Introduction
Understanding the nuances of heart health is vital, especially for seniors who may be more susceptible to conditions like bradycardia, which is defined as a resting heart rate of fewer than 60 beats per minute. This seemingly simple metric can indicate serious health risks, such as insufficient blood flow and potential complications like fainting or heart failure.
As caregivers and loved ones, recognizing the signs and symptoms of a dangerously low heart rate is essential. The stakes are high, and timely intervention can truly make a difference. Have you noticed any changes in your loved one’s heart rate?
What strategies can we employ to monitor and manage heart health effectively in older adults? By ensuring they live their lives with vitality and security, we can help them feel supported and cared for. Let’s explore ways to keep our seniors healthy and thriving.
Define Dangerous Low Heart Rate and Its Importance for Seniors
Bradycardia, which refers to a resting pulse rate of fewer than 60 beats per minute (BPM), can indicate a dangerous low heart rate and pose significant health risks, especially for seniors. This condition may cause a dangerous low heart rate, which can lead to insufficient blood flow and symptoms such as fatigue, dizziness, and even fainting. It’s essential for caregivers and patients to recognize this threshold, as it signals when medical help might be needed in the case of a dangerous low heart rate. For older individuals, a dangerous low heart rate can be particularly concerning due to age-related changes in heart function and the potential for underlying health issues.
