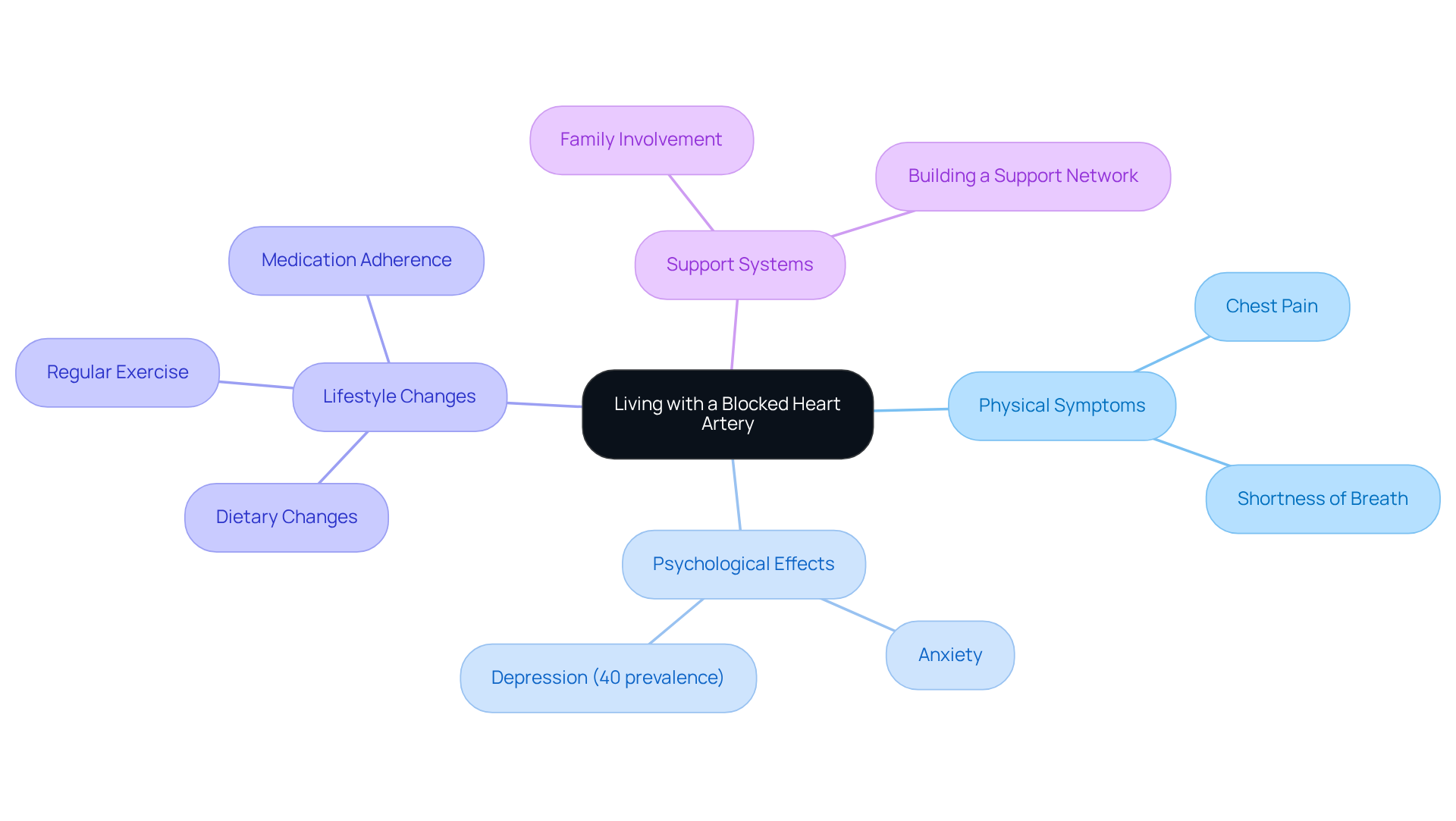
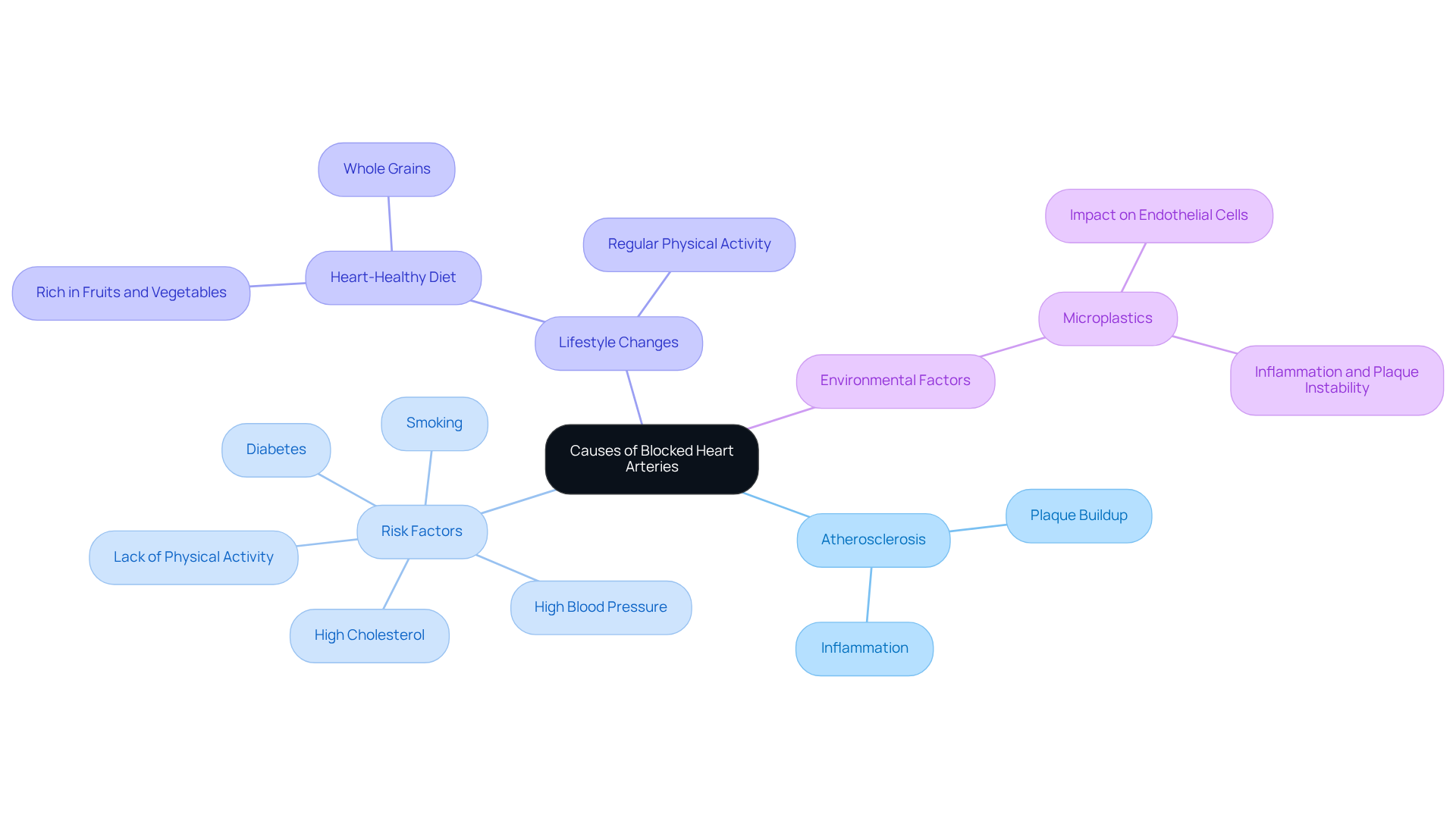
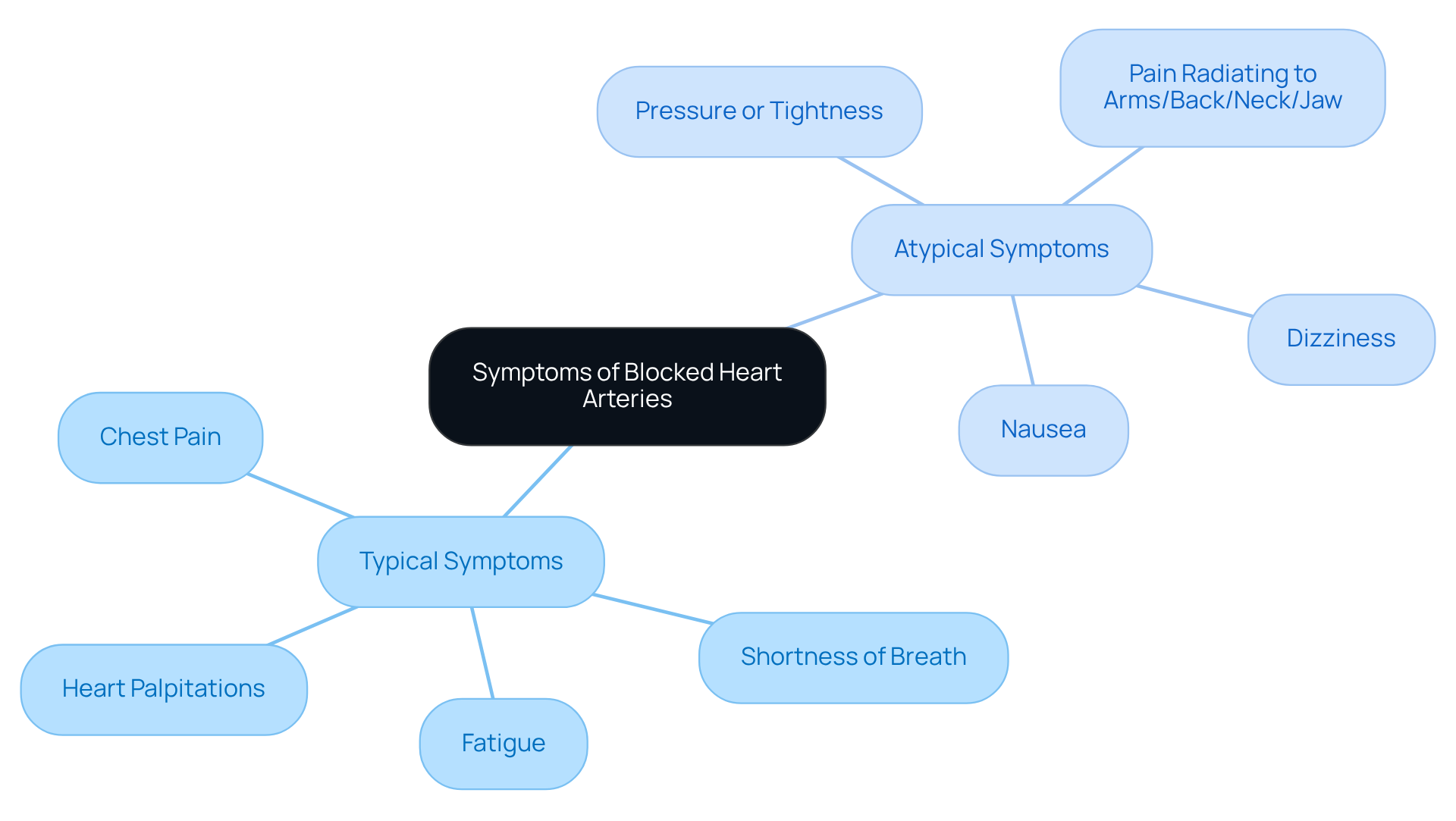
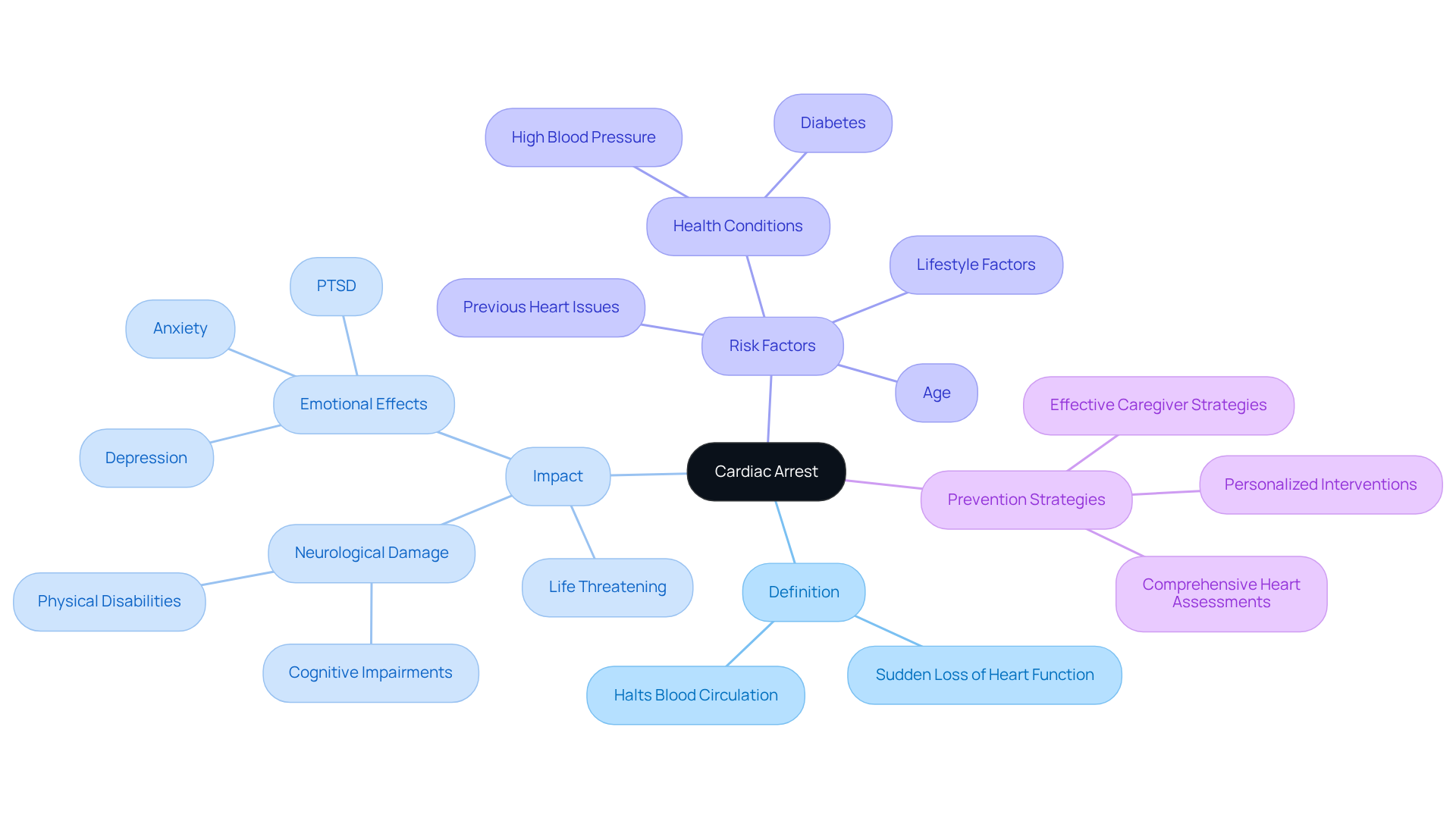
