Introduction
Imagine living with a heart condition that often goes unnoticed, quietly complicating your life without you even knowing it. As more seniors are diagnosed with Hypertrophic Cardiomyopathy (HCM), understanding how genetic testing can help is more important than ever. This condition can masquerade as other heart issues, leaving many unaware of its presence. By exploring the role of genetic testing, seniors and their families can make informed health decisions that truly matter.
What if you could navigate the testing process with confidence? How can being aware of HCM change your approach to heart health?
Define Hypertrophic Cardiomyopathy (HCM) and Its Implications
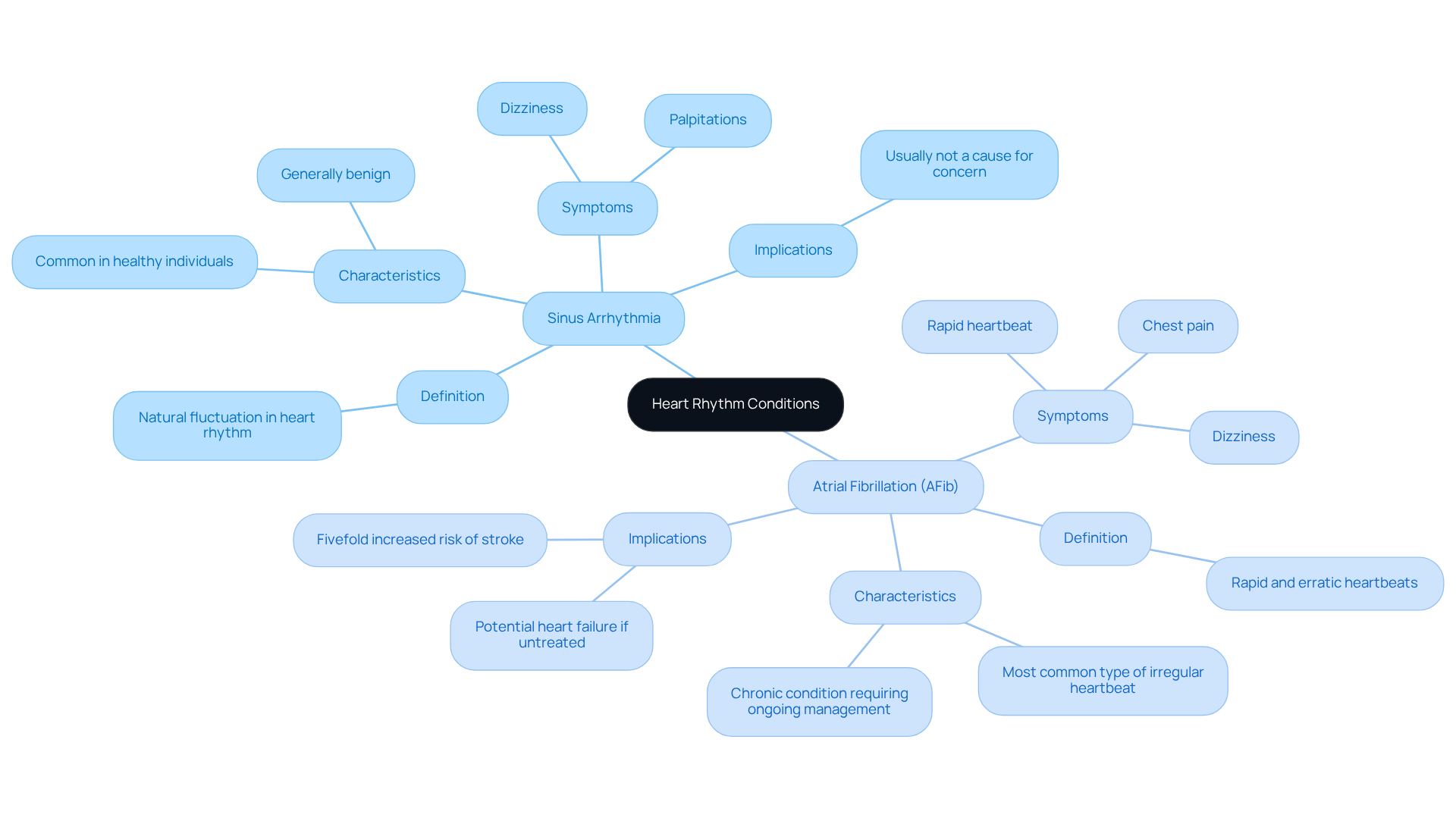
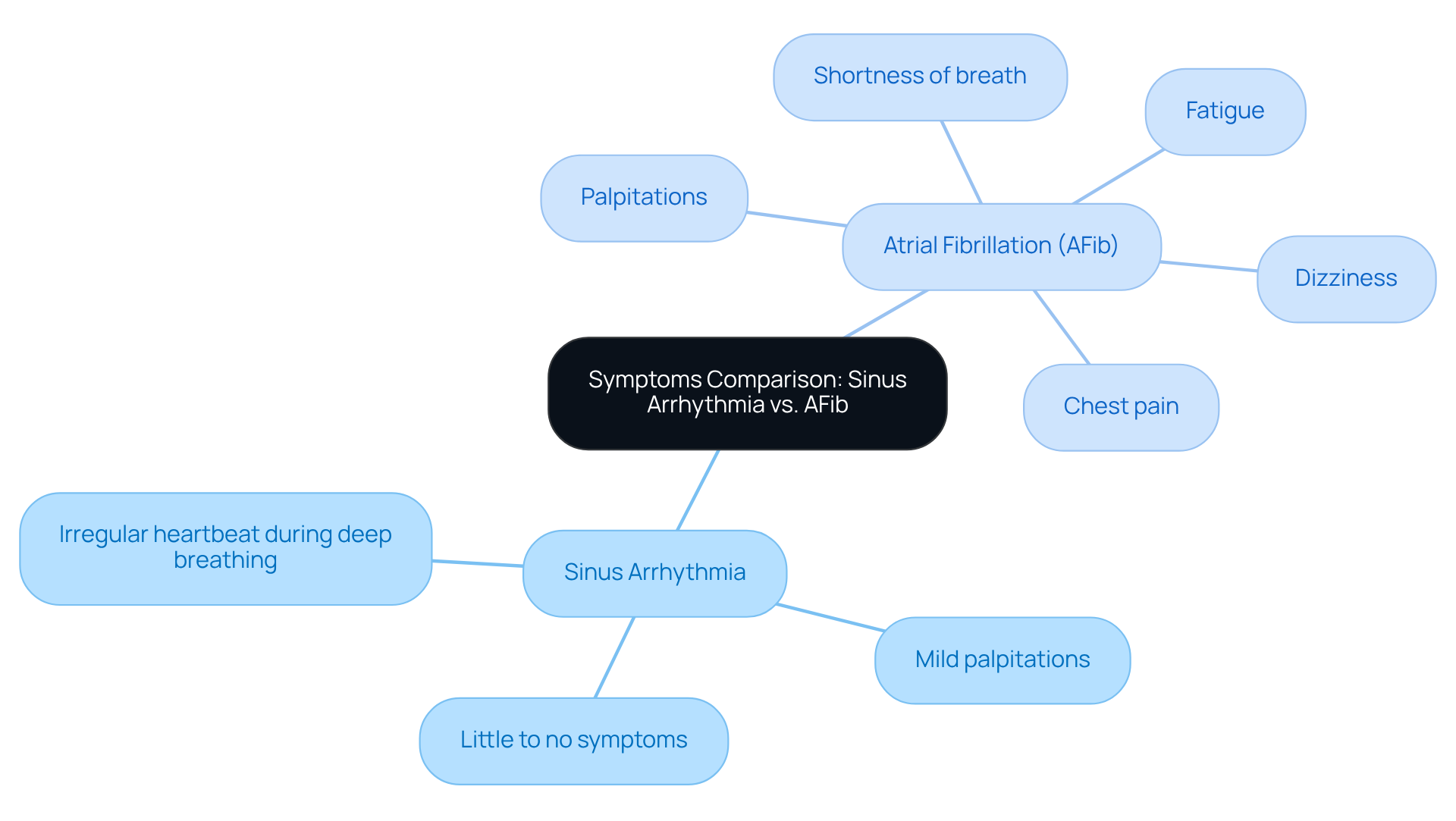
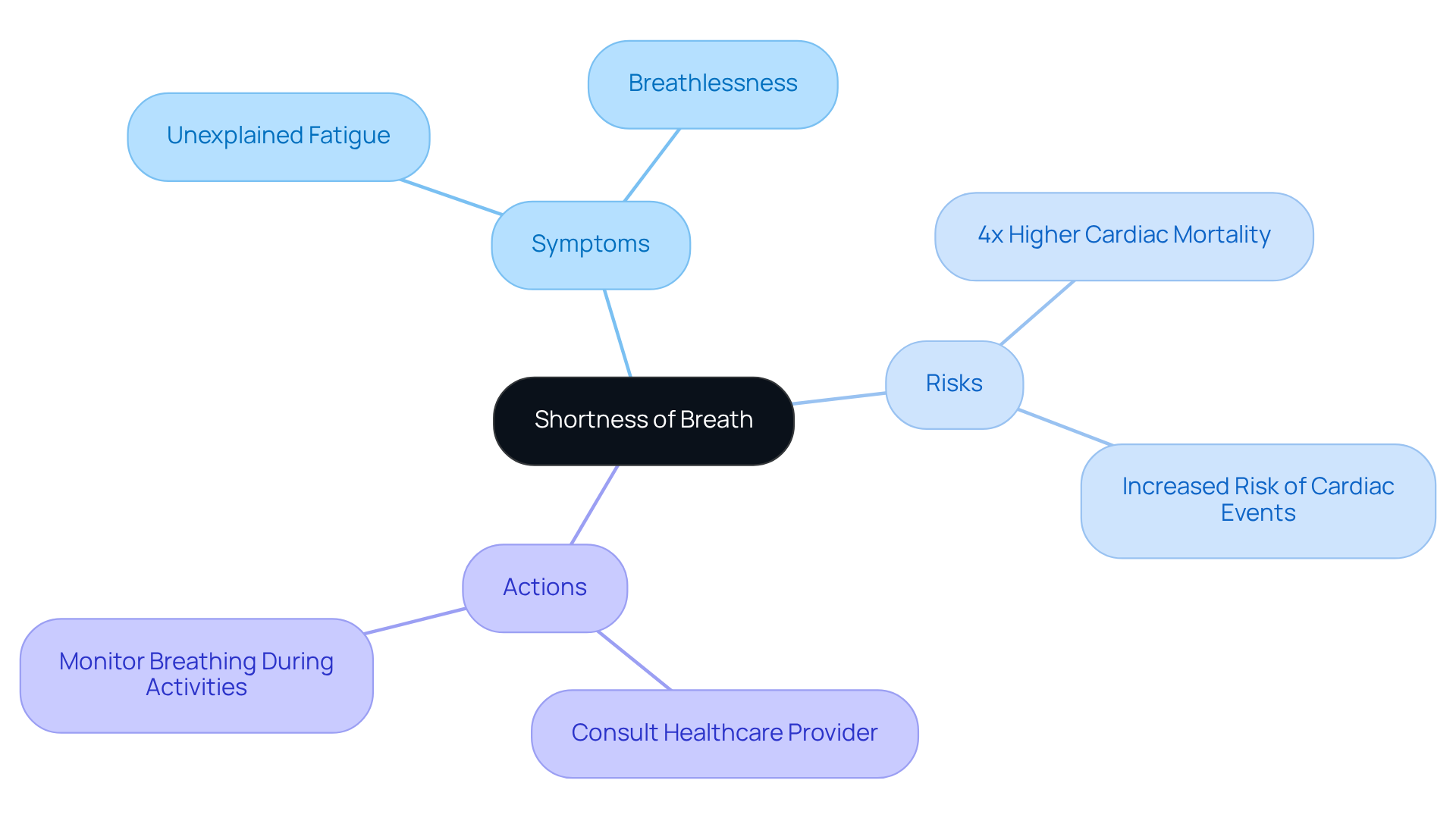
