Introduction
Moderate chronic microvascular ischemic changes are a significant yet often overlooked condition that affects the small blood vessels in the brain. This can lead to reduced blood flow and potential cognitive decline, which can be concerning, especially for older adults. As this condition becomes more common, it’s essential to understand its symptoms, diagnostic methods, and treatment options. Recognizing these aspects can empower individuals and caregivers to manage their health proactively.
How can you or your loved ones spot the early signs of this condition? What steps can be taken to lessen its impact on daily life? These questions are vital as they open the door to better health outcomes and an improved quality of life for those affected. By exploring these topics together, we can find ways to support each other and navigate this journey with compassion and understanding.
Define Moderate Chronic Microvascular Ischemic Changes
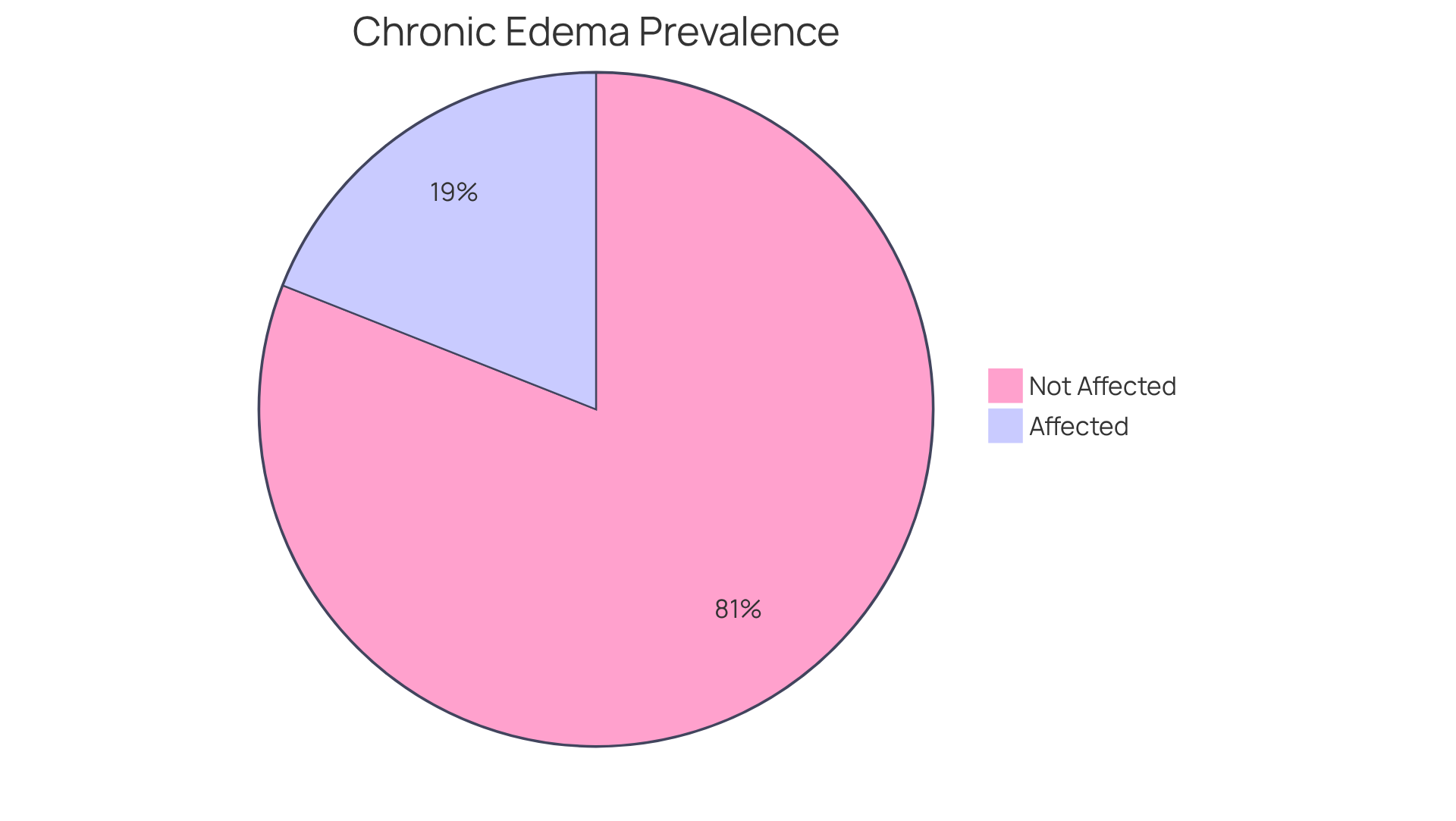
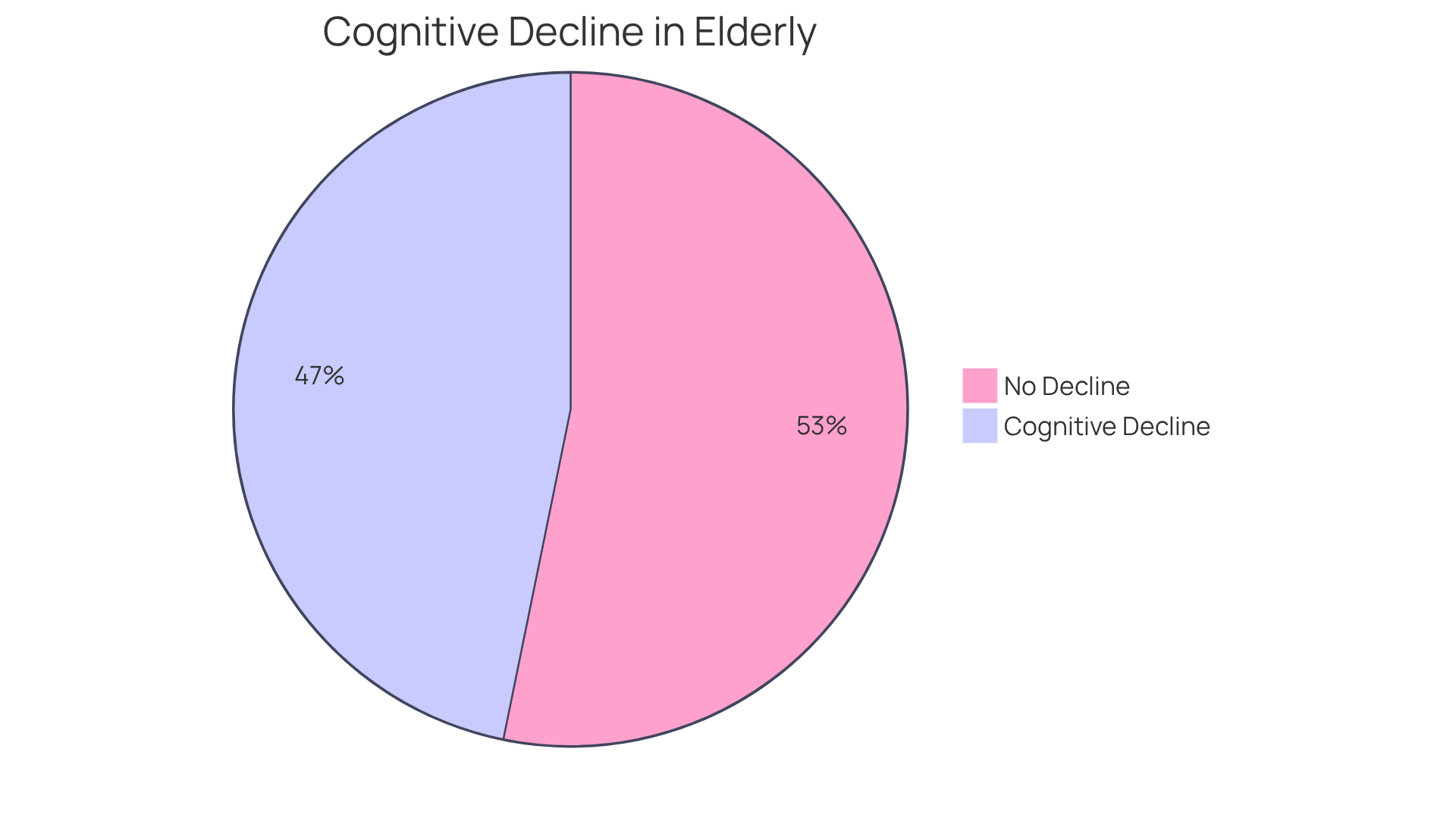
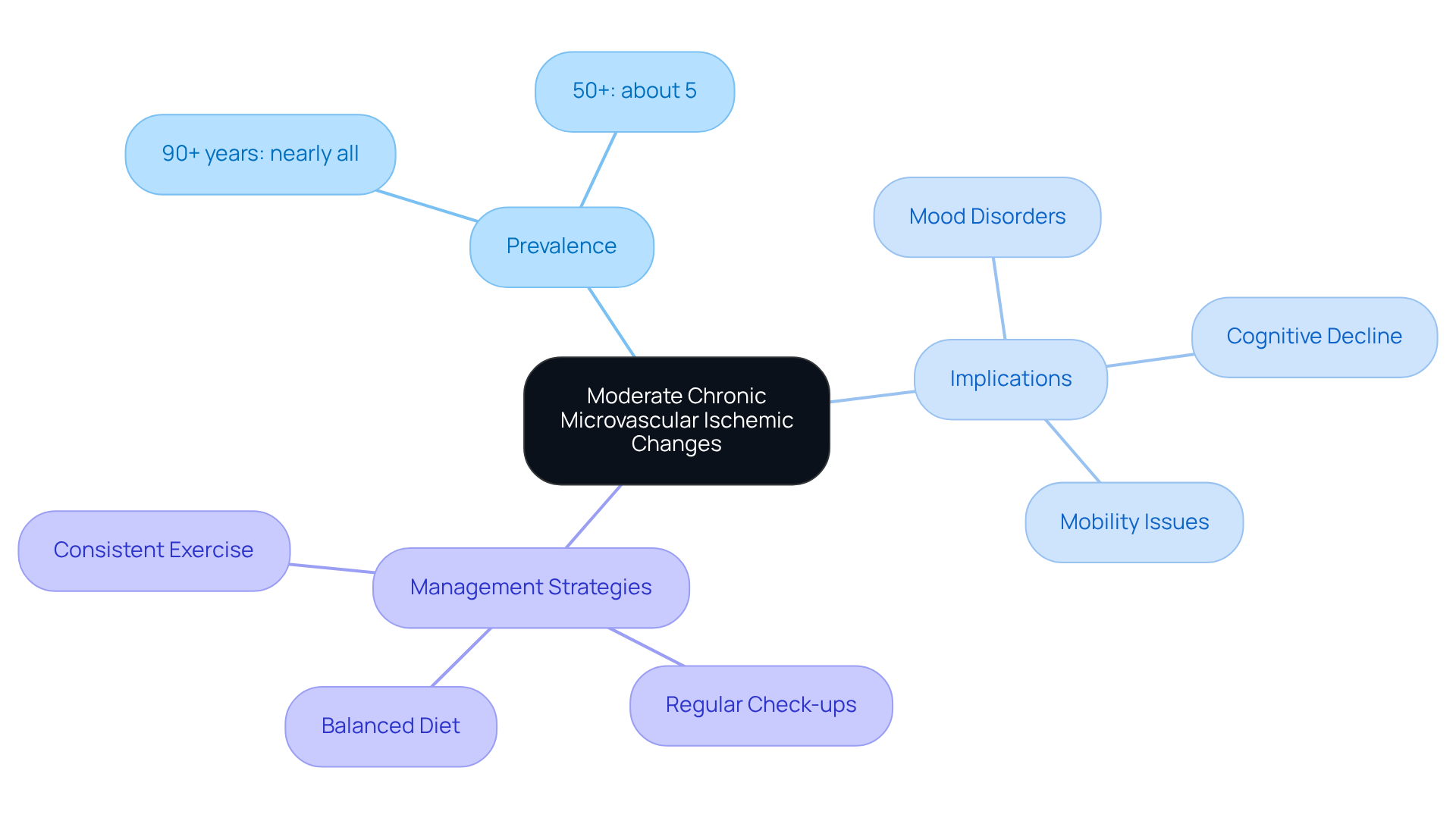
Moderate chronic microvascular ischemic changes refer to alterations in the small blood vessels of the brain that can lead to decreased blood flow and potential harm to brain tissue. You might notice these alterations marked by white matter hyperintensities (WMH) on MRI scans, which indicate areas of ischemia or insufficient blood supply. This condition is particularly prevalent among older adults, with nearly all individuals over the age of 90 showing signs of chronic small blood vessel alterations, while it affects only about 5% of those aged 50 and above. Such changes can significantly contribute to cognitive decline, mood disorders, and mobility issues, highlighting the importance of early detection and proactive management.
Have you or a loved one experienced any changes in memory or mobility? Studies suggest that moderate chronic microvascular ischemic changes are linked to a higher likelihood of dementia and strokes, with these changes accounting for around 25% of all obstructive strokes. The presence of WMH serves as a crucial indicator of moderate chronic microvascular ischemic changes, which correlate with cognitive impairments and functional decline. For example, an 85-year-old female patient with a total FLAIR WMH burden of 71.8mL presented with memory loss and gait disturbances, illustrating the real-world implications of this condition.
Recent research emphasizes the need for lifestyle modifications, such as regular health check-ups, a balanced diet, and consistent exercise, to help reduce the risks associated with moderate chronic microvascular ischemic changes. These strategies are vital for improving circulation and overall brain health, ultimately enhancing the quality of life for elderly patients. Understanding the impact of these changes is essential for developing effective management strategies that can lead to better patient outcomes.
Remember, you’re not alone in this journey. Seeking support and making small changes can make a significant difference in your health and well-being.
