Introduction
Peripheral Artery Disease (PAD) is a silent yet significant health concern that affects millions, especially seniors. It restricts blood flow to the limbs, leading to debilitating symptoms that can be distressing. As awareness grows, so does the potential for innovative treatments that promise to enhance quality of life and restore independence.
But with so many options available, how can individuals navigate the complexities of PAD management? It’s understandable to feel overwhelmed. This comprehensive guide delves into the latest advancements and personalized strategies for treating PAD, offering hope and clarity for those affected by this condition.
In addition to this, we’ll explore how these solutions can be tailored to meet your unique needs. Remember, you’re not alone in this journey. Together, we can find the most effective ways to manage PAD and improve your quality of life.
Define Peripheral Artery Disease (PAD)
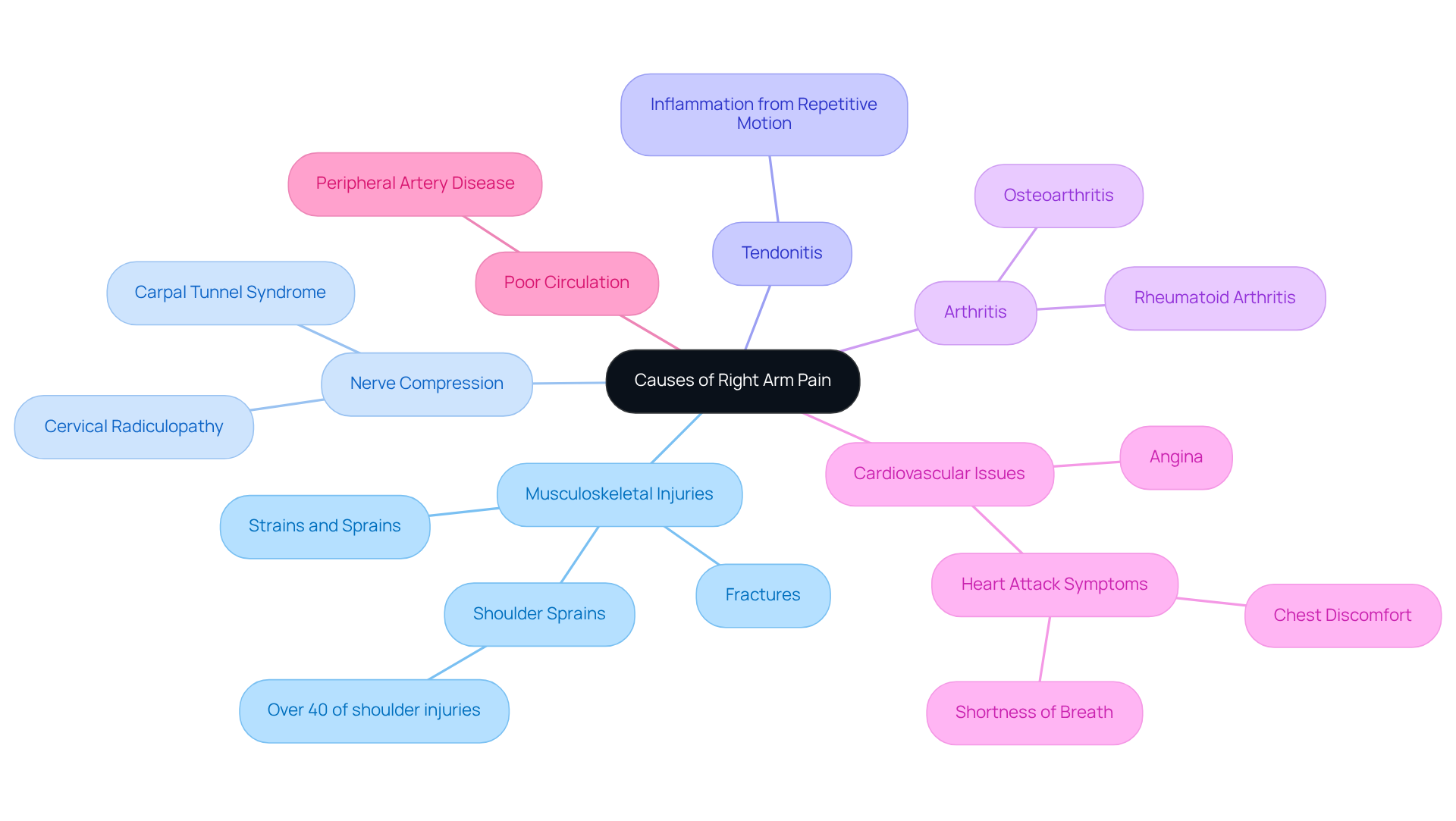
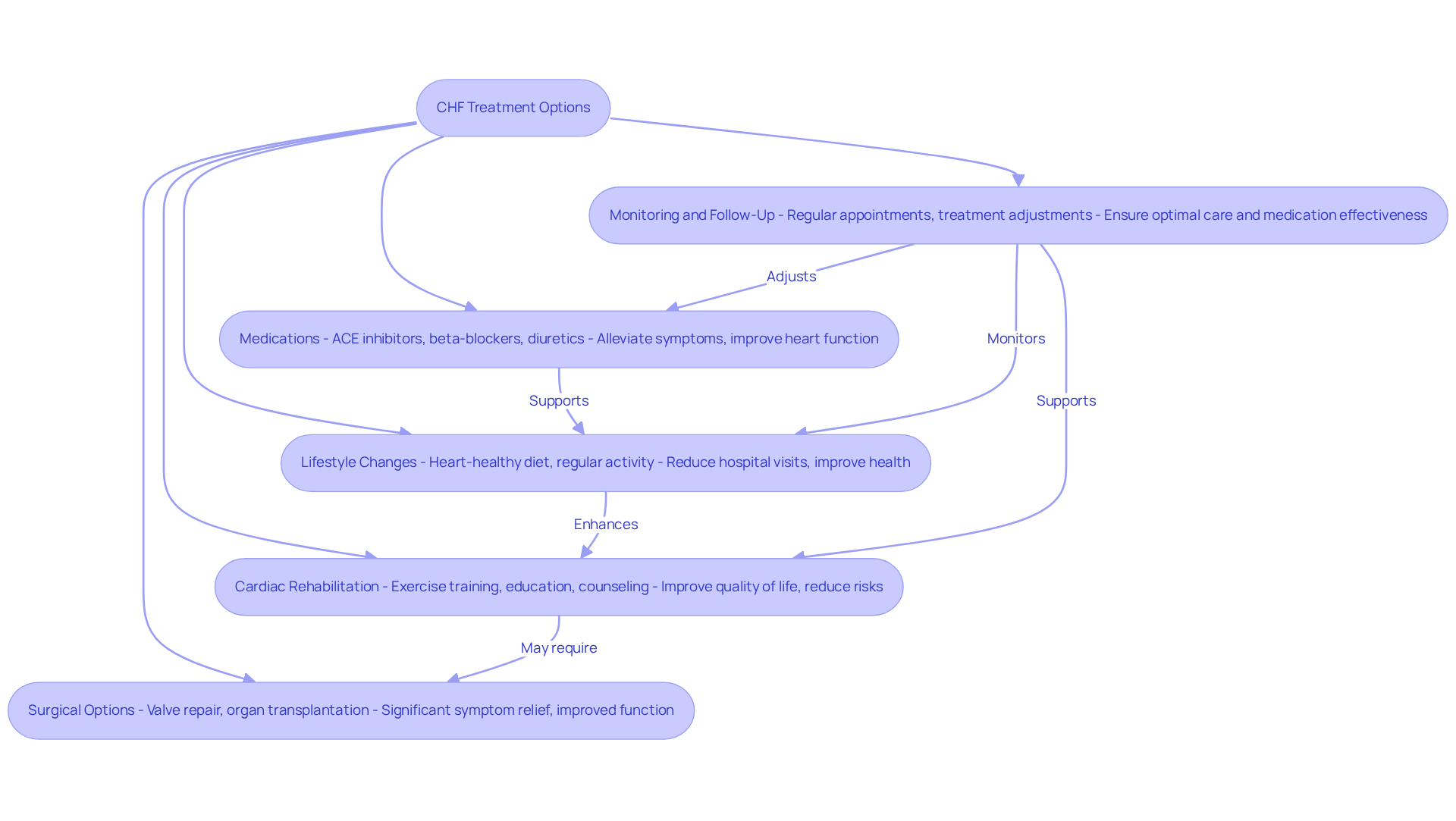
