Introduction
Navigating the complexities of joint pain treatment can feel overwhelming, can’t it? Especially when you’re faced with choices like Genicular Artery Embolization (GAE) and traditional surgery. GAE offers a minimally invasive alternative that not only aims to provide significant pain relief but also brings potential financial benefits through varying insurance coverage.
However, the intricacies of health insurance and the risks associated with each procedure can leave you wondering: is GAE truly a safer and more cost-effective solution, or does traditional surgery still hold the upper hand in effectiveness?
This article gently explores the nuances of both options, shedding light on the path toward informed decision-making for those seeking relief from chronic joint discomfort. Remember, you’re not alone in this journey, and understanding your choices is the first step toward finding the care you deserve.
Understand Genicular Artery Embolization (GAE) as a Non-Surgical Alternative
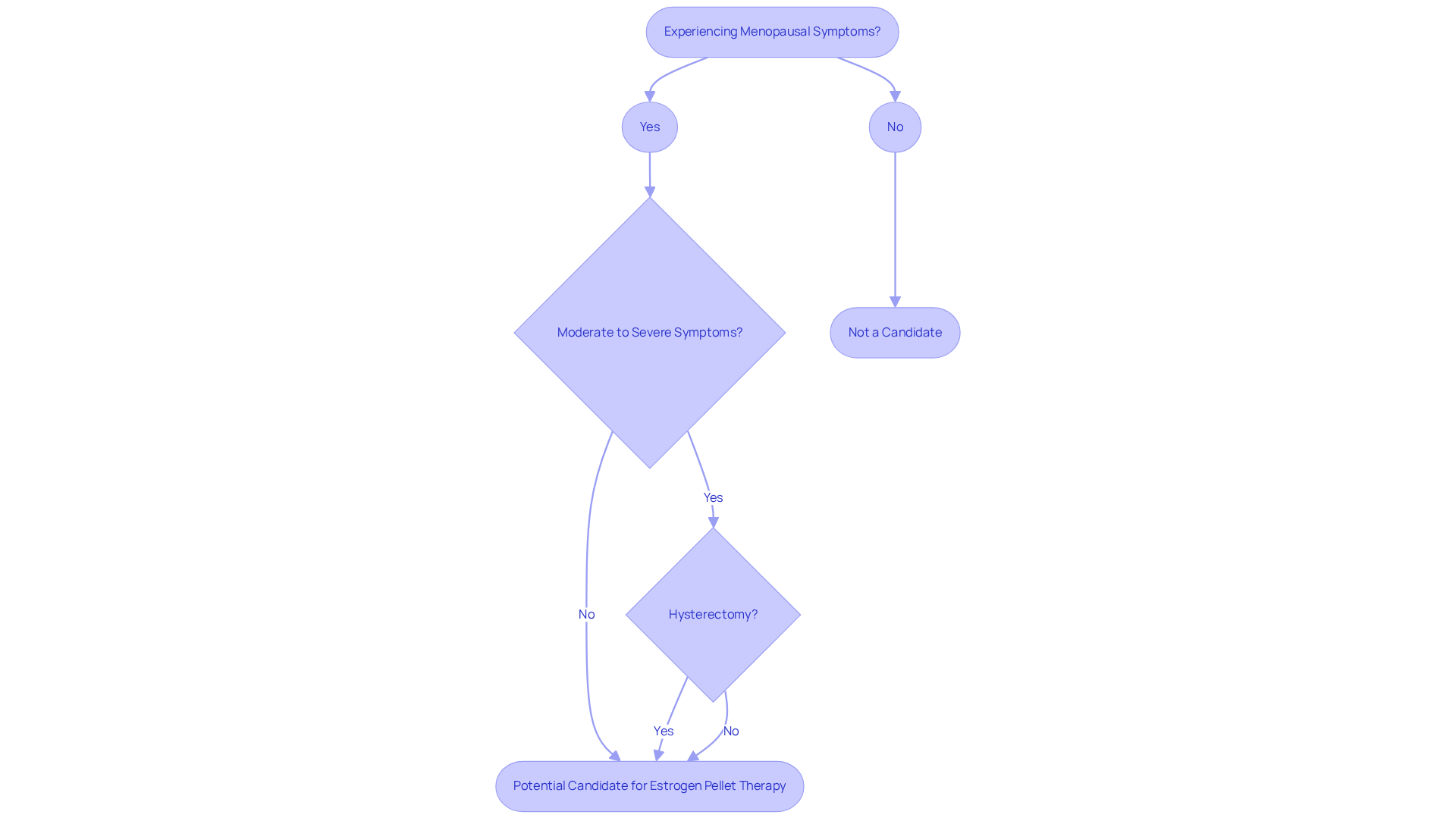
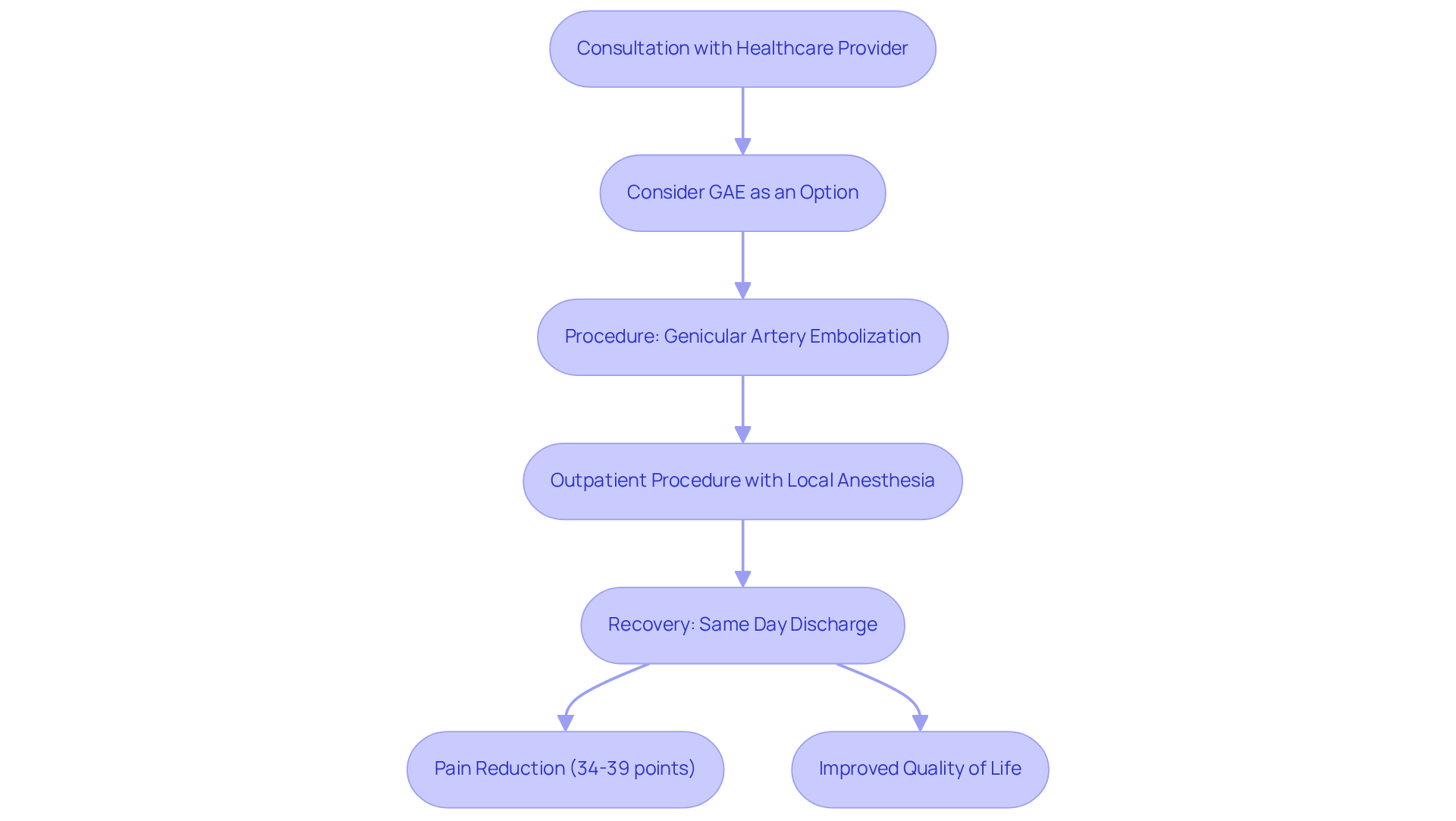
Genicular Artery Embolization (GAE) is a minimally invasive procedure, particularly for those dealing with osteoarthritis. This procedure involves selectively targeting arteries, which supply blood to the leg joint. By reducing blood flow to inflamed tissues, GAE aims to ease pain and improve function, all without the need for traditional surgical options like joint replacement.
