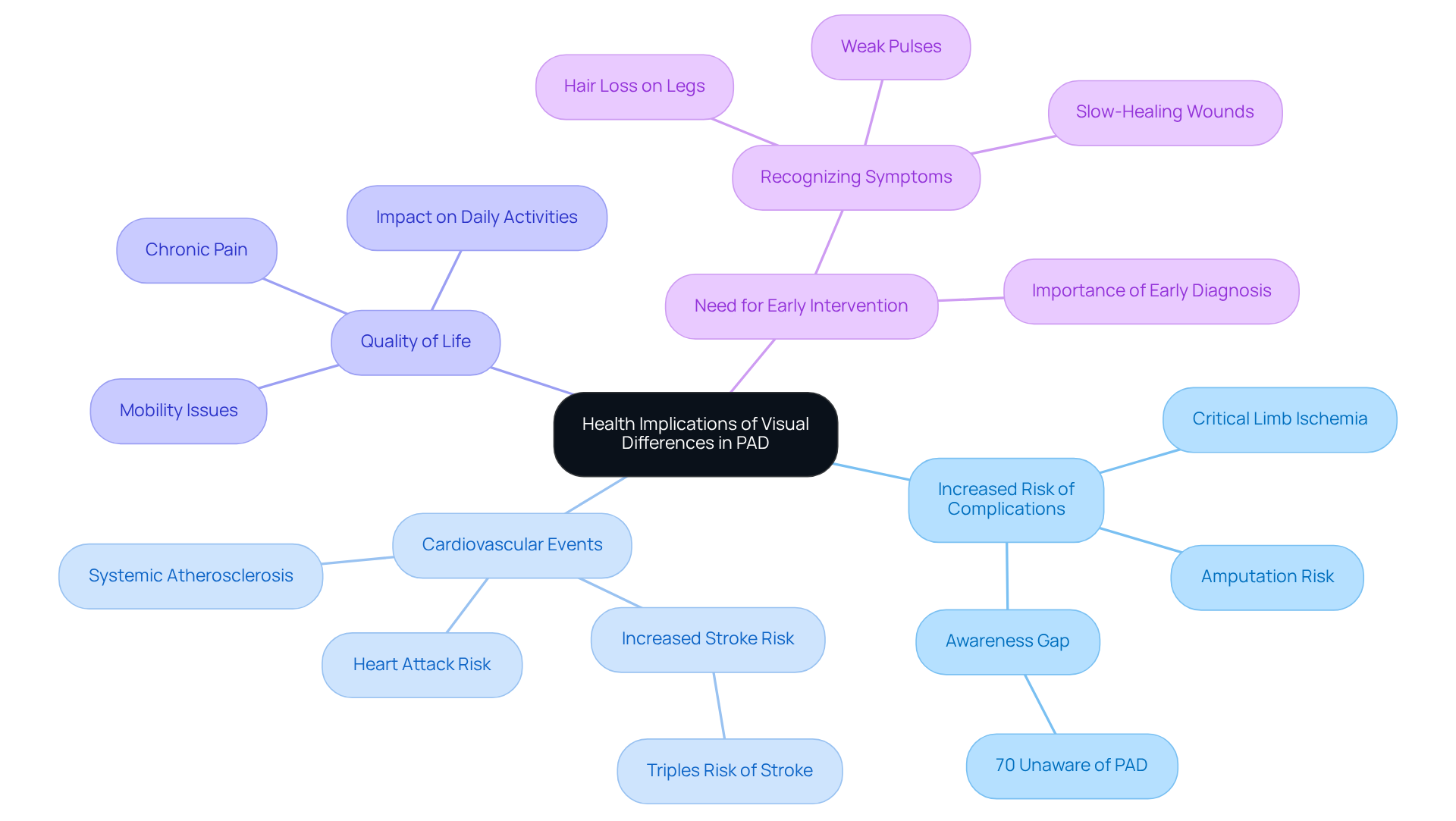
The visual indicators seen in legs affected by PAD carry important health implications that deserve your attention:
- Increased Risk of Complications: If you have PAD, it’s crucial to know that you face a higher risk of complications, including critical limb ischemia, which can lead to tissue death and even amputation. Shockingly, about 70 percent of those with PAD don’t even realize they have it, which only makes these risks worse.
- Cardiovascular Events: PAD is due to the systemic nature of atherosclerosis. If left untreated, PAD can triple your risk of stroke and significantly increase the likelihood of heart attacks and other cardiovascular diseases.
- Chronic Pain: Living with symptoms like pain, cramping, and mobility issues can really take a toll on your quality of life, making everyday activities feel daunting. As PAD progresses, chronic pain may develop, further affecting your overall well-being.
- Need for Early Intervention: It’s vital to recognize the signs of PAD, such as weak pulses, hair loss on the legs, and slow-healing wounds. Early diagnosis and treatment can make a world of difference, helping to prevent serious consequences like limb loss and improving your long-term health prospects.
Understanding these health implications underscores the importance of seeking help in legs as soon as possible. Please don’t hesitate to seek medical advice; you deserve support and care.
Conclusion
Recognizing the visual differences between healthy legs and those affected by Peripheral Artery Disease (PAD) is crucial for early diagnosis and intervention. By understanding key indicators – like changes in skin color, texture variations, and the presence of wounds – you can take important steps to care for your vascular health. These visual cues are vital; they help identify PAD and prevent serious complications.
