Introduction
Deep Vein Thrombosis (DVT) represents a serious health concern, especially for the elderly, whose unique vulnerabilities can lead to significant complications if not addressed promptly. This article aims to provide a compassionate guide, shedding light on the treatment options available for older patients facing this condition.
Yet, the path to effective management can be challenging—how can caregivers and patients feel empowered with the right knowledge and resources to tackle DVT effectively?
By delving into the nuances of DVT treatment, readers will discover essential strategies that not only address immediate worries but also lay the foundation for long-term health and well-being.
Understand Deep Vein Thrombosis (DVT)
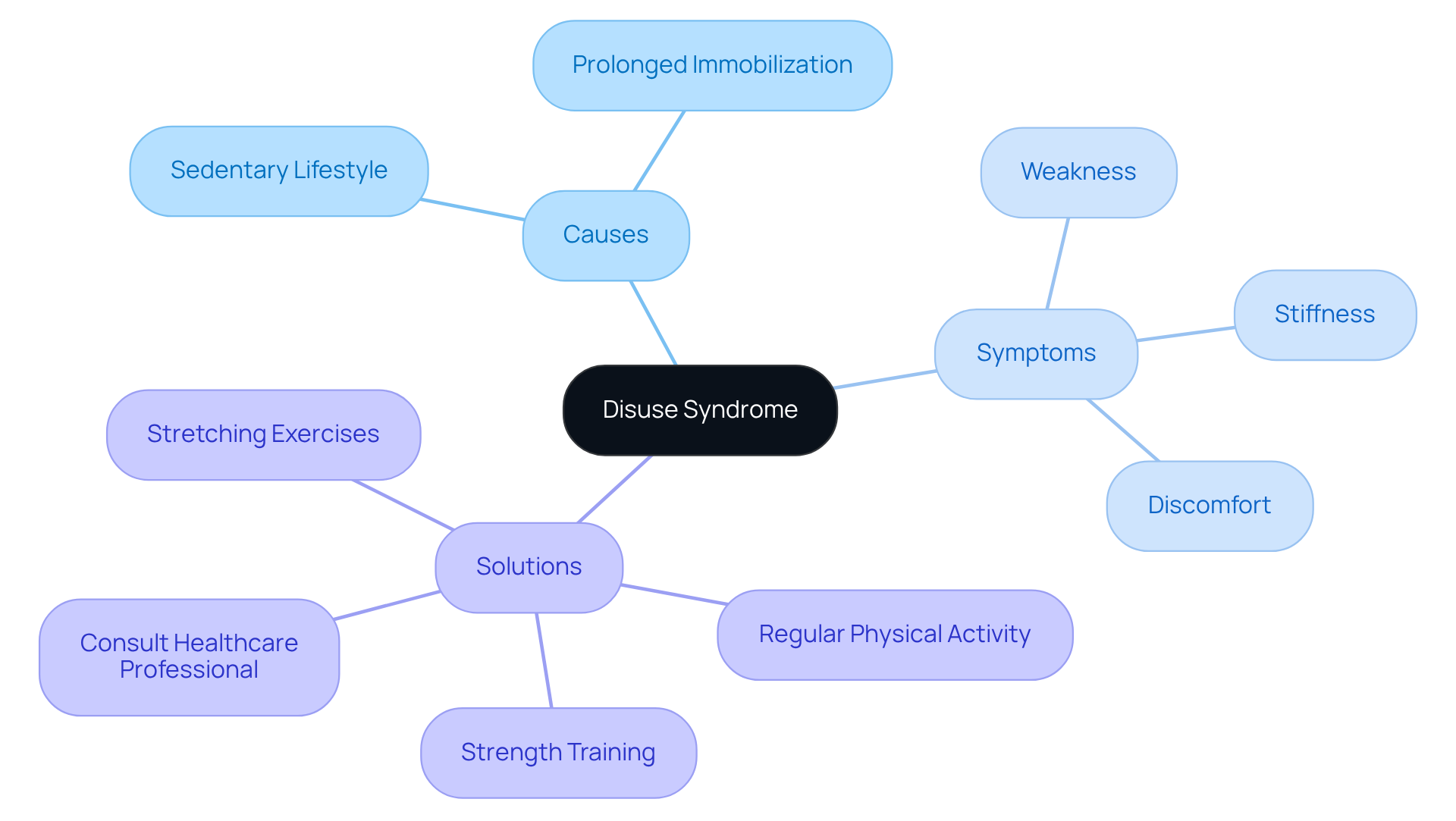
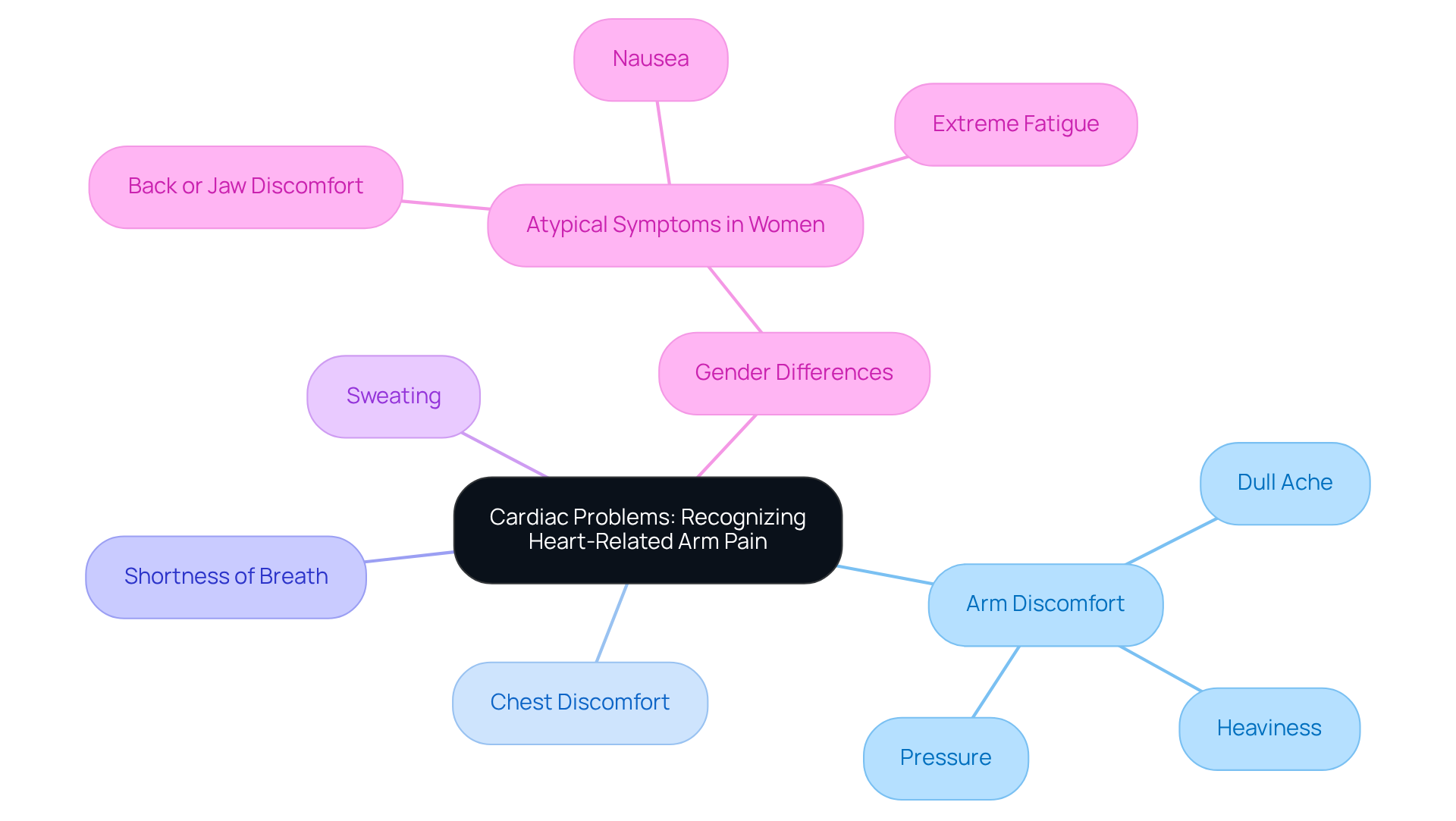
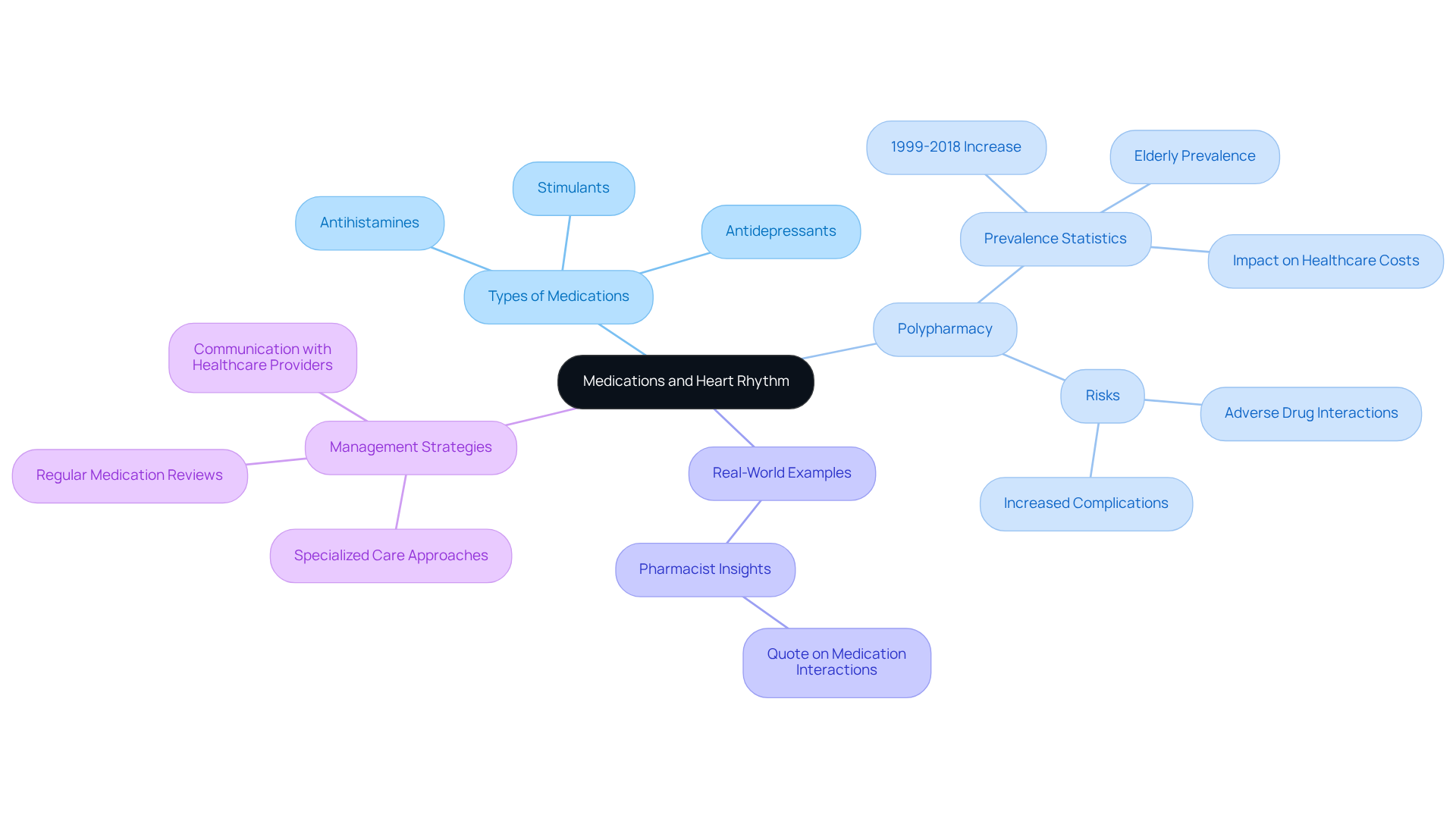
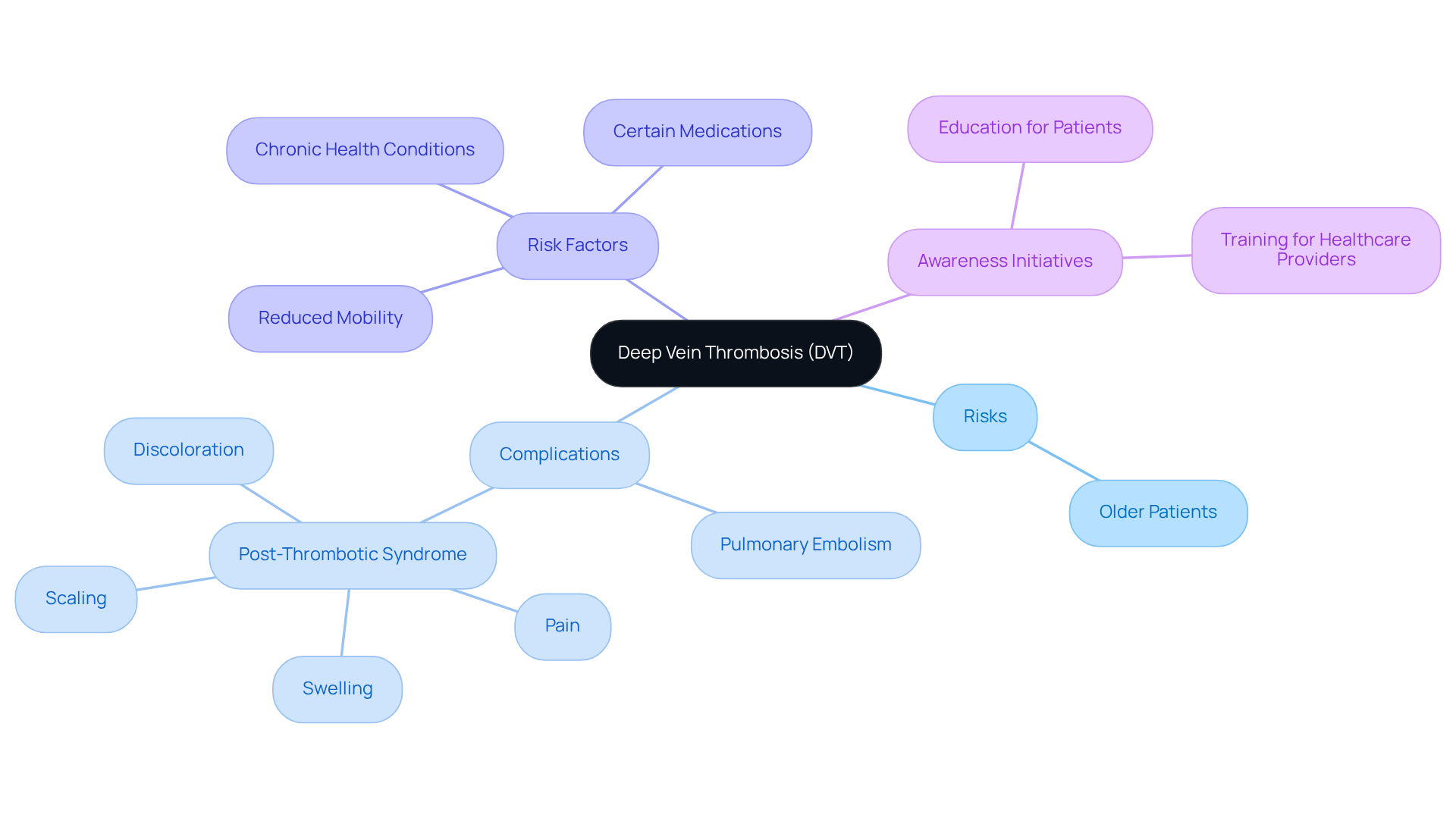
