Introduction
Feeling your heart race unexpectedly can be alarming, leaving you anxious about what it means for your health. With caffeine being a common trigger, understanding how long these sensations can last and their implications for heart health is crucial.
Let’s explore how long these sensations can last and what they might mean for your heart health. This article offers a practical checklist to help you monitor your symptoms effectively.
Recognizing the difference between normal reactions and those needing medical attention can empower you to take charge of your heart health.
Define Heart Palpitations and Their Symptoms
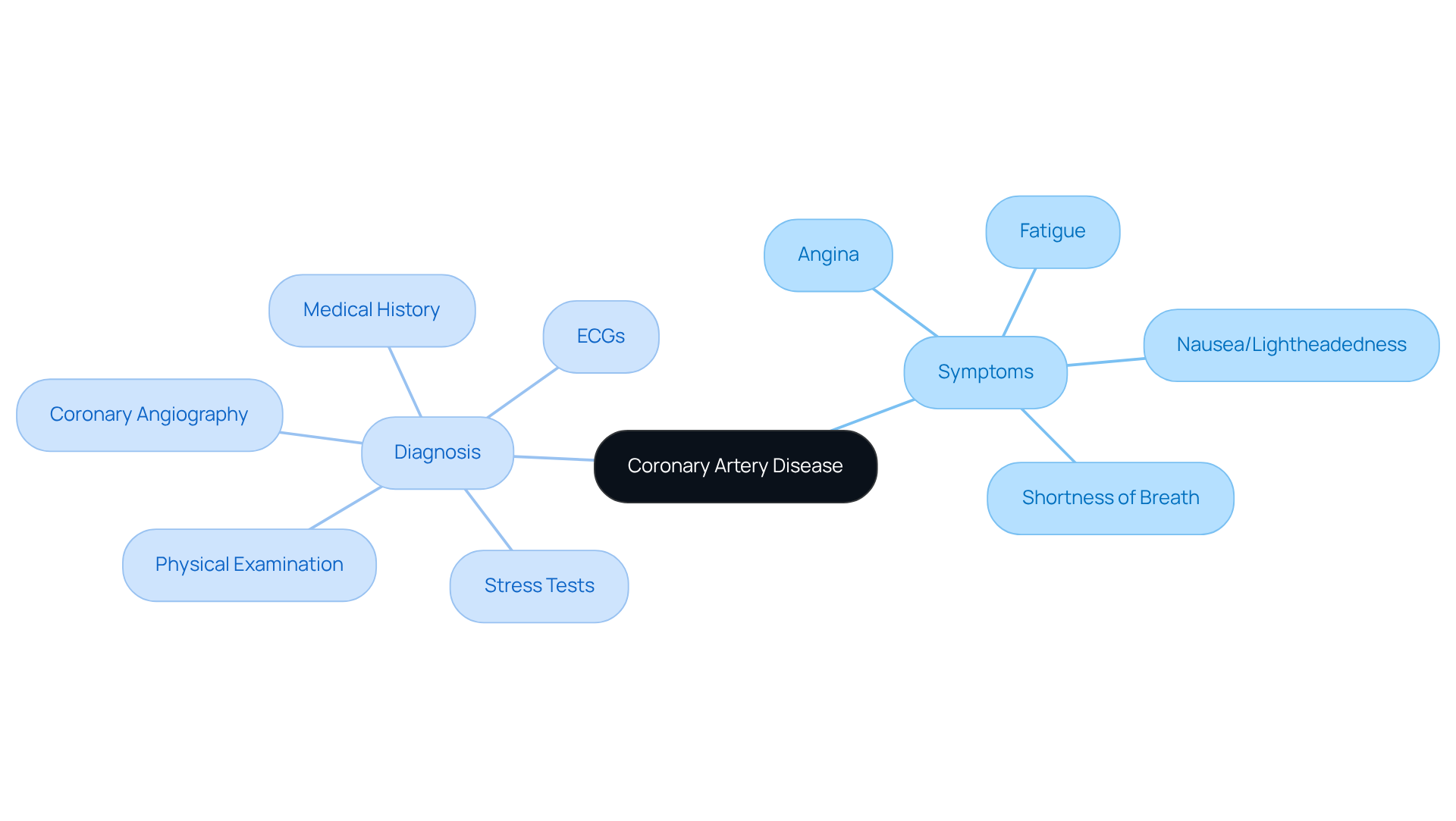
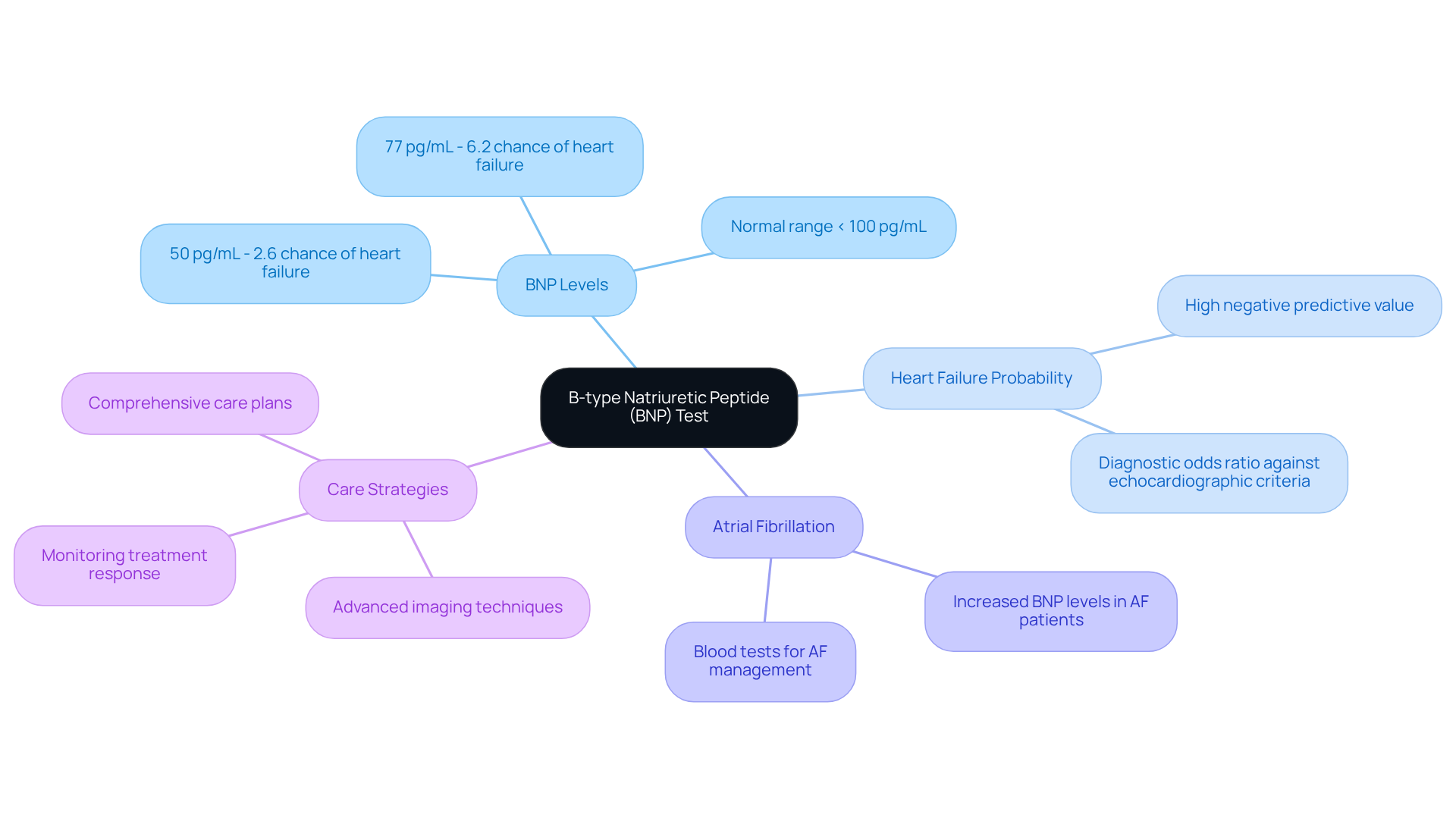
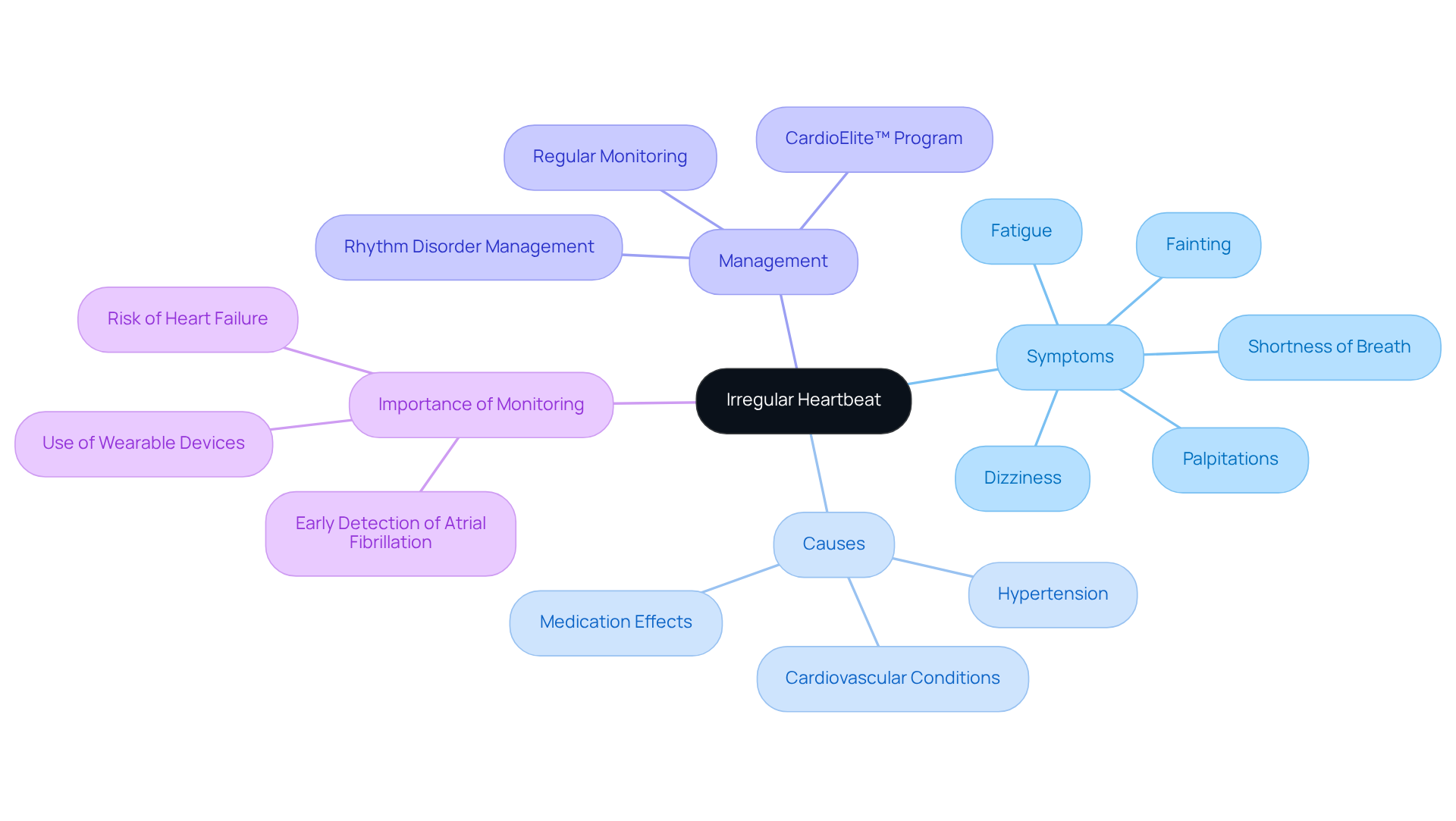
