Introduction
Many women find themselves feeling lost and uncomfortable as they navigate the changes of menopause. Bioidentical hormone therapy comes from natural plant sources and works to mimic your body’s own hormones, offering a hopeful way to manage hormonal imbalances.
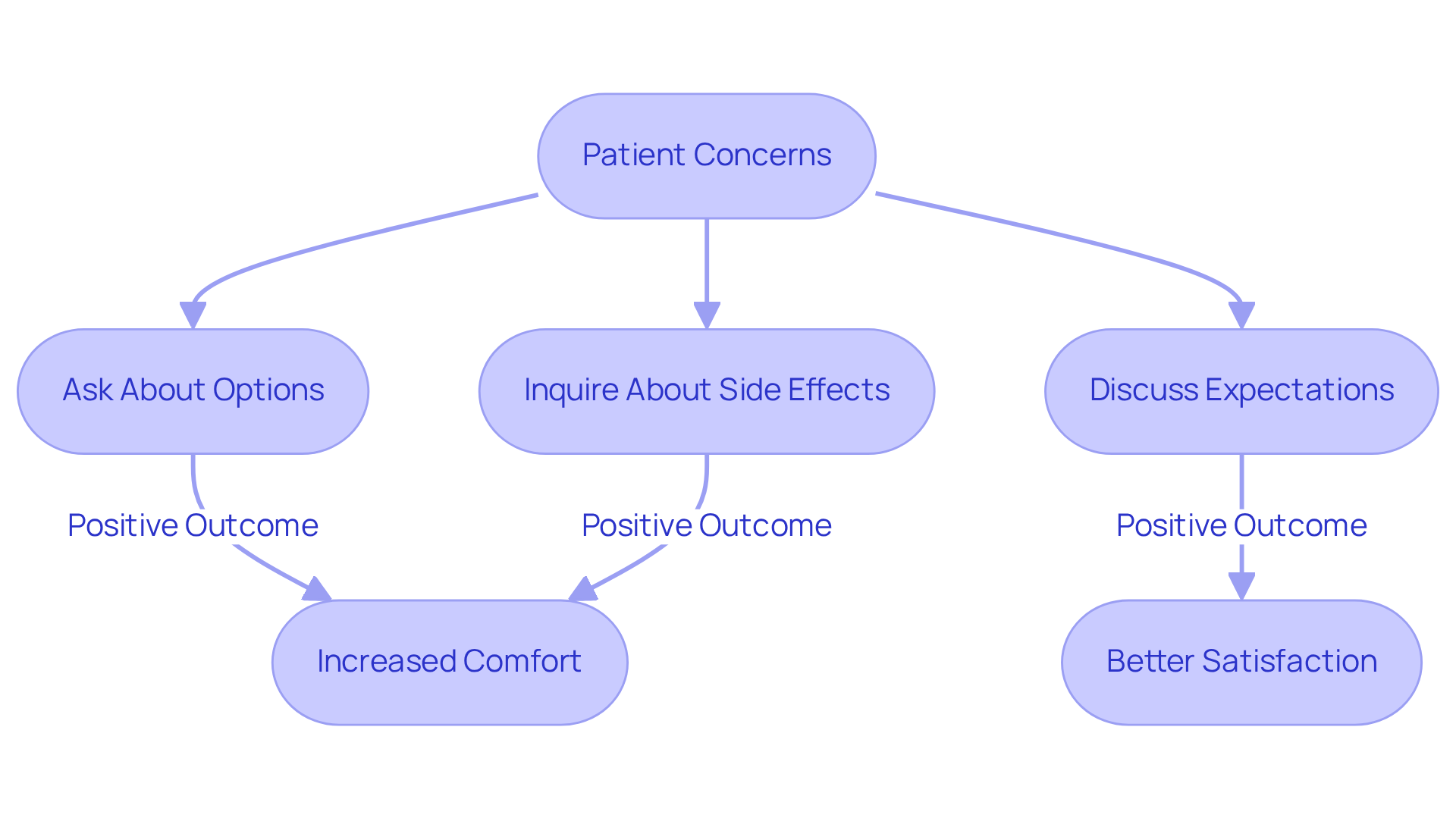
With so many options out there, how do you find the best way to feel your best during this transition? Remember, you’re not alone in this journey, and support is available to help you along the way.
