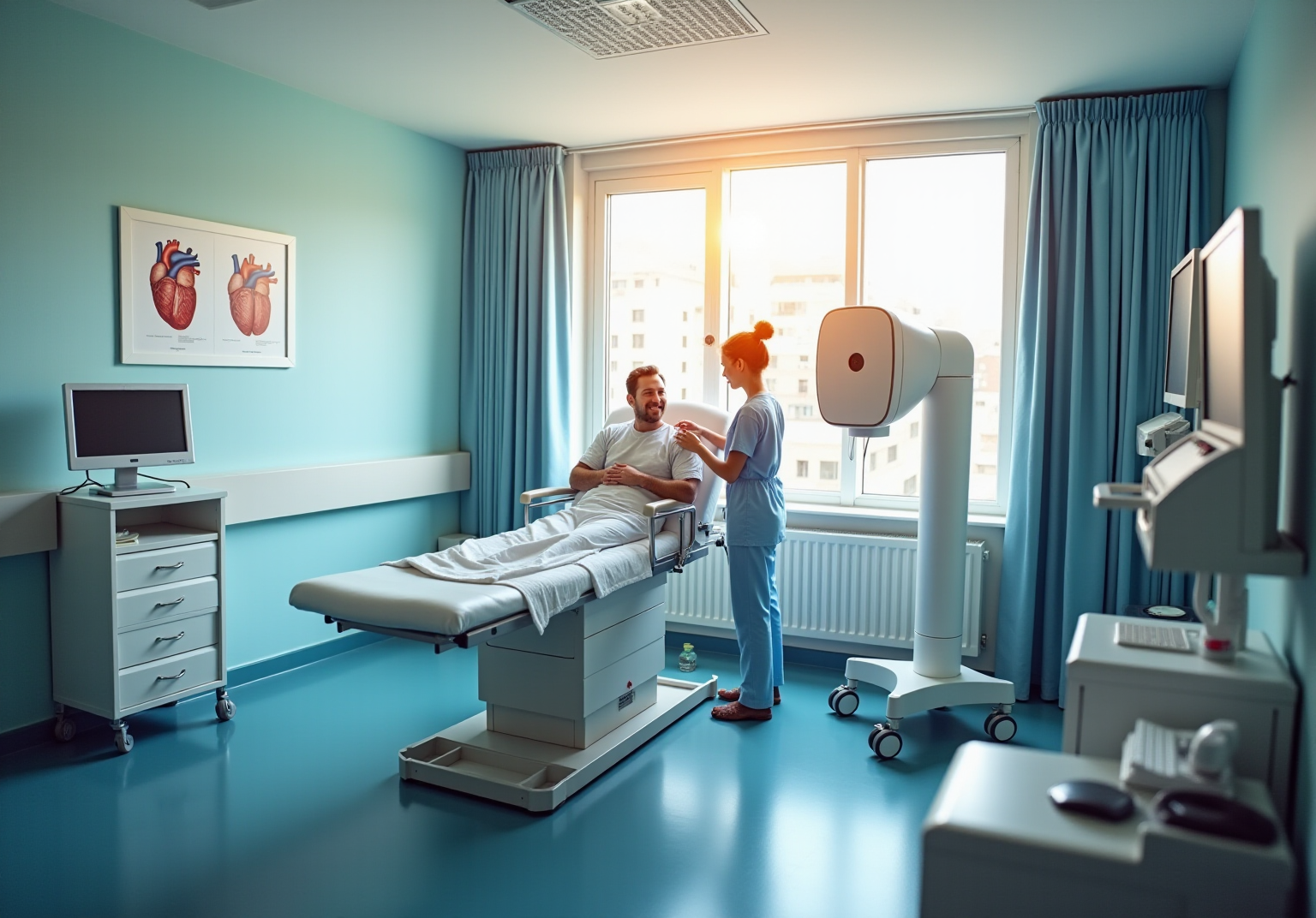
Introduction
Monitoring your heart health after valve replacement is incredibly important. Patients often face a variety of symptoms that could signal complications. In this article, we’ll explore ten key signs of heart failure that you should be aware of following your surgery. By recognizing these symptoms early, you can take steps to ensure your recovery stays on track and that your overall well-being is prioritized.
What subtle yet significant changes might indicate a need for medical attention? How can you navigate your post-operative journey with confidence? These are important questions, and we’re here to help you find the answers. Remember, you’re not alone in this journey; understanding your body’s signals is a vital part of your recovery.