Identify Symptoms of Moderate Chronic Microvascular Ischemic Changes
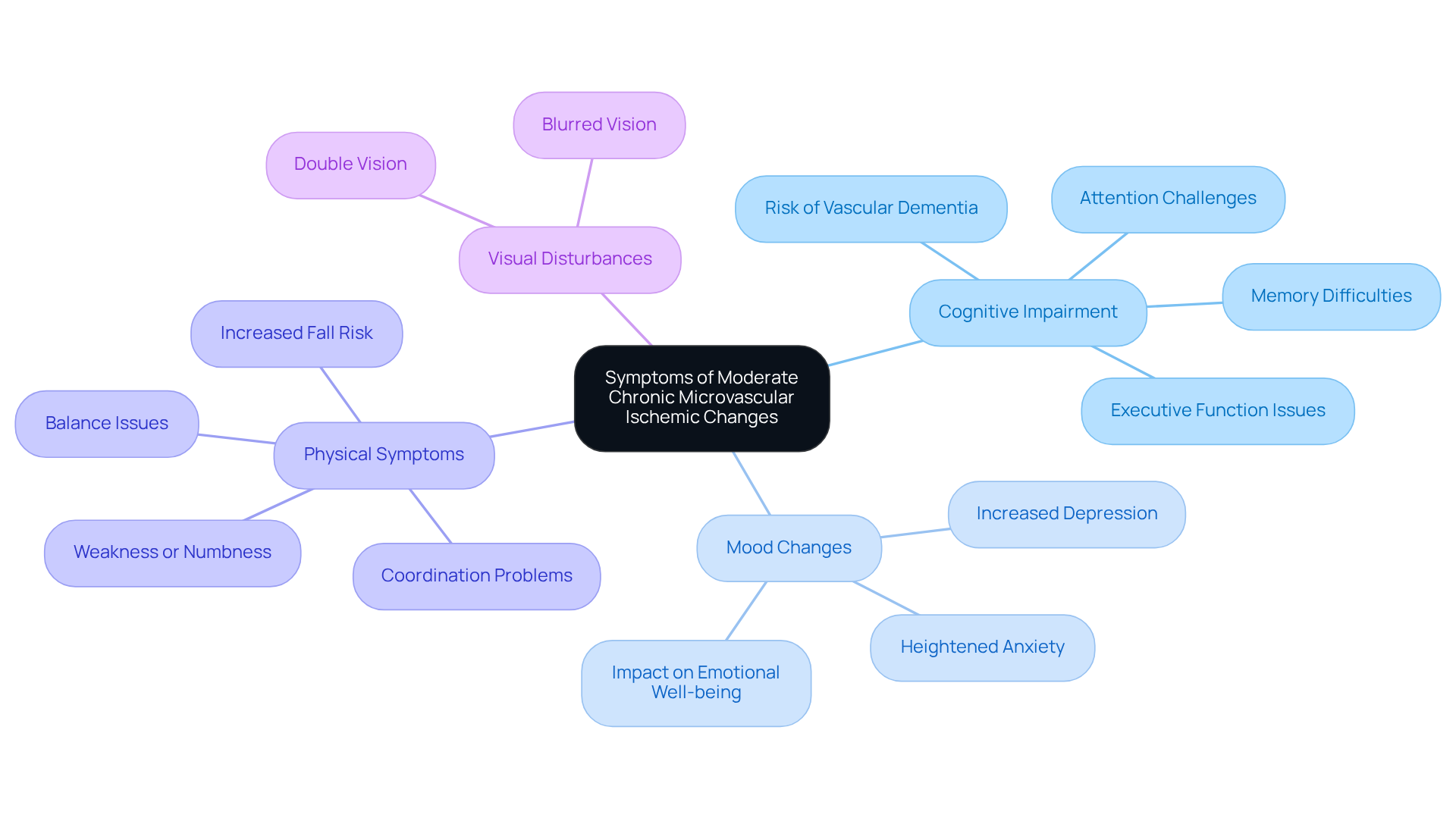
Symptoms of moderate chronic microvascular ischemic changes can manifest in various ways, significantly impacting daily life. It’s important to recognize these signs early, as they can lead to more serious health concerns. Here are some key symptoms to be aware of:
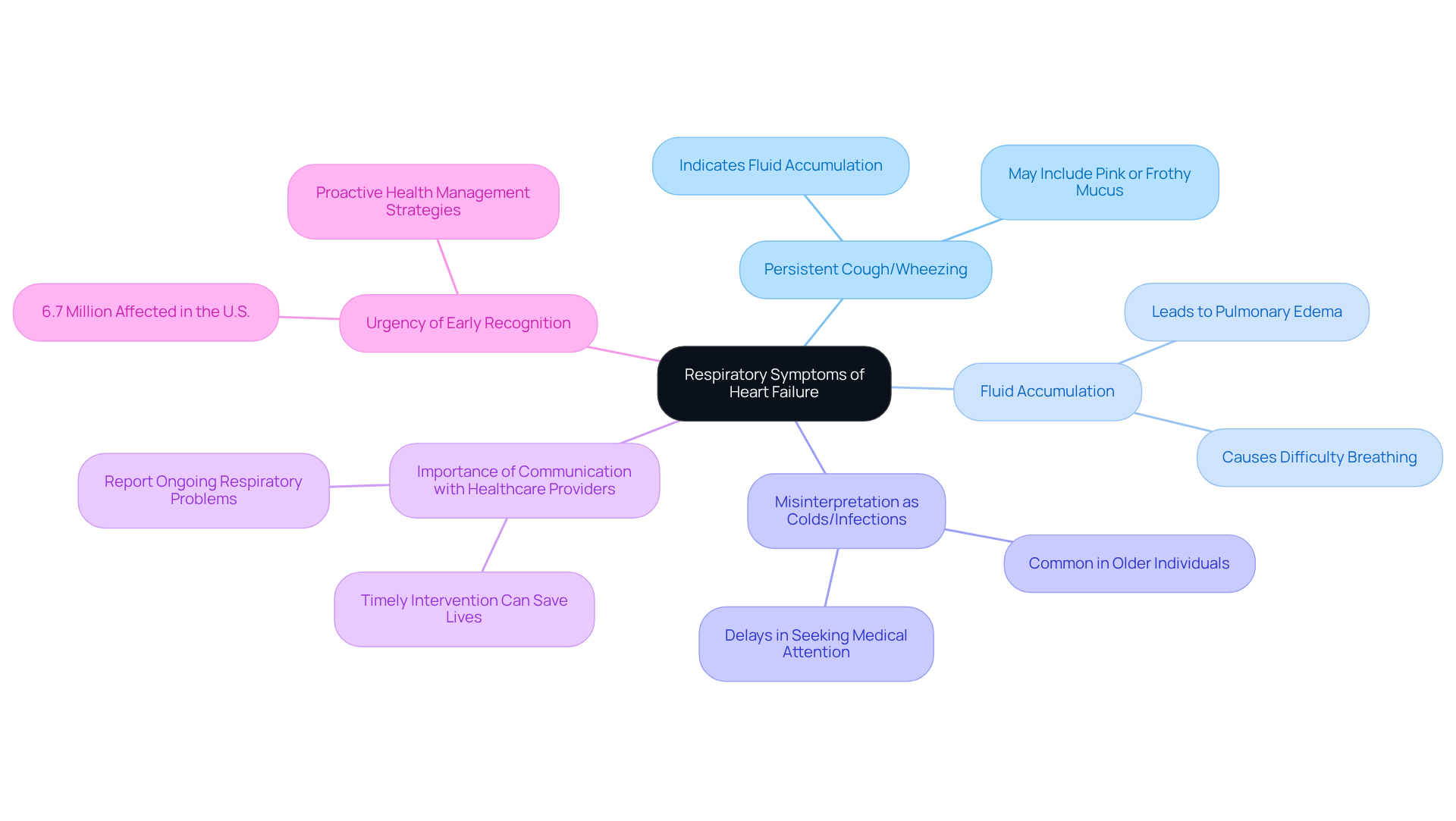
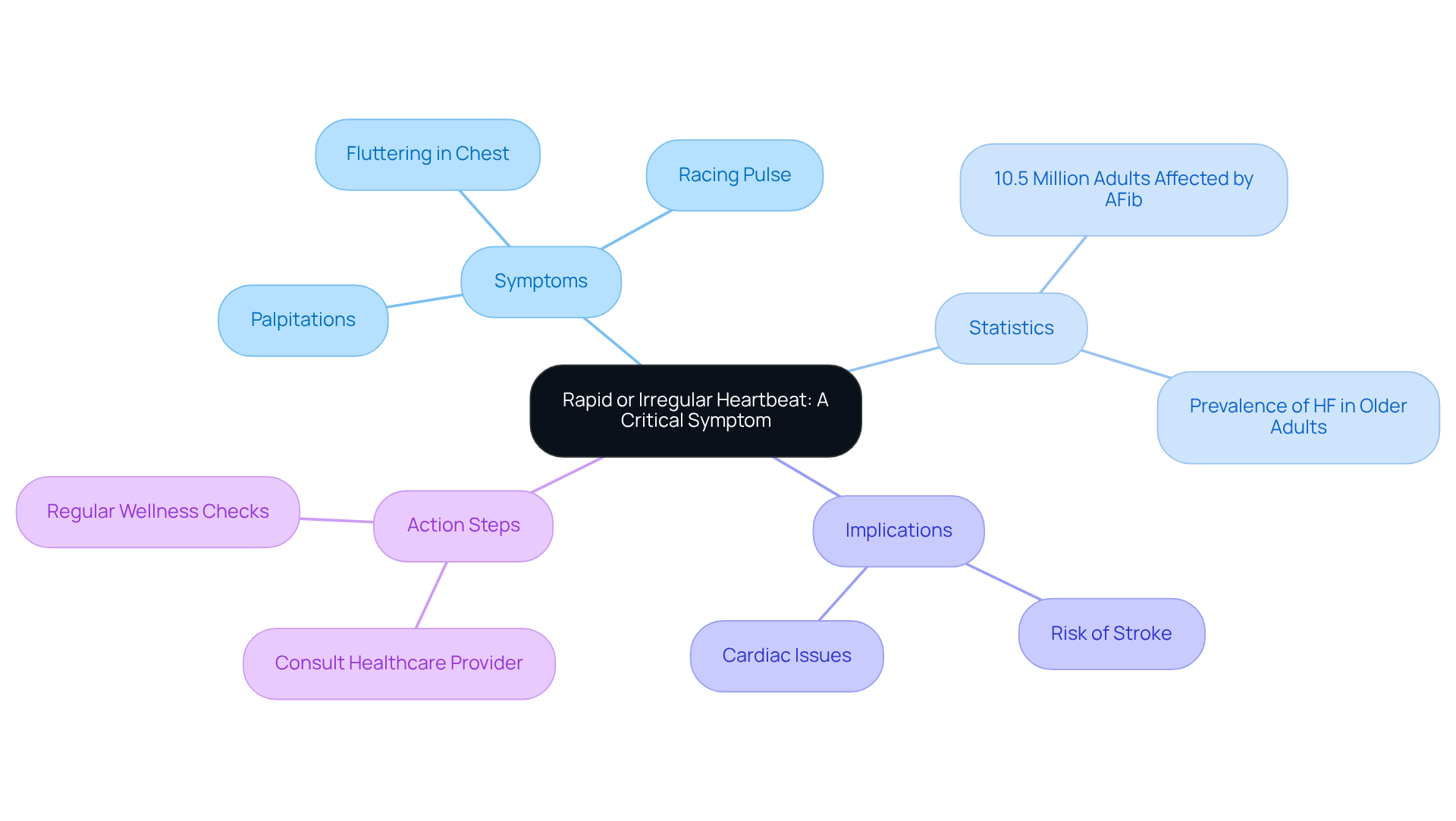
- Cognitive Issues: You might notice difficulties with memory, attention, and executive function. These challenges can make everyday tasks feel overwhelming and may affect your independence. Moderate chronic microvascular ischemic changes can even lead to vascular dementia, which is the second most common form of dementia after Alzheimer’s.
