Introduction
Focusing on heart health is more crucial than ever, especially as cardiovascular diseases remain a leading cause of mortality worldwide. It’s understandable to feel concerned about this; however, knowing the essential foods that contribute to a cardiac diet can empower you to make informed dietary choices that promote long-term wellness. This article gently explores ten vital foods that not only enhance heart function but also offer a myriad of health benefits.
What challenges might you face in incorporating these heart-healthy options into your daily meals? Understanding these obstacles is the first step toward overcoming them, leading to a healthier lifestyle. Remember, you are not alone in this journey, and there are supportive resources available to help you every step of the way.
Amavita Heart and Vascular Health: Comprehensive Cardiac Care Services
At Amavita Heart and Vascular Health, we understand that concerns about cardiovascular wellness can be daunting. That’s why we offer a wide range of services designed to improve your heart health. Our services address issues such as:
- Valve and structural cardiac conditions
- Arrhythmias
We prioritize your comfort and recovery through advanced treatments, including:
Studies show that nearly 90% of patients experience improved outcomes, allowing for quicker recovery times and greater comfort. You can trust that all our facilities meet strict quality standards regulated by the Agency for Health Care Administration (AHCA), ensuring a safe environment for your care.
Moreover, our commitment to innovative research means you can access cutting-edge therapies through active clinical trials. This dedication positions Amavita as a leading choice for cardiac care. Experts in the field, like Dr. Latha P. Palaniappan, emphasize the importance of patient-centered approaches, and we share that belief wholeheartedly.
At Amavita, we integrate technology with compassionate care, ensuring that you receive the attention you deserve. Our care model exemplifies this commitment, significantly reducing readmissions by up to 70% and enhancing hospital quality scores. We aim to be your strategic ally in improving cardiac services, providing you with the support you need every step of the way.
We invite you to reach out and discuss your heart health concerns with us. Together, we can create a plan that prioritizes your well-being and fosters a healthier future.
Fruits and Vegetables: Essential Components for Heart Health
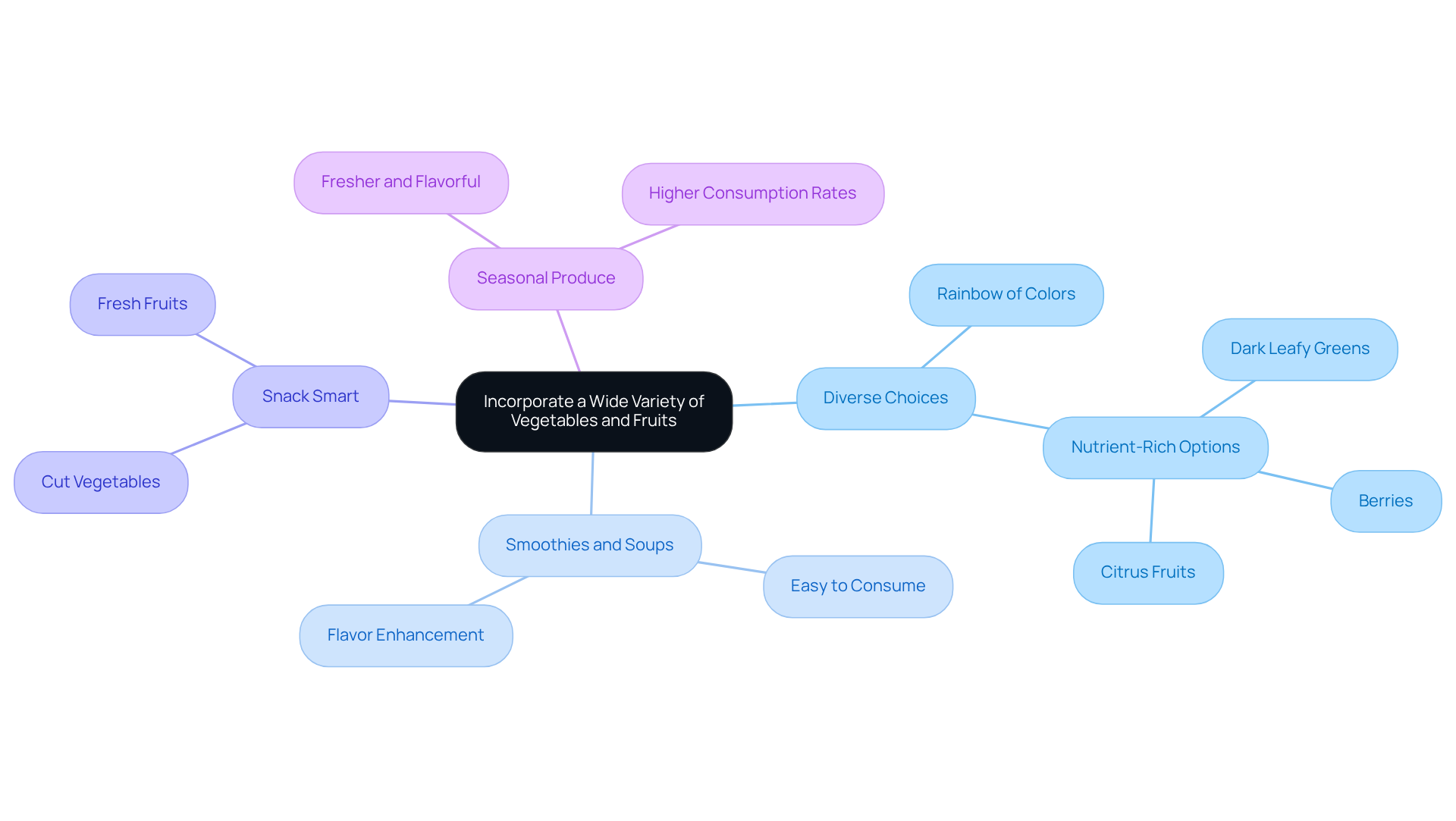
Fruits and vegetables are essential for your diet, packed with vital vitamins, minerals, and fiber. Leafy greens like spinach and kale, along with colorful fruits such as berries and oranges, significantly contribute to heart health. Studies have shown that these nutritious foods can help lower cholesterol, reduce inflammation, and enhance overall well-being. For instance, a systematic review published in the International Journal of Epidemiology found that a higher intake of fruits and vegetables is linked to a reduced risk of heart disease and improved mortality rates.