Have you ever felt unusually tired or dizzy? These could be signs of bradycardia, and it’s important to pay attention. Research shows that if a dangerous low heart rate goes undiagnosed and untreated, it can lead to serious complications, including heart failure and sudden cardiac arrest. That’s why regular pulse monitoring is vital for early detection and management of this condition. A thorough evaluation for bradycardia often includes an electrocardiogram to confirm the diagnosis, especially when pulse rates drop below 50 BPM.
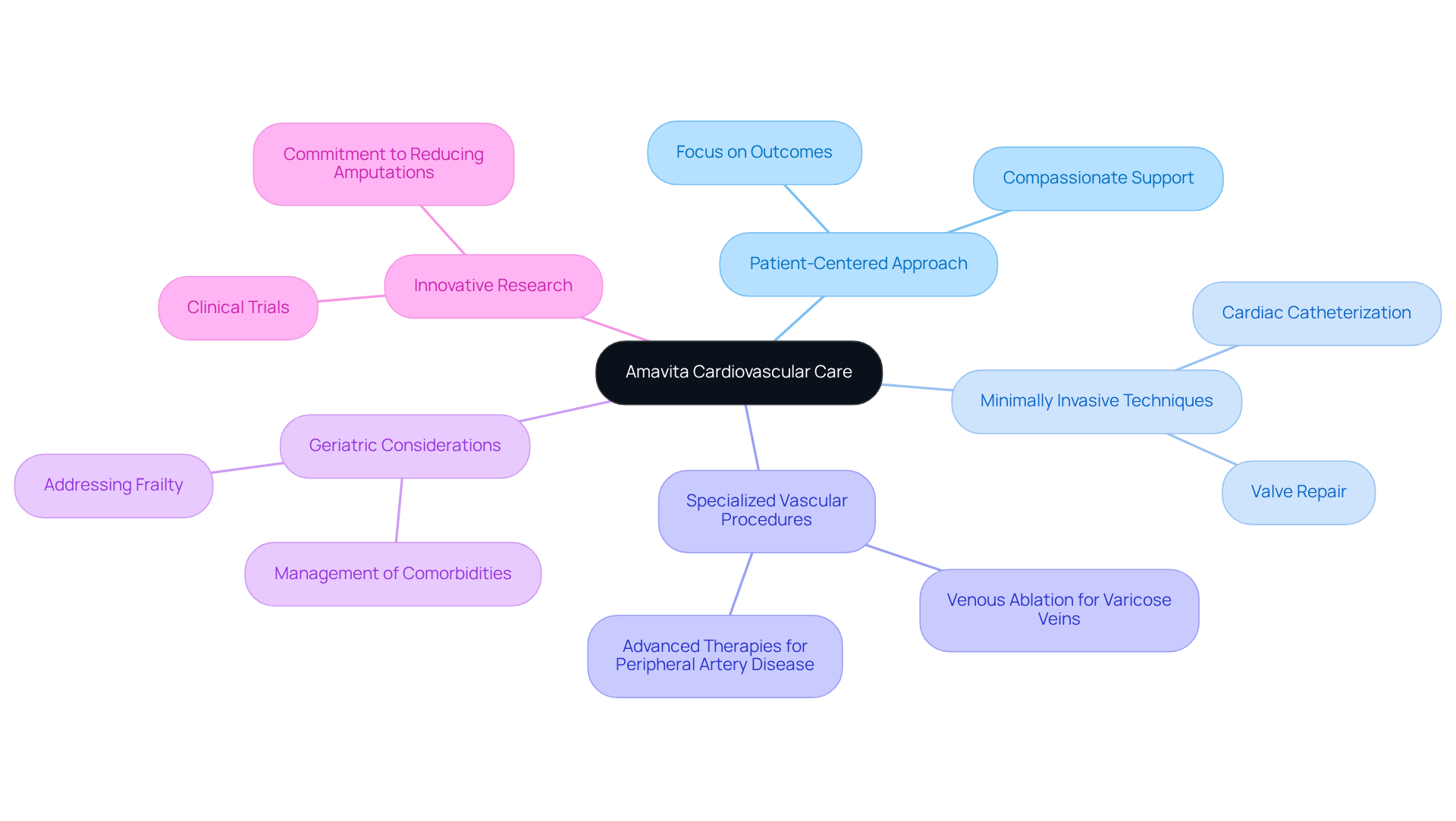
At Amavita Heart and Vascular Health, we understand how concerning these symptoms can be. That’s why we offer comprehensive arrhythmia management through our CardioElite™ program, which utilizes advanced treatments and innovative AI-powered diagnostic technology. This program not only allows for early detection but also empowers you to make informed choices, significantly improving outcomes for older adults.
Remember, being aware and acting quickly is key in managing a dangerous low heart rate. If you or a loved one are experiencing any symptoms, don’t hesitate to reach out for support. We’re here to help you navigate these challenges with care and compassion.
Identify Symptoms of Dangerously Low Heart Rate
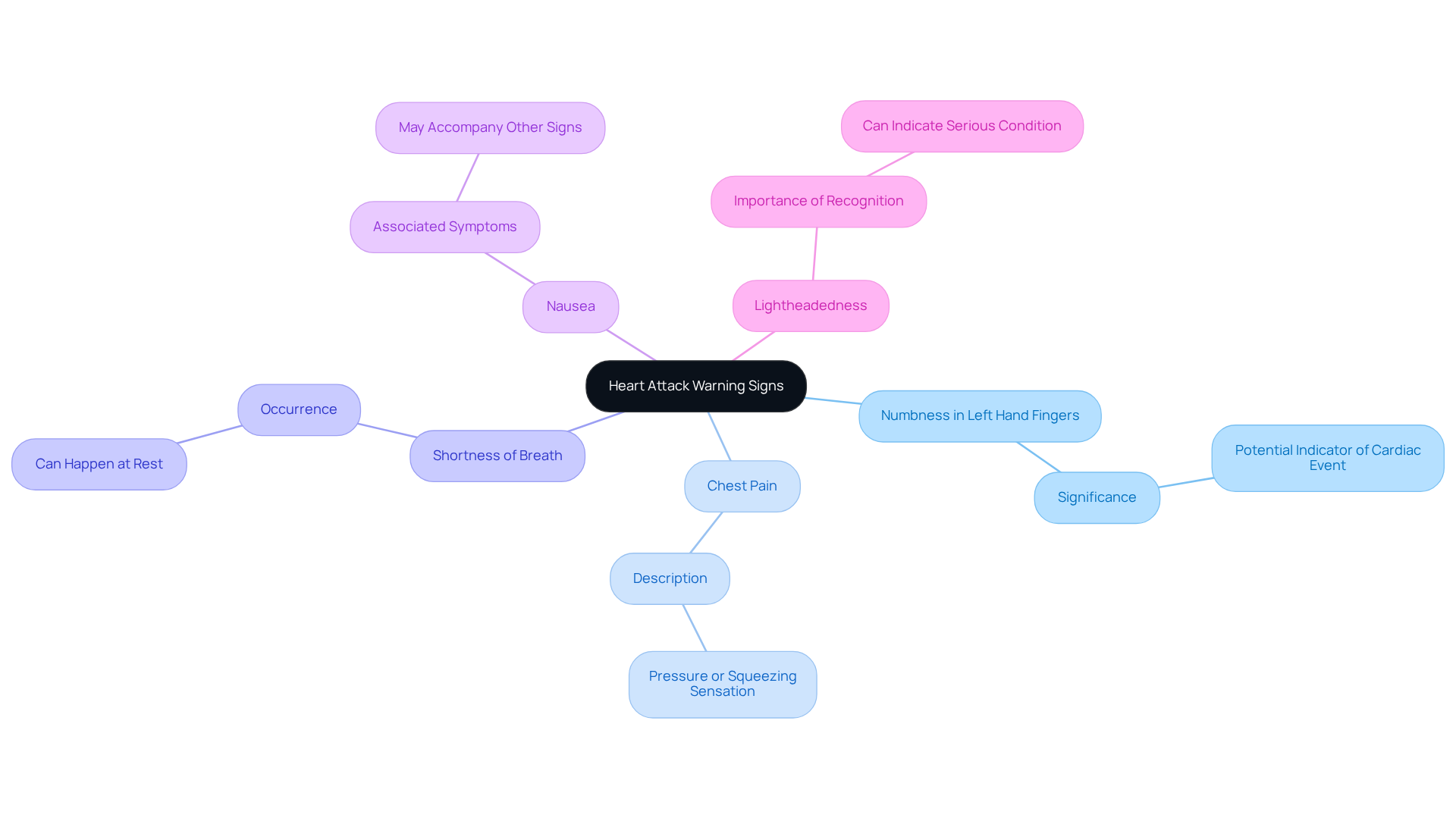
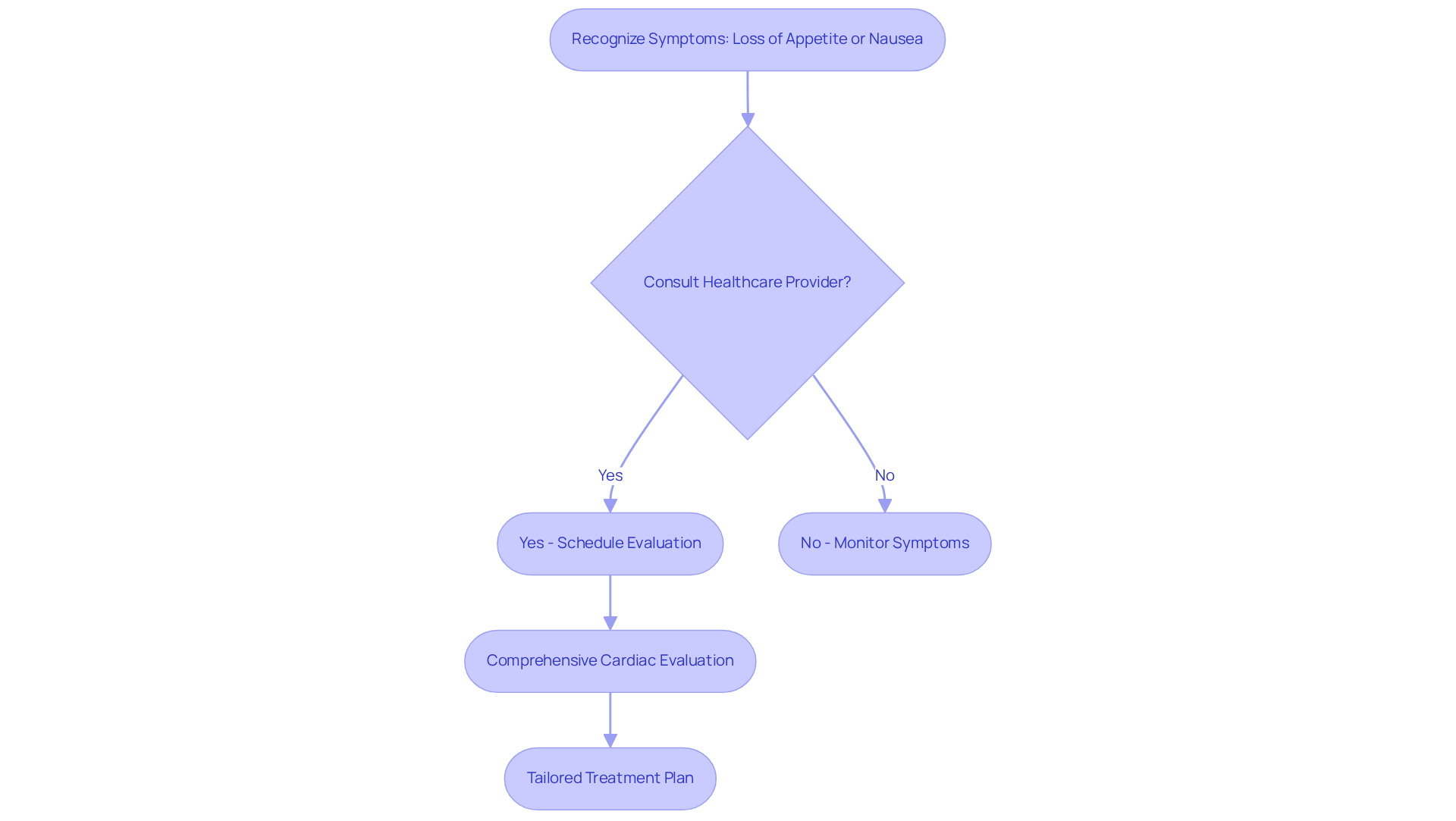
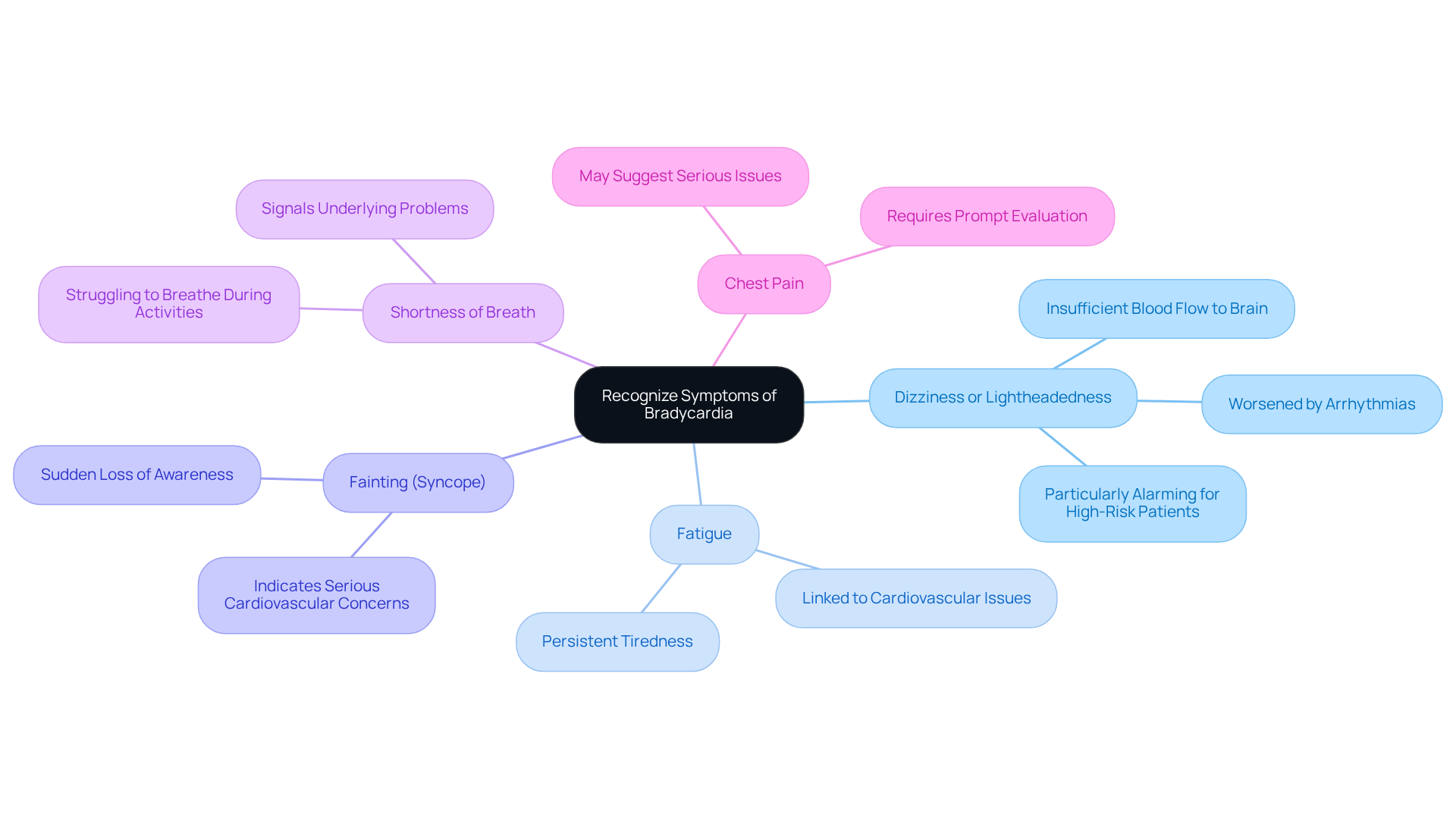
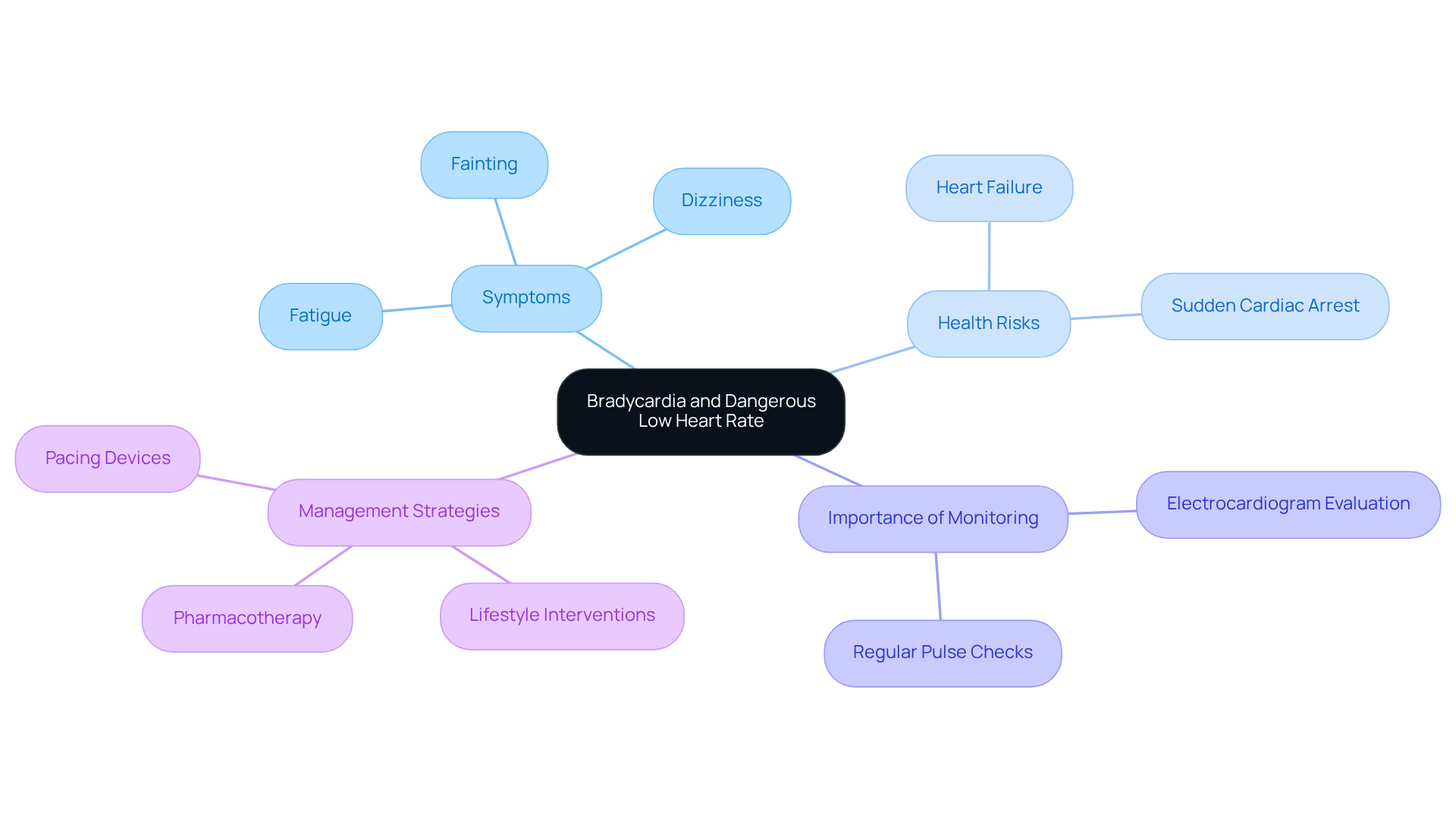
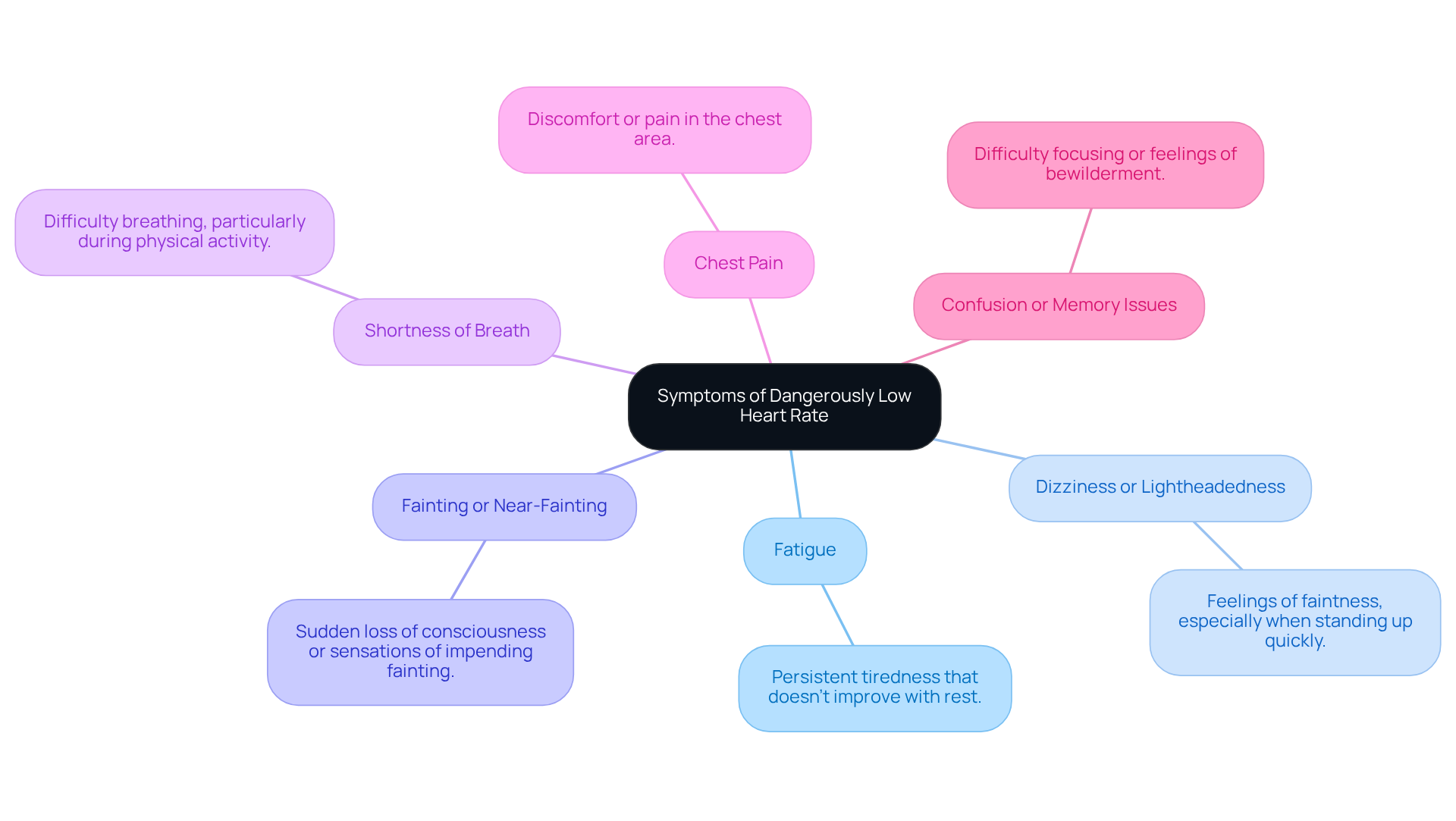
Common symptoms of a dangerous low heart rate can be concerning, especially for our elderly loved ones. Here are some signs to watch for:
- Fatigue: Persistent tiredness that doesn’t seem to improve with rest is often reported among seniors. This can indicate potential cardiovascular issues that deserve attention.
