Introduction
When it comes to heart health, choosing between a nuclear stress test and a standard stress test can feel overwhelming. This decision is crucial, as it can significantly impact your diagnosis and treatment. Each method has its own unique advantages, with nuclear tests offering advanced imaging that can uncover hidden issues in blood flow.
However, determining which test is right for you often depends on your individual health circumstances and risk factors. It’s important to consider the nuances of each testing method. How can you navigate this complex landscape to ensure you receive the most effective assessment tailored to your needs?
Remember, you’re not alone in this journey. Understanding your options is the first step toward taking control of your heart health. Reach out to your healthcare provider to discuss your concerns and explore the best path forward together.
Understanding Nuclear Stress Tests and Standard Stress Tests
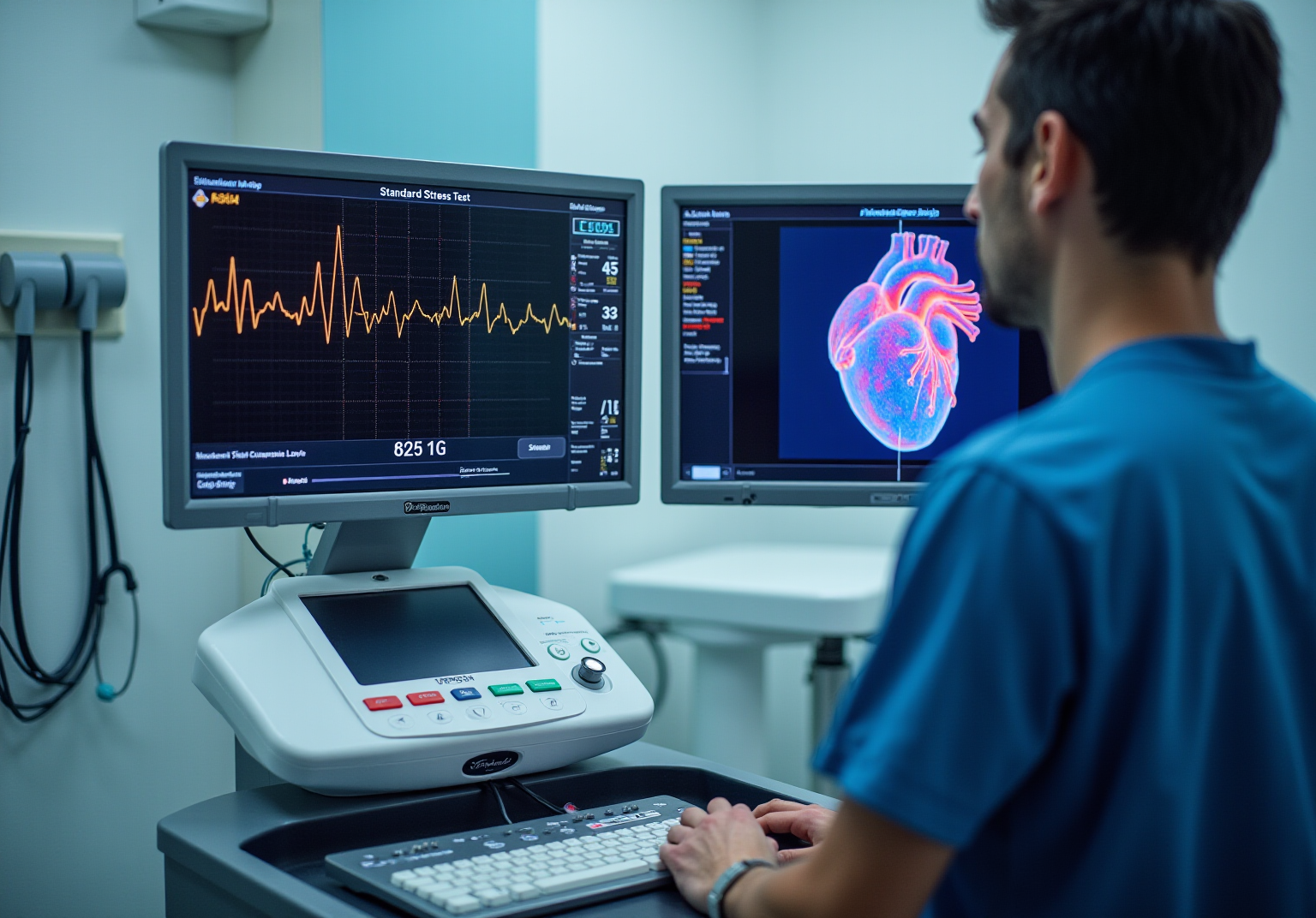
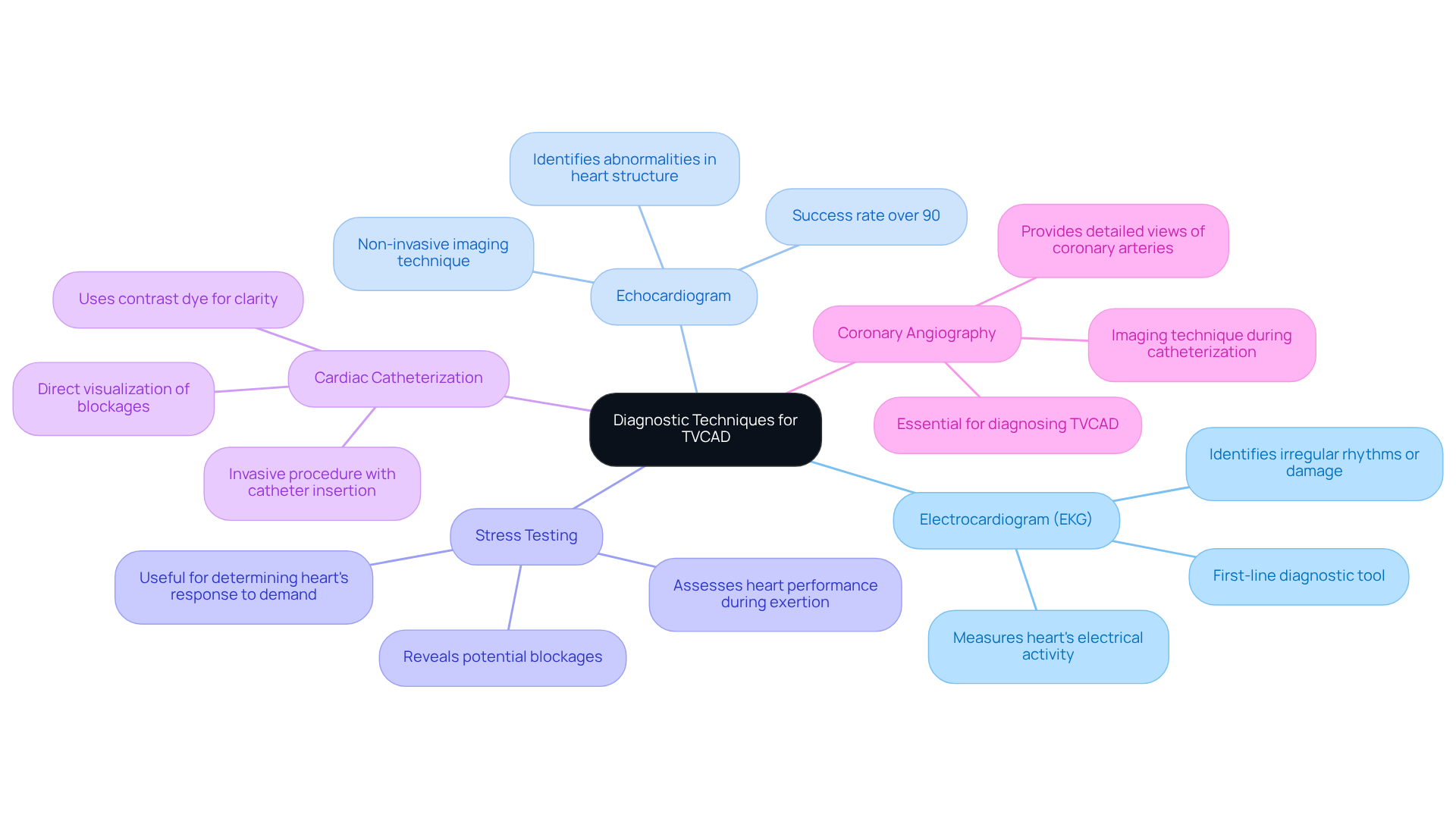
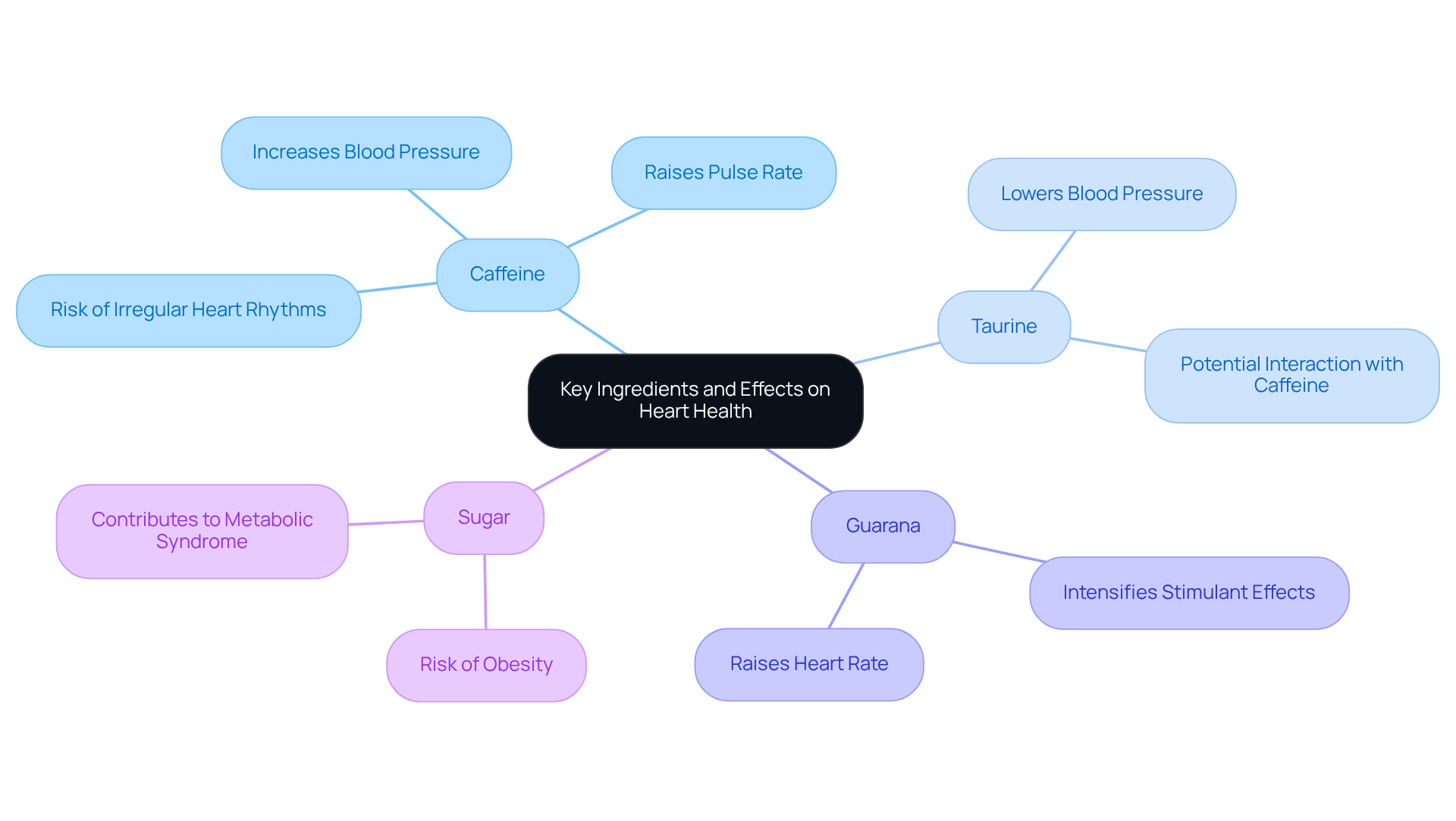
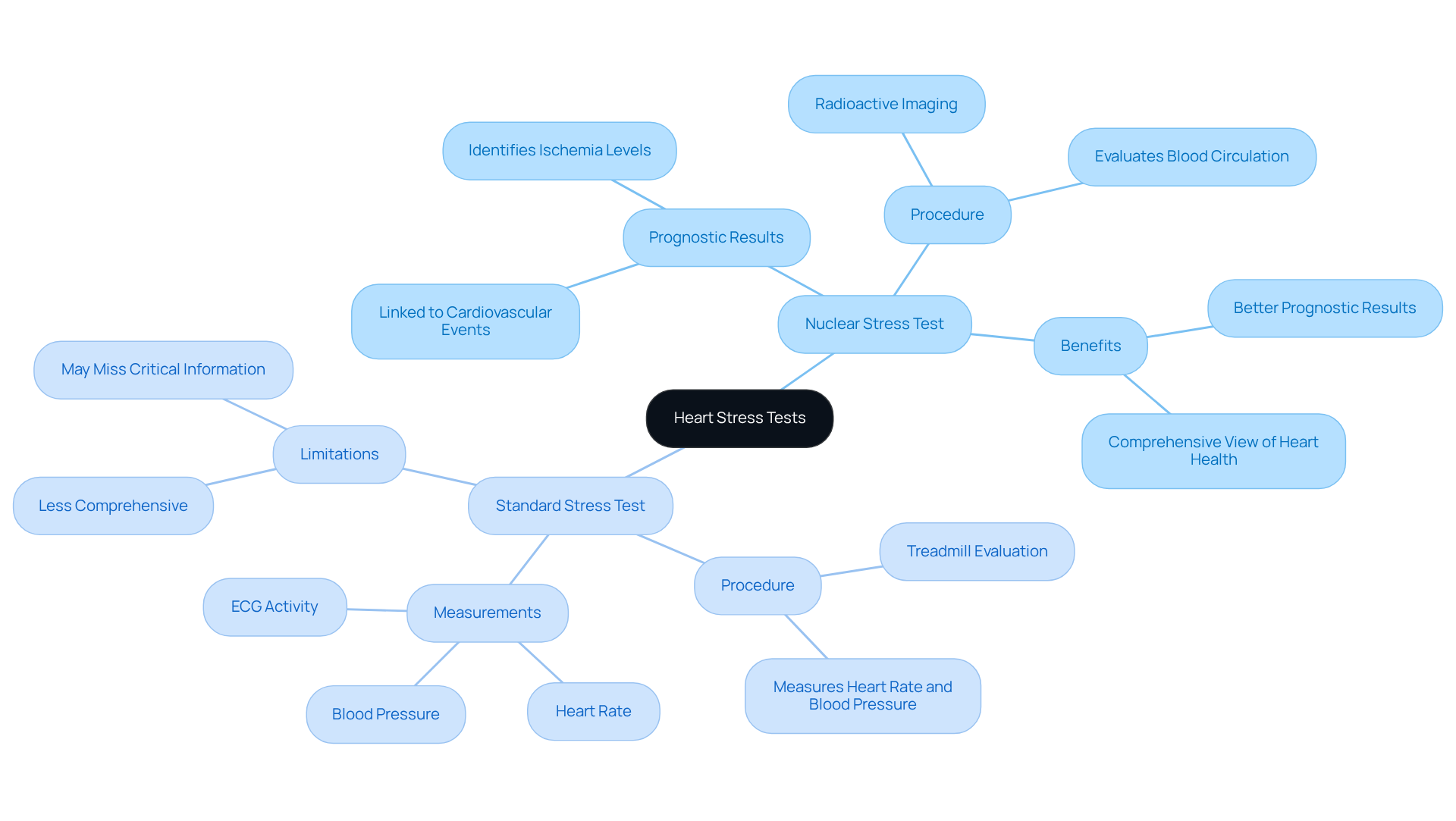
When it comes to heart health, understanding how your heart functions is crucial. A radioactive imaging procedure is an advanced technique that evaluates blood circulation to the heart muscle during both exertion and rest, using a small amount of radioactive material. This method generates detailed images of how your heart works, helping doctors diagnose conditions like coronary artery disease. In contrast, a standard evaluation, often done on a treadmill, looks at how your heart reacts to physical activity without imaging. It mainly measures heart rate, blood pressure, and electrical activity through an electrocardiogram (ECG). While both tests aim to assess heart function under stress, the imaging procedure offers a more comprehensive view of blood circulation and overall heart health.