is a common circulatory condition that can significantly impact your daily life. It occurs when arteries narrow, limiting blood flow to your limbs, especially your legs. This narrowing often results from atherosclerosis, where fatty deposits build up in the artery walls. If you’ve experienced leg pain during activities, known as claudication, or numbness, you’re not alone. In severe cases, PAD can lead to complications, causing ulcers or gangrene, which can affect your mobility and overall quality of life.
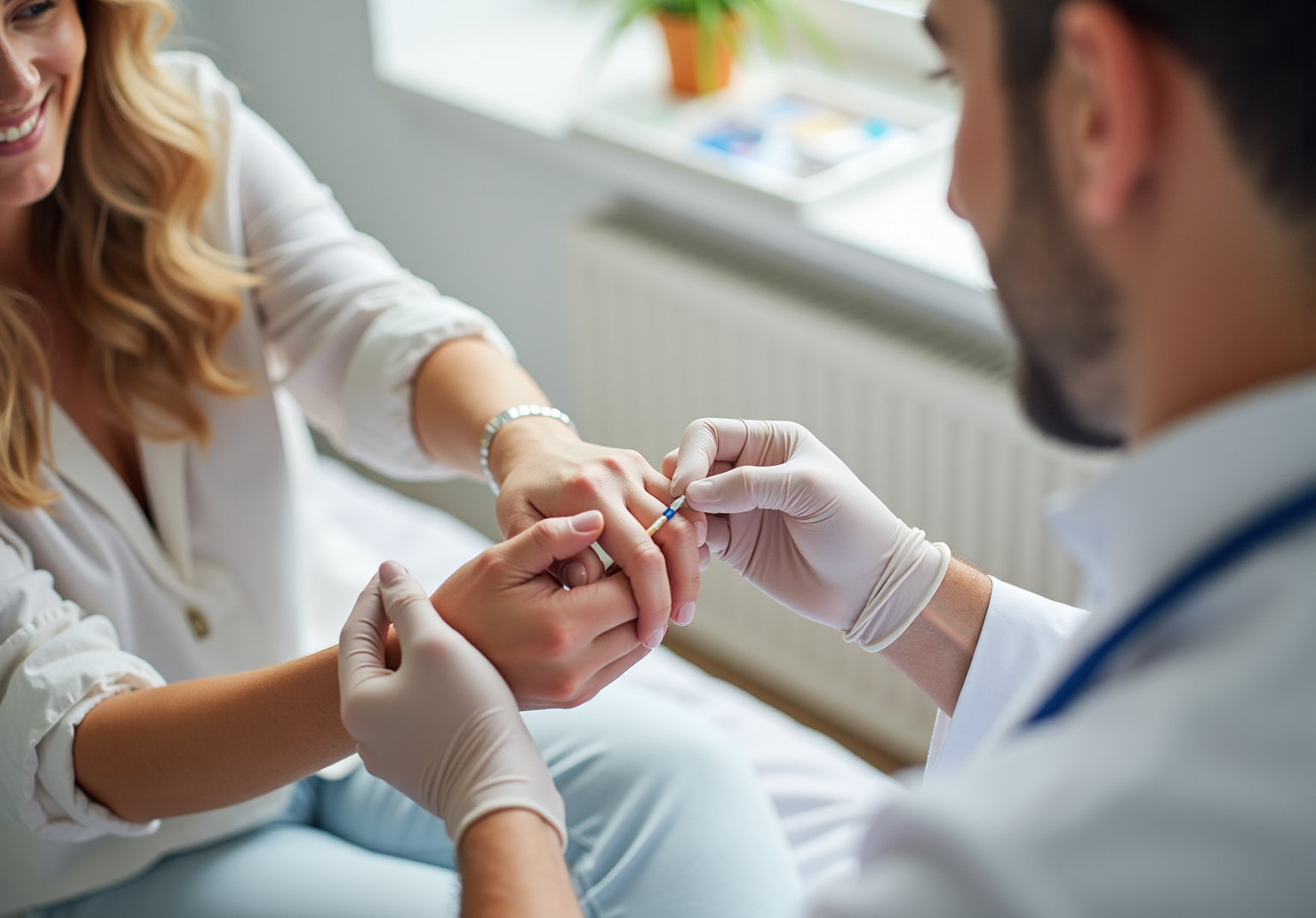
At Amavita Heart and Vascular Health, we understand the challenges associated with PAD. Our specialists are committed to providing support and exploring treatment options as well as innovative therapies. We use advanced imaging techniques to pinpoint blockages and offer procedures that can restore blood flow to your legs. Many of our patients report significant improvements in their walking distance and pain relief, often returning home the same day after outpatient procedures.
