Introduction
Facing medical procedures can often feel overwhelming, especially when the thought of surgery looms ahead. For those exploring alternatives, the Genicular Artery Embolization (GAE) outpatient clinic offers a compassionate option that not only reduces trauma but also supports a smoother recovery.
In this article, we’ll explore ten compelling reasons why GAE stands out as a thoughtful choice, highlighting its benefits, personalized care, and innovative approaches that truly make a difference.
As you navigate your health journey, you might wonder: could GAE be the supportive solution you’ve been seeking?
Amavita Heart and Vascular Health: Premier Provider of GAE Services
At Amavita Heart and Vascular Health, we understand that considering medical procedures can be daunting, especially for those seeking a surgical alternative. That’s why we proudly offer GAE services, led by our founder, Dr. Smith, a compassionate physician trained at Harvard. Our clinic is dedicated to combining advanced medical techniques with heartfelt care, ensuring that you feel supported every step of the way.
We prioritize your health, providing thorough evaluations and treatment plans tailored to your unique needs. This commitment not only establishes us as a trusted provider of GAE services but also reassures you that you’re in capable hands. Have you ever felt uncertain about your health options? We’re here to listen and guide you through your choices.
Our approach is rooted in understanding your concerns and addressing them with empathy. We believe that every patient deserves a treatment plan that reflects their individual circumstances. By choosing GAE, you’re not just opting for a procedure; you’re embracing a philosophy that values your well-being.
If you’re ready to explore your options or have questions about GAE, we encourage you to reach out. Your health journey is important to us, and we’re here to help you succeed.
Minimally Invasive GAE Procedure: A Less Traumatic Option
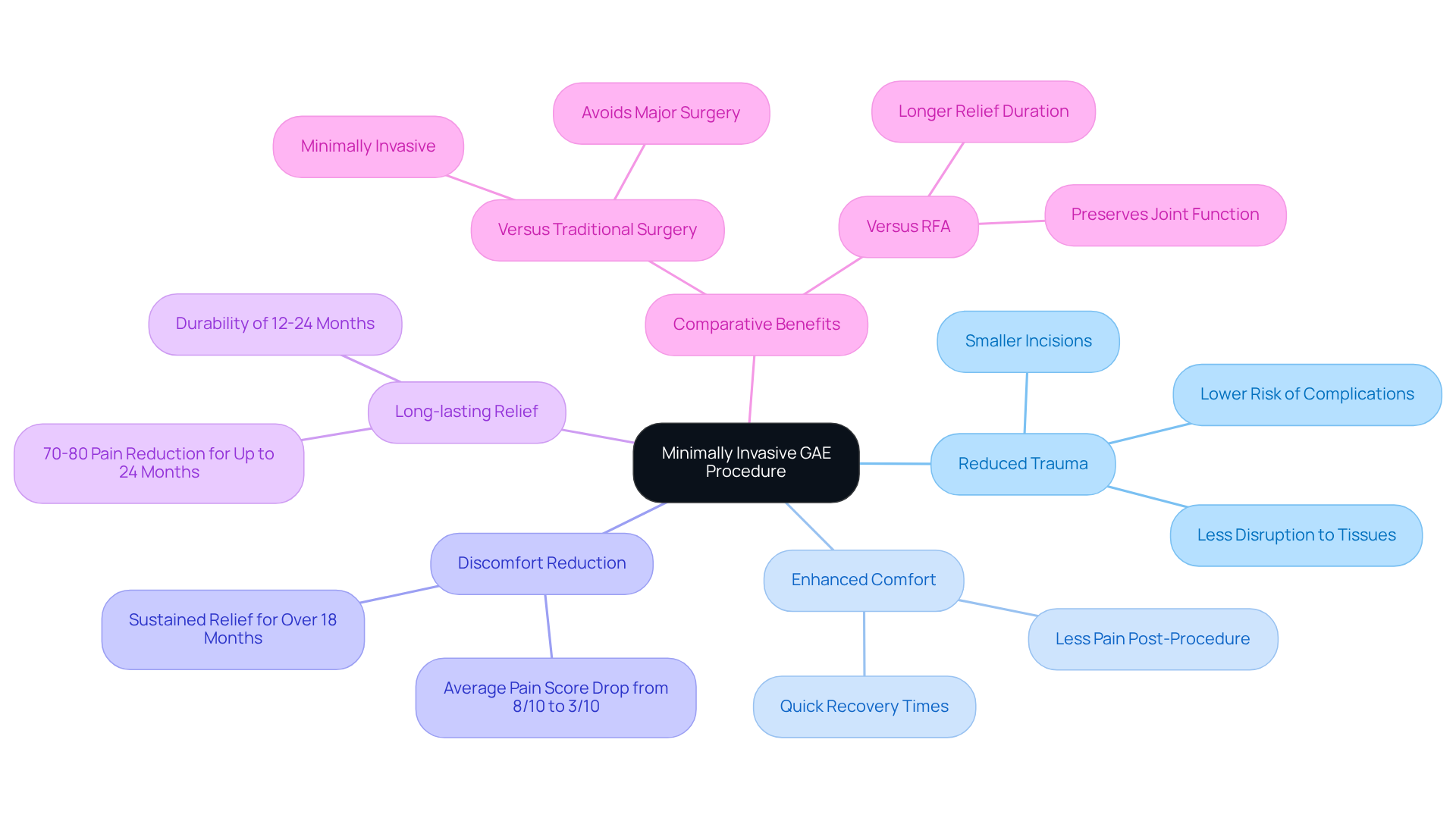
The Geniculate Artery Embolization (GAE) procedure offers a compassionate, minimally invasive option. With smaller incisions and less disruption to surrounding tissues, GAE not only reduces pain but also enhances comfort for individuals. Dr. Albert Chun, MD, shares that “GAE empathizes with your needs for durable, long-term relief,” underscoring its effectiveness in delivering lasting results.