- Dizziness or Lightheadedness: Many older adults experience feelings of faintness, particularly when standing up quickly. This can be a sign of inadequate blood flow, which is important to address.
- Fainting or Near-Fainting: Sudden loss of consciousness or sensations of impending fainting are critical symptoms that require immediate attention. It’s vital to take these seriously.
- Shortness of Breath: Difficulty breathing, especially during physical activity, can suggest that the heart isn’t pumping effectively. This is something to discuss with a healthcare provider.
- Chest Pain: Discomfort or pain in the chest area may accompany low heart rates and should never be ignored. It’s always better to be safe and seek help.
- Confusion or Memory Issues: Difficulty focusing or feelings of bewilderment can indicate inadequate blood circulation to the brain, which is a significant concern for older adults.
Recognizing these signs is essential for older adults and their families. Prompt medical care can help avert serious issues linked to a dangerous low heart rate. If you notice any of these symptoms, please don’t hesitate to reach out for support. Your health and well-being are important, and there are caring professionals ready to help.
Explore Causes of Dangerously Low Heart Rate
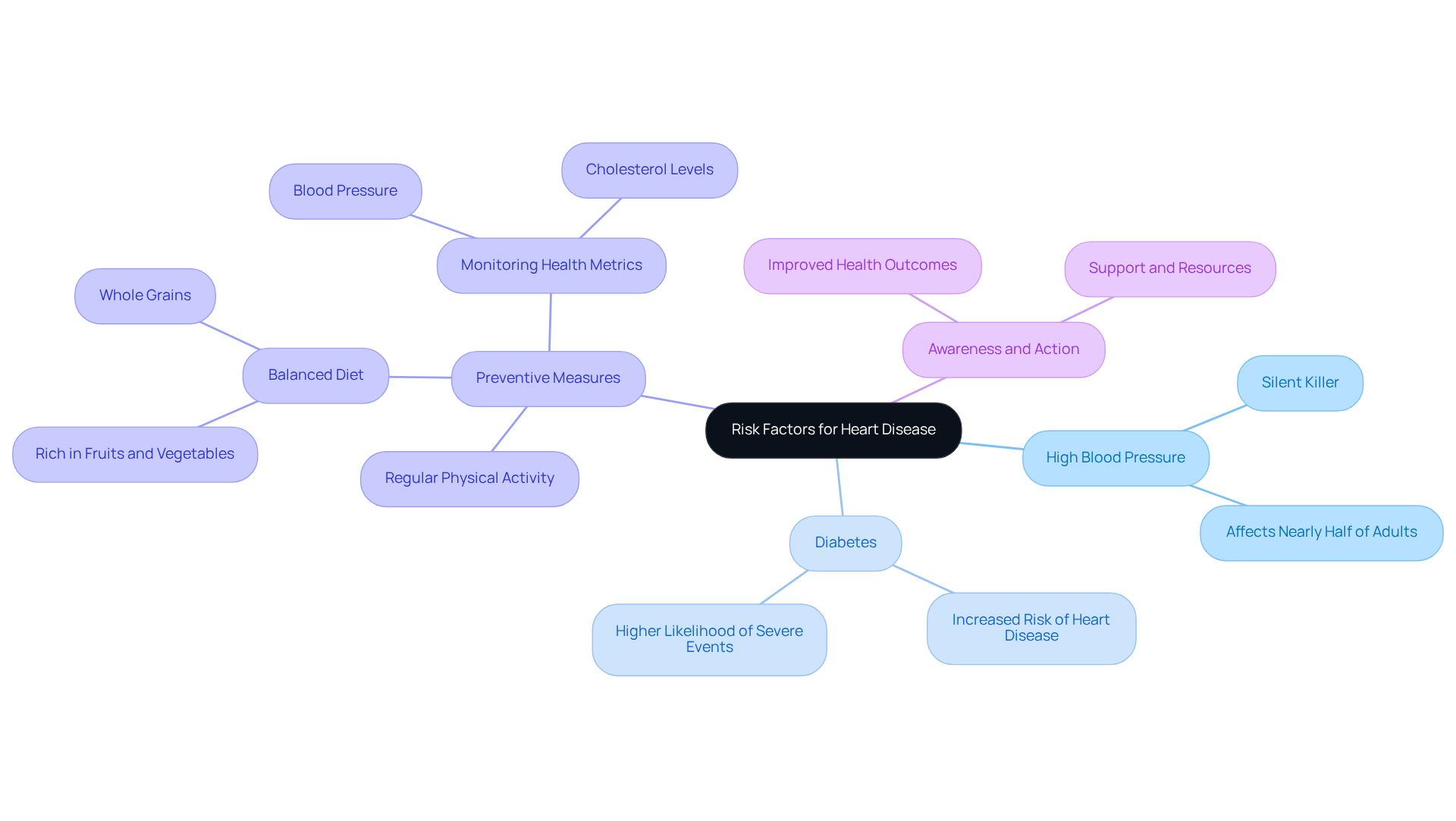
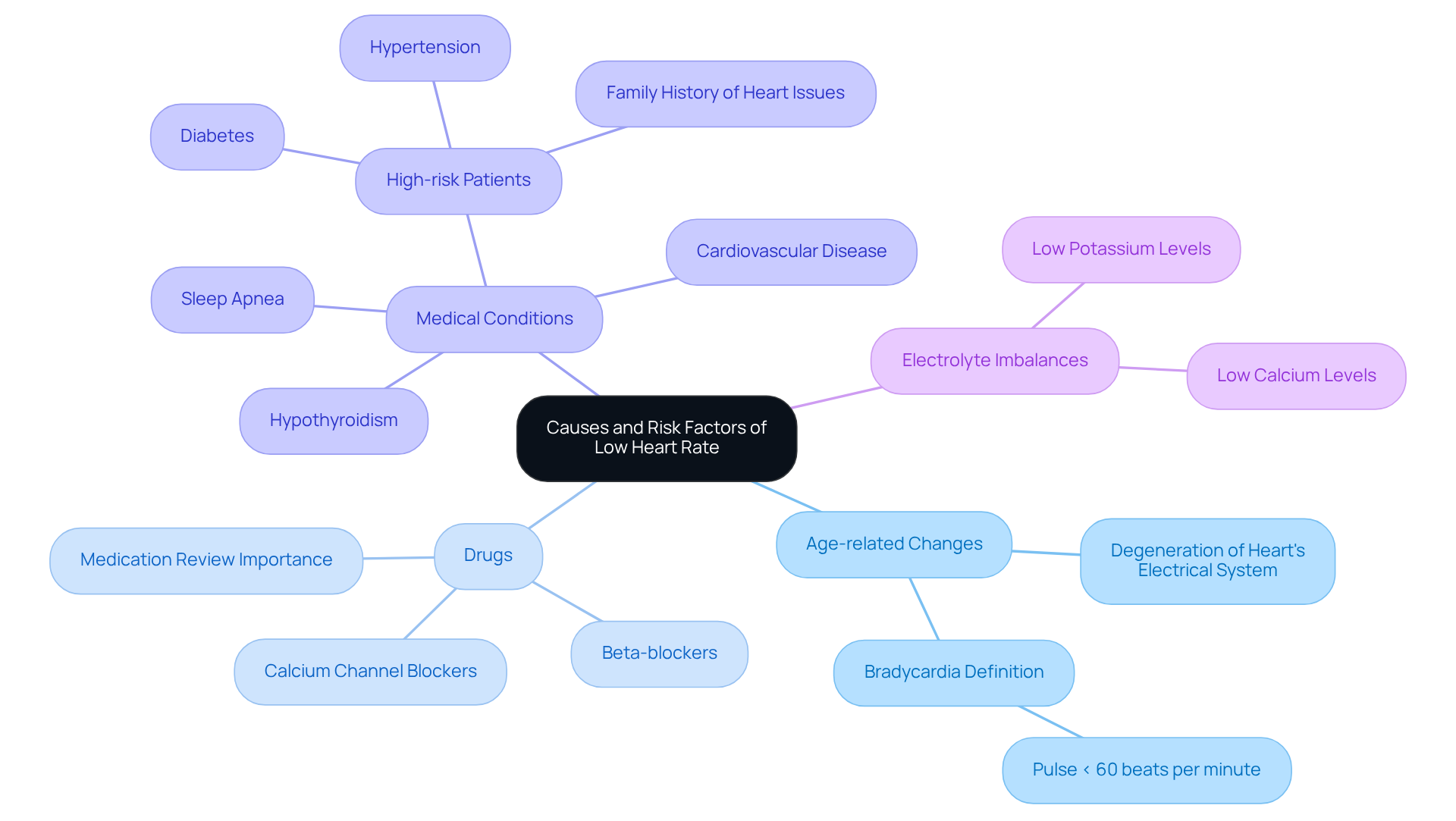
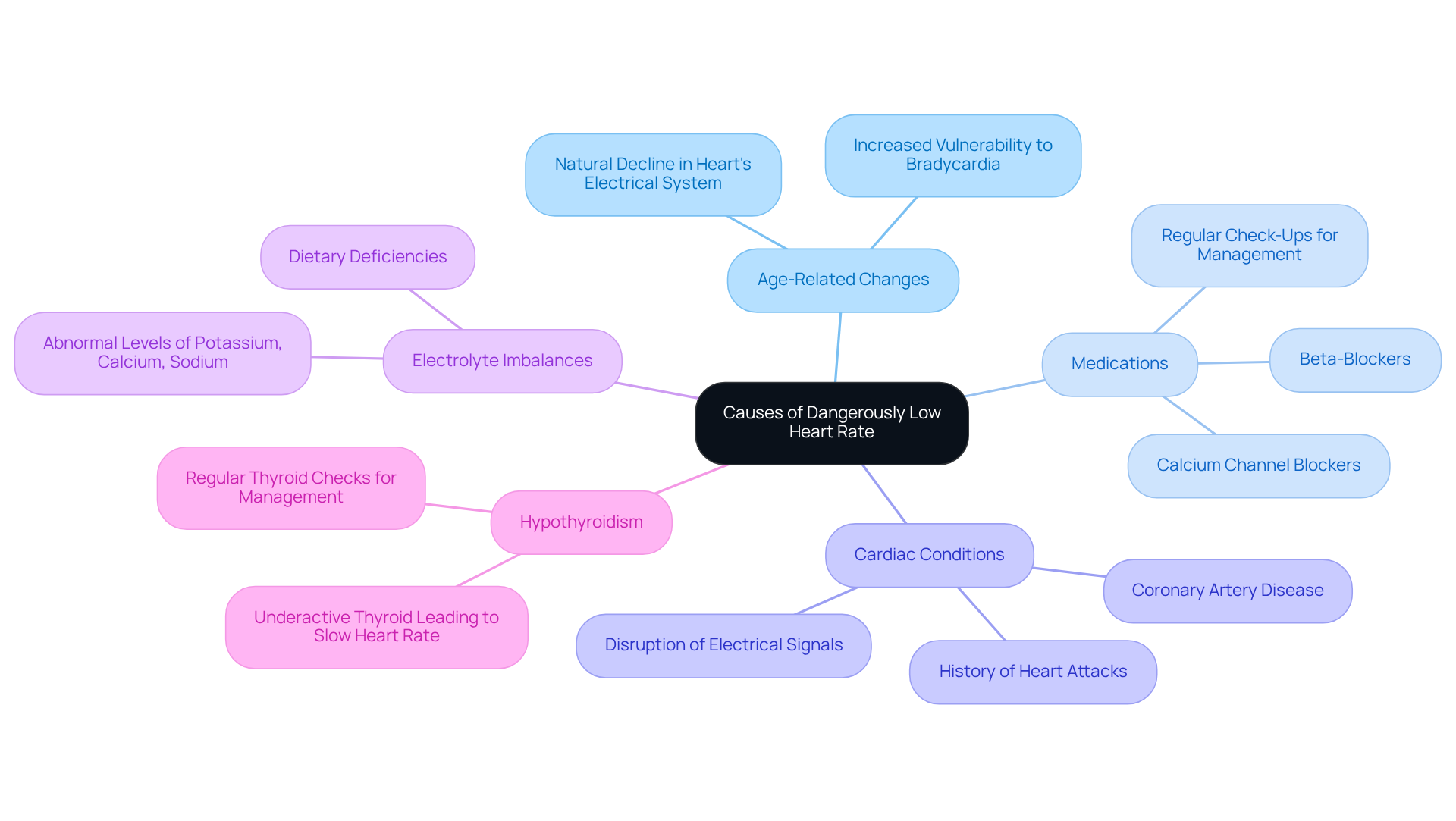
Several factors can contribute to a dangerous low heart rate in seniors, and understanding these can help you or your loved ones stay healthy and safe. Let’s explore some of these factors together:
