Introduction
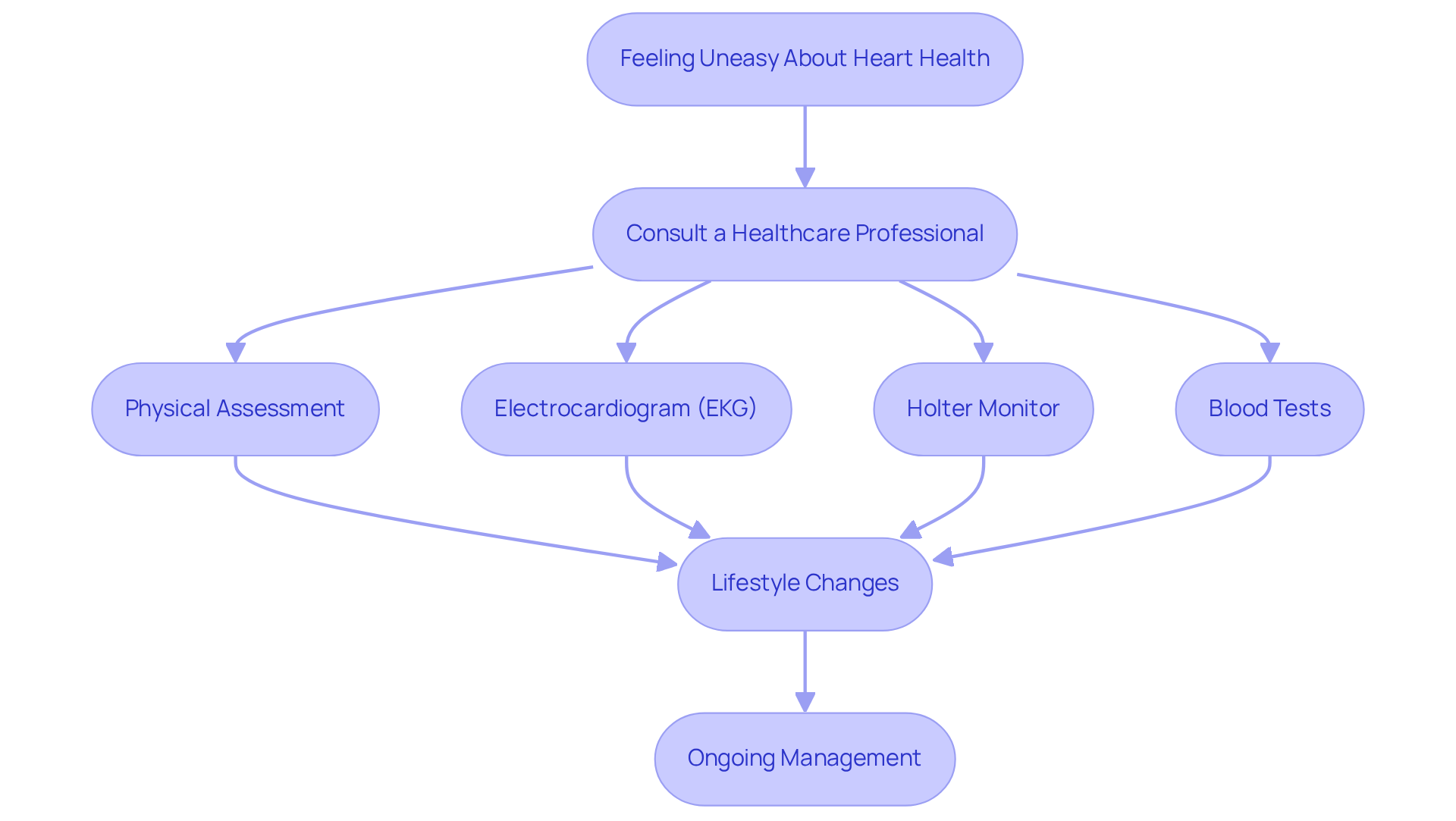
Knee pain is a common concern for many elderly individuals, and it can significantly impact their quality of life. This growing prevalence has led to interest in innovative treatments like Genicular Artery Embolization (GAE), a minimally invasive procedure that offers hope for relief from chronic discomfort.
GAE presents several benefits, such as a quick recovery and a high success rate, making it an appealing option for those seeking to regain their mobility and comfort. However, it’s crucial to consider the potential risks associated with same-day procedures, especially for older patients who may have underlying health conditions.
Families should reflect on various factors when weighing the advantages of GAE against its risks:
- What specific health concerns might your loved one have?
- How can you ensure that they receive the safest and most effective treatment possible?
By asking these questions, you can better navigate the decision-making process.
Ultimately, understanding the balance between the benefits and risks of GAE can empower families to make informed choices. Remember, you’re not alone in this journey; support is available to help you and your loved ones through every step of the treatment experience.
