Introduction
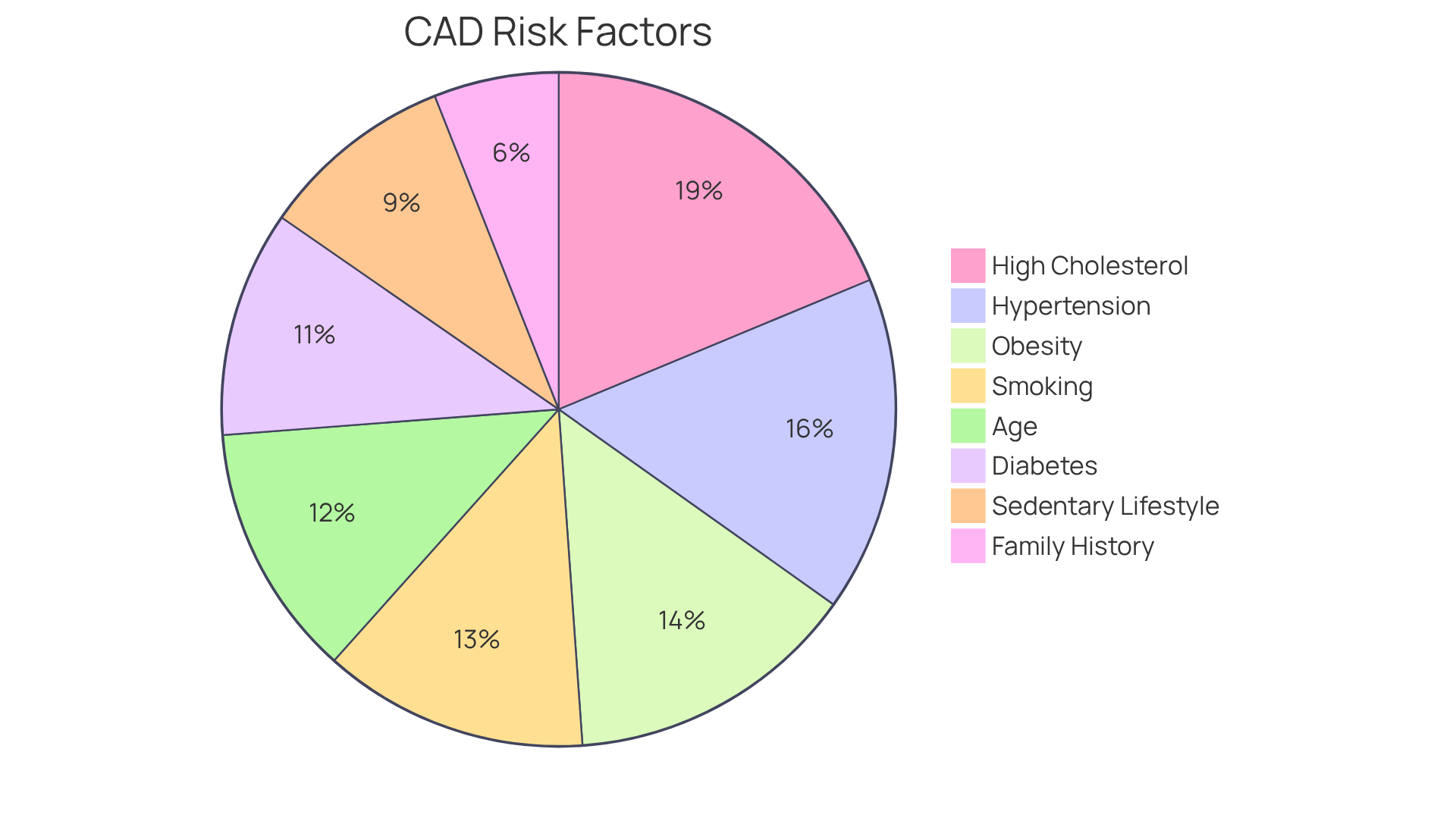
Understanding coronary artery disease (CAD) is essential, especially as heart health becomes a growing concern for many. With various risk factors at play, recognizing and managing them can greatly enhance your cardiovascular well-being. In this article, we’ll explore ten key risk factors for CAD, shedding light on how lifestyle choices, genetics, and demographics come together to influence heart health.
Have you ever wondered what steps you can take to reduce these risks? It’s important to know that you’re not alone in this journey. Many individuals share similar concerns, and there are effective strategies available to help you take charge of your heart health. Together, we can navigate these challenges and work towards a healthier future.
Amavita Heart and Vascular Health: Comprehensive Care for Coronary Artery Disease
At Amavita Heart and Vascular Health, we truly understand the concerns of patients facing the risk factors for coronary artery disease. Our compassionate approach, led by our team, a Harvard-trained cardiologist, ensures that you receive not just treatment, but care that feels personal and nurturing.
We utilize advanced technology and personalized treatment plans designed to optimize your health outcomes. By focusing on your individual needs, we aim to enhance your recovery time and significantly improve your overall well-being. In addition to this, our commitment to excellence allows us to effectively address the unique needs of our diverse Miami community.
But don’t just take our word for it-our patients’ testimonials speak volumes about the positive impact of our innovations on their health journeys. They highlight how our dedicated team has made a difference in their lives, reinforcing our reputation as a leader in cardiovascular care.
If you or a loved one are feeling anxious about your health, remember that you’re not alone. We’re here to support you every step of the way. Reach out to us today, and let’s embark on this journey towards better health together.
High Blood Pressure: A Major Risk Factor for Coronary Artery Disease
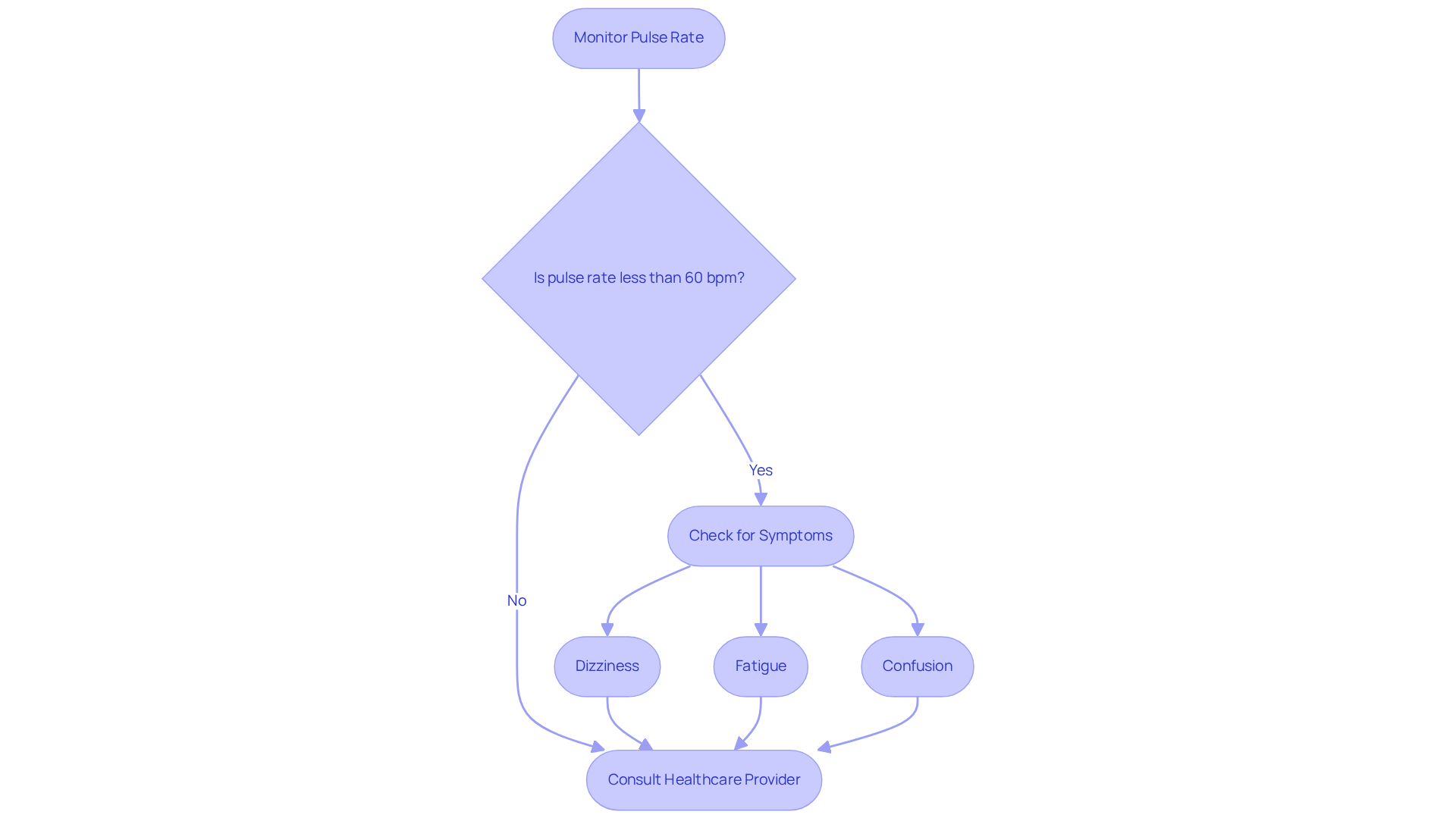
High blood pressure, or hypertension, can be a significant concern for many, as it is one of the key risk factors for coronary artery disease. This condition raises the risk of heart disease, which can be frightening. It’s important to understand that hypertension is one of the leading causes of heart disease as it damages arterial walls, making them more vulnerable to plaque buildup and ultimately leading to heart attacks.