For seniors, the effects of PAD can be particularly concerning. This condition can make daily activities more difficult, leading to a loss of independence and increased reliance on caregivers. Preventive measures are crucial to prevent complications like heart attacks or strokes, which are more common in those with PAD. Cardiologists emphasize that recognizing the signs early can lead to better outcomes, as timely intervention can slow the disease’s progression. Dr. David G. Armstrong, a leading expert in the field, notes, “Patients with chronic limb-threatening ischemia (CLTI) do better when they are treated by a team,” underscoring the importance of a collaborative approach in managing PAD.
Recent studies reveal that PAD is often underdiagnosed. Approximately 6.5 million people aged 40 and older in the United States are affected by this condition. Many individuals share their experiences of struggling to walk or engage in activities they once enjoyed, highlighting the need for increased awareness and education about PAD and chronic venous insufficiency. This is especially vital for seniors, as early detection and effective intervention can make a significant difference in their lives. Furthermore, ongoing research into the causes of PAD continues to evolve, providing insights that can lead to improved treatments and better management and outcomes for those affected. At Amavita, our commitment ensures that our patients benefit from the latest therapies, often before they become widely available elsewhere.
Explore Standard Treatments for PAD
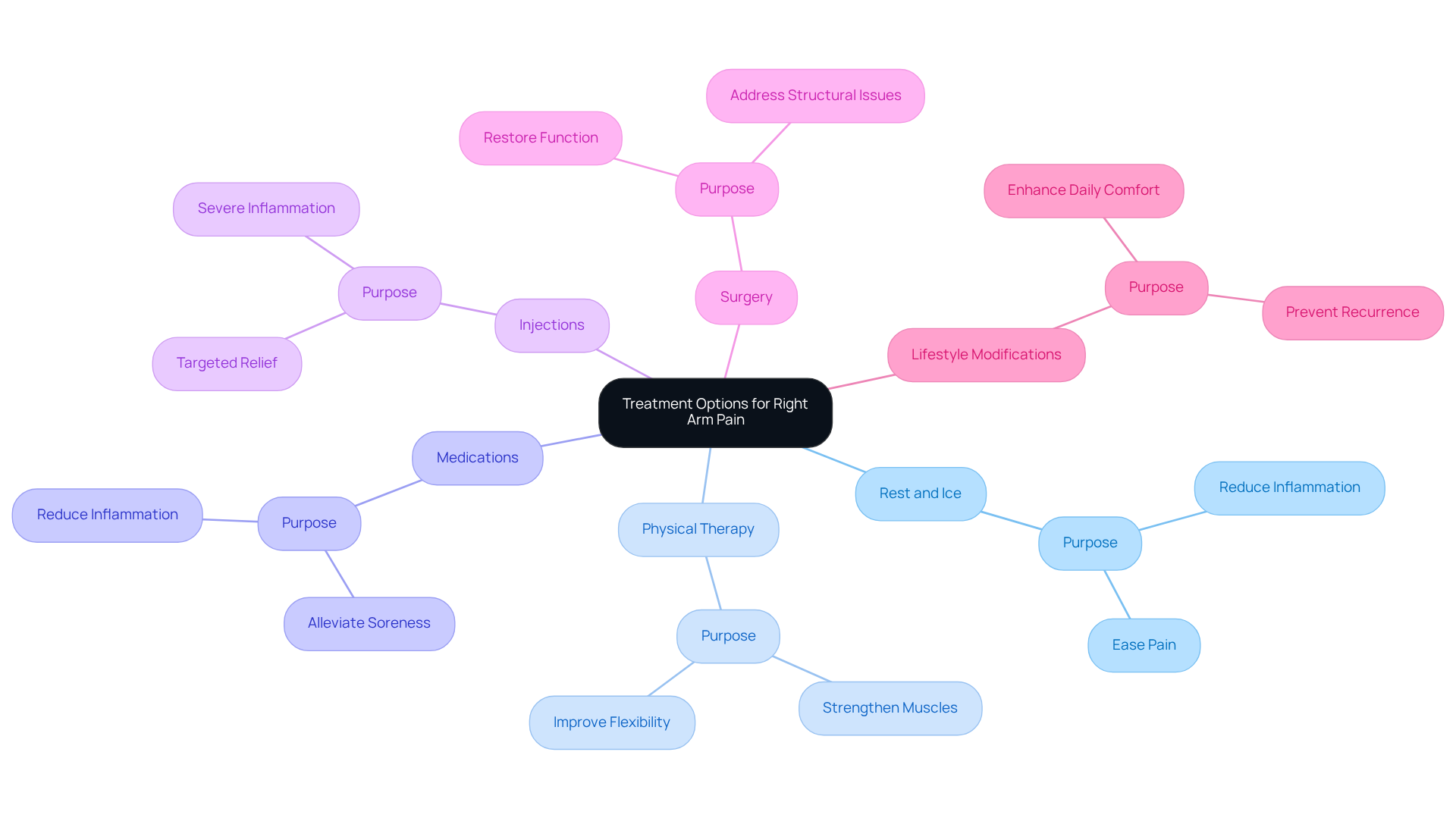
If you or a loved one is facing peripheral artery disease, it’s natural to feel concerned about your health. Understanding the steps you can take to manage this condition can be empowering. Conventional approaches for PAD often include lifestyle changes, medications, and, in some cases, procedures like angioplasty.