The American Heart Association encourages you to aim for five servings of fruits and vegetables each day to fully enjoy these health benefits. Incorporating a variety of produce not only boosts your nutrient intake but also makes your meals more enjoyable. As Dr. Andrew Freeman suggests, adding seasonings and sauces can enhance the flavor of vegetables, making them more appealing. By highlighting leafy greens and vibrant fruits, you can significantly improve your heart health.
However, it’s important to recognize that some individuals may face challenges in accessing fresh produce. If you find it difficult to incorporate these foods into your diet, remember that support is available. You’re not alone in this journey toward better health.
Whole Grains: Heart-Healthy Carbohydrate Choices
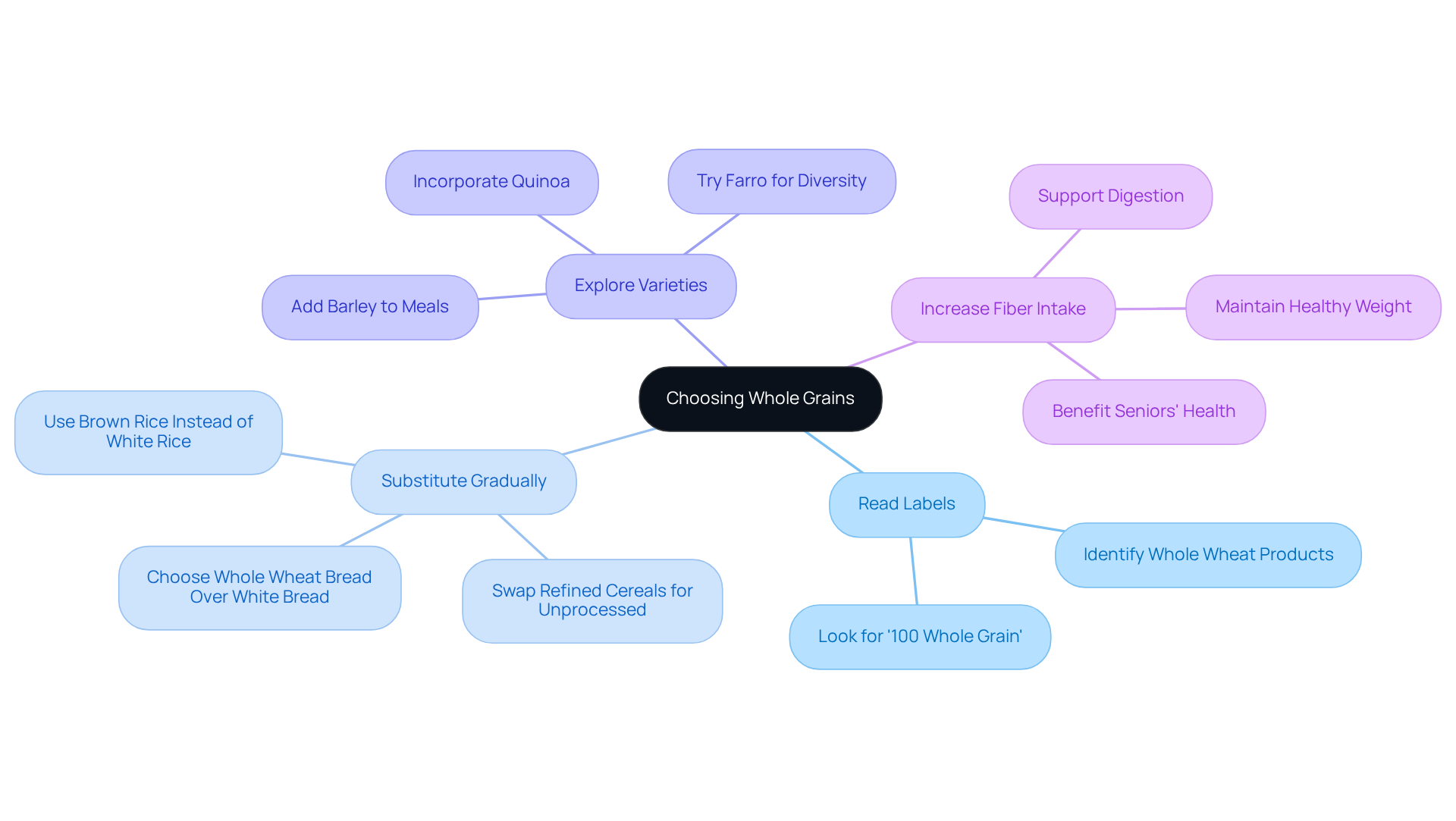
Whole grains, such as brown rice, quinoa, and whole wheat bread, are truly vital for a cardiac diet, thanks to their impressive fiber content. This fiber is essential for lowering and maintaining cholesterol levels, which many of us are concerned about. Unlike refined grains, which often lack important nutrients, whole grains keep their bran and germ, providing a richer nutrient profile that can support your overall health.