Unexplained Shortness of Breath
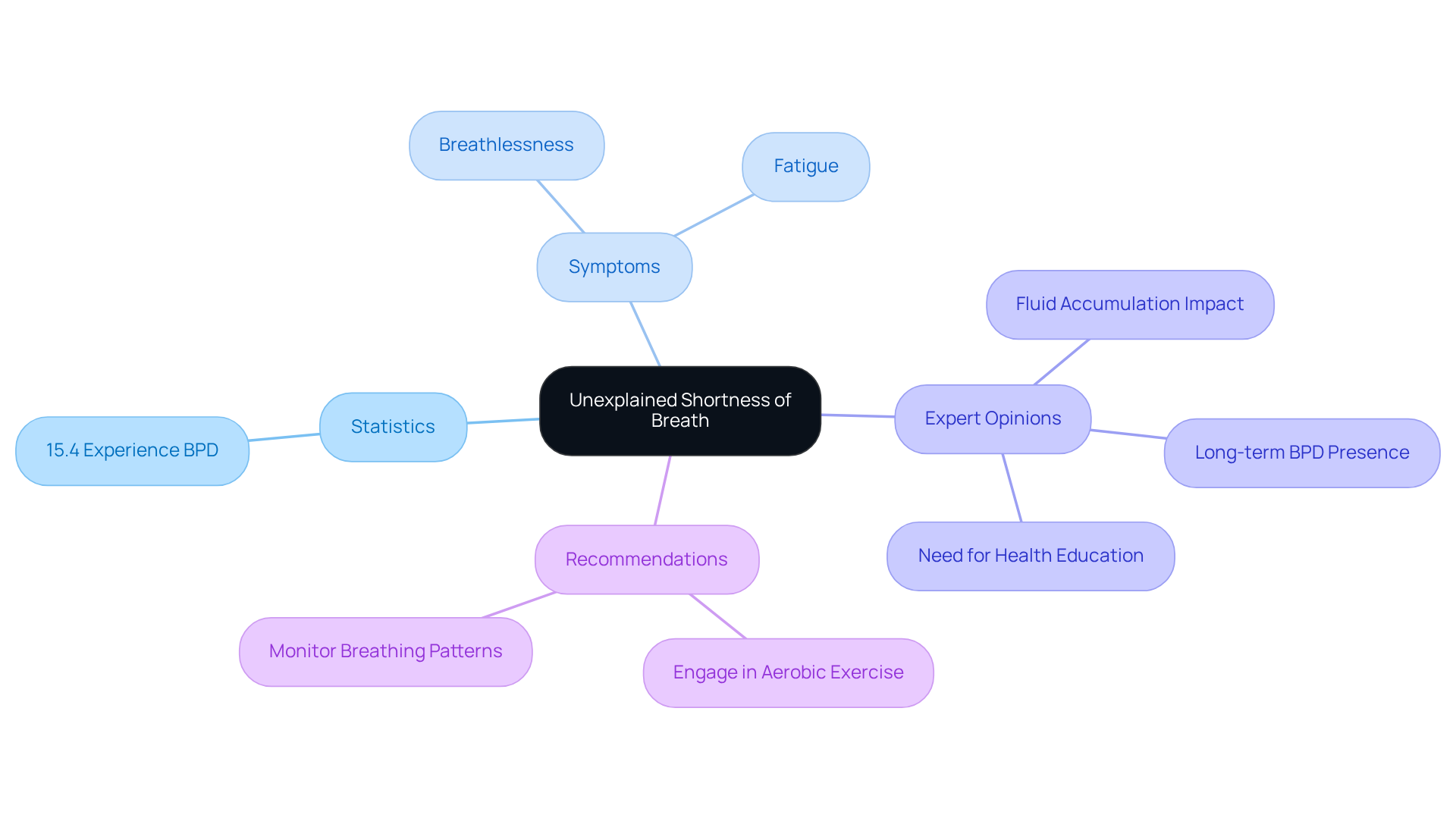
After valve replacement, many individuals may find themselves facing shortness of breath. This can be concerning, as it often signals fluid buildup or changes in heart function. Did you know that about 15.4% of patients experience shortness of breath? This can be a significant indicator of heart failure, especially if the symptom appears suddenly or worsens over time. Cardiologists remind us that fluid retention can increase pressure in the lungs, making it harder to breathe. As one cardiologist compassionately stated, “This is common post-surgery.”
Heart issues can also lead to symptoms like fatigue, which are important to address. Dr. Martinez-Clark, who specializes in cardiology, often sees how repairing or replacing damaged valves can greatly improve breathing and energy levels. Furthermore, bronchial pulmonary disease (BPD) is common among patients in this situation. Studies show that treatment can help alleviate these symptoms.
Understanding these risks and maintaining open communication with your healthcare team can significantly enhance your recovery and well-being. It’s essential to closely monitor your health for any changes and report any noticeable changes to your provider. Participating in light aerobic activities, as recommended by healthcare professionals, can also support your rehabilitation and improve your breathing function. Remember, you are not alone in this journey, and there are caring experts ready to help you every step of the way.
Persistent Fatigue and Weakness
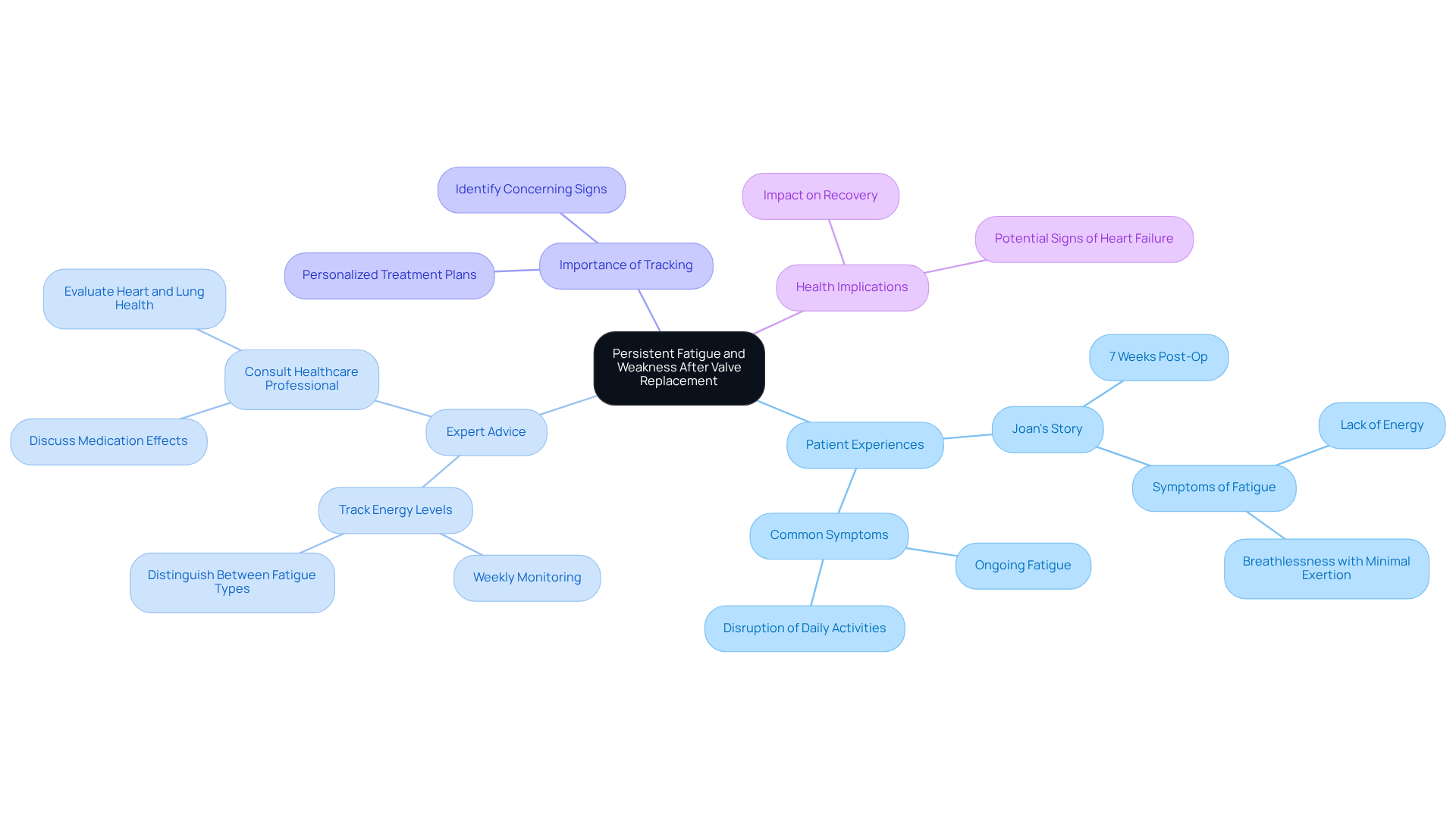
Many patients express feeling unusually fatigued or weak after surgery. While some fatigue is a normal part of recovery, persistent fatigue could be one of the signs of heart failure after valve replacement. Research shows that about 30% of individuals experience fatigue, with many noting that their energy levels are significantly lower.