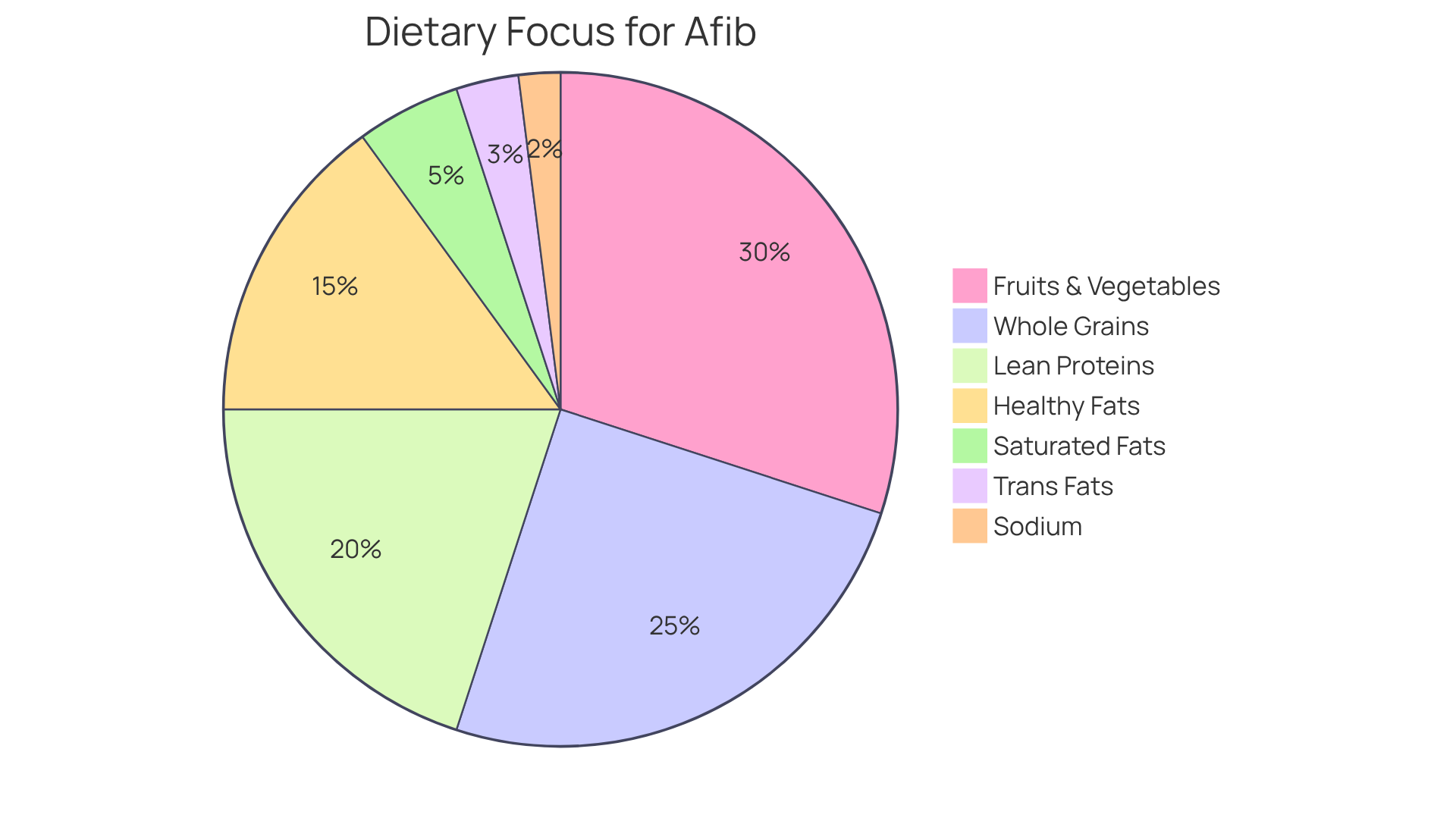
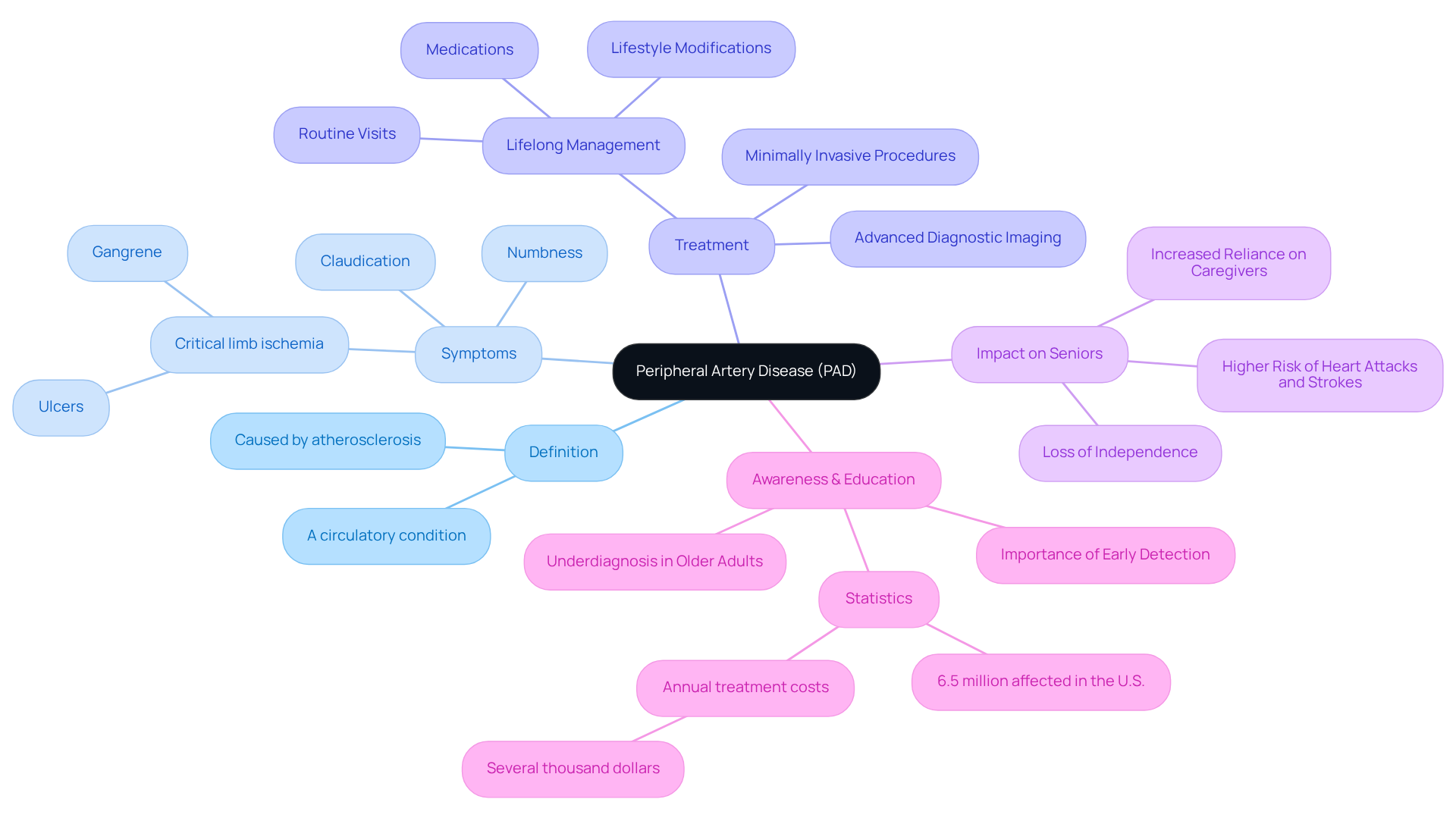
Making essential lifestyle changes can significantly enhance your vascular health. Consider adopting a diet filled with fruits, vegetables, and whole grains. Engaging in regular exercise—aiming for at least three sessions a week—can also make a difference. And if you smoke, quitting is one of the best gifts you can give your body. These changes not only help manage PAD but also improve your overall well-being.
Standard treatments include medications that play a crucial role in managing the condition. Antiplatelet agents are commonly prescribed to help prevent blood clots. Statins can assist in lowering cholesterol levels, which is vital for heart health. Another effective option is cilostazol, which enhances blood flow and alleviates the discomfort of claudication, an issue commonly addressed by healthcare providers.
In more severe cases, treatment may necessitate surgical interventions. Procedures like angioplasty, stenting, and bypass surgery aim to restore blood flow. These interventions work together to alleviate symptoms, enhance mobility, and significantly lower