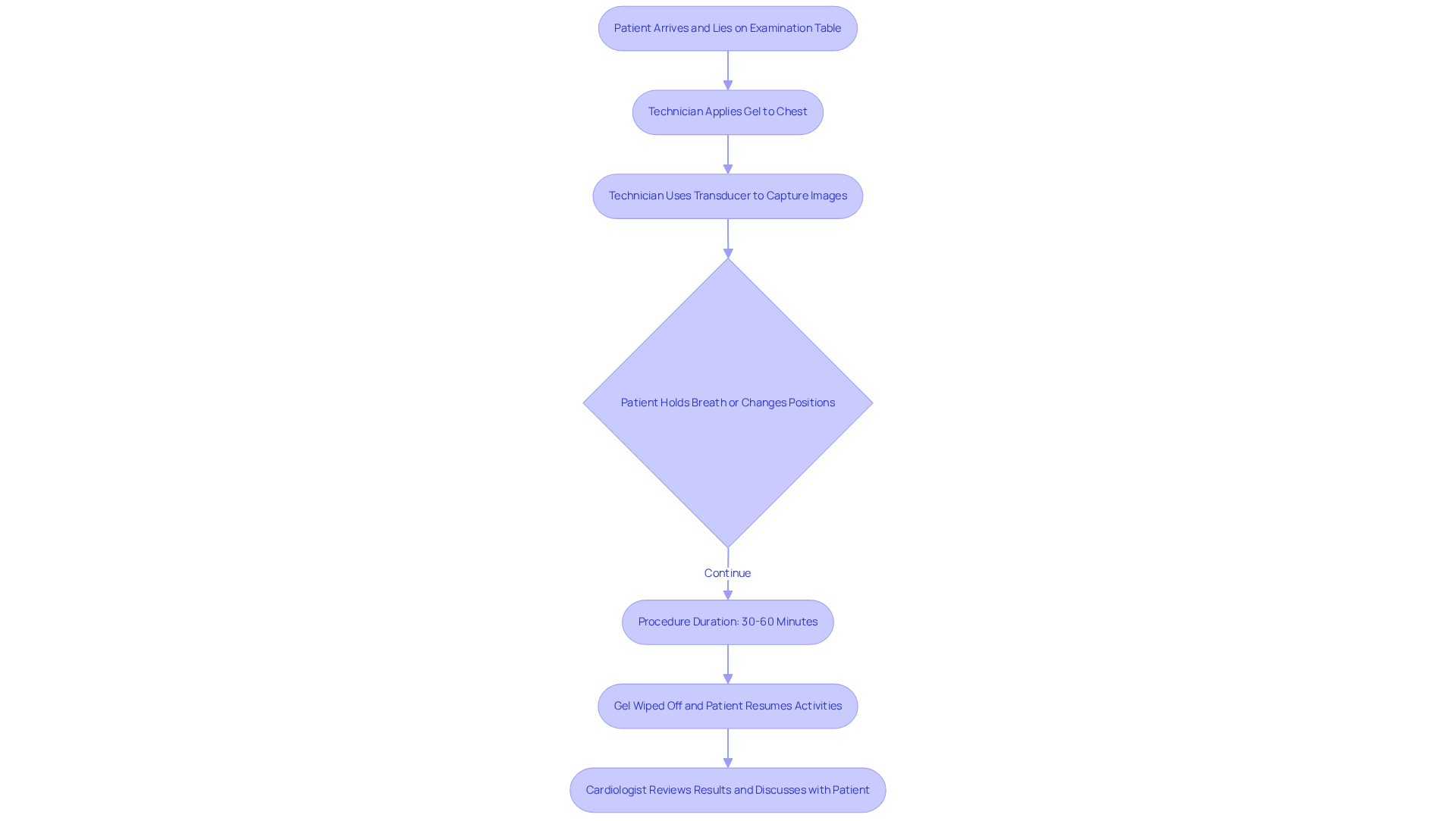
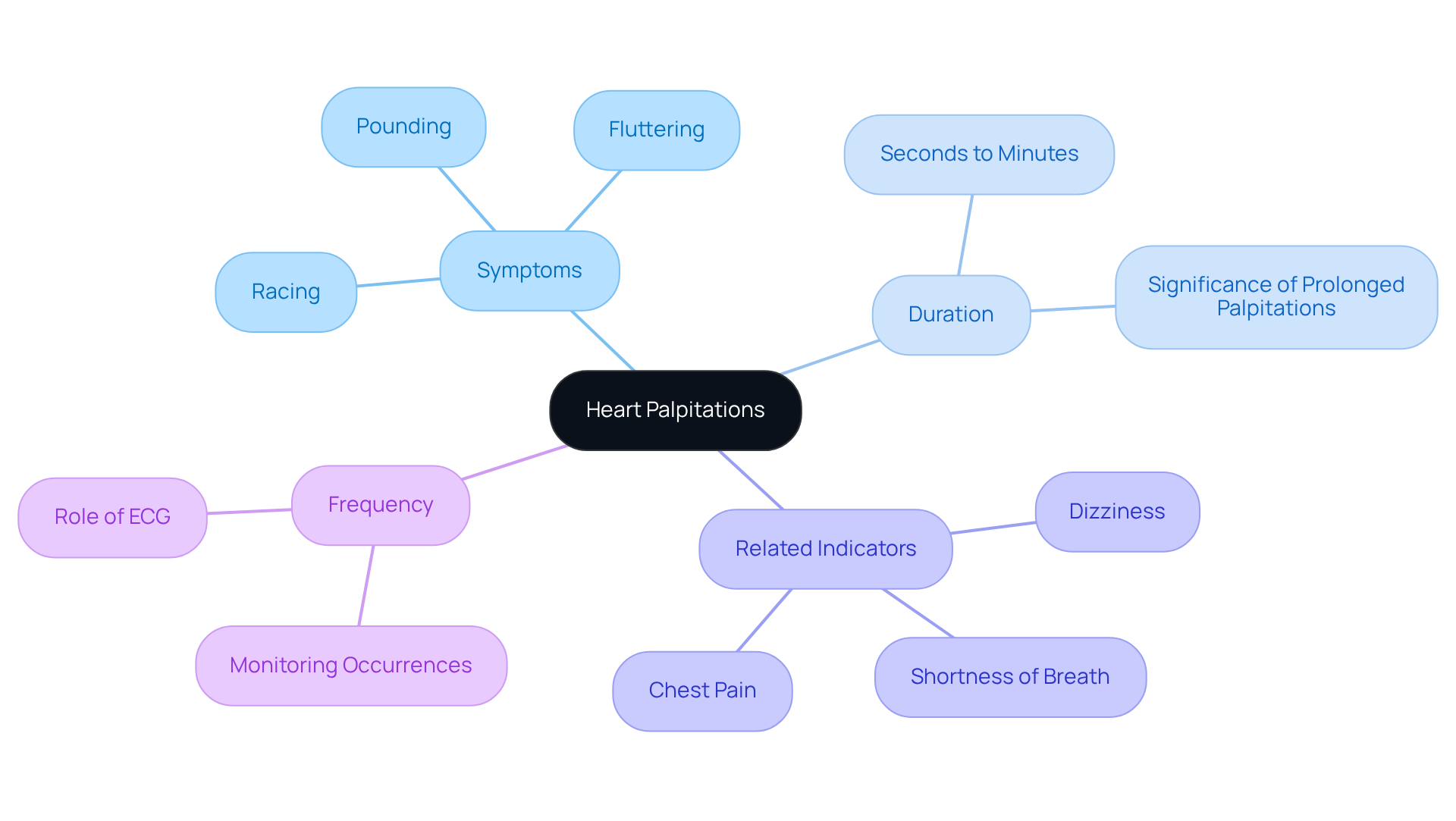
Experiencing a racing or fluttering sensation in your chest can be alarming, and it’s essential to understand what it might mean for your heart health. Palpitations can feel like a pounding sensation, often perceived in the chest, throat, or neck. Recognizing these sensations is crucial, as they may indicate an underlying heart problem, affecting approximately 8.3% of individuals in a studied population. At Amavita Heart & Vascular Health, our specialists are here to help diagnose and manage these signs effectively.
- Duration: When considering how long heart palpitations can last from caffeine, they can range from a few seconds to several minutes. Jotting down how long heart