Introduction
Recognizing the signs of stable angina is crucial, especially since millions face this common aspect of coronary artery disease each year. It’s understandable to feel overwhelmed, but effective management can not only ease your symptoms but also significantly enhance your quality of life. This makes it essential for both patients and healthcare providers to embrace supportive practices in treatment.
With various strategies available – from simple lifestyle changes to advanced medical interventions – you might wonder: how can you ensure you’re receiving the most effective care tailored to your unique needs? Remember, you’re not alone in this journey. Seeking help and guidance can lead to a more comfortable and fulfilling life.
Understand Stable Angina: Causes and Symptoms
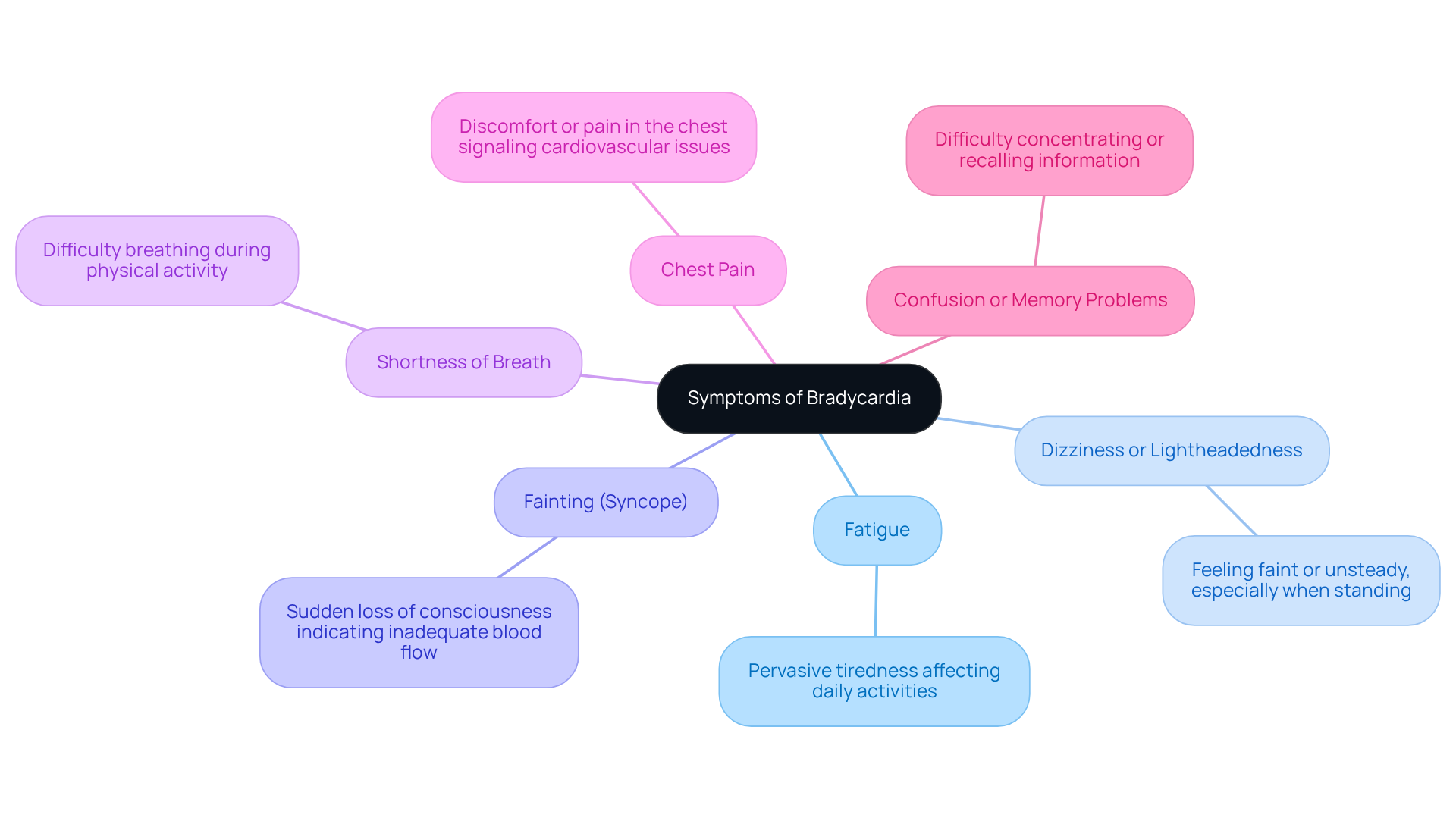
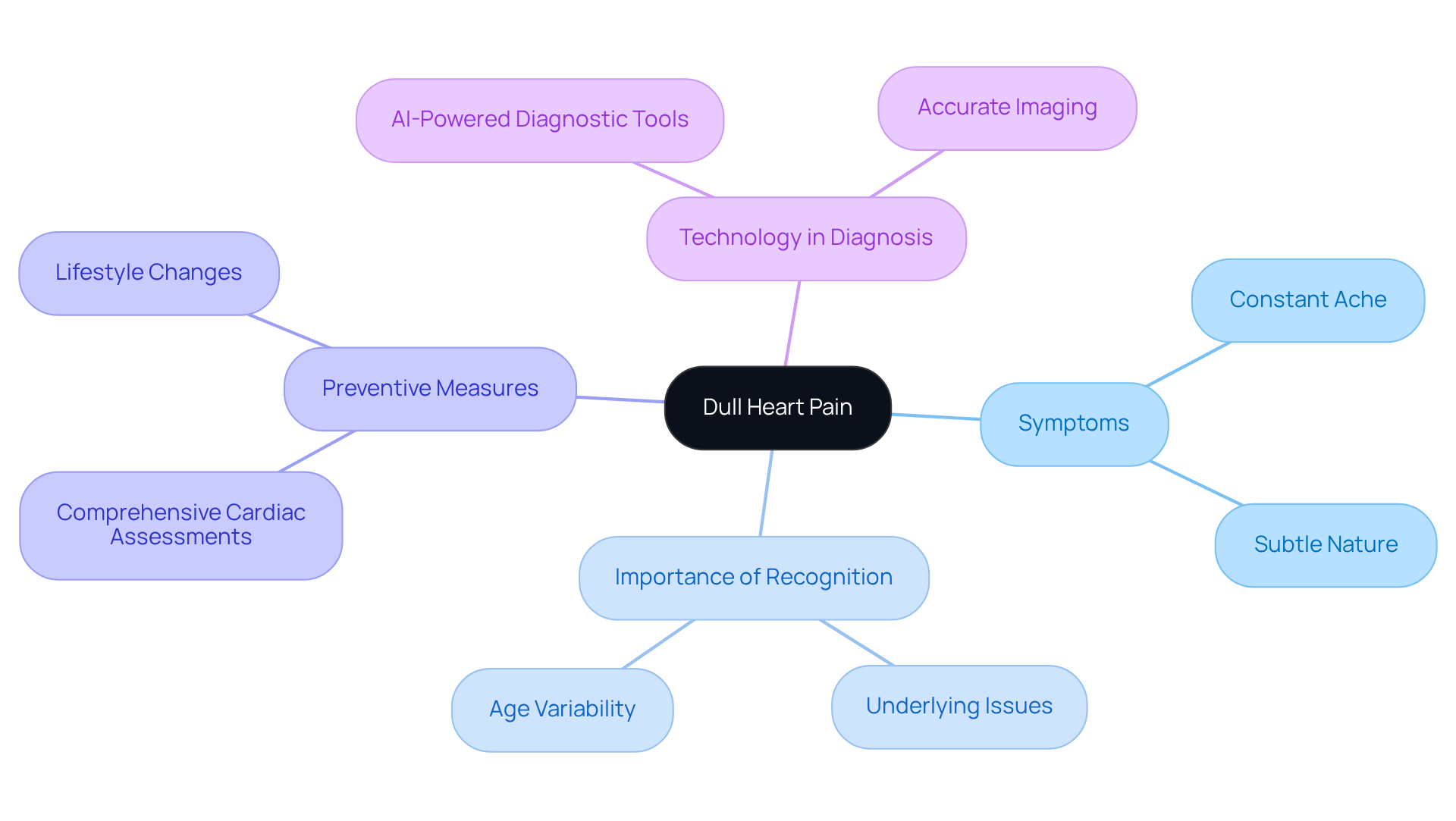
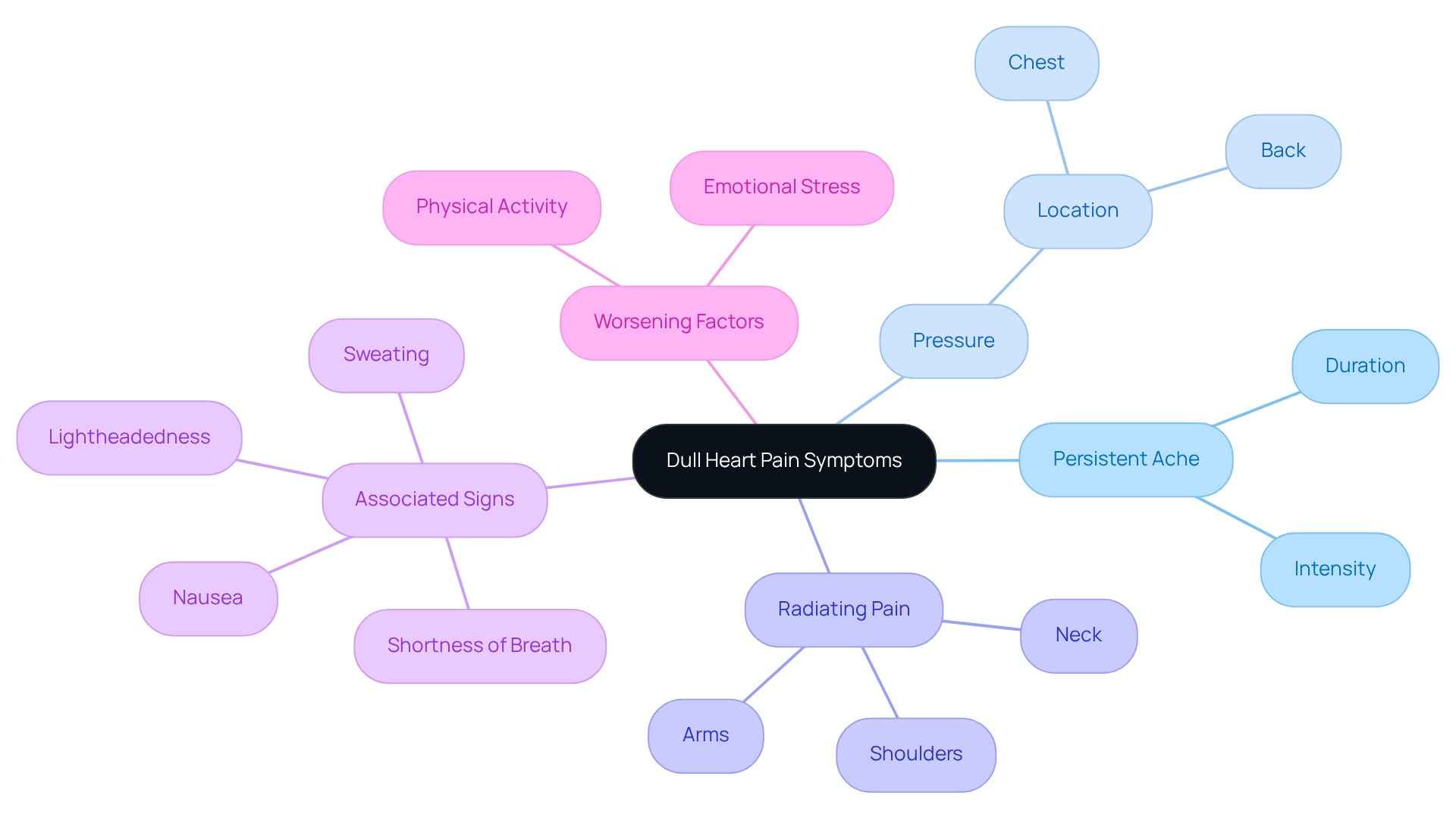
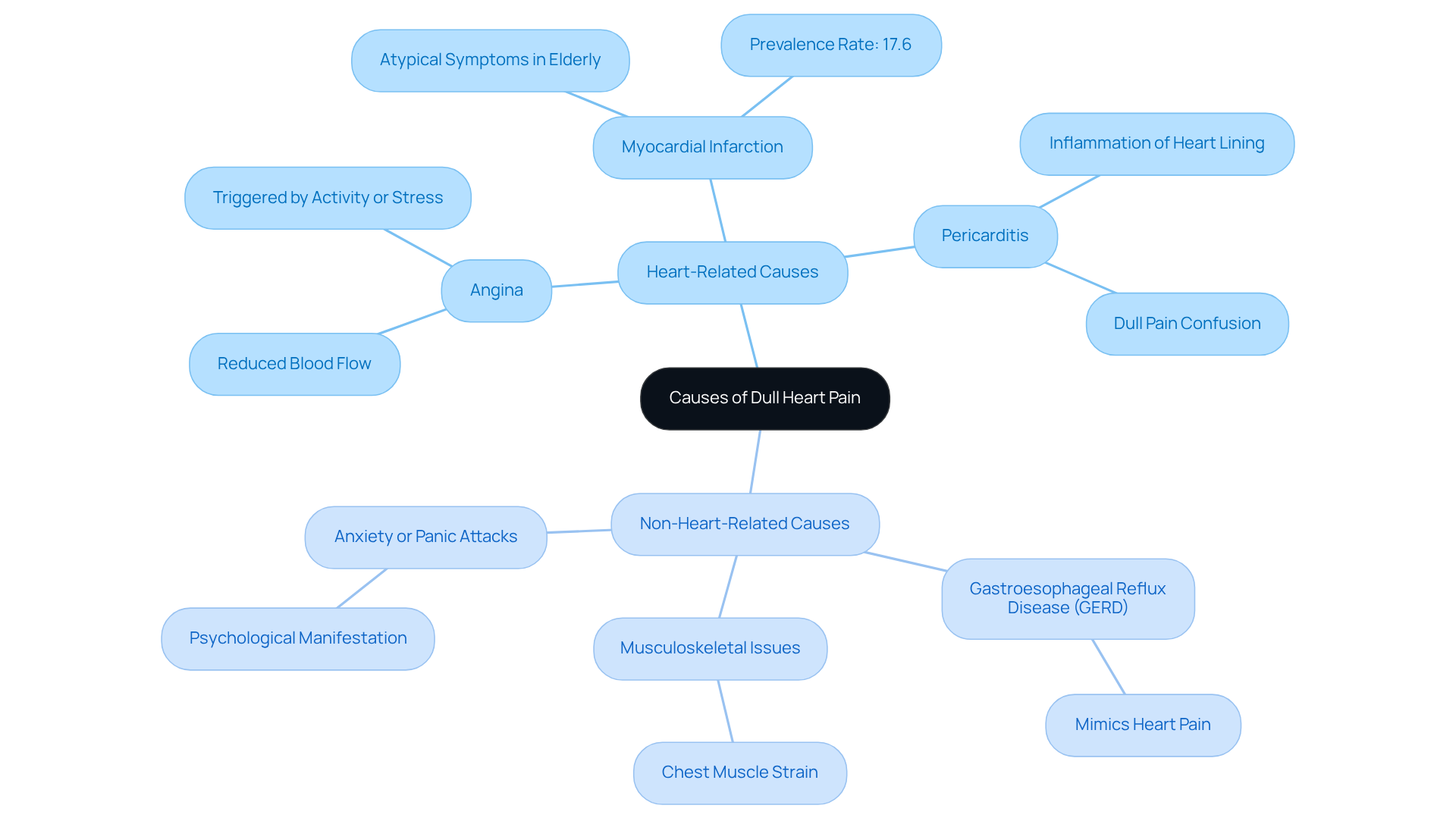
Stable chest pain is a common sign of coronary artery disease, and it can be quite concerning. This discomfort arises when the heart muscle doesn’t receive enough oxygen-rich blood, especially during times of physical exertion or emotional stress. Here are some key symptoms to be aware of:
- Chest pain or discomfort, often described as pressure or squeezing.