is a serious condition that involves the formation of a blood clot in a deep vein, most often in the legs. This condition can pose significant risks, particularly for older patients, who may face complications like pulmonary embolism if the clot dislodges and travels to the lungs. Factors that increase the likelihood of DVT in older adults include:
- Reduced mobility
- Certain medications that may make them more susceptible to clot formation
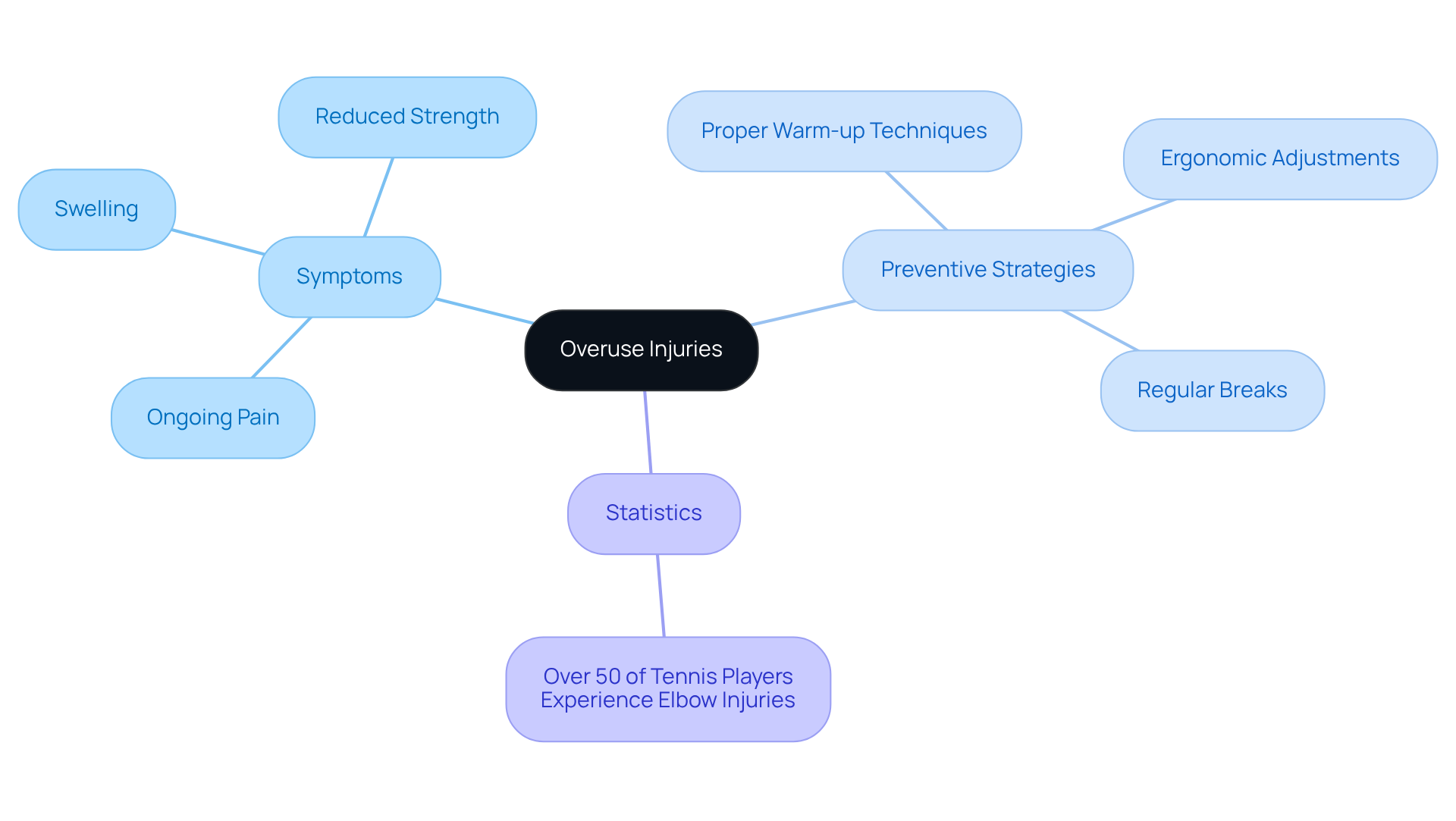
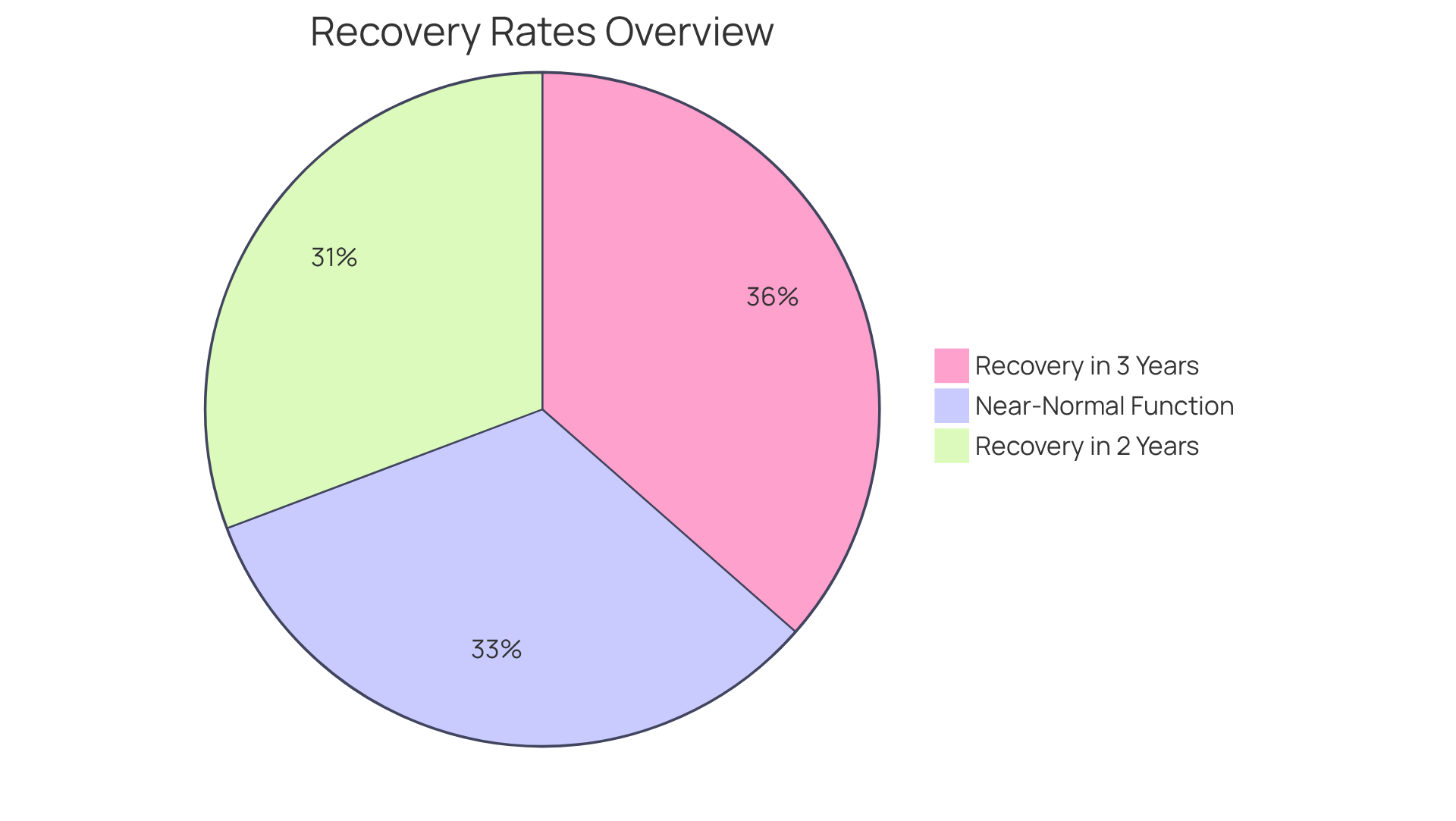
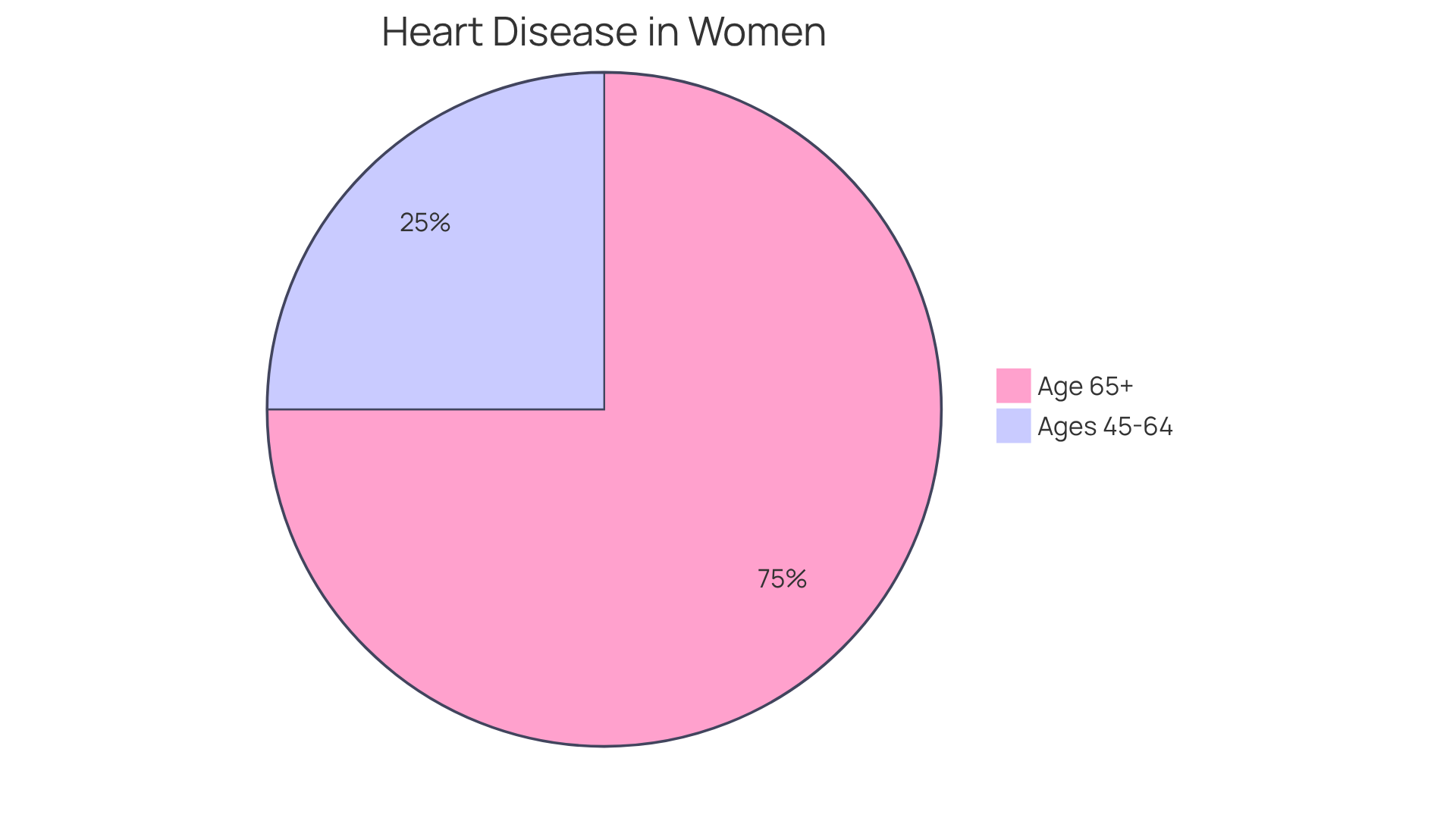
Awareness is essential, especially since studies show that elderly individuals are particularly at risk for its complications. For example, nearly one-third to one-half of those who have experienced a DVT may endure long-term effects, such as post-thrombotic syndrome, which can lead to swelling, pain, and discoloration in the affected limb. Additionally, the recurrence rate is notable, with approximately 33% of individuals experiencing another event within ten years.