Define Genicular Artery Embolization (GAE) Procedure
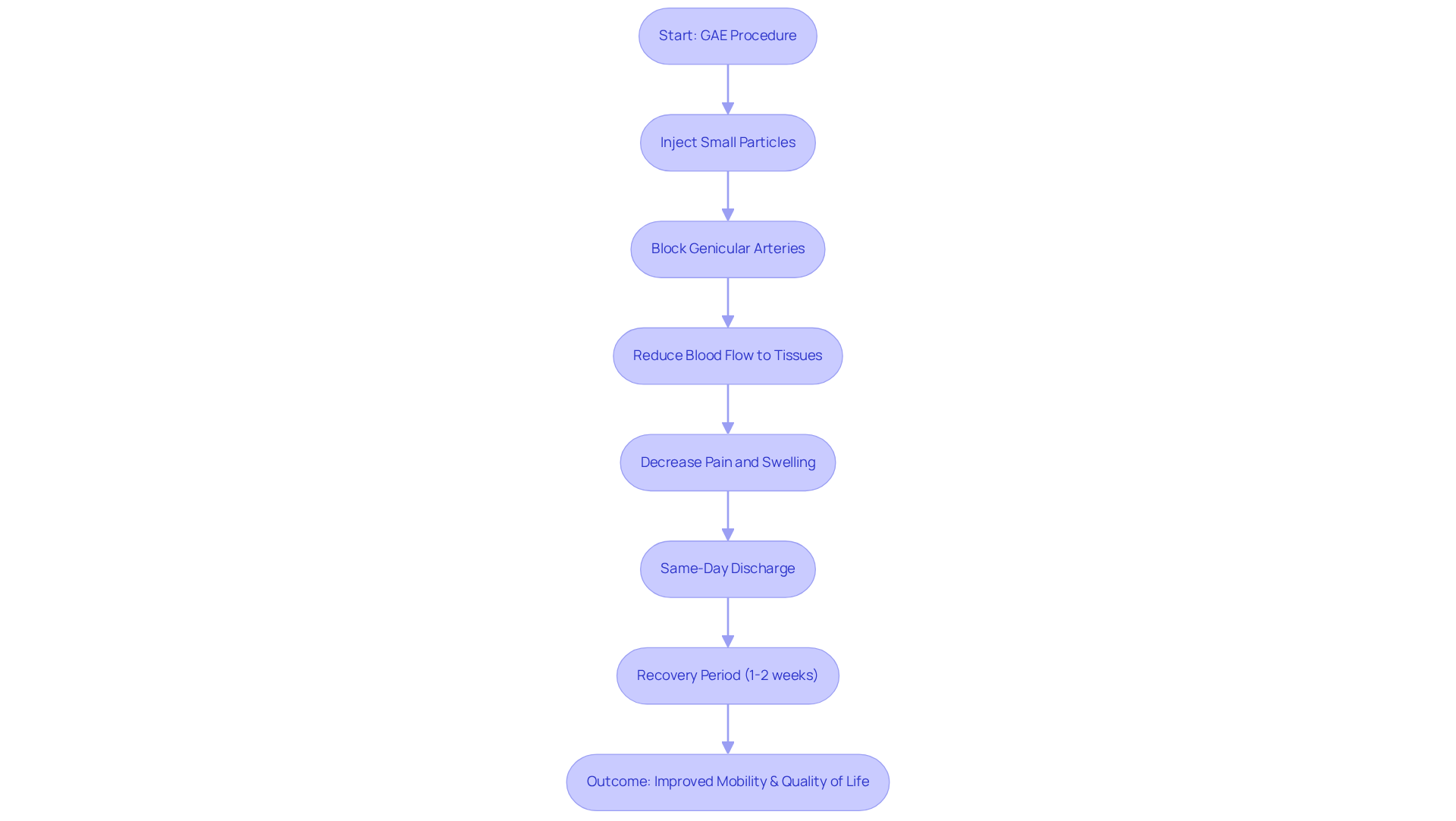
(GAE) is a remarkable procedure that aims to relieve pain, particularly from osteoarthritis. If you or a loved one has been struggling with knee pain, this innovative procedure might be just what you need. By injecting small particles into the genicular arteries that supply blood to the knee joint, GAE selectively blocks these arteries. This process reduces blood flow to inflamed tissues, leading to less pain and swelling. Performed under local anesthesia, GAE typically allows for same-day discharge, making it a convenient option for older individuals who may face higher risks associated with surgery compared to traditional surgeries.