the risk of serious cardiovascular events. It’s reassuring to know that these approaches align with the latest clinical guidelines, emphasizing a comprehensive strategy for managing PAD.
Remember, you’re not alone in this journey. Seeking support and guidance from healthcare professionals can make a world of difference. If you have questions or need assistance, don’t hesitate to reach out. Your health and well-being are what truly matter.
Discover Emerging Treatments for PAD
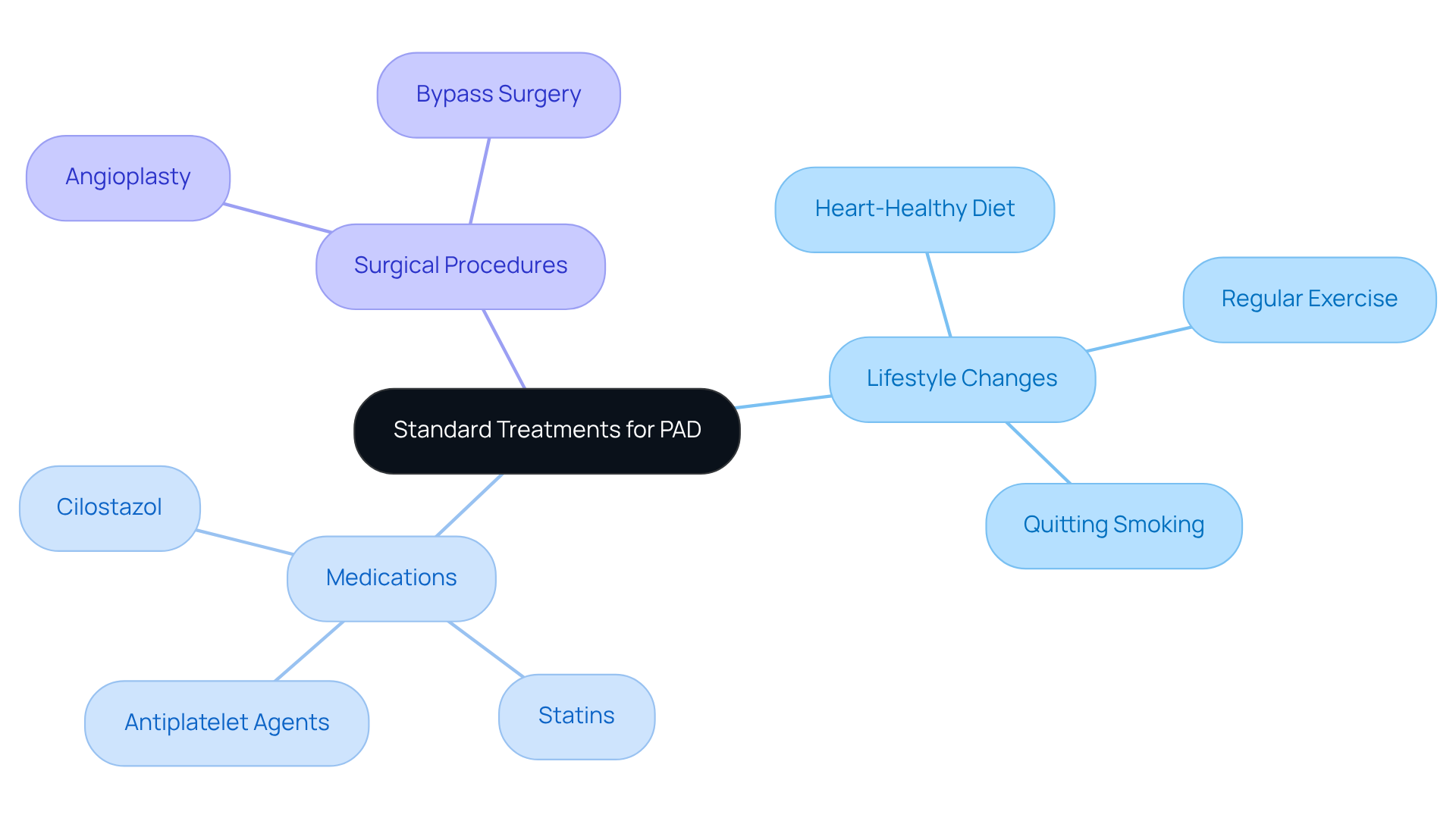
The landscape of care is being transformed by new technologies, which offer hope through advanced and innovative pharmacological therapies. At Amavita Heart and Vascular Health, we understand the concerns of high-risk individuals and are dedicated to providing focused cardiovascular treatment with the convenience of telehealth services. Recent advancements, like drug-eluting balloons, are designed to keep arteries open for longer, which can significantly reduce the need for repeat interventions. These devices have proven effective in clinical settings, with studies showing they enhance blood flow and relieve symptoms associated with PAD.