Have you ever felt overwhelmed by discomfort? Research indicates that many individuals experience a significant reduction in pain shortly after the procedure, with average scores dropping from 8/10 to 3/10 within weeks. Numerous testimonials reveal that many enjoy enduring relief for over 18 months. This makes the GAE an ideal choice for those seeking alternatives associated with major surgeries.
Furthermore, unlike Radiofrequency Ablation (RFA), which focuses on temporary nerve blocks, GAE preserves joint function and can delay or even avoid the need for more invasive procedures. This aspect is particularly appealing for individuals who prioritize their health and well-being. If you’re considering options for relief, know that the alternative to surgery could provide a supportive step towards a more comfortable life.
Effective Pain Management: GAE’s Role in Alleviating Knee Pain
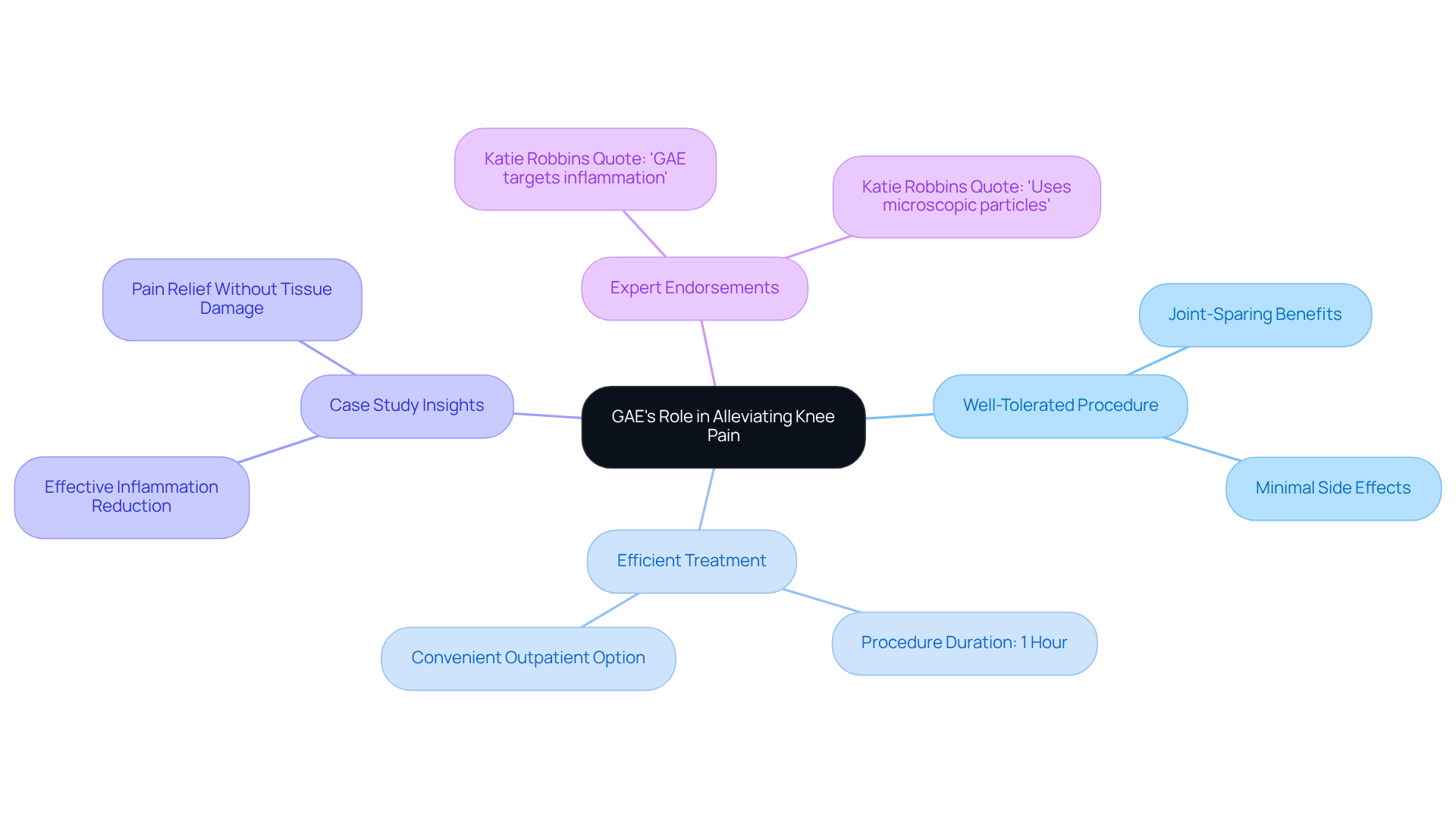
GAE has emerged as a highly effective treatment for managing knee discomfort, especially for those dealing with osteoarthritis. This procedure specifically targets the gastrocnemius muscle, relieving pressure on the knee joint and leading to significant pain reduction. By effectively reducing inflammation in the knee, GAE not only alleviates pain but also greatly improves the overall quality of life for patients.
With millions of adults in the U.S. experiencing knee discomfort daily, the GAE procedure provides a promising option for those seeking relief without resorting to more invasive surgical methods.
Key Benefits of GAE:
- Well-Tolerated Procedure: Orthopedic specialists emphasize that GAE is well-tolerated and provides joint-sparing benefits, making it an ideal choice for individuals looking to manage knee pain effectively.
- Efficient Treatment: The GAE procedure takes about one hour, making it a convenient choice for individuals seeking quick relief.
- Case Study Insights: A recent case study highlighted that GAE effectively reduces inflammation in the knee joint, offering relief without damaging healthy tissue. This is particularly beneficial for patients who have not found relief from conservative treatments and wish to avoid knee replacement surgery.
- Expert Endorsements: As Katie Robbins, an orthopedic specialist, states, “GAE is a treatment that targets inflammation in the knee joint,” showcasing its effectiveness in managing discomfort.
In addition to these benefits, it’s important to remember that seeking help is a sign of strength. The GAE procedure represents a valuable option for those seeking relief from knee pain, enhancing both mobility and function. If you or a loved one are struggling with knee pain, consider reaching out to a healthcare professional to discuss whether GAE might be the right choice for you.