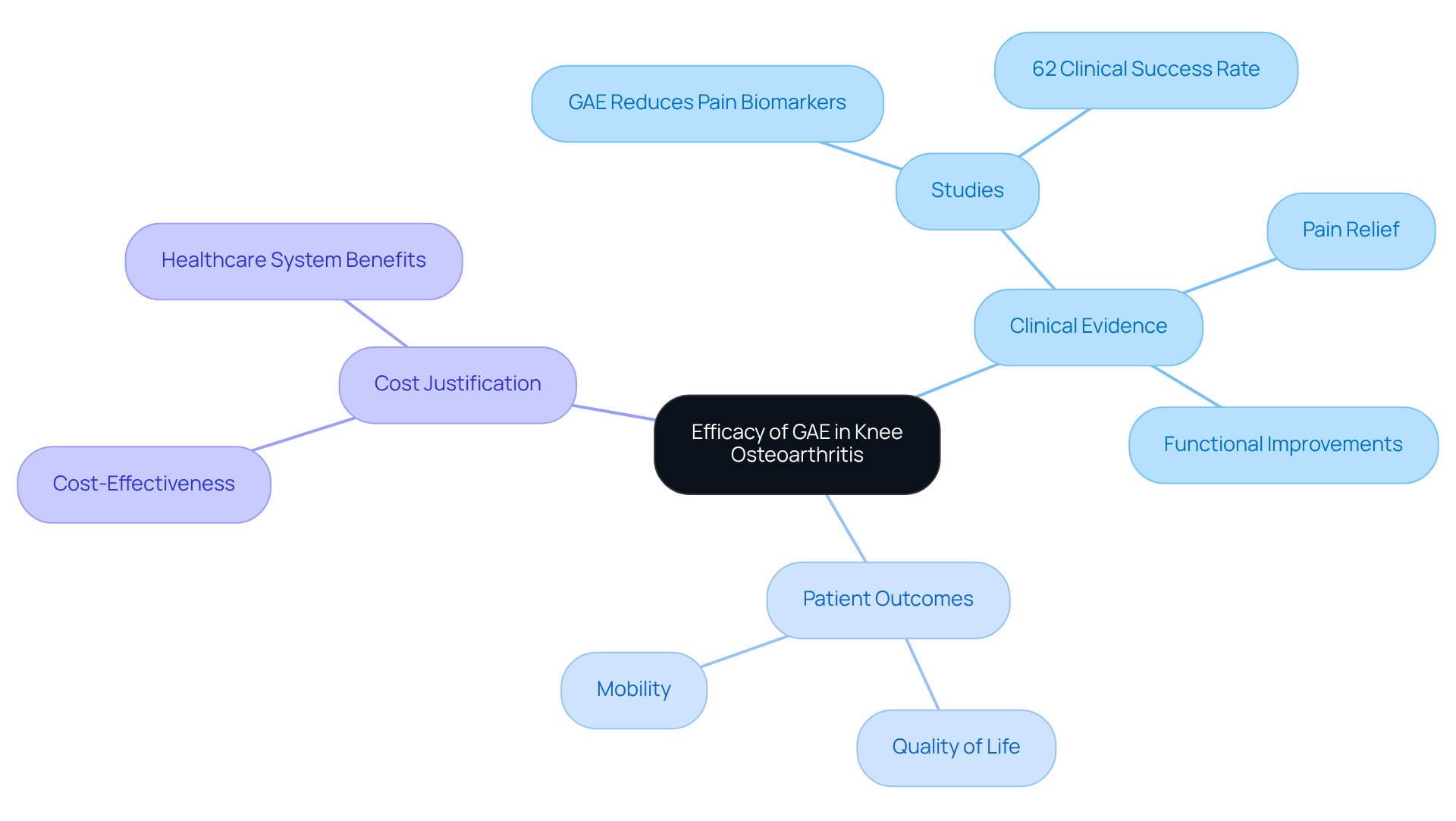
Looking ahead to 2025, many seniors are expected to benefit from GAE, reflecting its growing acceptance as a viable treatment alternative. With a success rate of 70-80% in alleviating pain, many patients report improved mobility and quality of life shortly after treatment. Imagine being able to enjoy your daily activities again! Plus, recovery time of just 1-2 weeks, which is much shorter than the 6-12 months often required for conventional joint surgeries.
Case studies highlight the effectiveness of GAE in managing discomfort for seniors. For instance, individuals who previously faced persistent joint pain and were not candidates for surgery have shared stories of lasting relief and improved functionality after the procedure. As one specialist noted, “GAE is a breakthrough for symptomatic OA of the joint poised to address the current OA treatment gap between conservative nonsurgical care and TKA.”