You might be wondering how these tests can impact your health. Recent discoveries suggest that individuals who undergo nuclear stress tests may experience better prognostic results compared to those who only receive conventional assessments. For instance, the research highlighted that the level of ischemia identified through advanced imaging methods is linked to significant cardiovascular events. This underscores the importance of thorough assessments for individuals with chronic conditions.
Cardiologists emphasize the advantages of imaging stress tests when comparing them to standard tests, noting that they can reveal critical information about heart health that standard tests might miss. This is especially beneficial for patients with unusual symptoms or those at a higher risk for heart disease. As technology continues to advance, its role in guiding treatment for a wider range of conditions is increasingly recognized, making it an essential tool in modern cardiovascular care.
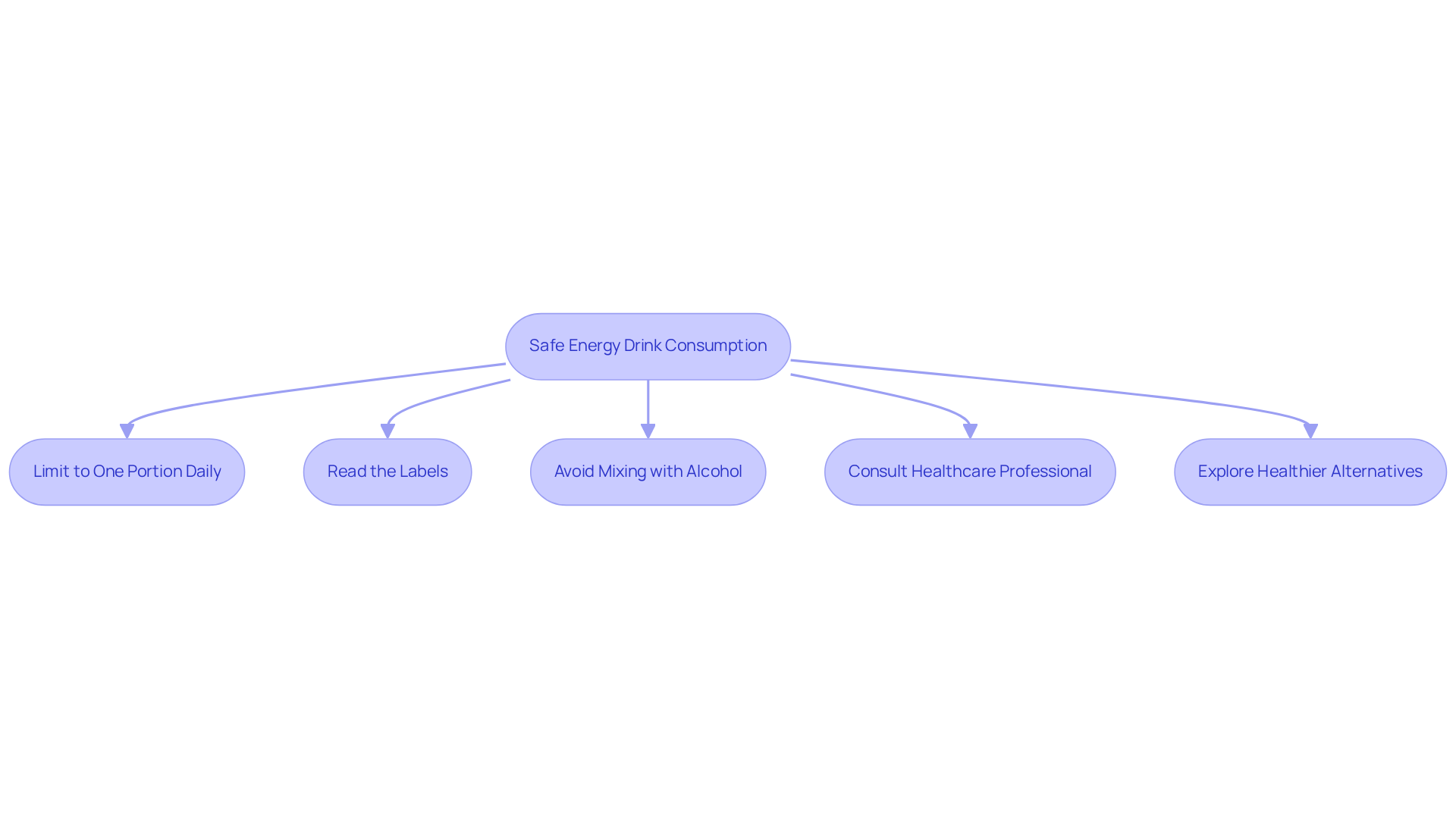
If you have concerns about your heart health, don’t hesitate to reach out for support. Understanding your options can empower you to take charge of your well-being. Remember, you’re not alone on this journey; there are compassionate professionals ready to help you every step of the way.