Rapid Recovery: Benefits of Choosing GAE Over Surgery
Are you or a loved one struggling with knee pain? If so, you might be feeling anxious about the recovery process associated with surgery, especially when considering the alternative to surgery. One of the standout benefits of choosing GAE is the rapid recovery. Patients often experience less postoperative discomfort, allowing them to return to their daily activities much sooner than they would after more invasive surgeries. Many individuals find they can walk and engage in light activities within just days of the procedure. This is a significant improvement compared to the weeks or even months required for recovery from traditional surgery, which can be especially concerning for older individuals who may have other health issues.
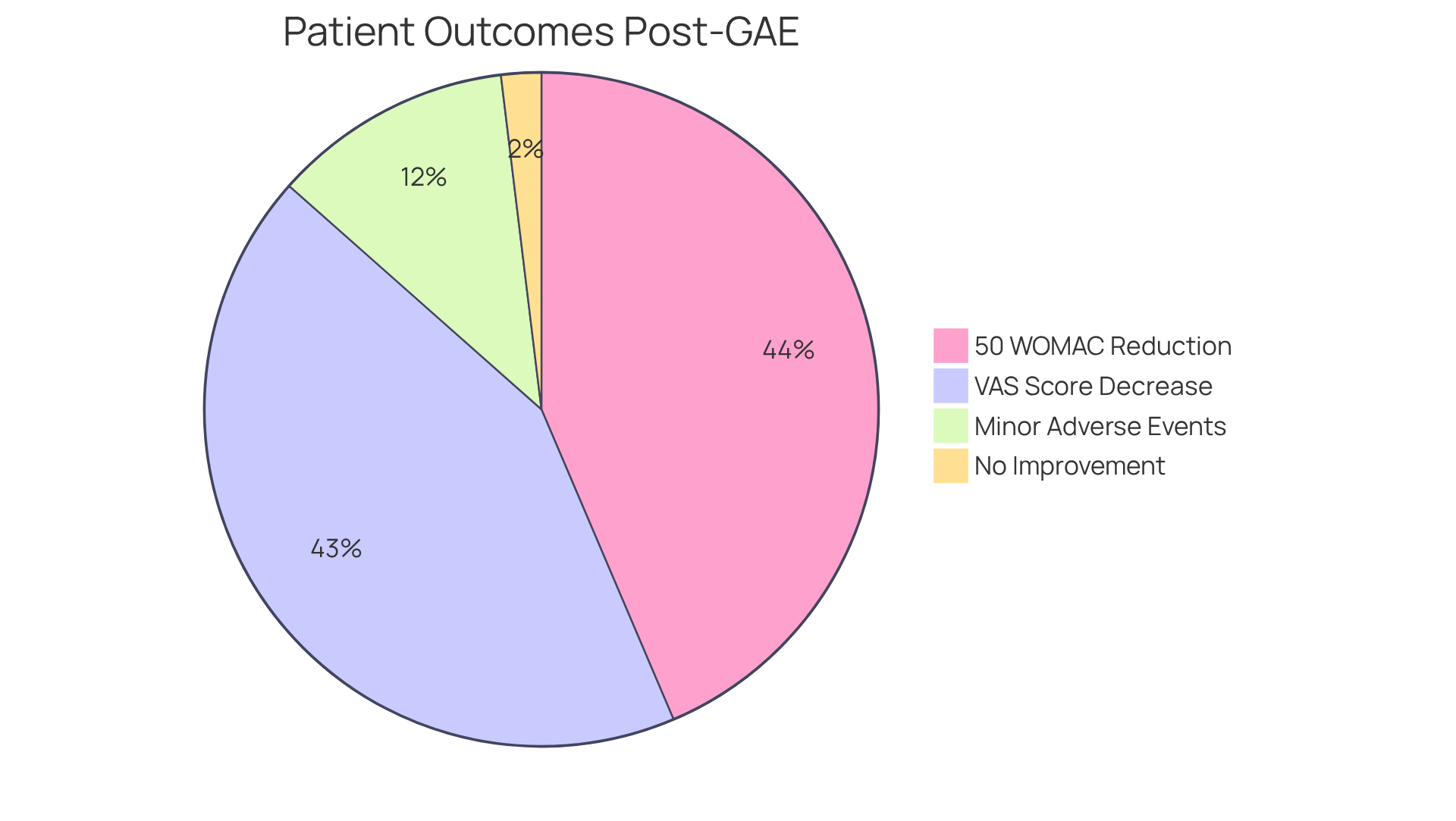
At 12 months post-GAE, statistics reveal a remarkable decrease in discomfort. The median Visual Analog Scale (VAS) score dropped from 8 to 3, indicating significant improvement for many patients. Furthermore, 68% of patients reported a decrease of at least 50% in their Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) scores. This emphasizes how GAE can be effective in managing discomfort and improving quality of life.
While the procedure is generally safe, it’s important to note that some minor adverse events, such as temporary skin discoloration and mild knee discomfort, have been reported. However, the overall benefits and safety make it an appealing option for those seeking relief from chronic pain.
As Dr. Alexandra I Stavrakis notes, “This prospective trial demonstrates that GAE is effective and durable in reducing pain symptoms from moderate or severe knee OA that is refractory to other conservative therapy, with an acceptable safety profile.” If you’re considering GAE, know that you’re not alone, and there are compassionate professionals ready to support you on your journey to relief.
Personalized Treatment Plans: Tailoring GAE to Individual Needs
At the clinic, we understand that each individual has unique needs. That’s why every person receives a customized treatment plan just for them. This ensures that the plan is not only suitable but also sensitive to each individual’s medical history, lifestyle, and personal preferences.
By focusing on the distinct situations of each person, we significantly enhance the chances of successful outcomes among those receiving care. Isn’t it comforting to know that your specific concerns are at the forefront of our approach?
We believe that everyone deserves support with their personal journey. Our commitment to understanding and addressing your emotions and concerns is what sets us apart. Together, we can navigate your treatment process with compassion and expertise, ensuring you feel valued and supported every step of the way.