- Age-Related Changes: As we age, our heart’s electrical system may change, leading to slower heart rates. This natural decline can make seniors more vulnerable to a dangerous low heart rate, characterized by fewer than 60 beats per minute. It’s important to be aware of this change and monitor heart health closely.
- Medications: Some medications, especially beta-blockers and calcium channel blockers, can lower pulse rates. While these are often prescribed for various heart issues, their side effects can lead to a dangerous low heart rate. Regular check-ups can help ensure that any changes are managed effectively.
- Cardiac Conditions: Existing heart conditions like coronary artery disease or a history of heart attacks can significantly affect heart rhythm. These issues may disrupt the normal electrical signals that control heartbeats, which can result in a dangerous low heart rate and increase the risk of bradycardia. If you have any concerns, discussing them with a healthcare provider can provide peace of mind.
- Electrolyte Imbalances: Abnormal levels of electrolytes, such as potassium, calcium, or sodium, can affect heart function. Seniors are particularly susceptible to these imbalances, which can stem from dietary deficiencies or certain health conditions. Keeping a balanced diet is crucial for heart health.
- Hypothyroidism: An underactive thyroid can lead to a slower heart rate, and this condition is more common in older adults. If left untreated, it can worsen the risk of a slow heart rate. Regular thyroid checks can help manage this risk effectively.
Understanding these causes is essential for seniors and caregivers alike. By being proactive about health, you can ensure timely medical intervention when necessary. Remember, you’re not alone in this journey-support is always available.