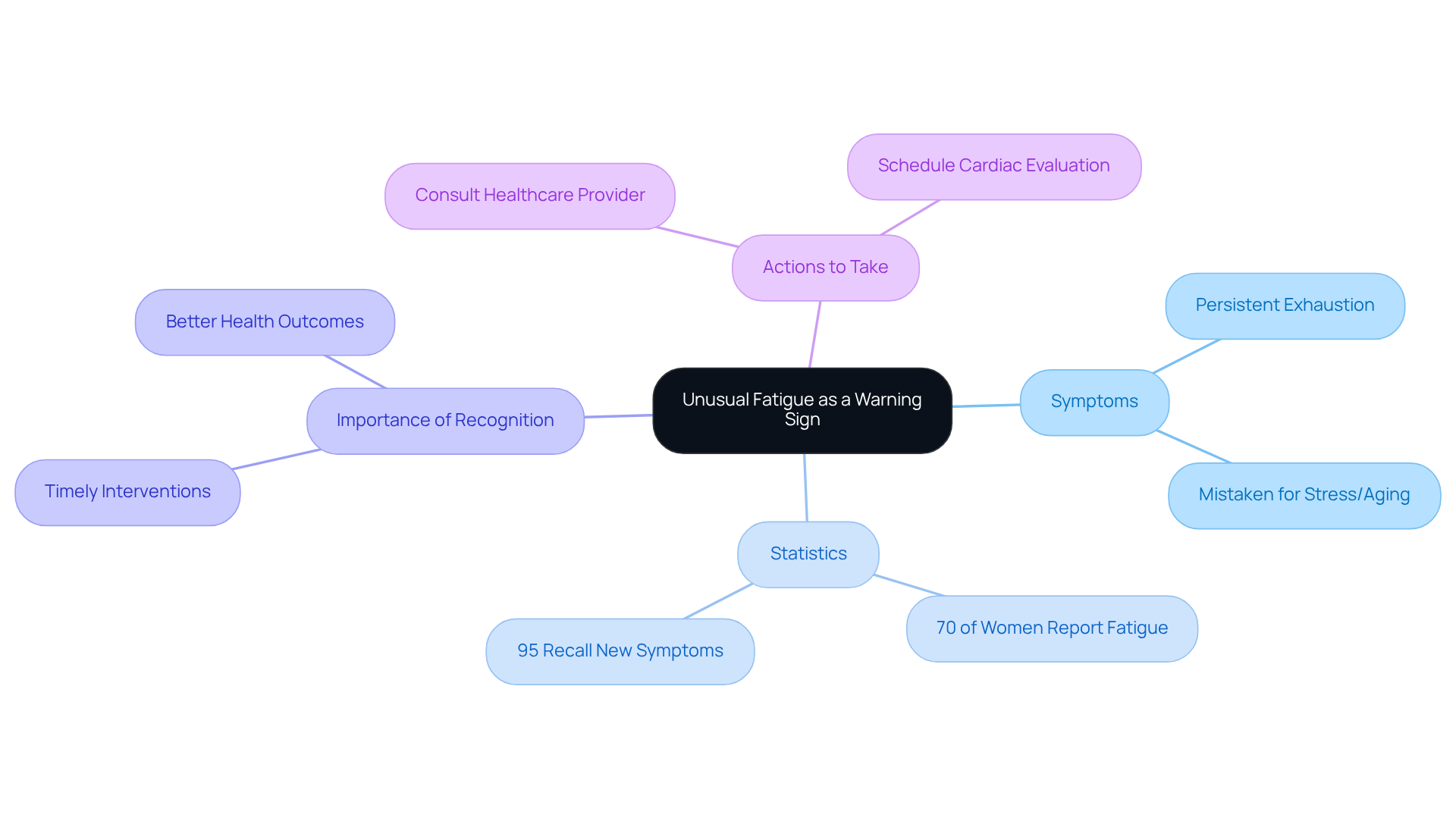
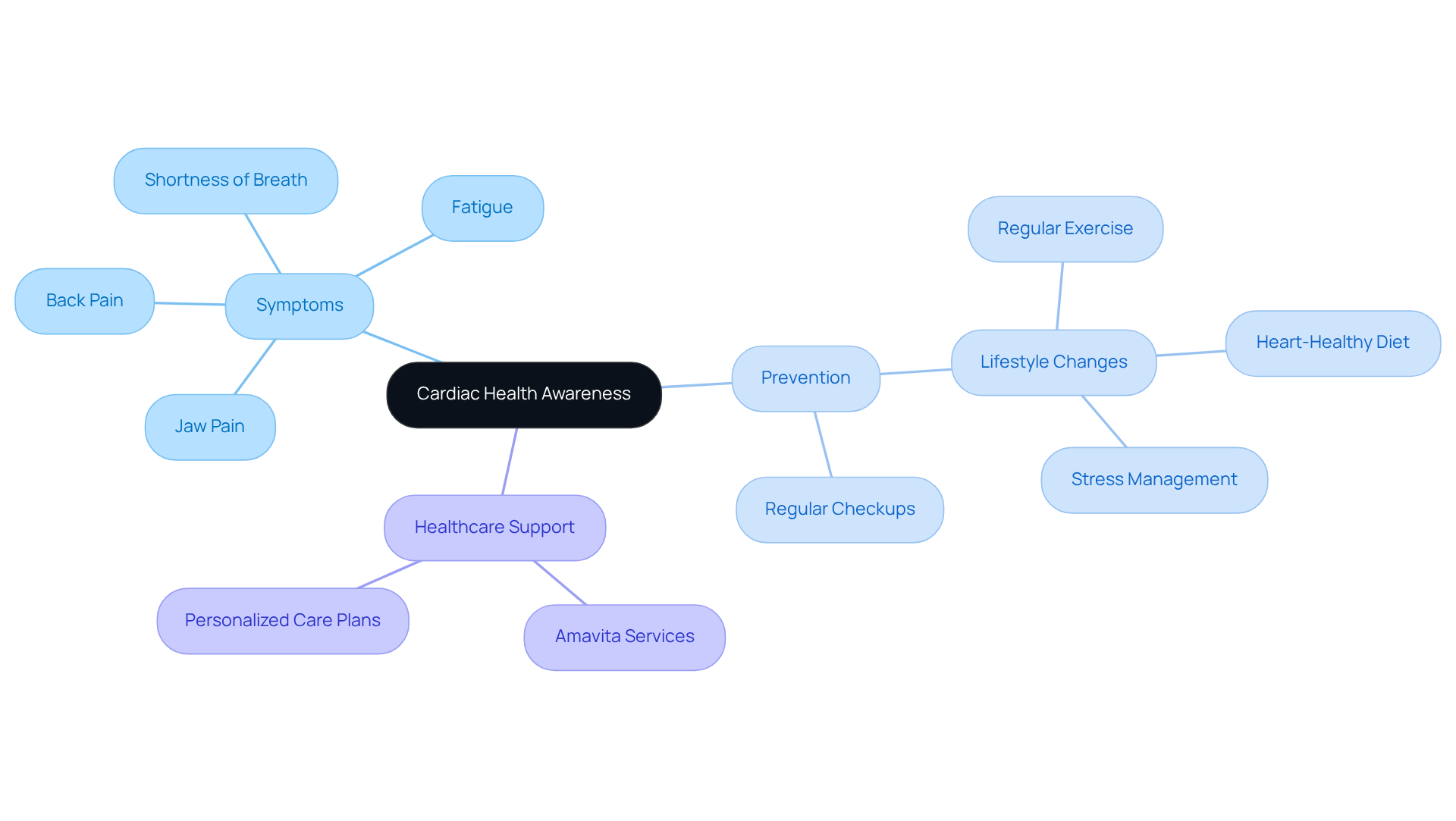
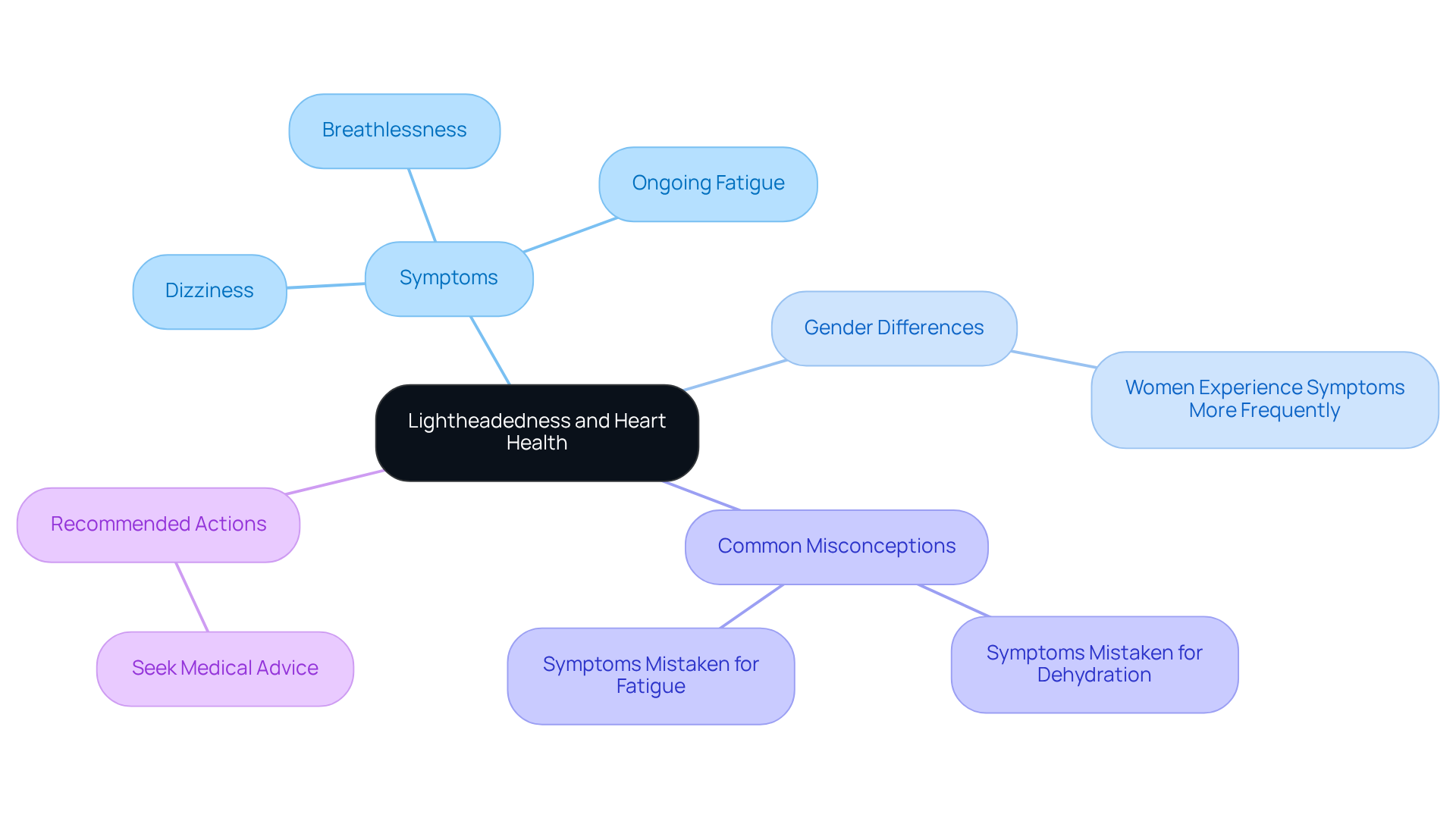
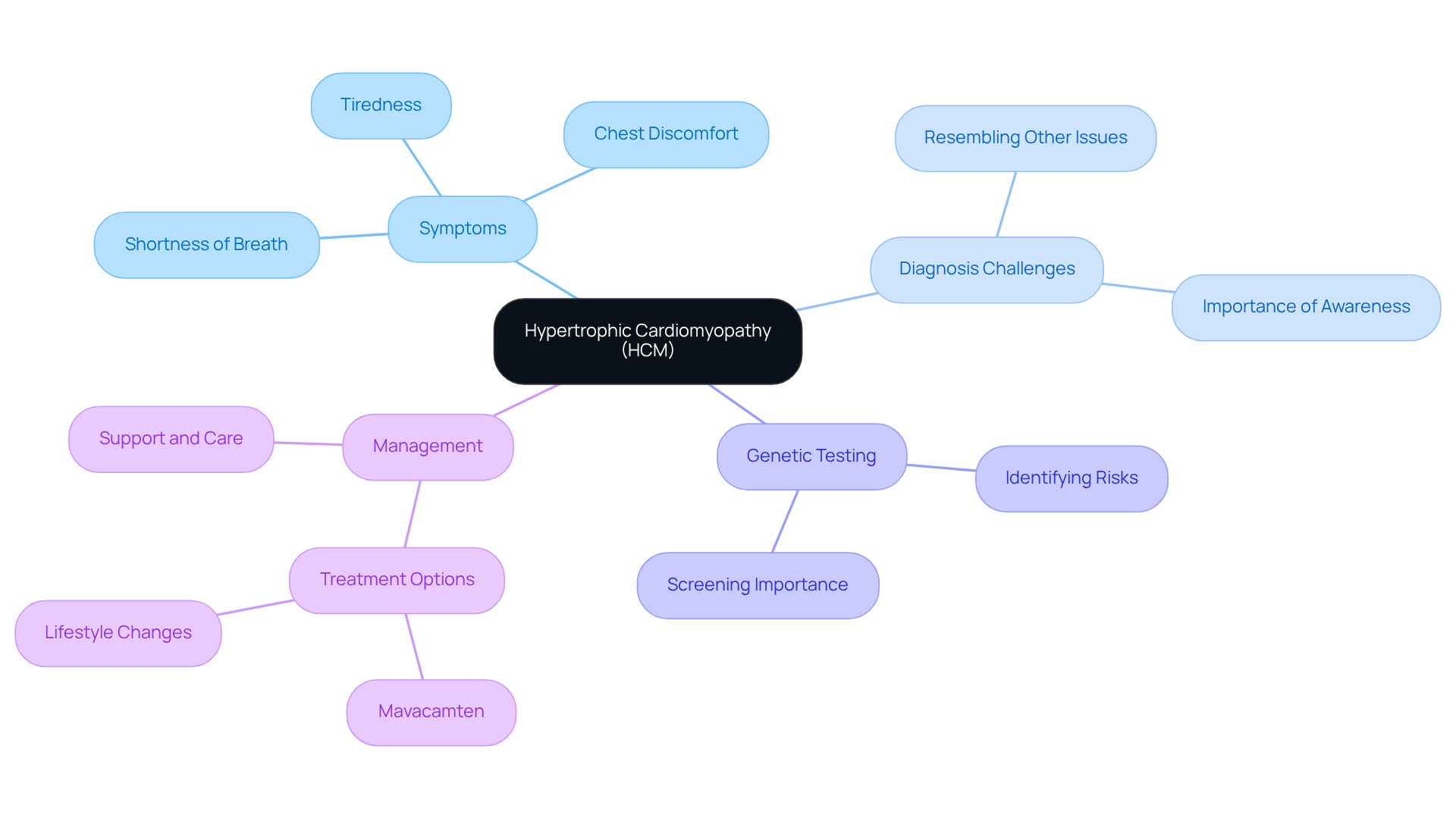
Have you ever felt unusually tired or experienced unexpected chest discomfort? These could be signs of a condition called Hypertrophic Cardiomyopathy (HCM), highlighting the importance of hypertrophic cardiomyopathy genetic testing for many seniors today. HCM can make it harder for your heart to pump blood, which might leave you feeling short of breath or experiencing discomfort in your chest. It’s important to listen to your body and seek help if you notice these signs.
For older adults, HCM can show up in unexpected ways, sometimes resembling other heart issues. This can make it tricky to diagnose, but