Performed on an outpatient basis, GAE typically uses local anesthesia, allowing for a quicker recovery than conventional surgeries. Most patients can return home the same day and often resume their regular activities within just a few days. This makes GAE an attractive option for anyone seeking relief from chronic knee pain without the risks associated with major surgery. It’s especially beneficial for older adults who may have other health issues that complicate recovery, aligning perfectly with a focus on geriatric care.
Recent studies show that GAE is highly effective, with about 99.7% of procedures achieving their goals. Patients who undergo GAE report a reduction in pain between 34 to 39 points on the discomfort scale over a year, highlighting its effectiveness in improving quality of life. Moreover, GAE offers a viable option as a treatment alternative for those not ready for surgery, particularly individuals with conditions like severe obesity or poorly controlled diabetes, who might not be candidates for traditional surgery.
As the medical field continues to seek innovative treatments, GAE stands out, especially for older adults looking for non-invasive solutions. If you or a loved one are struggling with knee discomfort, consider discussing GAE with your healthcare provider. You deserve to find relief and regain your mobility.
Compare Insurance Coverage for GAE and Traditional Surgery
Navigating insurance coverage can feel overwhelming, especially when you’re trying to make the best decision for your health. It’s important to know that coverage varies significantly among providers and plans. While many private insurers and Medicare may cover GAE, they often require documentation to validate the medical necessity