Thorough Evaluation Process: Ensuring GAE is Right for You
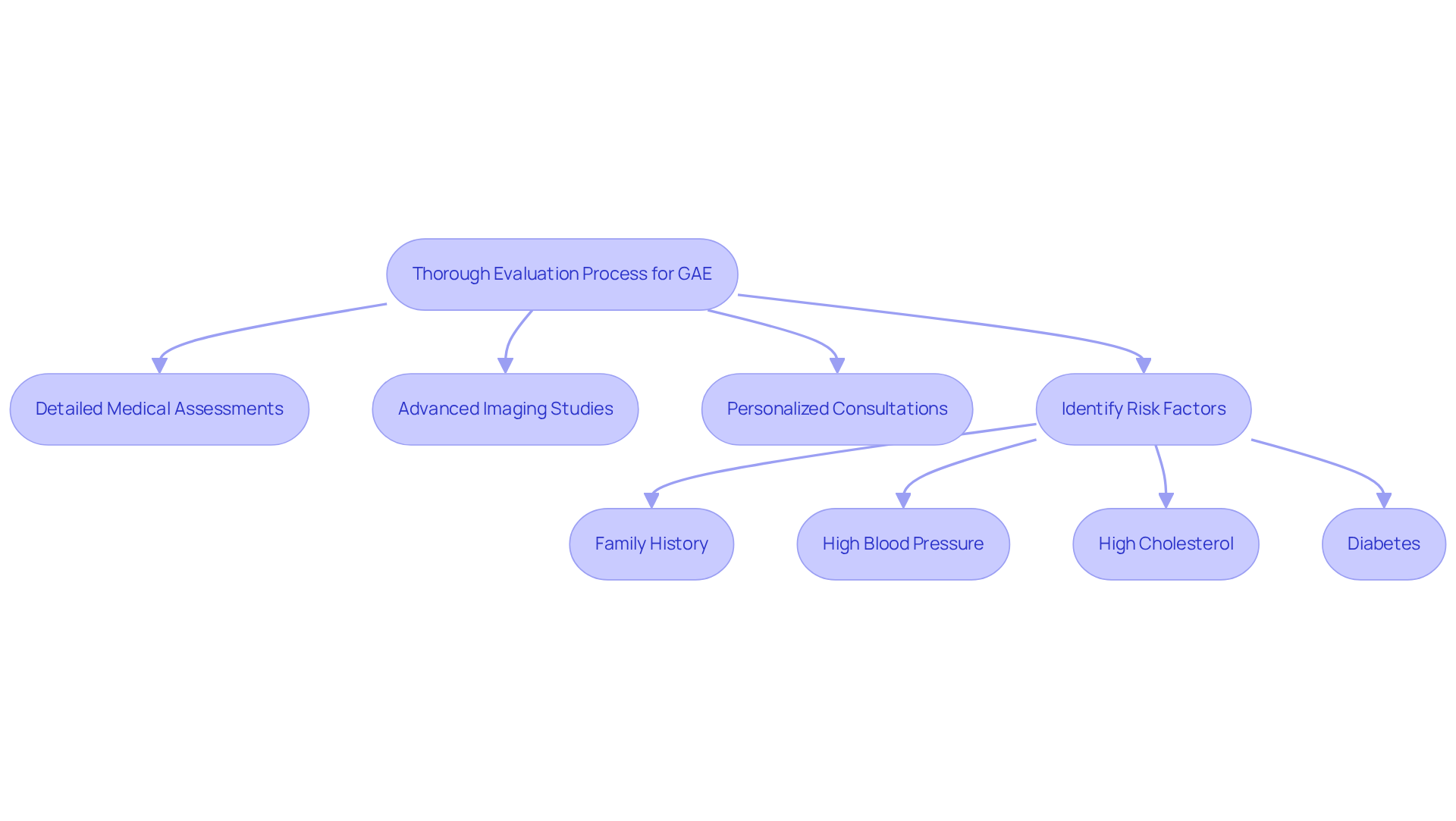
At Amavita, we understand that the journey to undergoing surgery can feel overwhelming. That’s why we start with a thorough evaluation process designed with your safety and comfort in mind. Each individual receives a comprehensive assessment, which includes:
This careful approach is essential for developing a tailored treatment plan.