- Mood Disorders: Feelings of depression and anxiety can become more pronounced, affecting your emotional well-being and overall quality of life. Research shows that mood disorders are common among those with chronic microvascular ischemic changes, underscoring the importance of mental health support.
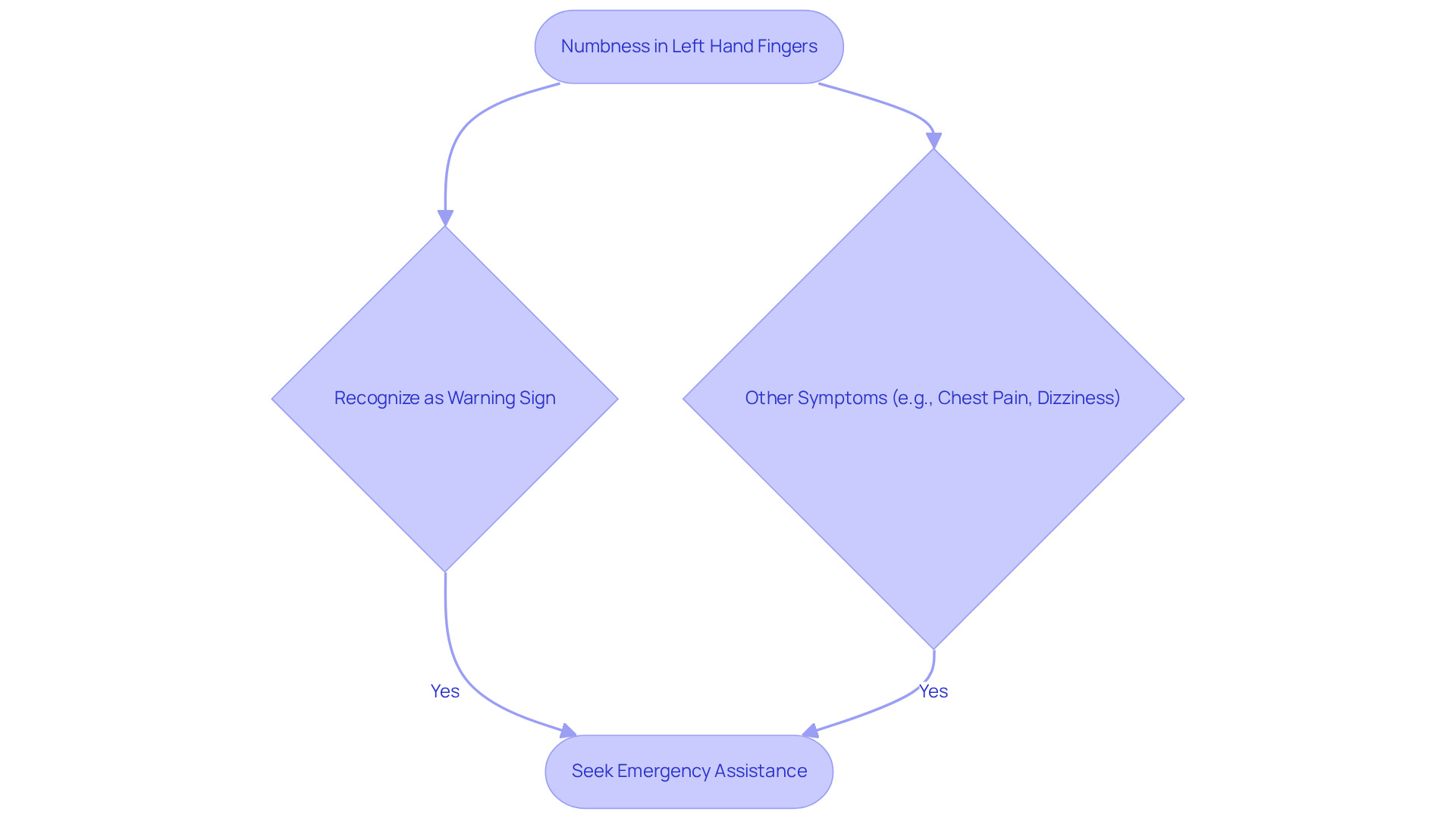
- Physical Symptoms: You may experience weakness or numbness, especially on one side of your body, along with balance and coordination issues. These symptoms can complicate mobility and increase the risk of falls, which is understandably concerning.