Introduction
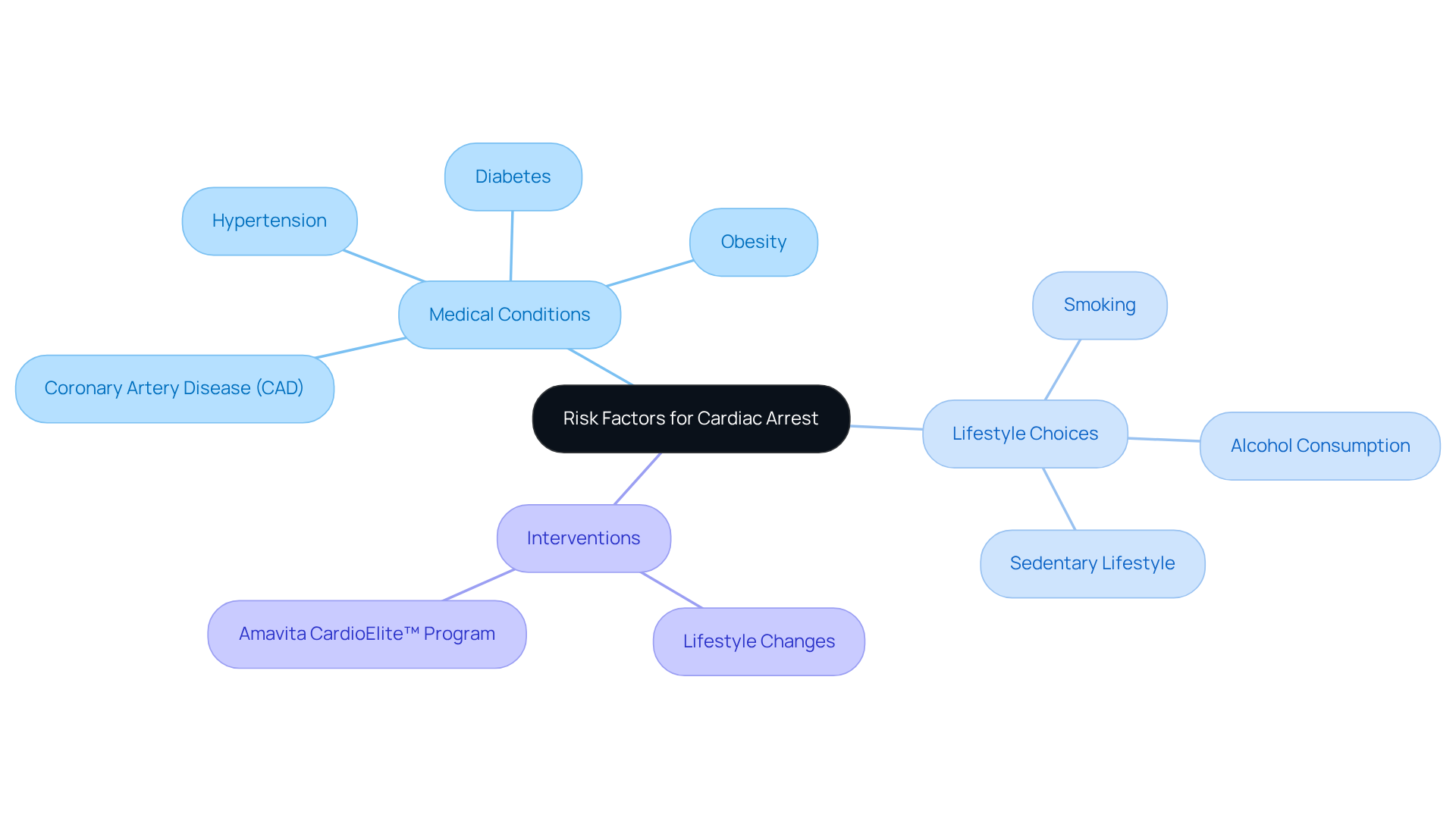
Understanding heart health is essential, and the calcium score serves as a pivotal indicator of cardiovascular well-being. By measuring the calcified plaque in coronary arteries through a specialized CT scan, this score provides critical insights into the risk of atherosclerosis and potential heart disease.
But what does a calcium score truly reveal about your heart health? How can it shape your preventive strategies? These questions are important, and the answers could be the key to a healthier future, helping to mitigate the risks of serious heart conditions.