Take Joan, for example. Seven weeks after her aortic valve replacement, she shares her struggle: “I am now 7 weeks post-op and am tired all the time and have no energy. Everything is a major effort, and I get out of breath with the slightest exertion.” This is a common experience, and it’s important to recognize it.
Dr. Rawn Salenger emphasizes the need to monitor fatigue levels. He advises patients to distinguish between typical post-exertion fatigue and concerning signs that may require medical attention. Although recovery often takes 12 weeks or more, any ongoing fatigue should prompt a conversation with a healthcare professional to rule out signs of heart failure after surgery.
At Amavita, we conduct thorough evaluations to pinpoint the specific cause of fatigue. This allows us to develop personalized treatment plans and restoring energy levels. It’s crucial to make this distinction, as many, like Joan, might initially think their tiredness is just a side effect of medications like metoprolol, rather than a potential sign of something more serious.
Understanding these nuances can greatly influence recovery and overall health outcomes. Remember, you’re not alone in this journey, and seeking help can lead to a brighter, more energetic future.
Swelling in the Legs or Abdomen
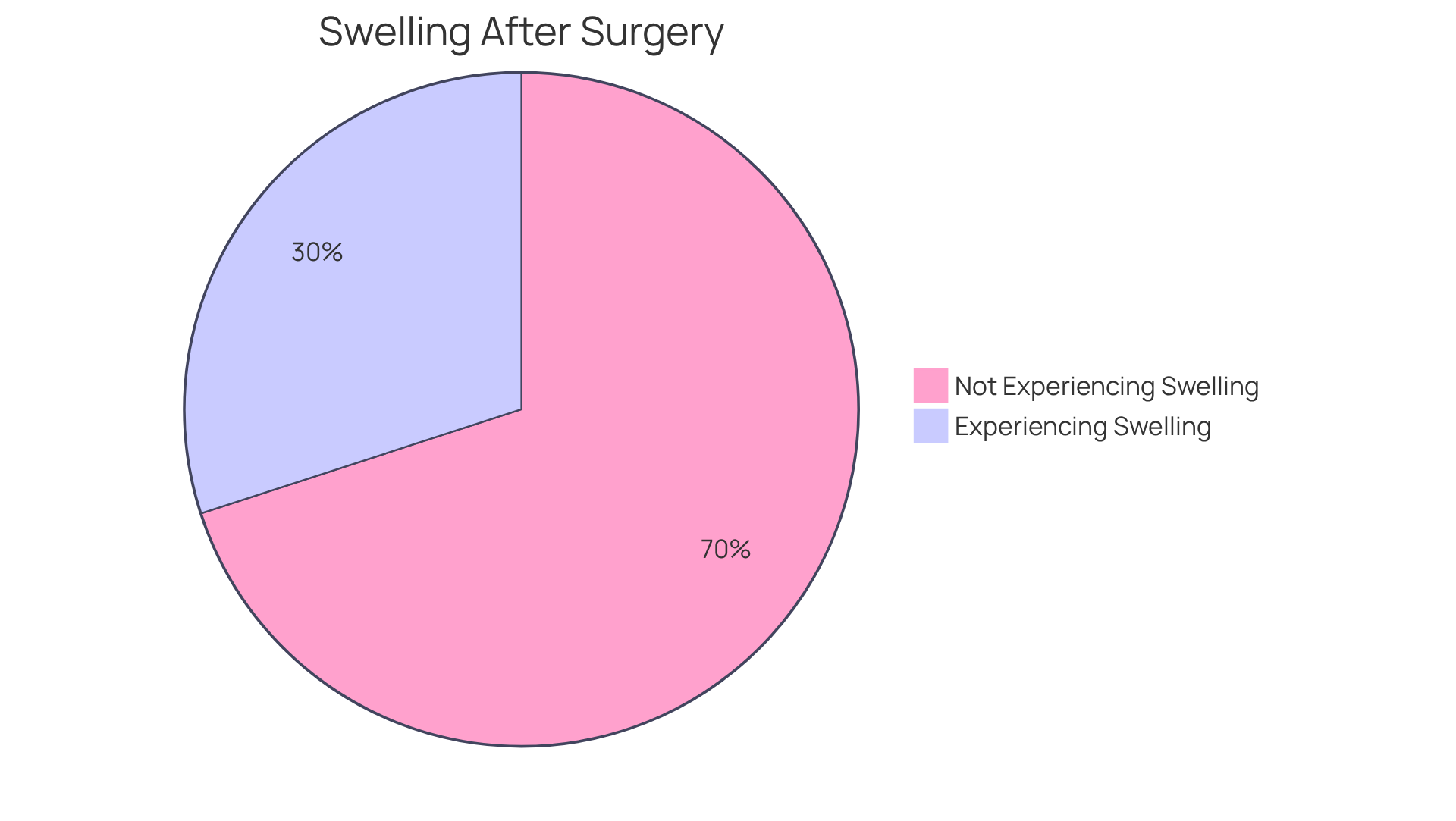
After valve replacement, many individuals may notice swelling, which can manifest as swelling in the legs or abdomen. This is not uncommon; studies indicate that about 30% of patients experience this after surgery. Recognizing the signs of heart failure is vital, as they can sometimes indicate complications, especially when accompanied by shortness of breath or fatigue.