palpitations last from caffeine during these episodes can greatly assist your healthcare provider in understanding your situation better. If an irregular heartbeat continues for more than 30 seconds, it may indicate a more severe issue, such as coronary artery disease, that needs prompt assessment.
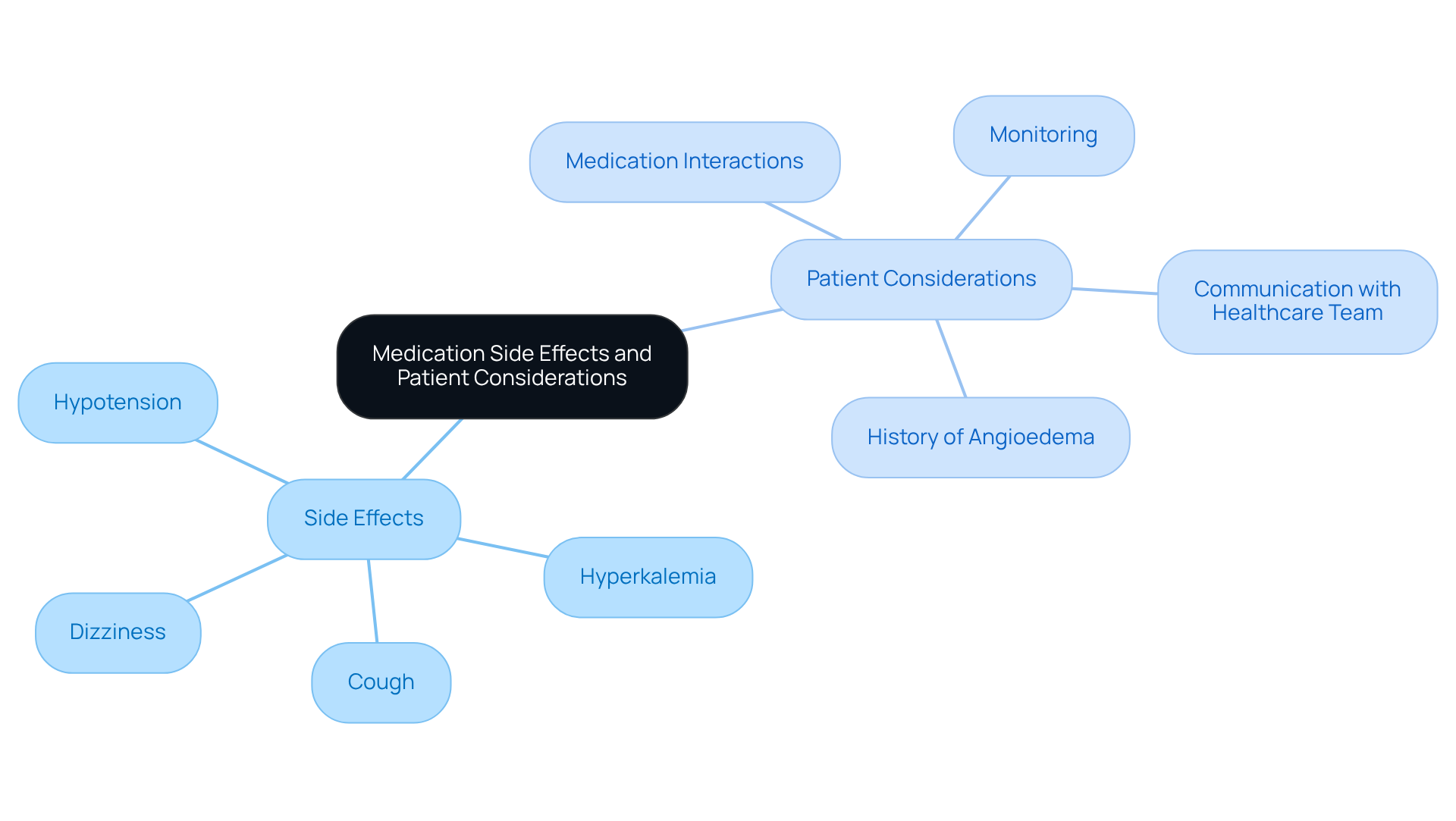
- Related Indicators: Pay attention to any accompanying signs such as dizziness, shortness of breath, or chest pain. These may indicate a more serious underlying condition, including coronary artery disease, that requires immediate medical attention. As stated by specialists at Amavita, symptoms such as chest discomfort along with an irregular heartbeat require immediate attention, as they may signify a cardiac event.