of the procedure. If you have Traditional Medicare Part B, you’ll find that it covers 80% of the costs associated with GAE, leaving you responsible for the remaining 20%. In contrast, traditional surgery is generally well-covered by most insurance plans, as it’s considered a standard treatment for severe osteoarthritis.
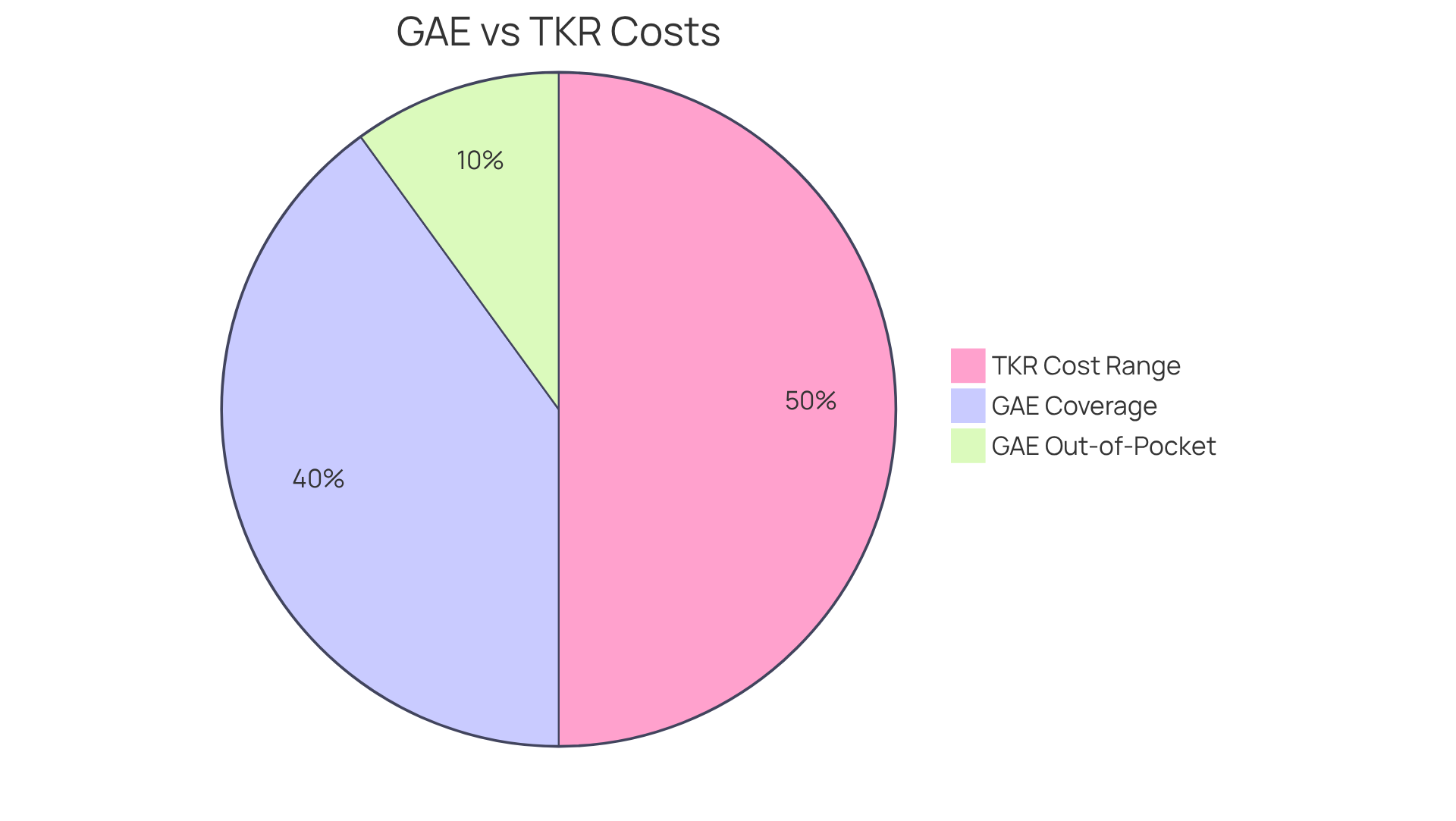
When it comes to out-of-pocket expenses, GAE typically ranges from $1,500 to $2,500, depending on your insurance plan. Most individuals under Traditional Medicare can expect to pay within this range for GAE. In comparison, traditional knee replacement surgeries can incur costs between $30,000 and $50,000, which includes hospital stays and rehabilitation. Additionally, keep in mind that the yearly Part B deductible for Medicare in 2025 is $240. This is an important factor to consider when assessing your overall expenses.
This stark difference in potential costs makes the GAE procedure an appealing choice for those concerned about financial burdens. However, it’s crucial to note that insurers like Anthem, Cigna, Humana, and Aetna may label GAE as investigational or experimental, which could pose coverage challenges. Always verify your specific coverage details with your insurance provider to avoid unexpected expenses. Furthermore, the GAE procedure can lead to lower overall costs due to less postoperative care required, further emphasizing its financial advantages over traditional surgery.
If you’re feeling uncertain about your options, remember that you’re not alone. Many patients share similar concerns, and it’s perfectly okay to seek guidance. Reaching out to your healthcare provider can help clarify your choices and ensure you feel supported every step of the way.