Comparing Effectiveness: Diagnostic Accuracy of Nuclear vs. Standard Stress Tests
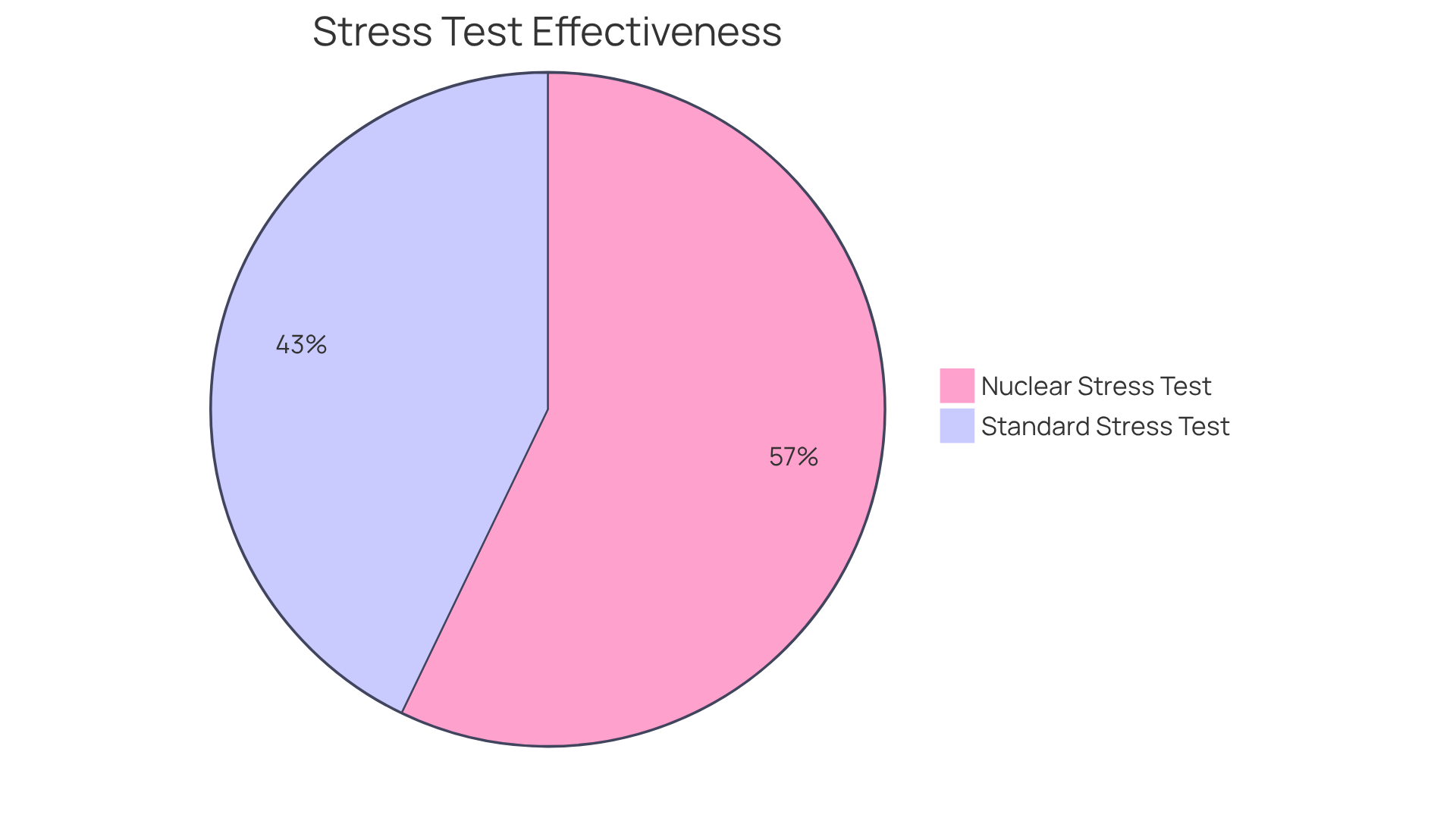
In the comparison of nuclear stress tests and standard stress tests, both are recognized for their exceptional ability to diagnose heart conditions, offering a level of precision that traditional assessments often lack. Have you ever felt uncertain about your heart health? Studies show that these atomic examinations can uncover issues that might go unnoticed, especially in individuals with unusual symptoms or those who struggle to exercise. In fact, research indicates that these evaluations have a responsiveness rate of about 84.8% for identifying obstructive coronary artery disease, especially when comparing the nuclear stress test to the standard stress test, which has a responsiveness rate of just 63.6% for conventional exercise assessments. This makes nuclear stress tests a preferred choice in complex clinical situations, providing peace of mind when it matters most.
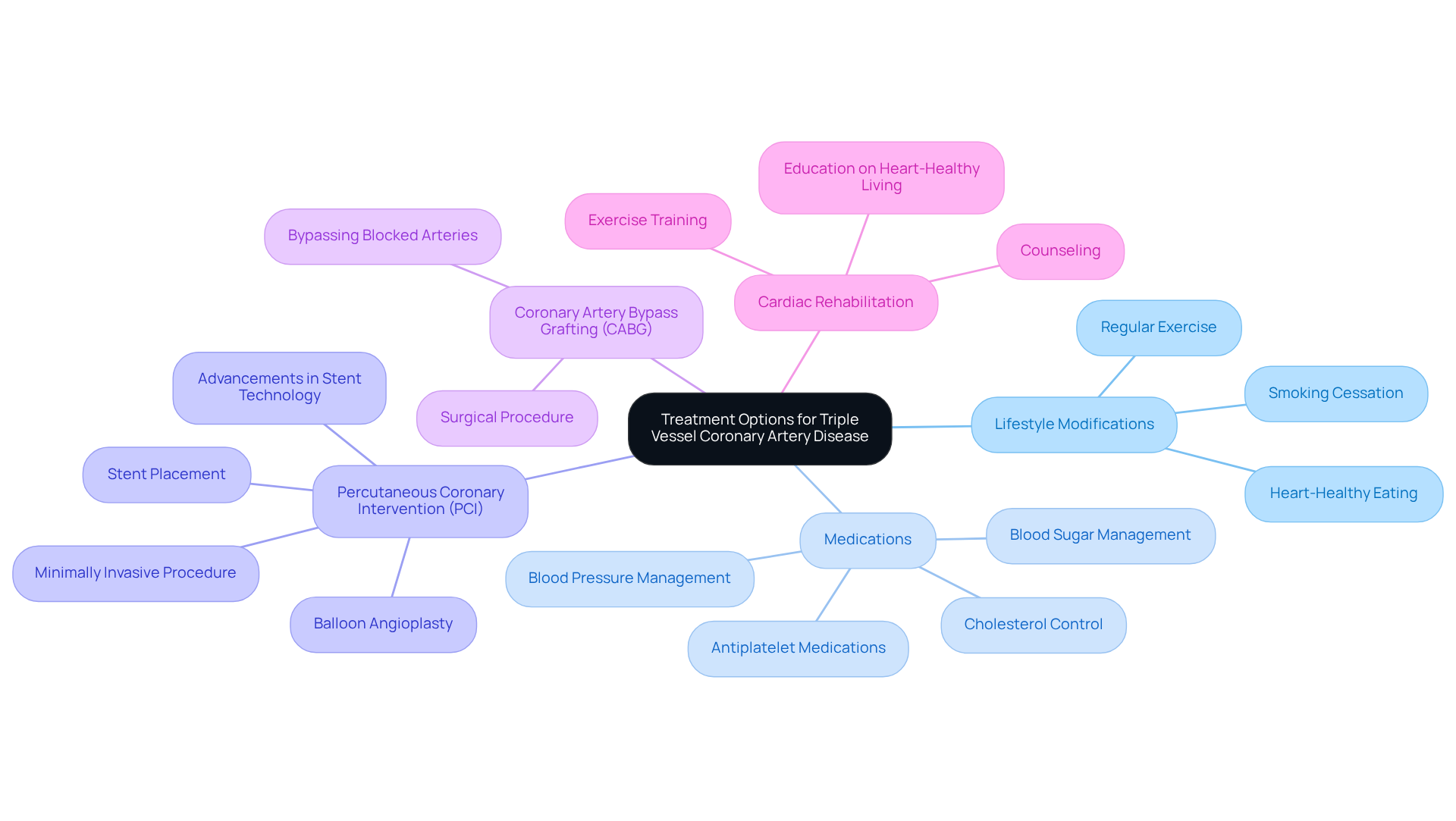
For example, a cardiac evaluation can pinpoint areas of the heart that aren’t receiving enough blood – a crucial indicator of ischemia that might be missed during a standard evaluation. This capability is particularly vital for those experiencing severe ischemia, where timely intervention can significantly improve outcomes. Indeed, individuals with severe ischemia who receive coronary interventions following a radioactive evaluation have been linked to over a 30% increase in survival compared to those treated solely with medication.