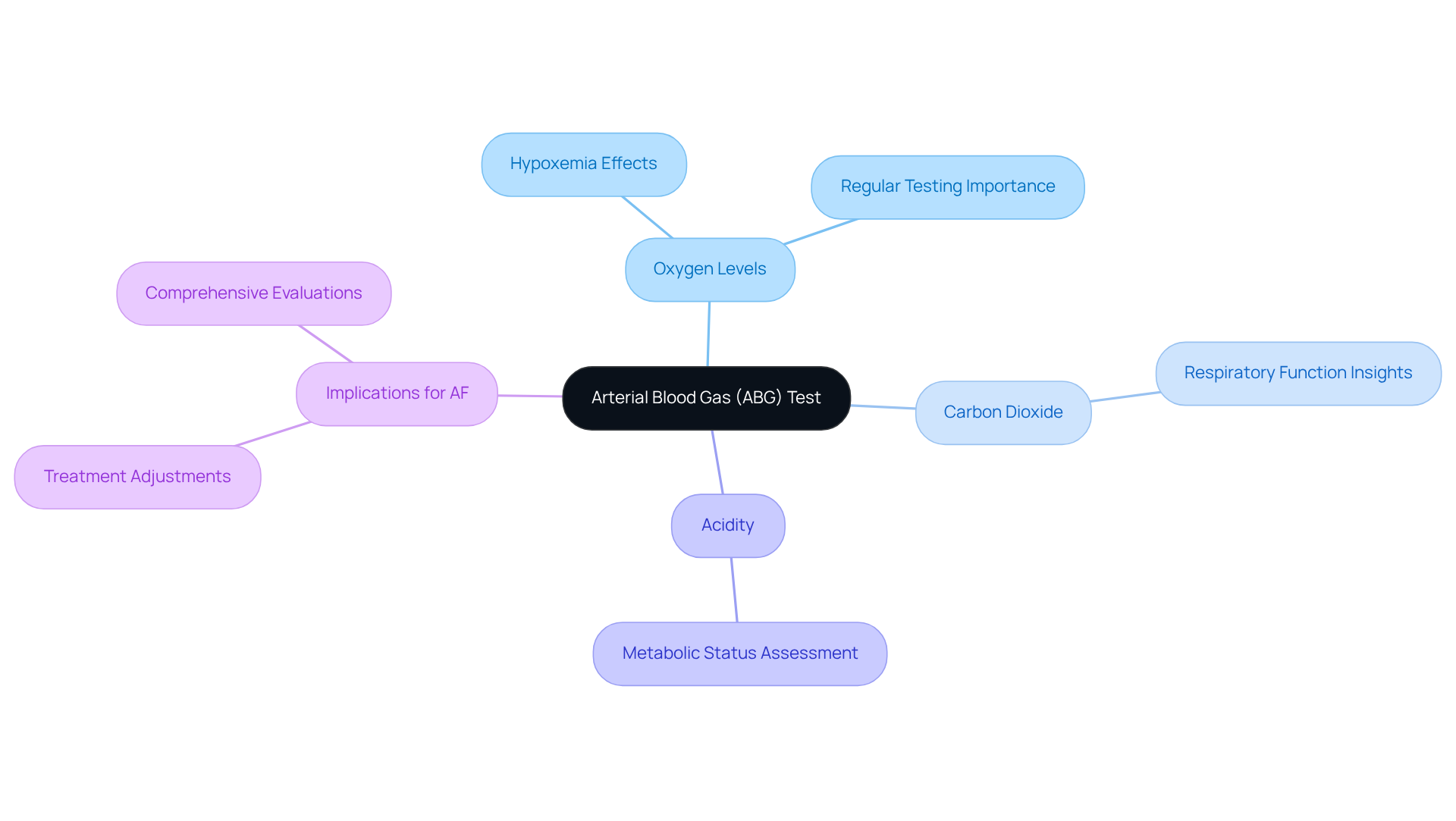
- Frequency: Monitoring how often you experience these heartbeats can help evaluate their importance. Frequent occurrences may warrant further evaluation to rule out potential heart issues. An electrocardiogram (ECG) is often suggested as soon as possible after irregular heartbeats start to diagnose any arrhythmias effectively. Our comprehensive arrhythmia management approach ensures that patients receive timely and effective care, utilizing advanced diagnostic technologies to enhance patient outcomes. Taking these symptoms seriously can lead to timely care and peace of mind, ensuring your heart health is in good hands.
Understand Caffeine’s Impact on Heart Palpitations
Have you ever felt your heart racing after enjoying a cup of coffee? You’re not alone, and it’s important to understand how caffeine affects you personally. Individual tolerance to caffeine can vary significantly. If you notice your heart racing after having caffeine, consider cutting back a bit to see if that helps you feel better.
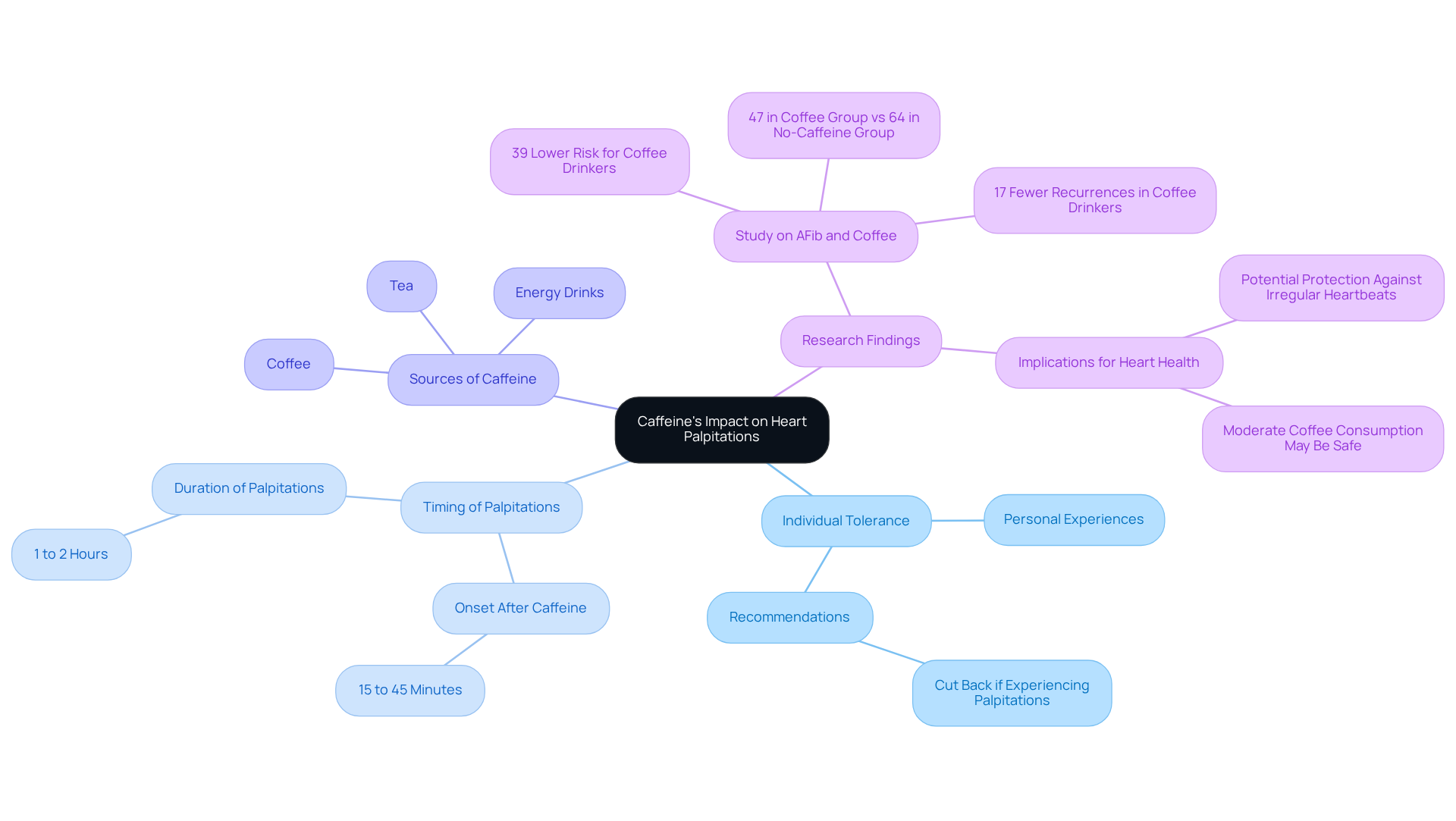
After consuming caffeine, palpitations typically occur 15 to 45 minutes later, raising the question of how long can heart palpitations last from caffeine, as they can persist for 1 to 2 hours. Paying attention to how your body reacts during this time can really help you understand your own sensitivity to caffeine.