Recent studies underscore the importance of preventive strategies, which have proven to enhance health outcomes for older individuals. These initiatives aim to educate both patients and healthcare providers about the signs and symptoms of DVT, promoting early intervention and preventive measures. Cardiologists stress that recognizing and managing DVT in a timely manner can greatly diminish the risk of severe complications, making awareness and education crucial components of effective treatment.
If you or a loved one are concerned about DVT, remember that seeking help is a vital step. There are resources and support available to guide you through understanding this condition better, ensuring you receive the care you need. Your health matters, and taking action can lead to a healthier future.
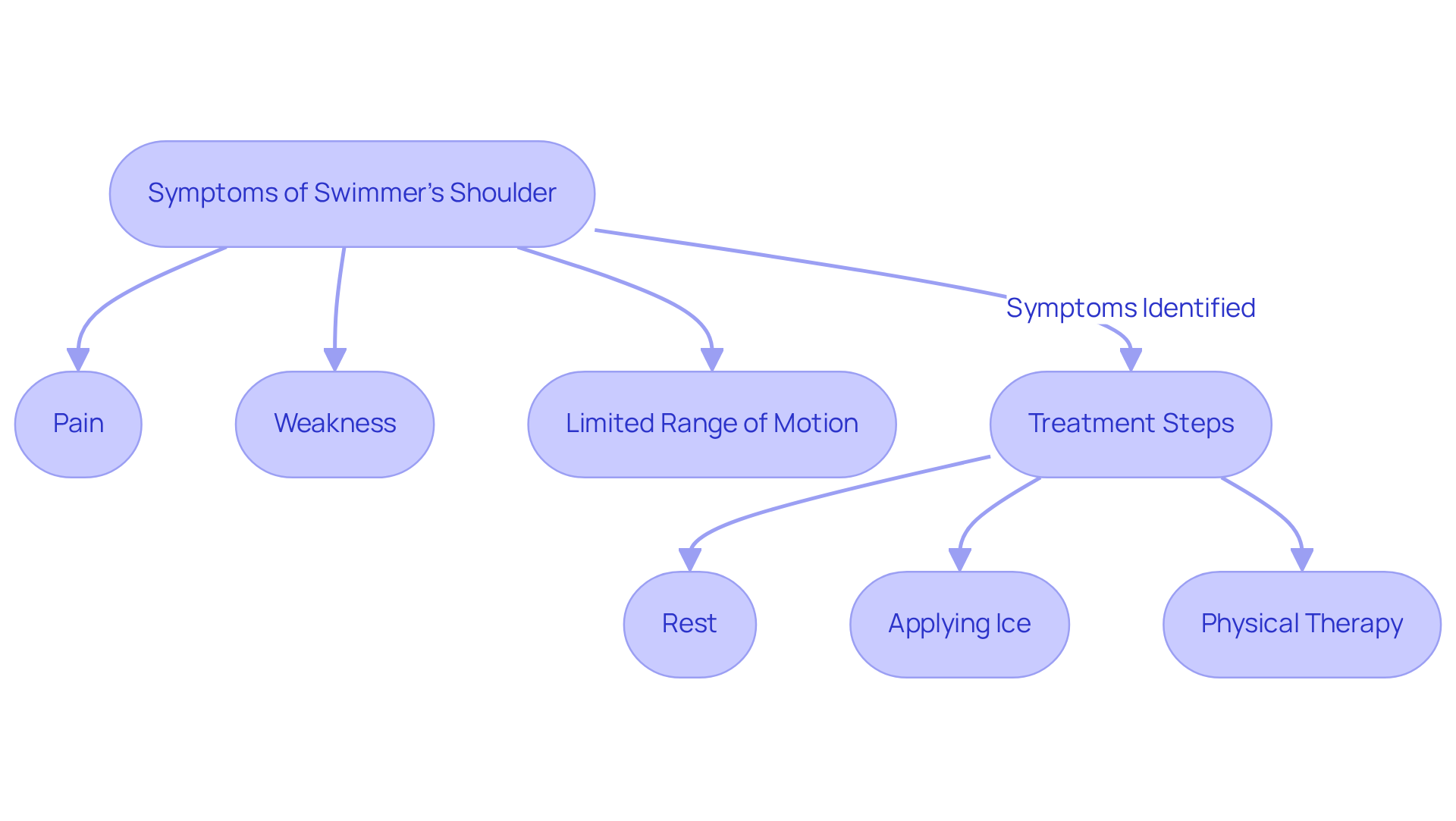
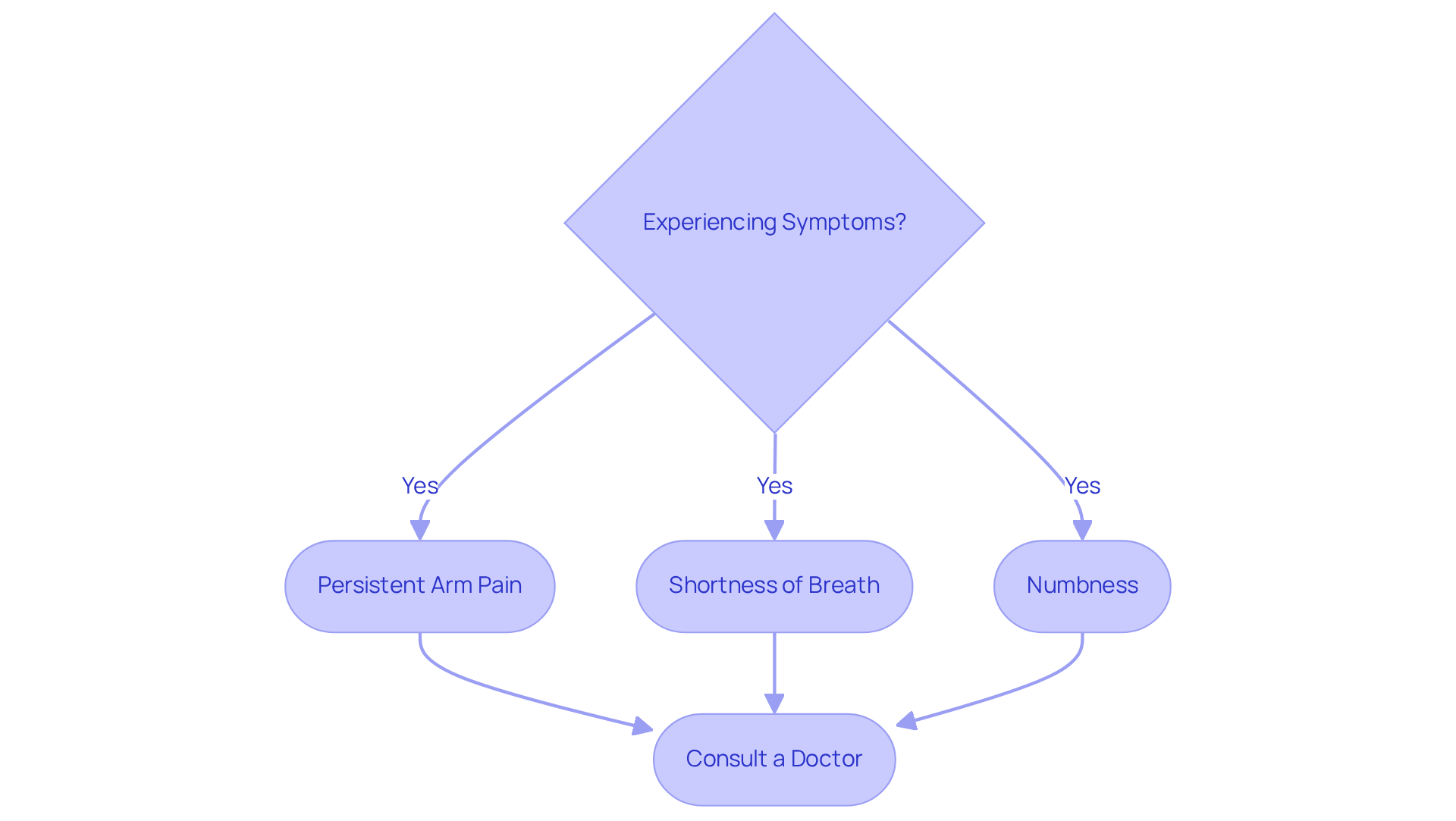
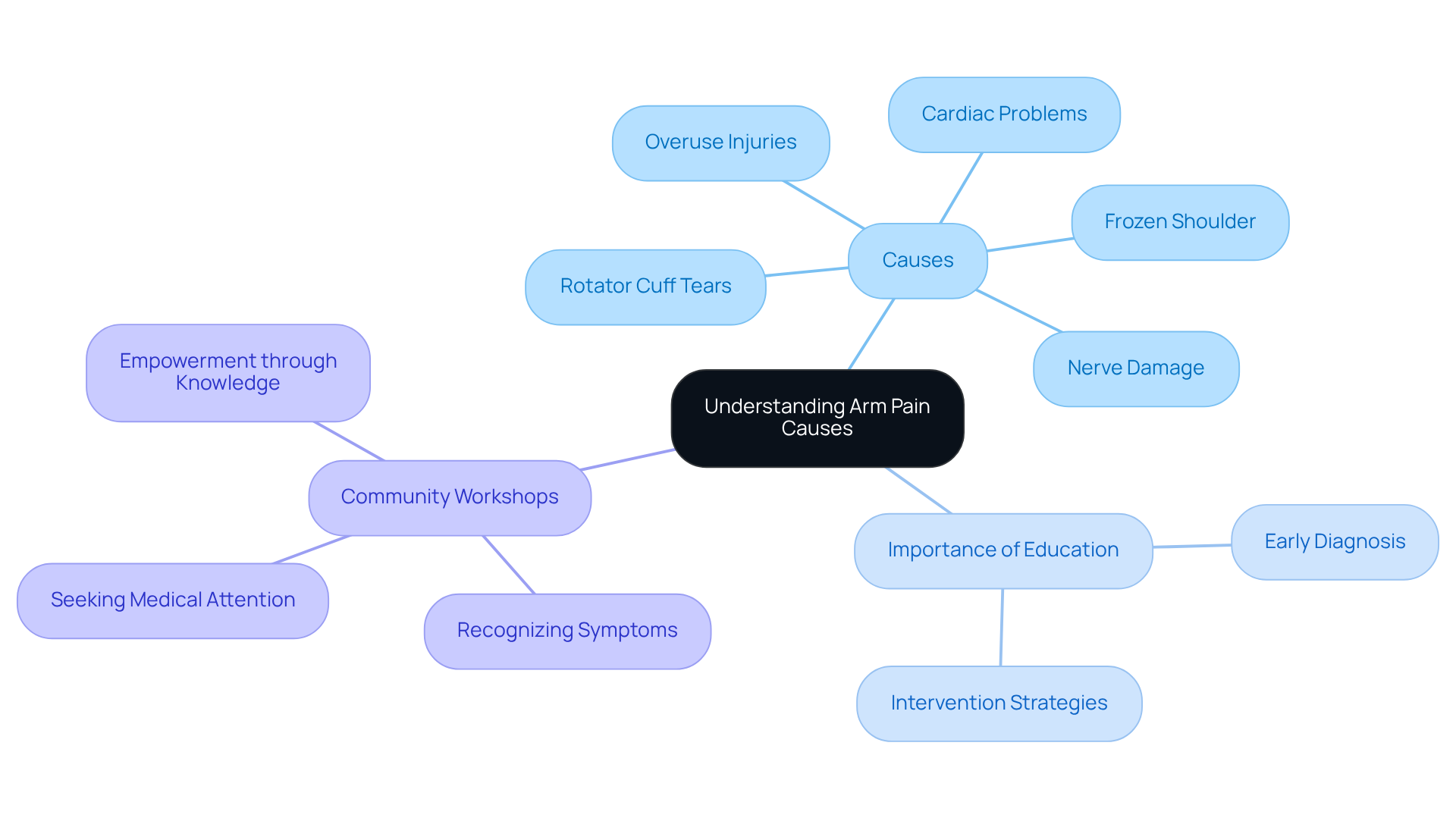
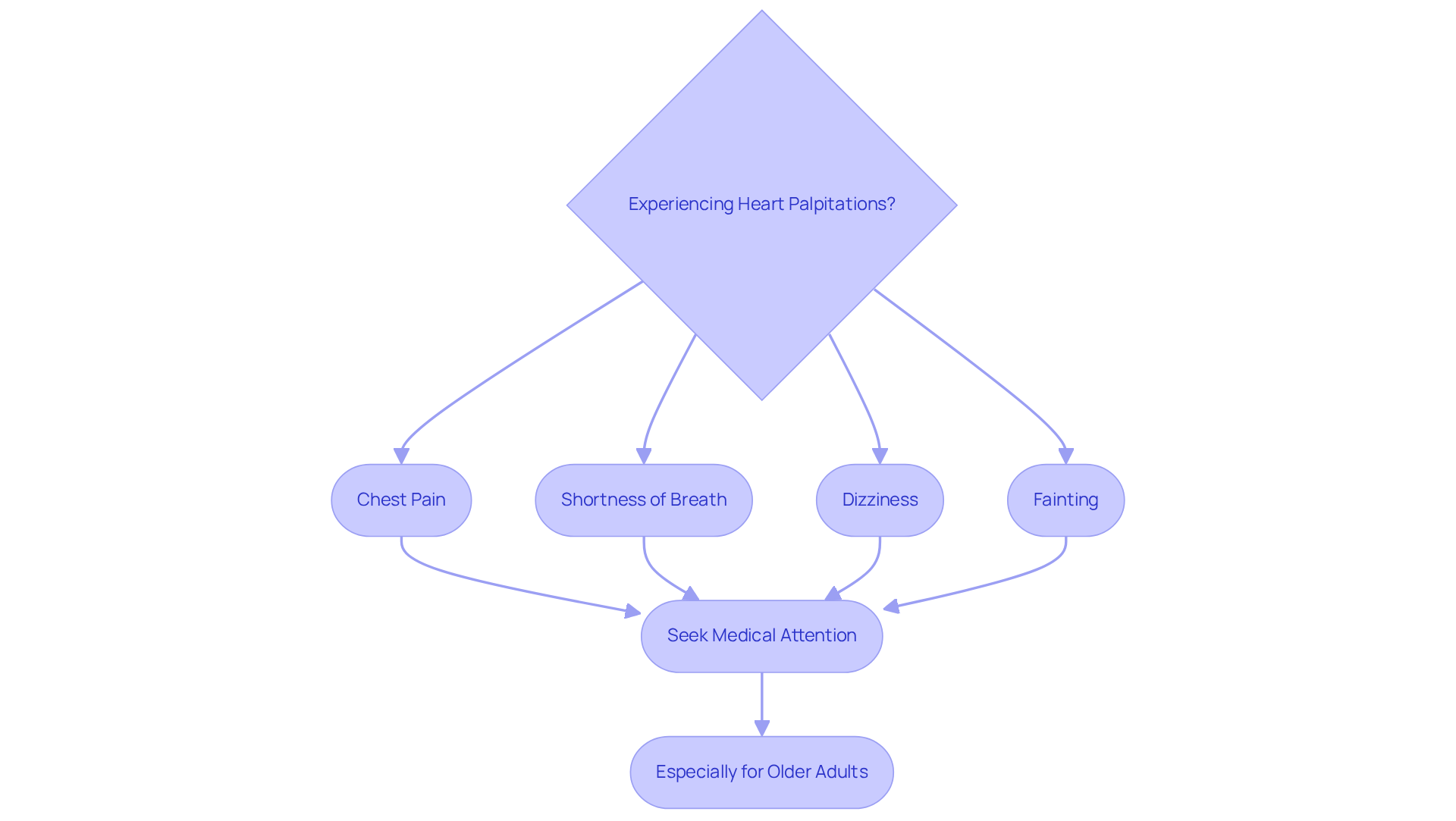
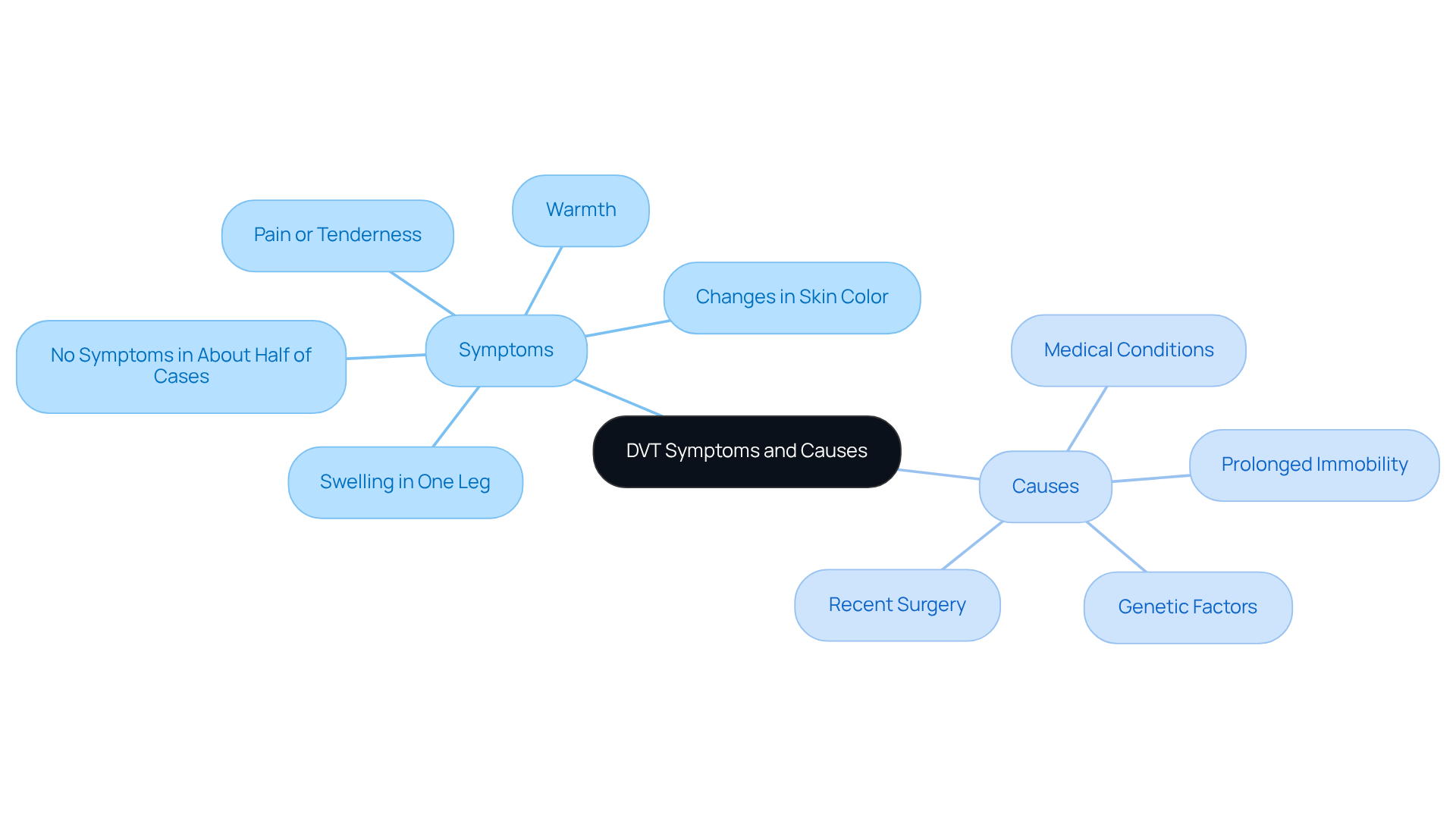
Identify Symptoms and Causes of DVT
can manifest through common symptoms:
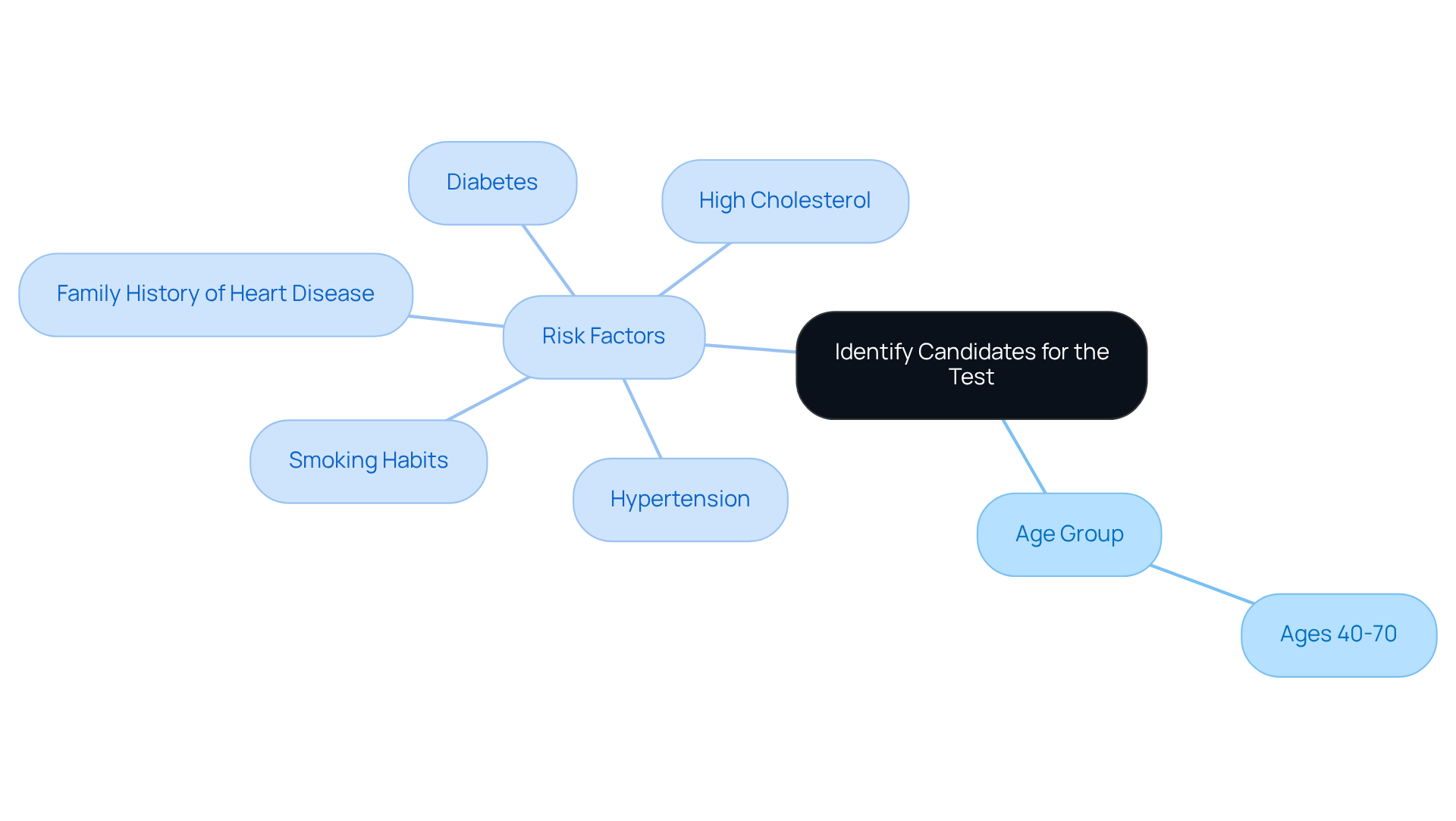
However, it’s important to note that about half of those with DVT may not experience any symptoms at all. This makes diagnosis challenging, particularly for our elderly patients. Factors such as recent surgery, certain medical conditions like cancer or heart disease, and genetic factors can all contribute to the development of DVT in older adults. Research indicates that as we age, especially after 40, the likelihood of developing DVT increases significantly. Additionally, conditions such as obesity and a history of thrombosis further elevate this risk.
Geriatric experts emphasize the importance of recognizing these signs early. Prompt medical action can help prevent complications, such as pulmonary embolism and post-thrombotic syndrome, which may lead to long-term issues. Furthermore, signs like swelling, pain, or visible veins in the legs could suggest chronic venous insufficiency (CVI), a condition where blood accumulates in the legs due to valve dysfunction. If left unaddressed, this can worsen throughout the day and potentially lead to skin ulcers.
At Amavita Heart and Vascular Health, we are dedicated to providing comprehensive care to manage CVI and enhance circulation. It’s crucial for caregivers and individuals to be aware of these factors and to reach out to their doctor promptly to understand if they notice any signs of the condition. Remember, you are not alone in this journey; we are here to support you every step of the way.