Evaluate Effectiveness and Outcomes of GAE vs. Traditional Surgery
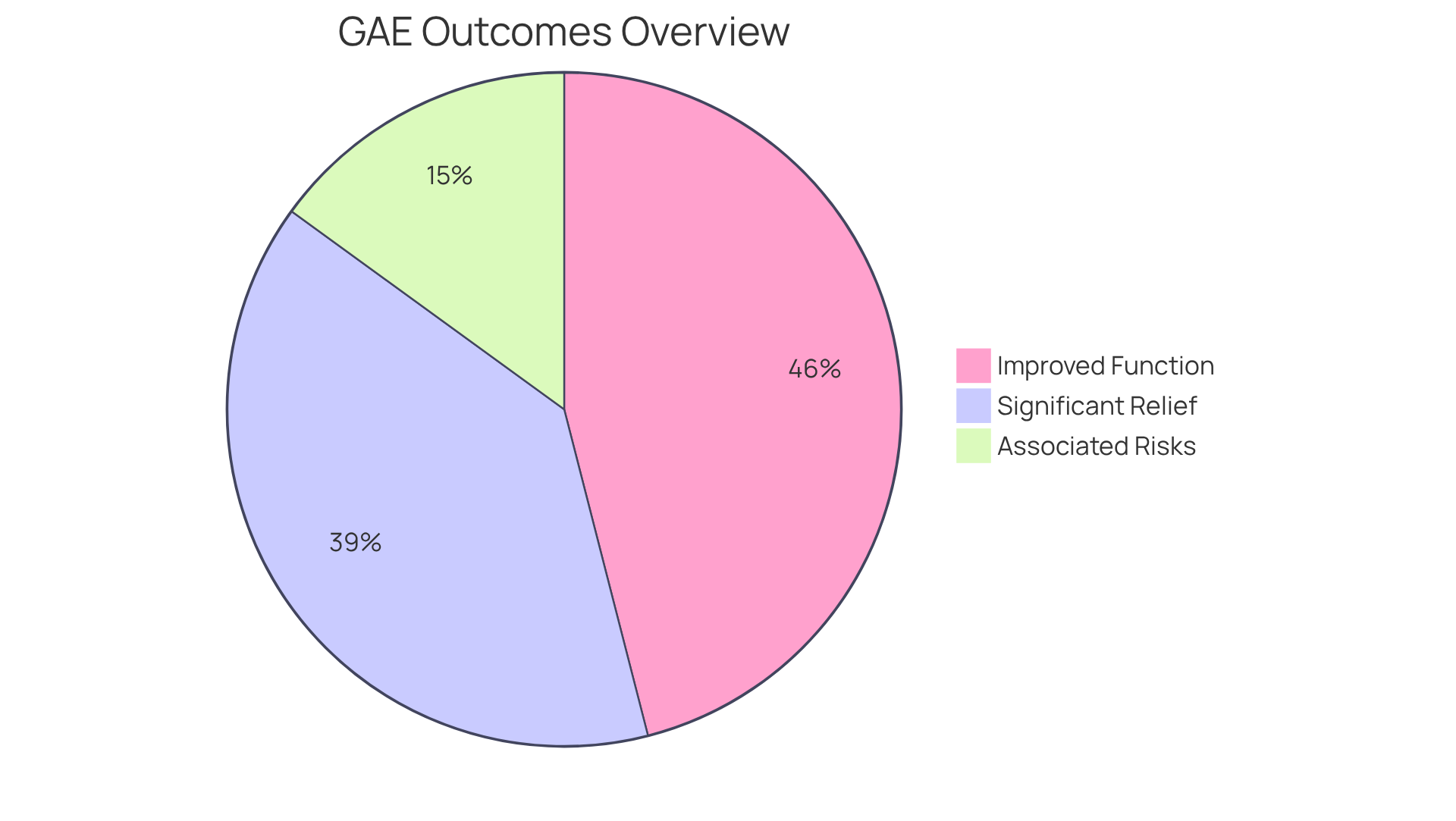
Genicular Artery Embolization (GAE) offers a promising solution for those struggling with joint pain. Research shows that:
- 78% of individuals experienced significant relief, with average discomfort scores dropping from 8/10 to 3/10.
- 92% reported improved joint function one year after the procedure.
- Many patients found enhanced mobility and a reduced need for pain medications, enjoying lasting benefits that can extend up to two years.
For individuals experiencing moderate to severe osteoarthritis and not prepared for surgery, the procedure offers a viable option.