Different sources of caffeine, like coffee, tea, and energy drinks, can affect your heart in various ways. Keeping a little journal about what you drink and how it makes you feel can be a great way to spot any triggers.
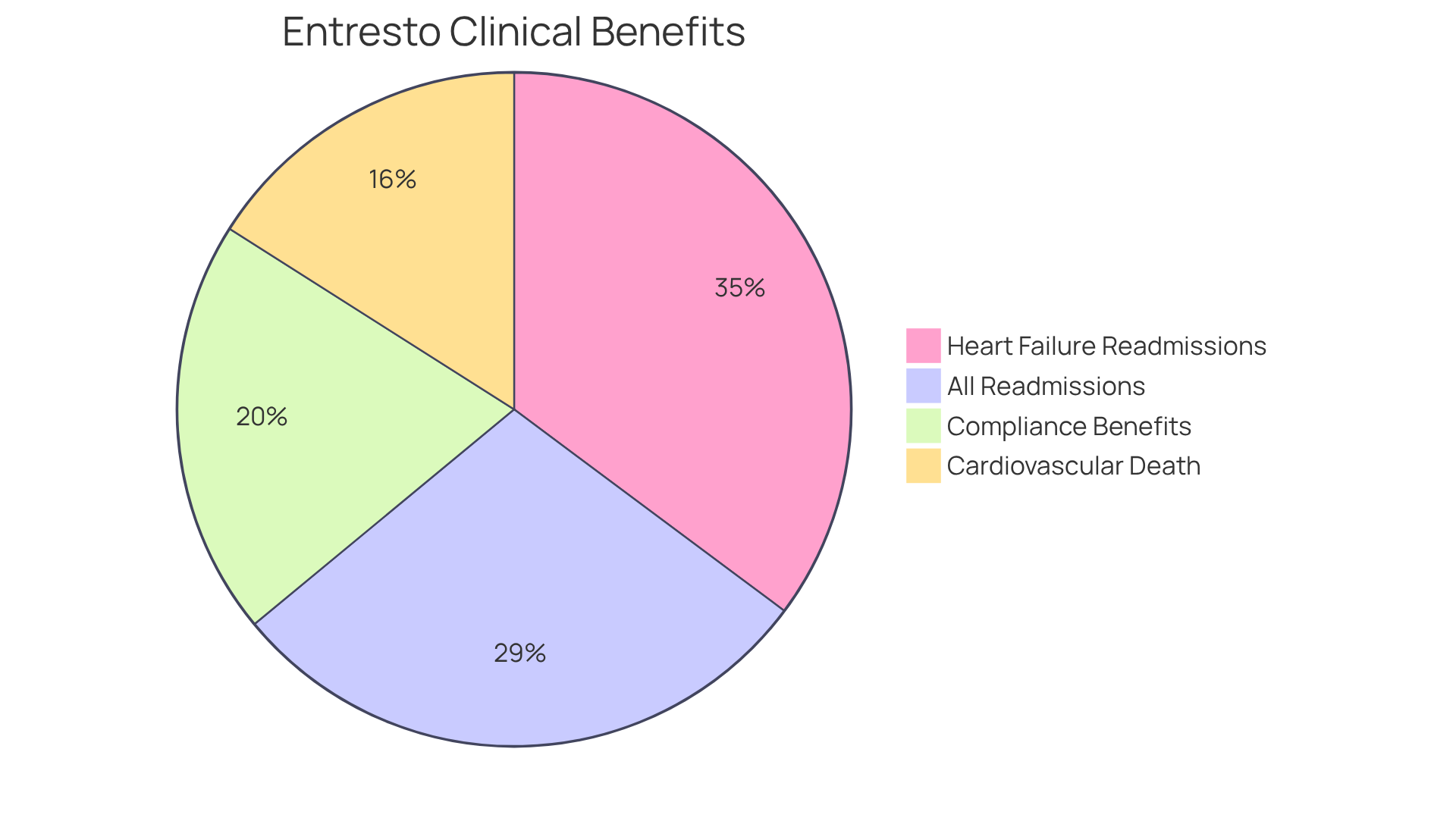
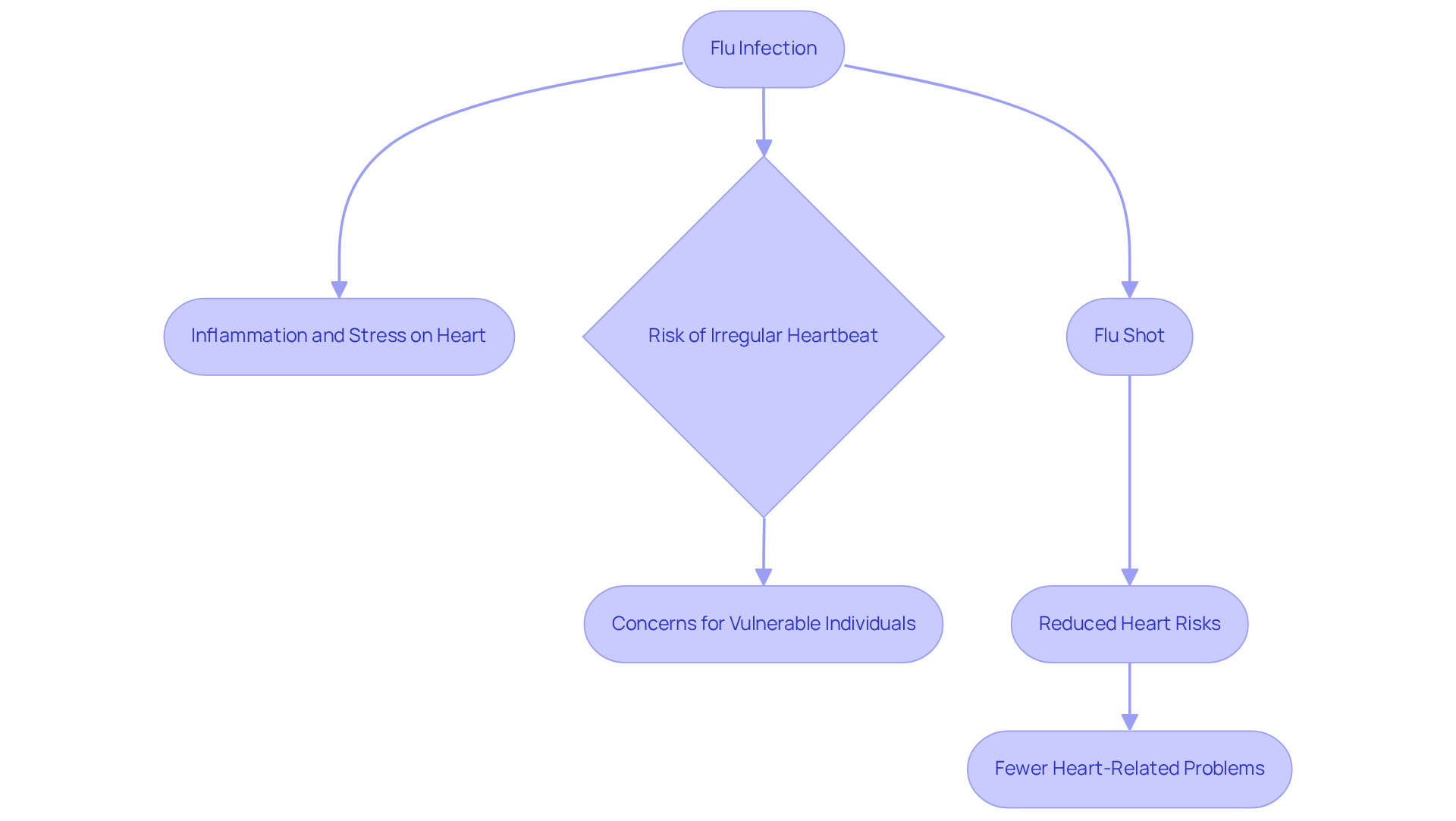
Research suggests that too much caffeine can make your heart race, especially if you’re sensitive to it. For instance, a study involving 200 adults diagnosed with atrial fibrillation found that those who consumed coffee had a 39% lower risk of experiencing recurrent irregular heartbeats compared to those who abstained. Interestingly, 64% of participants in the no-caffeine group experienced recurrent AFib episodes lasting more than 30 seconds. This implies that moderate coffee intake may not be detrimental and could even offer protection against irregular pulse patterns. Understanding your body’s response to caffeine can empower you to make choices that support your heart health and overall well-being.