- Pain that may radiate to the shoulders, neck, arms, back, teeth, or jaw.
- Episodes typically lasting a few minutes, often relieved by rest or nitroglycerin.
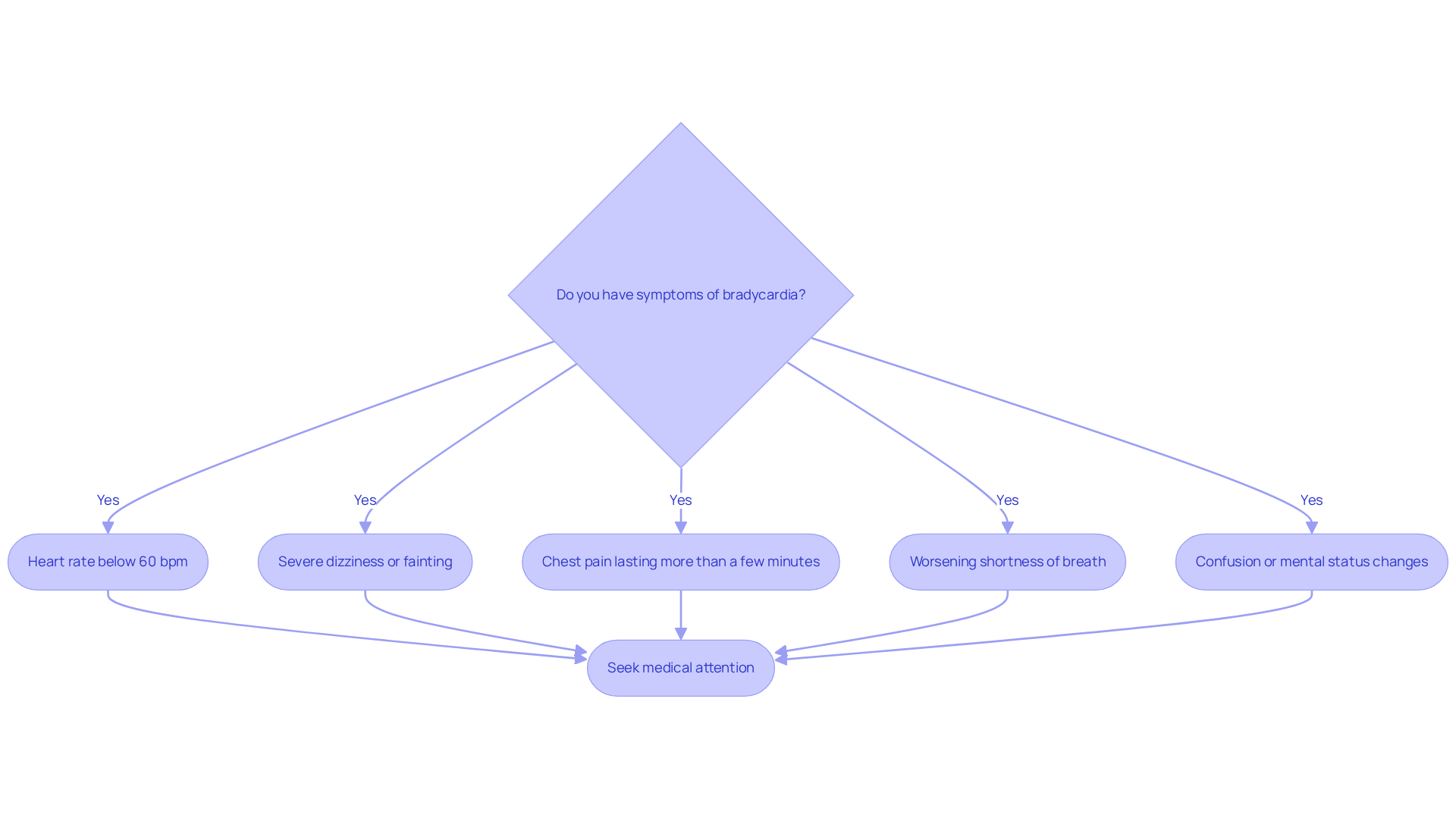
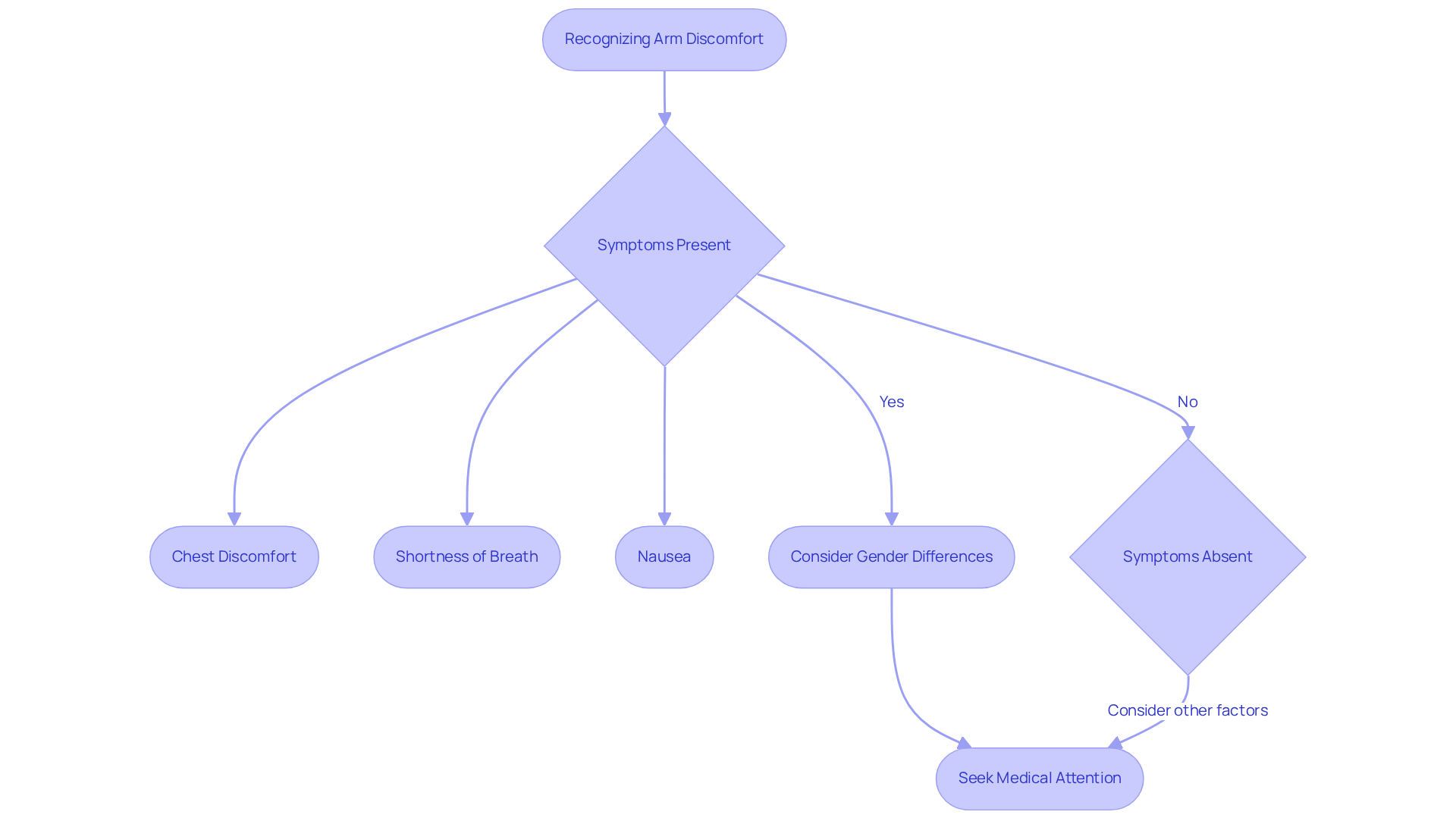
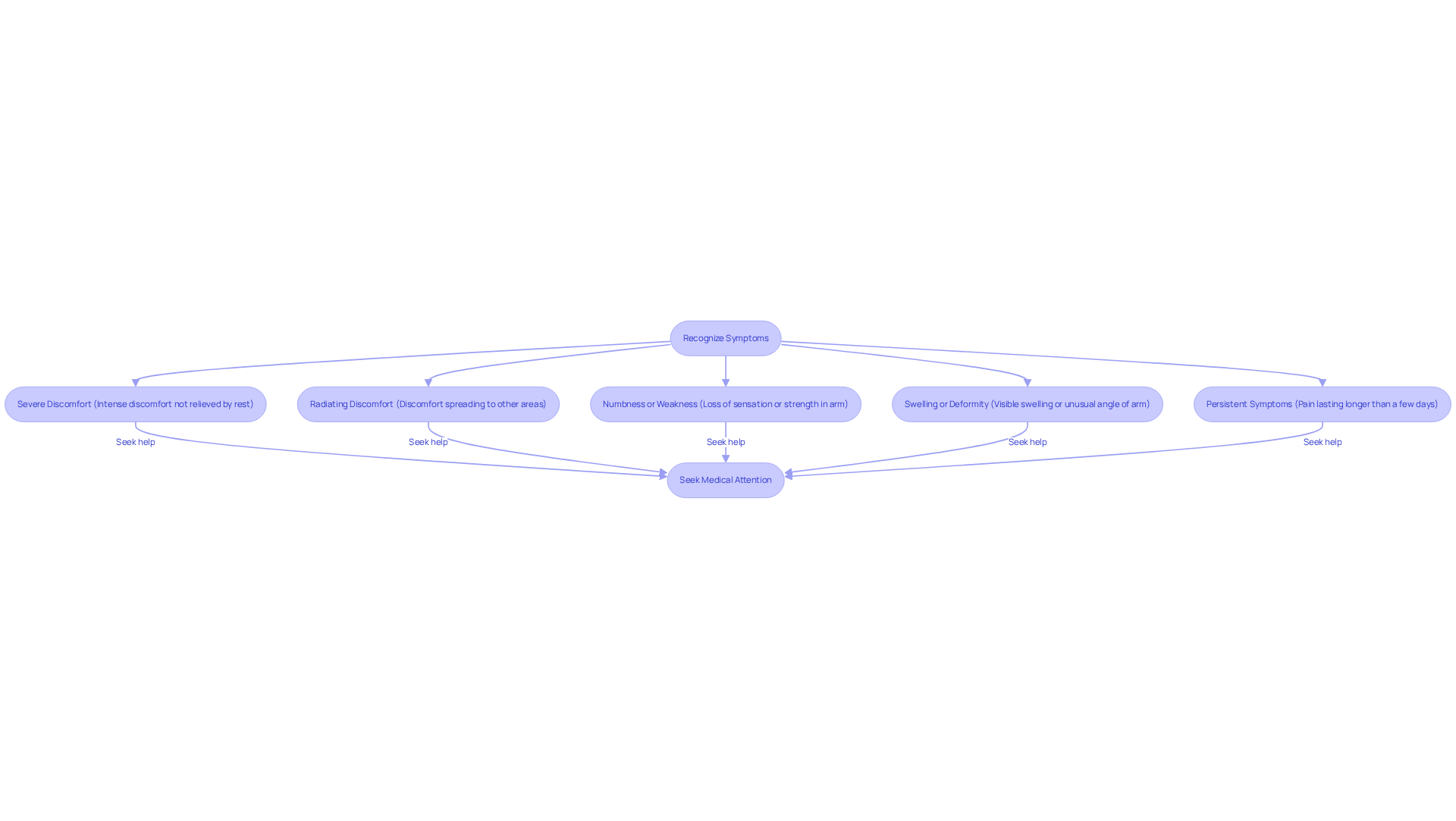
Recognizing these symptoms is crucial for both patients and healthcare providers. It allows for timely intervention, which can make a significant difference in your health journey. Did you know that around 11 million adults in the United States experience angina each year? This highlights just how common it is and underscores the importance of effective strategies.