- Visual Disturbances: Blurred or double vision can also occur, making it harder to perform daily activities.
Recognizing these symptoms is crucial for timely diagnosis and management. Experts in elderly care emphasize that addressing cognitive and mood-related issues can significantly improve patient outcomes. By seeking help early, you may not only delay the progression of these conditions but also enhance your quality of life. Remember, you’re not alone in this journey, and support is available to help you through.
Explain Diagnostic Methods for Moderate Chronic Microvascular Ischemic Changes
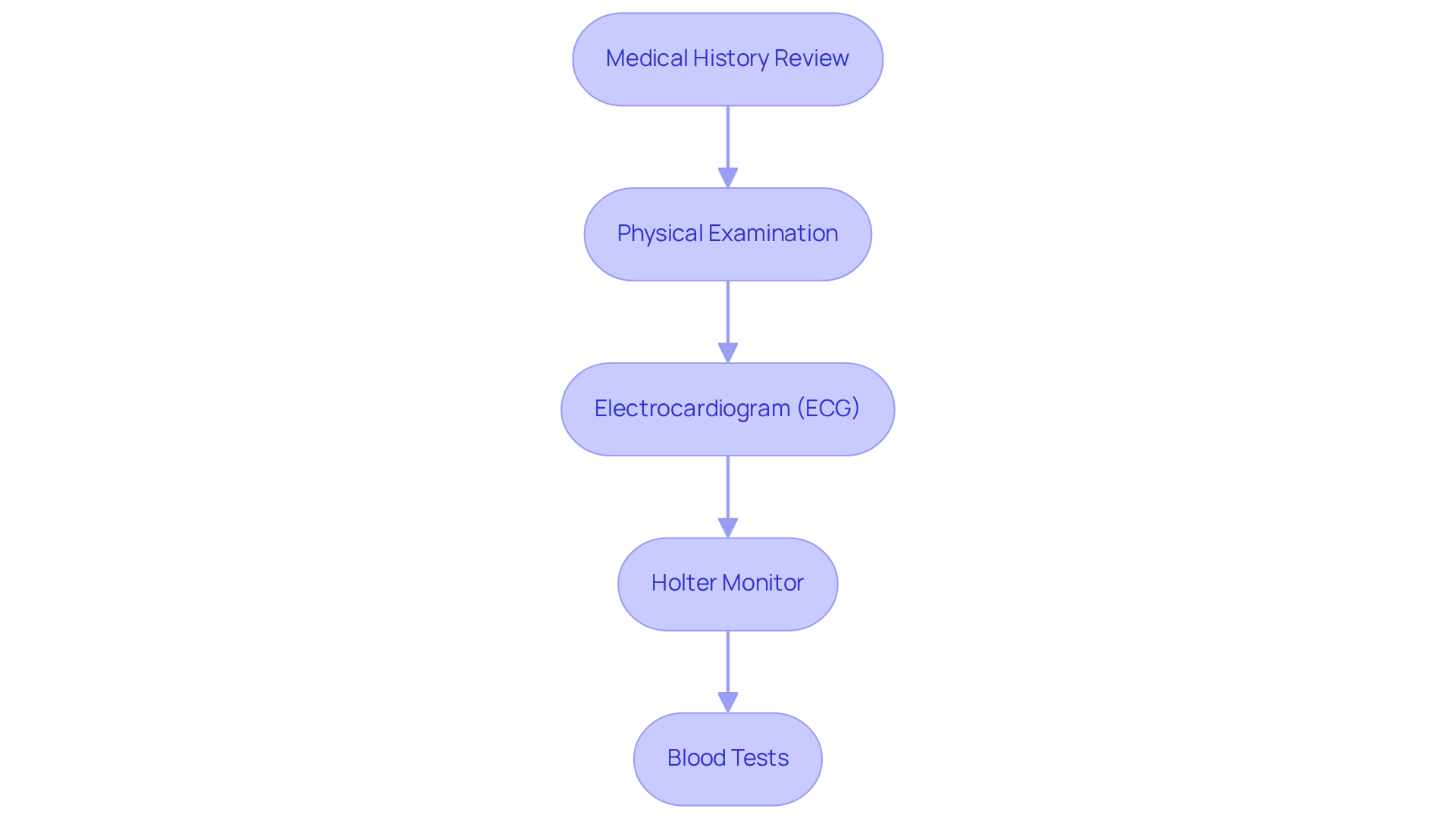
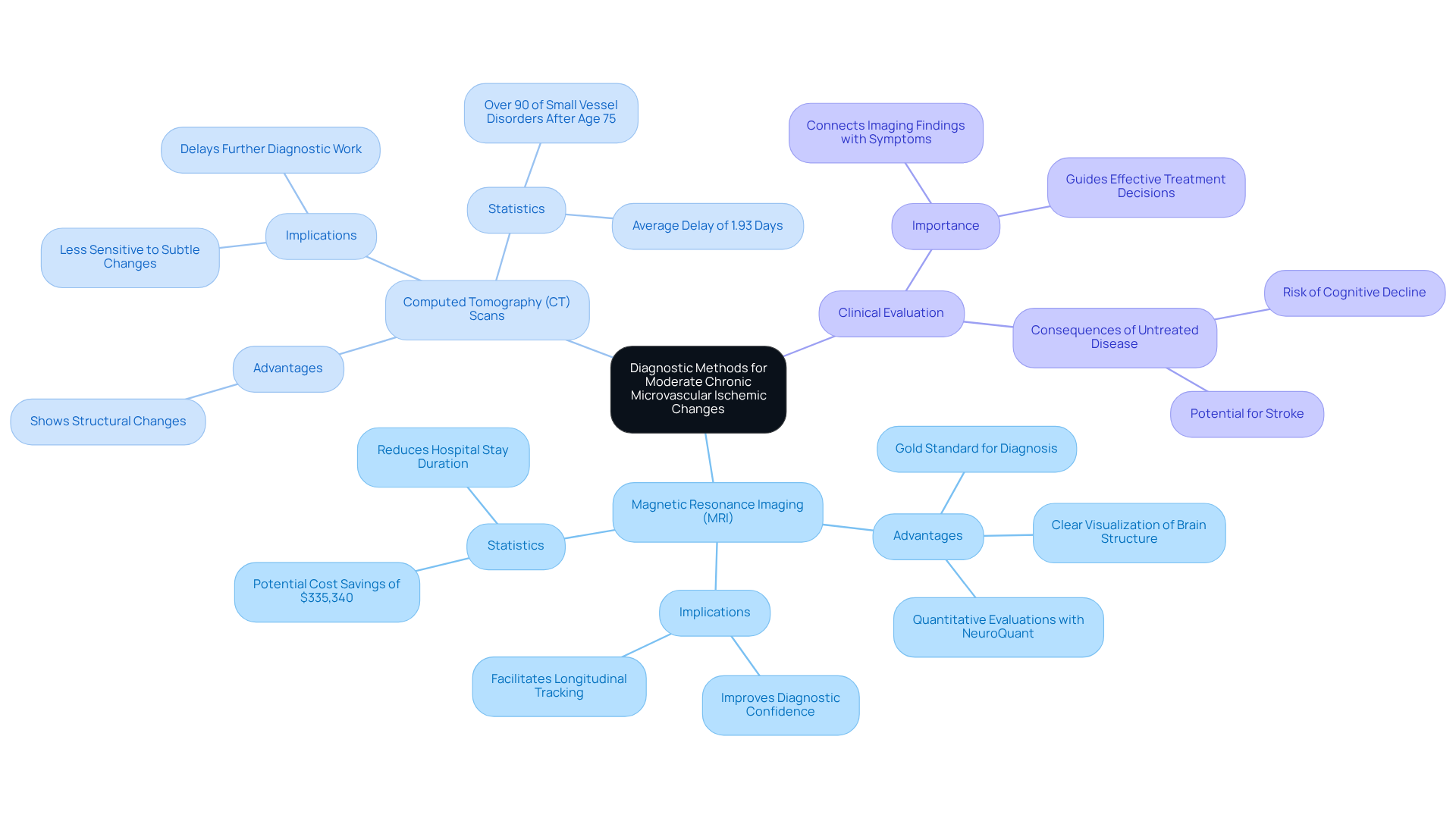
When it comes to diagnosis, several essential methods can help ensure you receive the best care possible:
- MRI: Often considered the gold standard, MRI is excellent at visualizing changes in brain structure, especially white matter lesions. It provides clear images that reveal important details about your brain’s health, including white matter hyperintensities, which may indicate microvascular issues. The technology enhances this process by offering quantitative evaluations of white matter hyperintensity burden. This can assist in monitoring your condition over time and boost your physician’s confidence in the diagnosis.
- CT scan: While CT scans can show structural changes in the brain, they tend to be less sensitive than MRI when it comes to detecting subtle blood flow changes. Research shows that initial CT evaluations can delay further diagnostic work by nearly two days, which might extend hospital stays and increase healthcare costs. This underscores the importance of choosing the right imaging method to ensure timely and effective diagnosis. It’s also worth noting that over 90% of cases occur after age 75, making precise diagnostic techniques even more crucial.
- Clinical evaluation: A thorough assessment of your symptoms and medical history is vital for connecting imaging findings with your clinical presentation. This evaluation helps doctors understand the full scope of your condition, guiding treatment decisions. It’s important to recognize that untreated small vessel disease can lead to serious long-term effects, such as cognitive decline and stroke, making accurate diagnosis essential.