Regular monitoring is essential for reducing these risks. Current guidelines suggest that patients aim to keep their blood pressure below 130/80 mmHg. This goal is crucial not just for halting the progression of CAD but also for improving overall health.
Regular monitoring is key, and lifestyle changes can make a big difference. Consider incorporating the following steps:
- A balanced diet rich in fruits and vegetables
- Engaging in regular physical activity
- Managing your weight
These steps can play a vital role in reducing blood pressure. For some individuals, especially those with stage 2 hypertension, preventive measures may be necessary. Early intervention can be critical in these cases.
By following these guidelines, you can significantly reduce the risk factors for heart disease and improve your long-term cardiovascular well-being. Remember, you’re not alone in this journey; healthcare professionals are here to help, and taking these steps can lead to a healthier, happier life.
High Cholesterol: Understanding Its Impact on Heart Health
Elevated cholesterol, particularly low-density lipoprotein (LDL) cholesterol, can be a significant concern for many, especially when it comes to heart health. When levels rise, plaque can build up in the arteries, narrowing them and restricting blood flow. This can greatly increase the risk of heart attacks and strokes. In fact, heart disease claims a life every 33 seconds. This statistic underscores the importance of addressing high cholesterol with urgency and care.
To manage cholesterol effectively, regular screenings are essential. Current recommendations suggest adopting a diet that includes plenty of fruits, vegetables, whole grains, and healthy fats, while being mindful to limit saturated and trans fats. Nutritionists often recommend incorporating foods rich in omega-3 fatty acids, like fish, and soluble fiber, found in oats and legumes, as these can help lower LDL levels.
In addition to dietary changes, staying active is crucial for managing cholesterol. Engaging in regular exercise can help raise high-density lipoprotein (HDL) cholesterol, often referred to as the ‘good’ cholesterol, while also lowering LDL levels. If lifestyle modifications alone aren’t enough to reach target cholesterol levels, your healthcare provider may discuss options like statins or other medications.
Research shows that reducing LDL cholesterol can significantly affect the risk factors for heart disease. Even slight decreases in LDL can lead to better cardiovascular outcomes, making it vital for those at risk to prioritize cholesterol management. By understanding the role of LDL cholesterol and following current guidelines, you can take meaningful steps toward improving your heart health. Remember, you’re not alone in this journey; support is available, and taking action today can lead to a healthier tomorrow.
Diabetes: Its Role in Increasing Coronary Artery Disease Risk
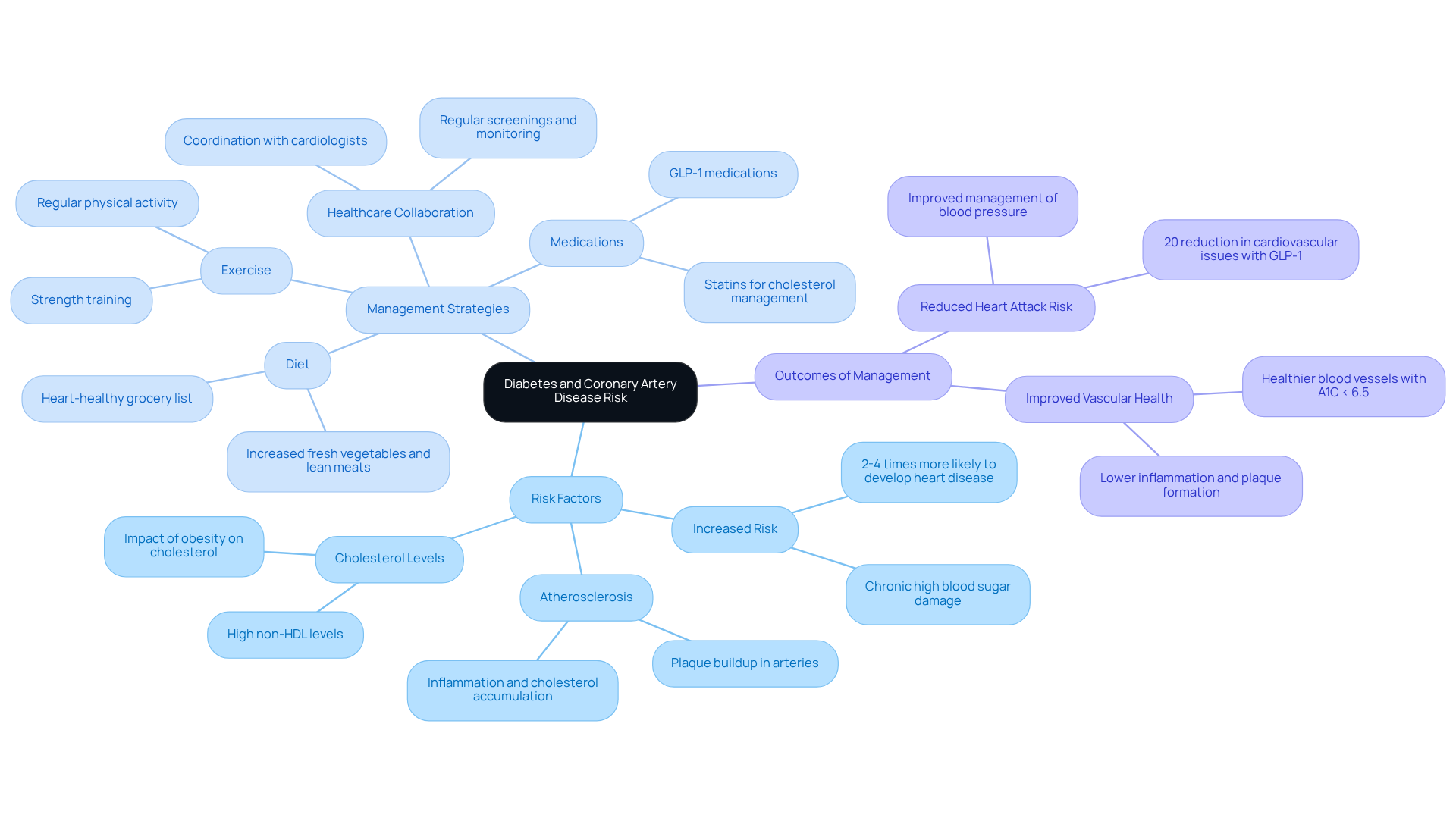
Diabetes can significantly increase the risk of coronary artery disease, primarily due to its damaging effects on blood vessels and cholesterol levels. When blood sugar levels rise, they can harm the arteries, leading to atherosclerosis, a condition where plaque builds up in the arteries and restricts blood flow to vital organs. It’s important to know that individuals with diabetes are two to four times more likely to develop coronary artery disease, highlighting the risk factors for heart disease compared to those without the condition.