Research from a meta-analysis involving 6,360 participants reveals a reassuring fact: individuals who consume higher amounts of whole grains enjoy a 26% lower risk of heart disease compared to those who eat very little. To truly benefit from these heart-healthy advantages, aim for at least three servings of whole grains each day. The Dietary Guidelines suggest that at least half of the grains you consume should be whole grains, which is a simple yet impactful change you can make.
As nutrition specialists emphasize, increasing your fiber intake not only promotes heart health but also helps in managing blood sugar levels. This is particularly significant, considering that only 7% of American adults meet the recommended fiber intake of 14g per 1,000 calories. Furthermore, diets rich in refined grains can lead to digestive issues and increased inflammation, making whole grains an essential choice for anyone looking to enhance their overall well-being.
Remember, making these small adjustments can lead to significant improvements in your health. You’re not alone in this journey; there are nutritionists to help you make these positive changes.
Oily Fish: Omega-3 Rich Foods for Cardiovascular Support
Fatty fish, such as salmon, mackerel, and sardines, are rich in omega-3 fatty acids, which are essential for heart health. Have you ever considered how following a cardiac diet can impact your heart health? Studies suggest that frequent intake of these fish can lead to considerable advantages. These include improved cholesterol levels, reduced blood pressure, and diminishing the risk of heart disease. A systematic review found that individuals who consume at least two servings of oily fish experience a notable reduction in major cardiovascular events by approximately one-sixth. Furthermore, omega-3 fatty acids are associated with enhanced cardiac rhythm and decreased inflammation, both essential for preserving heart health.
Experts recommend incorporating oily fish into your diet at least twice a week to maximize these benefits. The American Heart Association supports this guideline, emphasizing that the heart-healthy advantages of eating fish surpass those of omega-3 supplements. Notably, a large-scale study revealed that participants with low fish intake saw a 40% reduction in cardiovascular events when they increased their omega-3 consumption. This highlights the importance of whole foods over supplements for cardiovascular support.
However, it is essential to be aware of potential risks associated with certain types of fish, such as mercury contamination, particularly in larger fish. The FDA recommends that most adults should eat two servings of omega-3-rich fish per week while being mindful of the types of fish consumed. Cooking techniques also count; grilling, broiling, or baking fish can help enhance nutritional advantages compared to deep-frying.
In summary, incorporating oily fish as a staple in your diet improves heart health and aligns with the latest research supporting its role in lowering the risk of cardiac disease. Aim for a minimum of two servings per week to reap the full benefits of these nutrient-rich foods. Remember, taking small steps towards a healthier diet can make a significant difference in your overall well-being.
Nuts and Seeds: Nutrient-Dense Options for a Cardiac Diet
Nuts and seeds, such as almonds, walnuts, flaxseeds, and chia seeds, are packed with nutrients like fiber, protein, and healthy fats. Regularly including these in your diet can lead to improved heart health and a reduced risk of heart disease. Have you considered how these foods can benefit your health? Lily Henderson, National Nutrition Advisor at the New Zealand Heart Foundation, shares that “Benefits to cholesterol are seen with as little as a handful.” Research supports this, showing that just 15 grams of nuts daily can lower the risk of heart disease by about 20%. Almonds, in particular, offer remarkable benefits; a clinical trial published in August in the journal Nutrients found that consuming two ounces each day can lower cholesterol and improve overall cardiovascular health.
Nutritionists emphasize the importance of incorporating nutritious fats from nuts into your meals. These foods not only support heart health but also provide essential nutrients that contribute to your overall well-being. In addition to this, regular nut consumption is linked to reduced inflammation and improved artery condition. Imagine the positive impact a small handful of nuts or a tablespoon of seeds each day can have on your heart wellness journey.
To make these foods a part of your daily routine, consider adding nuts to your morning oatmeal, blending nut butter into smoothies, or sprinkling seeds on your salads. Each step you take towards better nutrition is a step towards a healthier heart.
Low-Fat Dairy: Heart-Healthy Calcium Sources
Low-fat dairy items, such as skim milk, yogurt, and reduced-fat cheese, are wonderful sources of calcium and vitamin D, both vital for maintaining bone strength and supporting heart health. Have you ever considered how your daily ? Research shows that getting enough and may even help lower blood pressure, which is beneficial for heart health. In fact, a study from the Atherosclerosis Risk in Communities study found that higher in coronary arteries.
To enjoy these benefits, it’s recommended to incorporate two to three servings of into your daily meals. The DASH plan suggests two servings of low-fat, each day to boost calcium intake. This is especially important since many older adults only consume about 875 mg of calcium daily, which is below the recommended amounts of 1,000 mg for men aged 51 to 70 and 1,200 mg for women aged 51 and older.
Furthermore, experts emphasize that obtaining calcium primarily from food sources, rather than supplements, is better for optimal health outcomes. Dr. Cardoso advises, “I tell my patients to ensure they’re receiving .” Remember, you are not alone in this journey towards better health, and making small dietary changes can lead to significant improvements.
