Introduction
Recognizing the signs of a heart attack can truly be a matter of life and death. Yet, many people may not be aware of the subtle symptoms that could signal danger. In this article, we’ll explore the critical warning signs that might indicate a heart attack, paying special attention to how these symptoms can differ between genders. It’s essential to understand these signs, particularly for women, who often experience atypical symptoms that can be easily overlooked.
Have you ever wondered what happens when these warning signs are misinterpreted or ignored? The stakes are high, and being informed could be the key to ensuring timely medical intervention and potentially saving a life. Remember, you’re not alone in this; understanding these signs can empower you to take action when it matters most.
Chest Pain or Discomfort
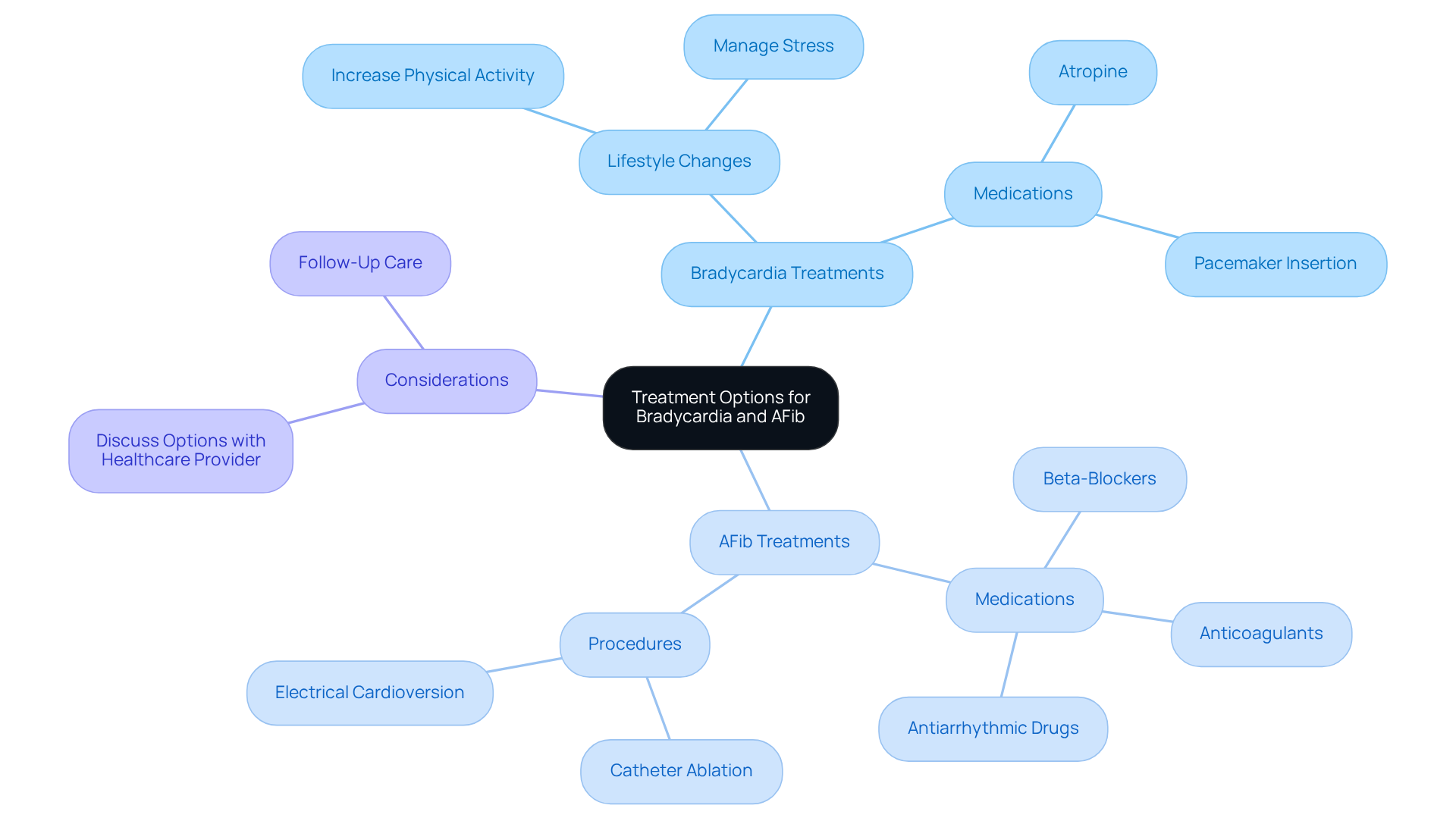
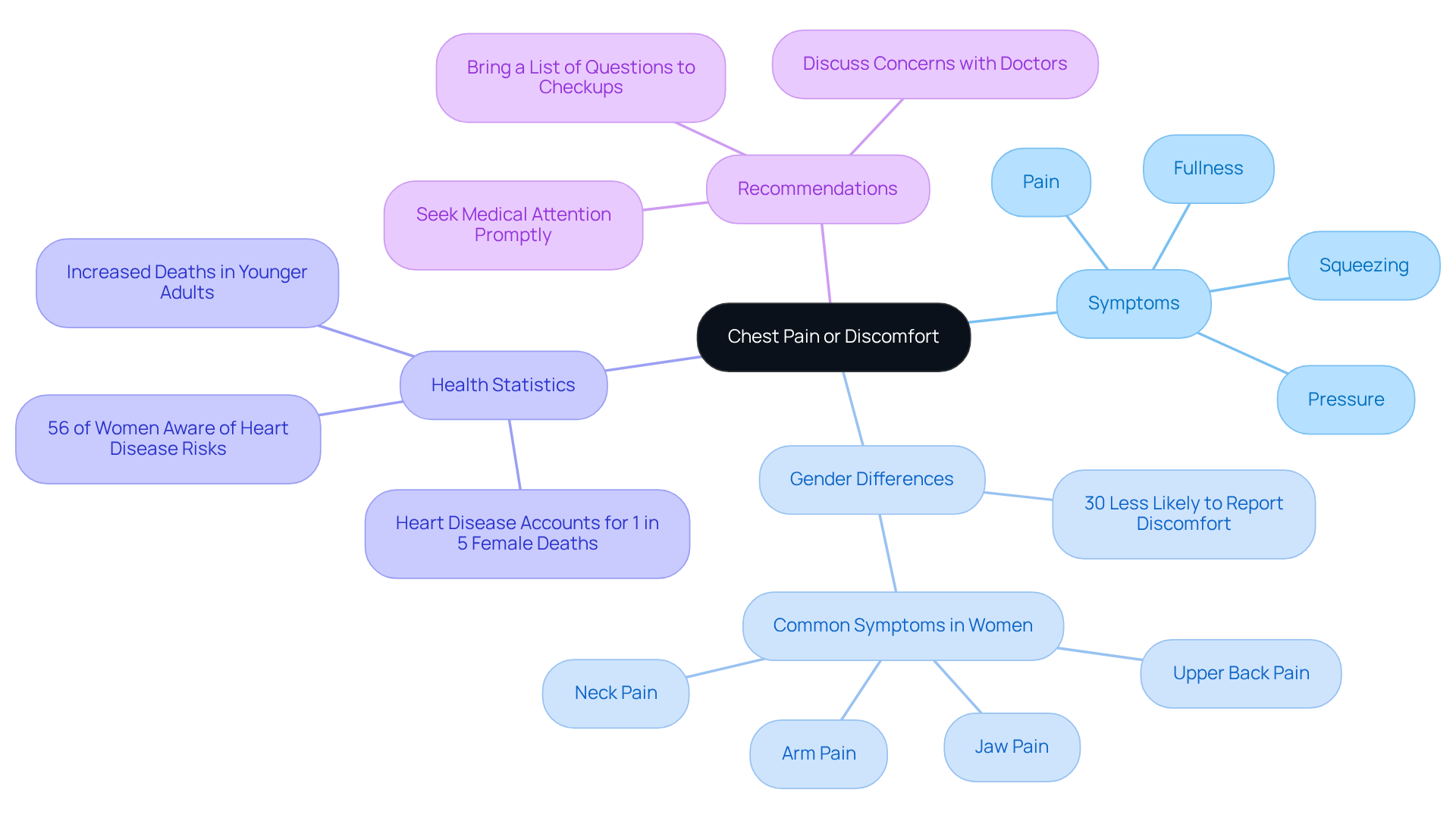
Chest pain or discomfort often feels like pressure, squeezing, fullness, or pain in the center or left side of the chest. This sensation can linger for several minutes or come and go. It’s important to recognize that the intensity of this symptom can vary widely and isn’t always severe. Many women and older adults might mistake this discomfort for heartburn or indigestion, which can lead to misunderstandings about their symptoms.