To help reduce these risks, it’s essential for patients to collaborate closely with their healthcare providers. Together, they can effectively manage diabetes through a heart-healthy diet, regular exercise, and appropriate medications. Endocrinologists stress that keeping A1C levels below the 6.5% threshold is vital for maintaining health and reducing the risk of complications.
Recent studies have shown that not only does diabetes management lower blood sugar but also significantly reduces the risk of heart attacks and strokes. For instance, participants using GLP-1 medications saw a 20% reduction in cardiovascular issues. Regular check-ups are crucial for monitoring health, allowing for early detection and intervention of potential problems. By prioritizing blood sugar management, individuals with diabetes can greatly enhance their overall well-being and decrease the likelihood of developing risk factors for heart disease.
Are you feeling overwhelmed by these risks? Remember, you’re not alone. With the right support and guidance, you can take meaningful steps towards a healthier heart. Don’t hesitate to reach out to your healthcare team for assistance—they’re here to help you every step of the way.
Obesity: A Contributing Factor to Coronary Artery Disease
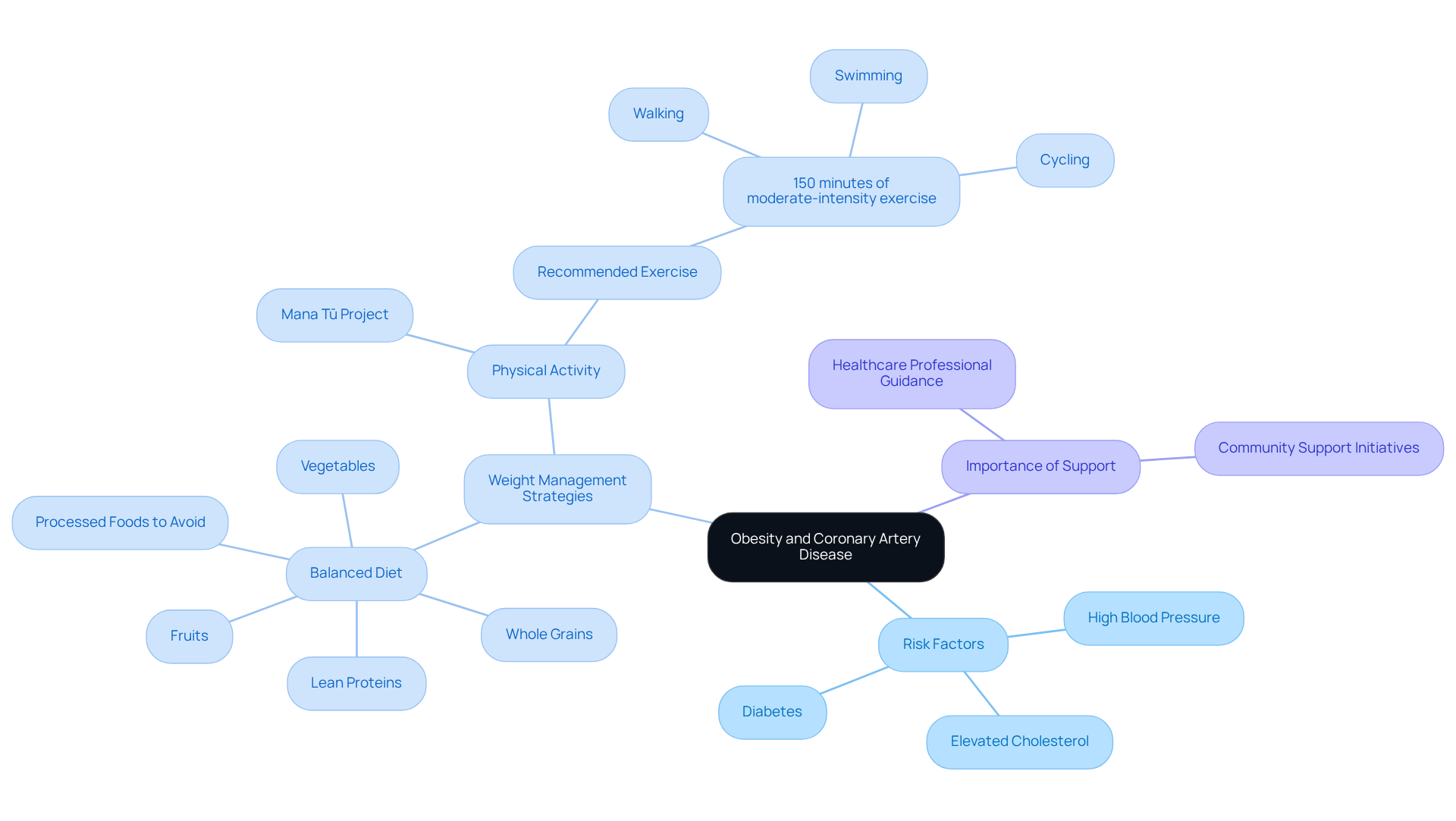
Obesity is a major concern regarding heart health, especially as it relates to the risk factors for coronary artery disease. Excess body weight can lead to hypertension, elevated cholesterol levels, and diabetes, all of which increase the risk of developing coronary artery disease. It’s crucial to maintain a healthy weight to mitigate these risks, and this can be achieved through a balanced diet and regular exercise. For our senior patients, effective strategies are especially important, as they can lead to improved health outcomes.
Have you ever considered how even modest weight loss can significantly impact your health? Research shows that shedding just 5-10% of your body weight can lower blood pressure and improve cholesterol levels, which helps in reducing the risk of heart disease. Dietitians emphasize the importance of meal plans that cater to individual preferences and medical conditions. They recommend focusing on nutrient-dense foods like:
- Fruits
- Vegetables
- Whole grains
- Lean proteins
while cutting back on processed foods that are high in sugars and unhealthy fats.
In addition to this, physical activity is vital. The Mana Tū project, for instance, highlighted a 10% average increase in physical activity among participants, showcasing the power of community-based initiatives in fostering healthier lifestyles. For elderly patients, aiming for at least 150 minutes of moderate-intensity exercise each week-whether it’s walking, swimming, or cycling-can make a world of difference.