Diagnose DVT Effectively
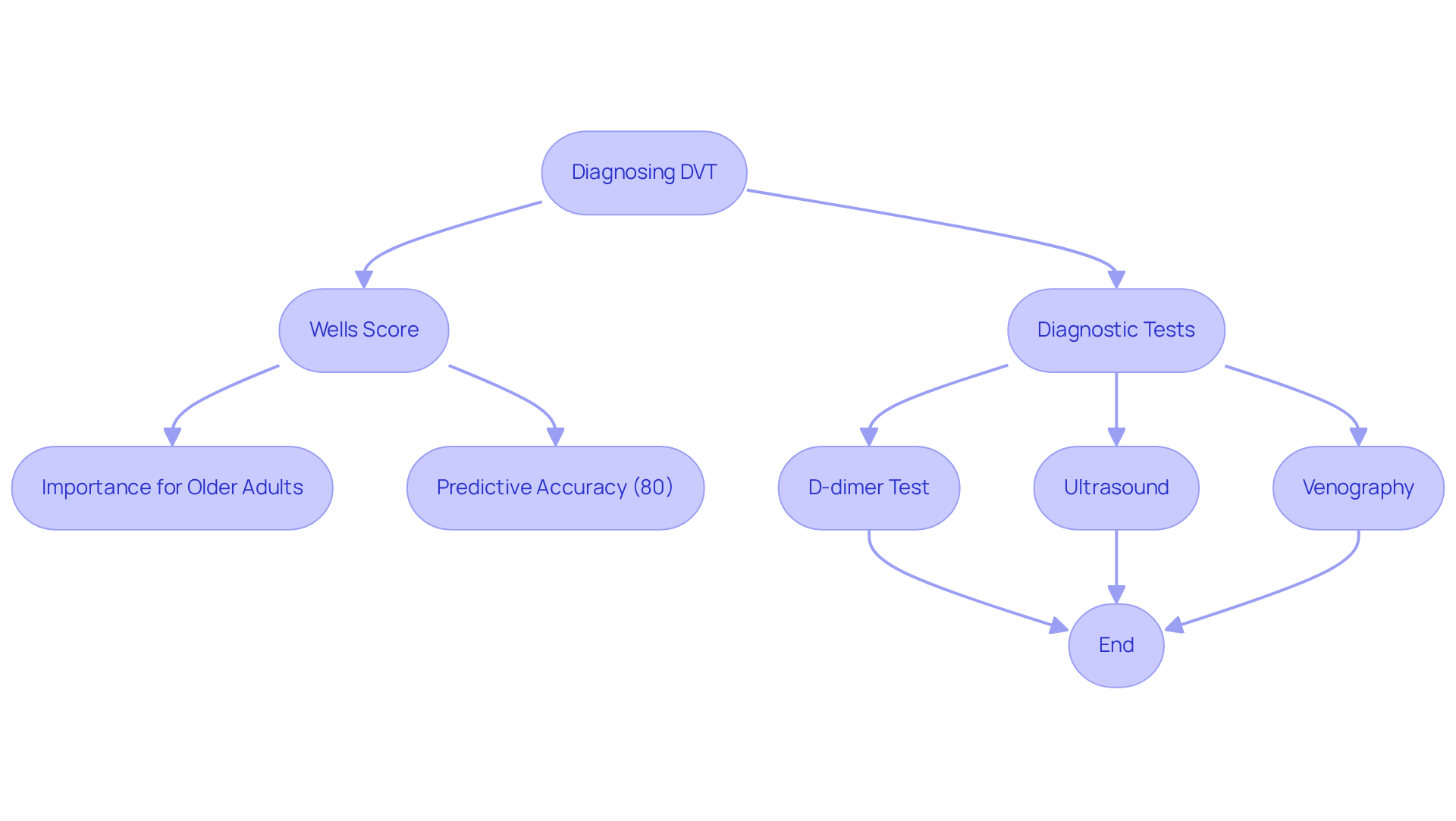
Diagnosing DVT requires a thoughtful evaluation that combines physical examinations with specific tests. One essential tool in this process is the Wells Score, which helps assess the likelihood of DVT based on an individual’s symptoms and contributing factors. This scoring system is particularly beneficial for older adults, as it takes into account age-related factors that may influence the risk of DVT.
Common tests used alongside the Wells Score include:
- D-dimer test: This test measures the levels of a substance released when a blood clot dissolves. Elevated D-dimer levels can suggest the presence of DVT, although they are not definitive on their own.
- Ultrasound: A test that uses sound waves to visualize blood flow in the veins, making it a primary method for detecting DVT.
- Venography: This X-ray test involves injecting a contrast dye into a large vein, allowing for the identification of clots. While less commonly used today, it can provide valuable information in certain cases.
The Wells Score has demonstrated high accuracy in diagnosing DVT, with studies indicating that it can effectively stratify risk in older individuals. For example, research suggests that the Wells Score can reliably predict DVT in approximately 80% of cases among older individuals. Experts highlight its significance, noting that a higher score correlates with an increased likelihood of DVT. Dr. Kahn, a respected researcher in vascular health, shares, “In individuals with acute DVT, early walking exercise is safe and may assist in alleviating acute issues,” underscoring the importance of early intervention.
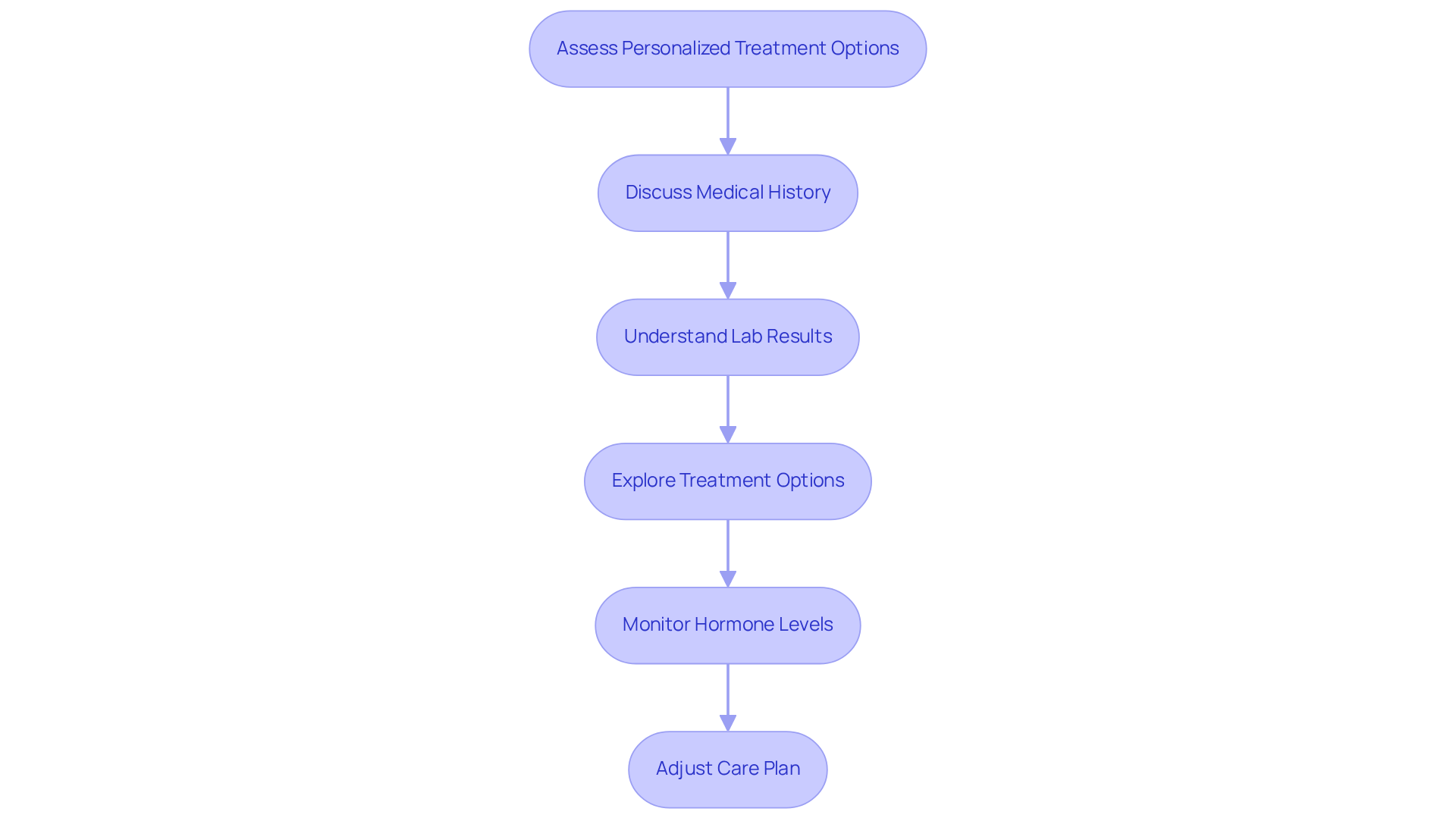
Understanding these diagnostic tools empowers patients and caregivers to engage more effectively with healthcare providers, ensuring better outcomes. Additionally, preparing for DVT appointments by listing symptoms, personal health information, and questions can facilitate better communication and enhance the overall healthcare experience. Remember, you are not alone in this journey, and seeking help is a positive step towards better health.