Understanding what triggers angina, like physical activity, stress, or extreme temperatures, can empower you to manage your condition better. By making lifestyle changes, such as engaging in regular physical activity and quitting smoking, you can significantly lower your risk of cardiovascular events. This proactive approach to heart health is vital.
Cardiologists emphasize that patient education is essential for managing angina effectively, as it not only alleviates symptoms but also enhances your overall quality of life. It’s essential for you to take an active role in your care. Remember, you’re not alone in this journey; support systems are available, and reaching out for help is a strong and positive step forward.
Conduct Comprehensive Exams and Tests for Accurate Diagnosis
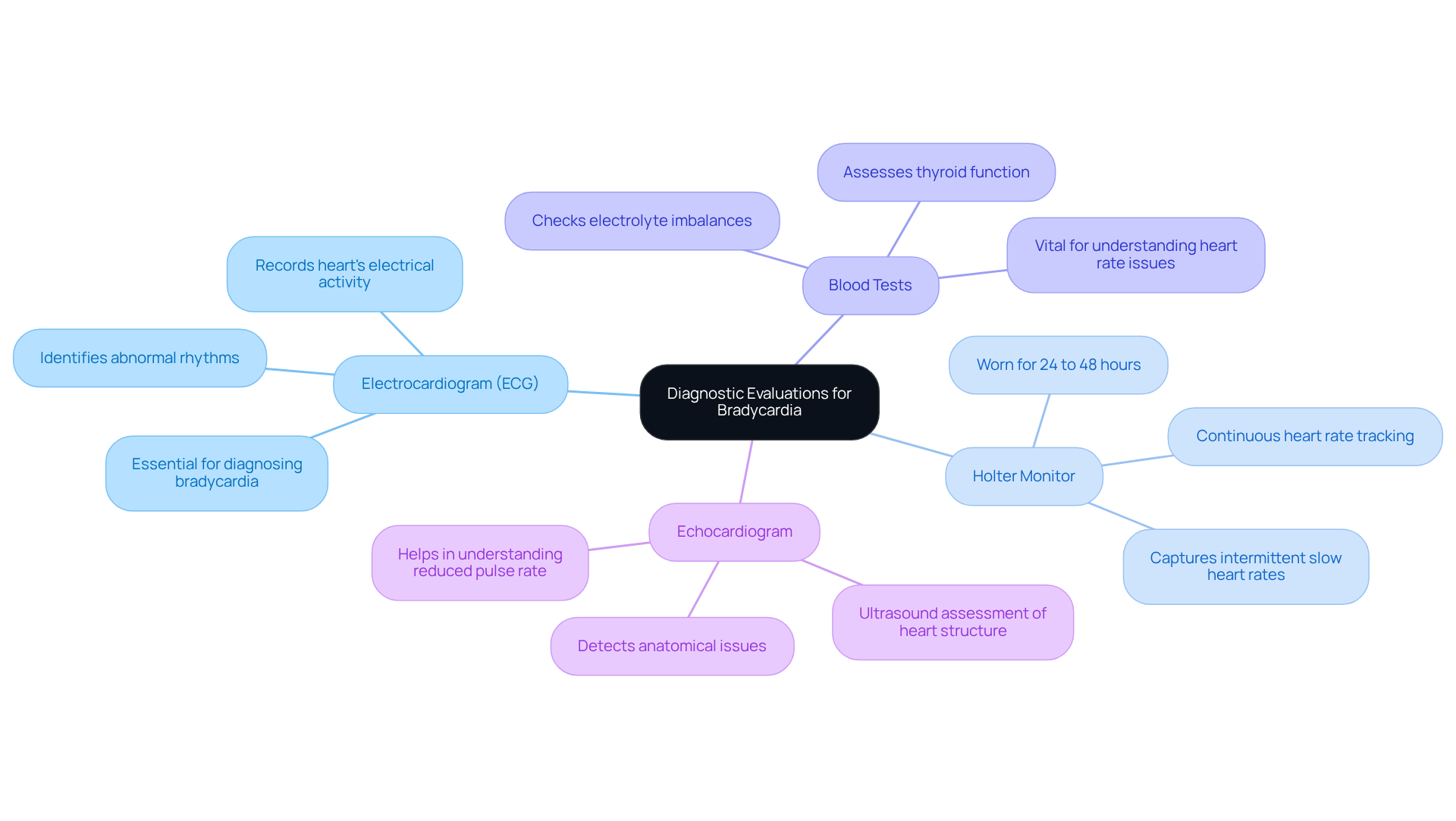
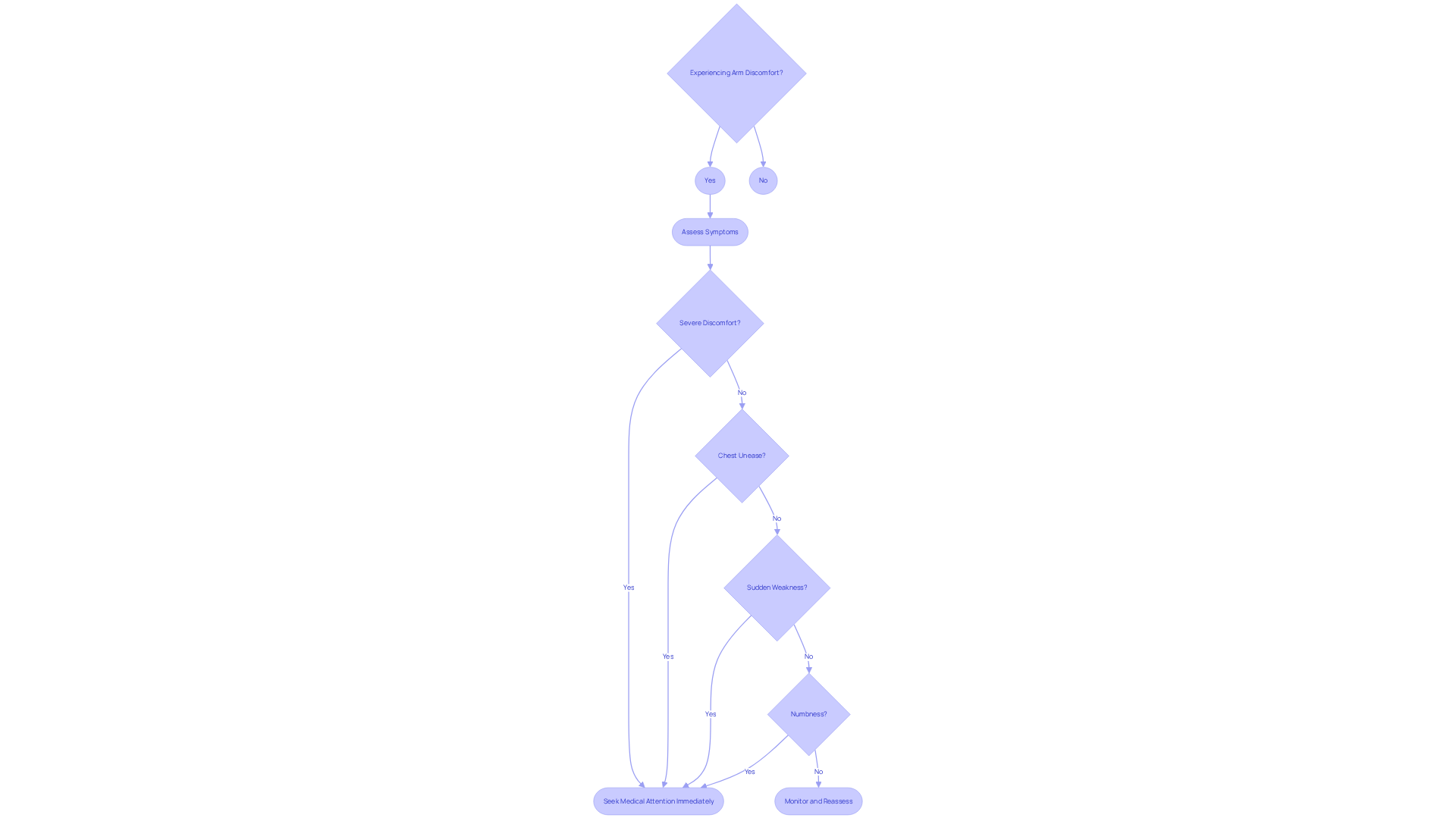
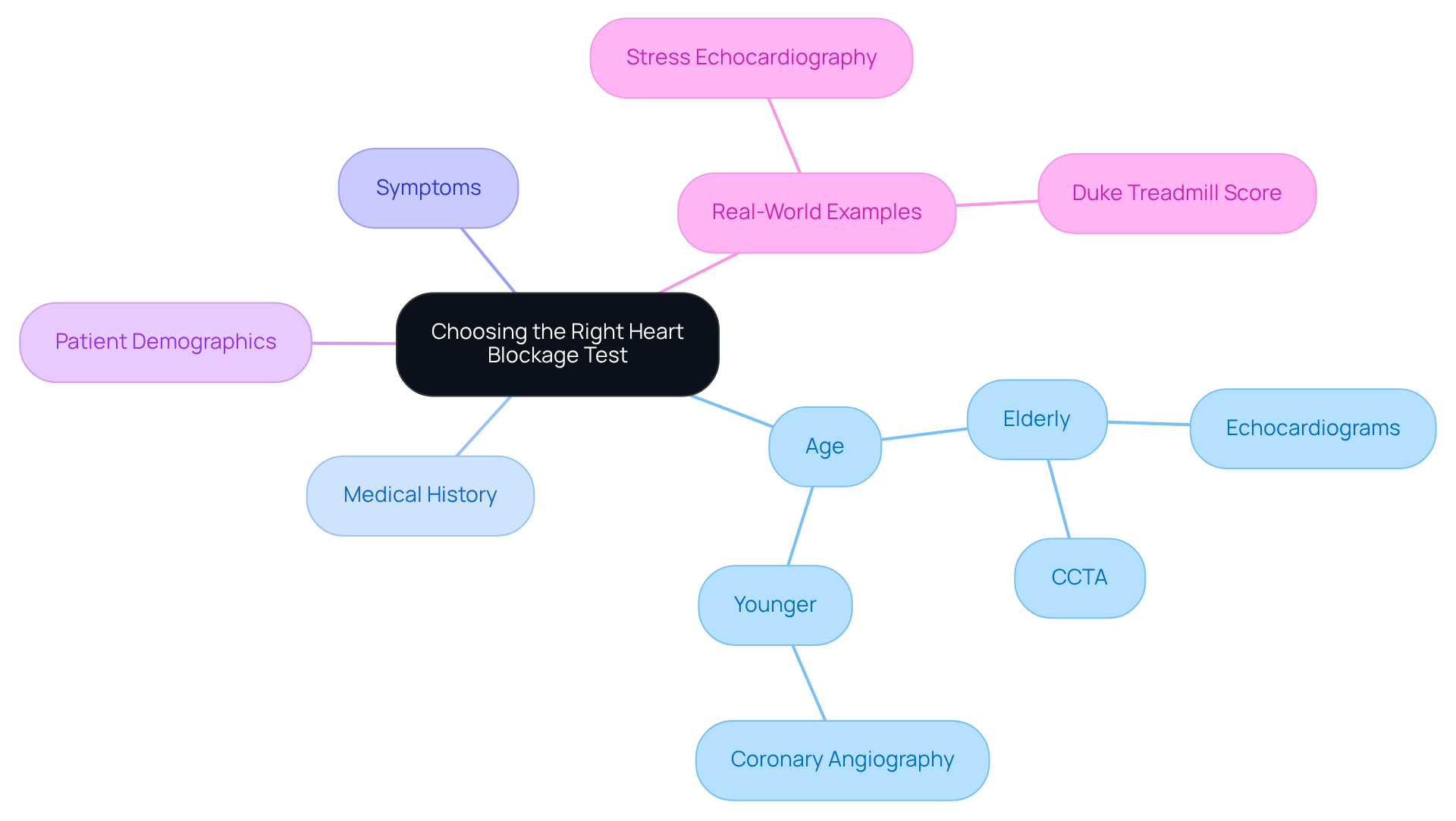