Did you know that studies show women are 30% less likely than men to report chest discomfort during a cardiac event? This highlights the need for everyone to understand that signs of a heart issue can manifest differently. In fact, women often experience discomfort in the upper back, arms, neck, and jaw, and they frequently report a range of symptoms compared to men. Heart disease is a significant health threat for women, accounting for one in five female deaths in the U.S. in 2023. If you experience any type of chest discomfort, it’s crucial to seek medical attention promptly, as this symptom is among the signs you may have a heart attack.
At Amavita Heart and Vascular Health®, our cardiologists emphasize the importance of being aware of the signs you may have a heart attack, particularly for women who may downplay their experiences out of fear of being seen as overreacting. We offer thorough cardiac assessments, along with lifestyle changes and preventive measures for high-risk patients, ensuring that all symptoms are properly evaluated. This approach facilitates accurate diagnosis and tailored treatment plans.
We encourage women to openly discuss their cardiovascular concerns with their doctors and to bring a list of questions to their medical checkups. Understanding these nuances can significantly impact timely diagnosis and treatment. Remember, you’re not alone in this journey, and we’re here to support you every step of the way.
Unusual Symptoms in Women
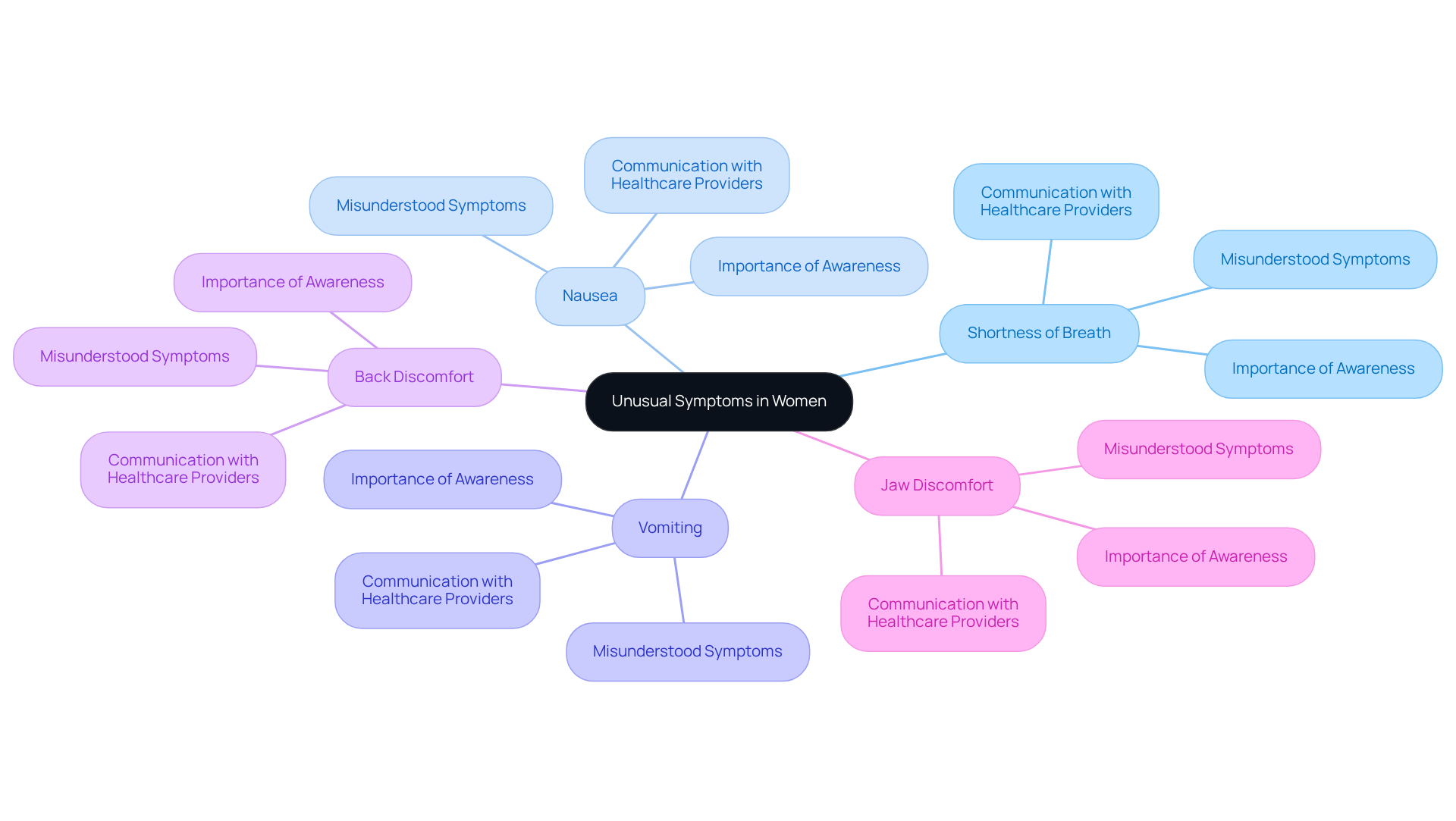
Women often exhibit unique signs you may have a heart attack, including shortness of breath, nausea, vomiting, and discomfort in the back or jaw. Unfortunately, these symptoms can be misunderstood as other health issues, leading to delays in receiving the care they need. Many women might describe signs you may have a heart attack as feelings of exhaustion or unease instead of the more commonly recognized chest discomfort. This misunderstanding can result in misdiagnosis and inadequate care.
Dr. Stacey Rosen highlights the importance of women being aware of these distinct symptoms and communicating them clearly to healthcare providers. It’s crucial to raise awareness to ensure timely medical intervention, as delays can worsen cardiovascular conditions. Did you know that studies show women are 30% less likely than men to report chest pain during a heart attack? They often describe their experience as discomfort rather than pain. This tendency emphasizes the need for tailored medical evaluations for women, as recognizing the signs you may have a heart attack can significantly improve outcomes.
At Amavita, the CardioElite™ program is dedicated to enhancing cardiac care by offering comprehensive evaluations and advanced imaging capabilities, especially for high-risk patients. For instance, the program has successfully identified unusual signs in women, leading to timely interventions that have improved patient outcomes. Cardiovascular disease remains the leading cause of death for women in the U.S., making it essential to recognize the signs you may have a heart attack early.