While standard stress tests are valuable for initial assessments due to their lower cost and accessibility, they often fall short in more complex situations when considering the differences between a nuclear stress test and a standard stress test. This is why radiological evaluations are increasingly recommended for individuals at higher risk or those with unclear symptoms. By opting for these nuclear tests, you can ensure a more accurate diagnosis and make well-informed treatment choices.
If you have concerns about your heart health, don’t hesitate to reach out for support. Remember, you’re not alone in this journey, and there are options available to help you feel secure and informed about your health.
Evaluating Safety: Risks and Considerations for Each Test Type
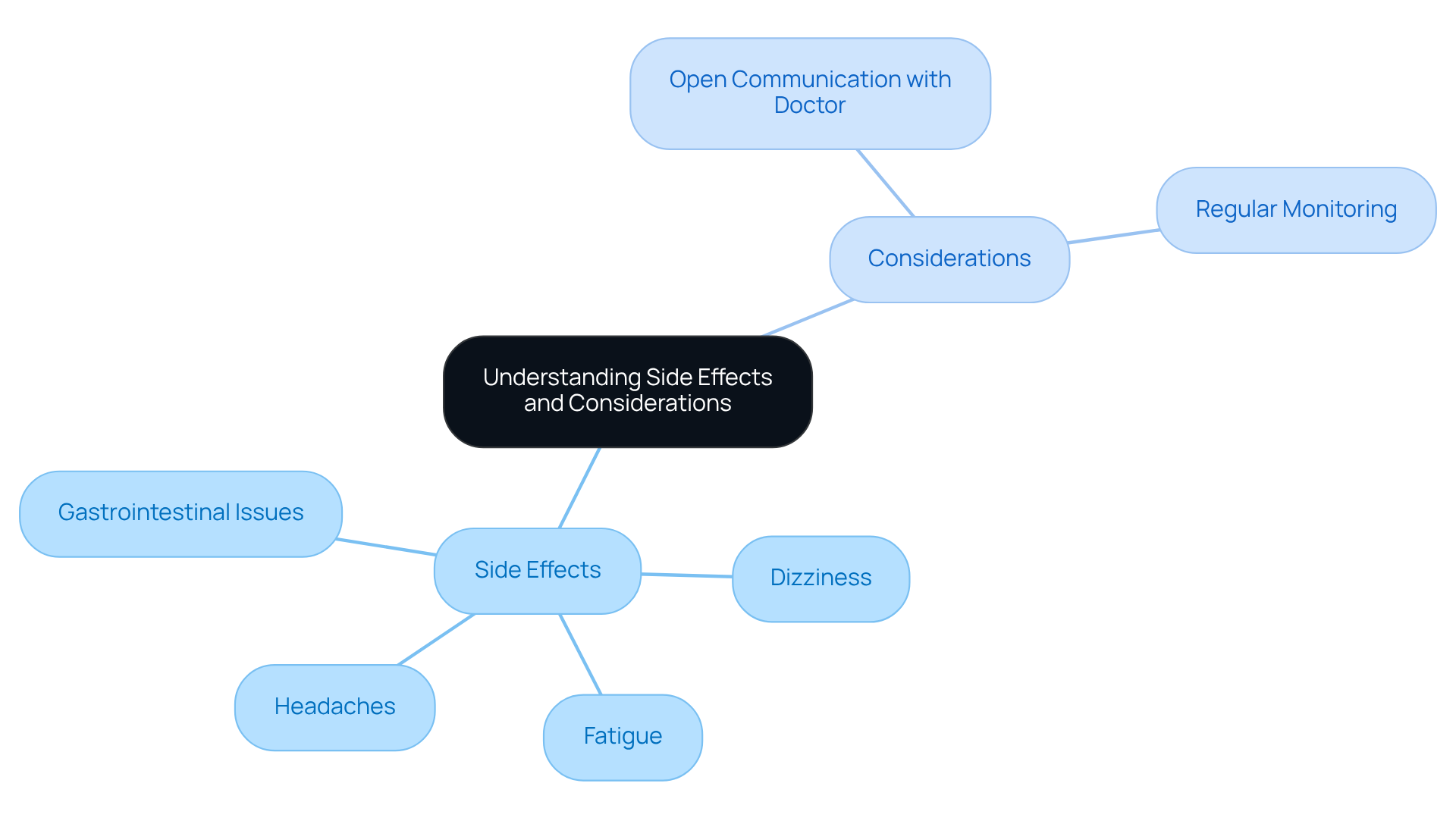
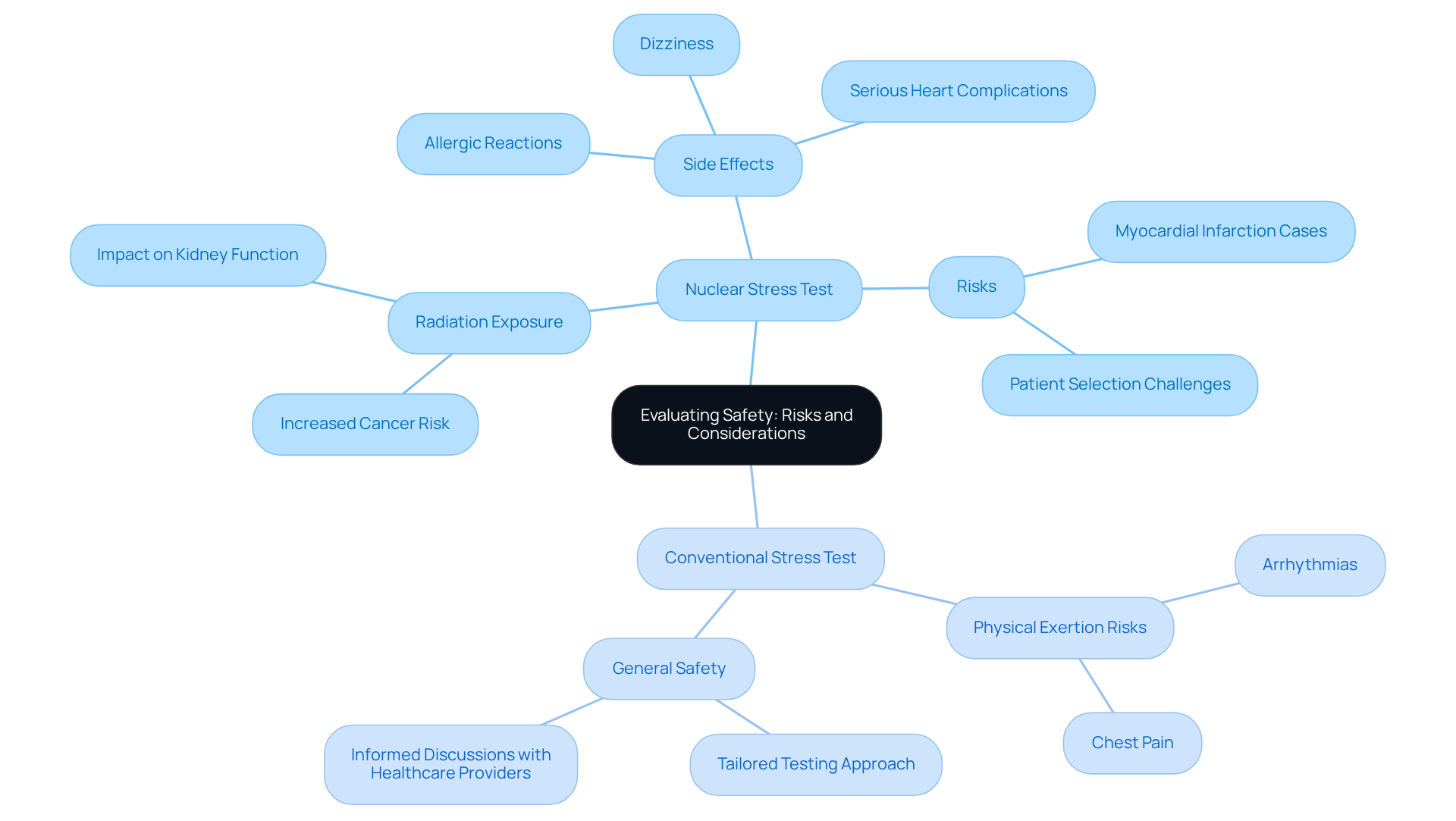
Both atomic and conventional evaluations come with their own set of risks, and it’s important to understand how they differ. When comparing tests, it’s important to note that side effects can be concerning, especially for elderly patients or those with existing health issues. Side effects may include:
- Allergic reactions to the radioactive tracer
- Dizziness
- In rare cases, serious heart complications
For example, the FAERS database has noted instances of adverse reactions like Lexiscan and Adenoscan. This highlights the need for careful selection of individuals for these tests.