Are you keeping an eye on your weight? A sudden increase can be a warning sign of worsening heart failure. It’s important to report any significant changes to your healthcare provider, as early intervention can make a difference. At Amavita Heart and Vascular Health®, we understand how concerning these symptoms can be. That’s why we emphasize regular monitoring, including follow-up appointments and personalized care strategies to effectively address your needs.
Real-life stories highlight the importance of awareness; individuals who promptly addressed their swelling often reported better outcomes and fewer complications. Staying informed about these signs can empower you to take control in your recovery journey. Remember, you’re not alone in this – we’re here to support you every step of the way.
Irregular Heartbeat or Palpitations
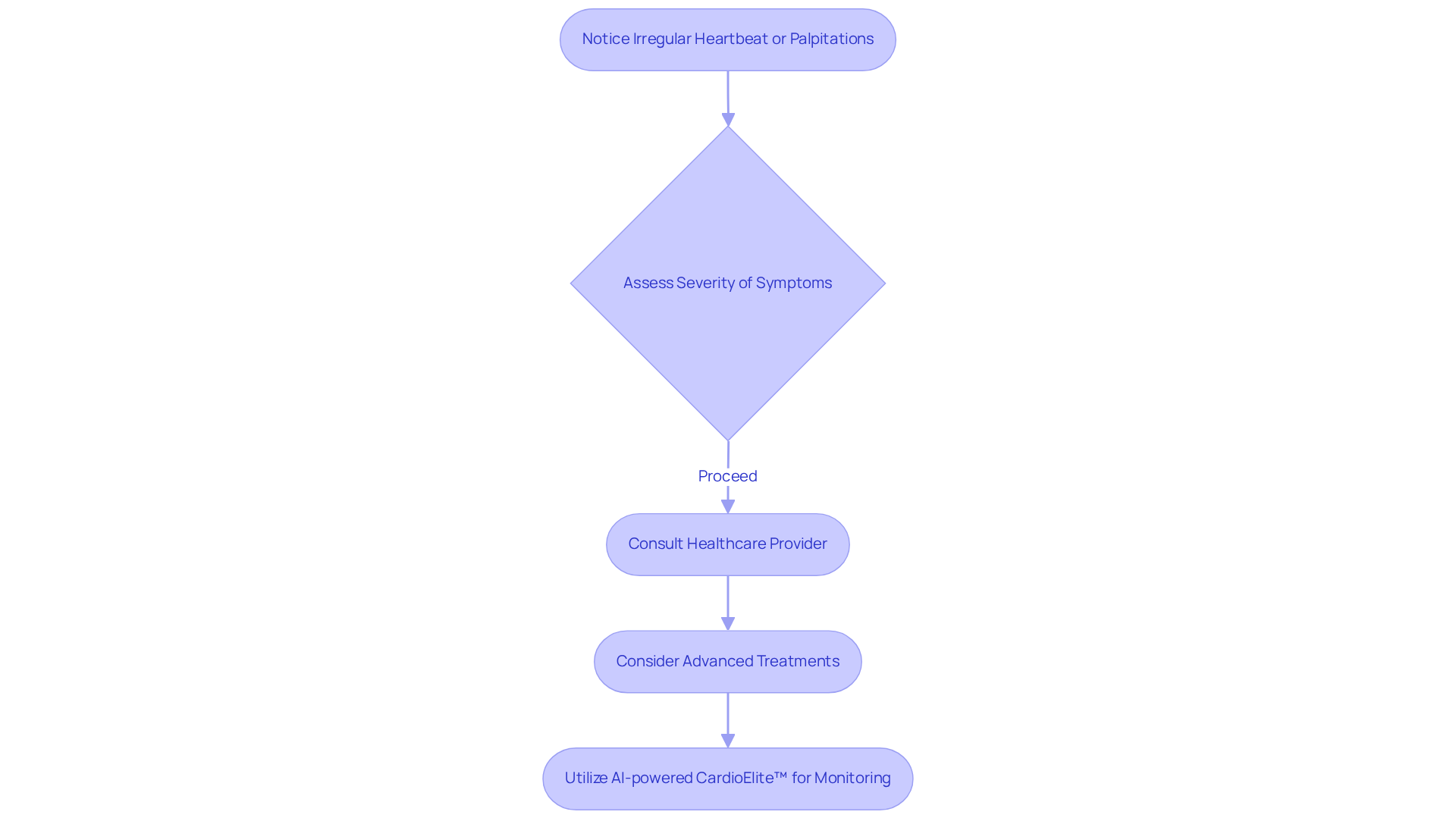
After valve replacement surgery, it’s not uncommon for patients to notice irregular heartbeat. While some of these irregularities can be harmless, it’s important to pay attention to ongoing or frequent palpitations. These could indicate more serious issues, such as arrhythmias or other complications.
At Amavita Heart and Vascular Health, we understand how concerning this can be. That’s why we prioritize thorough evaluations. Our team employs advanced monitoring techniques to help restore your heart’s natural rhythm.