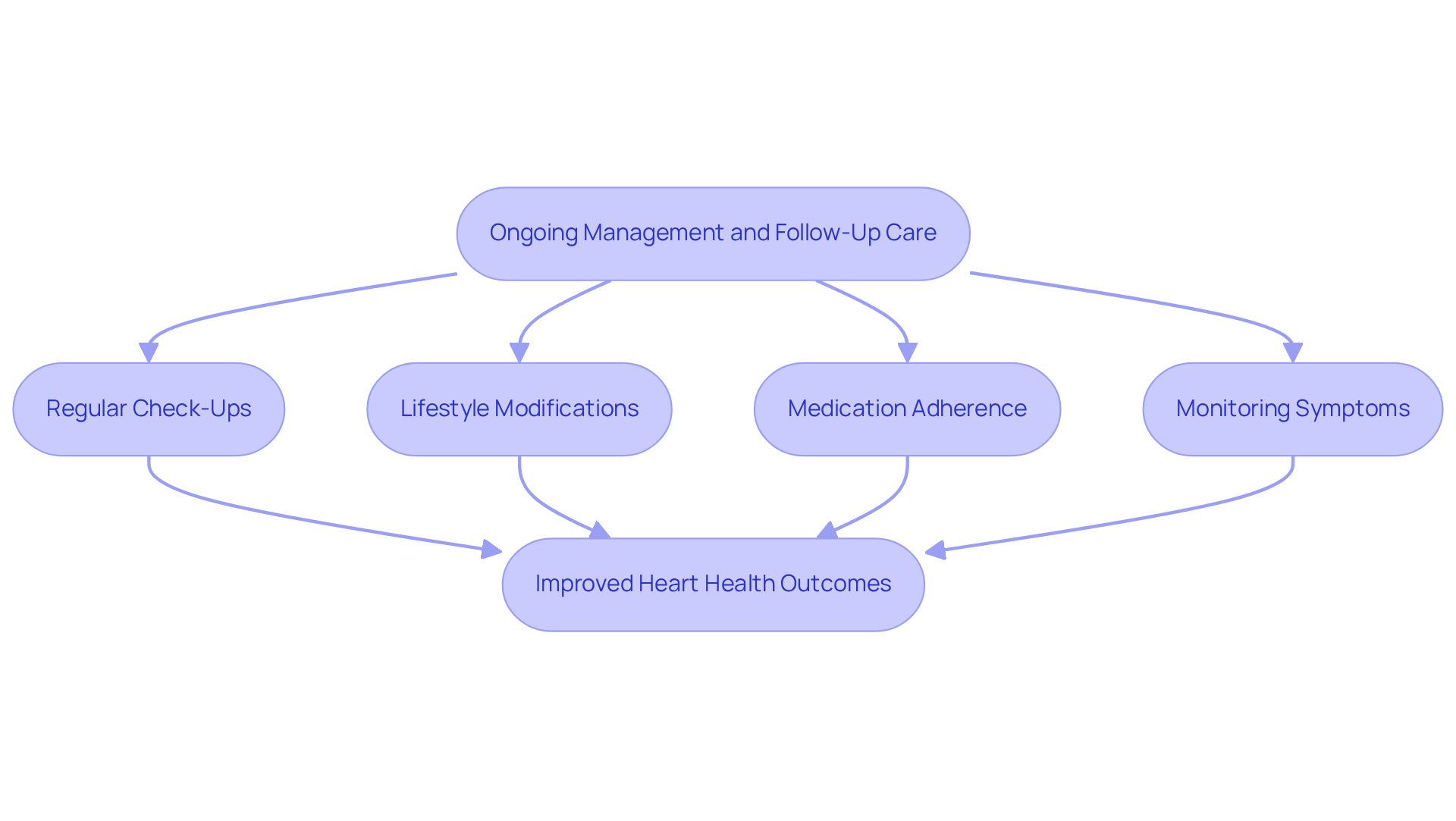
Regular checkups and open discussions about preventive measures with healthcare providers can greatly assist in managing heart health effectively. It’s vital that women receive the proactive, data-driven care they deserve. Remember, you are not alone in this journey; support is available, and taking these steps can lead to a healthier future.
Shortness of Breath
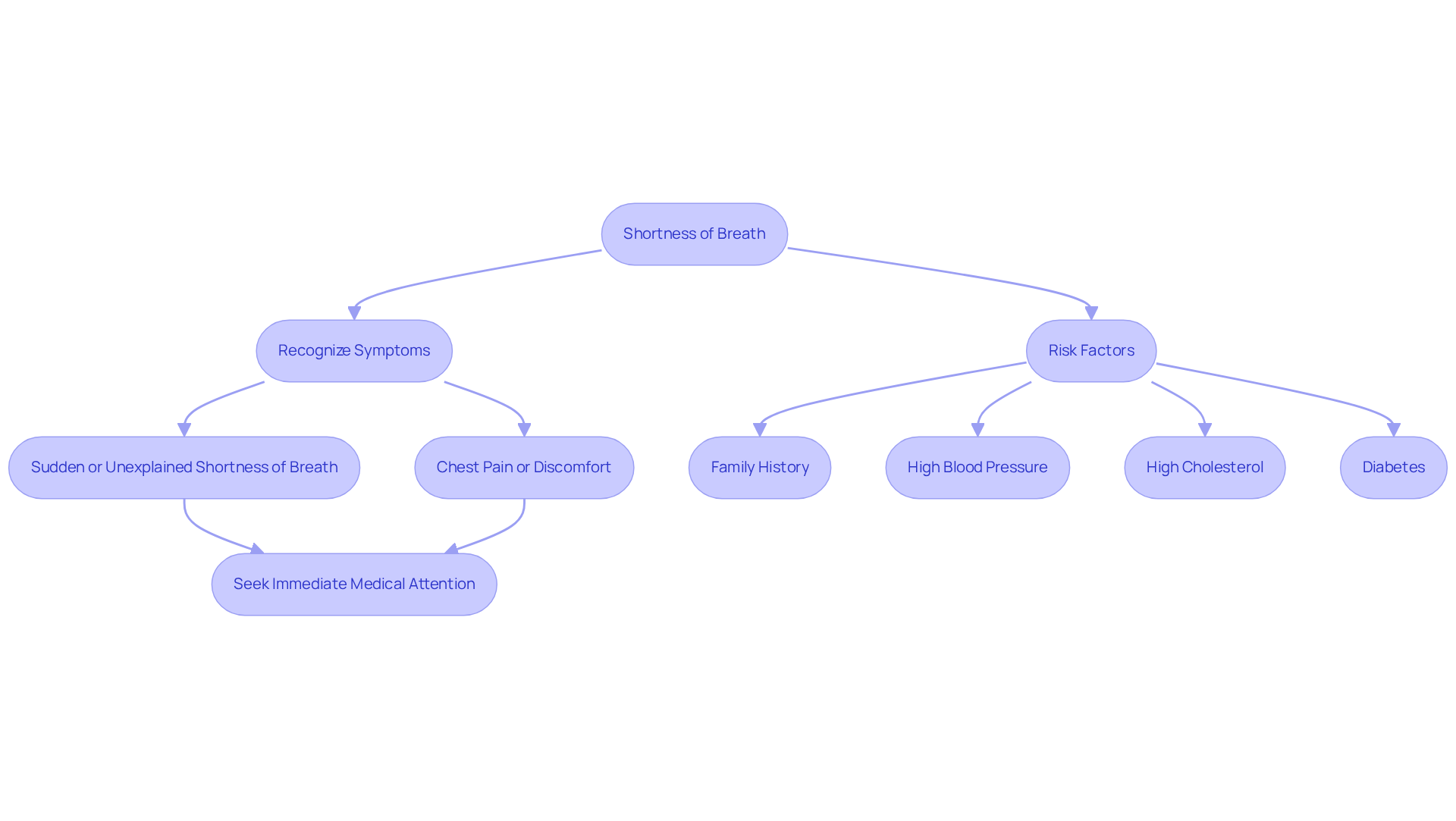
Shortness of breath can catch you off guard, whether you’re resting or being active, and it often comes with feelings of anxiety or panic. This symptom is particularly concerning for older adults, who might not always link it to physical exertion. Did you know that research shows shortness of breath is among the signs you may have a heart attack? In fact, patients experiencing this issue are four times more likely to face serious cardiac problems compared to those who don’t. Factors like family history, high blood pressure, high cholesterol, and diabetes can increase this risk.
Sadly, many older adults may not recognize shortness of breath as a serious issue, which can delay crucial medical help. If you experience sudden or unexplained shortness of breath, especially alongside other symptoms like chest pain or discomfort, these could be signs you may have a heart attack, and it’s essential to seek immediate medical attention. Recognizing this symptom early can be life-saving; timely intervention can prevent severe cardiac events.
At Amavita Cardiovascular Health®, we emphasize the importance of thorough cardiac assessments and preventive measures to significantly reduce your risk of heart attacks. Our innovative AI-powered diagnostic technology, including the amavita CardioElite™ program, enhances early detection and improves patient outcomes, ensuring that conditions are diagnosed accurately and promptly.