At Amavita Heart and Vascular Health®, we take a compassionate approach to patient care, particularly for those at high risk. Our team combines advanced risk evaluation tools, such as echocardiograms and cardiac MRI, with personalized interventions. This ensures that we consider each individual’s health status. In contrast, when considering standard evaluations, the risks mainly involve physical exertion, such as fatigue or chest pain during exercise. While both evaluation methods are generally safe, it’s crucial to assess the individual’s overall health, age, and specific cardiovascular risks.
Healthcare professionals stress the importance of evaluating each person’s circumstances. For instance, older adults may face unique challenges that could complicate the safety of either test type. Ultimately, having informed discussions with healthcare providers is essential in determining the most suitable testing method. Remember, you are not alone in this journey; we are here to support you every step of the way.
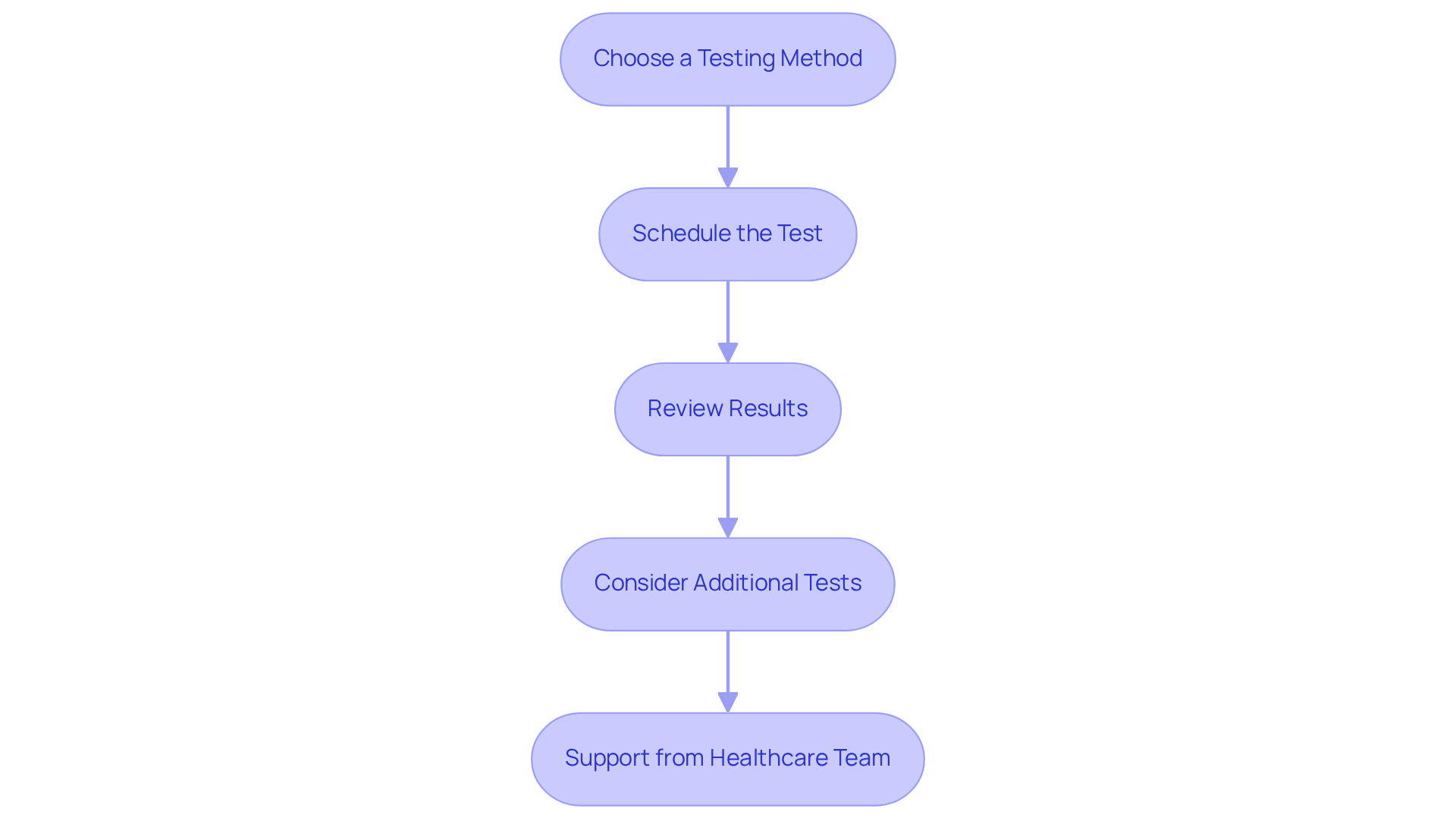
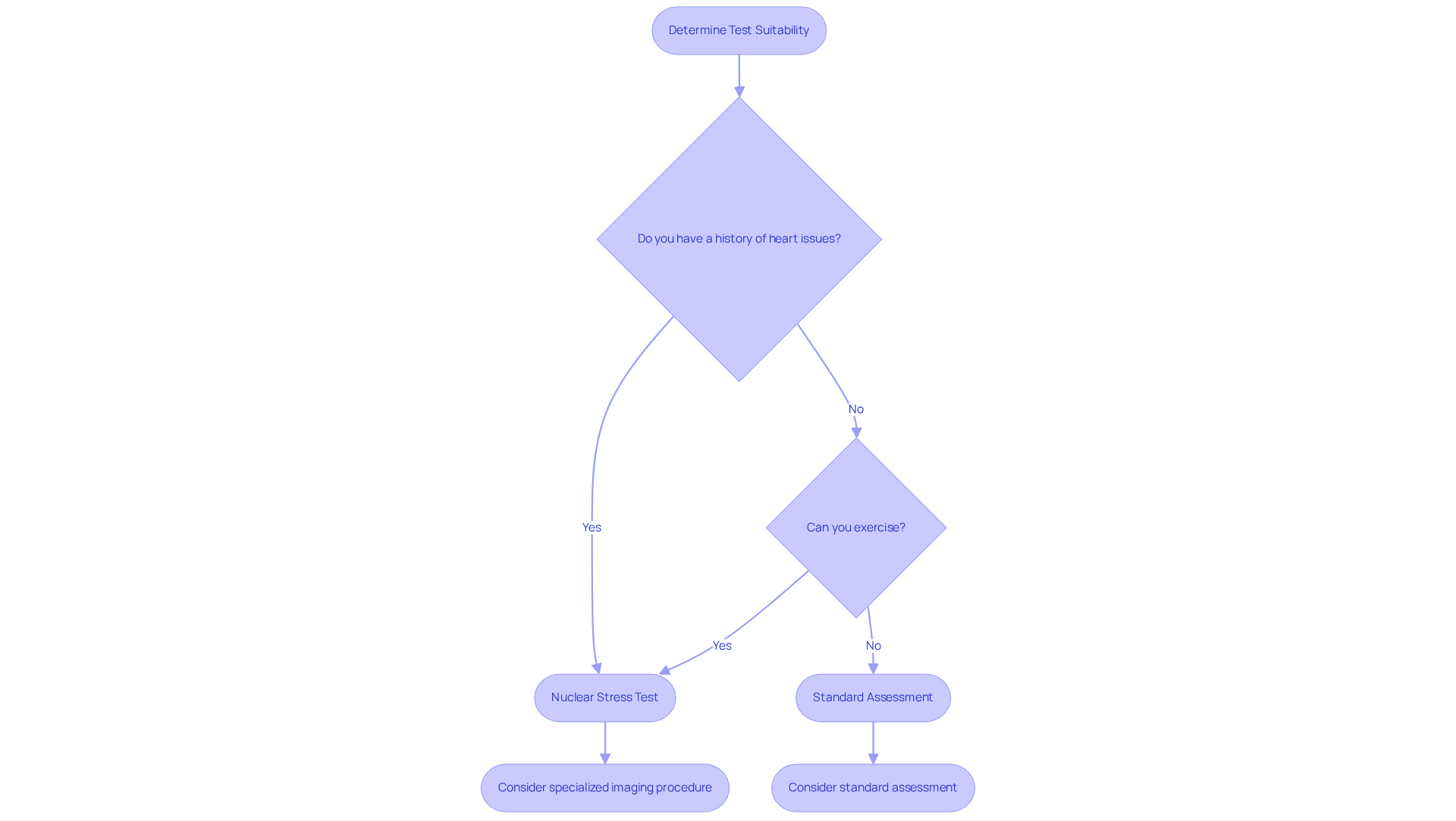
Determining Suitability: Choosing the Right Test for Individual Patient Needs
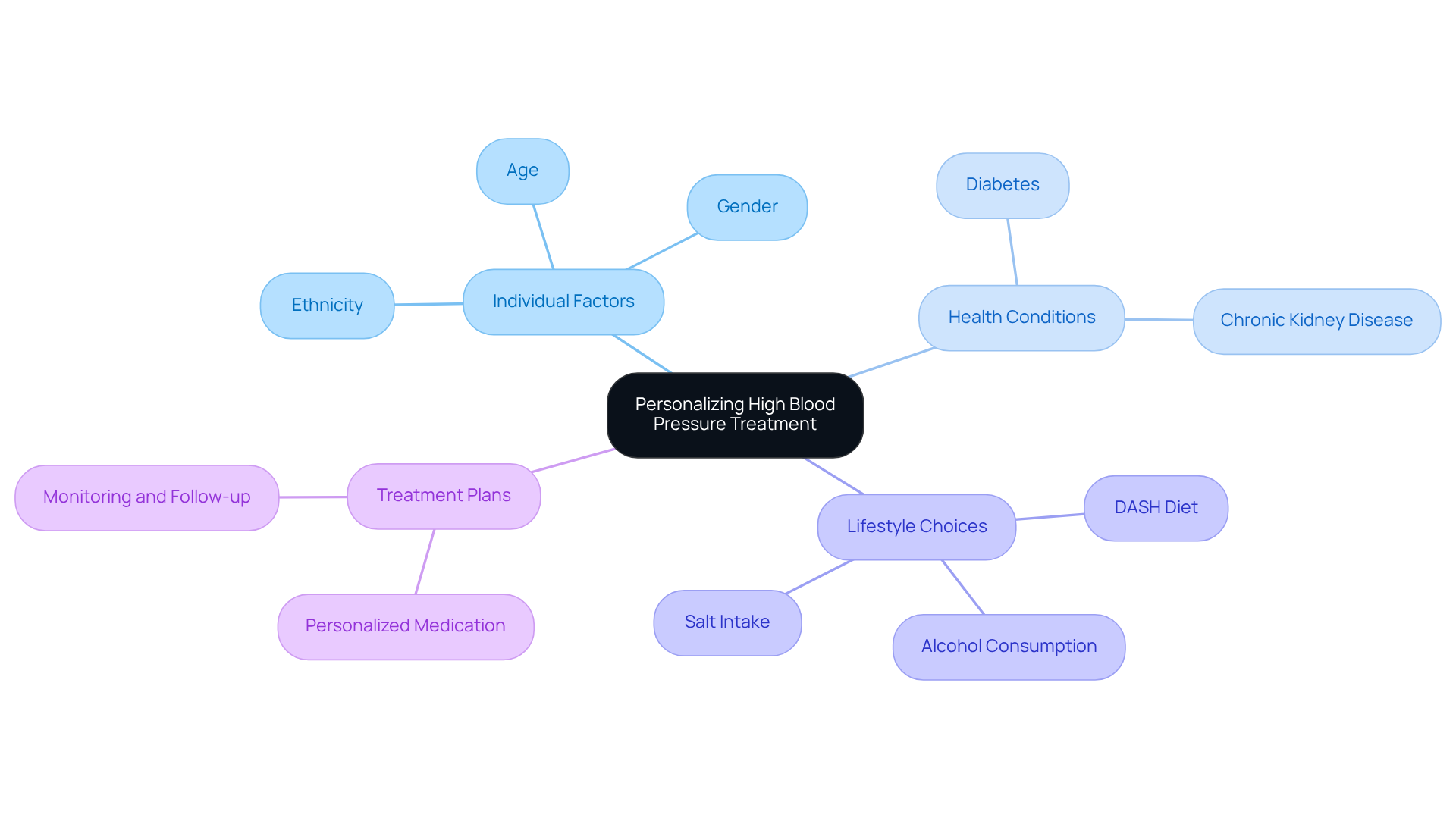
Choosing the right pressure evaluation depends on several important factors, including your medical history, symptoms, and ability to exercise, whether you opt for a nuclear stress test or a standard stress test. If you have a history of heart disease, unusual symptoms, or find it difficult to engage in physical activity, a nuclear test that assesses heart function might be more beneficial for you. On the other hand, if you’re younger or don’t have significant risk factors, a standard assessment may be sufficient for your evaluation.