Understand Diagnostic Approaches for Low Heart Rate
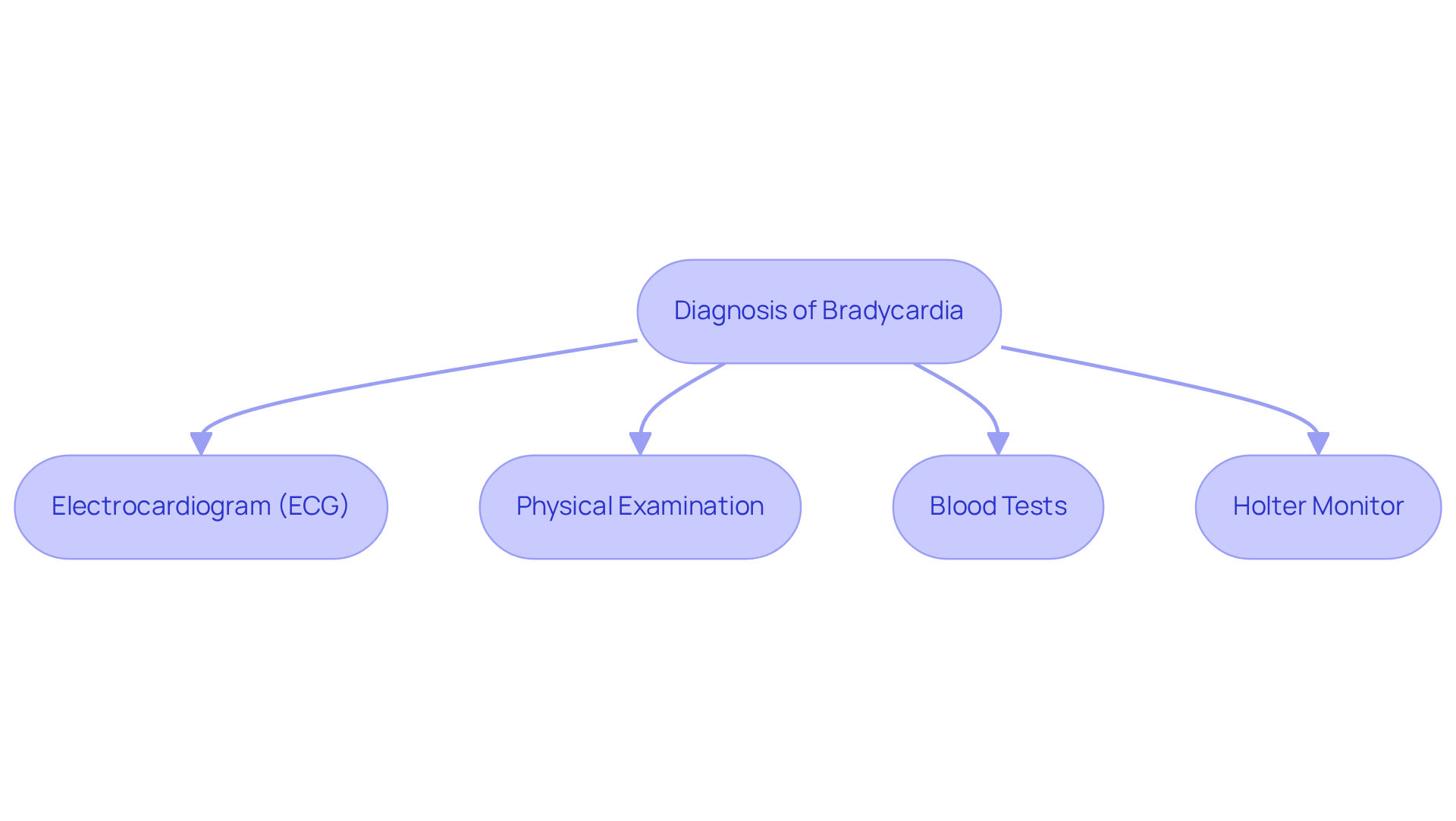
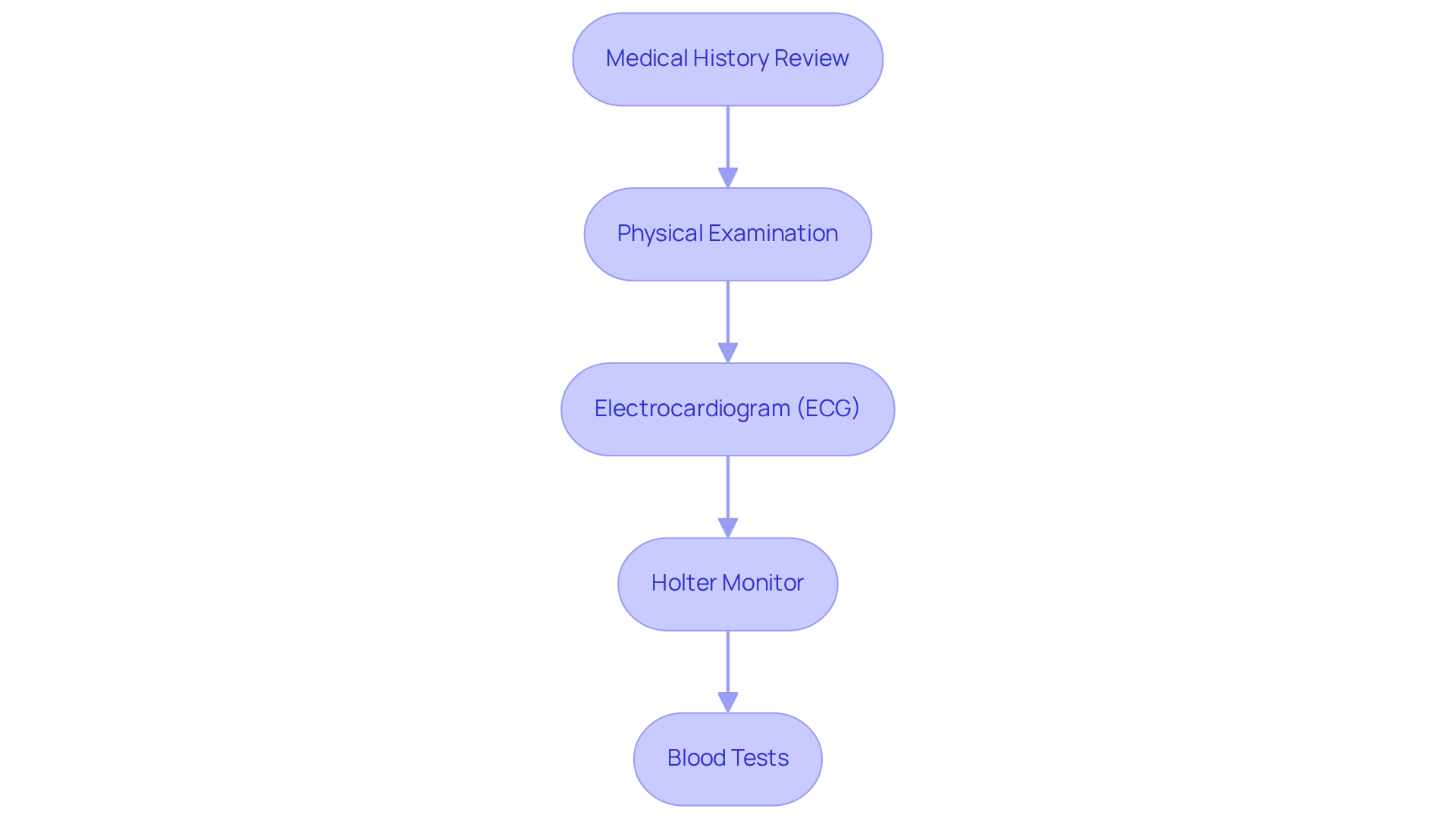
Diagnosing bradycardia can feel overwhelming, but understanding the process can bring peace of mind. Here’s a gentle overview of the key steps involved:
- Medical History Review: It all starts with a thorough discussion about your symptoms, medications, and overall health. This conversation is crucial as it helps identify potential causes of a dangerous low heart rate, like medication effects or underlying health conditions.
- Physical Examination: Your healthcare provider will check your pulse and blood pressure, which can reveal important insights about your heart’s health. For instance, the presence of cannon a-waves in the jugular venous pulse may indicate issues related to bradycardia.
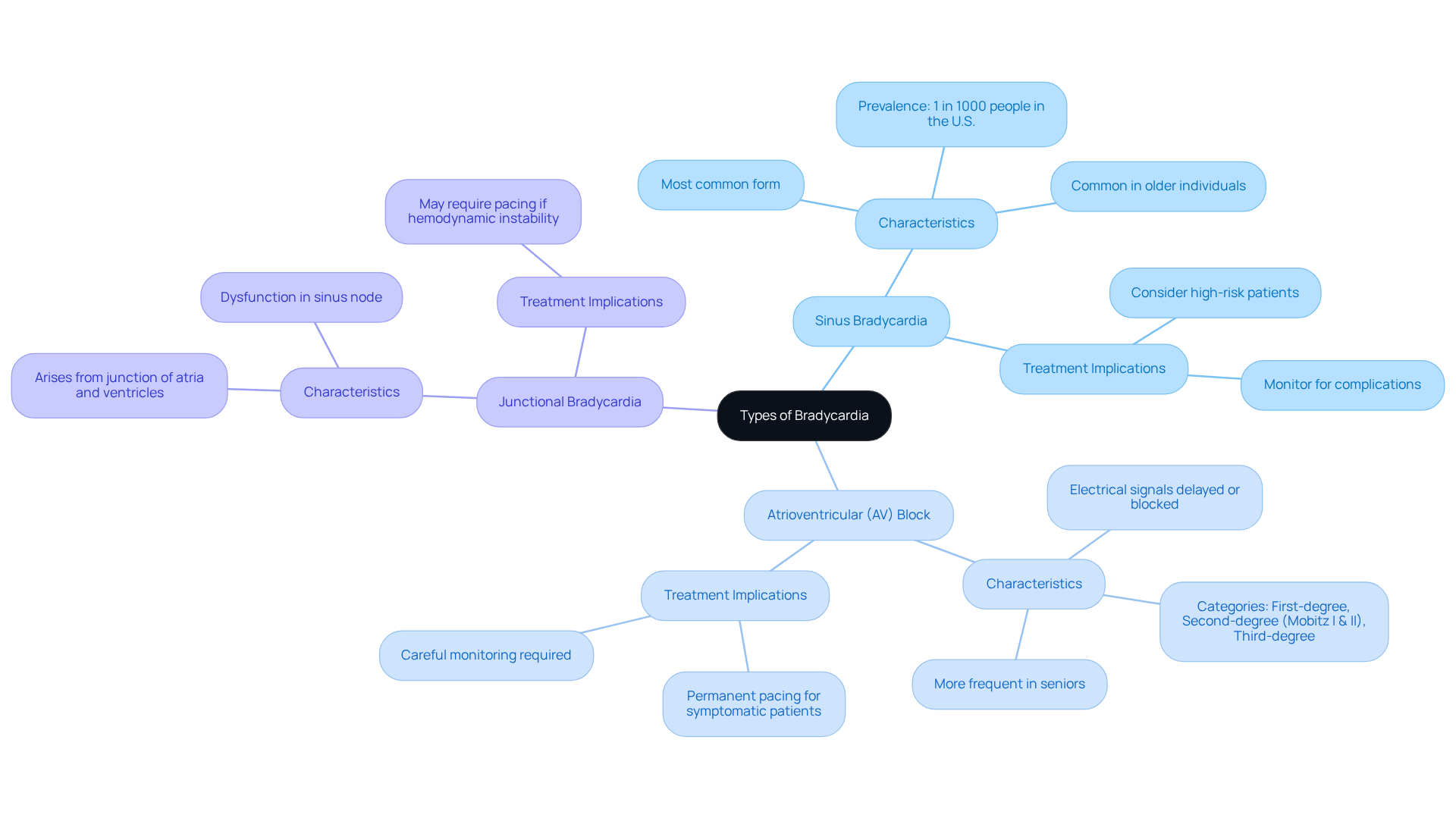
- Electrocardiogram (ECG): This essential test assesses your heart’s electrical activity, helping to identify a slow pulse. It can reveal specific rhythm abnormalities, such as sinus node dysfunction or atrioventricular (AV) block, which are common in older adults. It’s important to note that about one-third of patients with a dangerous low heart rate may experience syncope, underscoring the significance of ECG findings in symptomatic patients. At Amavita, our CardioElite™ program enhances this process with AI-powered diagnostics, offering real-time guidance and quick report generation to ensure timely interventions.