Define Bioidentical Hormones and Their Role in Women’s Health
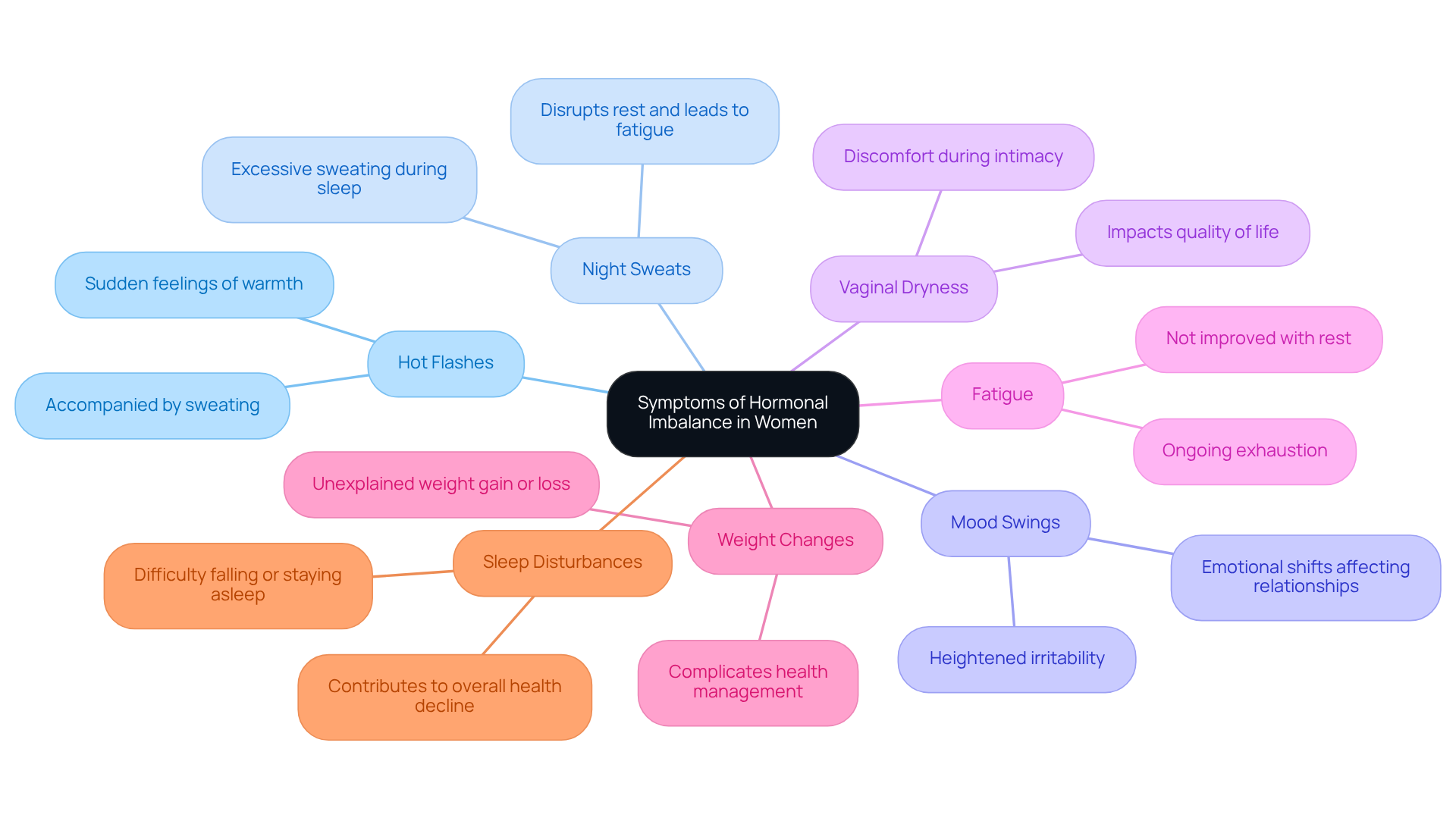
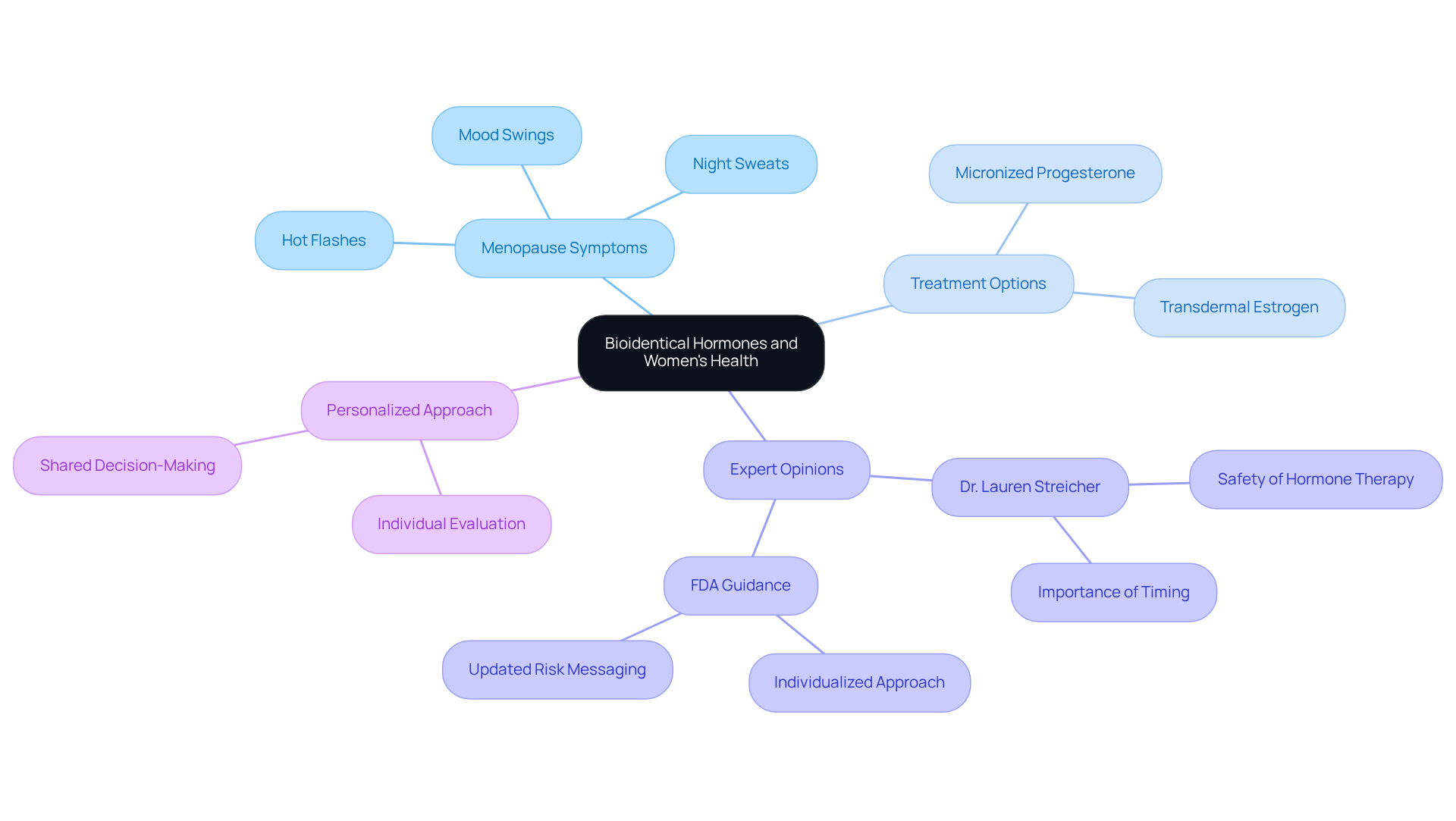
Navigating the changes of menopause can be daunting, leaving many women feeling uncertain and anxious. Bioidentical substances are made from plants and are just like the hormones your body naturally produces. They play a significant role in managing symptoms linked to hormonal imbalances, especially during menopause. Are you struggling with hot flashes, night sweats, or mood swings? Bioidentical hormone therapy for women in Florida can help relieve these symptoms. This treatment aims to balance your hormones, helping you feel better and enjoy life more fully.