Taking proactive steps for your cardiovascular health is vital. Why wait? Request an appointment today. As Dr. Daniel Berman wisely points out, ‘Patients often do not interpret shortness of breath as a serious symptom, but it may be one of the signs you may have a heart attack, suggesting the presence of serious coronary artery disease that may need treatment.’ Your health matters, and we’re here to support you every step of the way.
Pain Radiating to Arms or Jaw
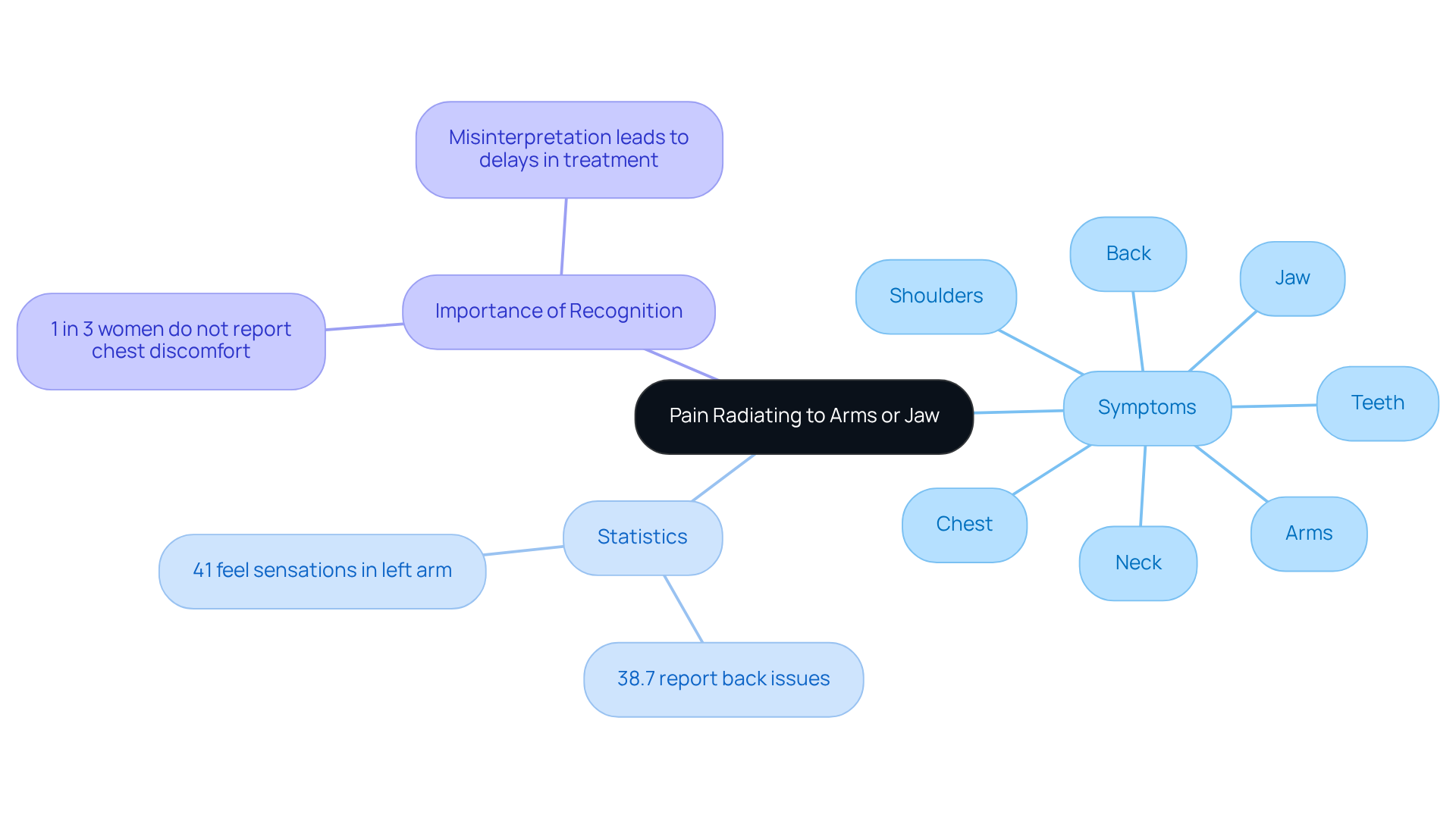
If you ever feel discomfort during a cardiac event, it’s important to know that this sensation can spread from your chest to other areas like your shoulders, neck, arms, back, jaw, and even your teeth. Many people mistakenly think this discomfort is just dental issues or muscle strain, which can lead to dangerous delays in getting the help they need. Did you know that 1 in 3 women who have a heart attack don’t report chest discomfort? Instead, they might feel unease in their jaw or arms. This is a significant concern, as many women report discomfort radiating to these areas, often misinterpreted as something less serious.
Recent findings show that:
- 38.7% of patients with non-classic discomfort reported back issues.
- 41% felt sensations in their left arm.
This highlights how crucial it is to recognize the signs you may have a heart attack as potential warnings of a cardiac event. If you experience such discomfort, especially alongside other symptoms like nausea or unusual tiredness, please seek urgent medical assistance right away.
At Amavita, we understand how overwhelming this can be. Our CardioElite™ program acts as a clinical force multiplier, offering comprehensive cardiovascular management tailored to your needs. By integrating advanced AI technology and AHA certification, we ensure that high-risk patients receive the proactive care they deserve. This approach not only helps reduce the risk of complications but also minimizes the chances of readmissions. Remember, you’re not alone in this journey; we’re here to support you every step of the way.
Nausea or Lightheadedness
Nausea, vomiting, or lightheadedness can often accompany a heart attack, but these signs are frequently misinterpreted as gastrointestinal issues. This misdiagnosis is especially common among women, who may not experience the typical crushing chest pain. Did you know that nearly half of all women live with some form of cardiovascular disease? This highlights just how important it is to recognize these symptoms.
At Amavita Heart and Vascular Health®, we truly care about your well-being. We emphasize the need for thorough cardiovascular evaluations and our preventive cardiology strategy. This approach combines advanced risk assessment tools with personalized care plans designed to lower the risk of cardiac events. If you experience nausea or lightheadedness, especially when paired with other warning signs like chest pain or shortness of breath, please seek medical attention without delay.
Dr. Naveen Bhamri reminds us that silent cardiac events can sometimes present as mild discomfort, bloating, or unusual heaviness in the chest. These symptoms can easily be confused with less serious conditions. Trusting your instincts is vital in these situations. If you notice these symptoms, don’t hesitate to consult a healthcare provider quickly. Your cardiovascular health is important, and we’re here to support you.