In addition to these advancements, we are excited about the potential of novel therapies, such as stem cell therapy and gene therapy, which are being actively researched to promote healing and improve circulation in affected areas. Clinical trials are currently evaluating the effectiveness of new medications, which have shown promise in helping individuals with PAD walk further and reduce cardiovascular risks. For example, a study involving around 800 individuals with diabetes and PAD found that those treated with GLP-1 drugs experienced significant improvements in mobility and overall health.
These groundbreaking approaches represent a significant shift towards more effective treatments for PAD, including minimally invasive procedures, which offer renewed hope for a better quality of life for those affected by this condition. At Amavita, our specialists are committed to providing advanced procedures, including angioplasty and stent placement, all with the convenience of outpatient care. We want our patients to return to their daily lives without the burden of limitations.
If you or a loved one are facing the challenges of PAD, know that you are not alone. We are here to support you every step of the way, ensuring you receive the compassionate care you deserve.
Personalize Your Treatment Plan for PAD
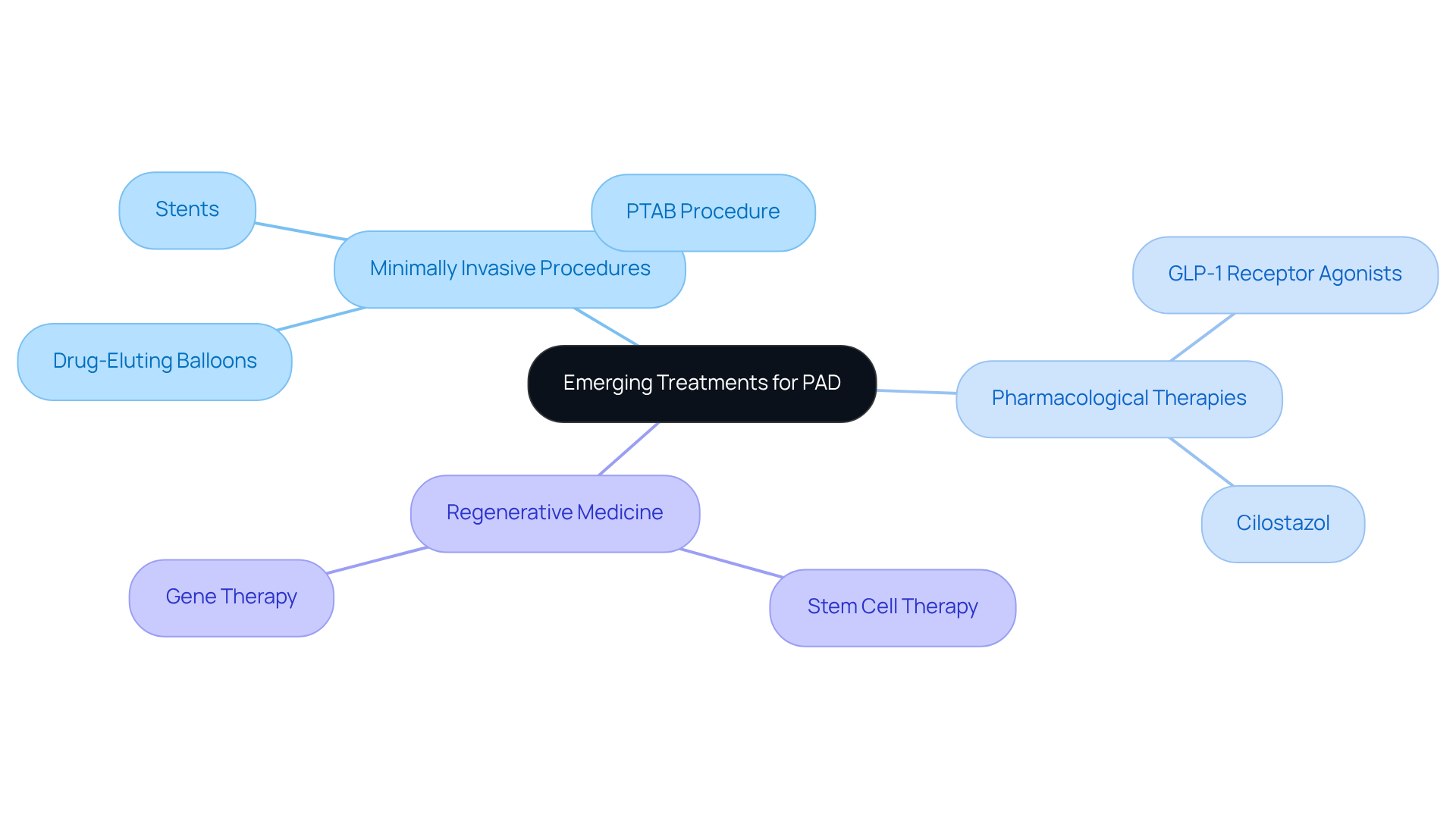
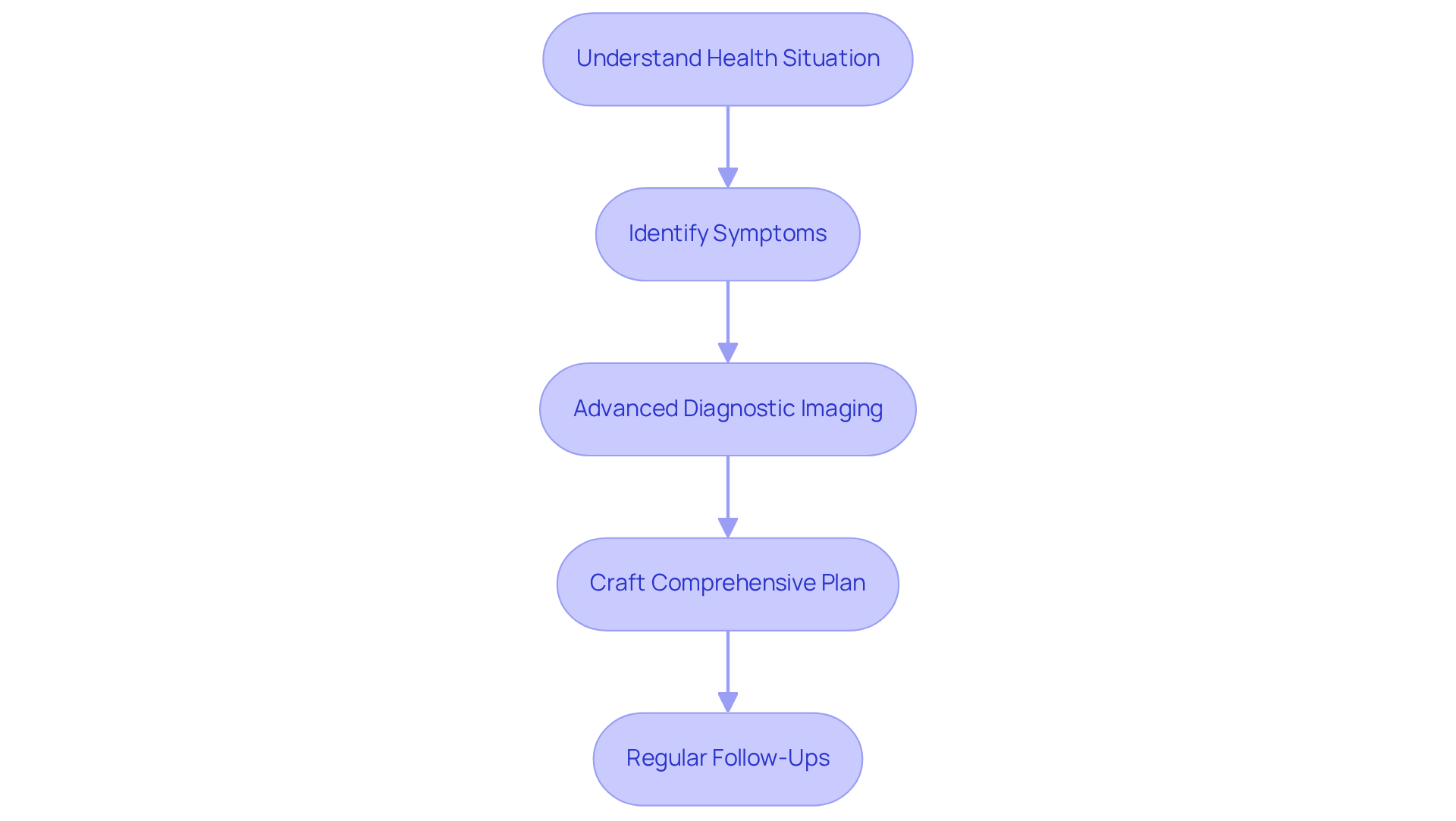
Creating a treatment plan for PAD starts with understanding your unique health situation, lifestyle, and specific symptoms, like leg discomfort or cramping when walking. At Amavita Heart and Vascular Health, our dedicated specialists use advanced imaging techniques to pinpoint any blockages. From there, we craft a comprehensive plan that includes lifestyle changes, medication management, and, if necessary, surgical interventions.
It’s crucial to work closely with your healthcare provider. Regular follow-ups play a vital role in monitoring and adjusting your care plan as needed, which can significantly impact your health outcomes. During these discussions, we consider various factors, including your existing health conditions, mobility levels, and personal preferences.