Recent advancements in GAE techniques continue to enhance its safety and efficacy, solidifying its role as a preferred option for older adults who wish to maintain their independence and active lifestyles. With ongoing studies and research supporting its benefits, GAE stands out as a treatment option from without the need for major surgery. If you’re considering your options, don’t hesitate to reach out for more information and support.
Identify Risks Associated with GAE Procedure
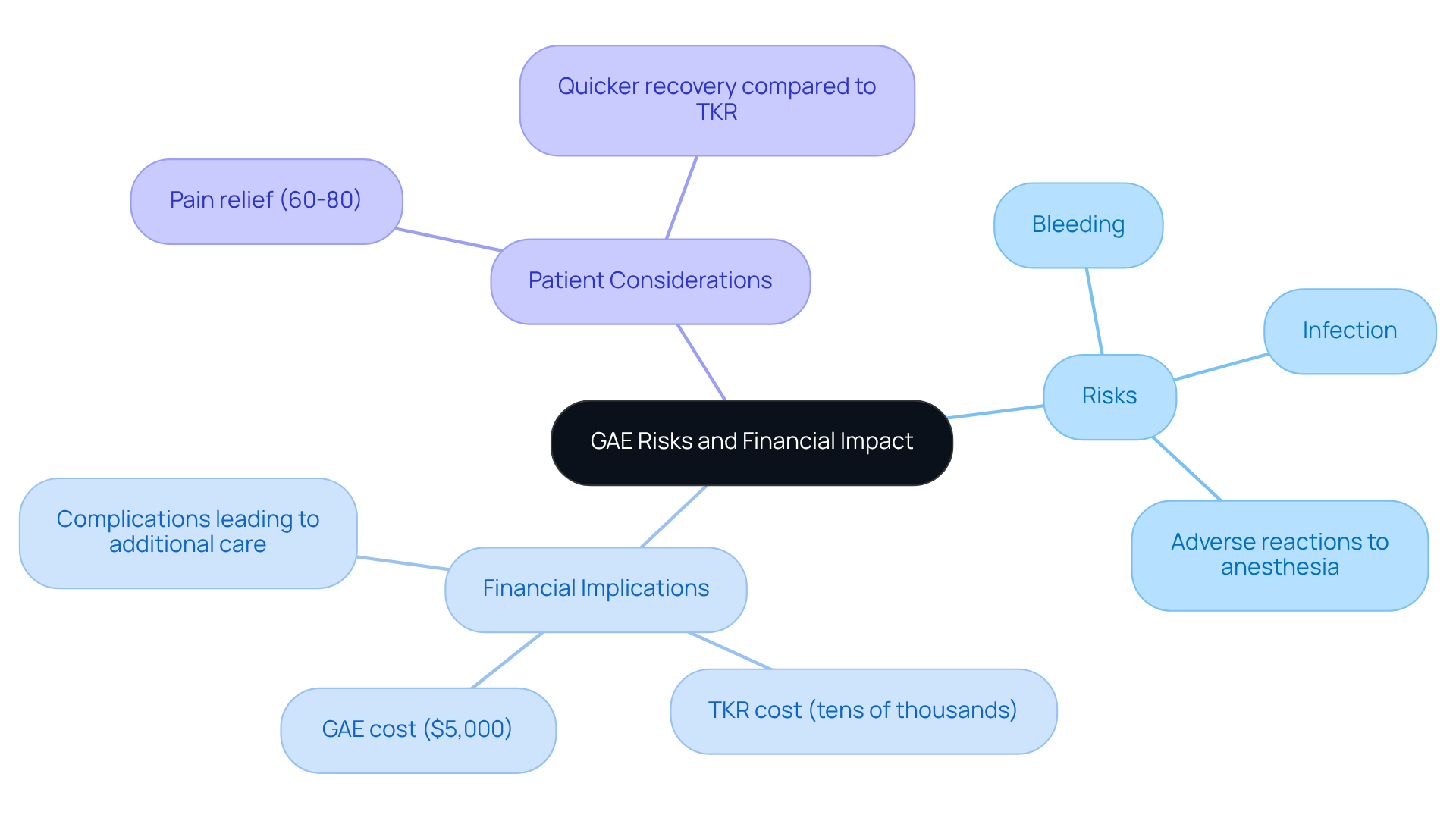
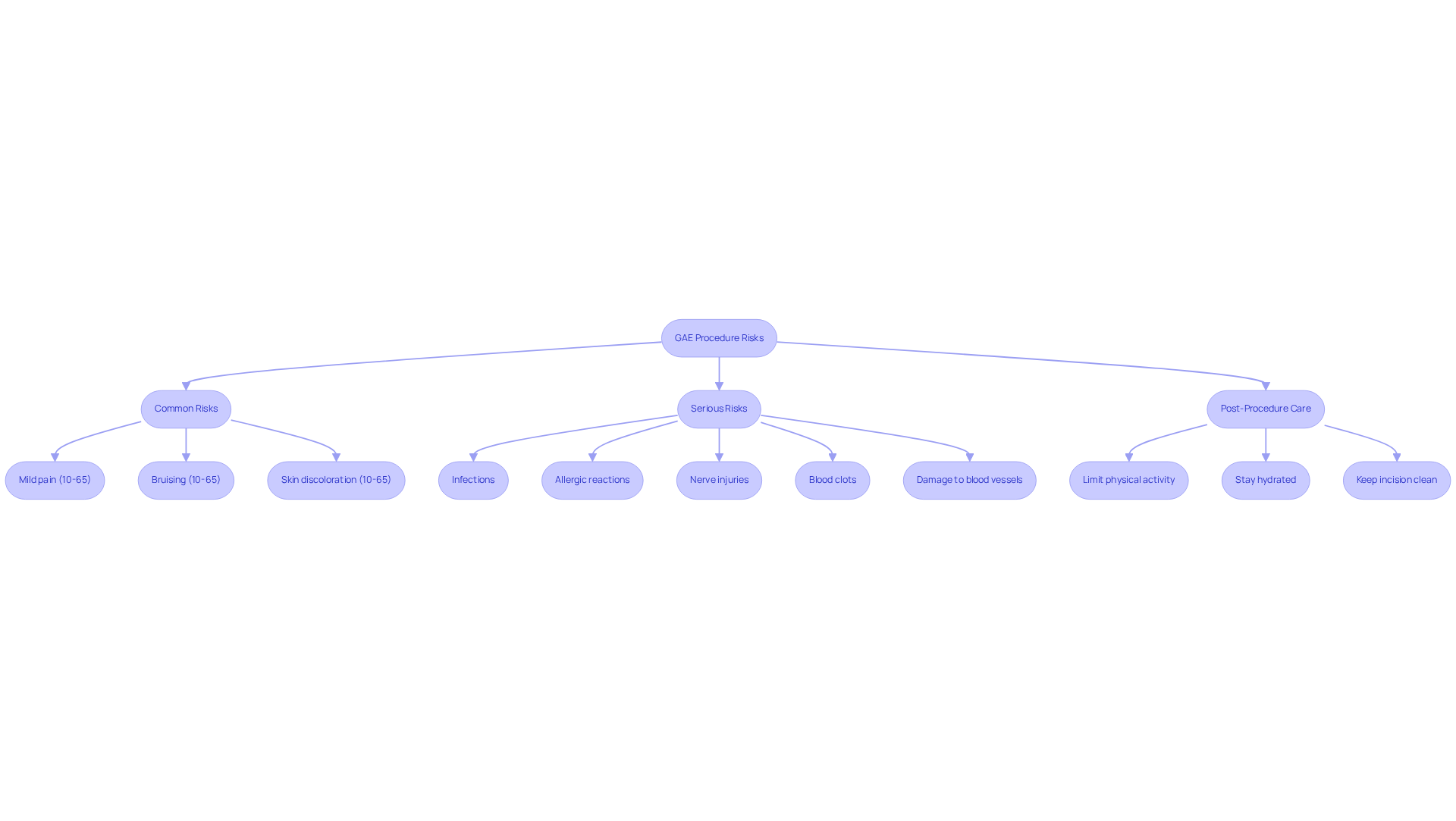
While Genicular Artery Embolization (GAE) is often regarded as a safe procedure, it’s crucial to be aware of the risks, particularly for our elderly loved ones. You might experience some mild pain, bruising, or discomfort—this happens in about 10-65% of cases due to non-target embolization, but don’t worry; it usually resolves within a few days.