understanding these differences is key to getting the right care. Recent studies show that HCM is becoming more common, with a significant rise in cases over the past decade. This highlights the importance of awareness and screening, especially for seniors who may have other health concerns.
It’s important to be aware that hypertrophic cardiomyopathy genetic testing can help identify risks for serious complications, but with the right support and management, many people can live fulfilling lives. By understanding HCM and its implications, we can work together to ensure you receive the compassionate care you deserve.
Explore the Role of Genetic Testing in HCM
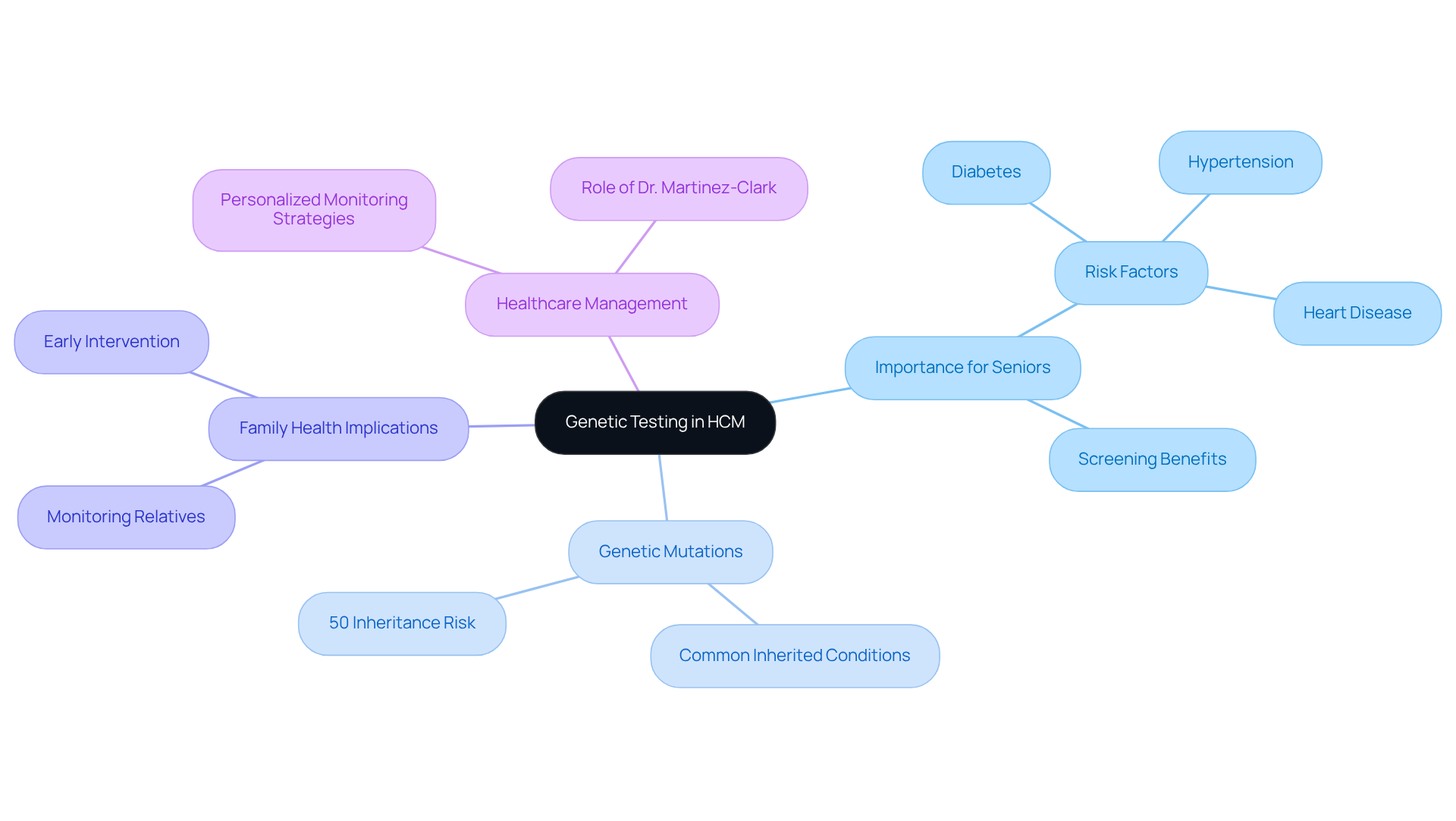
Many seniors worry about their heart health and the potential risks they face. Hypertrophic cardiomyopathy genetic testing is essential for diagnosing Hypertrophic Cardiomyopathy (HCM). It helps identify mutations in genes linked to this condition. For seniors, especially those at higher risk due to diabetes, hypertension, or a history of heart disease, understanding whether their condition is hereditary through hypertrophic cardiomyopathy genetic testing is crucial. This knowledge not only aids in screening but also helps manage the health of their relatives when hypertrophic cardiomyopathy genetic testing is utilized. Hypertrophic cardiomyopathy genetic testing indicates that HCM is the most common inherited heart condition, with a 50% chance of passing it on to biological children. This highlights the importance of screening for older adults with a history of the condition.