Healthcare professionals at Amavita are here to support you on your journey. They can help you set realistic goals, track your progress, and overcome any barriers you might face. By embracing these strategies, you can significantly lower your chances of coronary artery issues and enhance your overall quality of life. With projections suggesting that nearly 2 in 3 adults over 25 could be overweight or obese by 2050, it’s clear that addressing obesity is more urgent than ever. Remember, you’re not alone in this journey; support is available, and together we can work towards a healthier future.
Lack of Physical Activity: A Modifiable Risk Factor for Heart Disease
Living a sedentary lifestyle can really increase the risk of heart disease, and that’s something we should all be aware of. But here’s the good news: regular exercise can help you maintain a healthy weight, reduce stress, and improve your overall health. The American Heart Association suggests aiming for at least 150 minutes of moderate exercise each week.
Have you thought about what activities you enjoy? Finding something you love, like walking, swimming, or cycling, can make it easier to incorporate movement into your daily routine. It’s also wise to check in with your doctor before starting any new exercise program to ensure it’s safe and right for you.
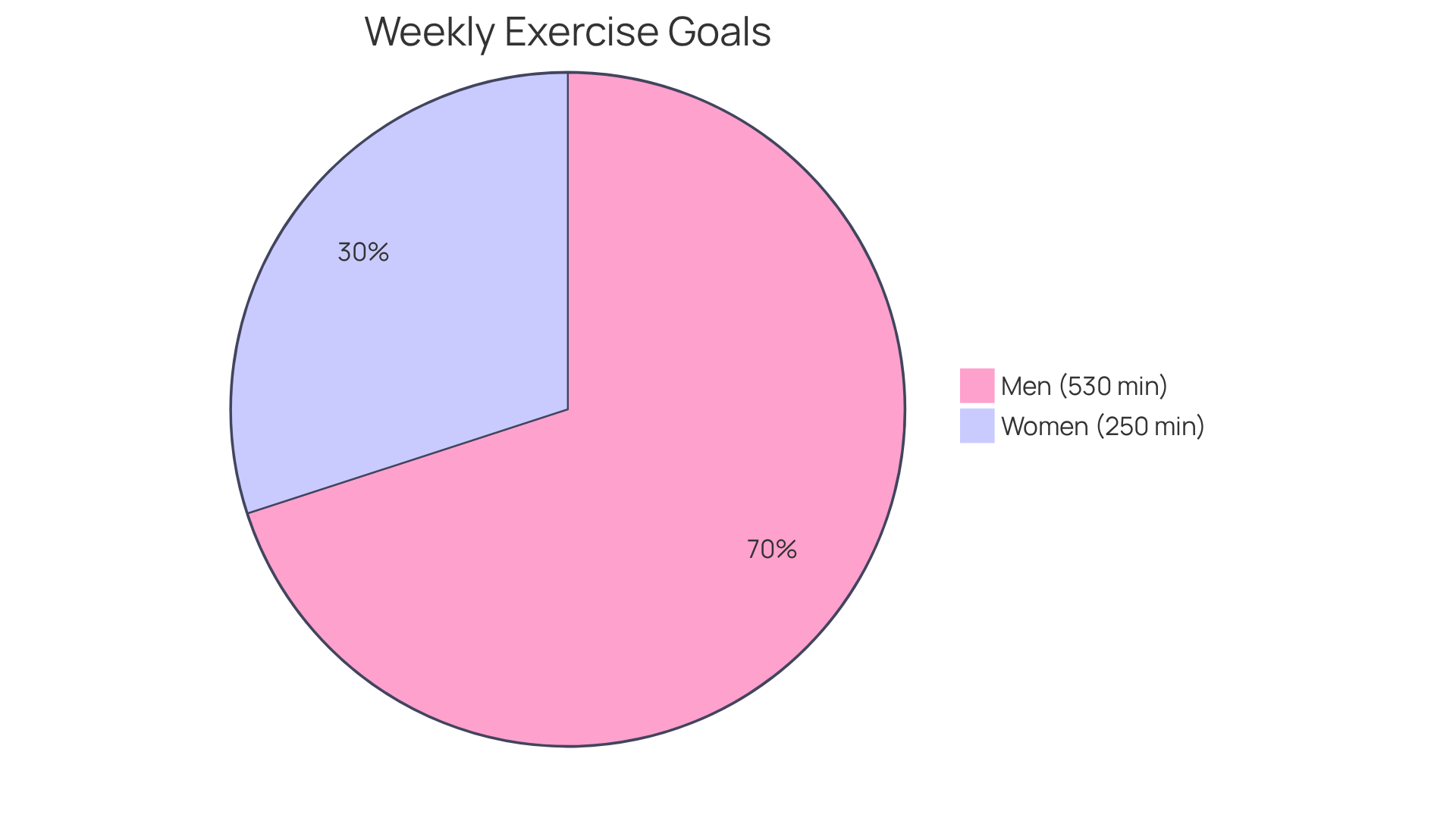
Research indicates that women who engage in about 250 minutes of moderate exercise weekly can reduce their risk of heart disease by around 30%. For men, increasing activity to about 530 minutes can yield similar benefits. Integrating these activities into your everyday life is crucial for heart health, especially for seniors. Remember, you’re not alone in this journey—taking small steps can lead to significant improvements.
Smoking: A Critical Risk Factor for Coronary Artery Disease
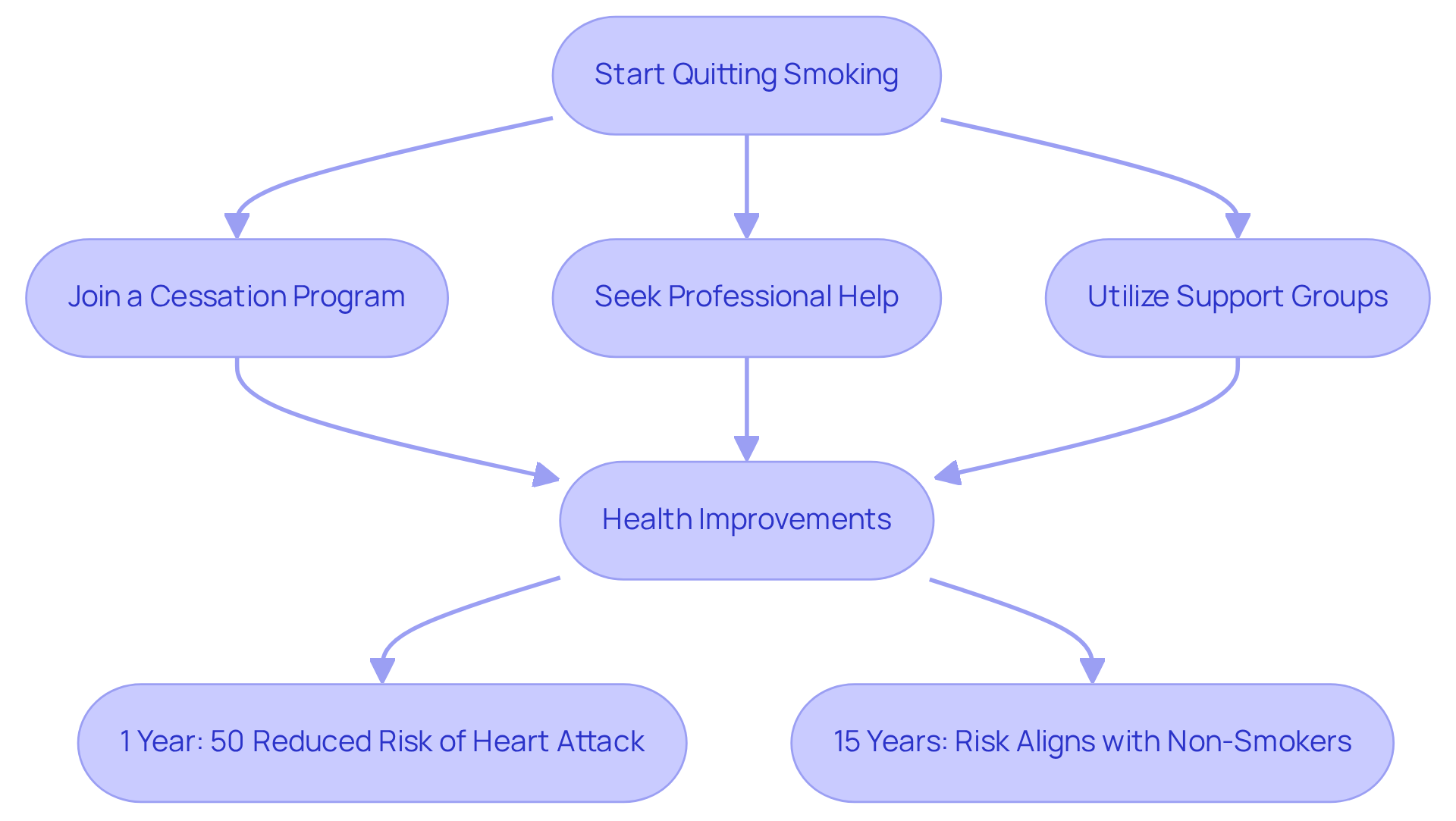
Smoking is one of the significant risk factors for coronary artery disease, harming blood vessels and accelerating plaque buildup. The consequences of smoking can be serious; even a small amount can greatly increase the risk of heart attack. Cardiologists want you to know that the benefits of quitting start right away. In fact, after 15 years, your risk can align with that of someone who has never smoked.