On the other hand, traditional surgery often provides a higher success rate in pain relief, with many individuals experiencing significant improvement. However, the recovery can be lengthy, often requiring weeks of rehabilitation and physical therapy. It’s important to consider complications such as infection, blood clots, and implant failure—concerns that are less common with GAE, although GAE does have its own risks, including bleeding, infection, and temporary skin discoloration.
While joint replacement may deliver quick and significant results for severe cases, GAE stands out as a gentle alternative for patients seeking a non-invasive option with a reassuring safety profile. Recent studies suggest that the procedure can effectively delay or reduce the need for surgery, making it a desirable choice for many individuals experiencing chronic pain.
If you’re feeling overwhelmed by your joint pain, know that there are options available. GAE could be the compassionate solution you’ve been looking for. Don’t hesitate to reach out for support and explore how this procedure might help.
Assess Risks and Complications of GAE Compared to Traditional Surgery
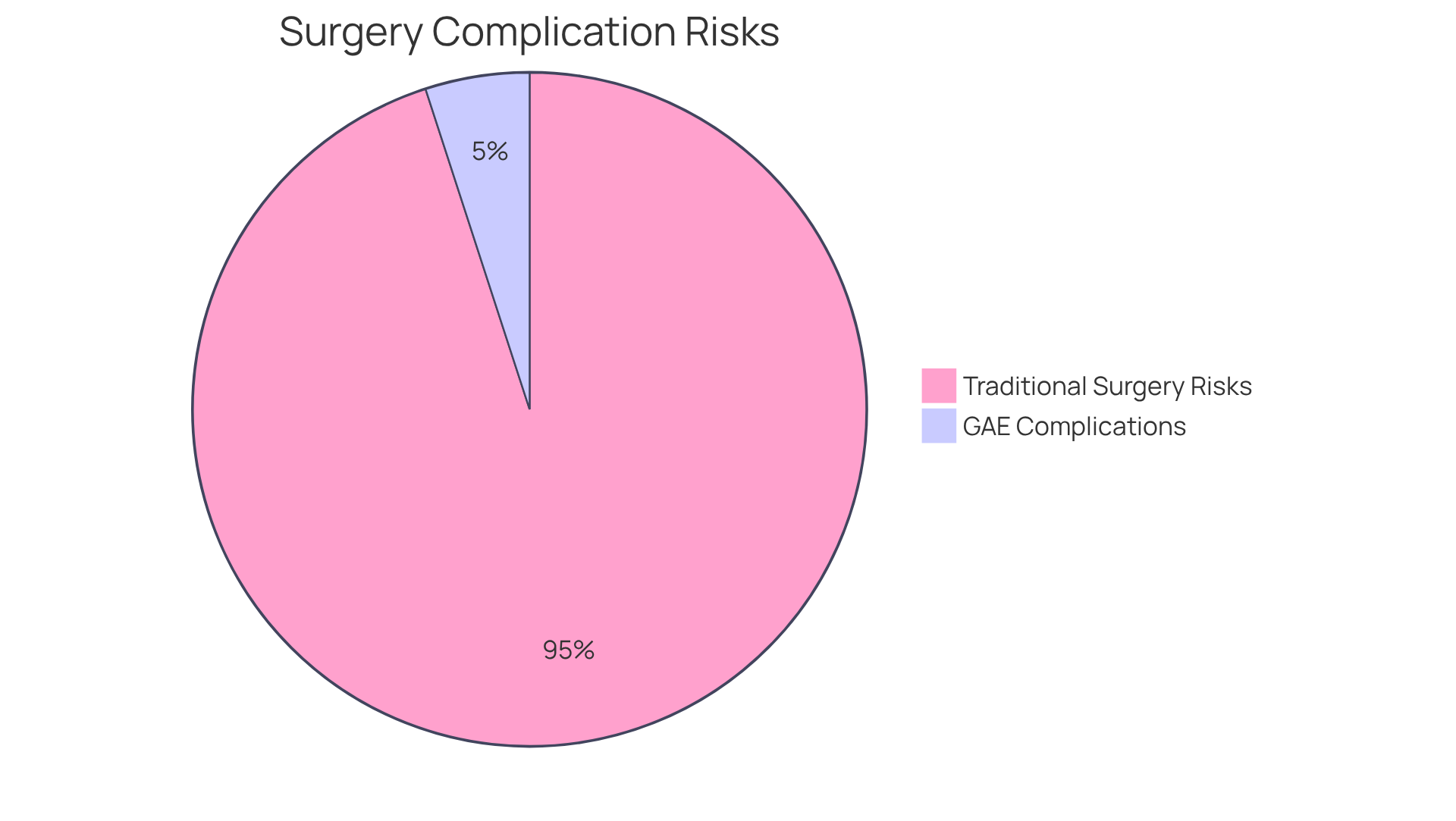
is often seen as a safe option for those dealing with joint discomfort. Most side effects are mild and temporary, such as slight discomfort, bruising, or skin discoloration at the injection site. Serious complications are quite rare, with research indicating that fewer than 5% of individuals experience significant negative effects. This makes GAE a viable choice, especially for those who may be feeling anxious about their health.