Hypertrophic cardiomyopathy genetic testing also aids in distinguishing HCM from other disorders that present similar symptoms. This ensures patients receive the best treatment possible. By understanding their genetic predispositions, families can monitor relatives who might be at risk, allowing for early intervention and management strategies. Results from DNA analysis are typically available within three months, providing timely information for patients and their families.
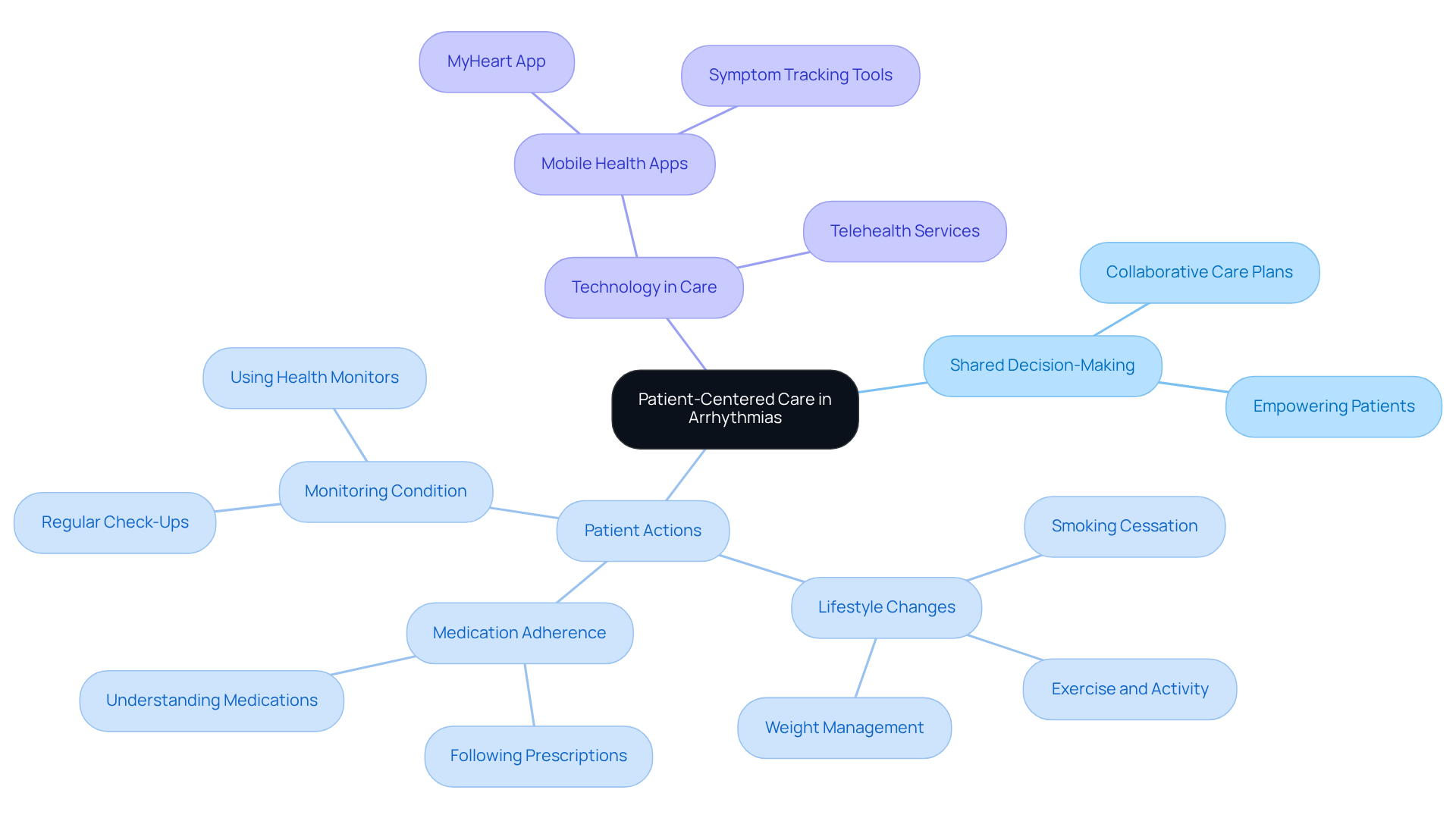
At Amavita Heart & Vascular Health, Dr. Martinez-Clark combines his Harvard training with years of experience to meet the unique needs of seniors. Real-life examples show that older adults who undergo DNA analysis benefit from personalized monitoring strategies, which may include regular echocardiograms to assess heart health. This proactive approach not only enhances individual patient care but also supports family health decisions. Understanding genetic risks empowers seniors to make informed health choices for themselves and their families.
Guide to Undergoing Genetic Testing for HCM
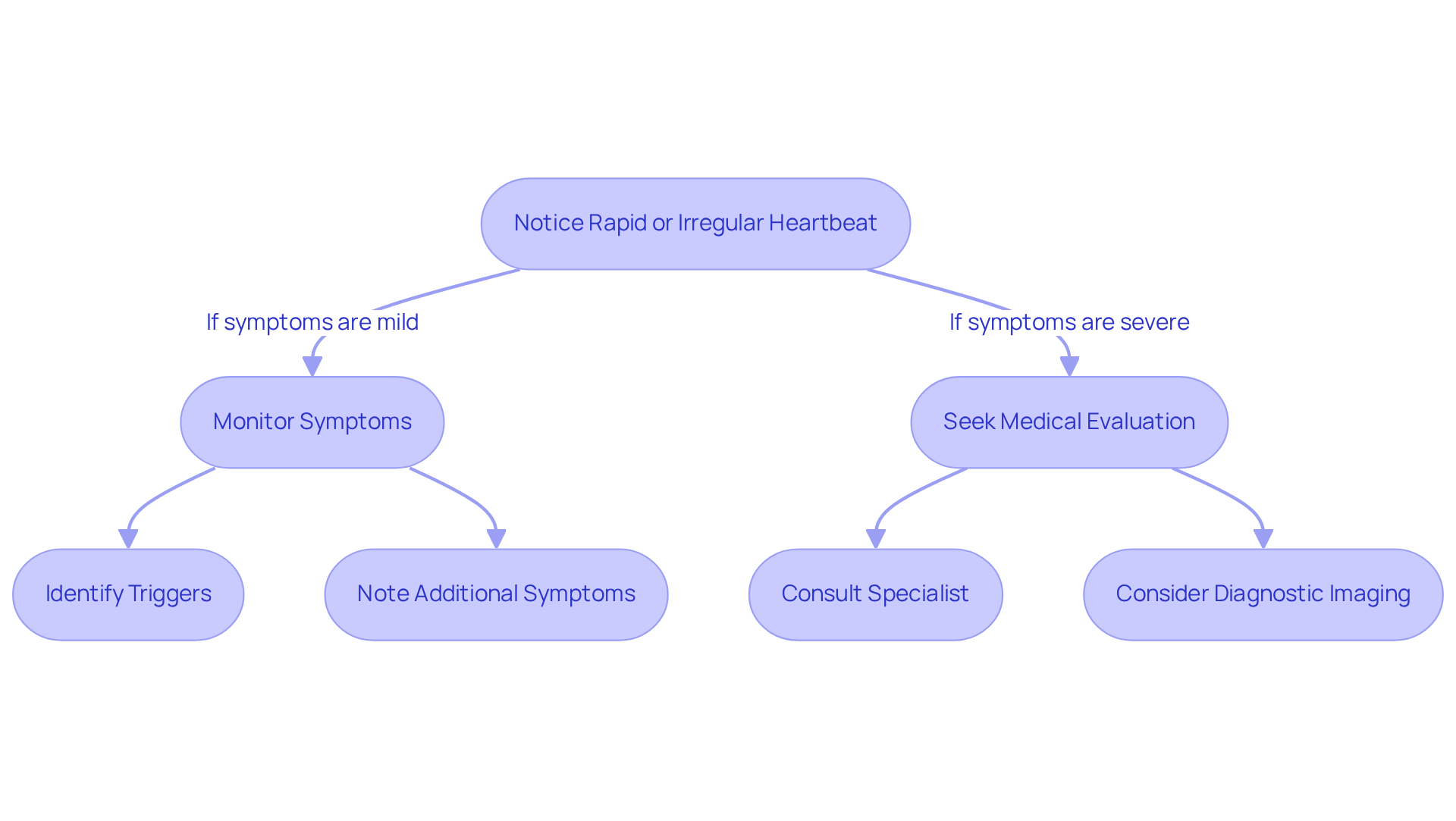
Navigating the journey of genetic testing for Hypertrophic Cardiomyopathy (HCM) can feel daunting, but understanding the steps involved can provide clarity and reassurance.