Monitor Duration and Frequency of Palpitations
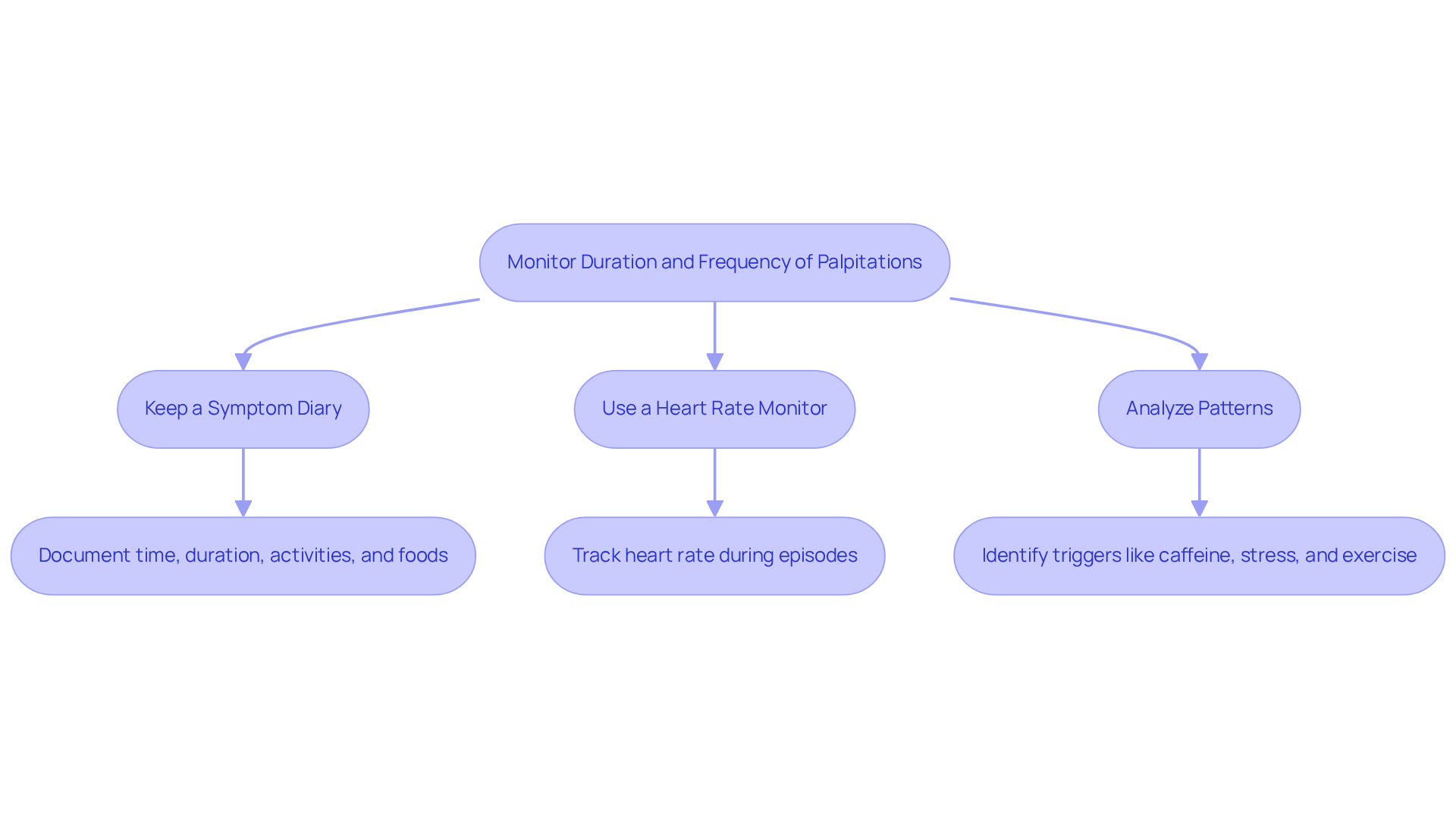
Experiencing palpitations can be unsettling, leaving many to wonder about their heart health and what steps to take next. Keeping a symptom diary can be a helpful first step. Document each episode of palpitations, including the time, duration, and any related activities or foods consumed. This practice is crucial for identifying potential triggers and patterns. We understand how important it is to monitor your symptoms, and we’re here to support you every step of the way.
In addition to this, using a heart rate monitor can provide valuable insights. Employ a wearable device to track your heart rate during episodes. These devices can offer critical data that helps healthcare providers understand your condition better. Our caring team will use this information to create a treatment plan that feels right for you, leveraging advanced technology for accurate diagnosis.
Furthermore, take time to analyze your diary entries for patterns. Are heart sensations more common after caffeine consumption, during stressful circumstances, or after exercising, particularly in relation to how long can heart palpitations last from caffeine? Recognizing these triggers can significantly assist in managing your symptoms. “Understanding your triggers is key to effective management of heart sensations,” emphasizes Dr. Pedro Martinez-Clark, a leading cardiologist at Amavita. Our team is committed to assisting you in recognizing these patterns to improve your cardiovascular health.
If you experience frequent or prolonged heartbeats, it’s important to consult with a professional. Share your findings with a healthcare provider for a thorough evaluation and tailored advice. Engaging with your healthcare team at Amavita can lead to better management strategies and improved outcomes, ensuring you receive the innovative care you deserve, often with the convenience of same-day procedures. Taking these steps not only empowers you but also brings you closer to a healthier heart and peace of mind.
Know When to Consult a Healthcare Professional
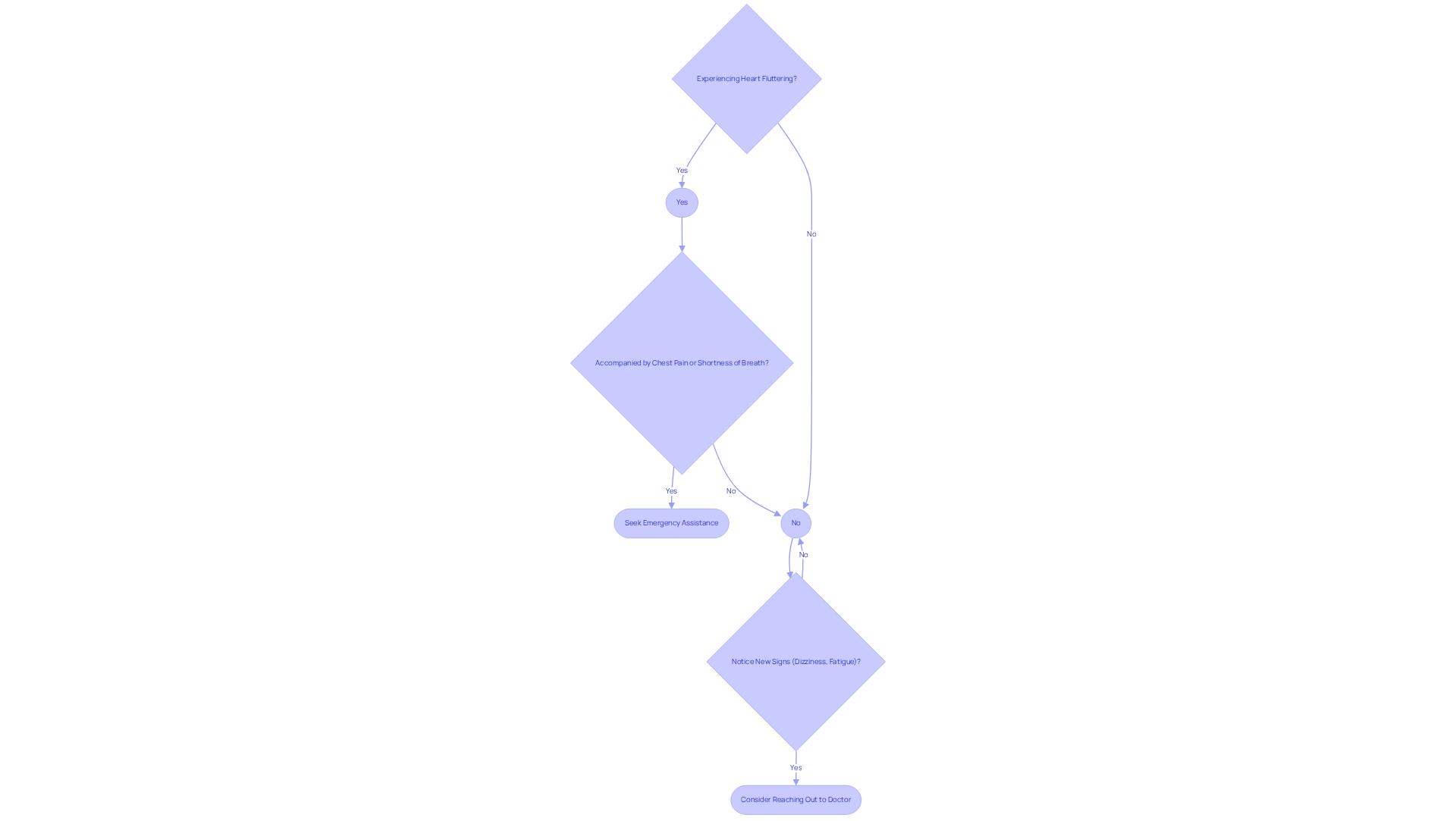
Experiencing heart fluttering can be unsettling, especially when accompanied by chest pain or shortness of breath. Please don’t hesitate to seek emergency medical assistance if you feel this way.