While complications are rare, they can occur. These may include:
- Allergic reactions to the contrast dye
- Damage to nearby blood vessels
For older individuals, the risks associated with anesthesia and the procedure itself can be heightened due to existing health conditions. It’s crucial to have a discussion about your personal health history to determine if GAE is the right choice for you.
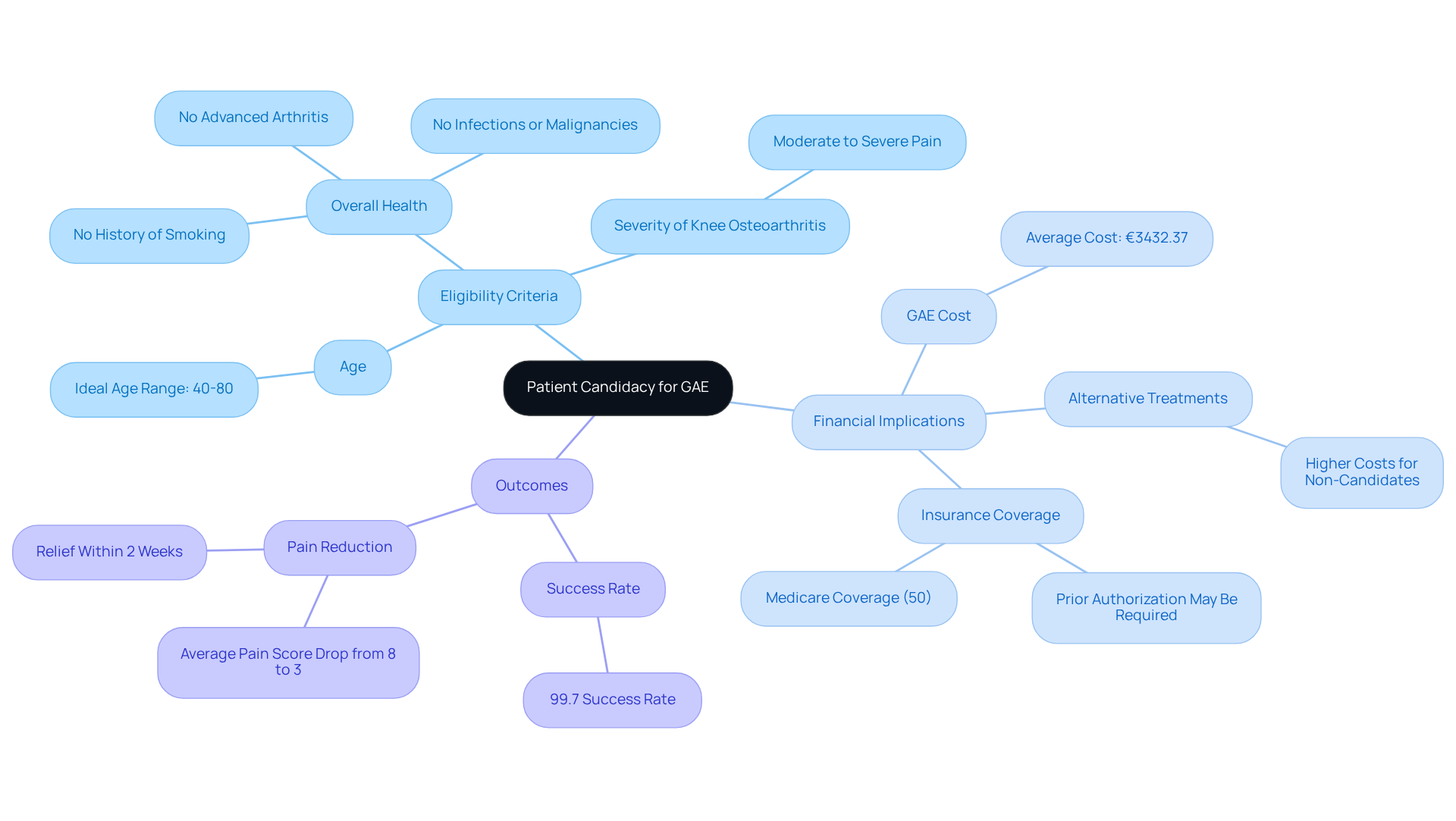
Studies show that GAE has a remarkable technical success rate of 99.7%, with complications occurring in about 5% of cases. This is reassuring, but it’s still essential to discuss any worries you may have with your doctor. After the procedure, taking care of yourself is vital. Make sure to:
- Limit physical activity
- Stay hydrated
- Keep the incision clean
These steps are key to a smooth recovery.
Regular follow-up visits are also important to monitor your progress and check for any side effects. Remember, you’re not alone in this journey. Your healthcare team is here to support you.