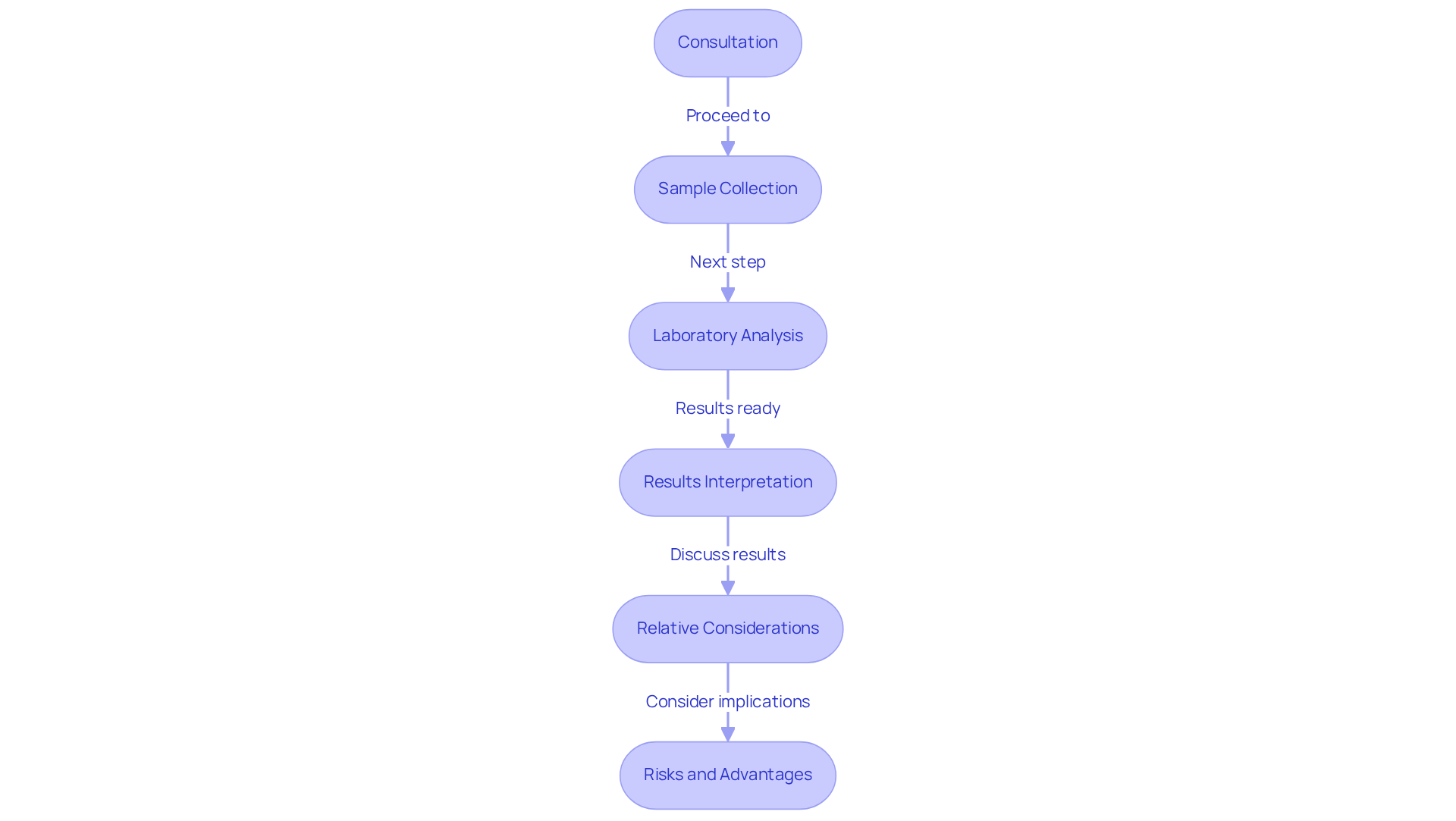
- Consultation: Your journey starts with a heartfelt consultation with a cardiologist or hereditary advisor who truly understands HCM. They will take the time to examine your medical history and family background, ensuring that the examination is suitable for you. This professional guidance is essential, as DNA testing is a valuable tool for diagnosing HCM and screening at-risk individuals.
- Sample Collection: A simple blood or saliva sample is collected, which is minimally invasive and typically takes only a few minutes. This step is quick and straightforward, allowing you to focus on what matters most-your health.
- Laboratory Analysis: The sample is sent to a laboratory for analysis, where it is examined for genetic mutations associated with HCM. Understanding these mutations can provide critical information for diagnosis and treatment options.
- Results Interpretation: After the analysis, a follow-up appointment is necessary to discuss the results. It’s completely normal to feel overwhelmed when you receive these results, as they can carry significant weight for you and your family. Knowing whether a mutation is present can help shape your treatment options and guide screening for your family.
- Relative Considerations: If a mutation is identified, relatives may be encouraged to undergo evaluation to assess their risk. First-degree relatives of individuals with HCM should think about screening if the relative has had a positive DNA examination. This proactive approach can help manage HCM effectively within families, ensuring that at-risk individuals receive appropriate care and monitoring.
- Risks and Advantages: Before moving forward with DNA analysis, it is crucial to consider the possible risks and advantages. Consulting with a doctor or hereditary advisor can provide insights into these aspects, helping you make informed decisions.
As Dr. Uzochukwu Ibe highlights, “It is important to collaborate with your physician, a hereditary advisor, or both to comprehend the evaluation process.”
Finally, remember, the insights gained from DNA analysis can empower you and your family to take proactive steps towards better health. Outcomes from DNA analysis are usually accessible within weeks, offering essential information for diagnosis and risk evaluation.