To improve your chances of quitting successfully, consider joining a smoking cessation program. These programs often combine:
All designed to help you on your journey. Recent studies show that pairing behavioral support with medical aids can significantly boost success rates. It’s important to seek help, especially since nearly two-thirds of smokers wish to quit, yet many find they need several attempts before achieving lasting success.
The positive impact of quitting extends beyond immediate health improvements; it significantly reduces the risk factors for coronary artery disease as well as other cardiovascular conditions. By prioritizing smoking cessation, you can take a crucial step toward better heart health and overall well-being. Remember, you’re not alone in this journey, and support is available to help you every step of the way.
Stress: Its Influence on Coronary Artery Disease Risk
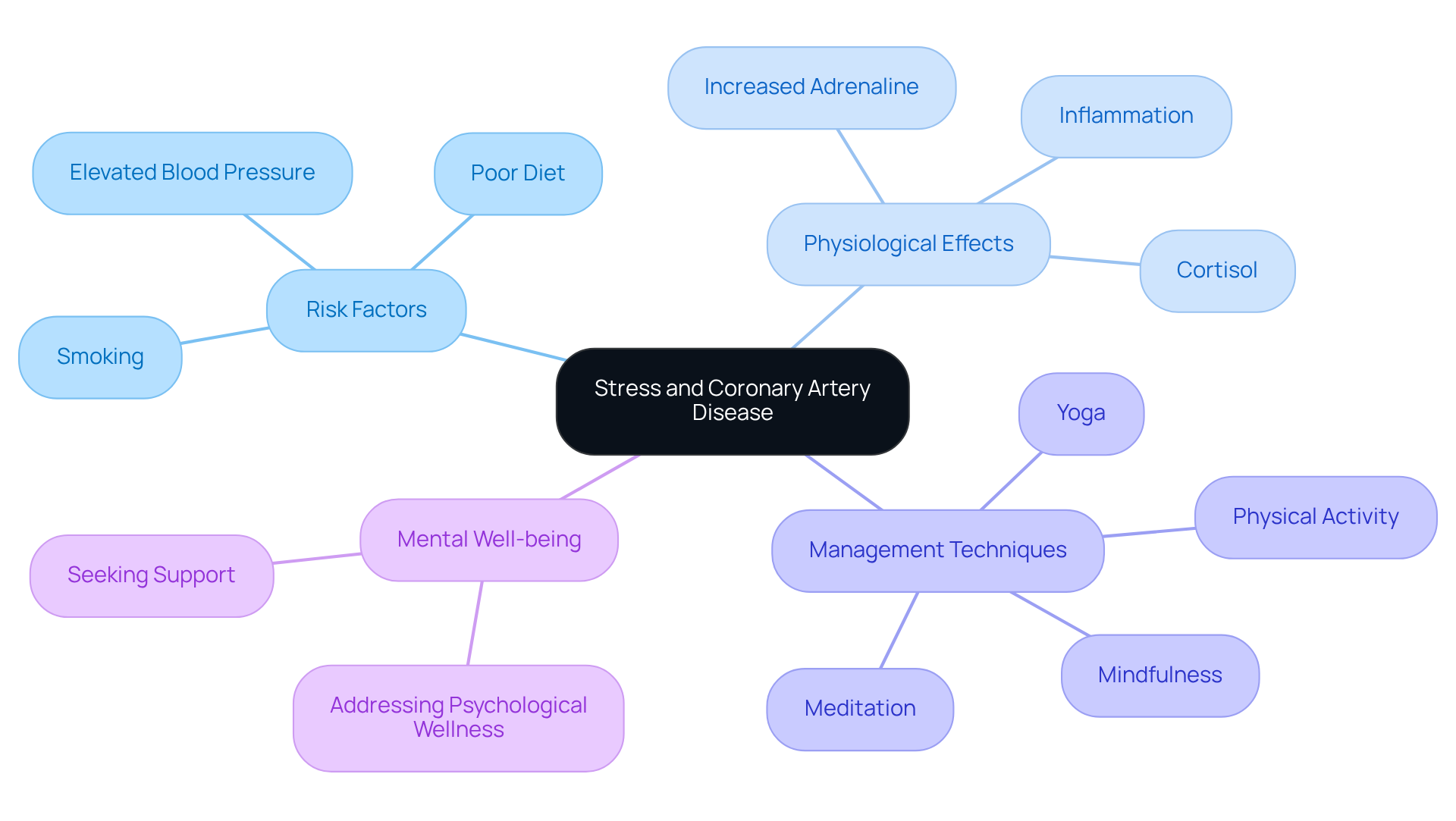
Stress can significantly impact heart health and is among the risk factors for coronary artery disease. It often leads to elevated blood pressure and unhealthy lifestyle choices, like poor diet and smoking. Did you know that individuals experiencing high stress and a history of depression are 2.5 times more likely to face a cardiac event compared to those with lower stress levels? The physiological effects of stress, such as increased heart rate, can disrupt normal heart function and promote inflammation in blood vessels, which are risk factors for coronary artery disease. That’s why effective stress management techniques are so crucial in reducing these risks.
At Amavita Heart and Vascular Health®, we prioritize comprehensive care. Our services, all available in one location, along with sophisticated risk assessment tools, help us identify patients who have risk factors for coronary artery disease due to high stress levels. Our approach combines lifestyle changes with personalized interventions tailored to your unique condition, lifestyle, and goals. Practices like mindfulness, meditation, yoga, and regular physical activity not only help lower stress levels but also boost your overall cardiovascular health. Engaging in mindfulness can significantly reduce the chances of developing risk factors for coronary artery disease by fostering a deeper awareness of your mental state and encouraging healthier coping strategies.