Evaluate the Benefits of GAE for Elderly Patients
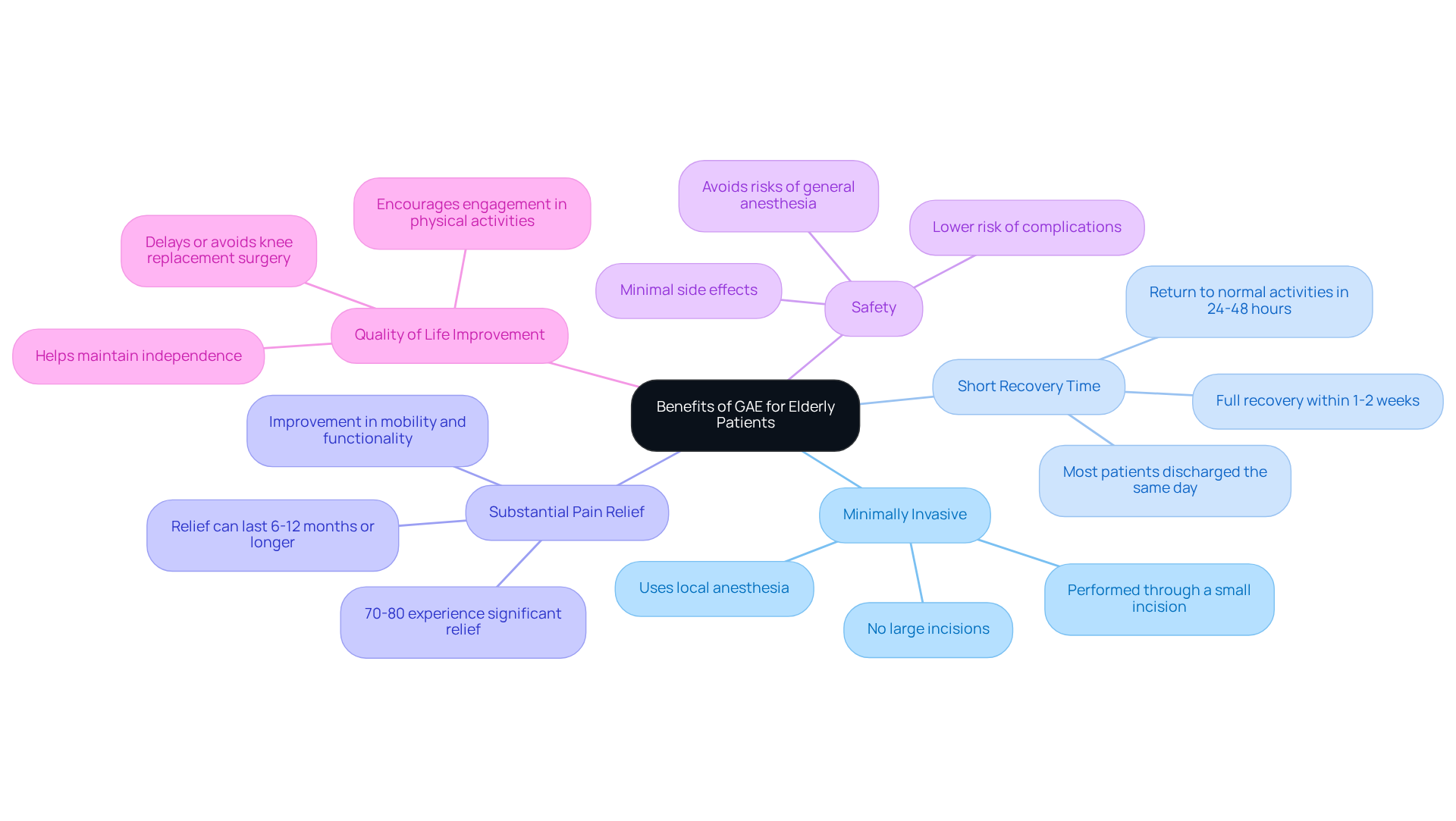
can be a wonderful option for older individuals facing knee pain. One of the most significant advantages is its minimally invasive nature, which often results in quicker recovery compared to traditional surgical methods. Most people find they can return to normal activities within just 24-48 hours after GAE. This is especially important for seniors who may have limited mobility and want to get back to doing what they love.
Clinical studies show that over 70-80% of individuals experience significant pain relief. This relief can empower them to engage more actively in physical therapy and rehabilitation, which is crucial for their recovery. Additionally, complications are avoided as it bypasses the dangers associated with general anesthesia, making it a safer choice for older adults who might have underlying health conditions.
Moreover, GAE can delay or even eliminate the need for more invasive procedures like joint replacement. This can significantly improve quality of life. By alleviating pain and improving mobility, GAE helps seniors maintain their independence and enjoy the activities they cherish.
As one expert notes, “GAE is ideal for adults with mild to moderate osteoarthritis of the knee who haven’t found relief from conservative treatments and want to avoid surgery.” If you or a loved one are struggling with knee pain, consider discussing GAE with your healthcare provider. It could be the supportive step you need towards a more active and fulfilling life.