Understand the Implications of Genetic Testing Results
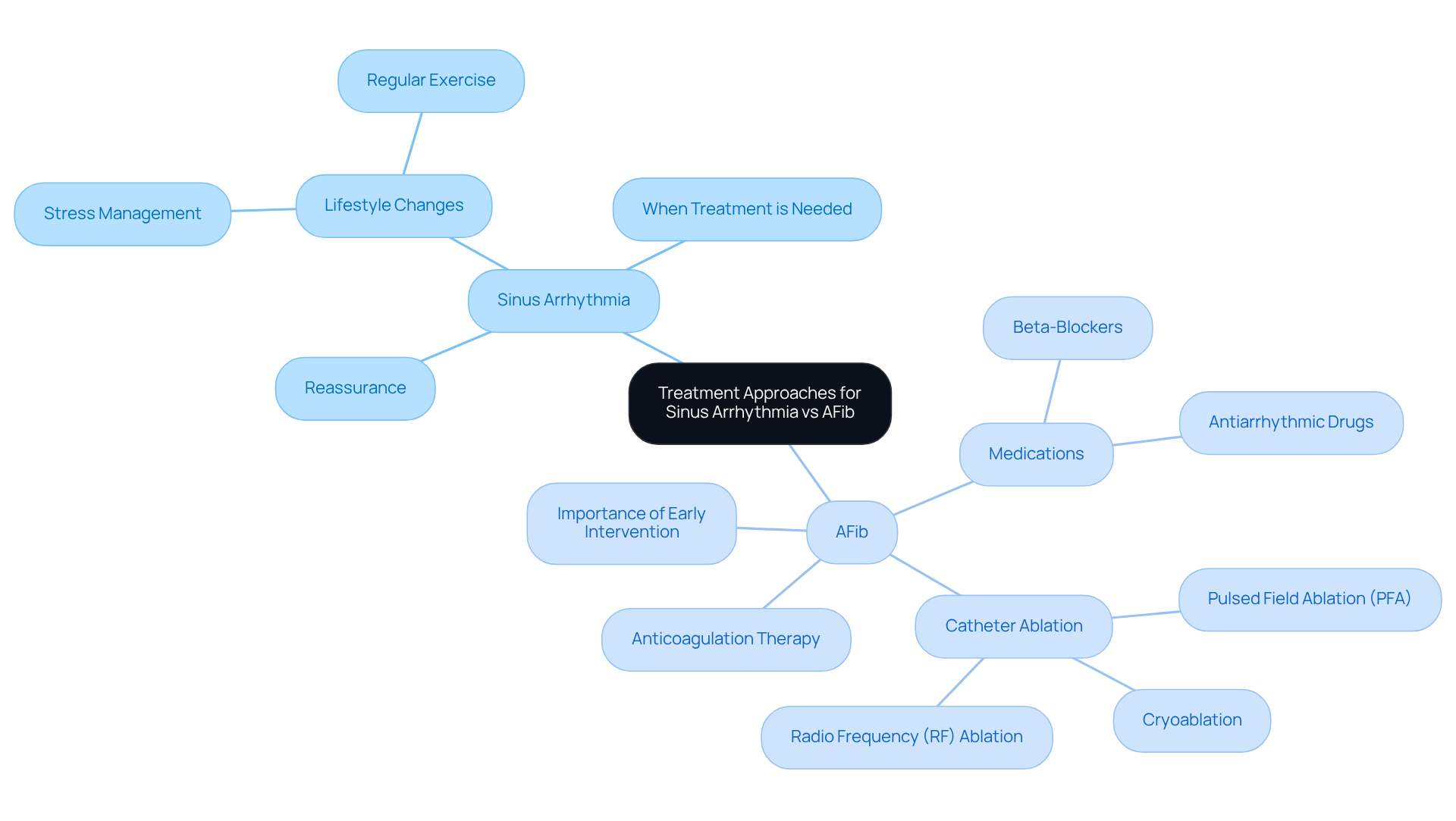
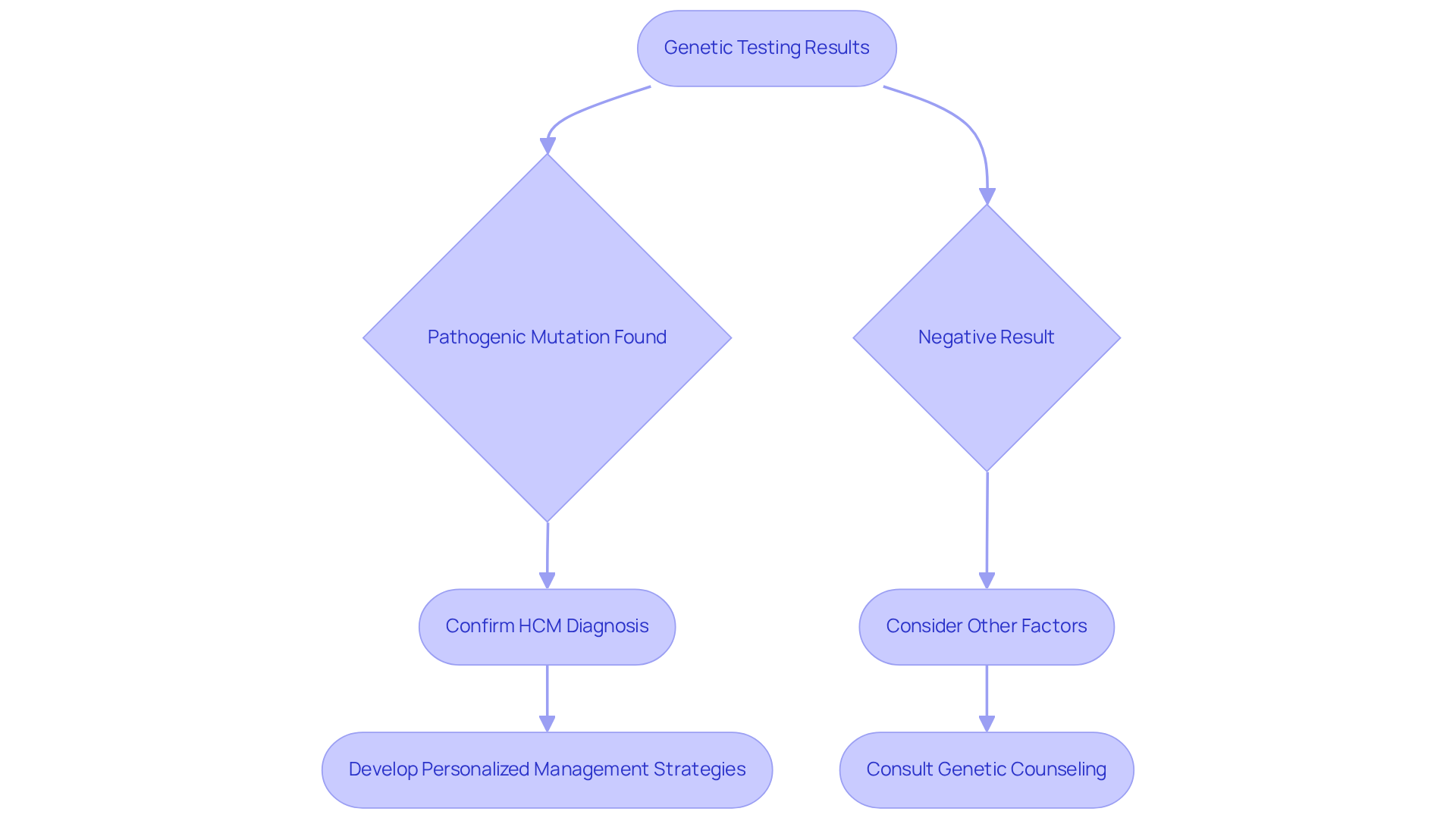
Understanding the results of hypertrophic cardiomyopathy genetic testing can feel overwhelming, but it’s a crucial step in caring for your health and that of your loved ones. If a pathogenic mutation is found, it confirms the HCM diagnosis. This allows for personalized management strategies that can include lifestyle changes and targeted medical care. But if the hereditary test result is negative, it doesn’t mean HCM is ruled out. It might just mean that the specific mutation hasn’t been found or that other factors are at play. It’s important to understand this, as it helps you make informed choices about your treatment and monitoring.
Good news from hypertrophic cardiomyopathy genetic testing can encourage family members to consider undergoing testing as well, which is vital for early detection and management of HCM. We recommend seeking genetic counseling, particularly for hypertrophic cardiomyopathy genetic testing, to help you and your family understand these results and what they mean for your health and lifestyle. With the right support and guidance, you can navigate these results and make informed choices for a healthier future.
Conclusion
Navigating the complexities of Hypertrophic Cardiomyopathy (HCM) can feel overwhelming, especially for seniors concerned about their heart health. Understanding HCM is vital, as it can lead to serious complications that may cause worry; being aware and taking proactive steps can make a significant difference. By recognizing symptoms and seeking genetic testing, older adults can better manage their health and understand the hereditary nature of HCM.
The importance of genetic testing in diagnosing HCM cannot be overstated, particularly for seniors at higher risk due to factors like diabetes or a family history of heart disease. Genetic testing can help you discover specific mutations related to HCM, which means your healthcare team can create a personalized monitoring and treatment plan just for you. Moreover, understanding genetic risks enables families to take preventive actions, ensuring that at-risk relatives receive timely evaluations.