- Holter Monitor: This portable device is worn for 24 to 48 hours, continuously monitoring your pulse. It provides valuable data on fluctuations that might not be captured during a standard ECG.
- Blood Tests: These tests check for electrolyte imbalances and thyroid function, both of which can significantly impact your heart rate.
Together, these diagnostic tools empower healthcare providers to uncover the underlying causes of a dangerous low heart rate and tailor treatment options just for you. For example, in a study involving older patients with symptomatic slow heart rates, the ECG played a vital role in identifying the condition, leading to timely interventions that improved outcomes. The effectiveness of ECG in diagnosing low pulse frequencies in elderly patients highlights its importance in clinical practice, especially considering that about 6.2% of this demographic experiences symptomatic slow heartbeat.
With the support of Amavita’s innovative CardioElite™ program, we are committed to pioneering advancements in cardiovascular management. Our goal is to enhance early detection and improve your overall health outcomes, ensuring you feel supported every step of the way.
Review Treatment Options for Managing Low Heart Rate
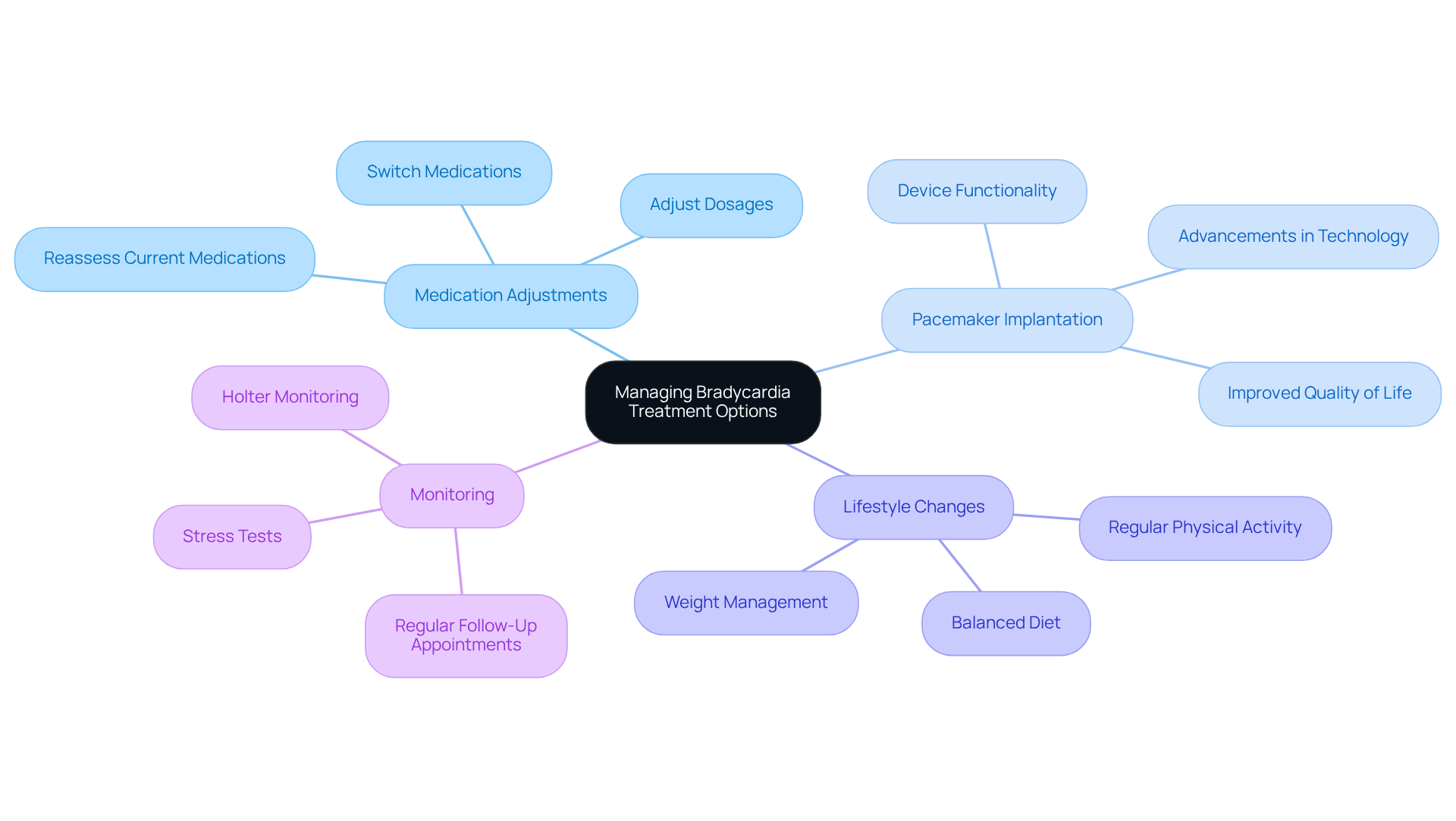
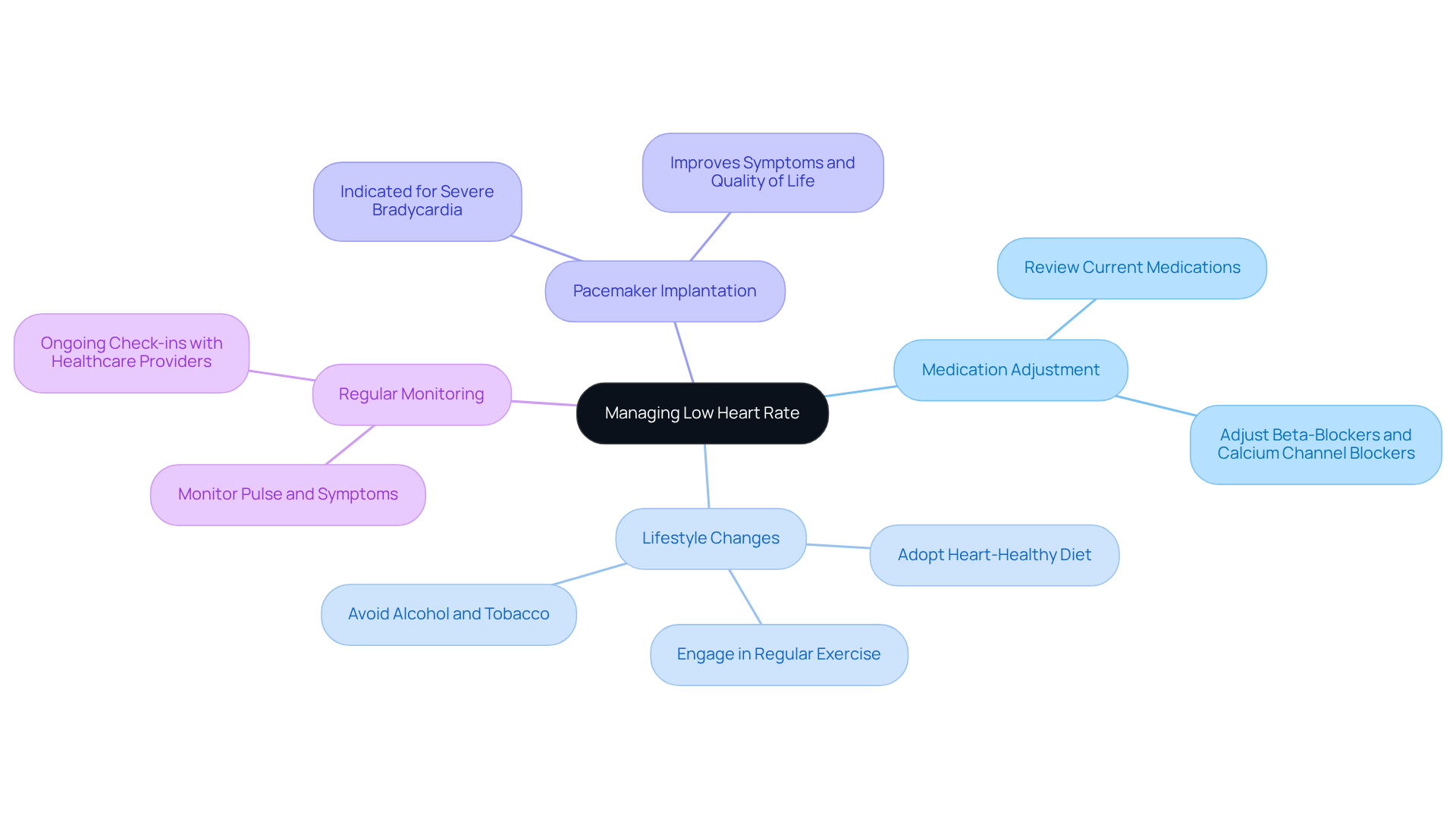
Managing bradycardia effectively requires a personalized approach that considers both the severity of the condition and its underlying causes. If you or a loved one is experiencing this, it’s important to know that there are several key treatment options available:
- Medication Adjustment: Have you reviewed your medications lately? It’s crucial to assess any drugs that might contribute to a low heart rate, such as beta-blockers or calcium channel blockers. Adjusting these can make a significant difference.
- Lifestyle Changes: Simple changes can lead to big improvements. Adopting a heart-healthy diet, engaging in regular exercise, and avoiding alcohol and tobacco can greatly enhance cardiac function. Studies show that lifestyle modifications can significantly boost cardiovascular health, especially for seniors.