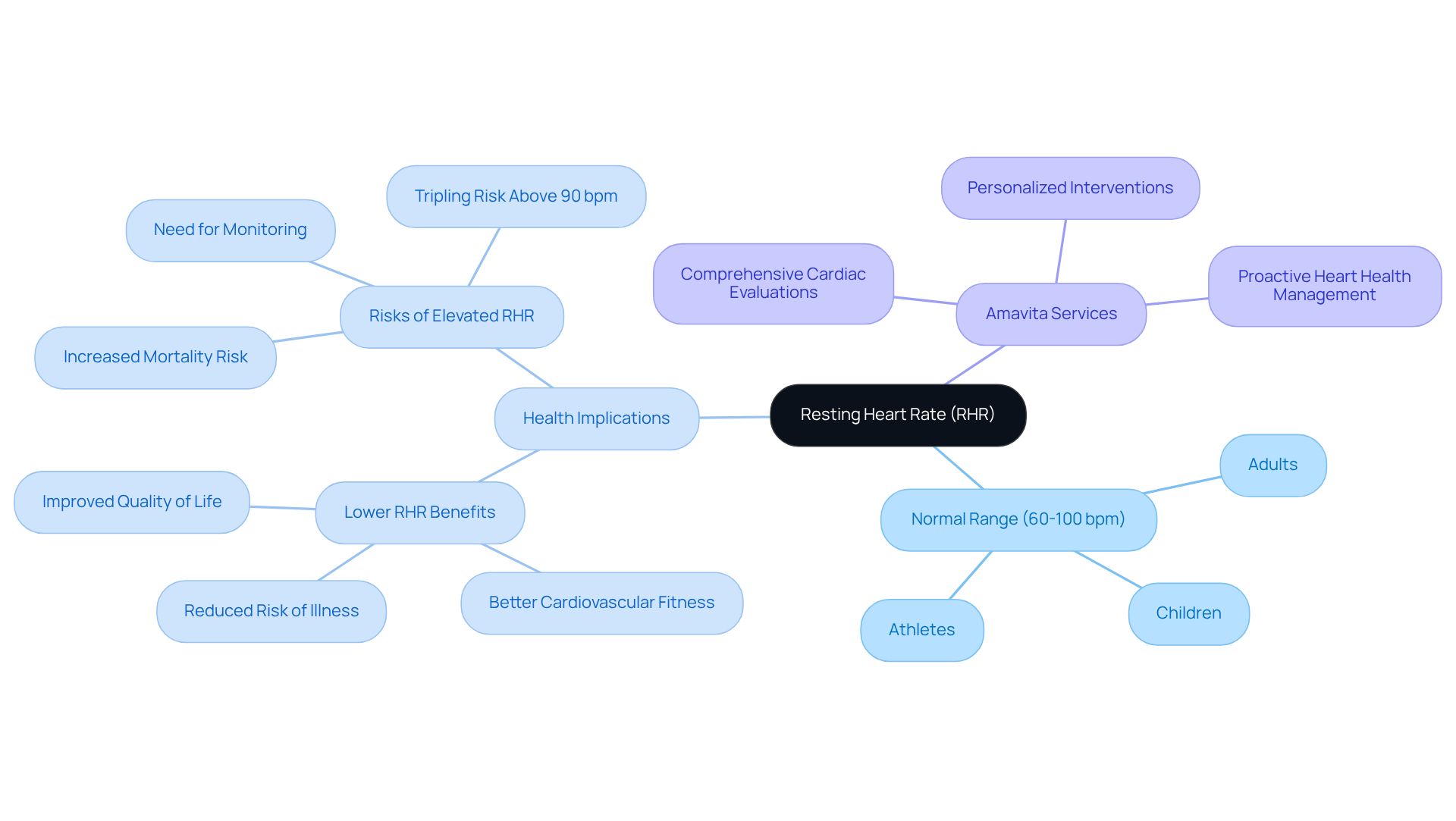
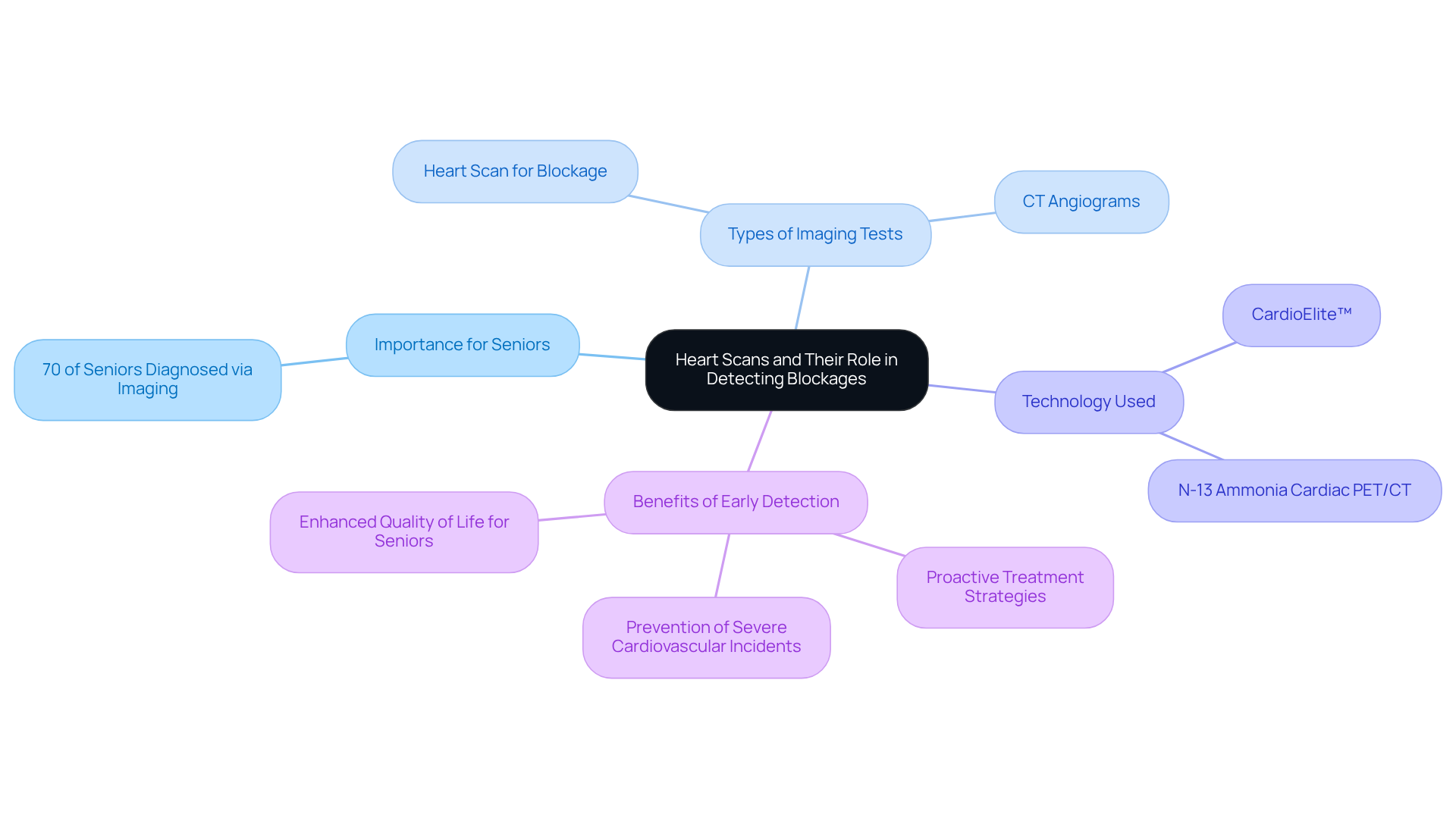
It’s important to know that many people experience palpitations, leading to around 684,000 emergency visits each year. If you’re feeling this way, it’s a good idea to talk to someone who can help. At Amavita Heart & Vascular Health, we’re here to provide comprehensive cardiac evaluations, including advanced imaging and testing, to assess your heart health and identify any potential risks.