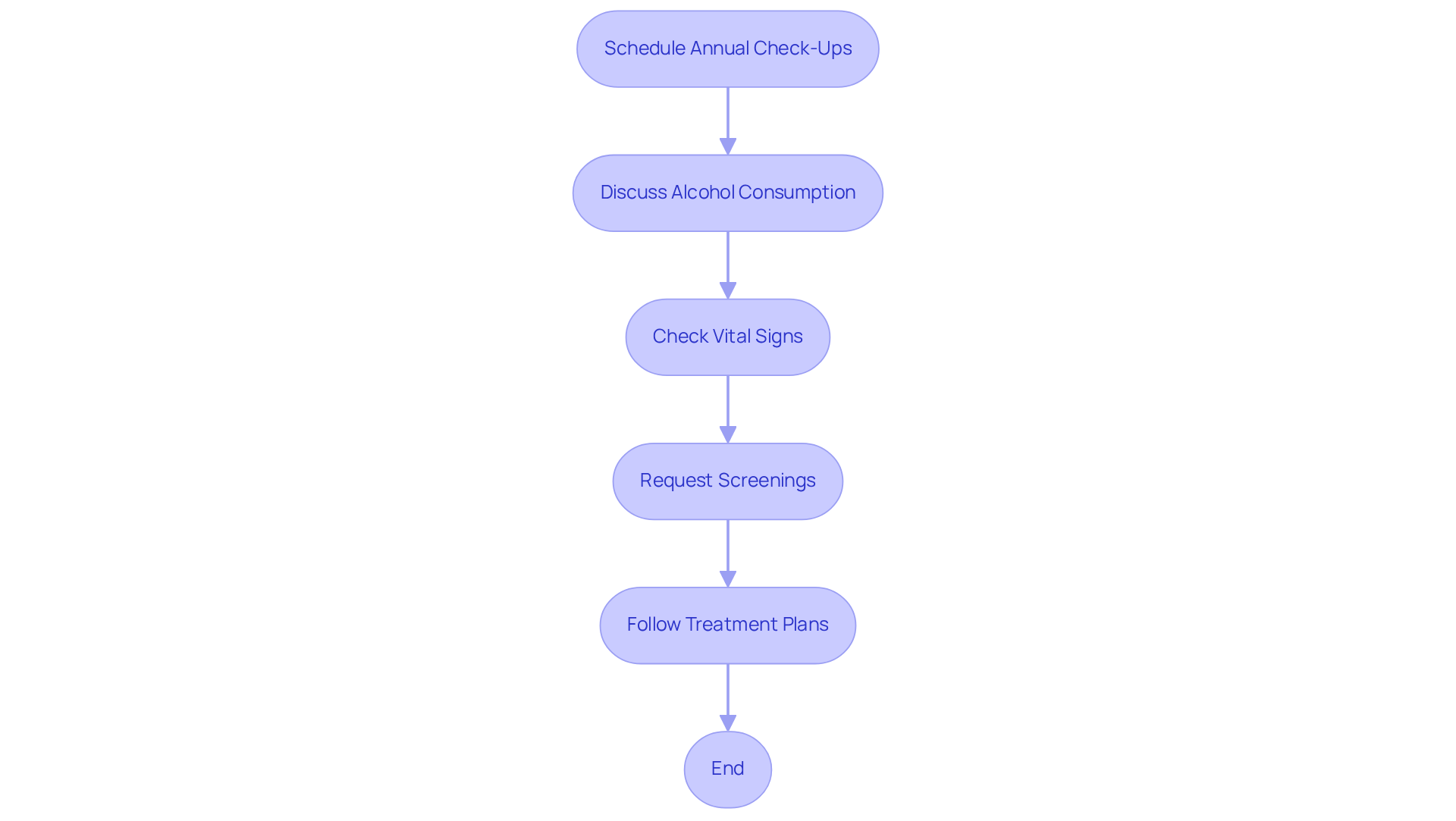
Ultimately, the significance of genetic testing for HCM extends beyond individual health; it fosters a proactive approach to heart care within families. Seniors are encouraged to engage in discussions with healthcare professionals about genetic testing and its implications. By taking these steps, you not only safeguard your health but also create a supportive environment for your loved ones, ensuring they too can thrive.
Frequently Asked Questions
What is Hypertrophic Cardiomyopathy (HCM)?
Hypertrophic Cardiomyopathy (HCM) is a condition that makes it harder for the heart to pump blood, potentially leading to symptoms such as shortness of breath and chest discomfort.
What are the symptoms of HCM?
Symptoms of HCM may include unusual tiredness, unexpected chest discomfort, and shortness of breath.
Why is HCM difficult to diagnose in older adults?
In older adults, HCM can present in unexpected ways that may resemble other heart issues, making it challenging to diagnose accurately.
How has the prevalence of HCM changed in recent years?
Recent studies indicate that HCM is becoming more common, with a significant rise in cases over the past decade.
Why is genetic testing important for HCM?
Hypertrophic cardiomyopathy genetic testing can help identify risks for serious complications associated with the condition, which is particularly important for seniors.
Can people with HCM live fulfilling lives?
Yes, with the right support and management, many people with HCM can lead fulfilling lives despite the condition.
List of Sources
- Define Hypertrophic Cardiomyopathy (HCM) and Its Implications
- Prevalence, incidence and mortality of hypertrophic cardiomyopathy based on a population cohort of 21.9 million in China – Scientific Reports (https://nature.com/articles/s41598-022-20042-9)
- Global trial shows targeted heart drug reduces obstructive hypertrophic cardiomyopathy in youth (https://medicalxpress.com/news/2026-03-global-trial-heart-drug-obstructive.html)
- Demographic and Regional Trends of Hypertrophic Cardiomyopathy-Related Mortality in the United States, 1999 to 2019 | Circulation: Heart Failure (https://ahajournals.org/doi/10.1161/CIRCHEARTFAILURE.121.009292)
- Bristol Myers Squibb Presents Positive Results from Phase 3 SCOUT-HCM Trial Demonstrating Efficacy and Safety of Camzyos (mavacamten) in Adolescents with Symptomatic Obstructive Hypertrophic Cardiomyopathy (oHCM) (https://news.bms.com/news/corporate-financial/2026/Bristol-Myers-Squibb-Presents-Positive-Results-from-Phase-3-SCOUT-HCM-Trial-Demonstrating-Efficacy-and-Safety-of-Camzyos-mavacamten-in-Adolescents-with-Symptomatic-Obstructive-Hypertrophic-Cardiomyopathy-oHCM/default.aspx)
- Prevalence, Patient Characteristics, and Treatment of Patients with Hypertrophic Cardiomyopathy: A Nationwide Payer Database Study – Cardiology and Therapy (https://link.springer.com/article/10.1007/s40119-024-00396-z)
- Explore the Role of Genetic Testing in HCM
- What to know about genetic testing for hypertrophic cardiomyopathy (https://medicalnewstoday.com/articles/genetic-testing-for-hypertrophic-cardiomyopathy)
- Genetic Testing for Hypertrophic Cardiomyopathy (https://heart.org/en/health-topics/cardiomyopathy/understand-your-risk-for-cardiomyopathy/genetic-testing-for-hcm)
- Gene Therapy for HCM Demonstrates Safety and Early Efficacy (https://consultqd.clevelandclinic.org/gene-therapy-for-hcm-demonstrates-safety-and-early-efficacy)
- Guide to Undergoing Genetic Testing for HCM
- What to Know About Genetic Testing for Hypertrophic Cardiomyopathy (https://resources.healthgrades.com/right-care/heart-health/what-to-know-about-genetic-testing-for-hypertrophic-cardiomyopathy)
- Hypertrophic cardiomyopathy genetic test reports: A qualitative study of patient understanding of uninformative genetic test results – PubMed (https://pubmed.ncbi.nlm.nih.gov/31408576)
- Genetic Testing for Hypertrophic Cardiomyopathy (https://heart.org/en/health-topics/cardiomyopathy/understand-your-risk-for-cardiomyopathy/genetic-testing-for-hcm)
- Understand the Implications of Genetic Testing Results
- Genetic Testing for Hypertrophic Cardiomyopathy (https://heart.org/en/health-topics/cardiomyopathy/understand-your-risk-for-cardiomyopathy/genetic-testing-for-hcm)
- The First Precision Medicine for a Genetic Heart Disease (https://hms.harvard.edu/news/first-precision-medicine-genetic-heart-disease)
- Genetic Testing (https://4hcm.org/diagnostic-tools/genetic-testing-an-overview)