On the other hand, traditional surgery comes with a higher risk of complications, including infections, blood clots, and even the possibility of implant failure. The recovery can be challenging, often involving physical therapy. This can be daunting for many, particularly for elderly patients or those with other health concerns.
Ultimately, while both procedures carry some risks, the GAE procedure presents a lower risk profile. This makes it a particularly suitable option for elderly patients or those with comorbidities that could complicate recovery from major surgery. If you’re feeling uncertain or have questions about your options, please reach out for support. You’re not alone in this journey, and there are resources to help you find the best path forward.
Conclusion
Genicular Artery Embolization (GAE) is truly a remarkable option for those struggling with joint pain, especially if you’re feeling uncertain about traditional surgical routes. This minimally invasive technique not only helps ease discomfort but also provides a hopeful alternative for anyone looking to find relief from chronic knee pain without the lengthy recovery that often comes with joint replacement surgery.
Many patients have found significant pain relief and improved mobility through GAE, which boasts a high success rate. While traditional knee replacement surgery can be effective, it often carries hefty costs and a greater risk of complications. When you consider the financial aspects, GAE can be a more budget-friendly choice, particularly when factoring in insurance coverage and out-of-pocket expenses. Plus, with its lower risk profile, GAE is especially appealing for older adults or those with existing health conditions.
As we navigate the ever-changing healthcare landscape, it’s essential to explore innovative treatments like GAE to enhance patient outcomes. If you’re dealing with chronic joint discomfort, it’s important to have open conversations with your healthcare provider. Understanding your options can empower you to consider GAE as a viable path toward reclaiming your quality of life.
Embracing alternatives like GAE not only supports your journey but also fosters a more informed approach to managing your health. Remember, you’re not alone in this; there are compassionate solutions available to help you feel better and live life to the fullest.
Frequently Asked Questions
What is Genicular Artery Embolization (GAE)?
Genicular Artery Embolization (GAE) is a minimally invasive technique aimed at alleviating joint discomfort, particularly for individuals suffering from osteoarthritis. It involves selectively blocking the genicular arteries that supply blood to the leg joint, reducing blood flow to inflamed tissues to ease pain and improve function.
How does GAE compare to traditional surgical options?
GAE is a non-surgical alternative to traditional procedures like joint replacement. It is performed on an outpatient basis using local anesthesia, which allows for quicker recovery compared to conventional surgeries.
What is the recovery process like after GAE?
Most patients can return home the same day after the GAE procedure and often resume regular activities within a few days, making it a convenient option for pain relief.
What are the success rates of GAE?
Recent studies indicate that GAE has a remarkable technical success rate of about 99.7%, with many patients reporting significant pain reduction of 34 to 39 points on the discomfort scale over a year.
Who can benefit from GAE?
GAE is particularly beneficial for older adults and individuals with health issues that complicate recovery from major surgeries. It serves as a viable option for those not ready for joint replacement surgery, especially individuals with conditions like severe obesity or poorly controlled diabetes.