Sudden Fatigue
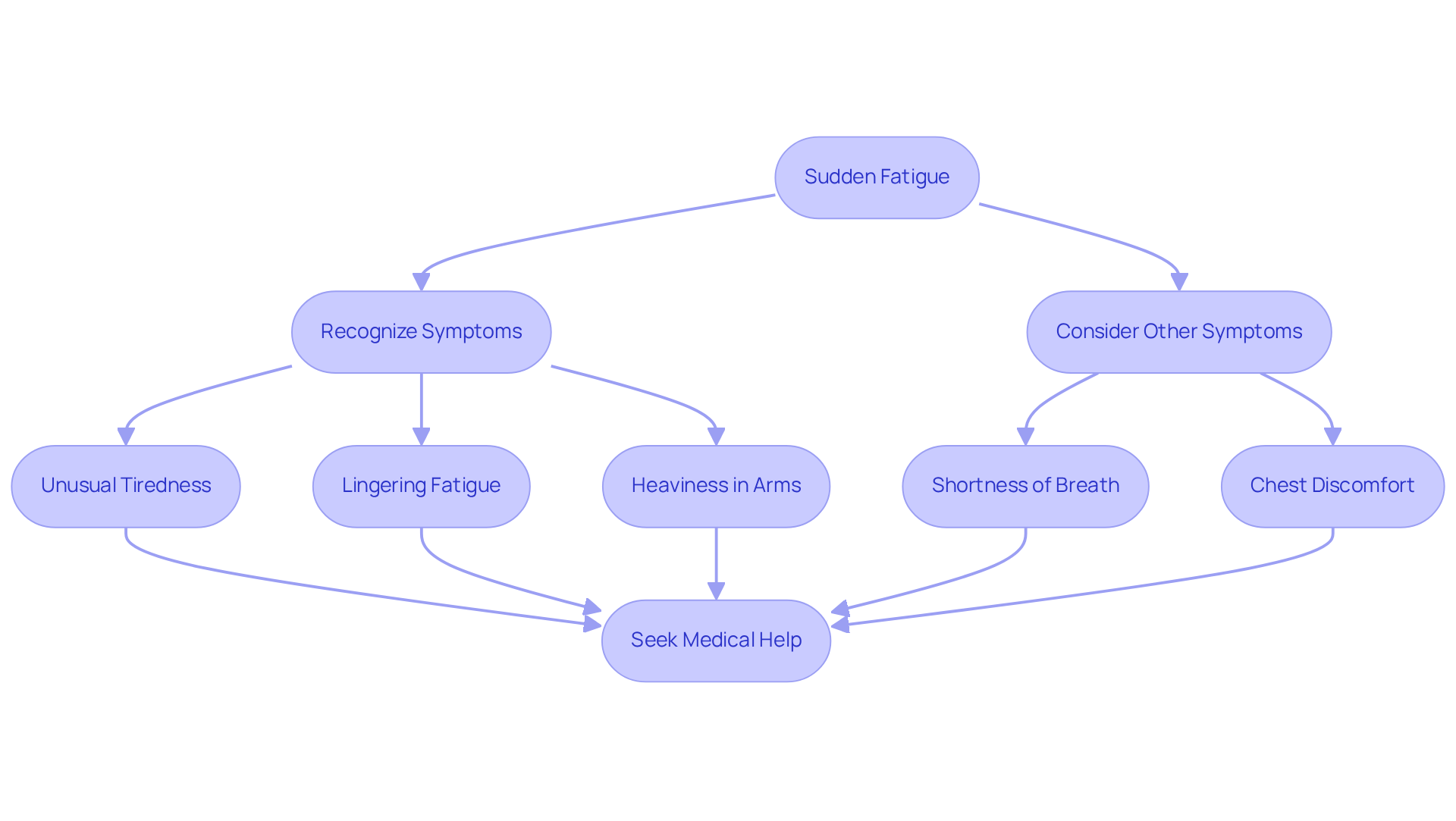
Feeling unusually tired or noticing a sudden dip in your energy levels can be a crucial warning sign of an impending cardiovascular event, especially for women. This type of fatigue often feels different from regular tiredness, lingering for days or even weeks before a heart issue arises. Dr. Quinones-Camacho points out that many women may experience profound fatigue that gets easily brushed aside, often attributed to stress or everyday exhaustion. However, research indicates that fatigue is one of the first signs you may have a heart attack reported by patients before a cardiac event, with some describing it as an unsettling feeling that something isn’t right.
For example, one case study highlighted a woman who felt overwhelming fatigue and an unusual heaviness in her arms, which she initially dismissed. If you notice a significant change in your energy levels, especially when paired with other symptoms like shortness of breath or chest discomfort, these could be signs you may have a heart attack, making it vital to reach out to a healthcare provider without delay. Recognizing these signs can lead to timely medical intervention, significantly reducing the risk of serious heart damage.
Amavita’s CardioElite™ program supports this proactive approach by offering advanced, real-time diagnostic data and 24/7 cardiology consultation. This program acts as a clinical force multiplier, ensuring that high-risk patients receive comprehensive cardiovascular management tailored to their unique needs. Remember, you’re not alone in this journey; seeking help is a strong and positive step towards better health.
Cold Sweats
Experiencing cold sweats, often accompanied by clammy skin, can be a critical indicator of a heart attack. This symptom might occur even without physical exertion and is frequently misinterpreted as anxiety or panic. If you notice cold sweats along with other concerning signs you may have a heart attack, such as chest pain or shortness of breath, it’s essential to seek prompt medical attention. Your health matters, and recognizing these signs can be life-saving.
Did you know that cold sweats are especially common among women during cardiac events? Many women describe symptoms that differ from the typical presentation. For example, Pamela Detrow experienced cold sweats and profound fatigue, which initially led to a misdiagnosis of a panic episode. It wasn’t until three days later that she received the correct diagnosis of a cardiac event. This highlights how important it is to acknowledge unusual symptoms and seek help.
Dr. Henock Saint-Jacques emphasizes that cold sweats can be a subtle yet significant indicator of cardiac distress, particularly in women. Understanding this connection can lead to timely medical intervention, which is crucial for improving outcomes. At Amavita Vascular and Cardiac Health®, we offer a preventive cardiology strategy that combines advanced risk evaluation tools with personalized interventions, including lifestyle changes and minimally invasive procedures. These efforts can significantly lower the risk of cardiac events.
If you or someone you know is experiencing cold sweats along with other signs you may have a heart attack, please don’t hesitate to call for emergency assistance. Remember, you’re not alone in this, and reaching out for help is a strong and important step towards better health.
Anxiety or Sense of Impending Doom
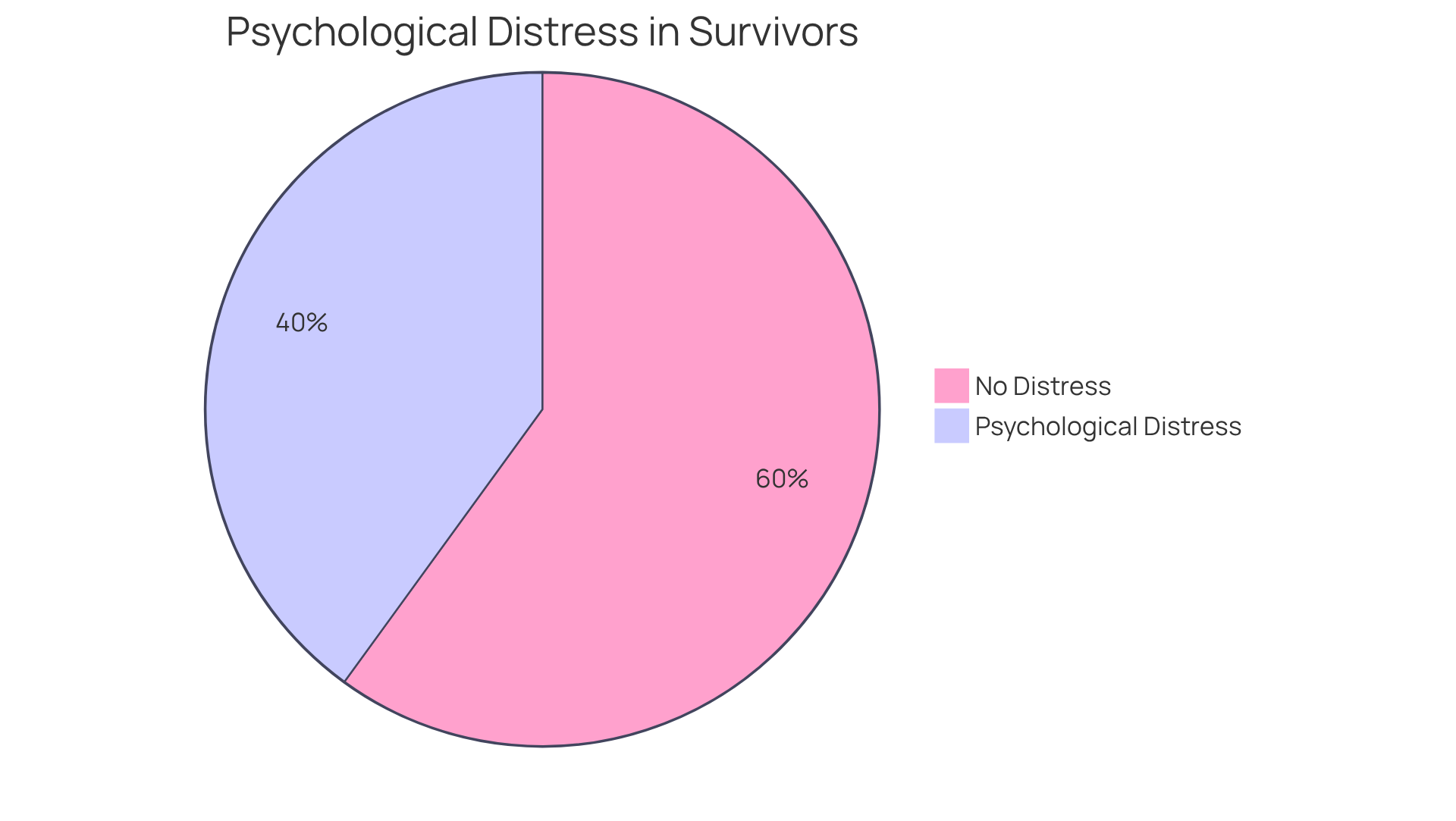
Anxiety and a sense of impending disaster are common feelings experienced by individuals during a cardiac event. Did you know that around 33% to 50% of survivors report some form of psychological distress? This distress can significantly impact recovery and overall health. These emotions can be just as important as physical symptoms, often leading to delays in seeking necessary medical help. For example, overwhelming anxiety or fear might prevent patients from calling for assistance, which can worsen their condition.