Discuss Post-Procedure Care and Recovery
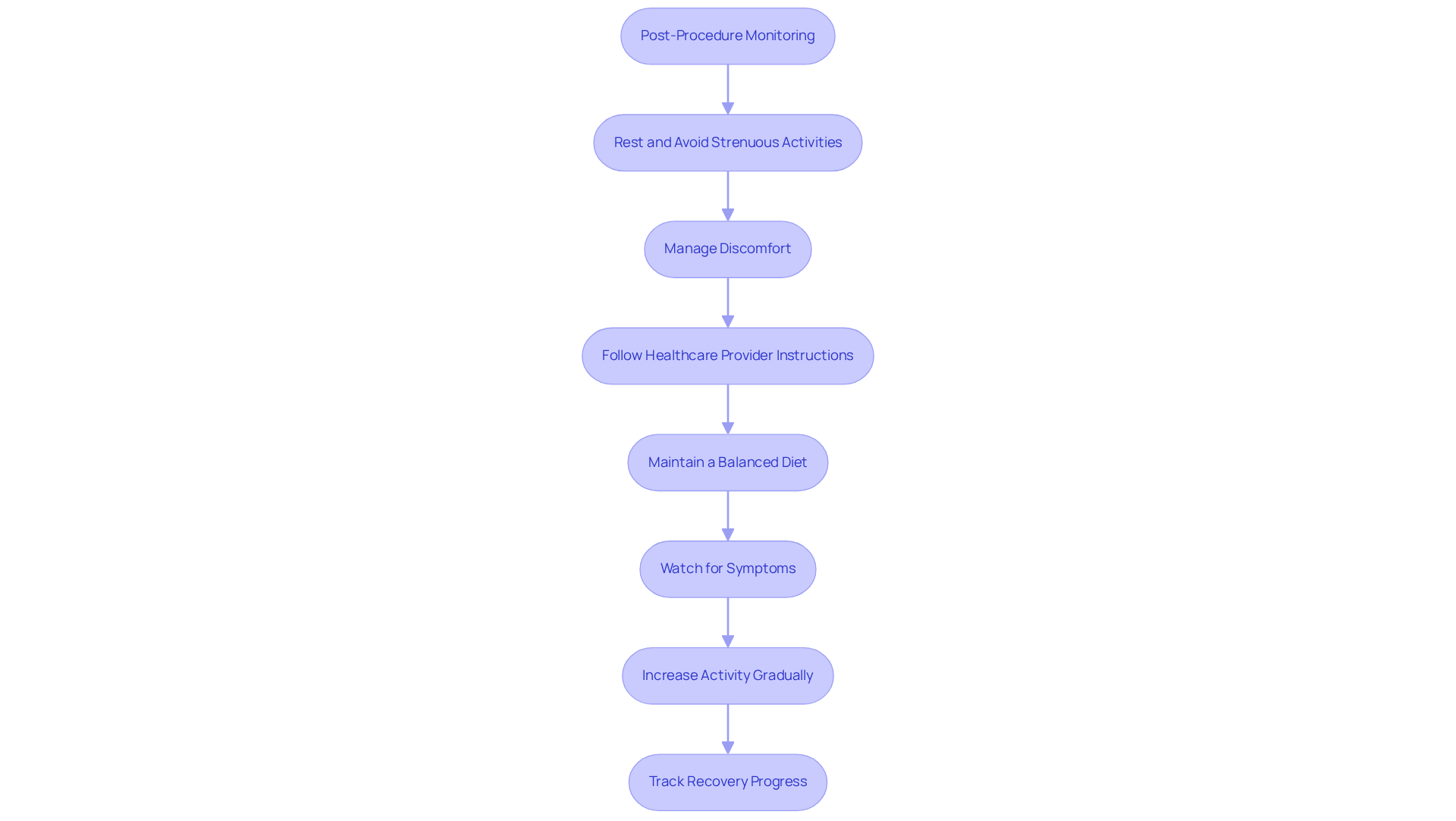
After undergoing Genicular Artery Embolization (GAE), it’s natural to have concerns about the procedure. Rest assured, individuals are closely monitored for a short period to ensure there are no immediate complications, considering the risks, and most can return home the same day. During recovery, it’s important to rest your knee and avoid strenuous activities for a few days. If you’re older, you might experience some slight discomfort or swelling, but don’t worry—this is usually manageable with over-the-counter pain relief.
Communication regarding activity levels and medications is crucial for a smooth recovery. A balanced diet rich in whole foods and staying hydrated can significantly aid in healing, helping to reduce inflammation and manage any discomfort. Regular follow-up appointments are essential for monitoring and evaluating how well the procedure worked for you.
Stay vigilant for any troubling symptoms, such as increased discomfort, swelling, or signs of infection at the injection site. If you notice anything concerning, please reach out to your healthcare provider right away. Typically, seniors can expect a gradual improvement in discomfort and functionality within the first few weeks, with many experiencing enhanced mobility.
As you recover, consider gradually increasing your activity by about 10% each week. The overall success rate of GAE is quite high, with over 70-80% of individuals reporting long-term benefits. This makes it a promising option for managing knee pain. Keeping a recovery journal or checklist can also be a helpful way to track your progress during this time. Remember, you’re not alone in this journey—support is available.
Conclusion
Genicular Artery Embolization (GAE) offers a hopeful solution for elderly patients grappling with chronic knee pain. This minimally invasive procedure stands as a gentle alternative to traditional surgeries, providing significant relief while allowing for a quicker recovery. For seniors who cherish their independence and quality of life, GAE can be an appealing option. Yet, it’s essential to understand the associated risks to make an informed choice about this treatment.