- Pacemaker Implantation: For those facing significant bradycardia, a pacemaker might be necessary to maintain a healthy pulse. This small device sends electrical signals to the heart, ensuring it beats at a suitable pace. Many patients find that this can greatly improve their symptoms and overall quality of life.
- Regular Monitoring: Ongoing check-ins with healthcare providers are essential. Regular monitoring of your pulse and symptoms allows for timely adjustments to your treatment plan, ensuring you receive the best care possible.
Together, these approaches aim to enhance cardiac function and improve the quality of life for older adults. It’s important to address the specific challenges that come with a dangerous low heart rate, and remember, you’re not alone in this journey. Seeking support and guidance can make all the difference.
Implement Preventive Strategies Against Low Heart Rate
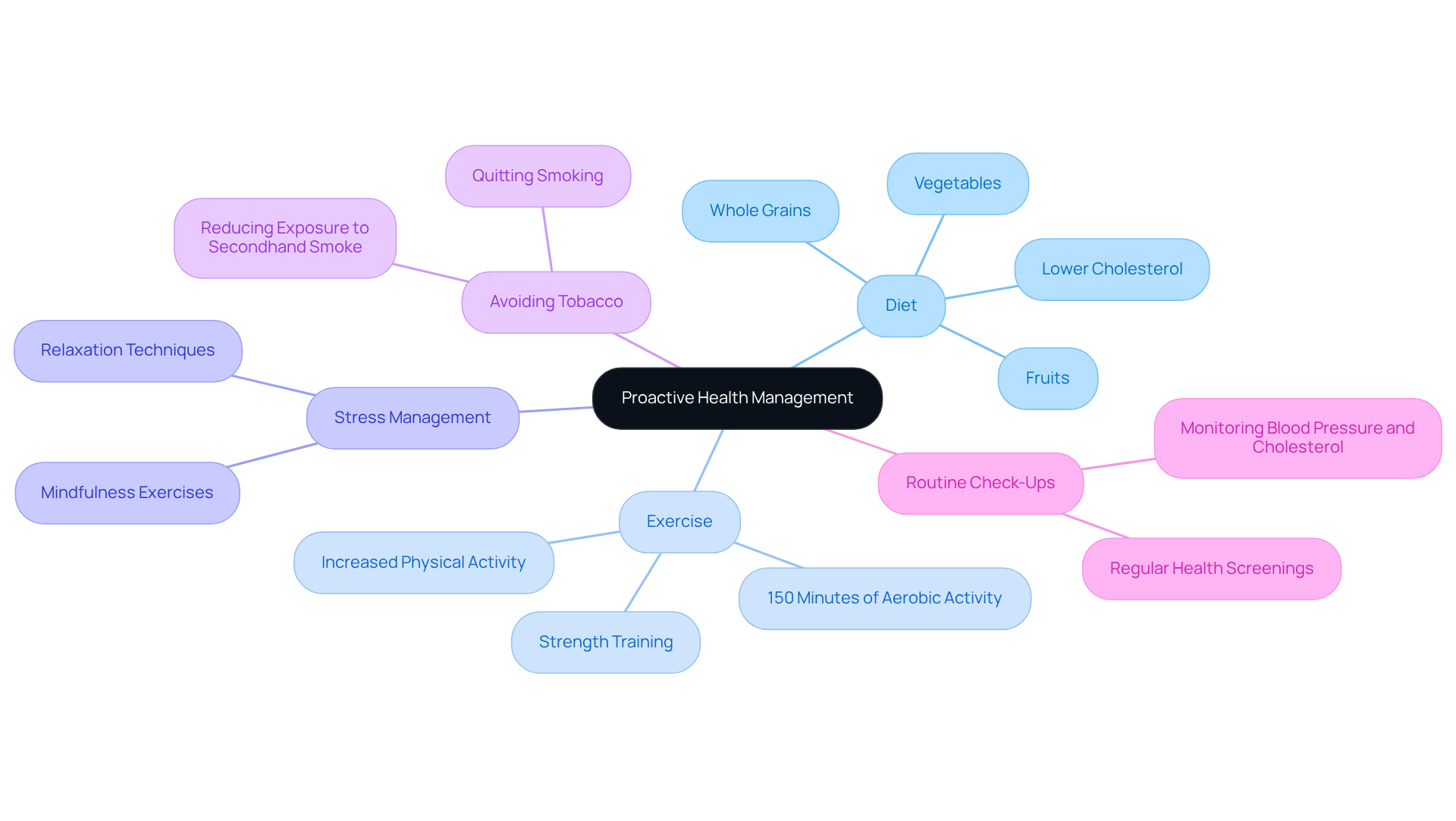
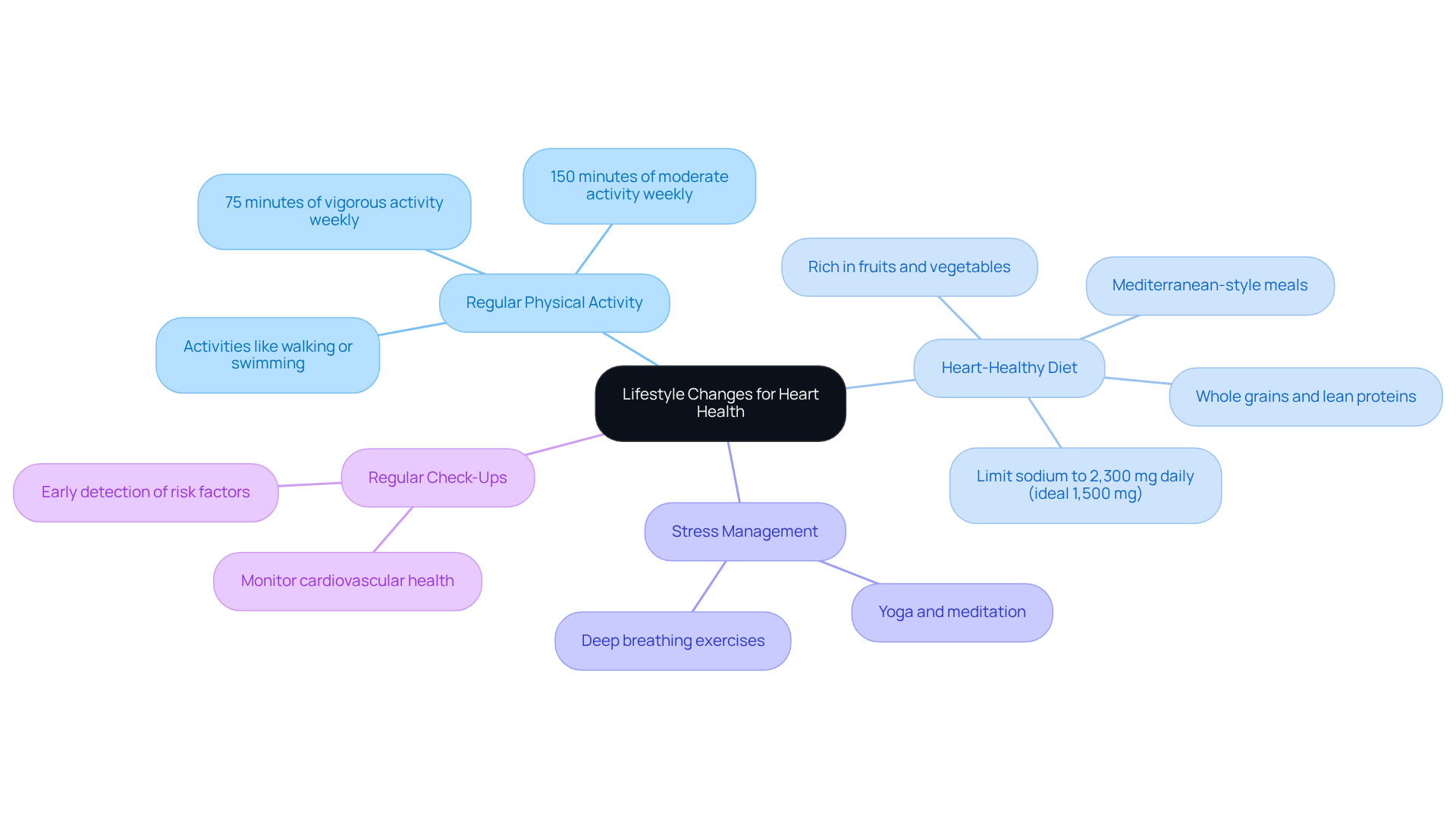
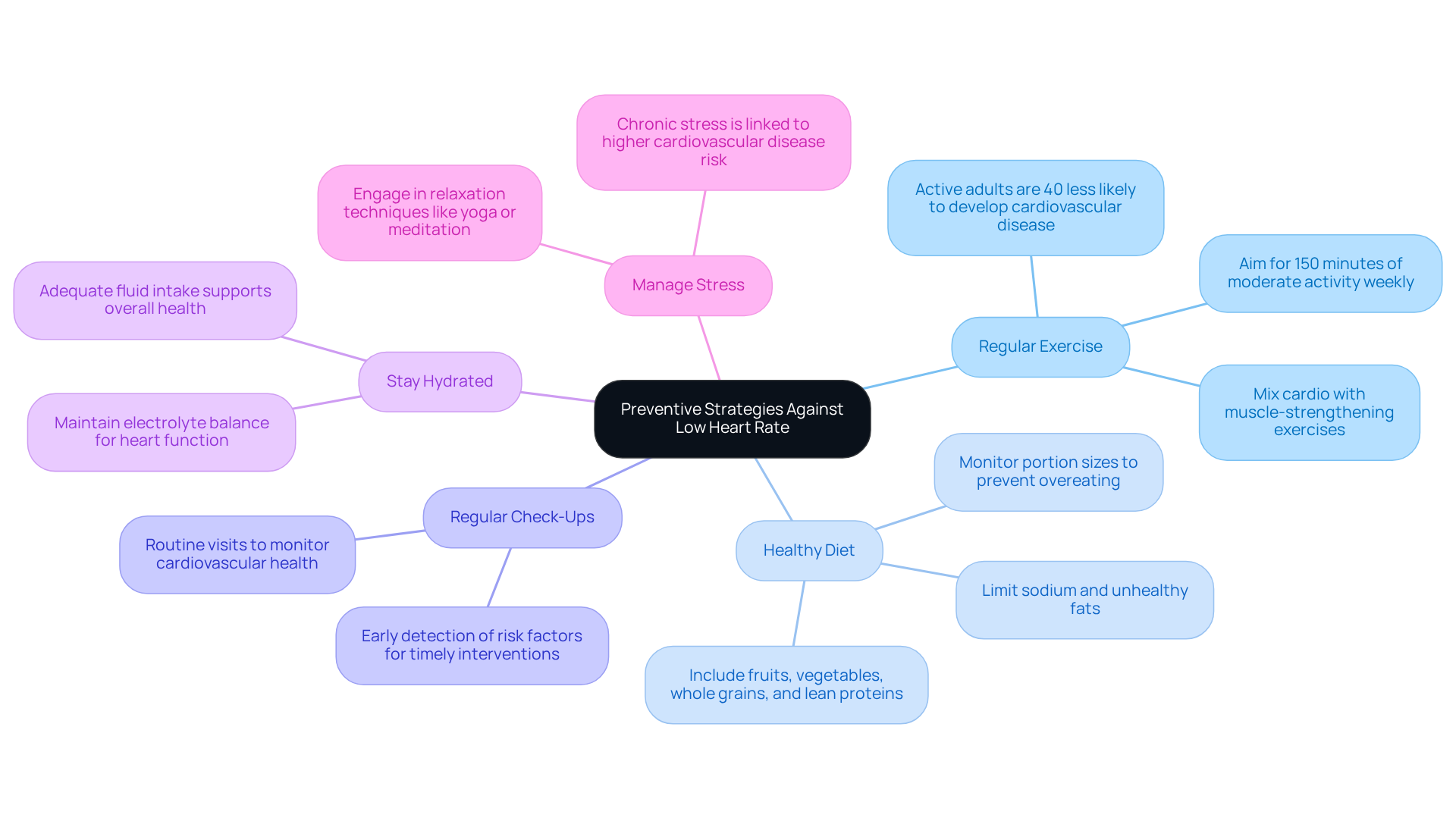
Caring for your heart is essential, especially as we age. Here are some gentle strategies to help maintain a healthy heart rate:
- Regular Exercise: Aim for at least 150 minutes of moderate-intensity physical activity each week. This isn’t just about staying fit; it’s about strengthening your heart. Did you know that active adults can be up to 40% less likely to develop cardiovascular disease or have a stroke? That’s a significant reduction in the risk of serious heart issues.