Recent studies show that over 1 million women in the U.S. enter menopause each year, highlighting how common these hormonal changes are. Many women feel overwhelmed and anxious as they navigate these changes. Fortunately, advancements in hormonal treatments, such as bioidentical hormone therapy for women Florida, including micronized progesterone and transdermal estrogen, have made these options safer and more effective. Experts like Dr. Lauren Streicher remind us that when done right, hormonal treatment can be safe and beneficial for many women. The FDA’s updated guidance supports this individualized approach, emphasizing the importance of personalized evaluation and shared decision-making to optimize health outcomes for women experiencing menopause.
With the right support and treatment, you can reclaim your well-being and embrace this new chapter of life.
Compare Bioidentical Hormone Therapy with Conventional Hormone Treatments
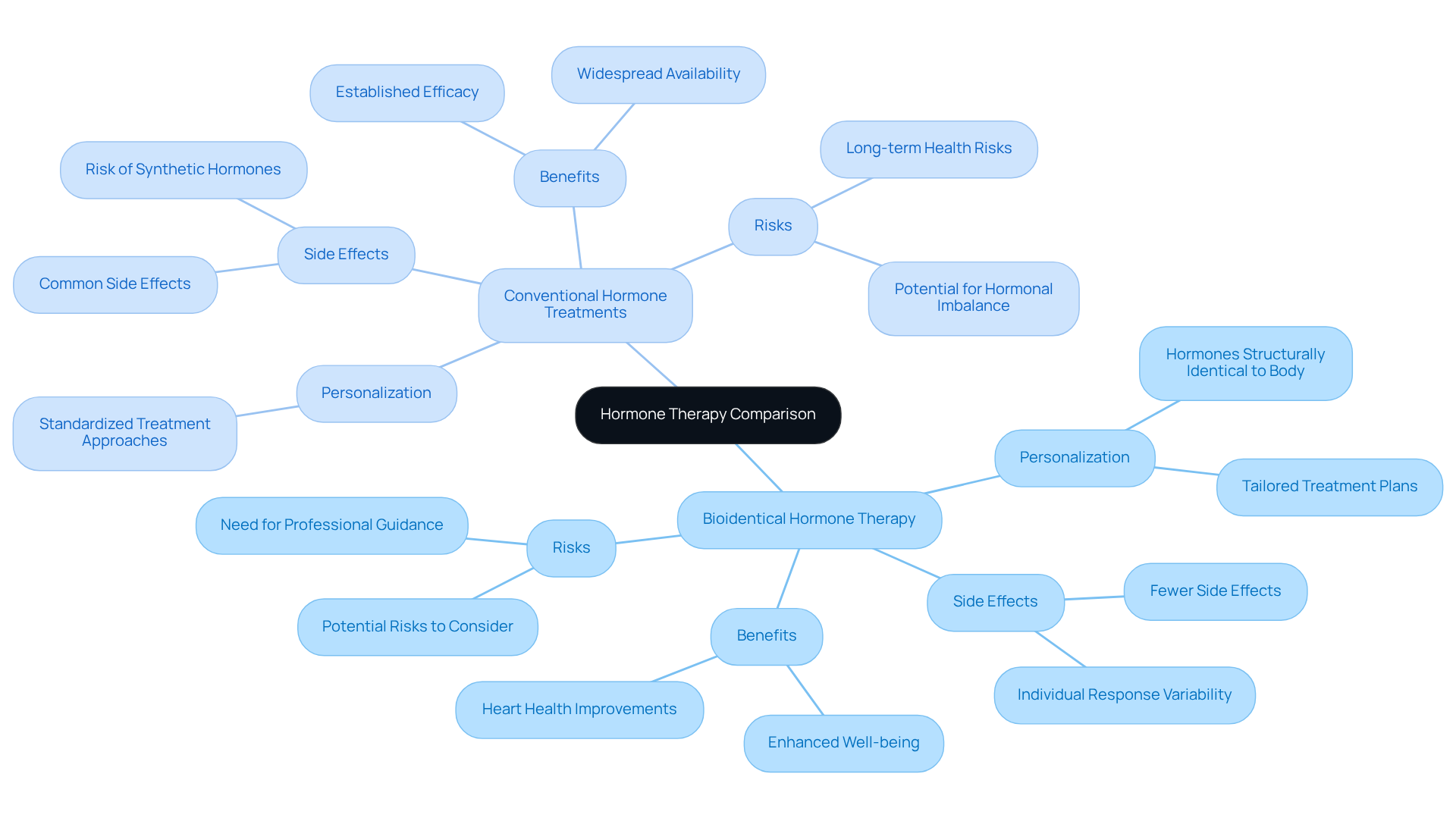
Bioidentical hormone replacement therapy offers a more personalized approach to hormone management, which can be a comforting option for many patients. Unlike traditional hormone replacement therapy, which often relies on synthetic hormones that may not perfectly match what your body naturally produces, bioidentical therapy uses hormones that are structurally identical to those made by your body. This can lead to fewer side effects and a treatment plan that feels tailored just for you.