Identifying stable angina can be a daunting experience, but a thorough assessment can provide clarity and peace of mind. This process involves understanding your medical history, conducting a physical examination, and utilizing various diagnostic tests. Let’s explore some key components of this journey together:
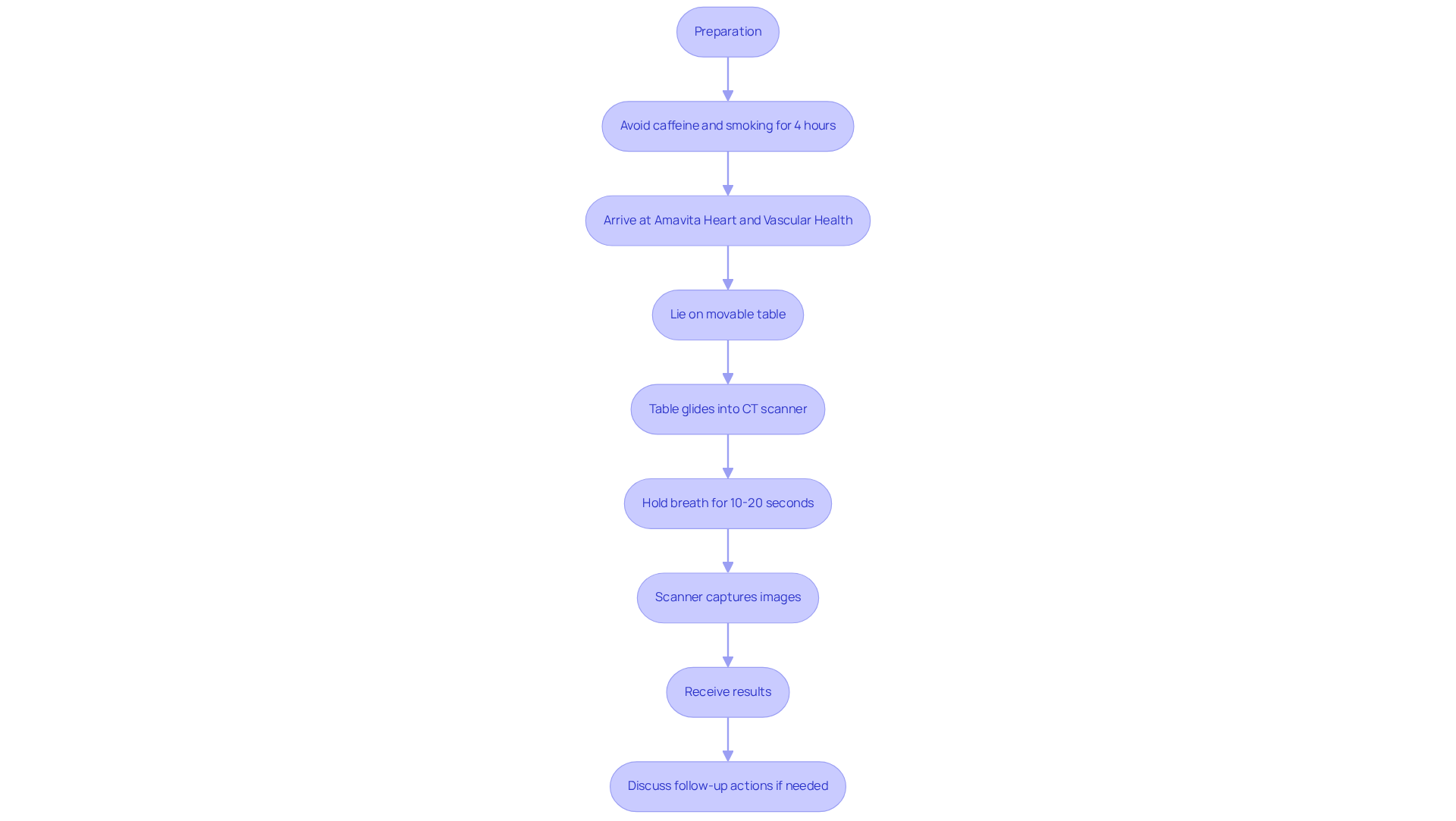
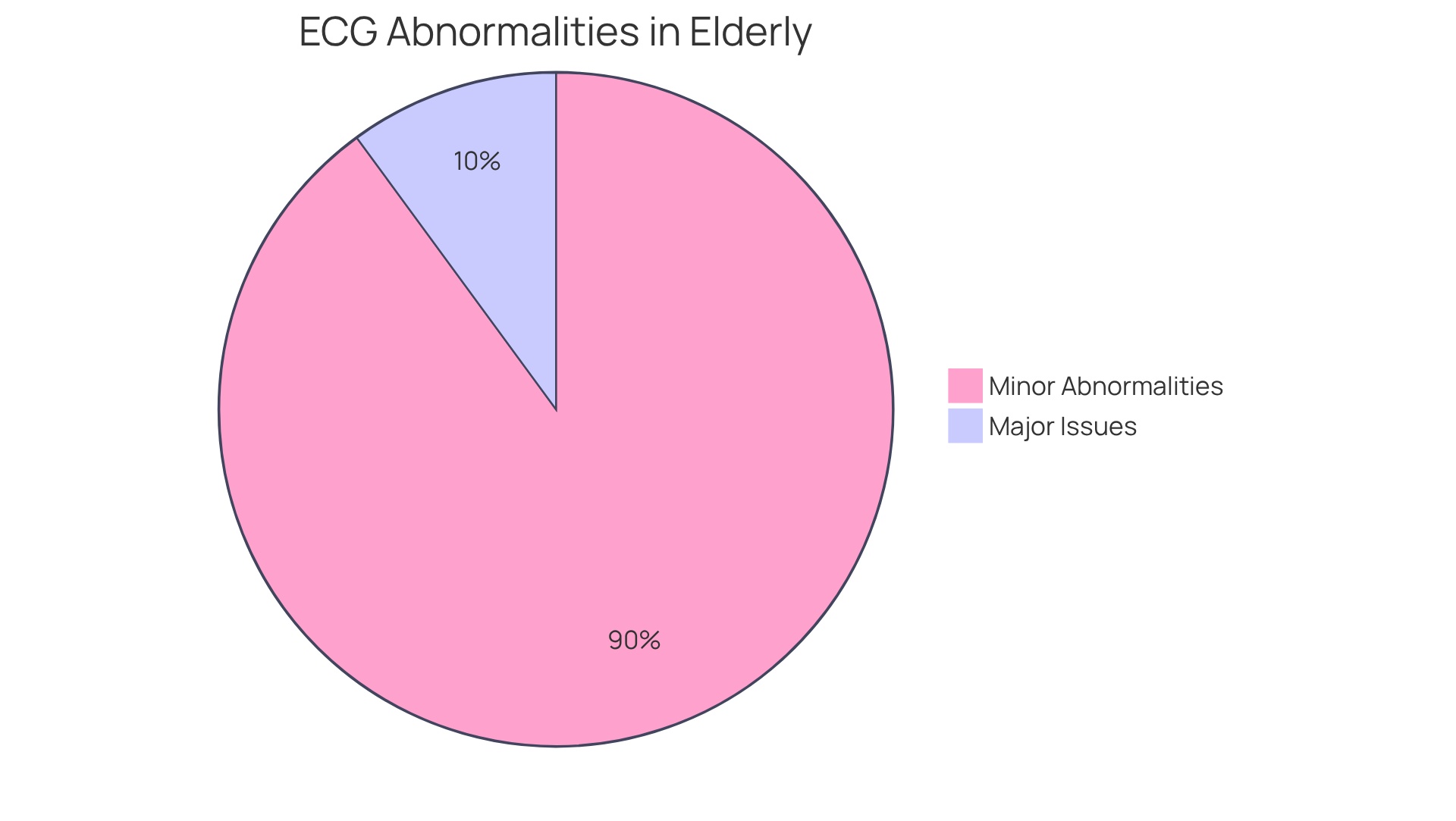
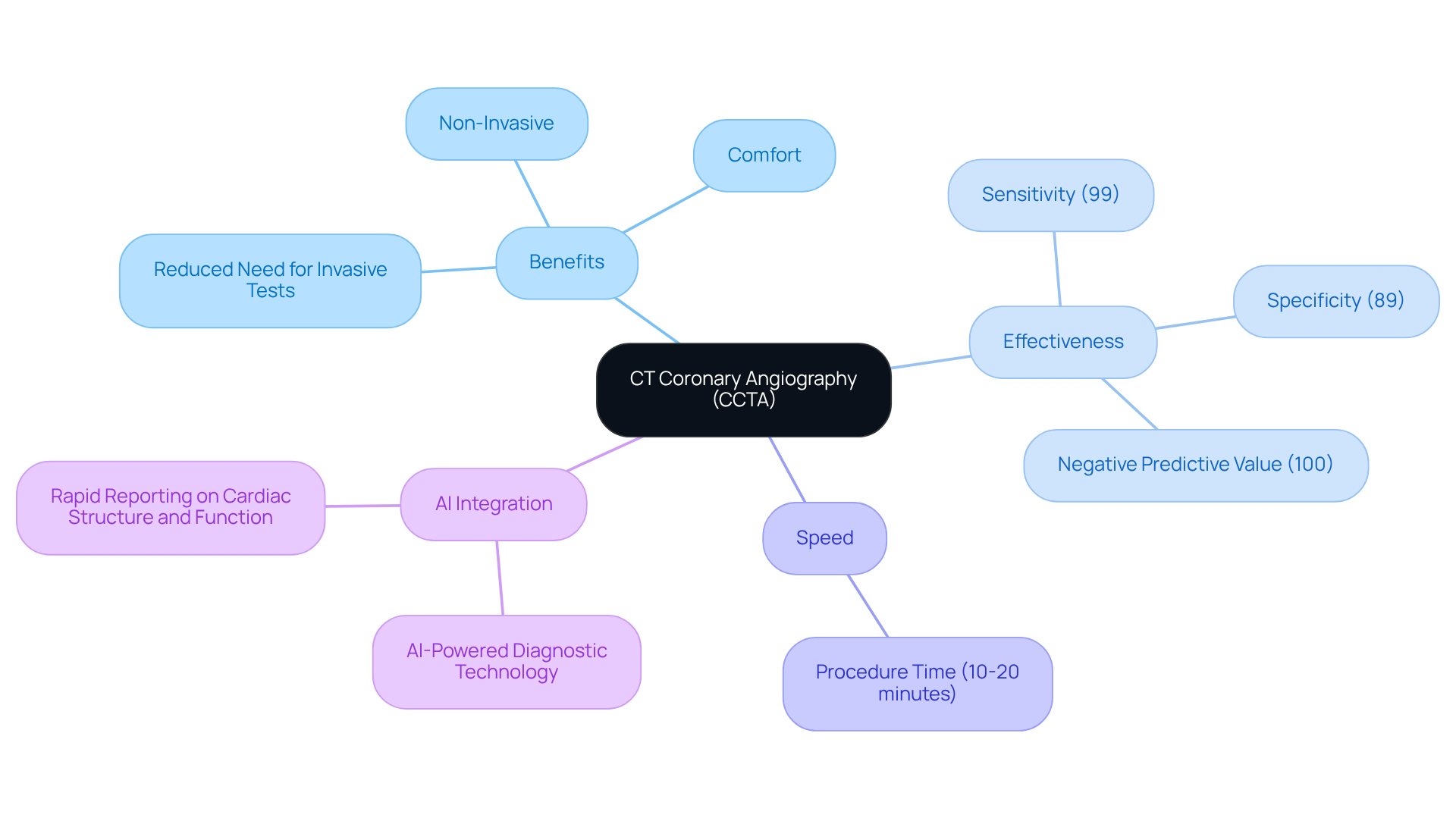
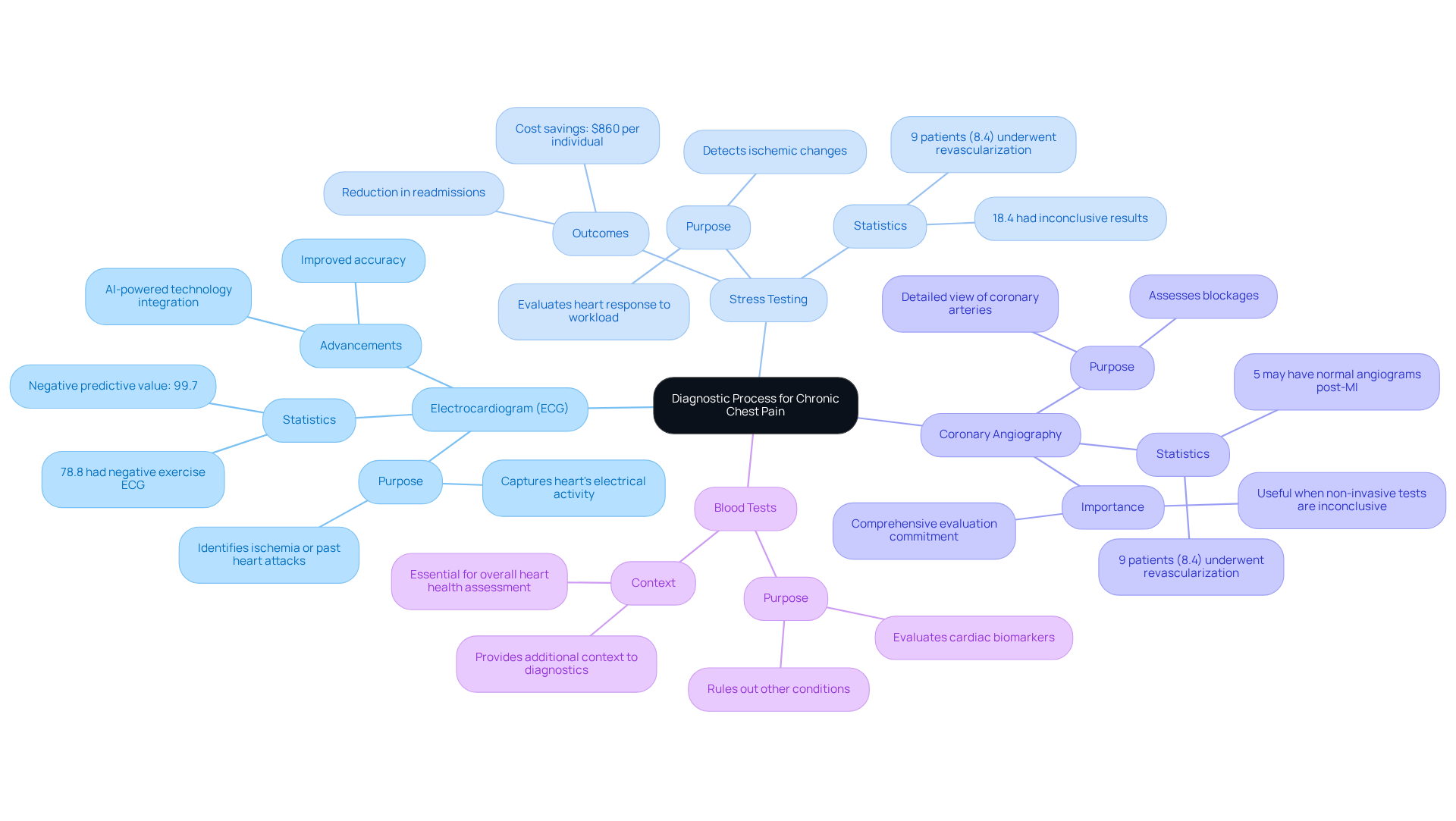
- Electrocardiogram (ECG): This vital test captures your heart’s electrical activity, helping to identify any signs of ischemia or past heart attacks. With recent advancements, its accuracy has significantly improved, making it an essential tool for diagnosing stable angina. Did you know that the negative predictive value of this test is an impressive 99.7%? This reinforces its reliability as a diagnostic tool. At Amavita, we enhance these assessments with AI-powered technology, ensuring timely interventions that can make a real difference in your care.