Furthermore, our AI-powered CardioElite™ program enhances early detection through real-time diagnostics. This means that any complications can be addressed promptly, ultimately improving your outcomes and reducing the risk of hospital readmissions.
To take charge of your heart health, consider keeping a record of any irregularities you experience. Discussing these with your healthcare provider can lead to better management and peace of mind. Remember, you’re not alone in this journey; we’re here to support you every step of the way.
Rapid Weight Gain
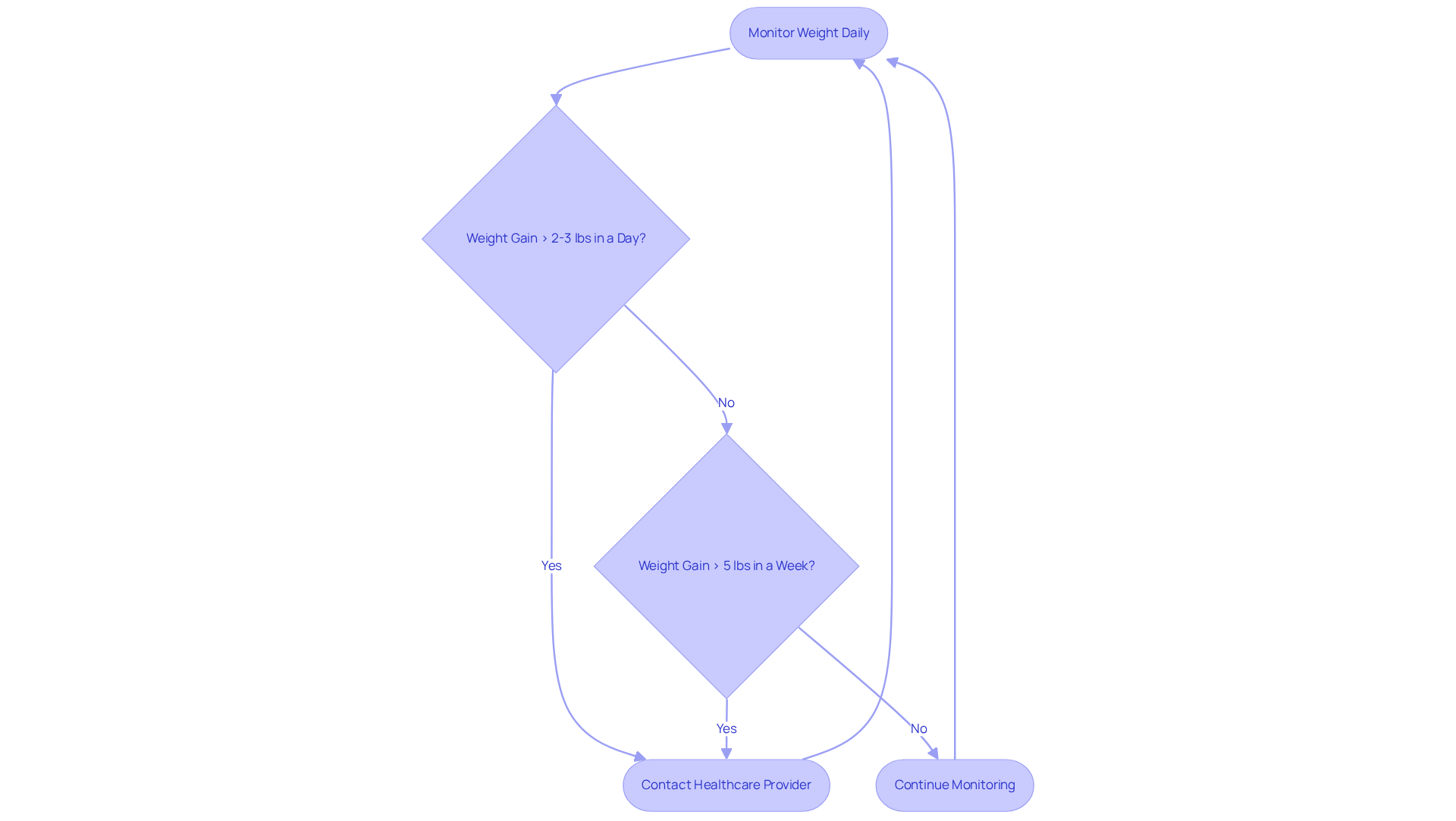
Recovering from cardiac replacement surgery can be a challenging journey, and it’s completely natural to have concerns about your health during this time. One important aspect to keep an eye on is your weight gain, which may lead to complications after valve replacement. If you notice a gain of more than 2-3 pounds in a single day, or 5 pounds within a week, it’s crucial to reach out to your healthcare provider right away for further evaluation.
Why is this so important? Studies show that many patients experience noticeable weight fluctuations, often because their bodies are working hard to manage fluid levels. By recognizing these changes early, you can take proactive steps that lead to better health outcomes, ultimately improving your quality of life.
Remember, you’re not alone in this. It’s okay to feel anxious or uncertain, but staying vigilant about your weight can make a significant difference. If you have any concerns, don’t hesitate to talk to your healthcare team. They’re there to support you every step of the way.
Chronic Cough or Wheezing
If you’ve recently had valve replacement surgery and find yourself dealing with a chronic cough, it’s important to pay attention. These symptoms can sometimes signal heart failure, which may indicate complications after valve replacement, suggesting that your heart is having a tough time pumping effectively. This can lead to increased pressure in the pulmonary veins, causing fluid to leak into lung tissues.
It’s completely understandable to feel anxious about these symptoms. If you’re experiencing ongoing respiratory issues, please don’t hesitate to reach out to your healthcare provider. They can help evaluate your situation and provide the care you need. Research indicates that many individuals report respiratory symptoms, highlighting the need to monitor for complications during your recovery.
Identifying these signs early can make a significant difference. By seeking help promptly, you can enable better health and quality of life. Remember, you’re not alone in this journey, and there are resources available to support you.