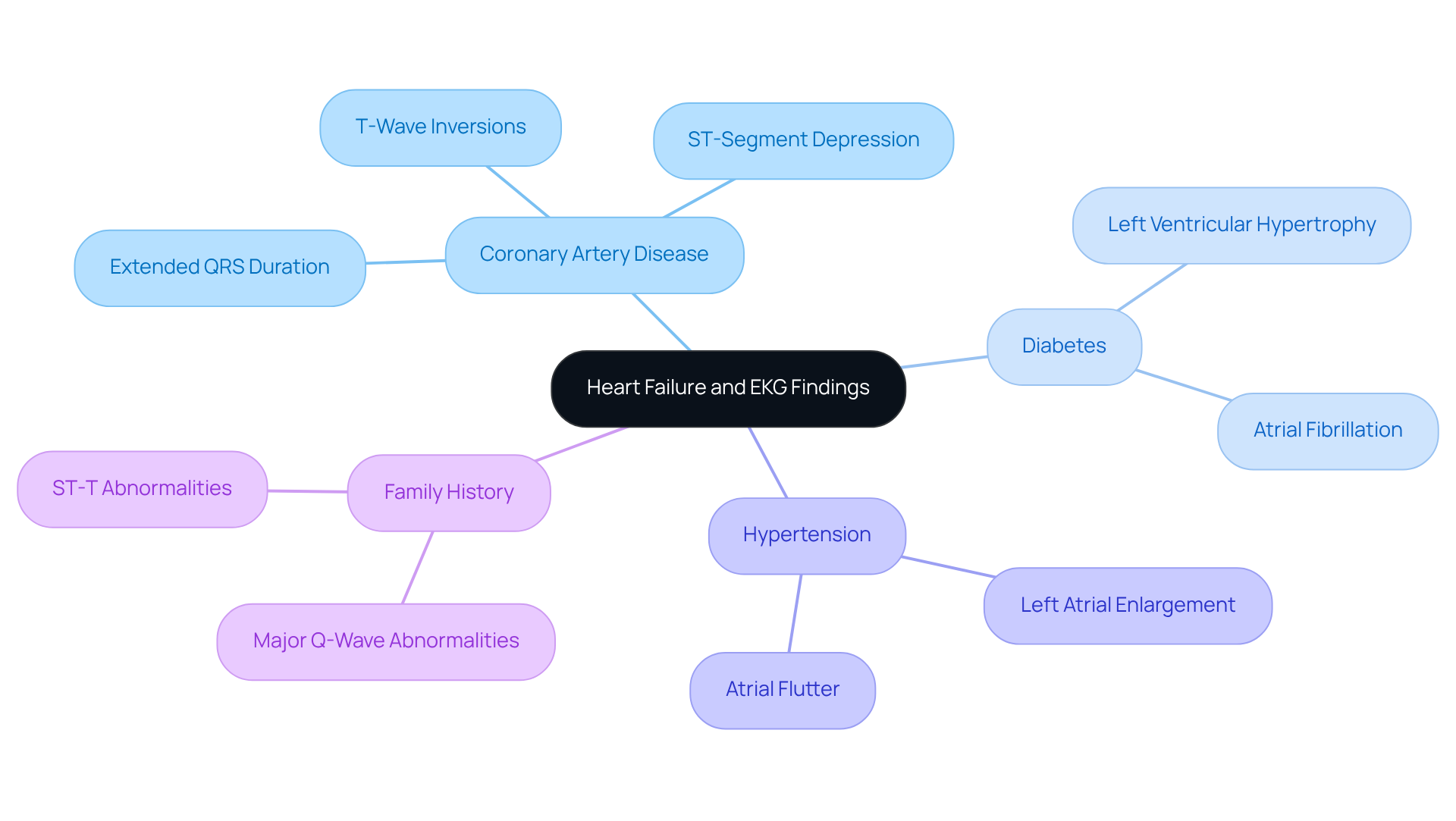
In addition to this, our evaluation process combines with tailored interventions. This is crucial for optimizing every step of the way. By identifying risk factors such as:
- Family history
- High cholesterol
- Diabetes
we can better determine the most suitable candidates for GAE.
Furthermore, by prioritizing these assessments, we ensure that you are well-informed and prepared for your treatment. We want you to feel confident and reassured, knowing that our team is dedicated to your care. Remember, you are not alone on this journey; we are here to help.
Safety First: Understanding the Risks and Benefits of GAE
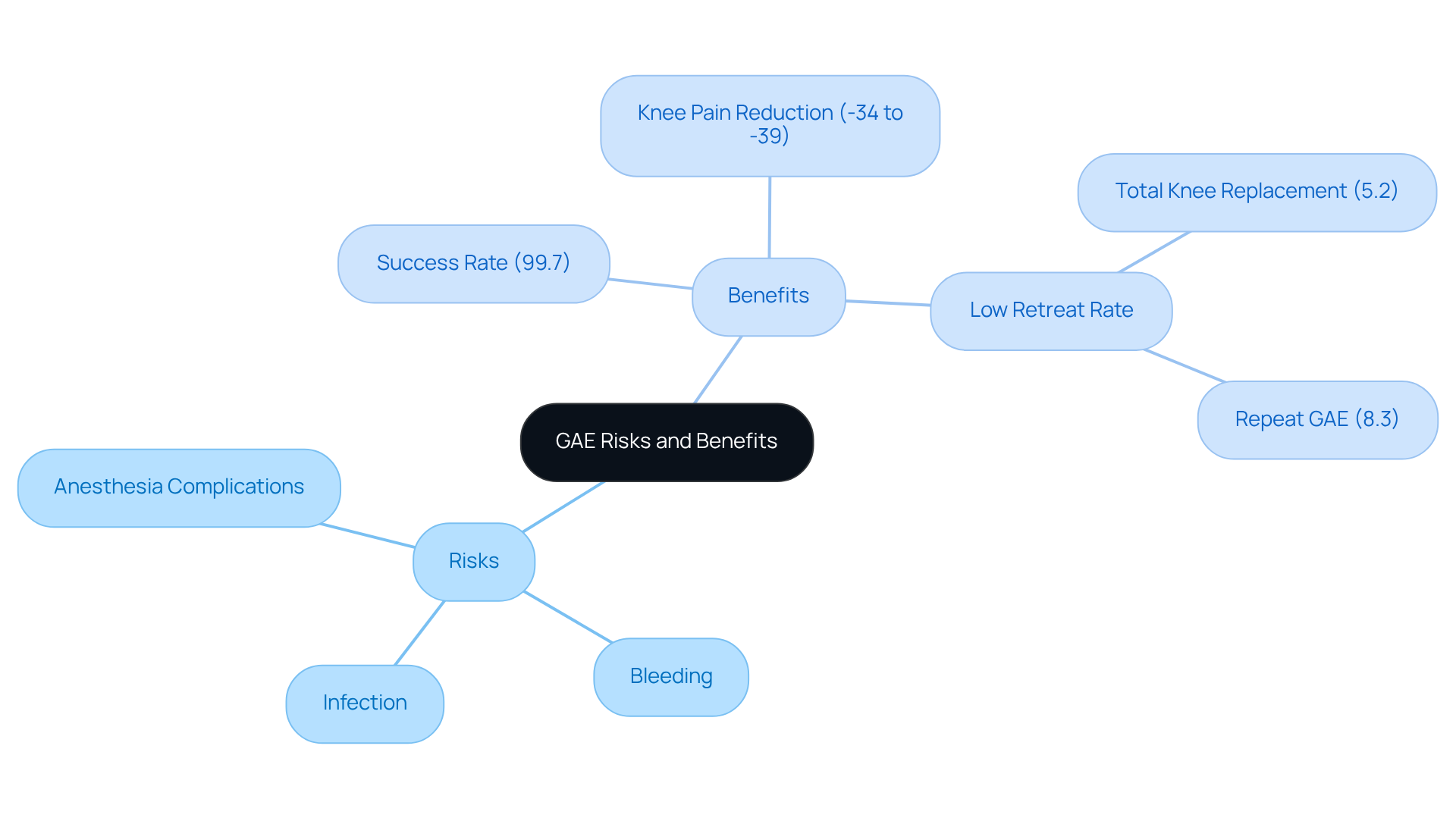
Understanding the risks and benefits of GAE is crucial for anyone considering this innovative procedure. You might be wondering if it’s the right choice for you. GAE is generally seen as a safe option, boasting a remarkable safety profile across numerous studies involving hundreds of patients. While there are potential risks—like infection, bleeding, and complications from anesthesia—these are often outweighed by the benefits of the procedure. In fact, studies over a 12-month period have shown a weighted mean difference in knee discomfort scores ranging from -34 to -39, indicating substantial relief that exceeds established minimal clinically important differences (MCIDs).