Did you know that about 12.2% of patients undergo a nuclear examination within 30 days of an outpatient visit? This statistic highlights how often this method is used for those needing thorough evaluations. Additionally, studies show that individuals who can perform treadmill exercises during a standard stress test have a mortality rate of less than 1% per year. This underscores the importance of patient capability when determining the most suitable test for you.
Cardiologists emphasize the need for personalized testing. For instance, Dr. Alan Rozanski points out that nuclear tests can provide a clearer distinction between high- and low-risk individuals compared to other clinical risk factors. This tailored approach ensures that the test you undergo aligns with your health status and treatment goals, ultimately enhancing your outcomes.
Remember, you are not alone in this journey. It’s essential to have open conversations with your healthcare provider about your concerns and preferences. They are here to support you and help you make informed decisions about your health.
Conclusion
Understanding the differences between nuclear stress tests and standard stress tests is essential for making informed decisions about your heart health. Both tests aim to evaluate how your heart functions under stress, but nuclear stress tests offer a more detailed view of blood circulation. This can lead to more accurate diagnoses and better treatment outcomes, especially for those at risk for heart disease.
Nuclear stress tests stand out for their higher diagnostic accuracy, particularly in identifying coronary artery disease. They have been shown to significantly improve prognostic outcomes for individuals experiencing severe ischemia. In contrast, while standard stress tests are valuable for initial assessments, they may miss critical information in more complex cases. It’s also important to consider safety; the considerations for each test type vary, which is why personalized evaluations based on your health profile and risk factors are so important.
Ultimately, choosing between a nuclear stress test and a standard stress test should be guided by a clear understanding of your health needs and circumstances. Have you had a chance to discuss your options with your healthcare provider? Engaging in open conversations can empower you to select the most appropriate testing method, ensuring you receive the best possible care. Taking proactive steps in your heart health assessments can lead to better outcomes and a greater sense of security in managing your cardiovascular health.
Frequently Asked Questions
What is a nuclear stress test?
A nuclear stress test is a radioactive imaging procedure that evaluates blood circulation to the heart muscle during exertion and rest, using a small amount of radioactive material to generate detailed images of heart function.
How does a standard stress test differ from a nuclear stress test?
A standard stress test is typically performed on a treadmill and measures the heart’s response to physical activity without imaging. It mainly assesses heart rate, blood pressure, and electrical activity through an electrocardiogram (ECG), whereas a nuclear stress test provides a more comprehensive view of blood circulation and overall heart health.
What are the benefits of advanced imaging evaluations like nuclear stress tests?
Advanced imaging evaluations, such as nuclear stress tests, may lead to better prognostic results compared to conventional assessments. They can reveal critical information about myocardial perfusion that standard tests might miss, particularly beneficial for patients with unusual symptoms or those at higher risk for heart disease.
What is the significance of the ISCHEMIA trial in relation to stress tests?
The ISCHEMIA trial highlighted that the level of ischemia identified through advanced imaging methods is linked to significant cardiovascular events, emphasizing the importance of thorough assessments for individuals with chronic coronary syndromes.
Why should someone consider a nuclear stress test over a standard stress test?
Individuals may consider a nuclear stress test over a standard stress test because it offers a more detailed assessment of heart function and blood circulation, which can be crucial for diagnosing conditions like coronary artery disease, especially in patients with atypical symptoms or higher risk factors.
What should someone do if they have concerns about their heart health?
If someone has concerns about their heart health, they should reach out for support and understand their options, as there are compassionate professionals ready to assist them in managing their well-being.
List of Sources
- Understanding Nuclear Stress Tests and Standard Stress Tests
- tctmd.com (https://tctmd.com/news/stress-testing-picks-novel-risk-patterns-stable-cad-patients-ischemia)
- Key trends in nuclear cardiology take center stage at ASNC 2025 (https://cardiovascularbusiness.com/topics/professional-associations/cardiology-associations/american-society-nuclear-cardiology-asnc/key-trends-nuclear-cardiology-take-center-stage-asnc-2025)
- Stress cardiac MRI tests may help improve angina diagnosis and treatment (https://newsroom.heart.org/news/stress-cardiac-mri-tests-may-help-improve-angina-diagnosis-and-treatment)
- New international guideline provides expert guidance for PET imaging of patients with coronary artery disease (https://eurekalert.org/news-releases/1098834)
- Nuclear Stress Tests: What You Need to Know – ASNC (https://asnc.org/resource/nuclear-stress-tests-what-you-need-to-know)
- Comparing Effectiveness: Diagnostic Accuracy of Nuclear vs. Standard Stress Tests
- mountsinai.org (https://mountsinai.org/about/newsroom/2022/stress-testing-can-help-determine-which-patients-are-likely-to-benefit-from-heart-procedures-to-improve-survival)
- snmmi.org (https://snmmi.org/Web/Web/News/Articles/New-International-Guideline-Provides-Expert-Guidance-for-PET-Imaging-of-Patients-with-Coronary-Arter.Mobile.aspx)
- UH First Site in Ohio to Provide More Accurate and Convenient PET MPI Cardiac Stress Test (https://news.uhhospitals.org/news-releases/articles/2025/06/uh-first-site-in-ohio-to-provide-more-accurate-and-convenient-pet-mpi-cardiac-stress-test)
- Diagnostic Accuracy of Exercise Stress Testing, Stress Echocardiography, Myocardial Scintigraphy, and Cardiac Magnetic Resonance for Obstructive Coronary Artery Disease: Systematic Reviews and Meta-Analyses of 104 Studies Published from 1990 to 2025 (https://mdpi.com/2077-0383/14/17/6238)
- Dr. Roach: Nuclear stress test is better diagnostic option for heart disease (https://detroitnews.com/story/life/advice/2020/10/16/keith-roach-nuclear-stress-test-better-diagnostic-option-heart-disease/114396246)
- Evaluating Safety: Risks and Considerations for Each Test Type
- FDA warns of rare but serious risk of heart attack and death with c… (https://fda.gov/drugs/drug-safety-and-availability/fda-warns-rare-serious-risk-heart-attack-and-death-cardiac-nuclear-stress-test-drugs-lexiscan)
- Nuclear Stress Test Safety for Seniors: Should a 70-Year-Old Have One? – Liv Hospital (https://int.livhospital.com/nuclear-stress-test-safety-for-seniors-over-70)
- Is a Nuclear Stress Test Safe for Elderly People? (https://healthline.com/health/is-nuclear-stress-test-safe-for-elderly)
- A nuclear threat to heart patients? U-M experts show impact from shortage of radioactive stress test tracer (https://ihpi.umich.edu/news/nuclear-threat-heart-patients-u-m-experts-show-impact-shortage-radioactive-stress-test-tracer)
- Determining Suitability: Choosing the Right Test for Individual Patient Needs
- A Patient’s Ability to Perform a Cardiac Stress Test Offers a Critical Window on Their Mortality Risk (https://mountsinai.org/about/newsroom/2025/a-patients-ability-to-perform-a-cardiac-stress-test-offers-a-critical-window-on-their-mortality-risk)
- medicalxpress.com (https://medicalxpress.com/news/2025-02-patient-ability-cardiac-stress-critical.html)
- Do you really need that test? New statement highlights need to reduce “low-value” heart care (https://newsroom.heart.org/news/do-you-really-need-that-test)
- Association Between Physician Billing and Cardiac Stress Testing Patterns Following Coronary Revascularization (https://jamanetwork.com/journals/jama/fullarticle/1104608)