Should you notice new signs like dizziness or unusual fatigue, please consider reaching out to your doctor. It’s always better to be safe and get the support you need. Our preventive cardiology approach combines advanced risk assessment tools with personalized interventions to help manage these symptoms effectively.
As we age, especially after 50, it’s common to face more heart rhythm challenges. Regular check-ups can help us stay ahead of any issues. At Amavita, we believe that cardiac care should be designed around your life, not just your condition.
If you find that irregular heartbeats are occurring frequently or lasting longer than normal, it’s crucial to consider how long can heart palpitations last from caffeine and consult a healthcare professional. Your well-being is our priority. Dr. Farid emphasizes that persistent palpitations affecting quality of life should prompt a visit to a healthcare provider for further evaluation and management. Our team is dedicated to providing innovative and compassionate cardiovascular care tailored to your specific needs, including minimally invasive treatments and outpatient services.
Conclusion
Many people worry when they experience heart palpitations, especially after consuming caffeine. Understanding how long these palpitations can last and their potential impact is essential for maintaining heart health. By recognizing your symptoms and knowing when to reach out for help, you can take charge of your heart health. The insights shared here emphasize the importance of monitoring your symptoms, their frequency, and any triggers related to caffeine intake, ultimately guiding you toward informed decisions about your cardiovascular well-being.
Key points to remember include that palpitations can vary in duration, lasting anywhere from seconds to hours after caffeine consumption. It’s also important to pay attention to any accompanying symptoms that might suggest a more serious issue. Keeping a symptom diary or using a heart rate monitor can help you identify patterns and triggers, leading to more effective management strategies. Engaging with healthcare professionals is crucial, especially if you experience persistent or concerning symptoms, to ensure you receive timely care and support.
Have you thought about how your caffeine intake affects your heart? Being proactive about your heart health is vital. Reflect on your caffeine consumption, monitor how your body responds, and don’t hesitate to consult with your healthcare provider when needed. Taking these steps can empower you to make choices that truly enhance your heart health and overall well-being.
Frequently Asked Questions
What are heart palpitations and how do they feel?
Heart palpitations are sensations of a racing or fluttering feeling in the chest, throat, or neck. They can feel like a pounding sensation and may indicate an underlying heart problem.
How common are heart palpitations?
Heart palpitations affect approximately 8.3% of individuals in the studied population.
How long can heart palpitations last, particularly from caffeine?
Heart palpitations from caffeine can last from a few seconds to several minutes. If an irregular heartbeat continues for more than 30 seconds, it may indicate a more severe issue that requires assessment.
What accompanying signs should I watch for with heart palpitations?
Accompanying signs to watch for include dizziness, shortness of breath, or chest pain. These may indicate a more serious condition that requires immediate medical attention.
How often should I experience heart palpitations before seeking further evaluation?
Frequent occurrences of heart palpitations may warrant further evaluation to rule out potential heart issues.
What diagnostic tests are recommended for heart palpitations?
An electrocardiogram (ECG) is often suggested as soon as possible after irregular heartbeats start to diagnose any arrhythmias effectively.
Why is it important to take heart palpitations seriously?
Taking heart palpitations seriously can lead to timely care and peace of mind, ensuring that any potential heart issues are addressed promptly.
List of Sources
- Define Heart Palpitations and Their Symptoms
- Know When to Worry About Heart Palpitations (https://healthline.com/health/heart/when-to-worry-about-heart-palpitations)
- Heart palpitations-Heart palpitations – Symptoms & causes – Mayo Clinic (https://mayoclinic.org/diseases-conditions/heart-palpitations/symptoms-causes/syc-20373196)
- When heart palpitations signal a more serious problem | HCA Houston Healthcare (https://hcahoustonhealthcare.com/healthy-living/blog/when-heart-palpitations-signal-a-serious-problem)
- Prevalence of palpitations, cardiac arrhythmias and their associated risk factors in ambulant elderly – PubMed (https://pubmed.ncbi.nlm.nih.gov/8818746)
- How serious are heart palpitations? Causes, symptoms and when to worry (https://heart.org/en/news/2026/02/09/how-serious-are-heart-palpitations-causes-symptoms-and-when-to-worry)
- Understand Caffeine’s Impact on Heart Palpitations
- Scientists Find This Popular Drink May Reduce Your Risk of Serious Heart Condition (https://prevention.com/food-nutrition/a70832180/coffee-safe-atrial-fibrillation-study)
- Coffee may protect people against irregular heartbeats, study finds (https://theguardian.com/us-news/2025/nov/10/coffee-irregular-heartbeat-protection-study)
- Daily coffee may reduce recurrence of irregular heart rhythms, study shows (https://wcnc.com/article/news/local/connect-the-dots/daily-coffee-irregular-heart-rhythms-study/275-27c4ea98-ad02-44b9-b627-e3928c4916d7)
- Coffee may protect against irregular heartbeats (https://nbcnews.com/health/heart-health/coffee-may-help-protect-against-afib-study-finds-rcna242576)
- Cup of coffee a day may not be harmful for some adults with AFib and could lower episodes (https://newsroom.heart.org/news/cup-of-coffee-a-day-may-not-be-harmful-for-some-adults-with-afib-and-could-lower-episodes)
- Monitor Duration and Frequency of Palpitations
- Monitoring for individual triggers may reduce episodes of atrial fibrillation (https://newsroom.heart.org/news/monitoring-for-individual-triggers-may-reduce-episodes-of-atrial-fibrillation)
- Wearable Medical Devices Statistics and Facts (2026) (https://media.market.us/wearable-medical-devices-statistics)
- A guide to consumer-grade wearables in cardiovascular clinical care and population health for non-experts – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC12404996)
- Abstract 15892: Symptom Diary Use Improves Outcomes for Heart Failure Patients | Circulation (https://ahajournals.org/doi/10.1161/circ.132.suppl_3.15892)
- Press Releases – HRS (https://hrsonline.org/advocacy-news/news-library/press-releases)
- Know When to Consult a Healthcare Professional
- When to Go to the Doctor for Heart Palpitations – UnityPoint Health (https://unitypoint.org/news-and-articles/when-to-go-to-the-doctor-for-heart-palpitations)
- When Heart Palpitations Are an Emergency (https://webmd.com/heart-disease/heart-palpitations-emergency)
- Analysis of Emergency Department Visits for Palpitations (From the National Hospital Ambulatory Medical Care Survey) – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC4011931)
- When Should You Worry About Heart Palpitations? (https://tuftsmedicine.org/about-us/news/when-should-you-worry-about-heart-palpitations)
- When to go to the doctor for heart palpitations (https://vcuhealth.org/news/when-to-go-to-the-doctor-for-heart-palpitations)