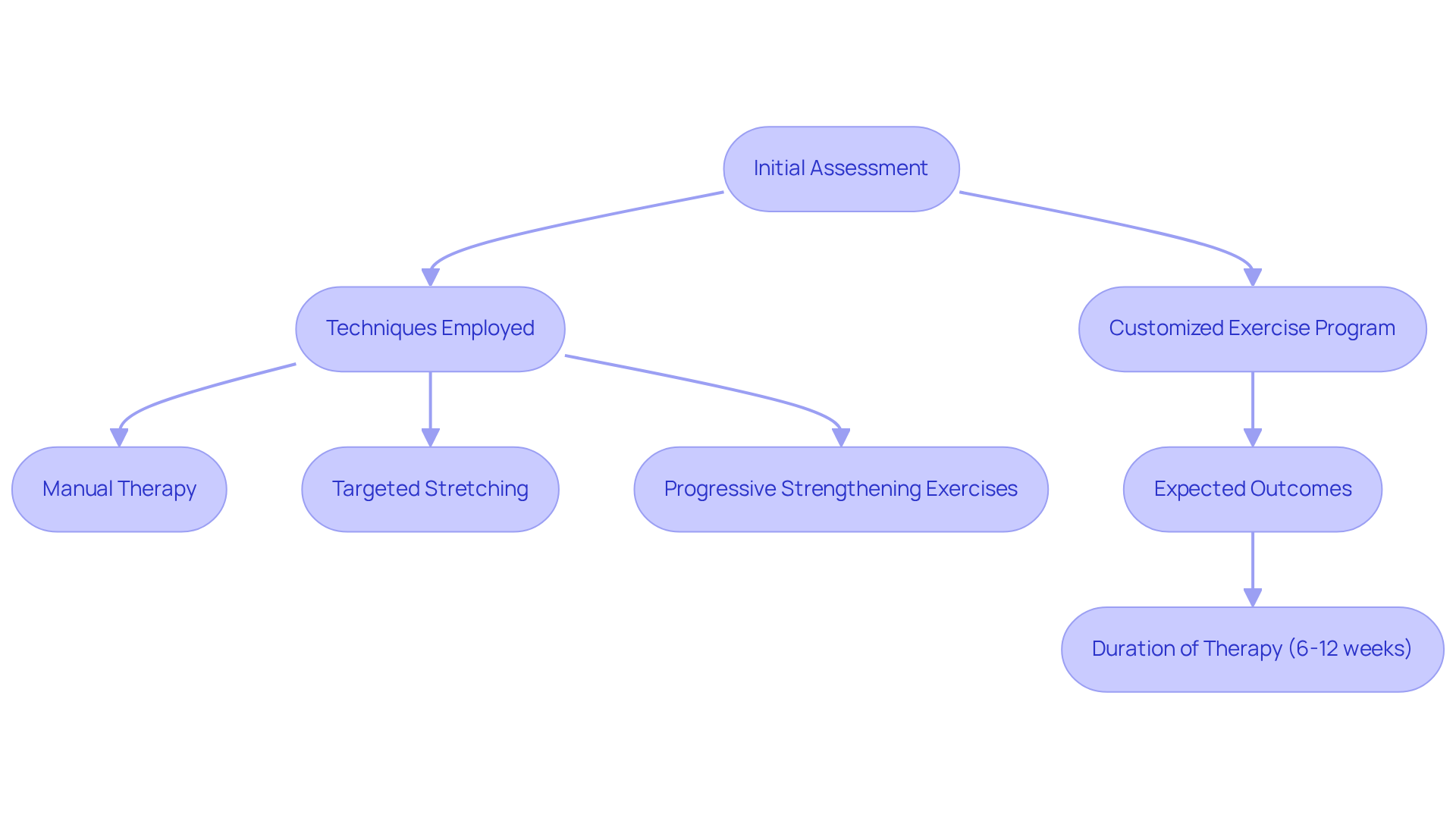
Implement Treatment Strategies for DVT
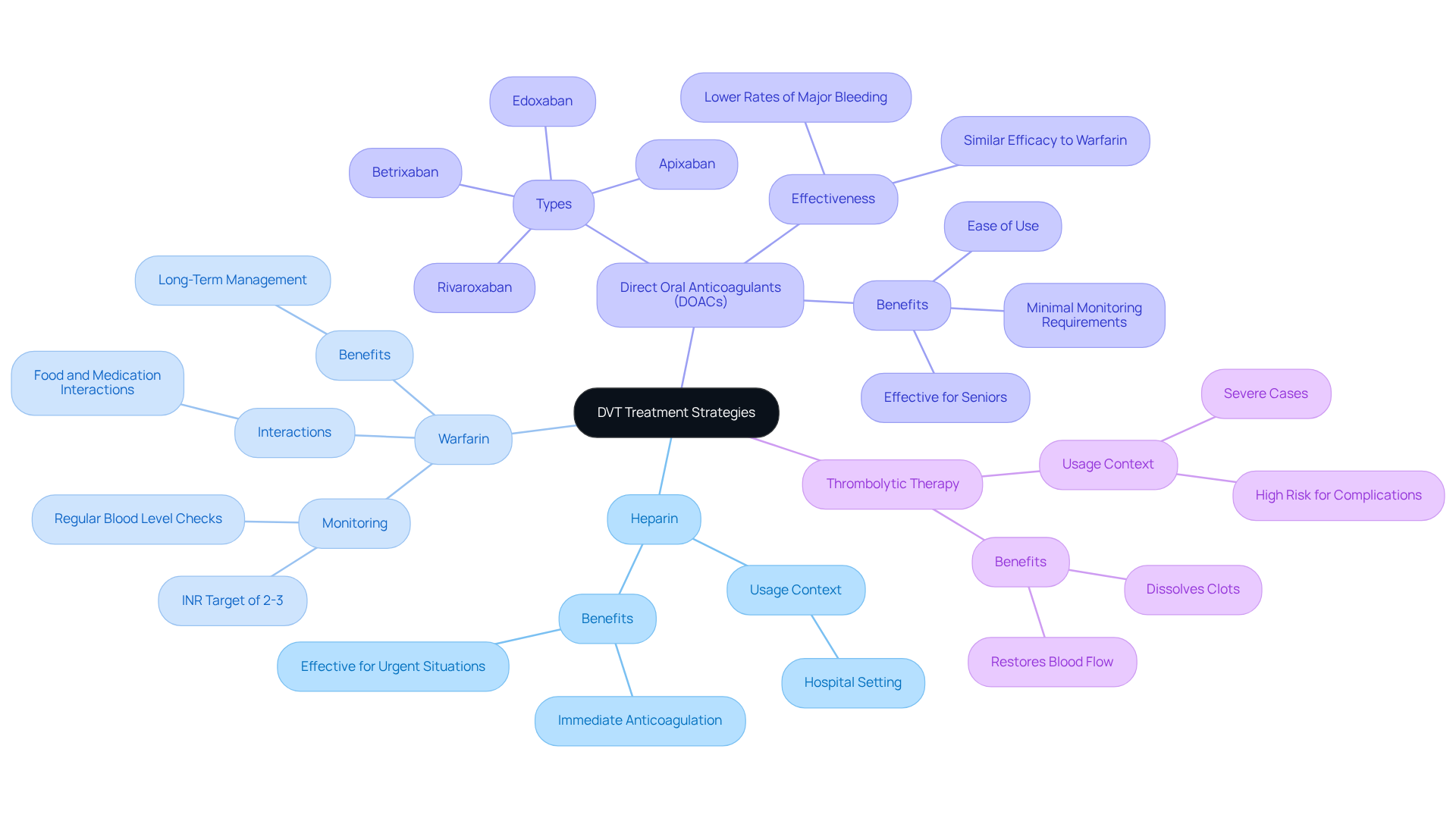
A crucial aspect of managing deep vein thrombosis (DVT) is understanding treatment options, primarily involving medications that prevent further clotting and reduce the risk of pulmonary embolism. Understanding DVT treatment can feel overwhelming, but rest assured, there are resources available.
- Heparin: Often given in a hospital setting, heparin acts quickly and is effective for immediate anticoagulation, providing peace of mind during urgent situations.
- Warfarin: This medication requires monitoring of blood levels to ensure it remains effective, as it may interact with various foods and medications. Your healthcare provider will guide you through this process, including information on dosage adjustments, making it manageable.
- Direct oral anticoagulants: Medications like rivaroxaban, apixaban, edoxaban, and betrixaban are gaining popularity for their ease of use and minimal monitoring requirements. These agents work by directly blocking specific factors in the coagulation cascade, making them suitable for many older adults.
Many hematologists highlight that DOACs offer significant benefits for seniors, simplifying management and reducing the frequency of blood tests. Studies show that these medications are as effective as traditional anticoagulants like warfarin, with lower rates of major bleeding complications. For context, understanding DVT treatment includes the use of low-molecular-weight heparins, which is typically 7-14 days and is important for your recovery.
In more severe cases, thrombolysis may be used to dissolve clots. This approach is typically reserved for individuals experiencing significant limb ischemia or those at high risk for complications. While success rates for thrombolysis can vary, recent data suggests that DOACs have shown promising results, with many patients reporting relief and an improved quality of life.
A systematic review by Kahn et al. found that engaging in early walking exercises is safe and may help alleviate acute symptoms, underscoring the importance of patient involvement in your treatment plan. Have you considered discussing your options with your healthcare provider? It’s essential to explore treatment alternatives while considering the most appropriate treatments tailored to your overall health and any other medications you may be taking.
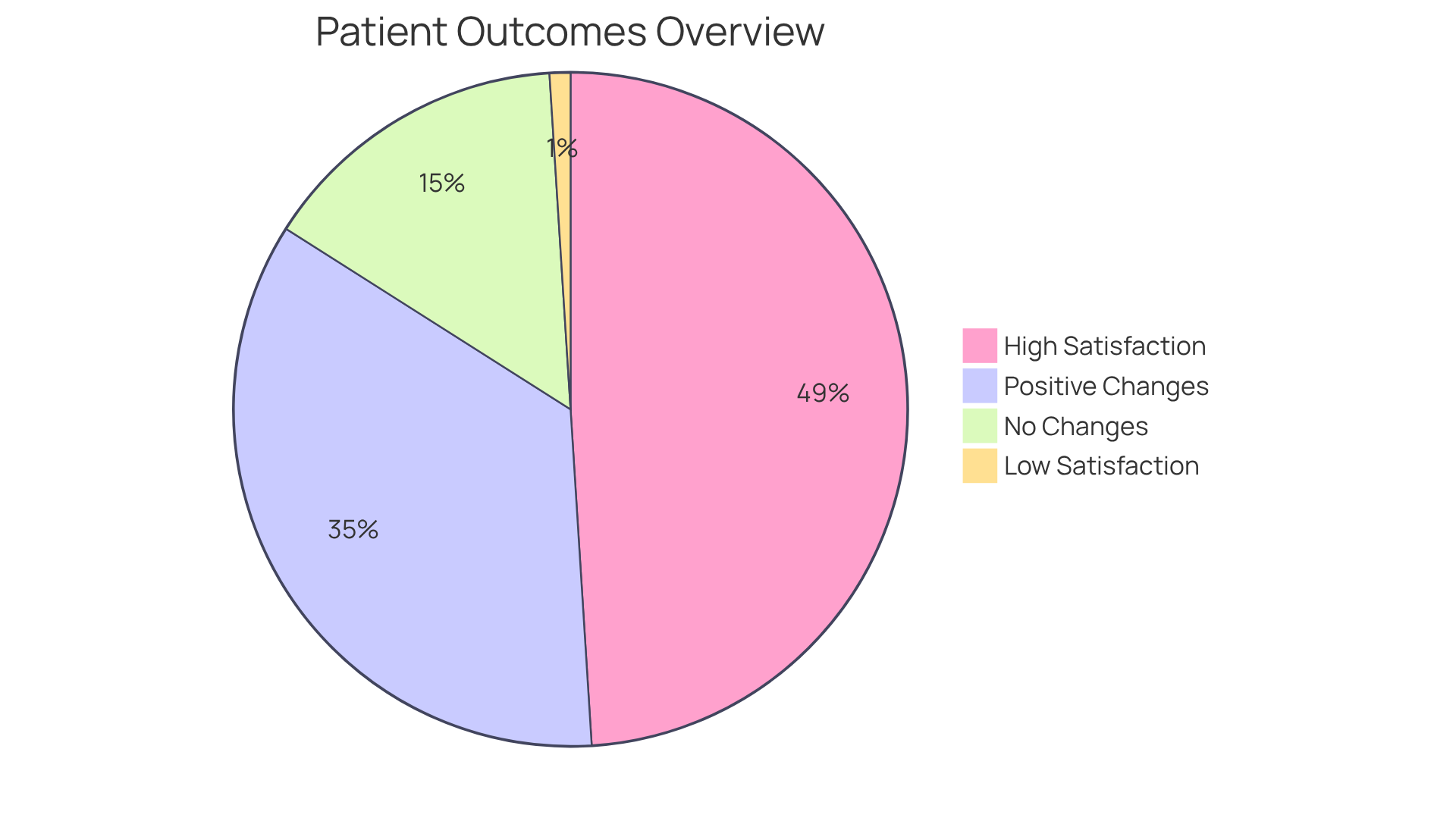
Success stories from older adults who have been treated with DOACs highlight the potential for improved health outcomes. Many individuals have been able to maintain an active lifestyle while minimizing the risks associated with this condition. Remember, you are not alone in this journey—support is available, and you deserve to feel empowered in managing your health.