Is GAE covered by insurance?
GAE may be considered as an alternative insurance coverage option to surgery for patients who are not candidates for traditional surgical procedures.
How can someone find out more about GAE?
Individuals struggling with knee discomfort should discuss GAE with their healthcare provider to explore this treatment option and find relief.
List of Sources
- Understand Genicular Artery Embolization (GAE) as a Non-Surgical Alternative
- Can Genicular Artery Embolization Ease Knee Pain? (https://cityofhope.org/hope-matters-blog/genicular-artery-embolization-gae)
- What Is The Newest Treatment for Knee Pain – GAE for Knee Pain (https://preferredvasculargroup.com/what-is-the-newest-treatment-for-knee-pain-in-2025)
- Genicular Artery Embolization Safe, Relieves Pain for Symptomatic Knee OA (https://rheumatologyadvisor.com/news/genicular-artery-embolization-safe-relieves-pain-for-symptomatic-knee-oa)
- An alternative to knee replacement surgery? NIH-funded study is testing a procedure for osteoarthritis knee pain – UChicago Medicine (https://uchicagomedicine.org/forefront/orthopaedics-articles/2025/january/new-embolization-treatment-under-study-aims-to-relieve-osteoarthritis-knee-pain)
- Genicular Artery Embolization: A Minimally Invasive Approach to Knee Osteoarthritis – InventUM (https://news.med.miami.edu/genicular-artery-embolization-a-minimally-invasive-approach-to-knee-osteoarthritis)
- Compare Insurance Coverage for GAE and Traditional Surgery
- northstarir.com (https://northstarir.com/news/genicular-artery-embolization-cost)
- Exploring GAE: An Alternative to Knee Replacement Surgery | CardioVascular Health Clinic (https://cvhealthclinic.com/news/exploring-gae-an-alternative-to-knee-replacement-surgery)
- GAE Procedure Cost: A Viable Alternative to Traditional Surgery? (https://amavita.health/blog/gae-procedure-cost-a-viable-alternative-to-traditional-surgery)
- Evaluate Effectiveness and Outcomes of GAE vs. Traditional Surgery
- What Is the Success Rate of Genicular Artery Embolization? (https://visfl.com/post/what-is-the-success-rate-of-genicular-artery-embolization)
- GAE vs Knee Replacement: When Less Is More – North Star Vascular and Interventional (https://northstarir.com/news/gae-vs-knee-replacement)
- Life-Changing Results: Patient Success After Genicular Artery Embolization – Pittsburgh Vascular Specialists (https://greaterpittsburghvascular.com/2024/11/16/life-changing-results-patient-success-after-genicular-artery-embolization)
- Exploring GAE: An Alternative to Knee Replacement Surgery | CardioVascular Health Clinic (https://cvhealthclinic.com/news/exploring-gae-an-alternative-to-knee-replacement-surgery)
- An alternative to knee replacement surgery? NIH-funded study is testing a procedure for osteoarthritis knee pain – UChicago Medicine (https://uchicagomedicine.org/forefront/orthopaedics-articles/2025/january/new-embolization-treatment-under-study-aims-to-relieve-osteoarthritis-knee-pain)
- Assess Risks and Complications of GAE Compared to Traditional Surgery
- Can Genicular Artery Embolization Ease Knee Pain? (https://cityofhope.org/hope-matters-blog/genicular-artery-embolization-gae)
- Risks of Knee Replacement Surgery | Plancher Orthopaedics (https://plancherortho.com/common-complications-of-knee-replacement-surgery-what-patients-should-know)
- Genicular Artery Embolization: A Minimally Invasive Approach to Knee Osteoarthritis – InventUM (https://news.med.miami.edu/genicular-artery-embolization-a-minimally-invasive-approach-to-knee-osteoarthritis)
- Genicular artery embolization for knee osteoarthritis: Results of the LipioJoint-1 trial (https://sciencedirect.com/science/article/pii/S2211568423002395)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9971280)