It’s also important to prioritize your mental well-being when facing stress. Seeking support when needed is essential, as addressing mental health is crucial in preventing the negative effects of stress on your heart. As Dr. Rachel Harris points out, focusing on our overall mental health is a key step in avoiding the unwanted physiological impacts of stress on our bodies. Remember to discuss stress during your medical appointments to ensure you receive comprehensive care. Incorporating stress management techniques into your daily routine can greatly enhance your cardiovascular well-being and reduce serious complications related to coronary artery conditions.
Genetics: Understanding Your Risk for Coronary Artery Disease
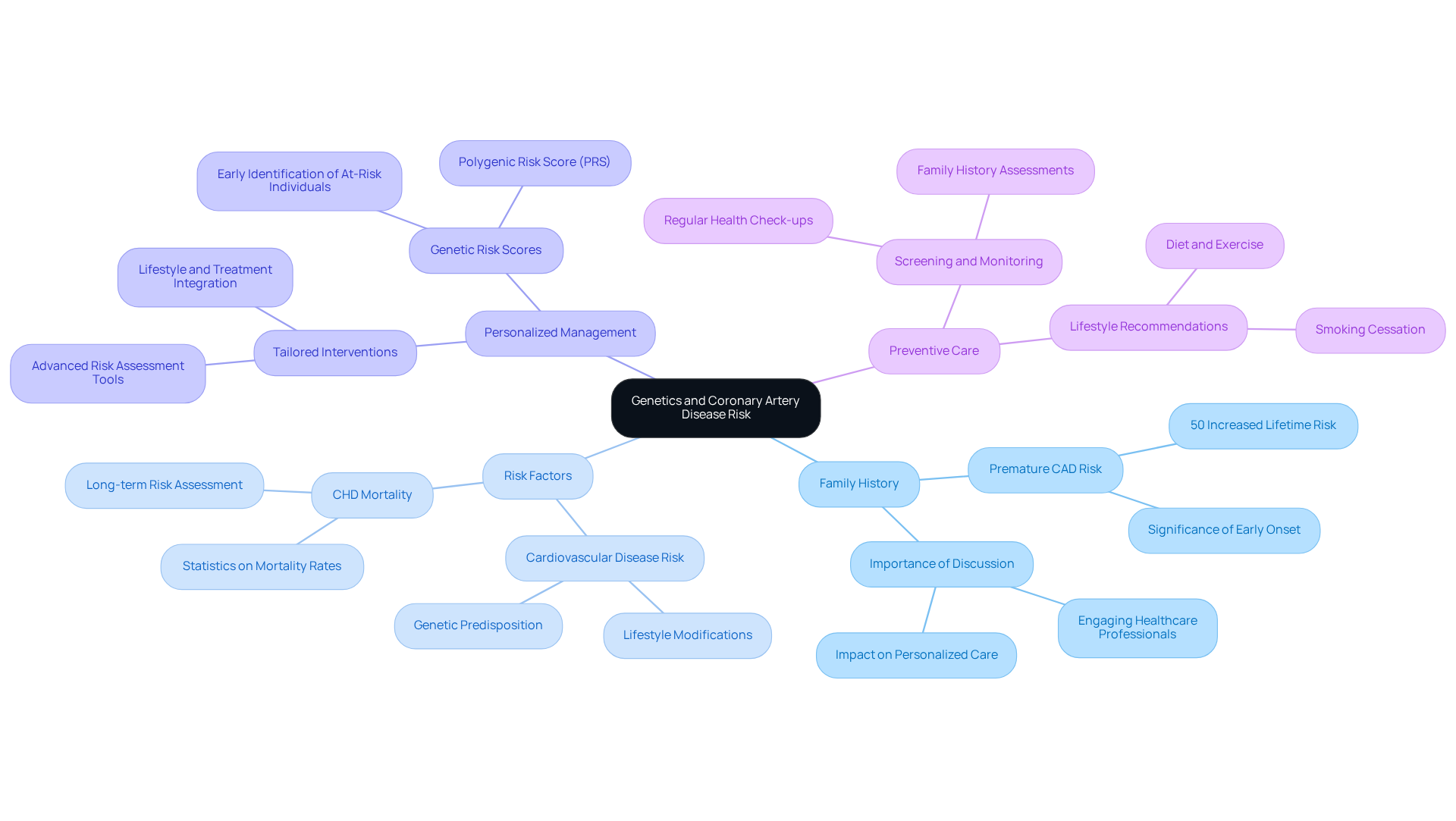
Genetics plays a vital role in understanding your risk for coronary artery disease (CAD). If you have a family history, it’s important to know that this can indicate increased susceptibility. In fact, individuals with a premature family history of CAD face a 50% greater lifetime risk for cardiovascular disease and coronary heart disease (CHD) mortality compared to those without such a background. This is why discussing your family health history with healthcare professionals is so crucial – it can help shape a prevention plan that truly fits your needs.
At Amavita Heart and Vascular Health®, we’re here to support you. Our team uses advanced technology to create tailored interventions that significantly reduce risks. Understanding your family background is essential for effective prevention of cardiovascular issues, as it helps identify potential risks, allowing for timely screenings and lifestyle changes that can make a real difference.
Have you thought about how your family’s medical history might impact your heart health? Engaging in open conversations about this can lead to better outcomes. Our program combines lifestyle modifications with advanced treatments to ensure you receive the best care possible.
Furthermore, our CardioElite™ program exemplifies our commitment to transforming cardiac care. We provide comprehensive management that not only reduces readmissions but also improves outcomes in skilled nursing facilities. Remember, you’re not alone in this journey; we’re here to help you every step of the way.
Age and Ethnicity: Demographic Factors in Coronary Artery Disease Risk
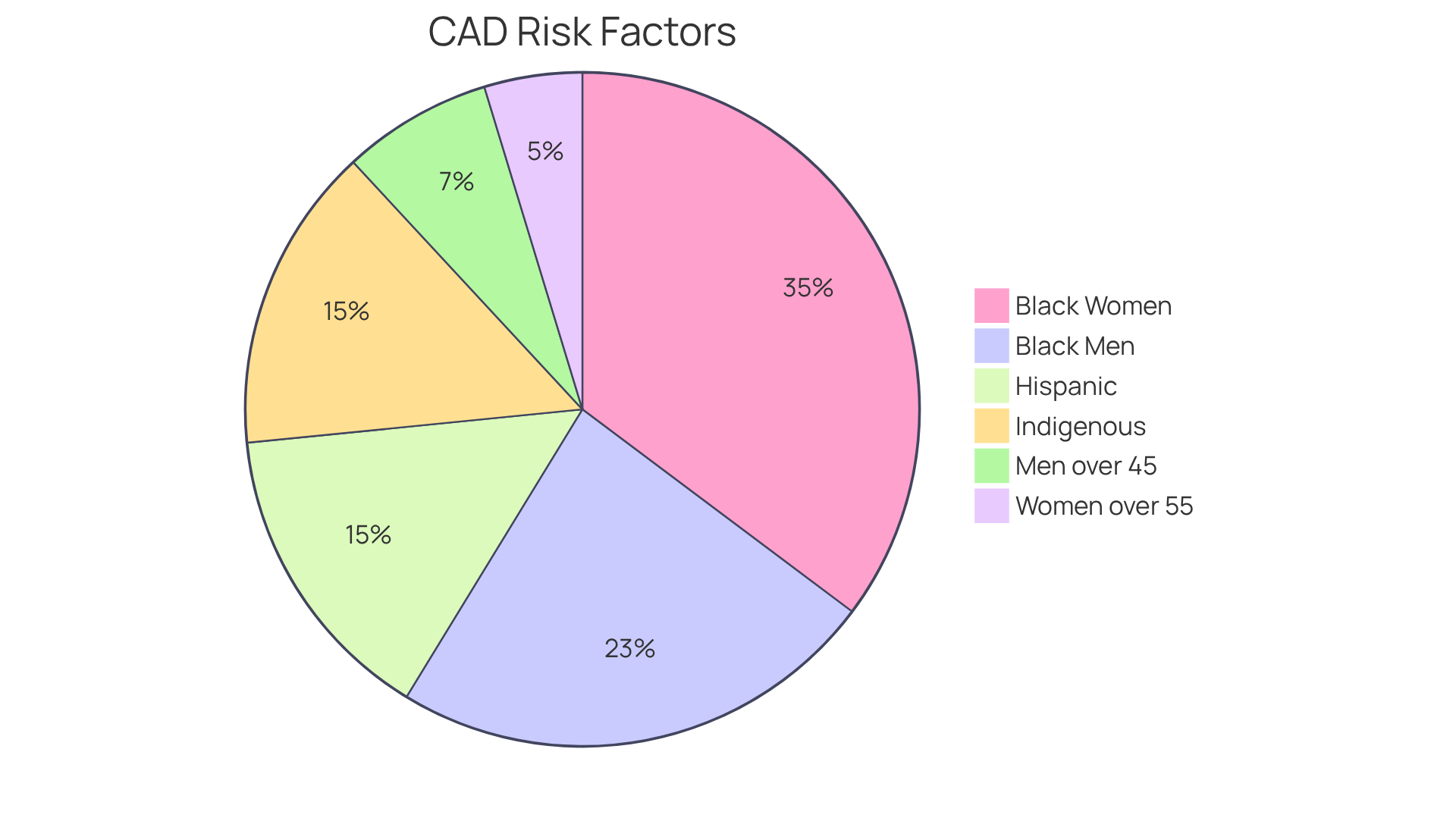
When it comes to heart health, understanding the risk factors involves considering the crucial roles of age and ethnicity. As we age, the likelihood of developing CAD increases, especially for men over 45 and women over 55, who represent significant populations. In fact, after reaching 40 years of age, men face a lifetime chance of 49%, while women have a 32% chance.