Manage and Prevent Future DVT Episodes
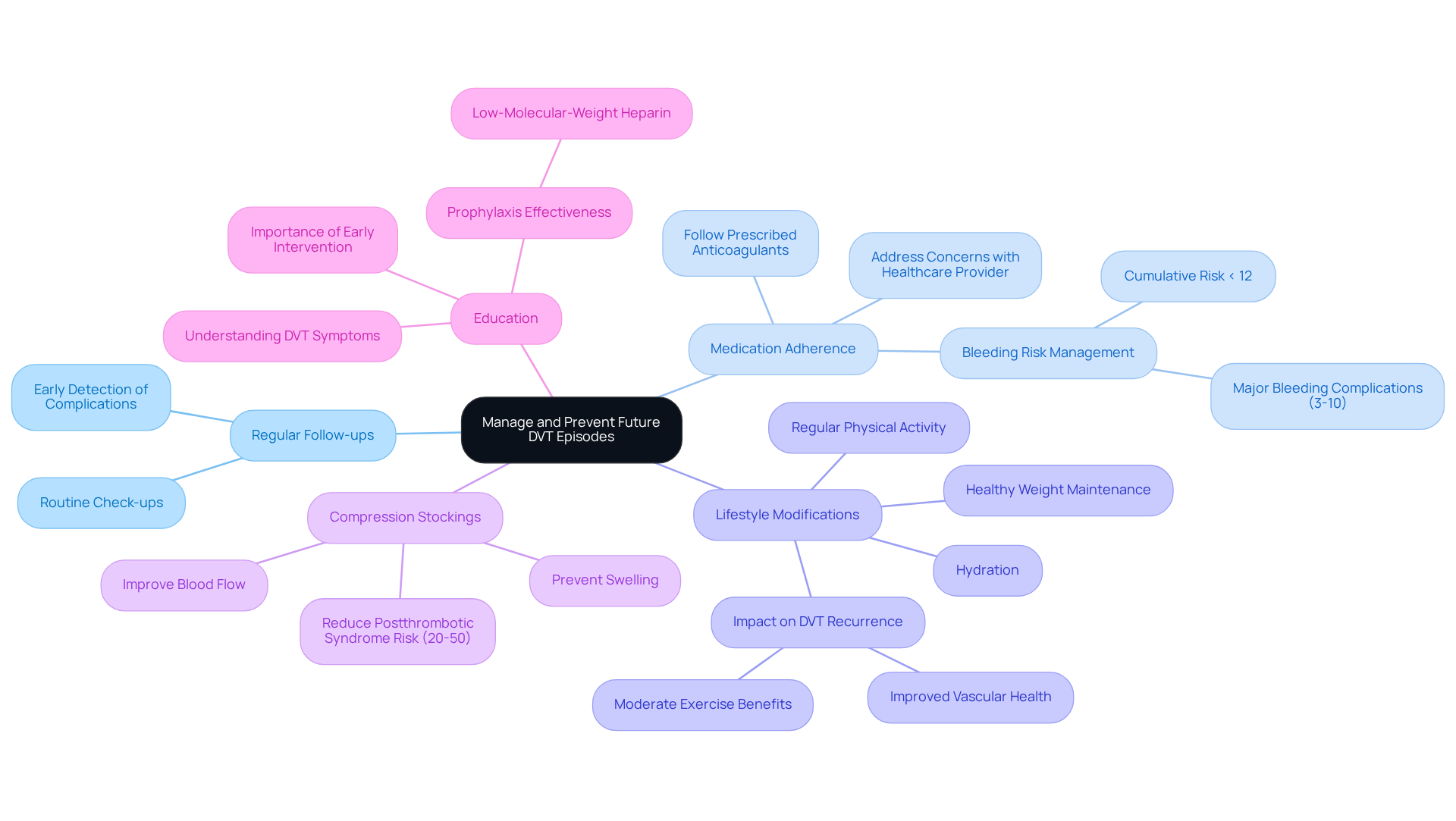
To effectively manage and prevent future episodes of DVT, elderly patients are encouraged to consider the following compassionate strategies:
- Regular check-ups: It’s important to schedule routine check-ups with healthcare providers to monitor health. Consistent follow-up is crucial, as studies show that early detection of complications can significantly improve outcomes. Remember, your health is a priority, and these appointments are a step towards better well-being.
- Medication adherence: Taking prescribed anticoagulants as directed is vital. Following medication plans helps keep the combined likelihood of bleeding issues from anticoagulation therapy under 12%. It’s worth noting that major bleeding complications arise in 3-10% of individuals, which emphasizes the necessity of addressing any concerns with your healthcare provider to ensure optimal management. You are not alone in this; your healthcare team is here to support you.
- Healthy lifestyle: Engaging in regular physical activity, maintaining a healthy weight, and staying hydrated can enhance circulation. Studies indicate that these lifestyle changes can lower the likelihood of DVT recurrence by improving overall health. Even moderate exercise can be beneficial in preventing thrombus formation, as cardiologists emphasize. The American College of Chest Physicians strongly recommends early ambulation as tolerated for individuals with DVT. Taking small steps can lead to significant improvements in your health.
- Compression stockings: Wearing graduated compression stockings may help prevent swelling and improve blood flow in your legs. These stockings are particularly effective in decreasing the likelihood of postthrombotic syndrome, which affects 20-50% of individuals with confirmed DVT. Their significance as a preventive measure cannot be overstated; consider them as a supportive tool in your journey to better health.
- Education: Staying informed about DVT and its contributing factors is essential to recognizing symptoms early and seeking prompt medical attention. Understanding the signs of DVT can lead to quicker interventions, which are critical in treatment. A case study on DVT prevention highlights the effectiveness of early prophylaxis with low-molecular-weight heparin, further supporting the need for awareness and proactive management. Knowledge is empowering, and being informed can make a difference in your health journey.
By implementing these strategies, elderly patients can significantly reduce their risk of recurrent DVT and understand how DVT is treated to enhance their overall health. Remember, you are taking important steps towards a healthier future, and support is always available.
Conclusion
Understanding and managing Deep Vein Thrombosis (DVT) is crucial, especially for elderly patients who face heightened risks and complications from this condition. It’s important to be aware of the potential dangers, and timely diagnosis along with effective treatment strategies can truly make a difference. By educating both patients and caregivers about the symptoms, causes, and available treatments, individuals can take proactive steps towards safeguarding their health.
Key insights discussed include:
- The critical role of early detection through vigilant monitoring of symptoms.
- The effective use of diagnostic tools like the Wells Score can aid in timely identification.
- Treatment options vary, ranging from anticoagulants to lifestyle modifications.
- Regular follow-ups, adherence to medication, and the use of compression stockings are essential strategies that can significantly lower the risk of recurrence and improve overall vascular health.
Ultimately, empowering elderly patients with knowledge and resources is vital for enhancing their quality of life and preventing future DVT episodes. It is essential to engage in open conversations with healthcare providers and stay informed about the latest treatment advancements. By adopting a proactive approach to health management, patients can foster better health outcomes. Taking these steps not only cultivates a sense of control over one’s well-being but also ensures that elderly individuals can lead active, fulfilling lives while minimizing the risks associated with DVT.
Frequently Asked Questions
What is Deep Vein Thrombosis (DVT)?
Deep Vein Thrombosis (DVT) is a serious condition characterized by the formation of a blood clot in a deep vein, most commonly in the legs. It poses significant risks, especially for older patients, as it can lead to complications like pulmonary embolism if the clot dislodges and travels to the lungs.
Who is at higher risk for developing DVT?
Older adults are at higher risk for developing DVT due to factors such as reduced mobility, chronic health conditions, and certain medications that increase susceptibility to clot formation.
What are the potential long-term complications of DVT?
Long-term complications of DVT can include post-thrombotic syndrome, which may cause swelling, pain, and discoloration in the affected limb. There is also a notable risk of recurrence, with approximately 33% of individuals experiencing another DVT event within ten years.
What symptoms should one look for in DVT?
Common symptoms of DVT include swelling in one leg, pain or tenderness, warmth, and changes in skin color. However, about half of those with DVT may not experience any symptoms at all.
What factors contribute to the development of DVT in older adults?
Contributing factors for DVT in older adults include prolonged immobility, recent surgery, certain medical conditions (like cancer or heart disease), genetic factors, obesity, and a history of blood clots.
Why is early recognition of DVT symptoms important?
Early recognition of DVT symptoms is crucial because prompt medical action can prevent severe complications, such as pulmonary embolism and post-thrombotic syndrome, which may lead to long-term health issues.
What should individuals do if they notice signs of DVT?
Individuals who notice signs of DVT should reach out to their doctor promptly to understand how DVT is treated. Seeking help is vital for managing the condition and ensuring proper care.
What resources are available for those concerned about DVT?
There are resources and support available to help individuals and their loved ones understand DVT better and navigate their care. It is important to take action for health and well-being.
List of Sources
- Understand Deep Vein Thrombosis (DVT)
- cdc.gov (https://cdc.gov/blood-clots/data-research/facts-stats)
- uhhospitals.org (https://uhhospitals.org/health-information/health-and-wellness-library/article/diseases-and-conditions/deep-vein-thrombosis)
- ncbi.nlm.nih.gov (https://ncbi.nlm.nih.gov/books/NBK507708)
- Identify Symptoms and Causes of DVT
- cdc.gov (https://cdc.gov/blood-clots/risk-factors/travel.html)
- newsinhealth.nih.gov (https://newsinhealth.nih.gov/2017/01/how-spot-prevent-deep-vein-thrombosis)
- cdc.gov (https://cdc.gov/blood-clots/data-research/facts-stats)
- ncbi.nlm.nih.gov (https://ncbi.nlm.nih.gov/books/NBK507708)
- mayoclinic.org (https://mayoclinic.org/diseases-conditions/deep-vein-thrombosis/symptoms-causes/syc-20352557)
- Diagnose DVT Effectively
- mayoclinic.org (https://mayoclinic.org/diseases-conditions/deep-vein-thrombosis/diagnosis-treatment/drc-20352563)
- emedicine.medscape.com (https://emedicine.medscape.com/article/1911303-treatment)
- Implement Treatment Strategies for DVT
- emedicine.medscape.com (https://emedicine.medscape.com/article/1911303-medication)
- emedicine.medscape.com (https://emedicine.medscape.com/article/1911303-treatment)
- Manage and Prevent Future DVT Episodes
- emedicine.medscape.com (https://emedicine.medscape.com/article/1911303-treatment)
- heart.org (https://heart.org/en/news/2024/06/05/do-you-really-need-compression-socks-on-long-flights)