These diagnostic tools are key to confirming any moderate chronic changes in blood flow and guiding your treatment options. As MRI technology continues to advance, the ability to detect small blood vessel ischemia is expected to improve, leading to better outcomes and more personalized care for you. Remember, you are not alone in this journey; support is available, and taking these steps can lead to a healthier future.
Outline Treatment Options for Moderate Chronic Microvascular Ischemic Changes
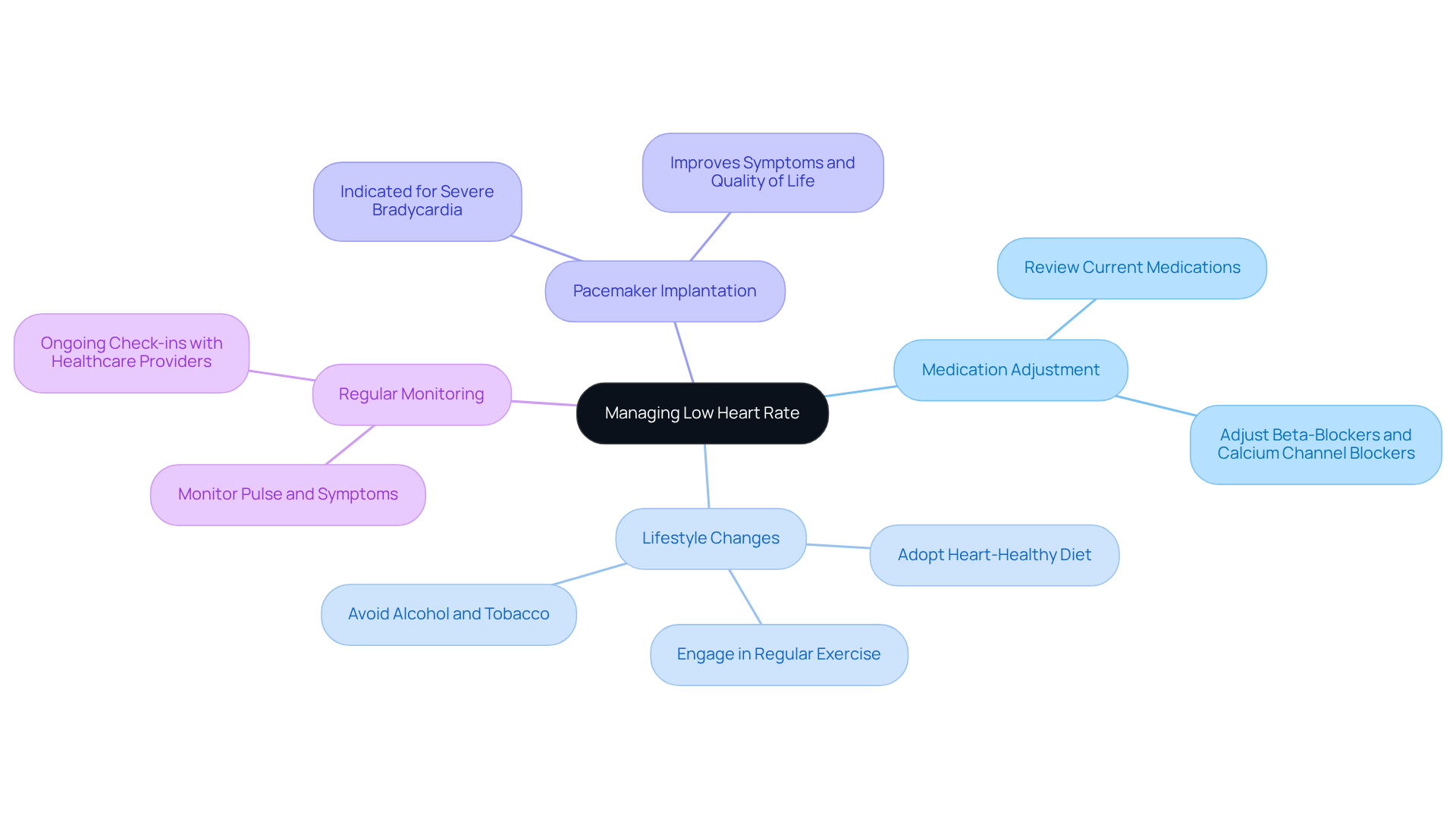
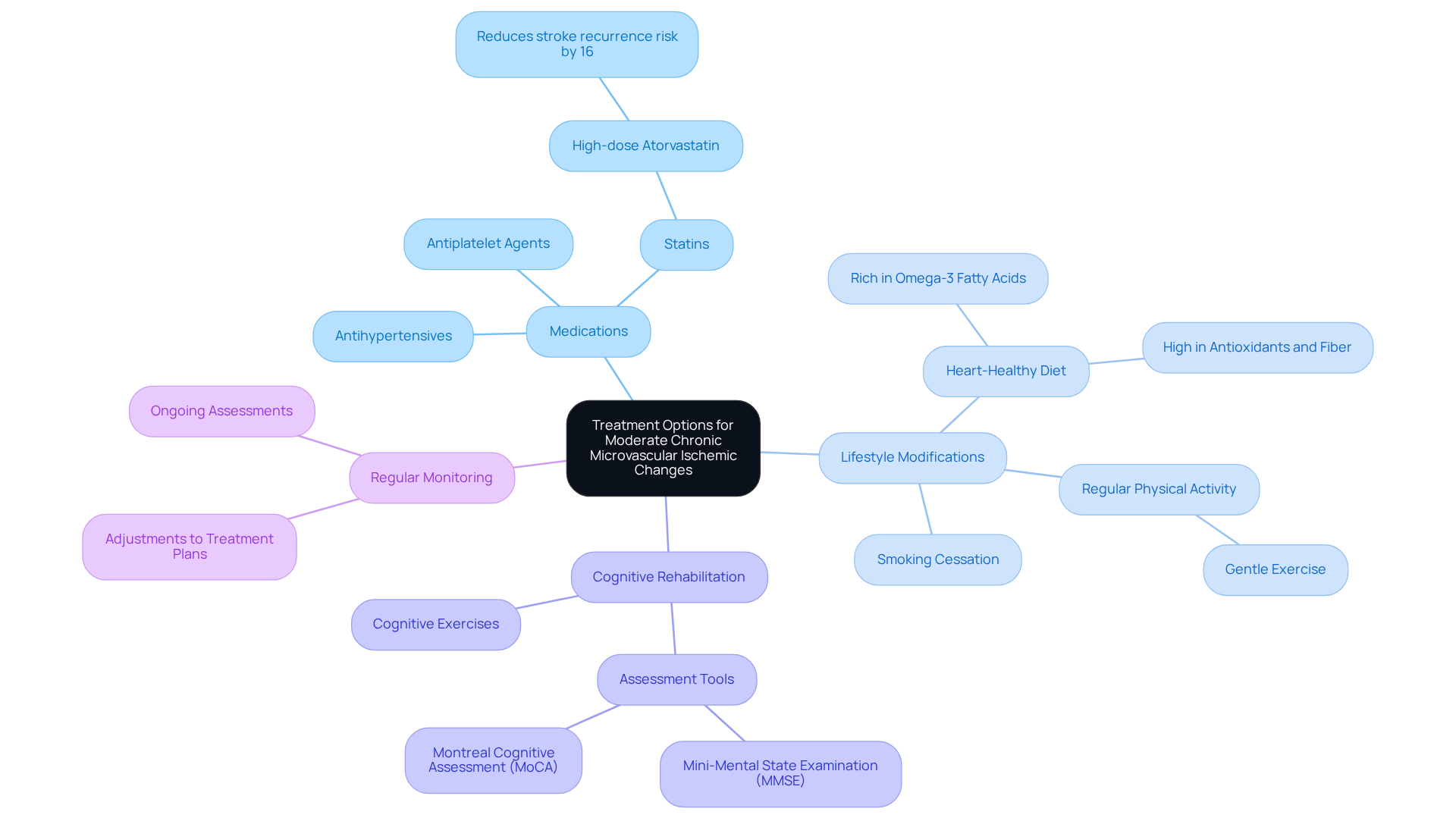
When it comes to treating moderate chronic microvascular ischemic changes, the focus is on managing risk factors and enhancing overall brain health through a compassionate, multifaceted approach:
- Medications: It’s essential to prescribe medications to control blood pressure, manage cholesterol levels, and reduce the risk of stroke. For example, high-dose atorvastatin has been shown to lower the relative risk of stroke recurrence by 16%. This highlights just how important treatment can be for your health.
- Lifestyle Modifications: Embracing a healthy diet, antioxidants, and fiber can significantly boost your well-being. Regular physical activity, even at a gentle pace, is linked to lower risks of ischemic stroke and cognitive decline. Quitting smoking is also vital, as it’s a major risk factor for cerebrovascular conditions. Research shows that making these changes can lead to better management of ischemia, ultimately enhancing your quality of life.
- Cognitive Rehabilitation: Engaging in cognitive exercises and therapies can help ease cognitive decline associated with microvascular ischemic conditions. Tools like the Mini-Mental State Examination (MMSE) and Montreal Cognitive Assessment (MoCA) can aid in early detection and intervention, allowing for personalized strategies tailored just for you.
- Regular Monitoring: Ongoing assessments and adjustments to treatment plans are crucial for effective management. Routine examinations help ensure that your blood pressure and cholesterol levels remain within target ranges, which is vital for slowing the progression of health issues.
At Amavita Heart and Vascular Center, we understand that high-risk patients, including those with diabetes, hypertension, or a family history of heart issues, can greatly benefit from comprehensive evaluations, along with thorough evaluations. These sophisticated tests, integrated into your care by Dr. Martinez-Clark—who brings extensive cardiovascular experience and Harvard training—ensure that your treatment strategies are tailored to your unique needs. Our goal is to slow disease progression and enhance your quality of life.