Furthermore, certain ethnic groups, such as African Americans, show a higher prevalence of CAD. This is influenced by a mix of genetic factors and lifestyle choices. For example:
- Black men are at a 1.6 times greater risk of cardiovascular conditions compared to white men.
- Black women face a staggering 2.4 times higher risk.
These disparities often stem from socioeconomic and clinical factors that can affect access to care.
It’s essential for healthcare providers to consider these demographic factors. By addressing these disparities, we can improve health outcomes across diverse communities. Remember, understanding your risk is the first step towards taking action. If you have concerns about your heart health, don’t hesitate to reach out for support. You are not alone in this journey.
Conclusion
Understanding the risk factors for coronary artery disease (CAD) is crucial for promoting heart health and preventing serious cardiovascular events. Have you ever wondered what you can do to protect your heart? This article highlights ten key risk factors that everyone should be aware of, emphasizing the importance of proactive management and lifestyle changes to help mitigate these risks.
Let’s explore some critical factors together. High blood pressure, high cholesterol, diabetes, obesity, lack of physical activity, smoking, stress, genetics, and demographic influences like age and ethnicity all play significant roles in increasing the likelihood of developing CAD. Each of these factors can feel overwhelming, but remember, you’re not alone. The article provides actionable insights for managing these risks through lifestyle modifications, regular screenings, and personalized medical care. The message is clear: awareness and proactive measures can significantly improve heart health and reduce the chances of developing coronary artery disease.
Ultimately, taking charge of your heart health means understanding your personal risk factors and seeking support from healthcare professionals. With the right guidance and a commitment to a healthier lifestyle, you can make meaningful strides towards reducing your risk of CAD. Engaging in regular exercise, maintaining a balanced diet, managing stress, and avoiding smoking are just a few steps that can lead to a healthier heart. It’s never too late to start this journey, and the support systems in place, such as those at Amavita Heart and Vascular Health, are ready to assist you every step of the way. Prioritizing your heart health today can pave the way for a healthier tomorrow.
Frequently Asked Questions
What is Amavita Heart and Vascular Health known for?
Amavita Heart and Vascular Health is known for providing comprehensive care for coronary artery disease (CAD) with a compassionate approach, utilizing advanced techniques and personalized treatment plans.
Who leads the care team at Amavita Heart and Vascular Health?
The care team is led by Dr. Pedro Martinez-Clark, a Harvard-trained cardiologist.
How does Amavita Heart and Vascular Health ensure quality care?
They focus on minimally invasive procedures to enhance recovery time and improve overall quality of life, along with culturally sensitive care to meet the diverse needs of the Miami community.
What role do patient testimonials play at Amavita Heart and Vascular Health?
Patient testimonials highlight the positive impact of the care received and reinforce the clinic’s reputation as a leader in cardiovascular care.
Why is high blood pressure a concern for coronary artery disease?
High blood pressure (hypertension) damages arterial walls, making them more vulnerable to plaque buildup, which can lead to heart attacks.
What is the recommended blood pressure goal for reducing the risk of coronary artery disease?
Patients are advised to keep their blood pressure below 130/80 mmHg.
What lifestyle changes can help manage high blood pressure?
Incorporating a balanced diet rich in fruits and vegetables, engaging in regular physical activity, and managing weight can help control hypertension.
What is the impact of high cholesterol on heart health?
Elevated low-density lipoprotein (LDL) cholesterol can lead to plaque buildup in arteries, increasing the risk of heart attacks and strokes.
How can individuals manage their cholesterol levels effectively?
Regular screenings, adopting a heart-healthy diet, engaging in regular exercise, and possibly using medications like statins can help manage cholesterol levels.
What dietary changes are recommended to lower LDL cholesterol?
A diet rich in fruits, vegetables, whole grains, healthy fats, and omega-3 fatty acids, while limiting saturated and trans fats, is recommended.
How does physical activity affect cholesterol levels?
Regular exercise can help raise high-density lipoprotein (HDL) cholesterol, which is beneficial, while lowering LDL cholesterol levels.
What should individuals do if lifestyle changes are not enough to manage cholesterol?
They should consult their healthcare provider for additional options, which may include cholesterol-lowering medications.