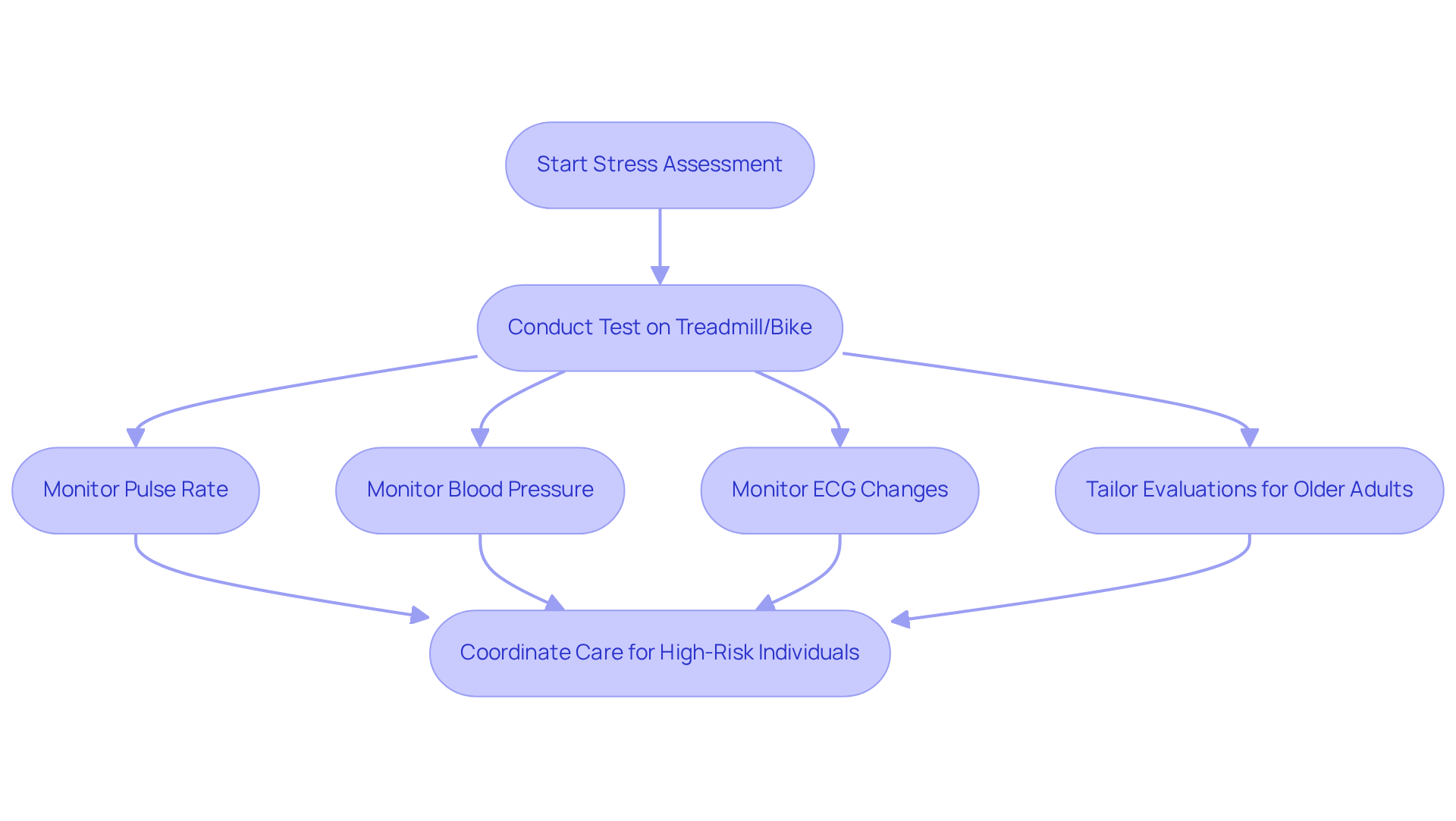
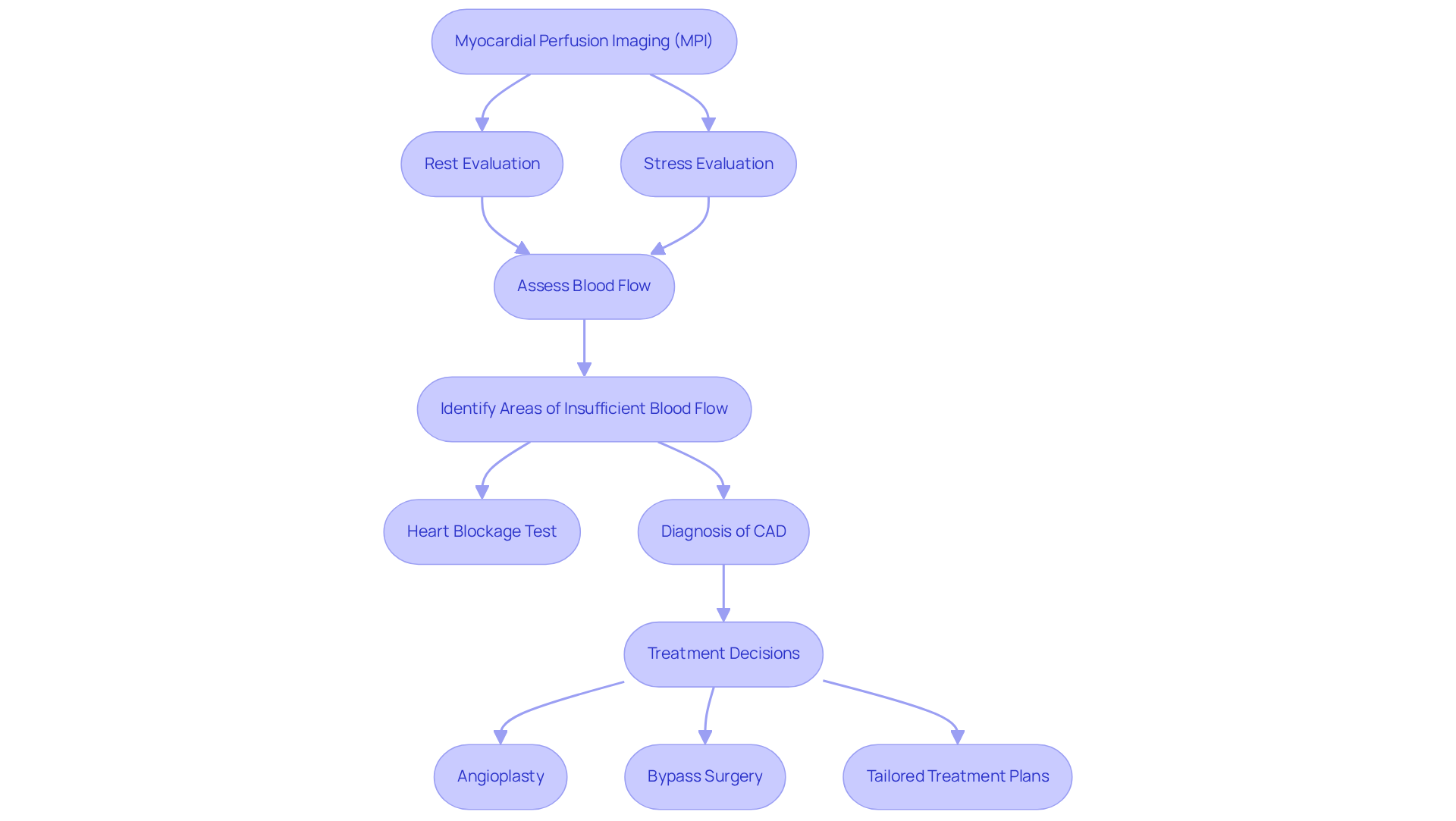
- Stress testing: Both exercise and pharmacologic stress tests are used to evaluate how your heart responds to increased workload. Current data shows that 93 individuals (18.4%) had inconclusive results, highlighting the importance of these tests in detecting ischemic changes. These tests provide crucial insights into your condition, with many individuals receiving stable angina treatment showing positive results. Our program has even demonstrated a significant reduction in readmissions, saving around $860 per individual while enhancing care.