Recognizing these psychological signs you may have a heart attack is crucial, as they can indicate a serious medical event. Addressing both the emotional and physical aspects of a heart event is vital for improving outcomes and ensuring timely treatment. Amavita’s CardioElite™ program offers comprehensive support that includes tackling psychological issues, helping patients manage their emotional well-being after a heart incident. This holistic approach is essential, especially since individuals experiencing ongoing psychological discomfort for up to a year are 1.5 times more likely to face future cardiac events. This highlights the urgent need to address psychological concerns for better long-term results.
If you or someone you know is struggling with these feelings, remember that support is available. You don’t have to face this alone.
Heartburn or Indigestion Symptoms
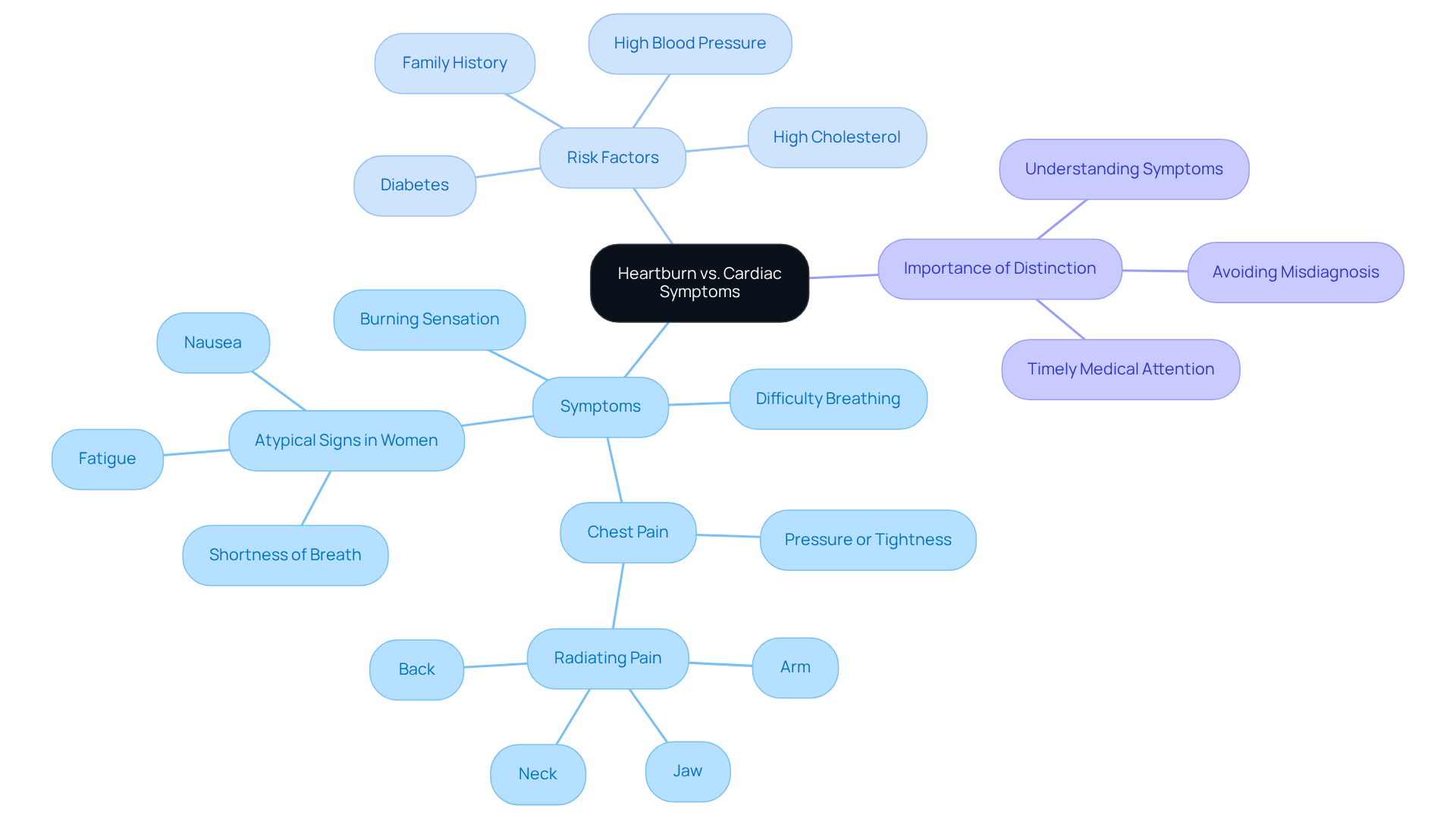
Acid reflux and discomfort that feels like digestive issues can sometimes occur during a cardiac event, leading to confusion and misdiagnosis. Many patients describe a burning sensation in their chest or throat, which is often mistaken for acid reflux. This overlap in symptoms is particularly concerning, as about two-thirds of individuals experience warning signs before a cardiac event, yet many may dismiss these signals as mere digestive problems.
It’s crucial to recognize that if discomfort resembling acid reflux is accompanied by other signs of a cardiac event – like chest pain, difficulty breathing, or unusual fatigue – seeking medical help right away is essential. Factors such as family history, high blood pressure, high cholesterol, or diabetes can increase the risk of a cardiac event, making it even more important to be aware of these signs. For instance, one case study highlighted a patient who initially attributed their discomfort to severe heartburn, only to later discover they were on the verge of a widowmaker cardiac event, where the main artery supplying blood to the heart becomes completely blocked.
Experts emphasize the importance of distinguishing between acid reflux and cardiac event symptoms. While indigestion typically presents as a burning sensation that can be relieved by antacids, a cardiac event often feels like pressure, tightness, or squeezing in the chest that doesn’t improve with medication. Additionally, women may experience atypical signs such as shortness of breath or nausea, which can complicate diagnosis further.
Understanding these differences is vital, especially for older adults and those with a history of heart issues, who may experience more subtle or unusual symptoms. At Amavita, we offer comprehensive cardiac evaluations and personalized care plans designed to address these concerns effectively. If you notice new or unusual chest discomfort, please consult a healthcare provider promptly; timely intervention can make a significant difference in outcomes. To learn more about our services or to schedule an appointment, we invite you to visit our website.