List of Sources
- Amavita Heart and Vascular Health: Comprehensive Care for Coronary Artery Disease
- beckersasc.com (https://beckersasc.com/cardiology/amavita-heart-and-vascular-health-opens-multimillion-dollar-asc)
- Enhanced Recovery and Reduced Complications with Minimally Invasive Coronary Artery Bypass Grafting Compared to Open Sternotomy – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC12212263)
- Miami Heart Study Advances Preventive Cardiology as Coronary Plaque Detected in Nearly Half of Asymptomatic Participants | Baptist Health South Florida (https://baptisthealth.net/baptist-health-news/miamiheartstudyadvancespreventivecardiologyascoronaryplaquedetectedinnearlyhalfofasymptomaticpartici)
- Coronary Atherosclerosis Across the Glycemic Spectrum Among Asymptomatic Adults: The Miami Heart Study at Baptist Health South Florida – PubMed (https://pubmed.ncbi.nlm.nih.gov/37772409)
- sciencedirect.com (https://sciencedirect.com/science/article/pii/S0022522321003433)
- High Blood Pressure: A Major Risk Factor for Coronary Artery Disease
- atmantan.com (https://atmantan.com/case_studies/high-blood-pressure-along-with-ibs-are-signs-of-ongoing-inflammation-in-the-body)
- Inspirational Cardiovascular Disease Quotes to Motivate (https://acibademhealthpoint.com/inspirational-cardiovascular-disease-quotes-to-motivate)
- New high blood pressure guideline emphasizes prevention, early treatment to reduce CVD risk (https://newsroom.heart.org/news/new-high-blood-pressure-guideline-emphasizes-prevention-early-treatment-to-reduce-cvd-risk)
- 2025 High Blood Pressure Guideline: Updated Hypertension Recommendations (https://international.heart.org/en/news-and-events/2025/august-high-blood-pressure)
- heart.org (https://heart.org/en/health-topics/high-blood-pressure/the-facts-about-high-blood-pressure/high-bp-top-10)
- High Cholesterol: Understanding Its Impact on Heart Health
- Most people with a genetic condition that causes significantly high cholesterol go undiagnosed, Mayo Clinic study finds – Mayo Clinic News Network (https://newsnetwork.mayoclinic.org/discussion/most-people-with-a-genetic-condition-that-causes-significantly-high-cholesterol-go-undiagnosed-mayo-clinic-study-finds)
- NIH research reveals new insights about how ‘bad’ cholesterol works in the body (https://nih.gov/news-events/news-releases/nih-research-reveals-new-insights-about-how-bad-cholesterol-works-body)
- publichealth.jhu.edu (https://publichealth.jhu.edu/2025/tens-of-thousands-of-heart-attacks-and-strokes-could-be-avoided-each-year-if-cholesterol-lowering-drugs-were-used-according-to-guidelines)
- New Drug Lowers ‘Bad’ Cholesterol by 58% in Clinical Trial (https://sciencealert.com/new-drug-lowers-bad-cholesterol-by-58-in-clinical-trial)
- Diabetes: Its Role in Increasing Coronary Artery Disease Risk
- New discovery could lower heart attack and stroke risk for people with type 2 diabetes (https://sydney.edu.au/news-opinion/news/2025/08/16/new-discovery-could-lower-heart-attack-and-stroke-risk-for-peopl.html)
- Cardiovascular risk factors in diabetic patients with and without metabolic syndrome: a study based on the Rafsanjan cohort study – Scientific Reports (https://nature.com/articles/s41598-022-27208-5)
- Managing Diabetes and Coronary Artery Disease | Mass General Brigham (https://massgeneralbrigham.org/en/about/newsroom/articles/diabetes-coronary-artery-disease)
- National Diabetes Statistics Report (https://cdc.gov/diabetes/php/data-research)
- Do you have diabetes? Here’s why you should see a cardiologist (https://nortonhealthcare.com/news/diabetes-heart-disease-why-you-need-a-cardiologist)
- Obesity: A Contributing Factor to Coronary Artery Disease
- Products – Data Briefs – Number 508 – September 2024 (https://cdc.gov/nchs/products/databriefs/db508.htm)
- New World Heart Report underscores urgent need to address obesity to reduce Cardiovascular Disease | World Obesity Federation (https://worldobesity.org/news/new-world-heart-report-underscores-urgent-need-to-address-obesity-to-reduce-cardiovascular-disease)
- Heart Health Risk Factors Continue To Increase (https://usnews.com/news/health-news/articles/2025-01-28/heart-health-risk-factors-continue-to-increase)
- Bias and inadequate treatment threaten heart health for millions facing obesity and CVD risk, warns World Heart Federation (https://world-heart-federation.org/news/bias-and-inadequate-treatment-threaten-heart-health-for-millions-facing-obesity-and-cvd-risk-warns-world-heart-federation)
- Alarming Rise in Cardiovascular Deaths for Those With Obesity Disproportionately Impacting Minorities and Women | SCAI (https://scai.org/media-center/news-and-articles/alarming-rise-cardiovascular-deaths-those-obesity-disproportionately)
- Lack of Physical Activity: A Modifiable Risk Factor for Heart Disease
- mcknights.com (https://mcknights.com/news/exercise-supports-healthy-aging-and-more-older-adults-need-to-get-moving-report-says)
- For heart health, physical activity favors women (https://statnews.com/2025/10/27/cardiac-health-study-exercise-provides-greater-benefit-women)
- abcnews.go.com (https://abcnews.go.com/Health/women-reach-heart-health-goals-exercise-men-new/story?id=126897192)
- Benefits of Physical Activity (https://cdc.gov/physical-activity-basics/benefits)
- Smoking: A Critical Risk Factor for Coronary Artery Disease
- By 2030, 40% Increase in Tobacco-Related Coronary Heart Disease Deaths Anticipated | SCAI (https://scai.org/media-center/news-and-articles/2030-40-increase-tobacco-related-coronary-heart-disease-deaths)
- Cardiovascular Disease: Even Occasional Smoking Linked to Higher Risk (https://healthline.com/health-news/occasional-smoking-increases-cardiovascular-disease-risk)
- betterhealth.vic.gov.au (https://betterhealth.vic.gov.au/health/healthyliving/smoking-and-heart-disease)
- Cardiologist says smoking for years does not mean quitting won’t help: 1 year after quitting heart attack risk drops 50% (https://hindustantimes.com/lifestyle/health/cardiologist-says-smoking-for-years-does-not-mean-quitting-won-t-help-1-year-quitting-heart-attack-drops-50-percent-101756866492905.html)
- Smoking just two cigarettes a day can wreak havoc on your heart, study shows (https://foxnews.com/health/smoking-just-two-cigarettes-day-can-wreak-havoc-your-heart-study-shows)
- Stress: Its Influence on Coronary Artery Disease Risk
- Yes, Stress Can Hurt Your Heart: 3 Things to Know (https://yalemedicine.org/news/stress-affects-your-heart)
- thecardiologyadvisor.com (https://thecardiologyadvisor.com/features/impact-of-psychological-stress-on-cardiovascular-disease-cvd-risk)
- Effect of stress on heart conditions: guide to early detection (https://mayoclinichealthcare.co.uk/news/effects-of-stress-on-heart)
- adventhealth.com (https://adventhealth.com/news/chronic-stress-and-its-affect-heart-health)
- Stress, Mental Health and Your Heart (https://bch.org/latest-news/2025/february/stress-mental-health-and-your-heart)
- Genetics: Understanding Your Risk for Coronary Artery Disease
- newsnetwork.mayoclinic.org (https://newsnetwork.mayoclinic.org/discussion/expert-explains-how-to-improve-heart-health-even-if-your-family-has-history-of-heart-conditions)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC3631594)
- Genetic risk and its role in primary prevention of CAD (https://oaepublish.com/articles/jtgg.2022.07)
- Genetics, its role in preventing the pandemic of coronary artery disease – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC8207986)
- How Genetics Influence Heart Disease | CardioVascular Health Clinic (https://cvhealthclinic.com/news/how-genetics-influence-heart-disease)
- Age and Ethnicity: Demographic Factors in Coronary Artery Disease Risk
- Black adults’ high cardiovascular disease risk not due to race itself (https://news.northwestern.edu/stories/2022/05/black-adults-high-cardiovascular-disease-risk-not-due-to-race-itself)
- Risk Factors for Coronary Artery Disease – StatPearls – NCBI Bookshelf (https://ncbi.nlm.nih.gov/books/NBK554410)
- CVD data gap disproportionately impacts minority races and ethnicities worldwide (https://nutritioninsight.com/news/cvd-heart-health-data-gap-race-ethnicity.html)
- Heart Disease and Black/African Americans (https://minorityhealth.hhs.gov/heart-disease-and-blackafrican-americans)
- Racial and Ethnic Disparities in Heart and Cerebrovascular Disease Deaths During the COVID-19 Pandemic in the United States – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC8191372)