Studies show that when testosterone replacement is done carefully and under the guidance of experienced professionals, it can offer important heart health benefits. However, it’s important to understand that while these therapies can be beneficial, they also come with potential risks that should not be overlooked. This is why having an open conversation with your healthcare provider is crucial to ensure the best care for your unique situation.
By discussing your options with a healthcare provider, you can find a treatment plan that feels right for you, ensuring your health and well-being are prioritized.
Explore Administration Methods and Dosage Selection for Bioidentical Hormones
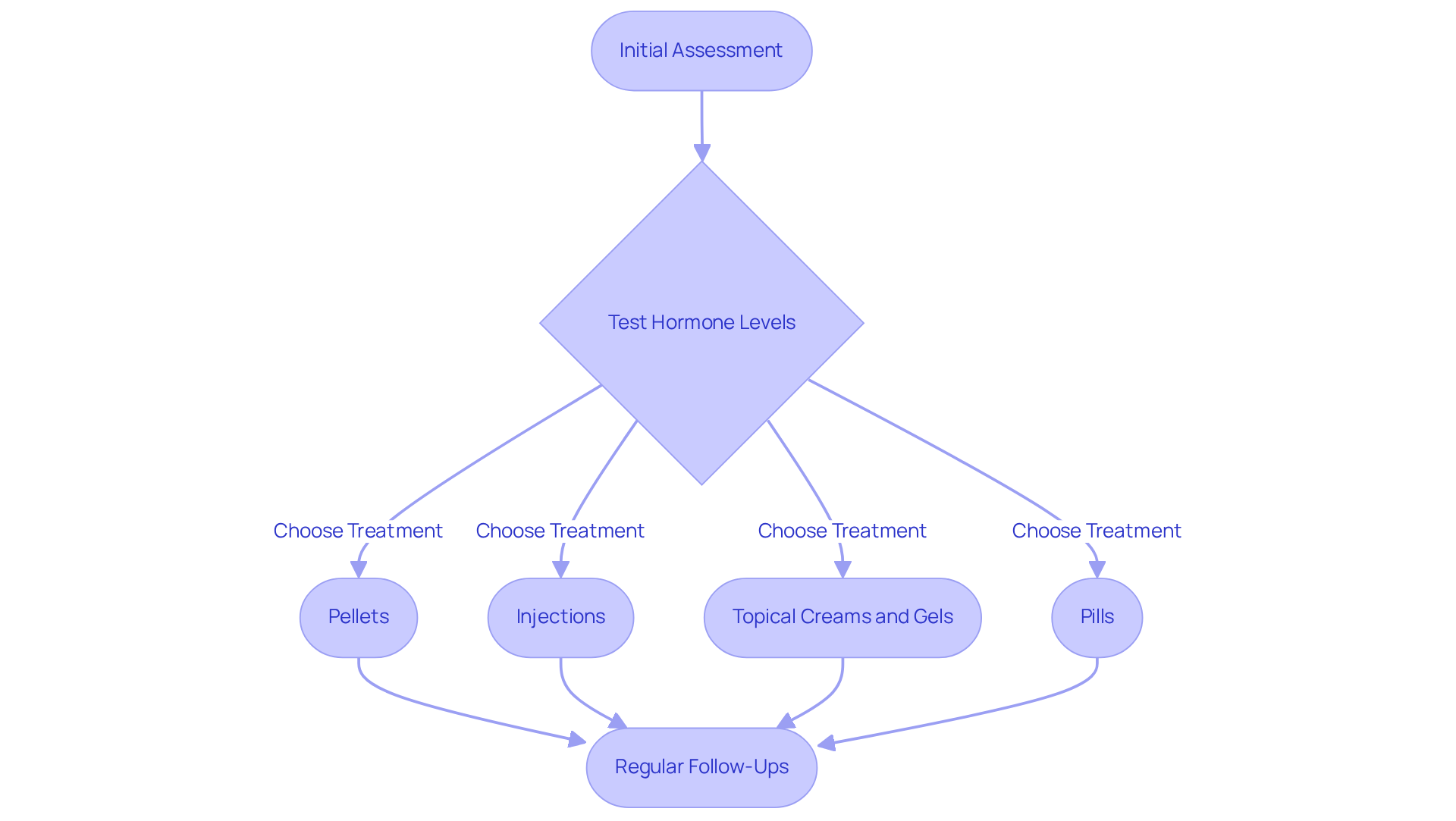
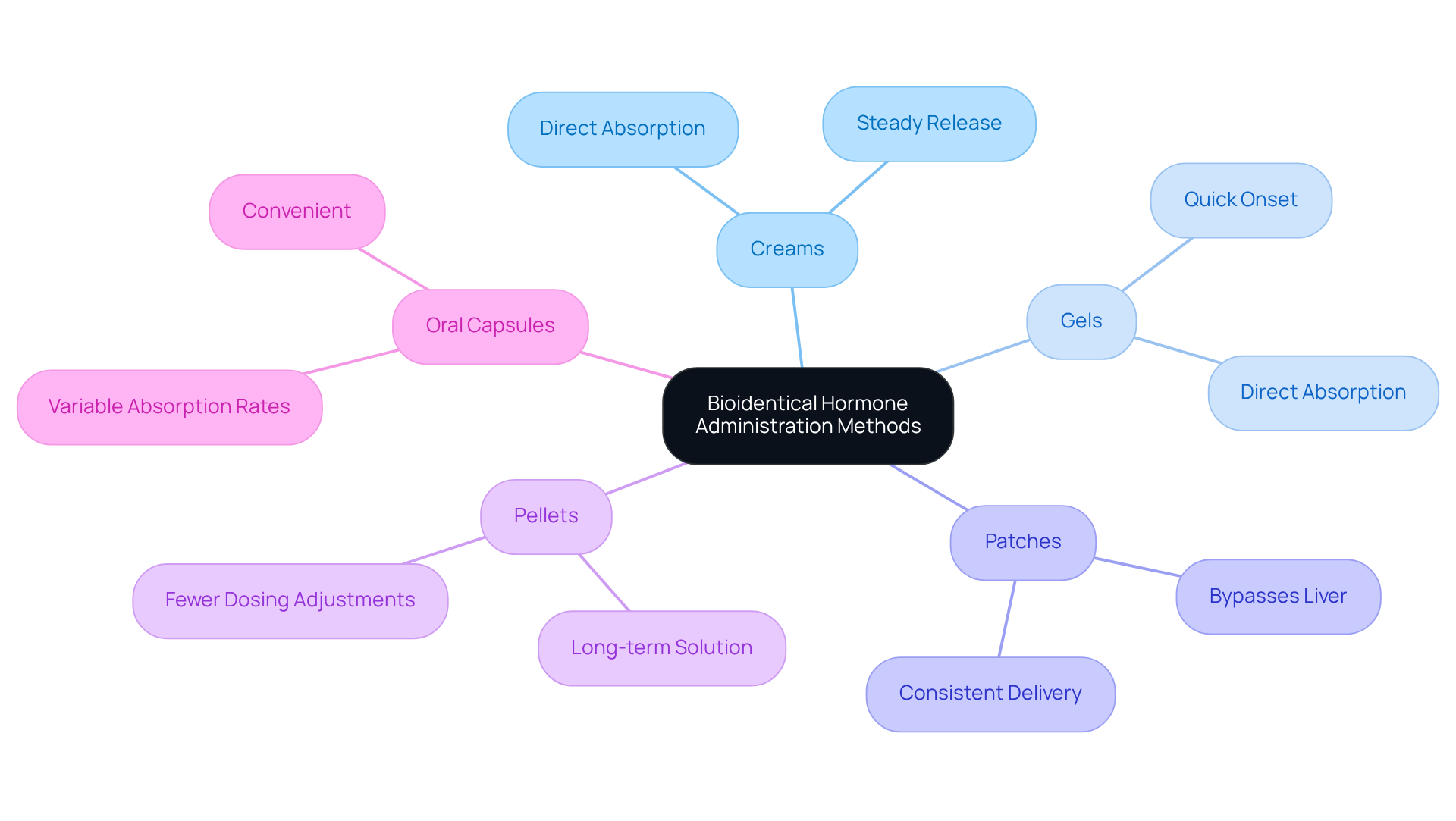
Are you feeling uncertain about the best treatment options for your hormonal health? Bioidentical substances can be administered in several ways, such as:
- creams
- gels
- patches
- pellets
- oral capsules
Each method has its own benefits. For instance, topical applications like creams and gels allow for direct absorption through the skin, ensuring a steady release of substances. Pellets, inserted under the skin, offer a long-term solution with fewer dosing adjustments. While oral capsules are convenient, they can have variable absorption rates, which might affect how well they work for you.
Choosing the right dosage is so important, and it should really reflect your unique hormonal levels, symptoms, and how you respond to treatment. Recent changes, like the FDA’s removal of the black box warning from endocrine treatments, highlight the significance of personalized approaches. This adjustment shows that bioidentical hormone therapy for women in Florida can be safe and beneficial when prescribed correctly, ultimately enhancing long-term health for women.
Case studies, such as that of Jennifer Skoog Mondesir, illustrate the positive outcomes of customized treatment. Many patients report feeling more energetic, stable in their moods, and overall better. Healthcare providers stress that regular monitoring is essential for achieving the best therapeutic results. Dr. Chad Gilliam notes, “Eliminating the black box warning provides females with greater access to treatments that can greatly enhance sleep, energy, mood, weight management, cognitive clarity, and overall quality of life.”
By regularly checking in, we can make the necessary adjustments to ensure you receive the best care tailored just for you. As we continue to learn about bioidentical treatments, focusing on personalized dosage selection remains vital in enhancing patient care. Understanding your unique health needs can lead to a more fulfilling and vibrant life, so don’t hesitate to reach out for support.