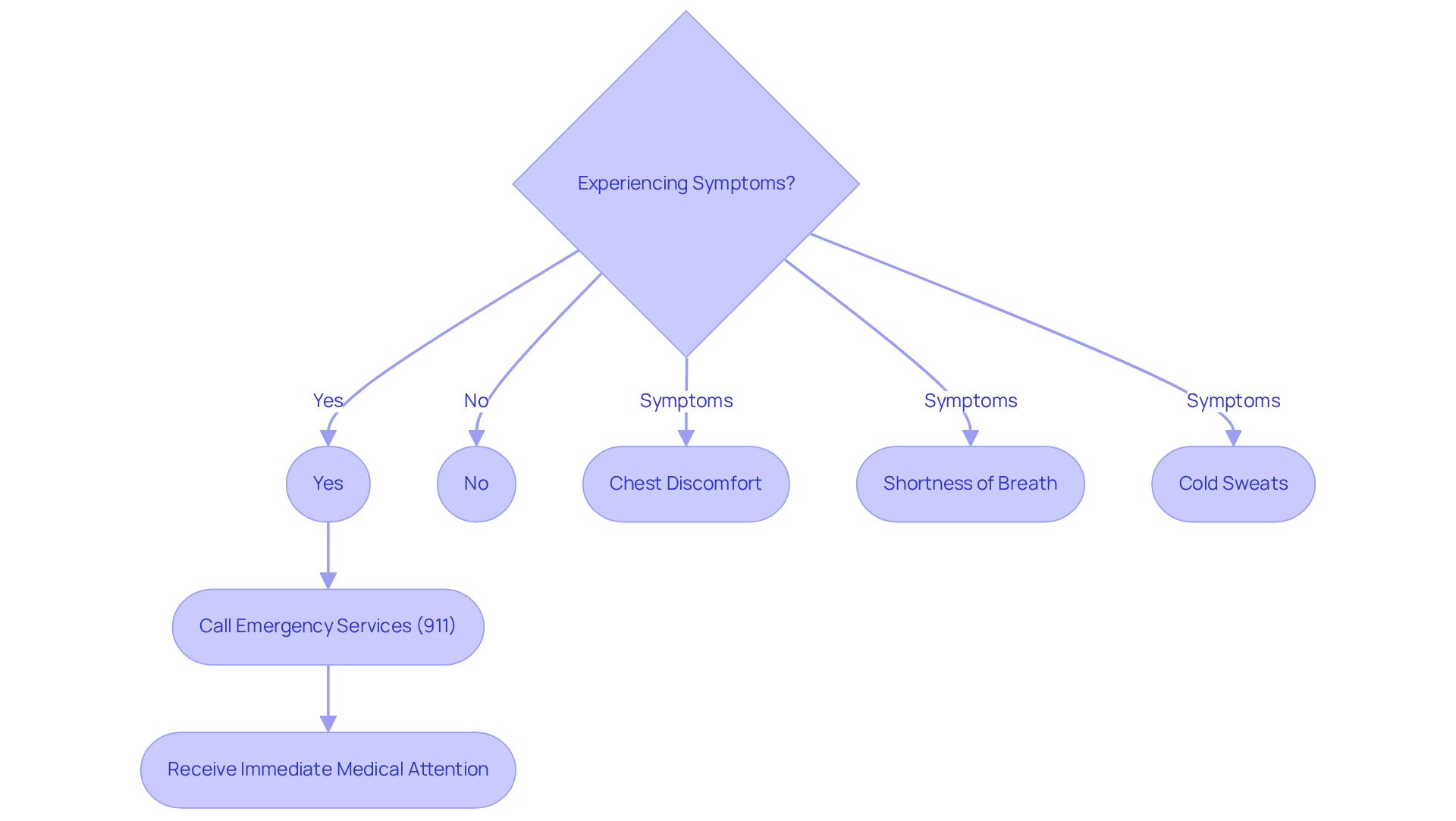
If you or someone you know is experiencing any signs you may have a heart attack, it’s crucial to seek medical help right away. Calling emergency services means that trained professionals can start treatment while on their way, which can significantly boost survival rates. Did you know that timely intervention can truly make a life-saving difference? Research shows that patients who receive care within minutes of their symptoms often have much better outcomes. Emergency departments are ready to perform an electrocardiogram (ECG) within just 10 minutes of arrival, allowing for quick diagnosis and treatment of cardiac issues.
At Amavita Cardiovascular Health®, we understand how important it is to have thorough cardiac assessments and preventive measures in place to reduce the risk of heart attacks. Our approach to preventive cardiology combines advanced risk assessment tools with personalized care, ensuring that those at high risk receive the tailored support they need. This includes lifestyle changes like healthier eating, exercise programs, and medication management to help lower risk factors.
Real-life stories show just how effective quick responses can be. For instance, there was a case where a cardiologist on a flight helped a traveler who was experiencing severe chest discomfort. By administering medication and monitoring their heart activity, they were able to prevent a potential heart attack. This highlights the importance of never hesitating to call 911-every second truly counts during a heart emergency. Remember, chest pain can sometimes feel like anxiety or heartburn, but it’s always important to take it seriously as it can be one of the signs you may have a heart attack. If you notice symptoms such as discomfort in your chest, arms, back, neck, or jaw, or if you experience shortness of breath, cold sweats, nausea, or lightheadedness, these could be signs you may have a heart attack, so don’t wait to seek help. Your quick action could save a life.
Conclusion
Recognizing the signs of a heart attack is crucial for timely intervention and improved outcomes. Have you ever wondered what symptoms to look for? Understanding these signs can empower you to seek medical attention promptly, potentially saving lives.
Heart attacks can present in various ways, and it’s important to be aware of the diverse symptoms. Common signs include:
- Chest pain
- Shortness of breath
- Nausea
- Fatigue
Sometimes, these can be misinterpreted as less serious conditions. This is especially true for women, who may experience atypical symptoms. Open communication with your healthcare provider is essential. Remember, discussing your concerns can lead to better care.
Seeking immediate medical help can significantly increase survival rates and improve recovery outcomes. Trust your instincts-don’t dismiss unusual symptoms. Timely action can lead to better health outcomes. Prioritizing heart health through regular check-ups, lifestyle changes, and awareness of symptoms is essential for everyone, particularly those at higher risk.
You are not alone in this journey. Support and resources are available to help you navigate the complexities of heart health. Together, we can safeguard your cardiovascular health.
Frequently Asked Questions
What does chest pain or discomfort feel like?
Chest pain or discomfort often feels like pressure, squeezing, fullness, or pain in the center or left side of the chest. This sensation can linger for several minutes or come and go, and its intensity can vary widely.
How do women experience chest discomfort differently than men?
Studies show that women are 30% less likely than men to report chest discomfort during a cardiac event. Women often experience discomfort in the upper back, arms, neck, and jaw, and they may describe their symptoms differently, sometimes mistaking them for heartburn or indigestion.
Why is it important for women to recognize signs of a heart attack?
Heart disease is a significant health threat for women, accounting for one in five female deaths in the U.S. in 2023. Recognizing the signs of a heart attack can lead to timely medical intervention, which is crucial for improving outcomes.
What unusual symptoms should women be aware of regarding heart attacks?
Women may exhibit unique signs of a heart attack, including shortness of breath, nausea, vomiting, and discomfort in the back or jaw. These symptoms can often be misunderstood as other health issues.
What is the significance of shortness of breath in relation to heart health?
Shortness of breath can indicate serious cardiac problems and is among the signs of a heart attack. Patients experiencing this symptom are four times more likely to face severe cardiac issues compared to those who do not.
What should someone do if they experience sudden or unexplained shortness of breath?
If you experience sudden or unexplained shortness of breath, especially alongside other symptoms like chest pain or discomfort, it is essential to seek immediate medical attention, as these could be signs of a heart attack.
How does Amavita Heart and Vascular Health® support patients?
Amavita offers thorough cardiac assessments, lifestyle changes, and preventive measures for high-risk patients. They also provide innovative diagnostic technology to enhance early detection and improve patient outcomes.
How can women effectively communicate their cardiovascular concerns to healthcare providers?
Women are encouraged to openly discuss their cardiovascular concerns with their doctors and to bring a list of questions to their medical checkups to ensure their symptoms are properly evaluated.