Lean Meats: Heart-Friendly Protein Choices
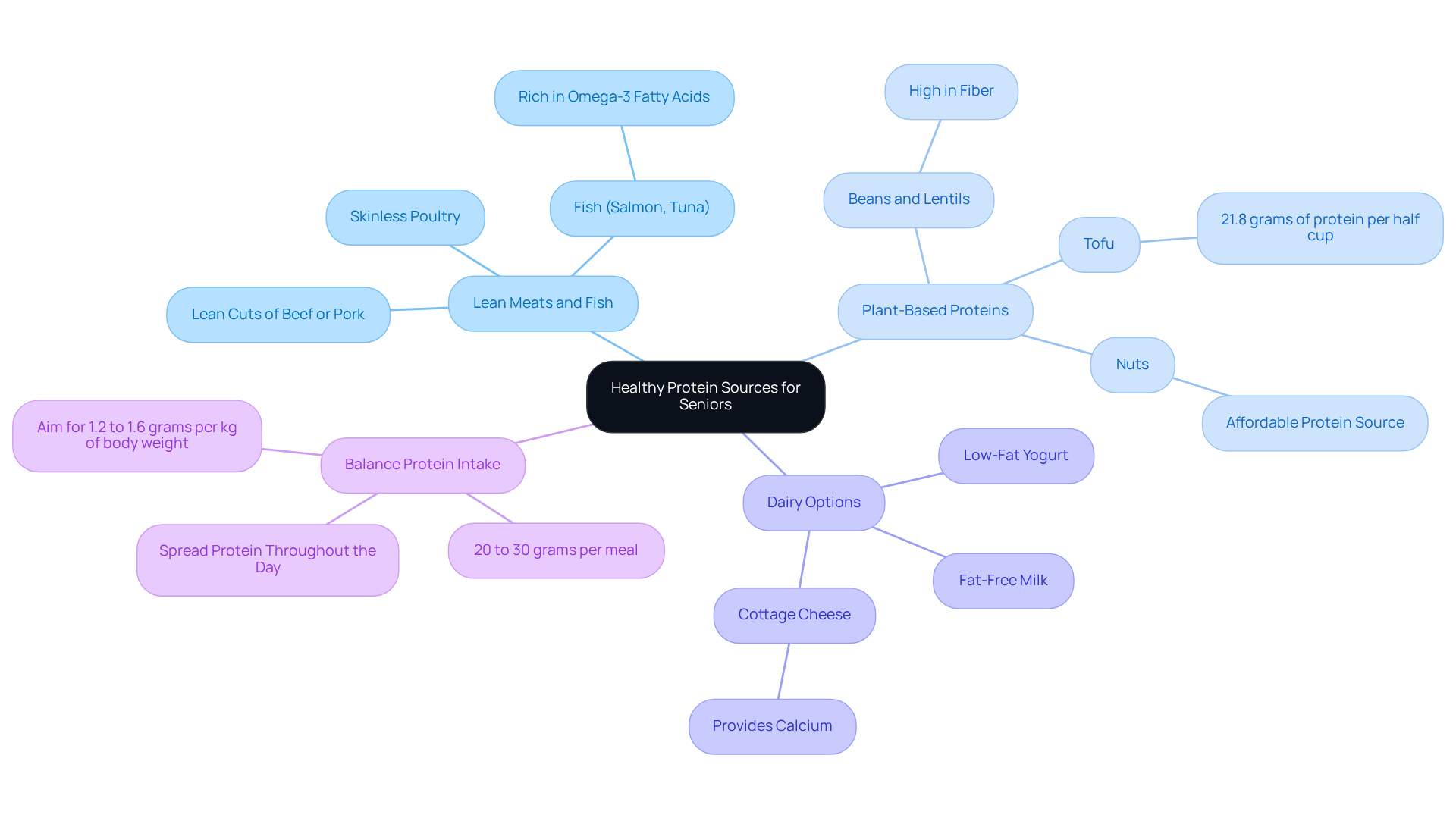
Lean meats, such as skinless poultry, fish, and choice cuts of beef or pork, are wonderful sources of protein without the concern of excessive saturated fat. These protein options are essential for maintaining muscle mass and overall health, particularly for older adults. When selecting meats, it’s important to prioritize those labeled as ‘lean’ and to be cautious with processed varieties, which often contain high levels of sodium and unhealthy fats.
Recent studies highlight the significance of protein sources in circulatory health, suggesting that incorporating lean meats into a balanced nutrition plan can positively influence heart health. For example, research indicates that a diet, which includes moderate amounts of lean red meat, can enhance gut microbiota diversity and lower cardiovascular risk factors, such as TMAO levels. As Wayne Campbell, a respected nutrition scientist, notes, “lean meats, when consumed as part of a balanced, nutritious meal plan, may not negatively affect gut or cardiovascular well-being.”
Moreover, protein intake is vital for maintaining strength and mobility as we age. This is especially important for older adults, as protein consumption can significantly impact overall health and quality of life. Therefore, integrating lean meats into your diet not only provides essential nutrients but also promotes long-term health outcomes. Consider incorporating lean meats into your meals while balancing them with plenty of fruits, vegetables, and whole grains. This holistic approach can be a comforting way to enhance your well-being.