Have you thought about how exercise therapy could benefit you? Research shows that these programs can greatly improve walking ability and overall cardiovascular health. For example, participants in supervised exercise therapy have experienced impressive gains in walking performance, with average improvements in walking distance of:
- 27.9 meters for those attending the least
- 38.2 meters for those in the middle
- 56.9 meters for the most engaged participants—all significantly better than those who did not participate.
This collaborative approach not only enhances the effectiveness of treatment but also fosters a nurturing environment for managing the condition. At Amavita, we are committed to providing innovative and compassionate cardiovascular care, including patient education, to ensure you feel supported every step of the way. Remember, you’re not alone in this journey; we’re here to help you thrive.
Conclusion
Understanding Peripheral Artery Disease (PAD) is crucial for effectively managing this condition. Recognizing the symptoms of PAD and knowing the treatment options available can significantly enhance your quality of life. By focusing on lifestyle changes, medication management, and innovative surgical interventions, it becomes clear that a comprehensive approach is essential for those affected by PAD.
Have you considered how early diagnosis can prevent complications? Lifestyle adjustments play a vital role in enhancing vascular health, and there are promising advancements in treatment technologies. From standard medications to groundbreaking therapies like regenerative medicine, the landscape of PAD treatment is evolving rapidly, offering hope for better patient outcomes. It’s important to remember that the collaborative effort between you and your healthcare provider is key in personalizing treatment plans that cater to your individual needs.