At Amavita, our dedicated team prioritizes your safety and well-being. We engage in thorough discussions about these factors, ensuring you feel informed and supported in your decision-making process. Research shows that individuals with higher baseline knee pain scores often experience greater responsiveness to GAE, reinforcing its effectiveness. Additionally, the low rate of retreatment—only 5.2% of individuals undergoing total knee replacement and 8.3% receiving repeat GAE within two years—suggests that GAE provides lasting relief. As noted by Bagla, “the rate of retreatment was low which could potentially suggest long-term effectiveness.”
In summary, while no procedure is without risks, the evidence strongly supports the GAE as a safe and effective option. If you’re looking to alleviate knee pain, we’re here to help you every step of the way. Remember, you’re not alone in this journey.
Accessible Care: GAE Services for Underserved Communities
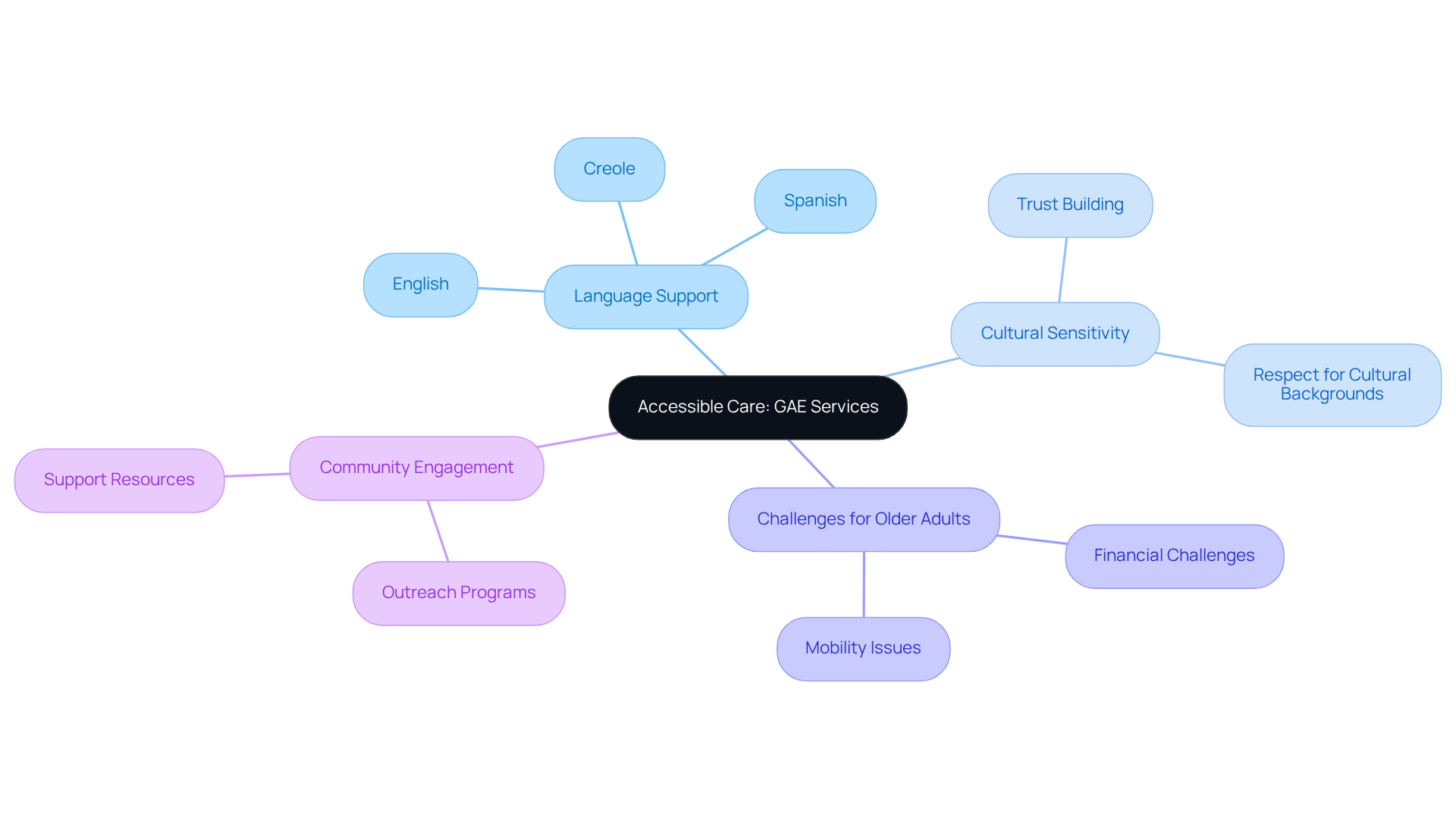
Amavita is truly committed to making GAE services accessible for underserved communities. By providing care in multiple languages—English, Spanish, and Creole—the clinic ensures that everyone receives the essential information and assistance they need. This dedication to accessibility not only builds trust but also encourages individuals from diverse backgrounds, especially the elderly, to seek the care they deserve.