Throughout this discussion, we’ve highlighted the effectiveness of GAE, showcasing a success rate of 70-80% in alleviating discomfort, alongside a remarkably low complication rate. While minor side effects like bruising and mild pain may arise, serious complications are quite rare. It’s crucial for older individuals, especially those with pre-existing conditions, to have open conversations with their healthcare providers about any personal health concerns. Emphasizing post-procedure care and a gradual recovery process reinforces the importance of a tailored approach to each patient’s unique situation.
Ultimately, the GAE procedure represents a significant advancement in managing knee pain for seniors. It not only enhances mobility and quality of life but also provides a pathway to avoid more invasive surgeries. As more individuals consider this option, engaging in open discussions with healthcare professionals is vital to weigh the benefits against the risks. Embracing this innovative treatment could be the key to reclaiming an active and fulfilling lifestyle.
Are you ready to take the next step towards relief? Your journey to a more comfortable life is just a conversation away.
Frequently Asked Questions
What is Genicular Artery Embolization (GAE)?
Genicular Artery Embolization (GAE) is a minimally invasive procedure designed to relieve persistent knee pain, particularly from osteoarthritis, by injecting small particles into the genicular arteries that supply blood to the knee joint, reducing blood flow to inflamed tissues.
How does the GAE procedure work?
The procedure involves injecting small particles into the genicular arteries, which selectively blocks these arteries, leading to reduced blood flow to inflamed tissues in the knee, resulting in less pain and swelling.
What type of anesthesia is used during the GAE procedure?
GAE is performed under local anesthesia.
What is the typical recovery time after GAE?
The recovery period after GAE is typically 1-2 weeks, which is shorter compared to the 6-12 months often required for conventional joint surgeries.
What is the success rate of GAE in alleviating joint discomfort?
GAE has a success rate of 70-80% in alleviating joint discomfort.
Who can benefit from GAE?
Many seniors and individuals who struggle with knee pain and are not candidates for traditional surgery may benefit from GAE.
What are the advantages of GAE over traditional surgeries?
GAE is a convenient option that allows for same-day discharge, has a shorter recovery period, and poses lower risks compared to traditional surgeries.
Are there any ongoing developments in GAE techniques?
Yes, recent advancements in GAE techniques continue to enhance its safety and efficacy, making it a preferred option for older adults seeking to maintain their independence and active lifestyles.
What do case studies say about the effectiveness of GAE?
Case studies highlight that individuals who previously faced persistent joint pain and were not candidates for surgery have experienced lasting relief and improved functionality after undergoing GAE.
Where can I find more information about GAE?
If you are considering GAE, it is recommended to reach out for more information and support from healthcare professionals.
List of Sources
- Define Genicular Artery Embolization (GAE) Procedure
- Genicular artery embolization for knee osteoarthritis: a systematic review with meta-analysis and cost-analysis (https://sciencedirect.com/science/article/pii/S0213911125000135)
- Genicular Artery Embolization: A Technical Review of Anatomy, Pathophysiology, Current Experiences, and Future Directions – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11943379)
- 8 Things to Know About Genicular Artery Embolization for Knee Pain in Seniors – Pittsburgh Vascular Specialists (https://greaterpittsburghvascular.com/2024/10/20/8-things-to-know-about-genicular-artery-embolization-for-knee-pain-in-seniors)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9971280)
- Early intervention in knee osteoarthritis with genicular artery embolization is associated with improved clinical outcomes – European Radiology (https://link.springer.com/article/10.1007/s00330-025-11702-1)
- Identify Risks Associated with GAE Procedure
- kneepaincentersofamerica.com (https://kneepaincentersofamerica.com/blog/potential-risks-and-side-effects-of-genicular-artery-embolization)
- oarsijournal.com (https://oarsijournal.com/article/S1063-4584(22)00615-X/fulltext)
- Evaluate the Benefits of GAE for Elderly Patients
- americankneepaincenters.com (https://americankneepaincenters.com/blog/6-benefits-of-genicular-artery-embolization)
- Genicular Artery Embolization for Knee Pain Relief (https://preferredvasculargroup.com/how-does-genicular-artery-embolization-relieve-knee-pain)
- 8 Things to Know About Genicular Artery Embolization for Knee Pain in Seniors – Pittsburgh Vascular Specialists (https://greaterpittsburghvascular.com/2024/10/20/8-things-to-know-about-genicular-artery-embolization-for-knee-pain-in-seniors)
- A New Option for Knee Pain: Genicular Artery Embolization (GAE) (https://richmondvascularcenter.com/news/a-new-option-for-knee-pain-genicular-artery-embolization-gae)
- Discuss Post-Procedure Care and Recovery
- Enhancing Recovery after GAE Procedure – CrannMed (https://crannmed.com/enhancing-recovery-after-gae-procedure)
- Recovery Tips After Genicular Artery Embolization (GAE) (https://unitedkneecenters.com/2025/02/19/recovery-tips-after-gae)
- GAE Recovery | Healing from Genicular Arterial Embolization (https://gaknees.com/what-is-gae/post-gae-recovery)
- “Arthritis Pain Relief: Minimally Invasive Procedures Offer Relief Without Surgery” I Vascular & Interventional Partners (https://vipinterventional.com/blog/arthritis-pain-relief-minimally-invasive-procedures-offer-relief-without-surgery-i-vascular-interventional-partners)
- Genicular Artery Embolization Explained | The Vascular Care Group (https://thevascularcaregroup.com/about-us/news/what-to-expect-before-during-and-after-genicular-artery-embolization)