Assess Risks and Benefits of Bioidentical Hormone Therapy
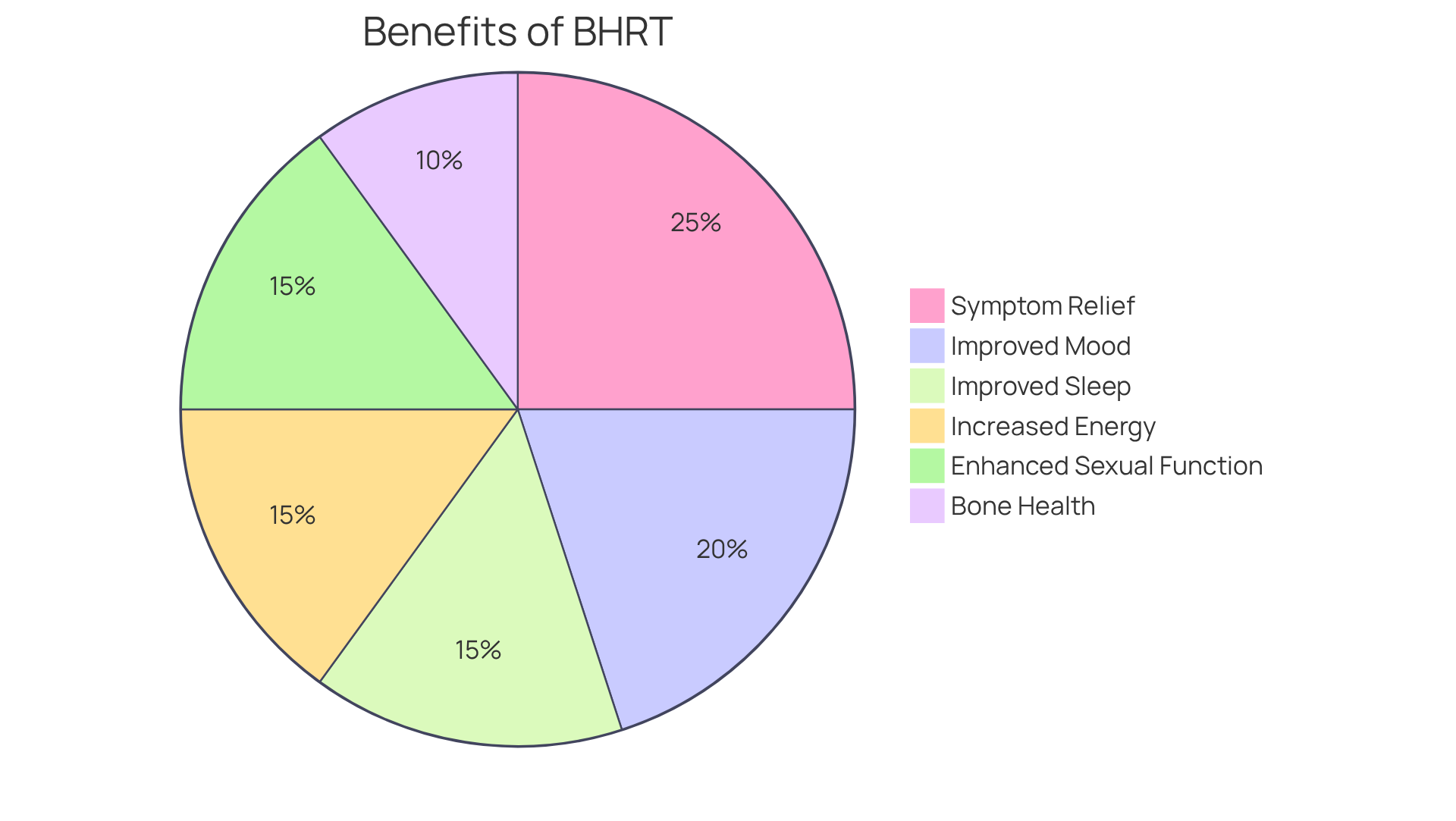
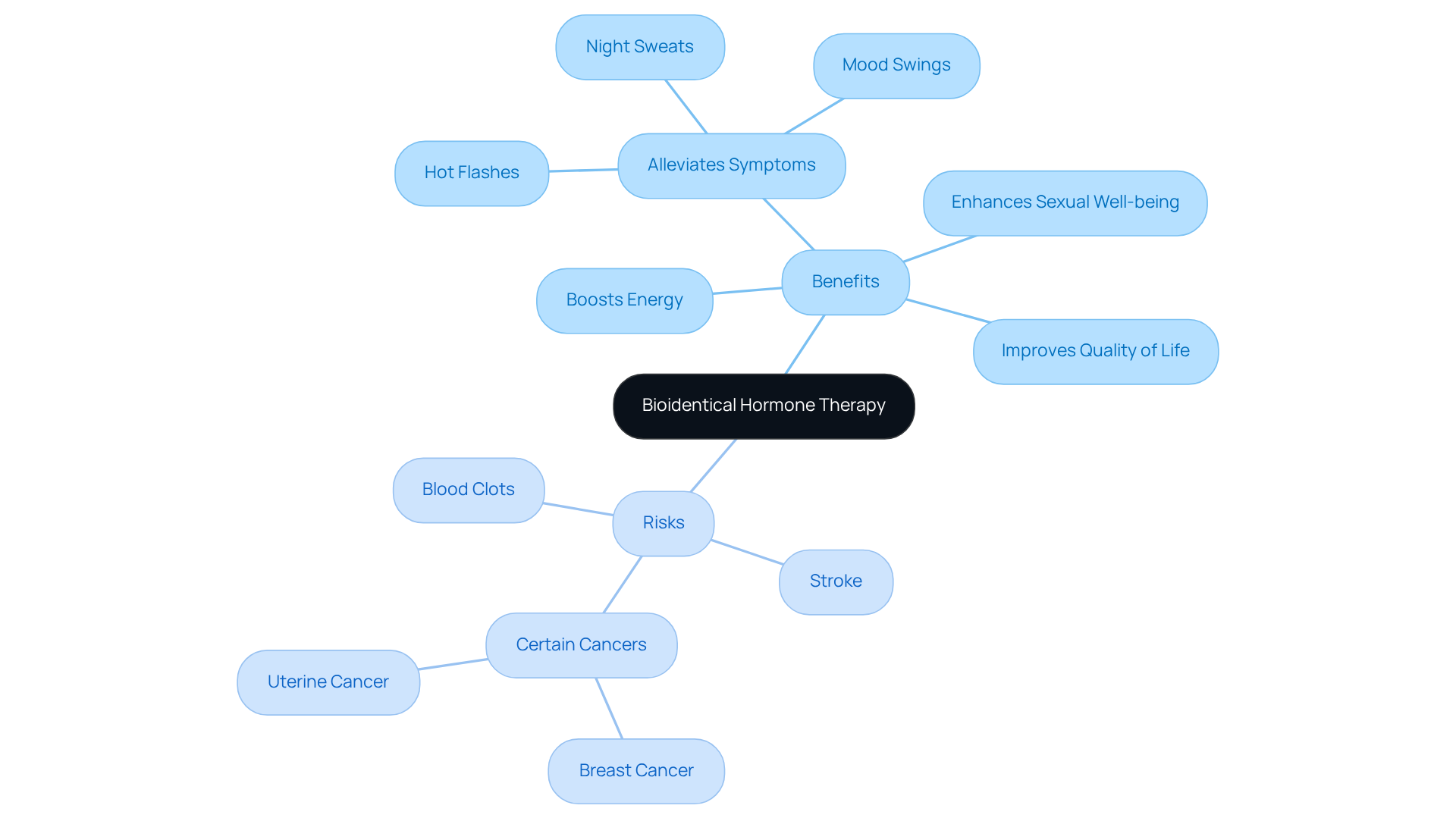
Navigating menopause can be challenging, and many individuals seek relief from symptoms that disrupt their daily lives. Many individuals experiencing menopause find that bioidentical hormone therapy for women in Florida can help alleviate uncomfortable symptoms such as hot flashes, night sweats, and mood swings, while also boosting energy and enhancing sexual well-being. Many women report a significant improvement in their overall quality of life after starting hormone replacement therapy.