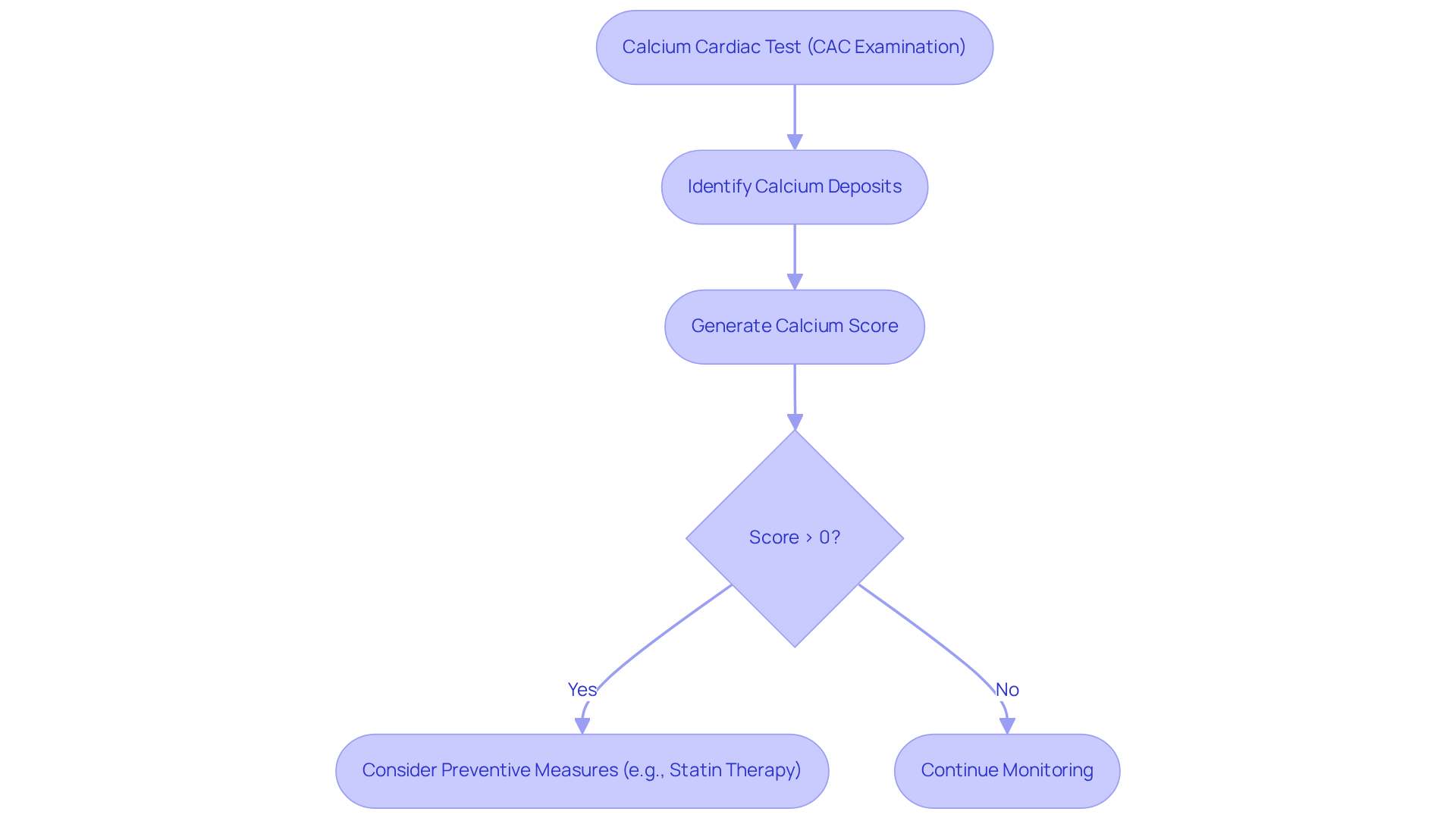
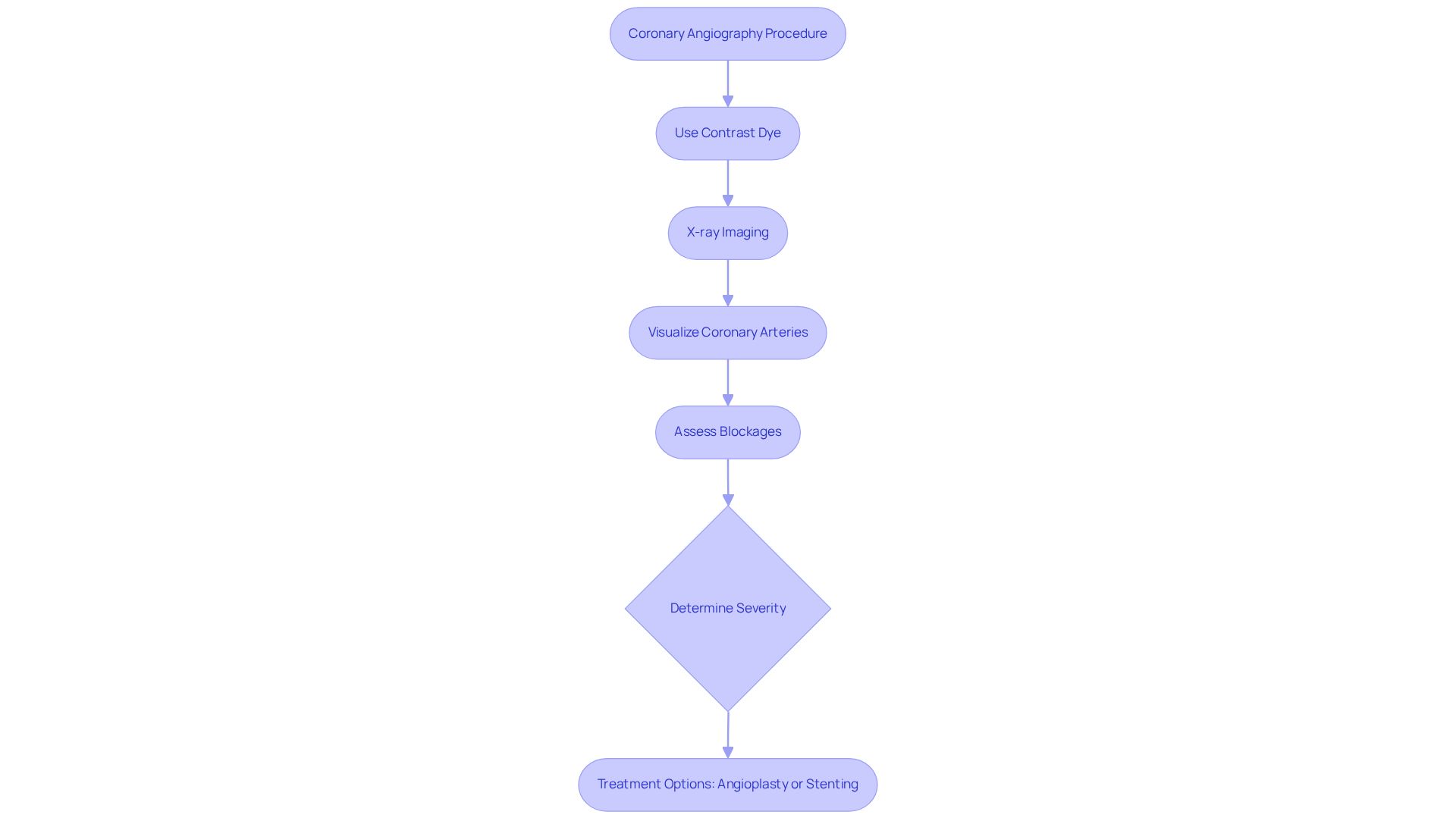
- Coronary angiography: This imaging technique offers a detailed view of your coronary arteries, allowing healthcare providers to assess any blockages. It’s particularly useful when non-invasive tests don’t provide clear answers. For instance, 9 individuals (8.4%) from a study underwent revascularization due to clinically significant blockages, showcasing the practical benefits of this diagnostic test. At Amavita, we are committed to patient-centered care, ensuring you receive a comprehensive evaluation.
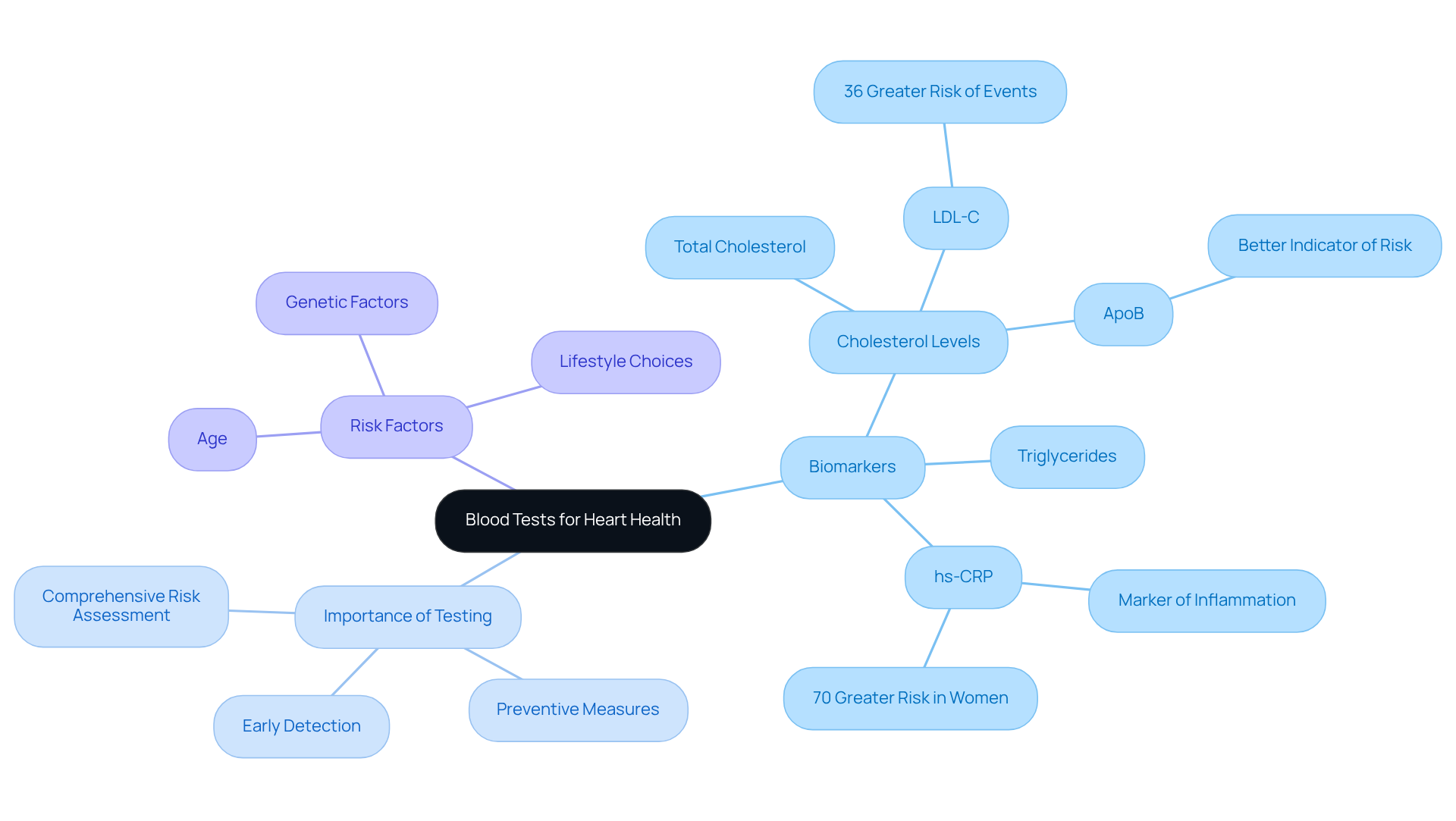
- Cardiac biomarker testing: Evaluating cardiac biomarkers is essential for ruling out other conditions and assessing your overall heart health. These tests can provide additional context to your diagnostic picture, ensuring a complete understanding of your cardiovascular status.
The American Heart Association (AHA) guidelines suggest that a comprehensive assessment is a reasonable approach for individuals experiencing consistent chest pain with a low likelihood of significant coronary artery disease. By embracing this thorough diagnostic approach, along with the advanced technologies available at Amavita Heart and Vascular Health®, we can ensure you receive the most suitable and effective care for your condition. Remember, you are not alone in this journey; we are here to support you every step of the way, enhancing your quality of life and health outcomes.