Processed Foods: Items to Avoid for Heart Health
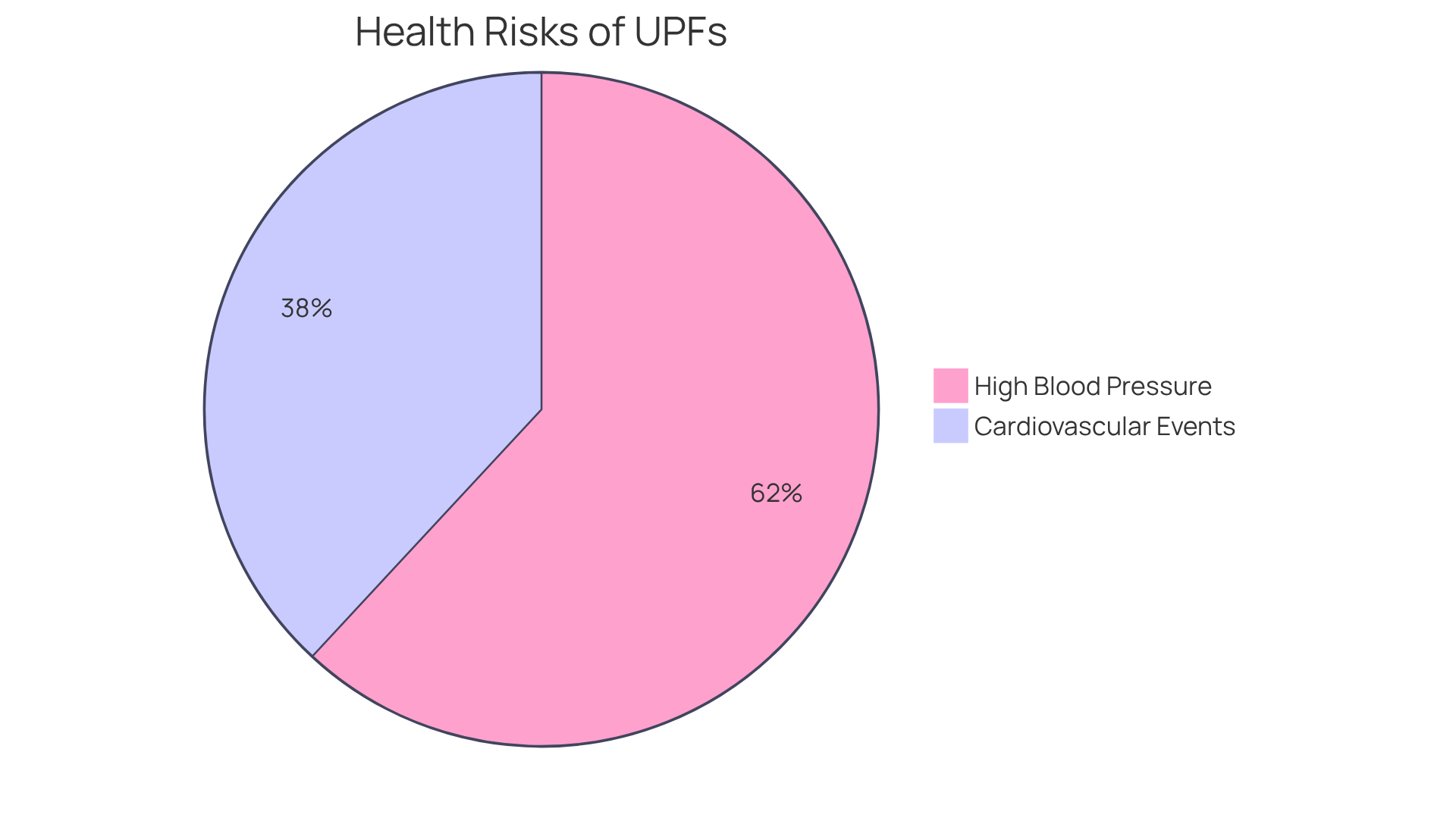
Processed foods, like fast food, packaged snacks, and sugary beverages, can be concerning due to their high levels of unhealthy fats, added sugars, and sodium. Have you ever wondered how these choices might affect your health? Studies reveal that individuals who consume the largest amounts of processed foods are:
- 39% more likely to develop high blood pressure
- 24% more likely to experience serious cardiovascular events, such as heart attacks and strokes
These ingredients not only contribute to health issues but also significantly elevate the risk of heart disease.
To support your heart health, it’s essential to adhere to a diet that limits the intake of these foods and focuses on whole, minimally processed foods. When shopping, consider looking for items with simple, recognizable ingredients and try to avoid those that contain chemical-sounding names. This small change can make a big difference in your health.
By making informed dietary choices from a balanced diet, you can effectively lower your risk of cardiovascular issues and enhance your overall well-being. Remember, you are not alone in this journey; taking these steps can lead to a healthier, happier you.
Sugar-Sweetened Foods: Reducing Intake for Better Heart Health
Sugar-sweetened foods, such as sodas, candies, and desserts, can significantly impact your health, especially if you are at a higher risk for conditions like diabetes or hypertension. Have you ever wondered how these choices affect your heart? Research has shown that consuming too much sugar is linked to higher triglyceride levels and lower HDL (good) cholesterol levels, both of which can be harmful to your heart health.