Increased Sleep Disturbances
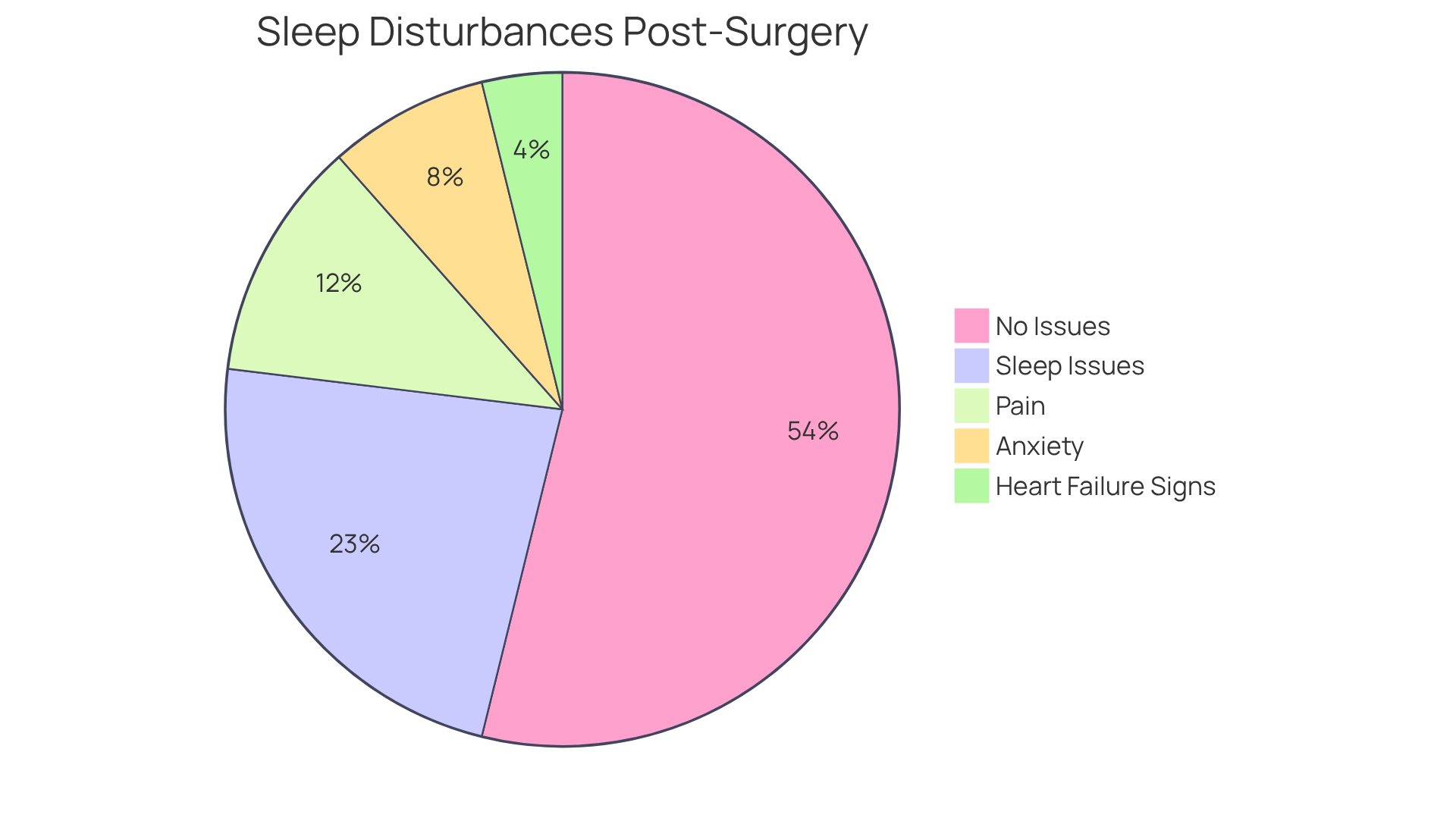
After valve replacement surgery, many patients find themselves facing sleep disturbances, which can be quite concerning. Studies show that around 30% of individuals experience significant sleep issues after their procedure. These disturbances can arise from various factors, such as pain, anxiety, and signs of heart failure after valve replacement.
Sleep quality is essential, as it plays a direct role in achieving restful sleep. Stress and discomfort can complicate sleep patterns even further. It’s important to address these concerns promptly. Sleep specialists emphasize that if sleep issues go unmanaged, they can lead to a decline in overall health and healing outcomes.
Dr. John Smith, a sleep expert, shares, “Addressing sleep concerns after surgery is crucial; it can greatly affect healing and overall well-being.” This highlights the importance of taking sleep issues seriously. Patients are encouraged to share any noticeable changes in their sleep patterns with their healthcare providers. Proactive management can significantly enhance recovery and improve quality of life.
Additionally, discussing these changes with caregivers or family members can provide extra support in managing sleep disturbances. Remember, you’re not alone in this journey, and there are resources available to help you find the restful sleep you deserve.
Confusion or Difficulty Concentrating
After surgery, it’s not uncommon for some patients to feel a bit confused or have trouble concentrating. These feelings can sometimes signal cognitive decline or even heart failure. If you’re experiencing breathlessness or fatigue, it’s important to share these symptoms with your healthcare provider. Ignoring heart problems, such as valve issues, can lead to serious complications, and we want to help you avoid that.
At Amavita Heart and Vascular Health, we truly care about your well-being. We specialize in treatments designed to improve your heart function and overall health. Our thorough cardiac assessments help us pinpoint the exact reasons behind your fatigue and cognitive changes. This way, we can create a plan that focuses on restoring your energy and enhancing your quality of life.
If you’re noticing these symptoms, please don’t hesitate to schedule a follow-up appointment. We’re here to listen to your concerns and provide the support you need. Additionally, our monitoring program allows us to detect potential complications early, ensuring you receive the best post-operative care possible. Remember, you’re not alone in this journey; we’re here to help you every step of the way.