Conclusion
Moderate chronic microvascular ischemic changes can be a significant concern, especially for our elderly loved ones. These changes in the brain’s small blood vessels may lead to reduced blood flow, which can affect cognitive function, mood, and mobility. Understanding this condition is essential for early detection and effective management, ultimately enhancing the quality of life for those affected.
Have you noticed any symptoms like cognitive difficulties, mood swings, or physical challenges? These can be linked to microvascular changes. Diagnostic tools, particularly MRI, are crucial for accurately identifying these issues. Treatment options vary, from medication to lifestyle changes and cognitive rehabilitation. Each of these elements is interconnected, highlighting the importance of a comprehensive approach to care.
Recognizing the significance of moderate chronic microvascular ischemic changes can empower individuals and their families to seek timely intervention and support. By embracing healthier lifestyles and engaging in regular monitoring and treatment, it’s possible to reduce the risks associated with this condition. Taking these proactive steps not only supports brain health but also fosters a better quality of life for everyone involved.
So, why not take that first step today? Reach out for support, whether it’s through a healthcare provider or a community resource. You’re not alone in this journey, and together, we can work towards a healthier future.
Frequently Asked Questions
What are moderate chronic microvascular ischemic changes?
Moderate chronic microvascular ischemic changes refer to alterations in the small blood vessels of the brain that can lead to decreased blood flow and potential harm to brain tissue, often indicated by white matter hyperintensities (WMH) on MRI scans.
Who is most affected by moderate chronic microvascular ischemic changes?
This condition is particularly prevalent among older adults, with nearly all individuals over the age of 90 showing signs of chronic small blood vessel alterations, while about 5% of those aged 50 and above are affected.
What are the potential consequences of moderate chronic microvascular ischemic changes?