Implement Advanced Treatment Strategies for Effective Management
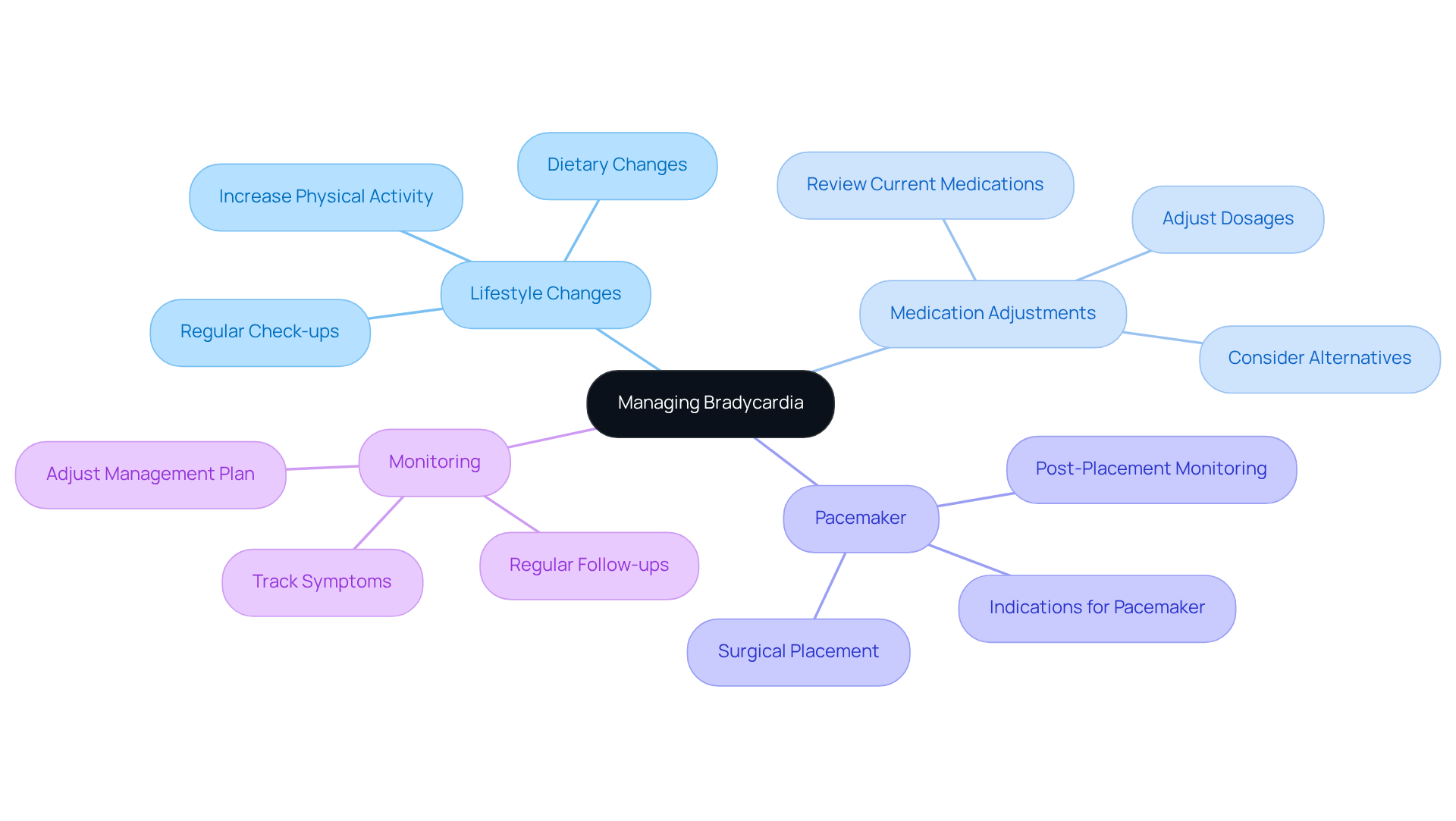
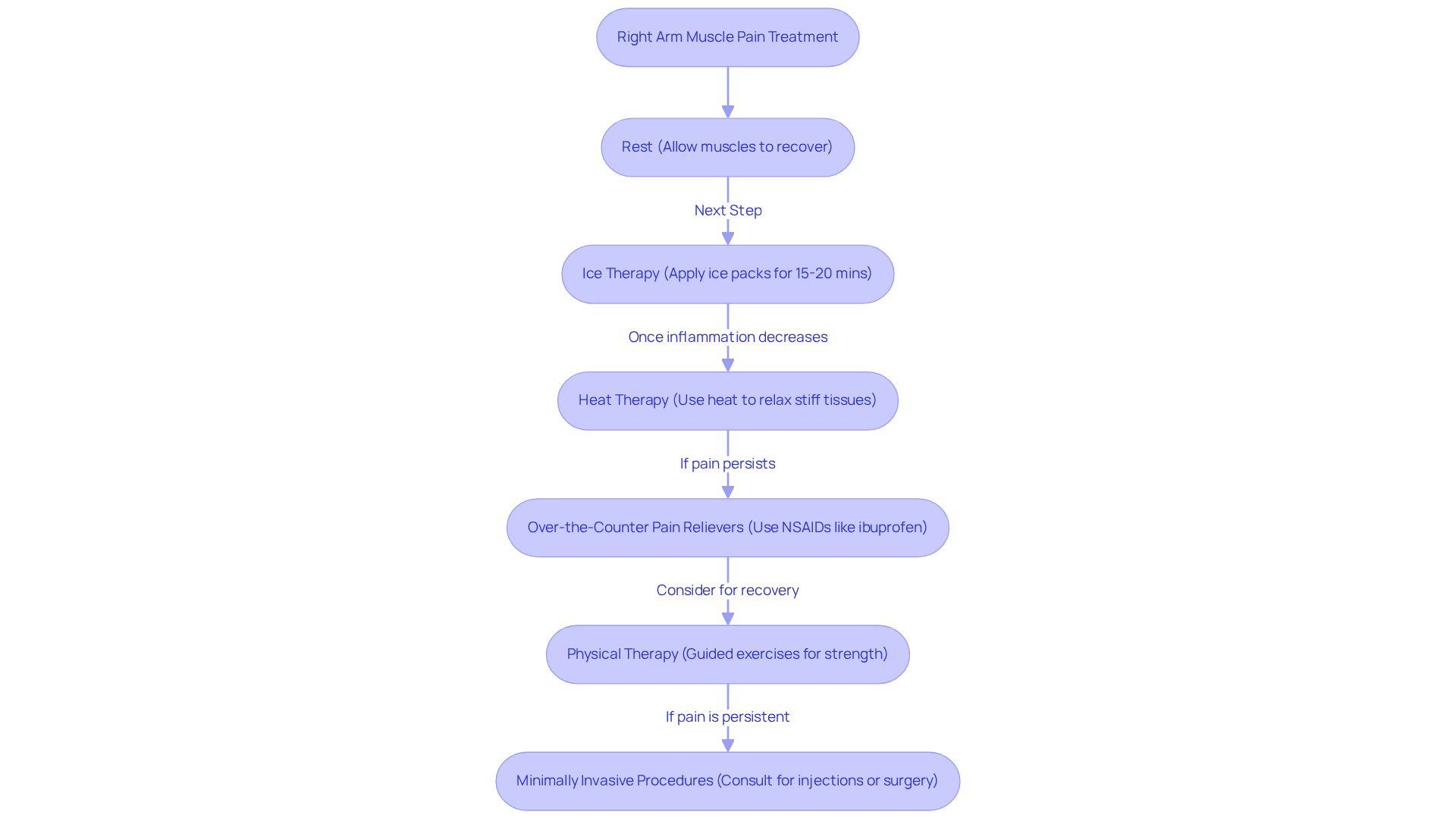
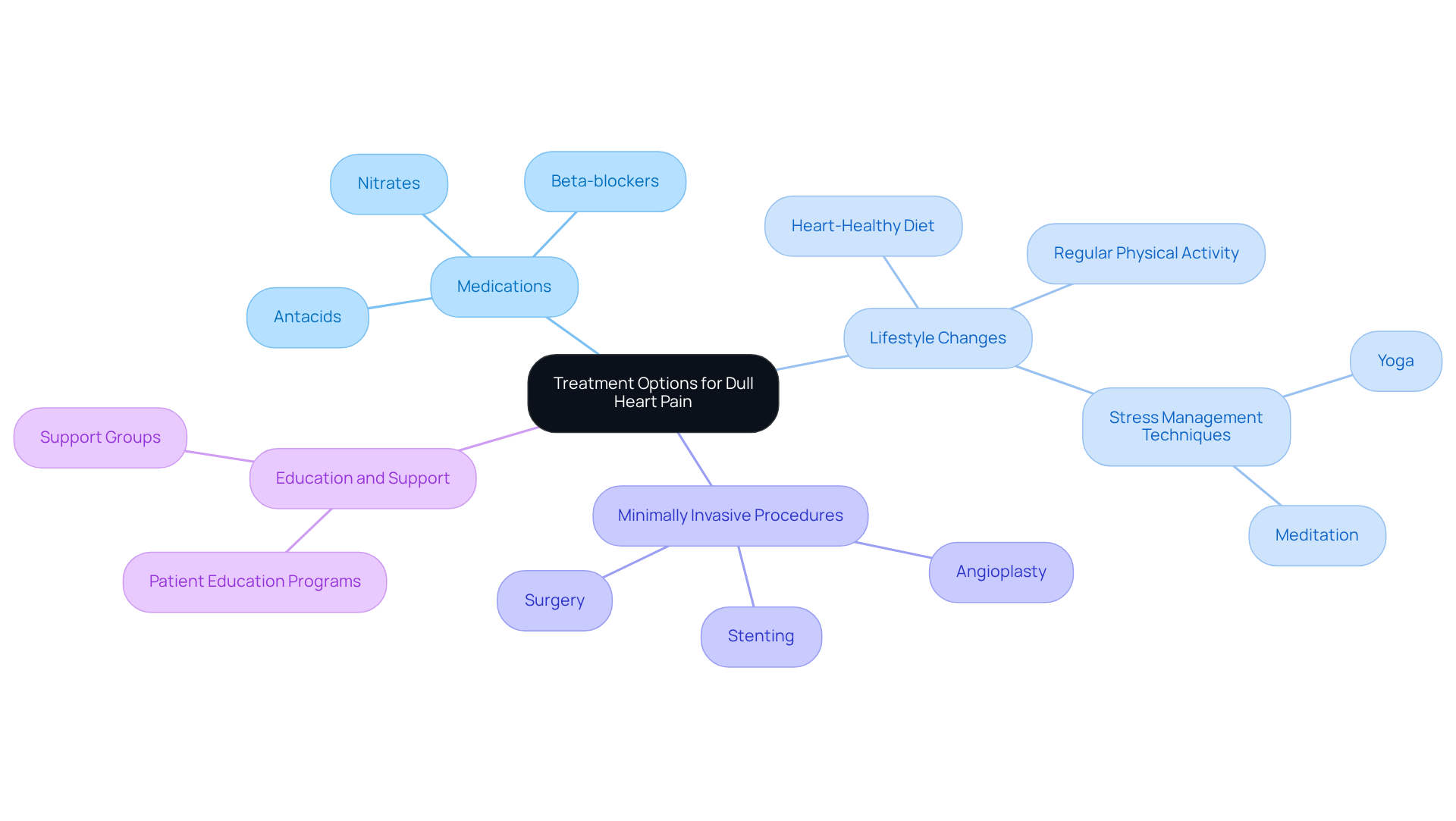
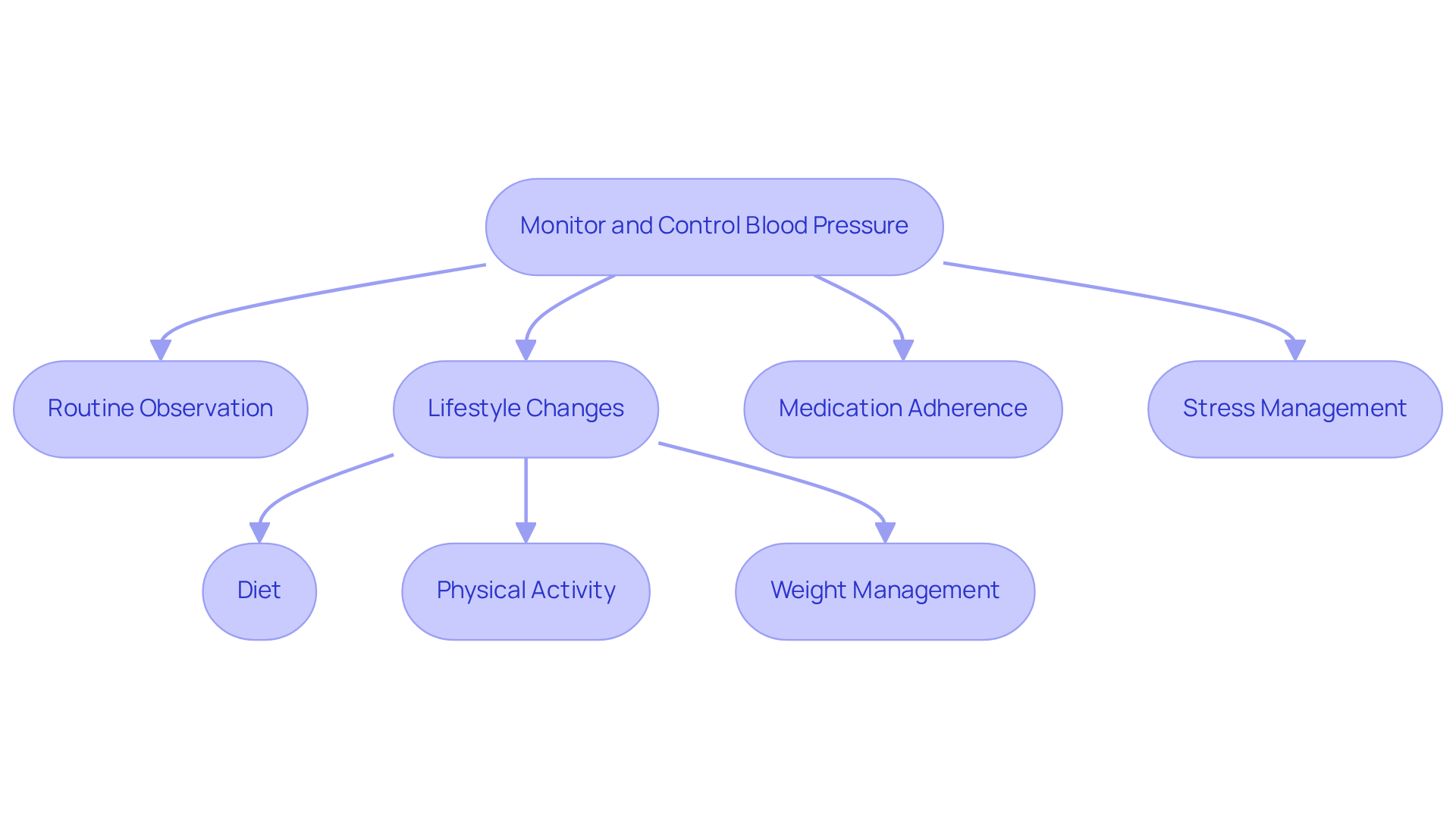
Managing stable angina can feel overwhelming, but with a comprehensive approach to treatment, it can make a significant difference. It’s important to consider lifestyle changes, medications, and, when necessary, interventional techniques in management. Here are some key strategies to help you on this journey:
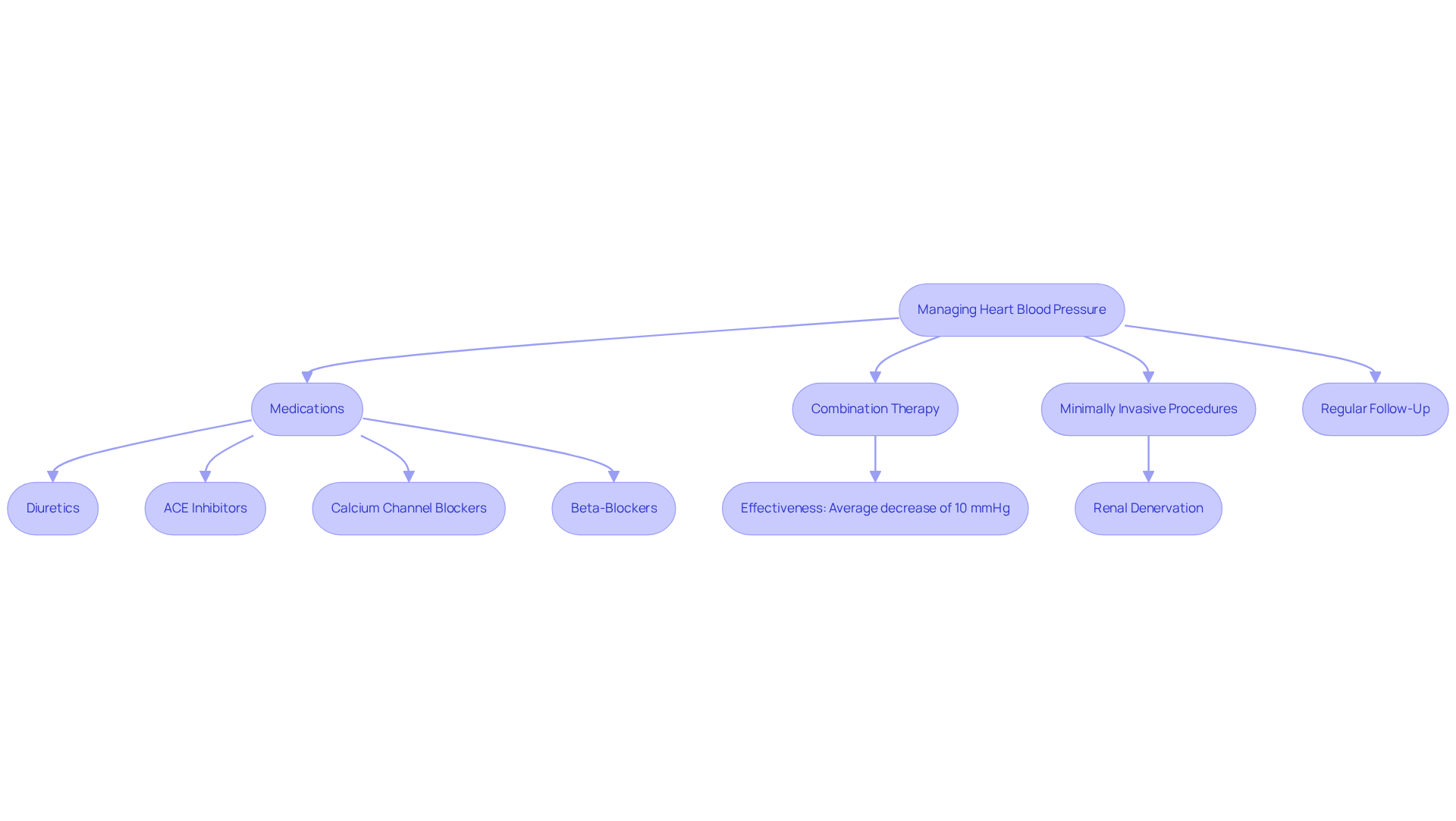
- Medications: Treatment options often include beta-blockers, calcium channel blockers, and long-acting nitrates. These medications are part of a broader strategy, working to reduce the workload on your heart and alleviate symptoms, helping you feel more comfortable in your daily life.