Chest Pain or Discomfort
Experiencing chest pain or discomfort after replacement surgery is a serious concern that shouldn’t be overlooked. It could signal complications, including heart issues. Dr. Joanne Murabito emphasizes that any new or worsening chest pain deserves immediate medical attention to rule out potential issues. Many patients do experience discomfort, which highlights the importance of monitoring this symptom closely.
At Amavita Heart and Vascular Health, our specialists are here to help. We use advanced technologies, including portable, FDA-cleared AI ultrasound technology, to accurately assess and identify any blockages. Recognizing the warning signs, such as chest tightness, is crucial for timely intervention and better outcomes.
Have you or a loved one noticed any concerning symptoms? Real-world examples show that patients who report these symptoms quickly often receive more effective treatment. This underscores the importance of early detection. For older individuals, it’s essential to acknowledge the emotional and physical challenges that come with healing. Keeping an open dialogue with healthcare professionals can significantly enhance their care experience.
Our procedures, such as angioplasty and stent placement, are designed to help most individuals return home the same day, often feeling relief from symptoms within just a few days. Remember, you’re not alone in this journey; we’re here to support you every step of the way.
Regular Monitoring and Follow-Up Care
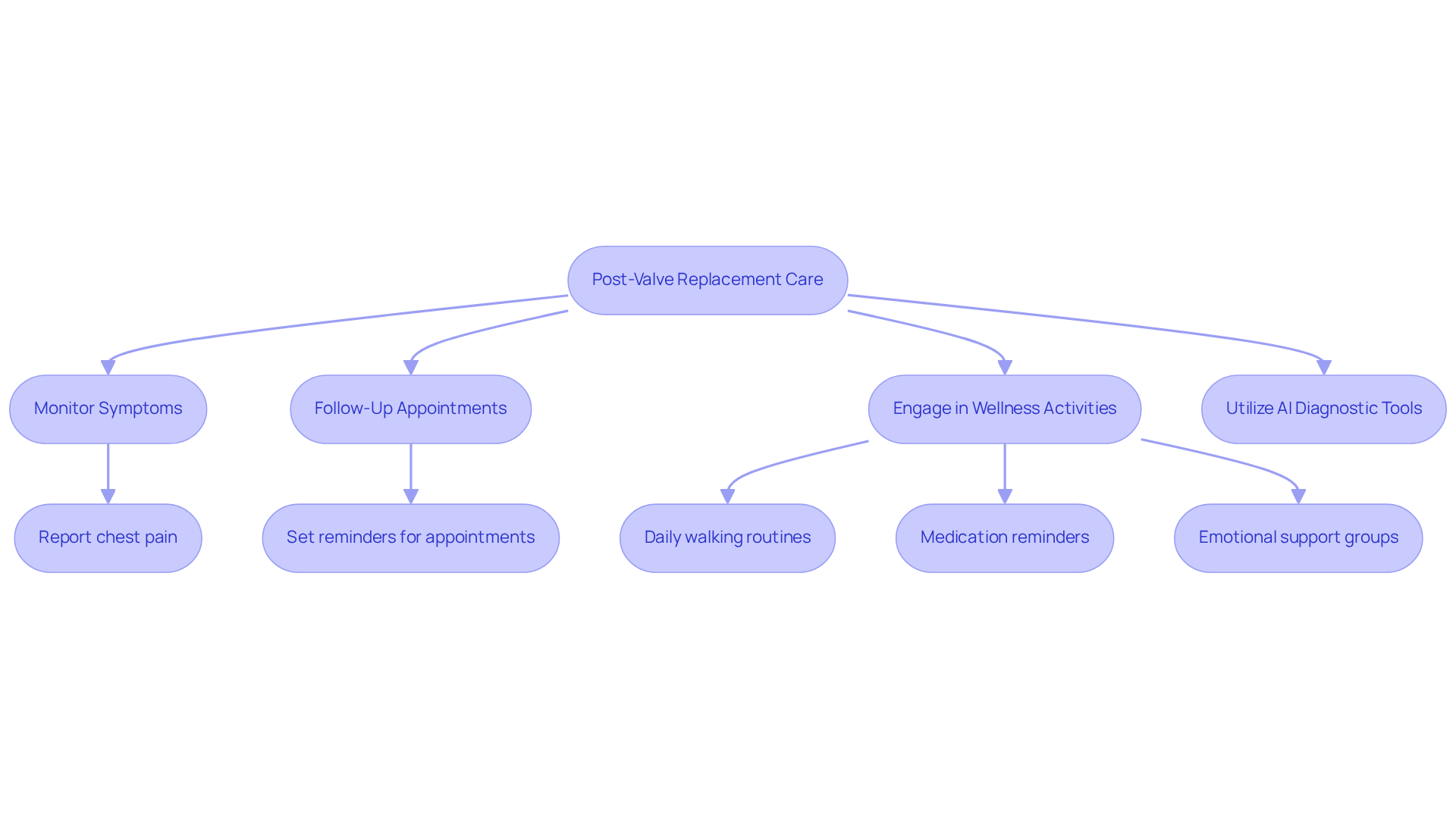
After valve replacement surgery, it’s crucial to keep a close eye on your recovery and health. Did you know that about 30% of patients miss their follow-up appointments? This can really slow down your healing process. At Amavita Heart and Vascular Health®, we understand how important it is to have thorough follow-up care to reduce the risk of heart attacks and improve your overall health.
If you notice any worrying symptoms like persistent chest pain, an irregular heartbeat, or feeling unusually tired, these could be signs of complications, so please reach out to your healthcare provider right away. Dr. Jane Smith, a cardiologist, reminds us, “Patient care requires a customized approach, considering their unique needs and possible complications.” Regular check-ins can help assess your physical activity, medication adherence, and emotional well-being, creating a supportive space for you to share your experiences.
Your healthcare team might suggest simple daily walking routines, reminders for your medications, or even emotional support groups as part of a comprehensive recovery plan. Furthermore, our innovative AI-driven diagnostic technology allows for real-time evaluations, ensuring accurate monitoring of your heart function and helping to catch any potential issues early.