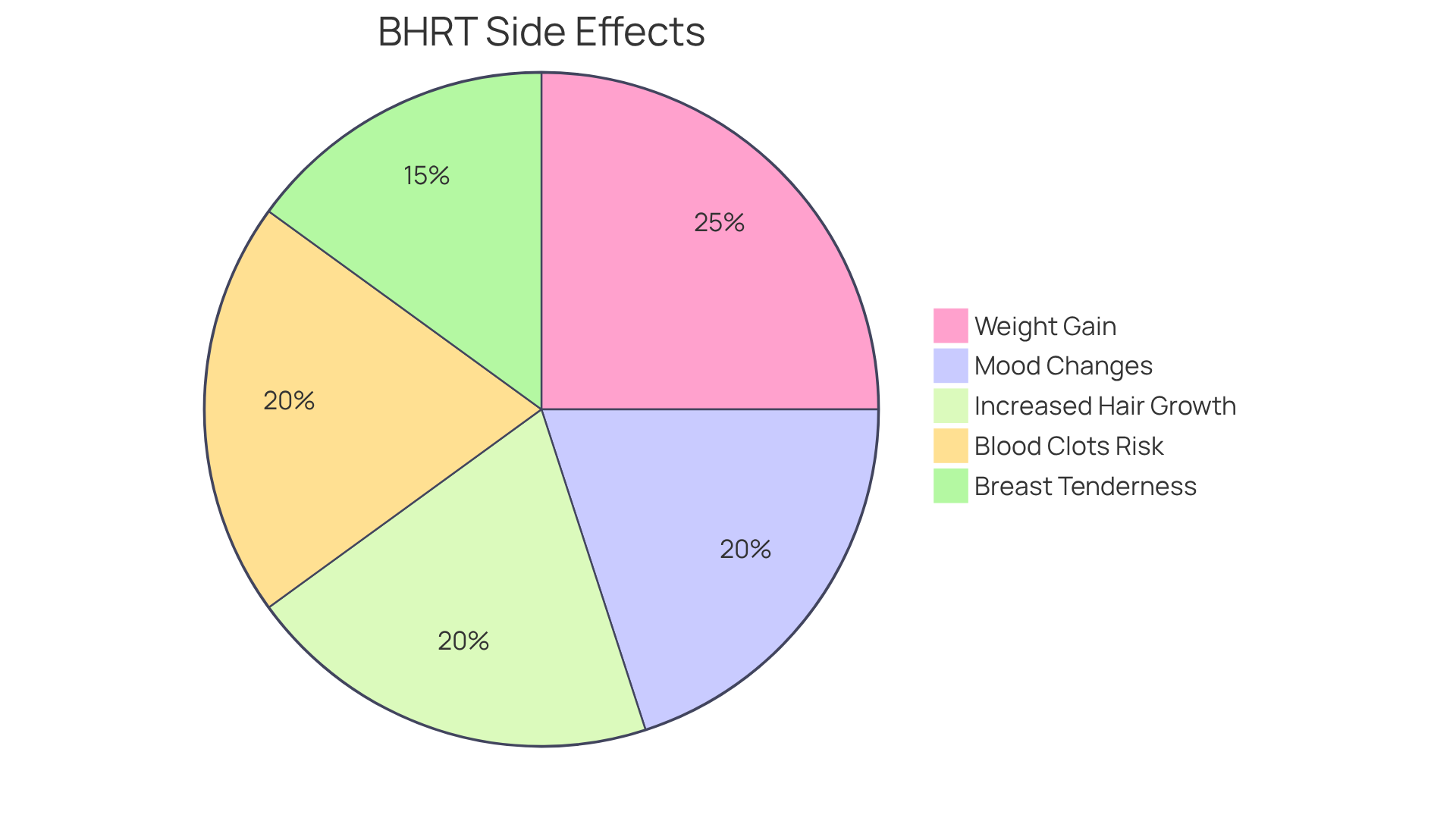
It’s important to consider both the benefits and the potential risks that come with this treatment. While many find relief, it’s essential to be aware that bioidentical hormone therapy for women in Florida can carry risks similar to those of traditional hormone treatments, including an increased chance of blood clots, stroke, and certain cancers. That’s why having an open conversation with your healthcare provider about your unique health history and any concerns you may have is so important before starting treatment.
Regular check-ins with your healthcare team can help you manage these risks and ensure that your treatment continues to support your well-being. By staying informed and connected with your healthcare team, you can make choices that truly support your well-being.
Conclusion
Bioidentical hormone therapy offers a compassionate solution for women navigating the challenges of menopause. This therapy uses hormones that match those your body naturally produces, providing a personalized way to ease the discomfort many women face during menopause. Many women in Florida are finding relief and renewed vitality through this tailored treatment option.