Have you ever felt hesitant about seeking medical help? You’re not alone. Data from the National Health Interview Survey shows that 7.3% of adults aged 18 and older have delayed or avoided medical care. This issue is particularly significant for older adults, who often face barriers when it comes to healthcare. The COVID-19 pandemic has only intensified these barriers, making it even more crucial to develop effective strategies for ensuring access to care. In response, Amavita has adapted its services to enhance accessibility, allowing individuals to receive care safely and effectively.
By prioritizing culturally sensitive care, Amavita directly addresses these challenges, improving individual engagement and outcomes in healthcare. With a team that understands the unique needs of Miami’s diverse community, including specialists like Anamary Muñoz, who specializes in GAE treatments, the organization empowers individuals to connect with healthcare professionals who respect their cultural backgrounds. If you’re looking for support, don’t hesitate to reach out to Amavita directly or visit their website for more information on available resources.
Ultimately, this compassionate approach leads to better health outcomes. Remember, you are not alone on this journey—help is available, and Amavita is here to support you every step of the way.
Innovative Research: Amavita’s Commitment to Advancing GAE Treatments
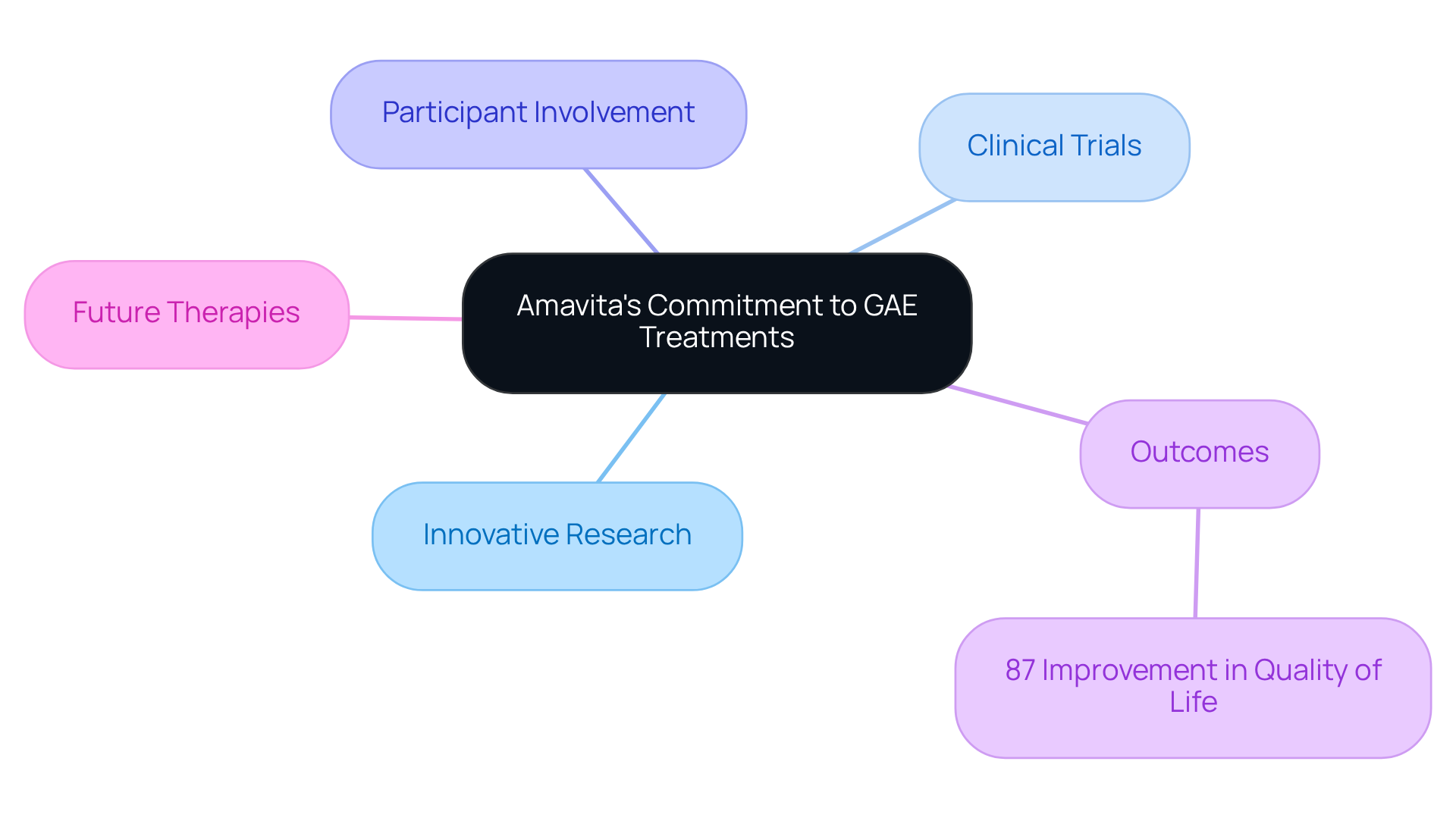
At Amavita, we understand that navigating health concerns can be daunting, especially for those dealing with knee osteoarthritis. That’s why we’re committed to being at the forefront of innovative research focused on enhancing patient outcomes. Our clinic actively participates in clinical trials, all aimed at improving the effectiveness of GAE.
In 2025, we’re excited about the significant advancements being explored in GAE technology, with a strong emphasis on participant involvement and positive outcomes. Recent studies have shown that GAE can lead to an impressive reduction in pain for individuals suffering from knee osteoarthritis. Many patients have reported enjoying prolonged benefits over time, which is truly heartening.
This dedication to research not only provides our patients with access to advanced treatments but also reinforces our role as a leader in cardiovascular care. By participating in these trials, you can gain early access to tomorrow’s therapies, which include the latest GAE techniques, ensuring you receive the most effective and least invasive options available.
We invite you to reach out and learn more about how we can support you on your journey to better health. Your well-being is our priority, and we’re here to help you every step of the way.