- Lifestyle changes: Embracing heart-healthy habits is essential. Regular exercise, a balanced diet filled with whole foods, and quitting smoking can lead to remarkable improvements in your quality of life. Research indicates that even a modest 10-15% weight loss in obese individuals can lower cardiovascular disease mortality by 21%. As Dr. Caldwell Esselstyn wisely notes, “food is medicine,” highlighting how crucial dietary choices are in managing heart health.
For those facing severe symptoms, treatment may involve revascularization procedures such as angioplasty or coronary artery bypass grafting (CABG) to restore proper blood flow. At Amavita, we utilize advanced minimally invasive techniques, including stenting, to ensure the best outcomes for our patients. However, it’s important to remember that many angioplasties are performed on individuals who may not see significant benefits, so careful consideration of options is vital.
Ongoing monitoring and regular follow-ups are key to effective management in stable angina. At Amavita, we prioritize comprehensive evaluations and diagnostic tests, such as diagnostic testing, to tailor treatment plans to your unique needs. Adjusting strategies based on your individual responses ensures optimal management of your condition. By involving you in your care, we foster a collaborative relationship that empowers you to take charge of your health.
By integrating these advanced approaches, healthcare providers at Amavita can significantly enhance the management of stable angina, leading to improved outcomes and a better quality of life for you.
Enhance Patient Education and Support for Long-Term Success
Managing stable chest pain effectively starts with strong education and support that truly care for patients. Here are some key strategies that can make a difference:
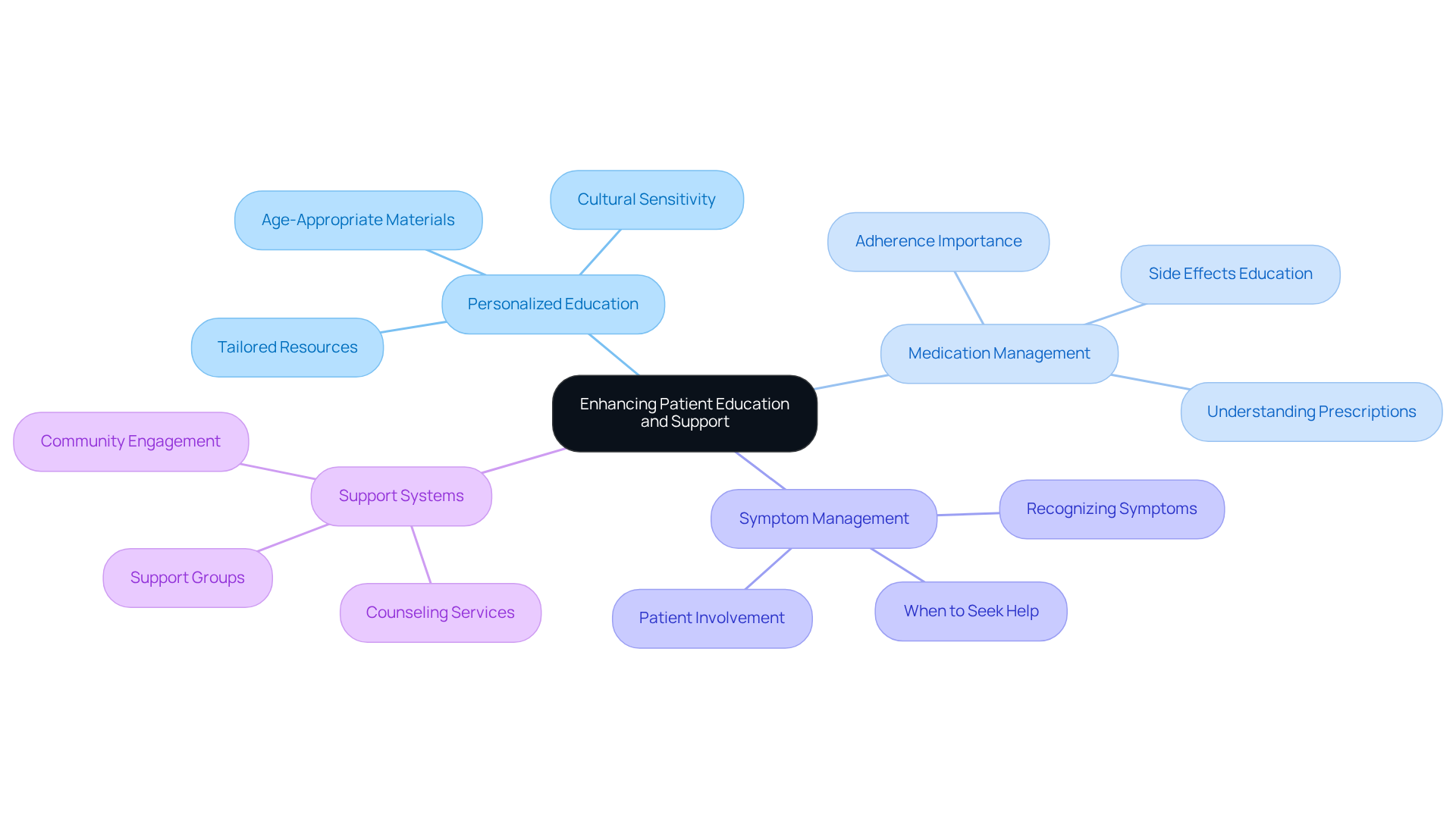
- Tailoring education to fit each patient’s age, literacy level, and cultural background can significantly enhance their understanding and retention of important information. Since many individuals with angina are older adults, these personalized approaches are not just helpful – they’re essential.
- It’s crucial to help individuals understand their prescribed medications, including how to use them properly, potential side effects, and the importance of sticking to their regimen. Research shows that when patients adhere to their medication plans, they experience fewer complications and better health outcomes.
- Teaching individuals to recognize their symptoms and when to seek medical help can prevent complications and improve their health. Involving patients in this process is not just beneficial; it’s a moral obligation. As Dr. Maureen Bisognano wisely noted, “Patients are our partners in care.”
- Encouraging participation in support groups or counseling can provide emotional support and foster a sense of community, which is vital for long-term management. Investing in client engagement can yield significant returns, with every pound spent returning three to five pounds in enhanced efficiency and reduced costs.
By prioritizing these educational and supportive measures, healthcare providers empower patients to take an active role in managing their stable angina treatment. This not only leads to better outcomes but also enhances their overall quality of life. Remember, you’re not alone in this journey – support is always available.
Conclusion
Understanding and managing stable angina is essential for improving the quality of life for millions affected by this condition. It’s important to recognize symptoms, undergo thorough diagnostic tests, and implement effective treatment strategies. By taking an active role in their care, patients can significantly enhance their health outcomes and manage their symptoms more effectively.
Have you considered how lifestyle modifications can impact your health? Medications and advanced diagnostic techniques play a crucial role in tailoring treatment plans to your needs. Personalized education and support systems are vital for empowering you and promoting adherence to treatment regimens. Proactively managing stable angina not only alleviates symptoms but also fosters a sense of community, encouraging you to engage in your health journey.
Ultimately, the significance of stable angina treatment lies in its ability to transform lives. By embracing the best practices outlined here, you and your healthcare provider can work together to navigate the complexities of this condition. It’s vital for anyone experiencing stable angina to seek support, stay informed, and actively participate in their management strategies. Together, we can pave the way for a healthier future.
Frequently Asked Questions
What is stable angina?
Stable angina is a type of chest pain that occurs when the heart muscle doesn’t receive enough oxygen-rich blood, often triggered by physical exertion or emotional stress.
What are the common symptoms of stable angina?
Common symptoms include chest pain or discomfort described as pressure or squeezing, pain that may radiate to the shoulders, neck, arms, back, teeth, or jaw, and episodes that typically last a few minutes, often relieved by rest or nitroglycerin.
How prevalent is stable angina in the United States?
Approximately 11 million adults in the United States experience angina each year, highlighting its commonality and the importance of effective treatment strategies.
What triggers episodes of stable angina?
Triggers for stable angina episodes can include physical activity, stress, or extreme temperatures.
How can lifestyle changes impact stable angina?
Engaging in regular physical activity and quitting smoking can significantly lower the risk of cardiovascular events and help manage stable angina.
Why is treatment for stable angina important?
Treatment for stable angina is essential for effectively managing chronic chest pain, alleviating symptoms, and enhancing overall quality of life.
How can patients take an active role in managing their stable angina?
Patients can take an active role by recognizing their symptoms, understanding their triggers, making lifestyle changes, and seeking support from healthcare providers.
List of Sources
- Understand Stable Angina: Causes and Symptoms
- Top Coronary Artery Disease News of 2023 (https://tctmd.com/news/top-coronary-artery-disease-news-2023)
- Memorable Cardiology Quotes (https://ajconline.org/article/S0002-9149(08)01715-3/fulltext)
- drsvenkatesan.com (https://drsvenkatesan.com/category/cardiology-quotes/page/2)
- Memorable Cardiology Quotes – TheKnowHow.Æ (https://theknowhow.ae/memorable-cardiology-quotes-heart)
- Checking your browser – reCAPTCHA (https://pmc.ncbi.nlm.nih.gov/articles/PMC12116826)
- Conduct Comprehensive Exams and Tests for Accurate Diagnosis
- The Value of Exercise Electrocardiography in Outpatients with Stable Chest Pain and Low Pre-Test Probability of Significant Coronary Artery Disease (https://mdpi.com/2077-0383/12/14/4670)
- Memorable Cardiology Quotes – TheKnowHow.Æ (https://theknowhow.ae/memorable-cardiology-quotes-heart)
- Evaluation and Management of Patients With Stable Angina: Beyond the Ischemia Paradigm: JACC State-of-the-Art Review (https://jacc.org/doi/10.1016/j.jacc.2020.08.078)
- Exercise ECG and CT Coronary Angiography for Patients With Suspected Stable Angina Pectoris (https://jamanetwork.com/journals/jamacardiology/fullarticle/2766244)
- Implement Advanced Treatment Strategies for Effective Management
- parade.com (https://parade.com/1187612/michelle-parkerton/quotes-about-heart-disease)
- Memorable Cardiology Quotes (https://ajconline.org/article/S0002-9149(08)01715-3/fulltext)
- Memorable Cardiology Quotes – TheKnowHow.Æ (https://theknowhow.ae/memorable-cardiology-quotes-heart)
- newsroom.heart.org (https://newsroom.heart.org/news/heart-stenting-relieved-chest-pain-and-improved-exercise-capacity)
- Enhance Patient Education and Support for Long-Term Success
- Continuity of care and medication adherence in patients with angina: a retrospective cohort study using Korea’s National Health Insurance data – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC12198798)
- Patient Engagement Quotes: For Every Purpose & Audience (https://nclusiv.co.uk/blog/f/patient-engagement-quotes-for-every-purpose-audience)
- 10 Patient Experience Quotes for Inspiration (https://carecloud.com/continuum/patient-experience-quotes-for-inspiration)