By prioritizing follow-up care and using available resources, you can enhance your recovery and well-being. To make the most of your recovery, consider setting goals and daily activities. Staying engaged in your recovery process is key, and remember, you’re not alone on this journey.
Conclusion
Recognizing the signs of heart failure after valve replacement is essential for a smooth recovery and maintaining your heart health. Here are ten key symptoms to keep an eye on:
- Unexplained shortness of breath
- Persistent fatigue
- Swelling
- Irregular heartbeats
- Rapid weight gain
- Chronic cough
- Sleep disturbances
- Dizziness
- Chest pain
- Decreased ability to exercise
Each of these indicators reminds us how important it is to monitor your health closely and communicate openly with your healthcare team during this recovery journey.
If you notice concerning symptoms like rapid weight gain, a chronic cough, or sleep disturbances, please don’t hesitate to reach out. These signs could indicate complications that need immediate attention. Regular follow-up care and advanced diagnostic tools can significantly enhance your recovery outcomes and improve your quality of life.
Staying informed and proactive about your heart health after valve replacement can empower you to take charge of your recovery. By recognizing symptoms early and seeking appropriate care, you can navigate your healing journey with confidence and support. Remember, you’re not alone in this process; your healthcare professionals are here to assist you every step of the way.
Frequently Asked Questions
What is a common issue patients face after valve replacement surgery regarding breathing?
Many individuals may experience shortness of breath after valve replacement surgery, which can signal fluid buildup or changes in heart function. About 15.4% of patients experience breathing pattern dysfunction, which can indicate signs of heart failure.
Why is it important to monitor breathing patterns after valve replacement surgery?
Monitoring breathing patterns is crucial as sudden changes or worsening symptoms can indicate heart failure. Fluid retention can increase pressure in the lungs, making it harder to breathe comfortably.
How can exercise help patients after valve replacement surgery?
Engaging in regular aerobic exercise can help alleviate symptoms such as breathing pattern dysfunction and fatigue, improving overall recovery and heart health.
What are some signs of persistent fatigue after valve replacement surgery?
While some fatigue is normal post-surgery, persistent weakness that disrupts daily activities could signal heart failure. About 30% of individuals report ongoing fatigue, with energy levels not returning to pre-surgery levels.
How should patients track their energy levels after surgery?
Patients are advised to track their energy levels weekly and distinguish between normal post-exertion fatigue and concerning signs that may require medical attention.
What should patients do if they experience ongoing fatigue after valve replacement?
Any ongoing fatigue should prompt a conversation with a healthcare professional to rule out signs of heart failure and to develop personalized treatment plans.
What is a common symptom of fluid retention after valve replacement surgery?
Swelling in the legs or abdomen is a common symptom, with about 30% of patients experiencing this after surgery. It can indicate heart failure, especially when accompanied by shortness of breath or fatigue.
Why is it important to monitor weight after valve replacement surgery?
A sudden increase in weight can signal worsening fluid retention, and it’s important to report any significant changes to a healthcare provider for timely intervention.
How can patients ensure better outcomes regarding swelling and fluid retention?
Staying informed about the signs of fluid retention and addressing them promptly can lead to better outcomes and fewer complications in recovery.
List of Sources
- Unexplained Shortness of Breath
- Breathing Pattern Dysfunction and Physical Activity of Patients Following a Median Sternotomy After Hospital Discharge: A Cross‐Sectional Study – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC12301566)
- Persistent Fatigue and Weakness
- Tired After Heart Surgery – Lethargic, Lacking Energy (https://heart-valve-surgery.com/heart-surgery-blog/2012/08/22/tired-after-heart-surgery)
- Swelling in the Legs or Abdomen
- parade.com (https://parade.com/1187612/michelle-parkerton/quotes-about-heart-disease)
- Strike for a good cause | St. Vincent’s Medical Center (https://stvincents.org/about-us/news-press/news-detail?articleId=67049&publicid=395)
- Rapid Weight Gain
- Heart Failure Signs and Symptoms (https://heart.org/en/health-topics/heart-failure/warning-signs-of-heart-failure)
- 7 Early Warning Signs of Congestive Heart Failure You Shouldn’t Ignore – Vasculearn Network (VLN) (https://thrombosis.org/patients/patient-articles/7-early-warning-signs-of-congestive-heart-failure-you-shouldn-t-ignore)
- Chronic Cough or Wheezing
- Coughing or wheezing: could it be heart failure? (https://heartfailurematters.org/understanding-heart-failure/coughing-or-wheezing)
- Heart Failure Signs and Symptoms (https://heart.org/en/health-topics/heart-failure/warning-signs-of-heart-failure)
- Increased Sleep Disturbances
- parade.com (https://parade.com/1187612/michelle-parkerton/quotes-about-heart-disease)
- 100 Anxiety Quotes to Help Calm Your Mind on Tough Days (https://today.com/life/quotes/anxiety-quotes-rcna126836)
- Chest Pain or Discomfort
- parade.com (https://parade.com/1187612/michelle-parkerton/quotes-about-heart-disease)
- Regular Monitoring and Follow-Up Care
- 10 Patient Experience Quotes for Inspiration (https://carecloud.com/continuum/patient-experience-quotes-for-inspiration)
- Heart Valve Surgery Recovery and Follow Up (https://heart.org/en/health-topics/heart-valve-problems-and-disease/recovery-and-healthy-living-goals-for-heart-valve-patients/heart-valve-surgery-recovery-and-follow-up)
- St Vincent’s Heart Health (https://svhhearthealth.com.au/rehabilitation/after-heart-valve-surgery)
- 10 Inspiring Patient Experience Quotes | Relias (https://relias.com/blog/patient-experience-quotes)
- Patients who see a cardiologist after surgery may have a lower risk of heart disease (https://escardio.org/news/press/press-releases/patients-who-see-a-cardiologist-after-surgery-may-have-a-lower-risk-of-heart-disease)