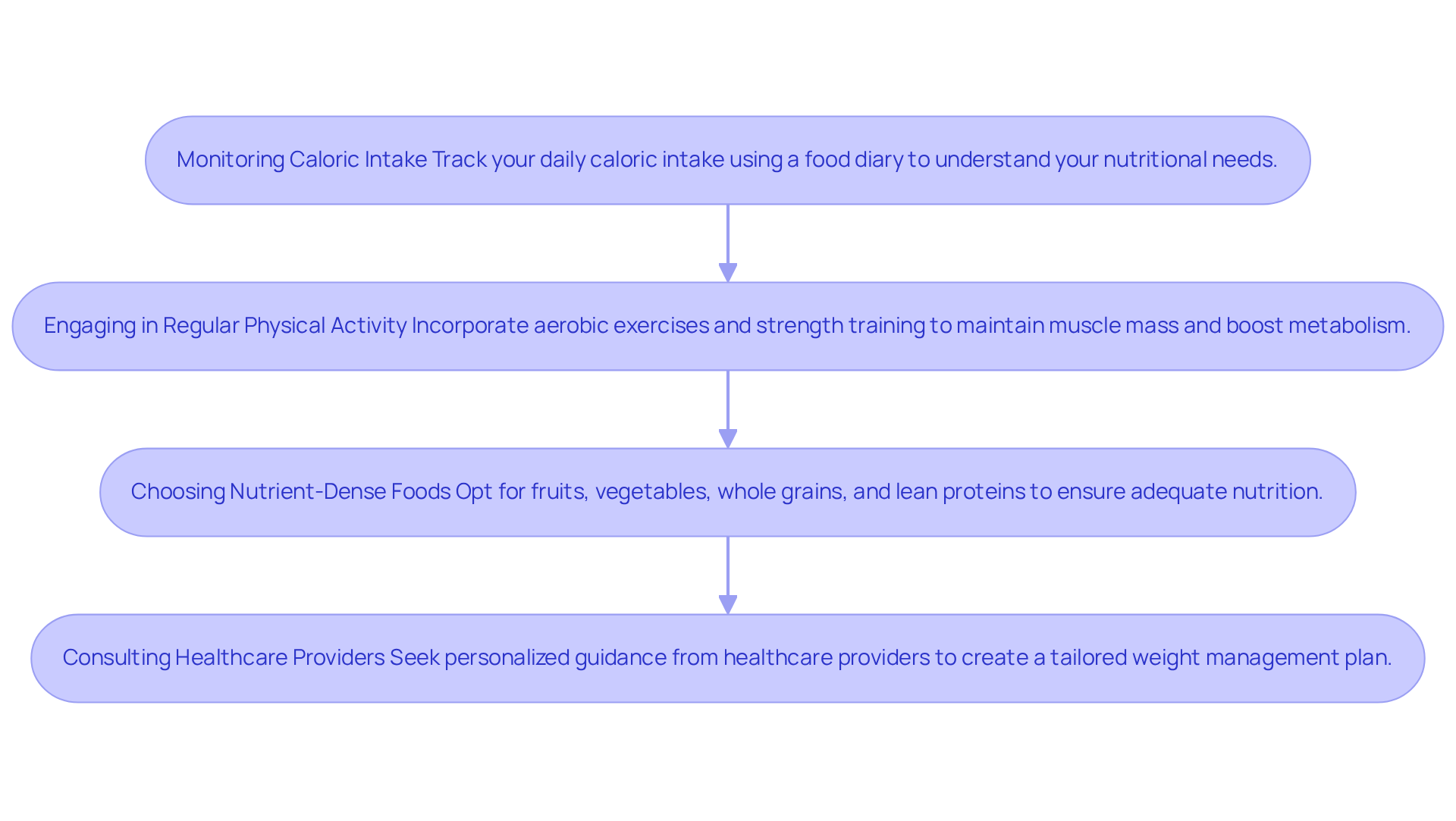
To reduce sugar intake, particularly if you fall into these at-risk categories, it’s advisable to keep track of your daily caloric intake. At Amavita Heart and Vascular Health, we truly believe that dietary changes can play a crucial role in reducing the risks associated with high sugar consumption. In fact, studies indicate that early dietary habits, like the first 1000 days of life, can lead to a lower risk of heart disease in the future.
Cardiologists emphasize that by making healthier food choices, you can achieve better cardiovascular outcomes. This highlights the importance of a diet tailored to your needs, along with the support we offer at Amavita. By making thoughtful choices to reduce added sugars, you can significantly improve your heart health. Remember, you are not alone on this journey; we are here to support you every step of the way.
Balanced Diet and Lifestyle: Keys to Sustaining Heart Health
To ensure your cardiovascular health is at its best, it’s important to follow a diet that embraces a balanced nutrition plan filled with a variety of fruits, vegetables, whole grains, lean proteins, and healthy fats. Studies show that a balanced diet is beneficial for heart health. For example, young adults who consume five or more servings of fruits and vegetables each day may see a 26% lower chance of developing calcified coronary artery plaque over two decades. Including fiber-rich foods, such as beans and whole grains, is also vital for heart health, as fiber helps regulate cholesterol levels and blood pressure.
The guidelines included in a cardiac diet for heart health. It emphasizes low sodium intake and encourages whole foods over processed ones. Regular physical activity complements these dietary choices, enhancing overall well-being. Simple activities like walking or taking the stairs can make a significant difference in maintaining a healthy cardiovascular system. Additionally, lifestyle factors such as avoiding smoking, managing stress, and getting enough sleep are essential parts of a heart-healthy routine.