This article highlights critical characteristics that set PAD-affected legs apart from healthy ones, emphasizing the importance of awareness. From skin discoloration and texture changes to variations in hair and nail growth, each visual feature offers insight into your circulatory health. Furthermore, the discussion on health implications underscores the urgent need for early intervention to reduce risks, including critical limb ischemia and increased cardiovascular events.
Ultimately, the message is clear: staying informed about the visual indicators of PAD can lead to timely medical intervention and a better quality of life. We encourage you to monitor your leg health closely and seek medical advice if you notice any concerning signs. By prioritizing awareness and education, you can navigate the challenges of PAD effectively and enhance your overall well-being.
Frequently Asked Questions
What is Peripheral Artery Disease (PAD)?
Peripheral Artery Disease (PAD) is a circulatory condition that occurs when narrowed arteries reduce blood flow to the extremities, particularly the legs, often due to atherosclerosis, where fatty deposits build up in the artery walls.
What are the visual indicators of PAD in the legs?
Key visual indicators of PAD in the legs include skin color changes (pale or bluish legs), texture changes (shiny, smooth skin), decreased hair growth on the lower limbs, slower toenail growth, and non-healing sores or ulcers.
Why is it important to recognize the signs of PAD?
Recognizing the signs of PAD is crucial for early diagnosis and intervention, which can greatly enhance health outcomes and reduce the risk of severe complications, such as amputations.
What percentage of amputations due to severe PAD are preventable with timely intervention?
85% of amputations due to severe PAD are preventable with timely intervention and appropriate care.
How many individuals with PAD are unaware of their condition?
Nearly 70% of individuals with PAD are unaware of their condition, highlighting the need for awareness and education.
What does the CardioElite™ system do?
The CardioElite™ system provides advanced bedside diagnostics for early detection of conditions like PAD, allowing for comprehensive cardiac assessments of high-risk patients.
What are the projections for PAD cases by 2050?
Projections indicate a staggering 220% increase in PAD cases by 2050, emphasizing the urgency of recognizing symptoms and proactive management.
What should you do if you or a loved one are experiencing symptoms of PAD?
If you or a loved one are experiencing symptoms of PAD, it is important to reach out for support and seek medical advice.
List of Sources
- Define Peripheral Artery Disease and Its Visual Indicators
- New Study Projects 360 Million Cases Of Peripheral Artery Disease By 2050, Driven By Metabolic Risk And Aging: Proactive Prevention Could Avert One In Three Cases – ALPS (https://limbpreservationsociety.org/news/new-study-projects-360-million-cases-of-peripheral-artery-disease-by-2050-driven-by-metabolic-risk-and-aging-proactive-prevention-could-avert-one-in-three-cases)
- Visual Guide: Peripheral Artery Disease Legs Pictures vs. Healthy Legs (https://amavita.health/blog/visual-guide-peripheral-artery-disease-legs-pictures-vs-healthy-legs)
- evtoday.com (https://evtoday.com/news/large-primary-care-study-outlines-pad-burden-and-incidence-in-united-states)
- Peripheral Artery Disease Gains National Attention: What New Federal Actions Mean for Patients – American Vascular Associates (https://americanvascular.com/peripheral-artery-disease-national-priority-amputation-prevention)
- New study finds Peripheral Artery Disease often underdiagnosed and undertreated (https://abc4.com/community/intermountainhealthcare/new-study-finds-peripheral-artery-disease-often-underdiagnosed-and-undertreated)
- Identify Characteristics of Healthy Legs
- New Year, Healthier Veins: Making Circulation a Priority in 2026: Texas Heart and Vein Multispecialty Group: Cardiovascular Doctors (https://thvmg.com/blog/new-year-healthier-veins-making-circulation-a-priority-in-2026)
- Your 2026 Vein Health Checklist | United Vein & Vascular Centers® (https://unitedveincenters.com/blog/your-2026-vein-health-checklist)
- Setting Achievable Vein Health Resolutions for 2026 | Metro Vein Centers (https://metroveincenters.com/blog/vein-health-resolutions-2026)
- Cardiologist Reveals the ‘Best Habit of All’ to Commit to in 2026 (https://today.com/health/diet-fitness/heart-health-resolution-cardiologist-tip-rcna251494)
- Discuss Health Implications of Visual Differences in PAD
- Study finds high rates of undiagnosed and untreated peripheral artery disease (https://news-medical.net/news/20250331/Study-finds-high-rates-of-undiagnosed-and-untreated-peripheral-artery-disease.aspx)
- Peripheral Artery Disease Gains National Attention: What New Federal Actions Mean for Patients – American Vascular Associates (https://americanvascular.com/peripheral-artery-disease-national-priority-amputation-prevention)
- 5 Major Health Complications Caused by Untreated Peripheral Artery Disease (https://advancedvcv.com/post/5-major-health-complications-caused-by-untreated-peripheral-artery-disease)
- Peripheral Artery Disease (PAD) Awareness Month Urges Screening and Advocacy in National Effort to Prevent Amputations | SCAI (https://scai.org/media-center/news-and-articles/peripheral-artery-disease-pad-awareness-month-urges-screening-and)
- Peripheral Artery Disease: The Symptoms Physicians Wish You Wouldn’t Ignore (https://baptisthealth.net/baptist-health-news/peripheral-artery-disease-the-symptoms-physicians-wish-you-wouldnt-ignore)