List of Sources
- Chest Pain or Discomfort
- Heart disease remains the top threat many women never see coming (https://abcnews.com/Health/heart-disease-remains-top-threat-women-coming/story?id=129718739)
- New study finds more young adults dying from heart attacks, especially women (https://click2houston.com/news/local/2026/03/04/new-study-finds-more-young-adults-dying-from-heart-attacks-especially-women)
- Heart disease threat projected to skyrocket in women (https://nypost.com/2026/02/27/health/heart-disease-threat-projected-to-skyrocket-in-women)
- What women don’t know about heart attacks could be deadly (https://news4jax.com/news/local/2026/02/06/what-women-dont-know-about-heart-attacks-could-be-deadly)
- American heart health worsening — Harvard Gazette (https://news.harvard.edu/gazette/story/2026/02/american-heart-health-worsening)
- Unusual Symptoms in Women
- A troubling forecast on women’s heart health – and what women and girls can do now to protect theirs (https://heart.org/en/news/2026/02/25/a-troubling-forecast-on-womens-heart-health-and-what-women-and-girls-can-do-now-to-protect-theirs)
- Women suffer heart attacks too. Understanding risks, symptoms and how to save yourself (https://apnews.com/article/women-heart-attack-warning-signs-d1e6644f01048de85425cb6738d435b4)
- Heart disease remains the top threat many women never see coming (https://abcnews.com/Health/heart-disease-remains-top-threat-women-coming/story?id=129718739)
- Shortness of Breath
- ‘Don’t ignore the signs’: Cardiologist warns subtle symptoms can signal heart disease (https://kxan.com/top-stories/dont-ignore-the-signs-cardiologist-warns-subtle-symptoms-can-signal-heart-disease)
- We Asked 3 Cardiologists What Heart Disease Symptom You Should Never Ignore, and They All Said the Same Thing – AOL (https://aol.com/asked-3-cardiologists-heart-disease-162500557.html)
- Clinical trial offers first-of-its-kind heart failure treatment (https://health.ucdavis.edu/news/headlines/clinical-trial-offers-first-of-its-kind-heart-failure-treatment/2026/02)
- Shortness of Breath Without Chest Pain Can Signify the Presence of High Risk Heart Disease (https://cedars-sinai.org/newsroom/shortness-of-breath-without-chest-pain-can-signify-the-presence-of-high-risk-heart-disease)
- Pain Radiating to Arms or Jaw
- What women don’t know about heart attacks could be deadly (https://news4jax.com/news/local/2026/02/06/what-women-dont-know-about-heart-attacks-could-be-deadly)
- We Should Pay Attention to “Referred Pain” – A Case of Acute Myocardial Infarction That Masked and Delayed the Diagnosis of Esophageal Perforation – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9107967)
- Heart disease remains the top threat many women never see coming (https://abcnews.com/Health/heart-disease-remains-top-threat-women-coming/story?id=129718739)
- Prevalence of classic and non-classic pain sites of coronary artery disease: a cross-sectional study – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11344326)
- Mercy Health: Heart attacks aren’t just about chest pain (https://wpsdlocal6.com/news/mercy-health-heart-attacks-arent-just-about-chest-pain/article_d4149bca-000e-4b7b-8b4b-31921626be6b.html)
- Nausea or Lightheadedness
- The sneaky heart attack symptoms many women miss (https://washingtonpost.com/video/wellbeing/the-sneaky-heart-attack-symptoms-many-women-miss/2026/02/17/adde750f-5475-4d76-9f8a-8147a83effce_video.html)
- Nurse practitioner knows heart symptoms should never be ignored | SSM Health (https://ssmhealth.com/newsroom/blogs/ssm-health-matters/february-2026/nurse-practitioner-knows-heart-symptoms-should-never-be-ignored)
- Could heart attack symptoms be mistaken for ‘gas’ issues? Max Hospital cardiologist explains | Today News (https://livemint.com/news/trends/could-heart-attack-symptoms-be-mistaken-for-gas-issues-max-hospital-cardiologist-explains-11760241438502.html)
- Sudden Fatigue
- Doctors Say These Symptoms Could Signal a Silent Heart Attack (https://prevention.com/health/a71078438/silent-heart-attack-signs)
- Doctors Say These Symptoms Could Signal a Silent Heart Attack (https://health.yahoo.com/conditions/cardiovascular/articles/doctors-symptoms-could-signal-silent-133331485.html)
- Two days before heart attack: Expert lists symptoms your body gives 48 hours prior (https://indiatoday.in/health/story/two-days-before-heart-attack-early-warning-signs-you-should-never-ignore-2865896-2026-02-10)
- Often dismissed as fatigue: Doctor warns of silent heart attack pattern, lists signs to watch out for – The Times of India (https://timesofindia.indiatimes.com/life-style/health-fitness/health-news/often-dismissed-as-fatigue-doctor-warns-of-silent-heart-attack-pattern-lists-signs-to-watch-out-for/articleshow/126094989.cms)
- How to recognize heart attack warning signs and reduce long-term risk (https://clickondetroit.com/features/2026/01/07/how-to-recognize-heart-attack-warning-signs-and-reduce-long-term-risk)
- Cold Sweats
- Heart disease remains the top threat many women never see coming (https://abcnews.com/Health/heart-disease-remains-top-threat-women-coming/story?id=129718739)
- 3 Subtle Heart Attack Symptoms Women Should Never Ignore: Harlem Cardiology on Madison Avenue: Cardiologists (https://harlemcardio.com/blog/3-subtle-heart-attack-symptoms-women-should-never-ignore)
- m.economictimes.com (https://m.economictimes.com/news/india/5-warning-signs-before-heart-attack-you-should-not-miss/sudden-dizziness-and-cold-sweats/slideshow/129824712.cms)
- Profound Fatigue, Cold Sweats, Dizziness May Signal Heart Attack (https://abcnews.com/Health/WomensHealth/heart-attack-symptoms-women-miss/story?id=12823615)
- Heart Attack Warning Signs (https://texasheart.org/heart-health/heart-information-center/topics/heart-attack-warning-signs)
- Anxiety or Sense of Impending Doom
- Depression and anxiety linked to increased risk of heart attack or stroke — Harvard Gazette (https://news.harvard.edu/gazette/story/2025/12/depression-and-anxiety-linked-to-increased-risk-of-heart-attack-or-stroke)
- Psychological distress common after a heart attack, may lead to future heart conditions (https://newsroom.heart.org/news/psychological-distress-common-after-a-heart-attack-may-lead-to-future-heart-conditions)
- Heart Condition? The Psychologist Will See You Now (https://yalemedicine.org/news/heart-condition-the-psychologist-will-see-you-now)
- Anxiety disorders and cardiovascular disease – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC5149447)
- Heartburn or Indigestion Symptoms
- Heart attack symptoms some may mistake for acid reflux (https://mirror.co.uk/news/health/heart-attack-symptoms-mistake-ageing-36984819)
- Heart attack vs heartburn: Colorado man’s close call highlights signs to know (https://koaa.com/news/local-news/heart-attack-vs-heartburn-colorado-mans-close-call-highlights-signs-to-know)
- Is It Heartburn or a Heart Attack? How to Know (https://everydayhealth.com/cardiovascular-diseases/heartburn-or-heart-attack-how-to-tell-the-difference)
- Heartburn or Heart Attack: Symptoms Doctors Say You Can’t Ignore (https://nationaljewish.org/specialties/gastroenterology/heartburn-or-heart-attack-symptoms-doctors-say-you-can-t-ignore)
- Seek Immediate Medical Attention
- Heart disease remains the top threat many women never see coming (https://abcnews.com/Health/heart-disease-remains-top-threat-women-coming/story?id=129718739)
- A man had heart attack symptoms on a flight. A cardiologist and a pocket-sized tool on board may have helped save his life | CNN (https://cnn.com/2025/05/18/us/plane-heart-attack-cardiologist)
- When chest pain strikes: What to expect at the emergency room – Harvard Health (https://health.harvard.edu/pain/when-chest-pain-strikes-what-to-expect-at-the-emergency-room)
- Emergency Physicians Share Tips to Recognize Signs of a Heart Emergency (https://emergencyphysicians.org/press-releases/2025/2-13-25-emergency-physicians-share-tips-to-recognize-signs-of-a-heart-emergency)
- Heart Disease Remains Arkansas’s Leading Killer: Know the Signs and Call 9-1-1 – Arkansas Department of Health (https://healthy.arkansas.gov/article/heart-disease-remains-arkansass-leading-killer-know-the-signs-and-call-9-1-1)