Ultimately, the message is clear: proactive management and awareness of PAD can lead to improved mobility and a better quality of life. If you’re affected by PAD, don’t hesitate to seek support and explore the latest treatment options available. By staying informed and engaged in your care, you can navigate the challenges of PAD more effectively, ensuring a healthier future. Remember, you’re not alone in this journey; support is available, and together, we can work towards a brighter tomorrow.
Frequently Asked Questions
What is Peripheral Artery Disease (PAD)?
Peripheral Artery Disease (PAD) is a circulatory condition characterized by the narrowing of arteries, which limits blood flow to the limbs, particularly the legs. This narrowing is often caused by atherosclerosis, where fatty deposits accumulate in the artery walls.
What symptoms might indicate the presence of PAD?
Common symptoms of PAD include leg pain during activities, known as claudication, and numbness. In severe cases, it can lead to critical limb ischemia, resulting in ulcers or gangrene.
How does PAD affect seniors?
For seniors, PAD can significantly impact daily activities, leading to a loss of independence and an increased reliance on caregivers. Early diagnosis and proactive management are crucial to prevent complications such as heart attacks or strokes.
What treatments are available for PAD?
Treatments for PAD include advanced diagnostic imaging to identify blockages and minimally invasive procedures that can restore blood flow to the legs. Many patients experience significant improvements in walking distance and pain relief, often returning home the same day after outpatient procedures.
Why is early diagnosis important for PAD?
Early diagnosis is essential because recognizing the signs of PAD can lead to better outcomes. Timely intervention can slow the disease’s progression and reduce the risk of serious complications like heart attacks or strokes.
How common is PAD among older adults?
PAD is often underdiagnosed, especially among older adults. Approximately 6.5 million people aged 40 and older in the United States are affected by this condition.
What is the importance of a collaborative approach in managing PAD?
A collaborative approach in managing PAD is important because patients with chronic limb-threatening ischemia (CLTI) tend to have better outcomes when treated by a team of specialists, as emphasized by Dr. David G. Armstrong.
What ongoing efforts are being made to improve PAD treatment and management?
Ongoing research into the causes of PAD is evolving, leading to new treatments and better management strategies. At Amavita, there is a commitment to research and innovation, ensuring that patients benefit from the latest therapies.
List of Sources
- Define Peripheral Artery Disease (PAD)
- New Study Projects 360 Million Cases Of Peripheral Artery Disease By 2050, Driven By Metabolic Risk And Aging: Proactive Prevention Could Avert One In Three Cases – ALPS (https://limbpreservationsociety.org/news/new-study-projects-360-million-cases-of-peripheral-artery-disease-by-2050-driven-by-metabolic-risk-and-aging-proactive-prevention-could-avert-one-in-three-cases)
- cacvi.org (https://cacvi.org/new-treatments-for-pad)
- jnj.com (https://jnj.com/media-center/press-releases/johnson-johnson-one-year-data-demonstrate-durable-performance-and-safety-of-the-shockwave-javelin-peripheral-ivl-catheter-in-late-breaking-presentation-at-viva-2025)
- Study finds high rates of undiagnosed and untreated peripheral artery disease (https://news-medical.net/news/20250331/Study-finds-high-rates-of-undiagnosed-and-untreated-peripheral-artery-disease.aspx)
- BD Achieves Milestone in AGILITY Study of Revello™ Vascular Covered Stent for Treatment of Peripheral Artery Disease (https://news.bd.com/2025-11-04-BD-Achieves-Milestone-in-AGILITY-Study-of-Revello-TM-Vascular-Covered-Stent-for-Treatment-of-Peripheral-Artery-Disease)
- Explore Standard Treatments for PAD
- health.ucdavis.edu (https://health.ucdavis.edu/news/headlines/vascular-surgery-provides-patients-with-new-minimally-invasive-treatment-for-peripheral-artery-disease-/2025/05)
- jamanetwork.com (https://jamanetwork.com/journals/jama/article-abstract/2835911?resultClick=1)
- New Clinical Practice Guideline on the Management of Intermittent Claudication | Society for Vascular Surgery (https://vascular.org/news-advocacy/articles-press-releases/new-clinical-practice-guideline-management-intermittent)
- Updated Guideline for Peripheral Artery Disease: What’s New and Implications for Clinical Practice – PCNA (https://pcna.net/news/updated-guideline-peripheral-artery-disease)
- acc.org (https://acc.org/Latest-in-Cardiology/Articles/2025/04/02/13/44/Exercise-Therapy-in-Symptomatic-Peripheral-Artery-Disease)
- Discover Emerging Treatments for PAD
- health.harvard.edu (https://health.harvard.edu/diseases-and-conditions/a-new-approach-to-peripheral-artery-disease)
- cacvi.org (https://cacvi.org/new-treatments-for-pad)
- BD Achieves Milestone in AGILITY Study of Revello™ Vascular Covered Stent for Treatment of Peripheral Artery Disease (https://news.bd.com/2025-11-04-BD-Achieves-Milestone-in-AGILITY-Study-of-Revello-TM-Vascular-Covered-Stent-for-Treatment-of-Peripheral-Artery-Disease)
- health.ucdavis.edu (https://health.ucdavis.edu/news/headlines/vascular-surgery-provides-patients-with-new-minimally-invasive-treatment-for-peripheral-artery-disease-/2025/05)
- uabstvincents.org (https://uabstvincents.org/news/cardiology-team-at-uab-st-vincents-performs-innovative-new-treatment-for-peripheral-artery-disease)
- Personalize Your Treatment Plan for PAD
- cacvi.org (https://cacvi.org/new-treatments-for-pad)
- Checking your browser – reCAPTCHA (https://pmc.ncbi.nlm.nih.gov/articles/PMC11307706)
- usavascularcenters.com (https://usavascularcenters.com/blog/does-peripheral-artery-disease-require-multiple-treatments)
- acc.org (https://acc.org/Latest-in-Cardiology/Articles/2025/04/02/13/44/Exercise-Therapy-in-Symptomatic-Peripheral-Artery-Disease)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9798808)