Experts remind us that achieving cardiovascular health is a continuous journey. Dietary changes may seem overwhelming, but they don’t have to be perfect. It’s okay to enjoy an occasional treat, like birthday cake, as long as the overall focus remains on healthier choices. By incorporating these dietary and lifestyle habits into your daily routine, you can create a comprehensive approach that supports your heart health and enhances your quality of life.
Conclusion
Incorporating essential foods into a cardiac diet is crucial for maintaining and enhancing heart health. By emphasizing a balanced intake of fruits, vegetables, whole grains, lean proteins, and healthy fats, you can significantly reduce the risk of cardiovascular diseases. Each food group plays a unique role in promoting heart wellness, reinforcing the importance of making informed dietary choices for long-term health benefits.
Consider the key food categories highlighted in this article:
- Fruits and vegetables provide vital nutrients.
- Whole grains support healthy cholesterol levels.
- Oily fish are rich in omega-3 fatty acids, known for their cardiovascular benefits.
- Nuts and seeds contribute essential nutrients while minimizing unhealthy fats.
- Low-fat dairy and lean meats also provide important nutrients.
However, it’s vital to avoid processed and sugar-sweetened foods to reduce health risks associated with heart disease.
Ultimately, adopting a cardiac diet menu, complemented by a healthy lifestyle, can lead to significant improvements in cardiovascular health. Remember, small, consistent changes can lead to substantial benefits over time. Whether through dietary adjustments or lifestyle modifications, prioritizing heart health is a journey worth taking. Support is available to guide you on this path toward a healthier future. You are not alone in this; reaching out for help is a positive step towards your well-being.
Frequently Asked Questions
What services does Amavita Heart and Vascular Health offer for cardiac care?
Amavita Heart and Vascular Health offers a wide range of services, including treatments for coronary artery disease, valve and structural cardiac conditions, and arrhythmias, as well as minimally invasive procedures like cardiac catheterization and heart valve repair.
How effective are the minimally invasive procedures at Amavita?
Studies show that nearly 90% of patients experience significant benefits from minimally invasive procedures, leading to quicker recovery times and greater comfort.
What standards do Amavita facilities meet?
All Amavita facilities meet strict quality standards regulated by the Agency for Health Care Administration (AHCA), ensuring a safe environment for patient care.
What is the CardioElite™ program at Amavita?
The CardioElite™ program at Amavita integrates personalized treatment plans with compassionate care, significantly reducing readmissions by up to 70% and enhancing hospital quality scores.
Why are fruits and vegetables important for heart health?
Fruits and vegetables are essential for heart health as they are packed with vital vitamins, minerals, and fiber. They can help lower blood pressure, reduce inflammation, and improve overall cardiovascular well-being.
How many servings of fruits and vegetables should one aim for daily?
The American Heart Association recommends aiming for four to five servings of fruits and vegetables each day to enjoy their health benefits.
What are some examples of heart-healthy whole grains?
Heart-healthy whole grains include brown rice, quinoa, and whole wheat bread, which are rich in dietary fiber essential for lowering cholesterol levels and maintaining healthy blood pressure.
What is the recommended daily intake of whole grains?
It is recommended to aim for at least three servings of whole grains each day, with at least half of the grains consumed being whole grains.
How does increasing dietary fiber benefit heart health?
Increasing dietary fiber promotes cardiovascular health, helps manage blood sugar levels, and can lower the risk of hypertension, which is significant since only 7% of American adults meet the recommended fiber intake.
What challenges might individuals face in accessing fresh produce for heart health?
Some individuals may face difficulties accessing fresh produce, but support is available to help incorporate these essential foods into their diet for better health.
List of Sources
- Amavita Heart and Vascular Health: Comprehensive Cardiac Care Services
- Roundup: Heart Disease Still No. 1 Cause of Death as Risk Factors Rise Post-COVID; and More News (https://baptisthealth.net/baptist-health-news/heart-disease-still-top-cause-of-death-as-risk-factors-rise)
- nationalpress.org (https://nationalpress.org/topic/research-advances-in-cardiac-care)
- Fruits and Vegetables: Essential Components for Heart Health
- heartfoundation.org.au (https://heartfoundation.org.au/healthy-living/healthy-eating/fruit-vegetables-and-heart-health)
- Increasing fruit and vegetable consumption to reduce the risk of noncommunicable diseases (https://who.int/tools/elena/interventions/fruit-vegetables-ncds)
- A diet high in fruits and vegetables may reduce your heart and kidney disease risk, study says | CNN (https://cnn.com/2024/08/06/health/fruits-vegetables-heart-kidney-disease-wellness)