These changes can significantly contribute to cognitive decline, mood disorders, and mobility issues, and are linked to a higher likelihood of vascular dementia and strokes.
How are white matter hyperintensities (WMH) related to this condition?
The presence of WMH serves as a crucial indicator of moderate chronic microvascular ischemic changes and correlates with cognitive impairments and functional decline.
Can you provide an example of how this condition affects individuals?
An example is an 85-year-old female patient with a total FLAIR WMH burden of 71.8mL who presented with cognitive decline and gait disturbances, illustrating the real-world implications of this condition.
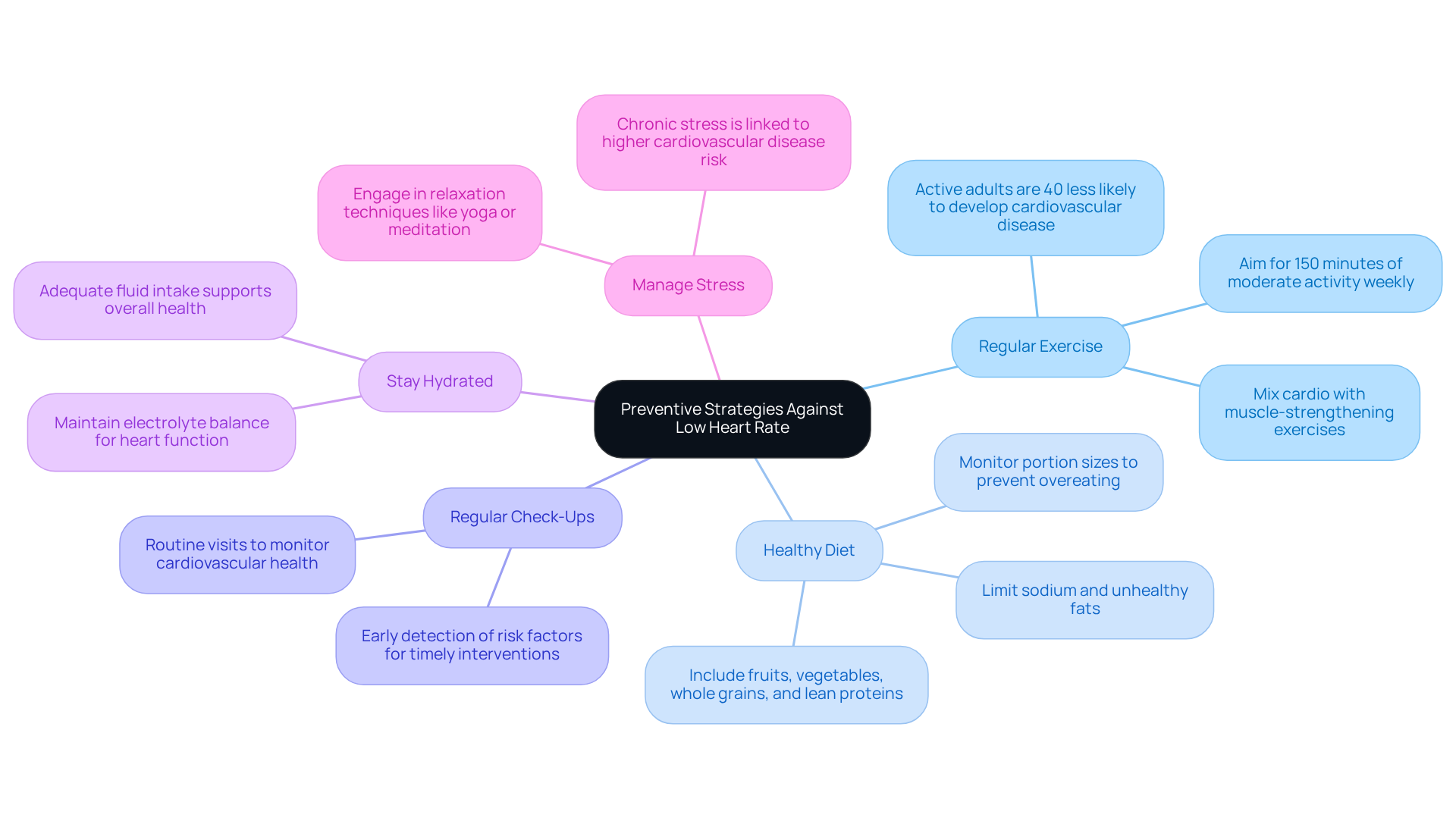
What lifestyle adjustments can help reduce risks associated with chronic small vessel alterations?
Regular health check-ups, a balanced diet, and consistent exercise are vital lifestyle adjustments that can help improve circulation and overall brain health.
Why is understanding moderate chronic microvascular ischemic changes important?
Understanding the impact of these changes is essential for developing effective management strategies that can lead to better patient outcomes and enhance the quality of life for elderly patients.
List of Sources
- Define Moderate Chronic Microvascular Ischemic Changes
- cortechs.ai (https://cortechs.ai/understanding-microvascular-ischemic-disease-and-the-value-of-neuroquant-microvascular-reports)
- medicalnewstoday.com (https://medicalnewstoday.com/articles/327112)
- amavita.health (https://amavita.health/blog/understanding-chronic-microvascular-ischemic-changes-in-the-brain)
- Cerebral Small Vessel Disease: Current and Emerging Therapeutic Strategies (https://aginganddisease.org/EN/10.14336/AD.2024.1515)
- Identify Symptoms of Moderate Chronic Microvascular Ischemic Changes
- medicalnewstoday.com (https://medicalnewstoday.com/articles/327112)
- my.clevelandclinic.org (https://my.clevelandclinic.org/health/diseases/22927-microvascular-ischemic-disease)
- int.livhospital.com (https://int.livhospital.com/chronic-microvascular-ischemic-disease-dementia)
- amavita.health (https://amavita.health/blog/understanding-chronic-microvascular-ischemic-changes-in-the-brain)
- Explain Diagnostic Methods for Moderate Chronic Microvascular Ischemic Changes
- Early MRI Versus CT Scan for Evaluation of Cerebrovascular Events in a Community Hospital: A Cost Minimization Analysis – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC7810171)
- Research finds causal evidence tying cerebral small-vessel disease to Alzheimer’s, dementia – UT Health San Antonio (https://news.uthscsa.edu/research-finds-causal-evidence-tying-cerebral-small-vessel-disease-to-alzheimers-dementia)
- cortechs.ai (https://cortechs.ai/understanding-microvascular-ischemic-disease-and-the-value-of-neuroquant-microvascular-reports)
- my.clevelandclinic.org (https://my.clevelandclinic.org/health/diseases/22927-microvascular-ischemic-disease)
- Outline Treatment Options for Moderate Chronic Microvascular Ischemic Changes
- my.clevelandclinic.org (https://my.clevelandclinic.org/health/diseases/22927-microvascular-ischemic-disease)
- Lifestyle modifications and control of cardiovascular risk factors in older adults with hypertension: from NHANES 1999–2018 – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC12272962)
- Cerebral Small Vessel Disease: Current and Emerging Therapeutic Strategies (https://aginganddisease.org/EN/10.14336/AD.2024.1515)
- Effectiveness of antihypertensive drugs for secondary prevention of ischaemic stroke: a nationwide historic cohort study (https://bmjopen.bmj.com/content/15/12/e107816)