- Healthy Diet: Nourishing your body with a balanced diet filled with fruits, vegetables, whole grains, and lean proteins is vital. By limiting sodium and unhealthy fats, you can help regulate your blood pressure and cholesterol levels, both crucial for your heart health.
- Regular Check-Ups: Don’t underestimate the power of routine visits to your healthcare provider. These check-ups allow for monitoring your cardiovascular health and adjusting medications if needed. Early detection of any risk factors can lead to timely interventions, ultimately improving your health outcomes.
- Stay Hydrated: Keeping yourself well-hydrated is key. Adequate fluid intake helps maintain electrolyte balance, which can influence your pulse rate and overall heart function.
- Manage Stress: Stress can take a toll on your heart. Engaging in relaxation techniques like yoga or meditation can significantly lower your stress levels. Remember, chronic stress is linked to a higher risk of cardiovascular disease, so finding ways to manage it is essential for your heart health.
By embracing these strategies, you can reduce the risks associated with a dangerous low heart rate and enhance your overall cardiovascular well-being. Remember, you’re not alone on this journey; support is always available.
Conclusion
Bradycardia, or a dangerously low heart rate, is a serious health concern for seniors that truly deserves our attention and care. Understanding what this condition means is vital for both individuals and their caregivers. Recognizing the symptoms and acting quickly can help prevent serious complications. We can’t stress enough how important it is to monitor heart rates, especially for older adults who may face unique health challenges.
In this article, we’ve shared important insights about the symptoms, causes, diagnostic approaches, treatment options, and preventive strategies related to low heart rates in seniors. From noticing signs of fatigue and dizziness to understanding how medications and lifestyle choices play a role, each aspect is crucial for maintaining cardiovascular health. Regular check-ups and consultations with healthcare providers can lead to early detection and personalized treatment plans, which can significantly improve outcomes.
Ultimately, managing a dangerously low heart rate isn’t just about addressing a medical issue; it’s about enhancing the quality of life for seniors. By staying informed and proactive, individuals and their families can navigate the complexities of heart health together. Embracing a heart-healthy lifestyle and seeking support when needed can empower seniors to lead fulfilling lives while minimizing the risks associated with bradycardia. Remember, you’re not alone in this journey; support is always available.
Frequently Asked Questions
What is considered a dangerous low heart rate?
A dangerous low heart rate, known as bradycardia, is defined as a resting pulse rate of fewer than 60 beats per minute (BPM).
Why is a dangerous low heart rate particularly concerning for seniors?
For seniors, a dangerous low heart rate can pose significant health risks due to age-related changes in heart function and the potential for underlying health issues.
What symptoms might indicate a dangerously low heart rate?
Common symptoms include fatigue, dizziness or lightheadedness, fainting or near-fainting, shortness of breath, chest pain, and confusion or memory issues.
What should caregivers and patients do if they recognize symptoms of bradycardia?
It is essential to seek medical help if symptoms of bradycardia are observed, as prompt medical care can help prevent serious complications.
How can bradycardia be diagnosed?
A thorough evaluation for bradycardia often includes an electrocardiogram (ECG) to confirm the diagnosis, especially when pulse rates drop below 50 BPM.
What are the potential complications of untreated bradycardia?
If left undiagnosed and untreated, bradycardia can lead to serious complications, including heart failure and sudden cardiac arrest.
What services does Amavita Heart and Vascular Health offer for managing bradycardia?
Amavita Heart and Vascular Health offers comprehensive arrhythmia management through their CardioElite™ program, which utilizes advanced treatments and AI-powered diagnostic technology for early detection and informed choices.
What is the importance of regular pulse monitoring for seniors?
Regular pulse monitoring is vital for early detection and management of bradycardia, helping to identify potential issues before they lead to serious complications.
List of Sources
- Define Dangerous Low Heart Rate and Its Importance for Seniors
- hrsonline.org (https://hrsonline.org/news/societies-publish-new-guidance-treatment-slow-irregular-heartbeats)
- thecardiologyadvisor.com (https://thecardiologyadvisor.com/ddi/bradycardia)
- Study: New heart rhythm measure signals risk of cognitive decline in older adults (https://mcknights.com/news/study-new-heart-rhythm-measure-signals-risk-of-cognitive-decline-in-older-adults)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC10689927)
- Tracking heart rate for seniors: Here’s why it’s beneficial (https://care.com/c/why-seniors-should-measure-heart-rate)
- Identify Symptoms of Dangerously Low Heart Rate
- Bradycardia – Symptoms and causes (https://mayoclinic.org/diseases-conditions/bradycardia/symptoms-causes/syc-20355474)
- thecardiologyadvisor.com (https://thecardiologyadvisor.com/ddi/bradycardia)
- Bradycardia: Causes, Symptoms & Treatment | Tampa General Hospital (https://tgh.org/institutes-and-services/conditions/bradycardia-slow-heart-rate)
- my.clevelandclinic.org (https://my.clevelandclinic.org/health/diseases/17841-bradycardia)
- 8 Signs of Bradycardia to Take Seriously (https://phoenixheart.com/8-signs-of-bradycardia-to-take-seriously)
- Explore Causes of Dangerously Low Heart Rate
- Bradycardia – Symptoms and causes (https://mayoclinic.org/diseases-conditions/bradycardia/symptoms-causes/syc-20355474)
- Bradycardia: Causes, Symptoms & Treatment | Tampa General Hospital (https://tgh.org/institutes-and-services/conditions/bradycardia-slow-heart-rate)
- my.clevelandclinic.org (https://my.clevelandclinic.org/health/diseases/17841-bradycardia)
- Bradycardia: Slow Heart Rate (https://heart.org/en/health-topics/arrhythmia/about-arrhythmia/bradycardia–slow-heart-rate)
- What Can Cause a Low Heart Rate? Key Insights for Seniors (https://amavita.health/blog/what-can-cause-a-low-heart-rate-key-insights-for-seniors)
- Understand Diagnostic Approaches for Low Heart Rate
- hrsonline.org (https://hrsonline.org/news/societies-publish-new-guidance-treatment-slow-irregular-heartbeats)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC10689927)
- Bradycardia – Symptoms, diagnosis and treatment | BMJ Best Practice US (https://bestpractice.bmj.com/topics/en-gb/832)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9021000)
- mayoclinic.org (https://mayoclinic.org/diseases-conditions/bradycardia/diagnosis-treatment/drc-20355480)
- Review Treatment Options for Managing Low Heart Rate
- Significance of Asymptomatic Bradycardia for Subsequent Pacemaker Implantation and Mortality in Patients >60 Years of Age (https://sciencedirect.com/science/article/abs/pii/S0002914911017802)
- Understanding Treatment for Low Heart Rate: A Guide for Seniors (https://amavita.health/blog/understanding-treatment-for-low-heart-rate-a-guide-for-seniors)
- Long-Term Incidence of Bradycardia and Pacemaker Implantations Among Cross-Country Skiers: A Cohort Study | Circulation (https://ahajournals.org/doi/10.1161/CIRCULATIONAHA.123.068280)
- hrsonline.org (https://hrsonline.org/news/societies-publish-new-guidance-treatment-slow-irregular-heartbeats)
- Implement Preventive Strategies Against Low Heart Rate
- Physical Activity Benefits for Adults 65 or Older (https://cdc.gov/physical-activity-basics/health-benefits/older-adults.html)
- Flagship Health | Cardiovascular Disease Prevention for Seniors (https://flagshiphealth.org/resources/blog/cardiovascular-disease-prevention-for-seniors)
- Prevention (https://heart.org/en/news/prevention)
- Heart Benefits of Moving More | CardioSmart – American College of Cardiology (https://cardiosmart.org/topics/healthy-living/move-more/exercise-and-heart-health)
- Massive study uncovers how much exercise is needed to live longer (https://ama-assn.org/public-health/prevention-wellness/massive-study-uncovers-how-much-exercise-needed-live-longer)