- Heart-healthy diet: 8 steps to prevent heart disease (https://mayoclinic.org/diseases-conditions/heart-disease/in-depth/heart-healthy-diet/art-20047702)
- okheart.com (https://okheart.com/news/the-heart-health-benefits-of-colorful-fruits-and-vegetables)
- Whole Grains: Heart-Healthy Carbohydrate Choices
- sciencedaily.com (https://sciencedaily.com/releases/2025/09/250909031513.htm)
- news-medical.net (https://news-medical.net/news/20250702/Looking-for-a-natural-way-to-lower-blood-pressure-Whole-grains-might-be-the-answer.aspx)
- theguardian.com (https://theguardian.com/wellness/2025/mar/24/are-whole-grains-healthy)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9185912)
- wholegrainscouncil.org (https://wholegrainscouncil.org/blog/2024/12/2025-dietary-guidelines-advisory-committee-report-affirms-importance-whole-grains)
- Oily Fish: Omega-3 Rich Foods for Cardiovascular Support
- Omega-3s for heart health? Exploring potential benefits and risks (https://nhlbi.nih.gov/news/2024/omega-3s-heart-health-exploring-potential-benefits-and-risks)
- mayoclinic.org (https://mayoclinic.org/diseases-conditions/heart-disease/in-depth/omega-3/art-20045614)
- news.mcmaster.ca (https://news.mcmaster.ca/two-servings-of-fish-per-week-helps-prevent-recurrent-heart-disease)
- Are you getting enough omega-3 fatty acids? (https://heart.org/en/news/2023/06/30/are-you-getting-enough-omega-3-fatty-acids)
- ods.od.nih.gov (https://ods.od.nih.gov/factsheets/Omega3FattyAcids-HealthProfessional)
- Nuts and Seeds: Nutrient-Dense Options for a Cardiac Diet
- foxnews.com (https://foxnews.com/food-drink/eating-one-type-nut-daily-could-lower-bad-cholesterol-improve-heart-health-study-finds)
- nutsforlife.com.au (https://nutsforlife.com.au/resource/nuts-seeds-and-heart-health-re-release)
- mayoclinic.org (https://mayoclinic.org/diseases-conditions/heart-disease/in-depth/nuts/art-20046635)
- Can nuts and seeds improve your heart health? (https://heartfoundation.org.nz/wellbeing/healthy-eating/nutrition-facts/nuts-and-seeds-for-heart-health)
- nutsforlife.com.au (https://nutsforlife.com.au/new-research-cholesterol-lowering-benefits-of-nuts-confirmed)
- Low-Fat Dairy: Heart-Healthy Calcium Sources
- health.harvard.edu (https://health.harvard.edu/heart-health/calcium-and-heart-disease-whats-the-connection)
- Which milk is safer for your heart? Decades of Norwegian data provide the answer (https://news-medical.net/news/20250805/Which-milk-is-safer-for-your-heart-Decades-of-Norwegian-data-provide-the-answer.aspx)
- sciencedirect.com (https://sciencedirect.com/science/article/pii/S0002916525004526)
- Is low-fat milk better than whole milk for heart health? | Harvard T.H. Chan School of Public Health (https://hsph.harvard.edu/news/is-low-fat-milk-better-than-whole-milk-for-heart-health)
- heart.org (https://heart.org/en/news/2024/04/15/cracking-the-calcium-code-to-understand-its-role-in-health)
- Lean Meats: Heart-Friendly Protein Choices
- medicalxpress.com (https://medicalxpress.com/news/2025-09-mediterranean-style-diets-cardiovascular-independent.html)
- news-medical.net (https://news-medical.net/news/20250123/Lean-red-meat-in-balanced-diet-supports-gut-and-heart-health-study-reveals.aspx)
- RFK Jr.’s new dietary guidelines could be controversial. Here’s what to watch for (https://npr.org/sections/shots-health-news/2025/10/08/nx-s1-5564026/dietary-guidelines-rfk-saturated-fat-2025)
- purdue.edu (https://purdue.edu/hhs/news/2025/07/purdue-nutrition-science-research-examines-metabolic-health-effects-of-red-meat-during-grilling-season)
- medpagetoday.com (https://medpagetoday.com/primarycare/dietnutrition/117590)
- Processed Foods: Items to Avoid for Heart Health
- Excessive ultraprocessed foods (UPFs) and poor nutrition tied to poor health (https://newsroom.heart.org/news/excessive-ultraprocessed-foods-upfs-and-poor-nutrition-tied-to-poor-health)
- acc.org (https://acc.org/About-ACC/Press-Releases/2025/05/08/14/10/Eating-Ultra-Processed-Foods-May-Harm-Your-Health)
- bhf.org.uk (https://bhf.org.uk/informationsupport/heart-matters-magazine/news/behind-the-headlines/ultra-processed-foods)
- ewg.org (https://ewg.org/news-insights/news/2025/08/link-between-ultra-processed-food-and-cardiovascular-disease)
- Sugar-Sweetened Foods: Reducing Intake for Better Heart Health
- hcplive.com (https://hcplive.com/view/reducing-sugar-intake-in-childhood-may-reduce-cardiovascular-disease-in-adulthood)
- physiology.org (https://physiology.org/detail/news/2025/04/25/popular-sugar-substitute-may-harm-brain-and-heart-health)
- Balanced Diet and Lifestyle: Keys to Sustaining Heart Health
- usnews.com (https://usnews.com/news/health-news/articles/2025-06-09/dont-sweat-the-weight-healthy-eating-helps-your-heart-regardless)
- Diet is key to heart health | Penn Medicine (https://pennmedicine.org/news/diet-is-key-to-heart-health)
- nhlbi.nih.gov (https://nhlbi.nih.gov/news/2025/nih-supported-dash-diet-named-best-heart-healthy-diet-and-best-diet-high-blood-pressure)
- gatorcare.org (https://gatorcare.org/2025/02/03/food-for-thought-american-heart-month-2025)
- nutrition.ucdavis.edu (https://nutrition.ucdavis.edu/news/fuel-your-heart-how-nutrition-supports-cardiovascular-health)