Patient Testimonials: Real Experiences with Amavita’s GAE Services
are powerful stories that highlight the compassionate impact of Amavita. Many individuals have shared their heartfelt experiences, showcasing the empathetic support they received and the significant improvements in their health following the procedure. These personal narratives not only affirm the effectiveness of GAE but also reflect the community fostered by Amavita and his dedicated team.
In addition to this, prospective patients can find comfort and confidence in the journeys of others who have successfully navigated their treatment at Amavita. It’s reassuring to know that they are not alone in their recovery. Have you ever felt uncertain about seeking help? Remember, there’s a community ready to support you every step of the way.
Your well-being is our priority, and we’re here to help you achieve your health goals. Reach out today to learn more about how we can assist you on your path to better health.
Conclusion
Choosing the GAE outpatient clinic instead of surgery offers a caring approach to managing knee discomfort and improving overall health. This innovative procedure minimizes trauma and promotes quick recovery, while also providing personalized treatment plans tailored to individual needs. With a focus on compassionate care and thorough evaluations, clinics like Amavita Heart and Vascular Health ensure that patients feel supported every step of the way.
The article highlights several key benefits of GAE, such as its minimally invasive nature, effective pain management, and the significant improvement in quality of life for those dealing with knee osteoarthritis. Patient testimonials further emphasize the positive impact of this treatment, showcasing the nurturing environment created by healthcare professionals dedicated to patient well-being.
Ultimately, the GAE outpatient clinic is more than just a medical procedure; it represents a commitment to accessible, empathetic care that empowers individuals to reclaim their health. If you’re struggling with chronic knee pain or considering alternatives to surgery, exploring GAE could be your first step toward a more comfortable and fulfilling life. Why not reach out to a healthcare provider today to discover how GAE can make a difference in your health journey?
Frequently Asked Questions
What is Heart and Vascular Health’s approach to patient care?
Heart and Vascular Health combines advanced medical techniques with compassionate care, ensuring thorough evaluations and personalized treatment plans tailored to each patient’s unique needs.
Who leads the GAE outpatient clinic at Heart and Vascular Health?
The GAE outpatient clinic is led by Dr. Pedro Martinez-Clark, a physician trained at Harvard, who emphasizes empathy and support for patients.
What is the Geniculate Artery Embolization (GAE) procedure?
GAE is a minimally invasive procedure that significantly reduces trauma compared to traditional surgery, using smaller incisions and causing less disruption to surrounding tissues.
How does GAE compare to traditional surgical methods in terms of recovery?
GAE lowers the risk of complications and enhances comfort, allowing for a quicker recovery with less downtime compared to major surgeries.
What kind of pain relief can patients expect from the GAE procedure?
Patients often experience a significant reduction in discomfort levels shortly after the procedure, with average pain scores dropping from 8/10 to 3/10 within weeks, and many enjoy lasting relief for over 18 months.
How does GAE affect joint function compared to Radiofrequency Ablation (RFA)?
Unlike RFA, which focuses on temporary nerve blocks, GAE preserves joint function and can potentially delay or avoid the need for joint replacement.
Who can benefit from the GAE outpatient clinic alternative to surgery?
Individuals dealing with knee discomfort, particularly those with osteoarthritis, can benefit from GAE as it effectively targets inflammation and enhances mobility.
How long does the GAE procedure take?
The GAE procedure typically takes about one hour, making it a convenient option for individuals seeking effective treatment.
What do experts say about the effectiveness of the GAE procedure?
Orthopedic specialists endorse GAE as a well-tolerated, minimally invasive procedure that targets inflammation in the knee joint, providing effective pain management without damaging healthy tissue.
What should individuals do if they are considering GAE for knee pain relief?
Individuals struggling with knee pain should reach out to a healthcare professional to discuss whether GAE might be the right choice for them.
List of Sources
- Minimally Invasive GAE Procedure: A Less Traumatic Option
- sacmd.com (https://sacmd.com/alternatives-to-surgery-gae-and-radiofrequency-ablation-in-virginia-2025)
- Real Patient Stories: Life After GAE for Knee Osteoarthritis in DC – SURGICAL ASSOCIATES, LLC (https://sacmd.com/patient-stories-life-after-gae-for-knee-osteoarthritis-in-dc)
- Effective Pain Management: GAE’s Role in Alleviating Knee Pain
- A New Option for Knee Pain: Genicular Artery Embolization (GAE) (https://richmondvascularcenter.com/news/a-new-option-for-knee-pain-genicular-artery-embolization-gae)
- nyulangone.org (https://nyulangone.org/news/minimally-invasive-procedure-relieves-painful-symptoms-knee-osteoarthritis)
- Rapid Recovery: Benefits of Choosing GAE Over Surgery
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC8542160)
- Thorough Evaluation Process: Ensuring GAE is Right for You
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9971280)
- Data review presents geniculate artery embolization as an emerging minimally invasive technique for knee OA (https://aaos.org/aaosnow/2025/aug-sept/clinical/clinical01)
- Safety First: Understanding the Risks and Benefits of GAE
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9971280)
- Accessible Care: GAE Services for Underserved Communities
- FastStats (https://cdc.gov/nchs/fastats/access-to-health-care.htm)
- Innovative Research: Amavita’s Commitment to Advancing GAE Treatments
- diagnosticimaging.com (https://diagnosticimaging.com/view/interventional-radiology-research-genicular-artery-embolization-knee-oa)
- recoverytrial.net (https://recoverytrial.net/case_studies/from-buckinghamshire-to-worldwide-impact-dr-raha-west2019s-journey-with-the-recovery-trial)
- Medable Clinical Research Translation Case Study (https://lionbridge.com/case-study/medable-clinical-research-translation-case-study)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9971280)
- Patient Testimonials: Real Experiences with Amavita’s GAE Services
- 45 Statistics on Patient Reviews for Healthcare Professionals (https://repugen.com/blog/statistics-on-patient-reviews-for-healthcare-professionals)
- Patient Experience, Satisfaction and Billing Statistics | CallMiner (https://callminer.com/blog/101-statistics-on-patient-experience-satisfaction-billing-and-more)