Throughout our discussion, we’ve highlighted the benefits of bioidentical hormones, such as their ability to reduce symptoms like hot flashes and mood swings, while also improving overall quality of life. The comparison with conventional hormone treatments shows how bioidentical therapy can lead to fewer side effects and a more comfortable experience. Furthermore, the importance of individualized dosage selection and administration methods ensures that each woman can find a regimen that suits her unique needs.
Understanding bioidentical hormone therapy can truly make a difference for women like you, who are looking to enhance their health and well-being during menopause. Engaging in open dialogue with healthcare providers and staying informed about the benefits and risks can empower you to make informed decisions about your treatment options. Embracing this knowledge can lead to a more fulfilling and vibrant life, encouraging women to take proactive steps in their health journey.
Frequently Asked Questions
What are bioidentical hormones?
Bioidentical hormones are substances made from plants that are identical to the hormones naturally produced by the body. They are used to help manage symptoms linked to hormonal imbalances, particularly during menopause.
How do bioidentical hormones help women during menopause?
Bioidentical hormone therapy helps relieve symptoms associated with menopause, such as hot flashes, night sweats, and mood swings, by balancing hormones and improving overall well-being.
How common is menopause among women in the U.S.?
Over 1 million women in the U.S. enter menopause each year, indicating that hormonal changes during this time are quite common.
What advancements have been made in hormonal treatments for menopause?
Advancements include the development of safer and more effective options such as micronized progesterone and transdermal estrogen, which are part of bioidentical hormone therapy.
What do experts say about the safety of hormonal treatment?
Experts like Dr. Lauren Streicher emphasize that when done correctly, hormonal treatments can be safe and beneficial for many women.
What does the FDA’s updated guidance suggest regarding hormonal treatments?
The FDA’s updated guidance supports an individualized approach to hormonal treatments, highlighting the importance of personalized evaluation and shared decision-making to optimize health outcomes for women experiencing menopause.
How can women reclaim their well-being during menopause?
With the right support and treatment, including bioidentical hormone therapy, women can reclaim their well-being and embrace the changes that come with menopause.
List of Sources
- Define Bioidentical Hormones and Their Role in Women’s Health
- Estrogen Patch Shortages Likely Driven By Empowered Women Seeking Relief, Expert Says (https://usnews.com/news/health-news/articles/2026-04-27/estrogen-patch-shortages-likely-driven-by-empowered-women-seeking-relief-expert-says)
- Bioidentical Hormones: Doctor Kausik Roy’s Guide to Natural Menopause Relief in 2026 – Austin MD Aesthetics & Wellness (https://austinmdclinic.com/bioidentical-hormones-doctor-kausik-roys-guide-to-natural-menopause-relief-in-2026)
- Hormones for menopause are safe, study finds. Here’s what changed (https://npr.org/sections/health-shots/2024/05/01/1248525256/hormones-menopause-hormone-therapy-hot-flashes)
- How the FDA’s Latest Decision Is Changing Hormone Therapy in 2026 – Madison Wellness & Aesthetic Center (https://madisonfamilycare.com/blog/how-the-fdas-latest-decision-is-changing-hormone-therapy-in-2026)
- Compare Bioidentical Hormone Therapy with Conventional Hormone Treatments
- The Clarion-Ledger (https://clarionledger.com/press-release/story/101903/baskin-aesthetics-reveals-insights-on-bioidentical-hormone-therapy-following-recent-fda-updates-on-menopausal-treatments)
- Comparison of Two Delivery Methods of Bioidentical Hormone Replacement Therapy | Published in North American Proceedings in Gynecology & Obstetrics (https://napgo.org/article/147434-comparison-of-two-delivery-methods-of-bioidentical-hormone-replacement-therapy)
- HRT Case Studies for Women | Hormone Therapy Research (https://bellissimomedical.com/case-studies-for-women)
- HHS Advances Women’s Health, Removes Misleading FDA Warnings on Hormone Replacement Therapy (https://fda.gov/news-events/press-announcements/hhs-advances-womens-health-removes-misleading-fda-warnings-hormone-replacement-therapy)
- Explore Administration Methods and Dosage Selection for Bioidentical Hormones
- The Clarion-Ledger (https://clarionledger.com/press-release/story/101903/baskin-aesthetics-reveals-insights-on-bioidentical-hormone-therapy-following-recent-fda-updates-on-menopausal-treatments)
- US FDA approves labeling changes to menopause hormone therapies (https://reuters.com/business/healthcare-pharmaceuticals/us-fda-approves-labeling-changes-menopausal-hormone-therapy-products-2026-02-12)
- How the FDA’s Latest Decision Is Changing Hormone Therapy in 2026 – Madison Wellness & Aesthetic Center (https://madisonfamilycare.com/blog/how-the-fdas-latest-decision-is-changing-hormone-therapy-in-2026)
- Why the ‘mad scramble’ to fill hormone therapy prescriptions for menopause (https://npr.org/2026/03/10/nx-s1-5742817/menopause-hormone-therapy-shortages)
- Assess Risks and Benefits of Bioidentical Hormone Therapy
- FDA Expert Panel on Menopause and Hormone Replacement Therapy for Wome (https://fda.gov/patients/fda-expert-panels/fda-expert-panel-menopause-and-hormone-replacement-therapy-women-07172025)
- Bioidentical Hormones: Therapy, Uses, Safety & Side Effects (https://my.clevelandclinic.org/health/treatments/15660-bioidentical-hormones)
- HHS Advances Women’s Health, Removes Misleading FDA Warnings on Hormone Replacement Therapy (https://fda.gov/news-events/press-announcements/hhs-advances-womens-health-removes-misleading-fda-warnings-hormone-replacement-therapy)