In addition to this, knowing your calcium score can empower you to take proactive steps towards better heart health. It’s not just about numbers; it’s about understanding your body and making informed choices. Remember, you’re not alone in this journey. Seeking support and guidance can make all the difference.
Define Calcium Score: What It Measures and Its Importance
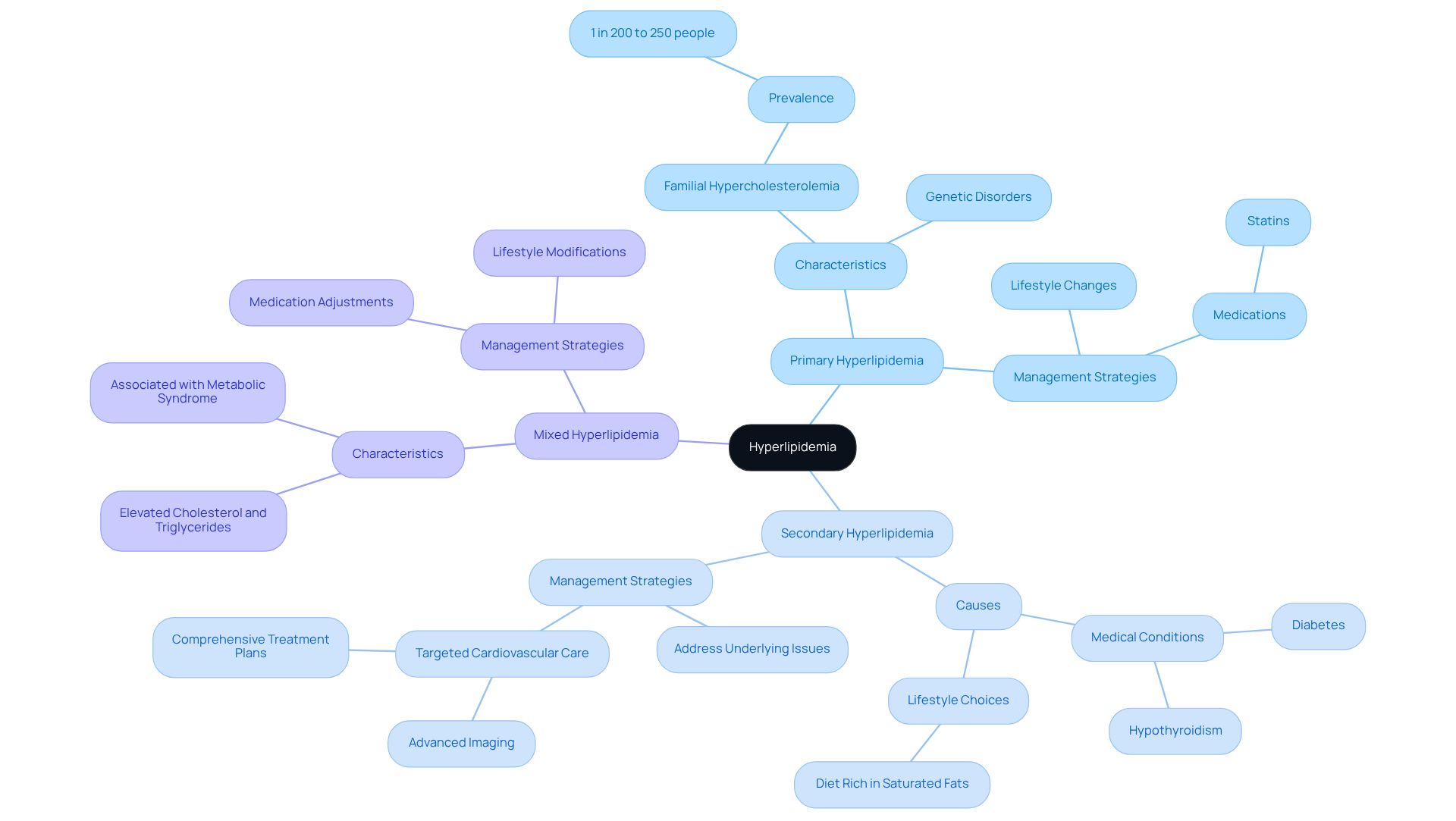
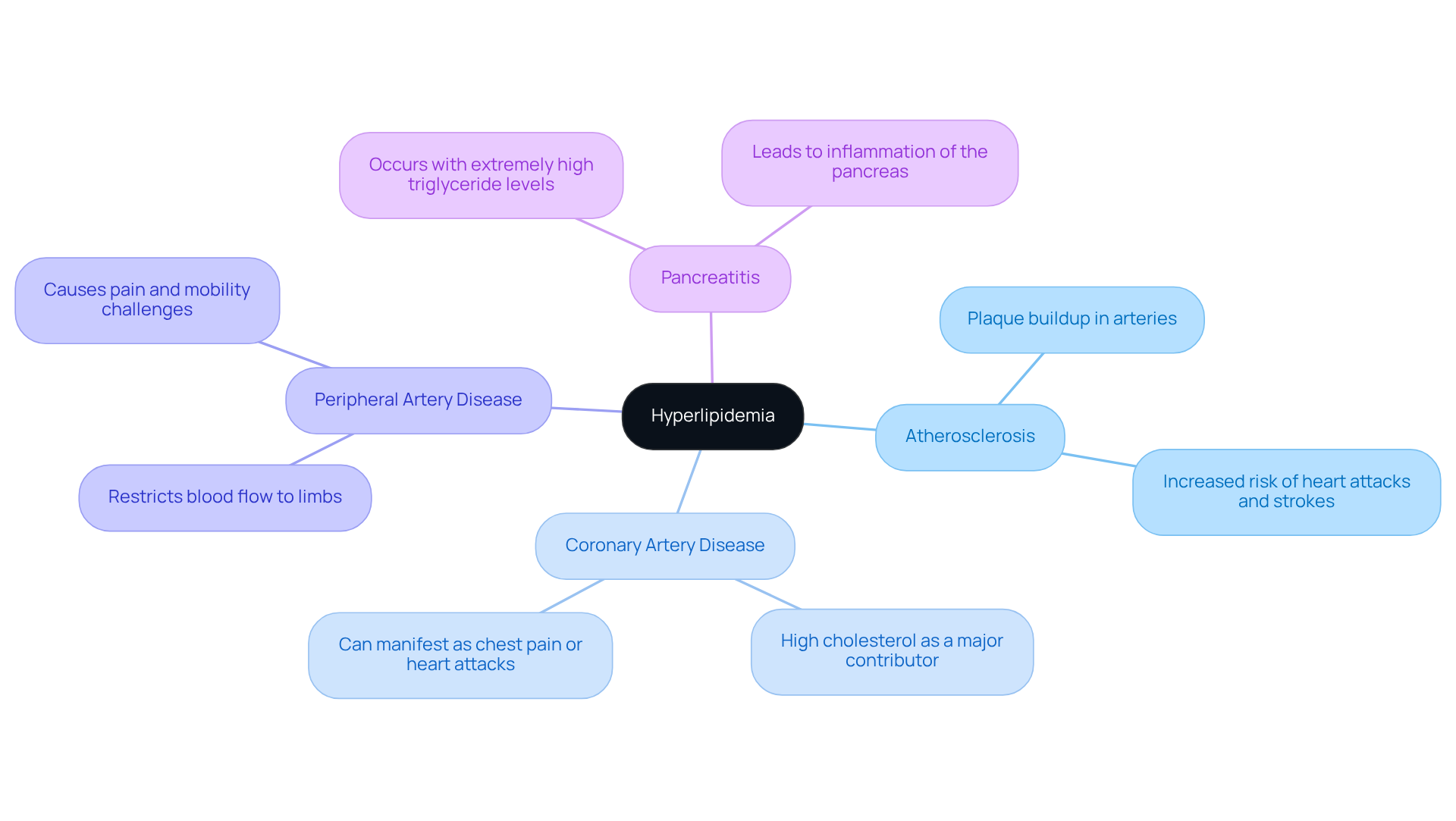
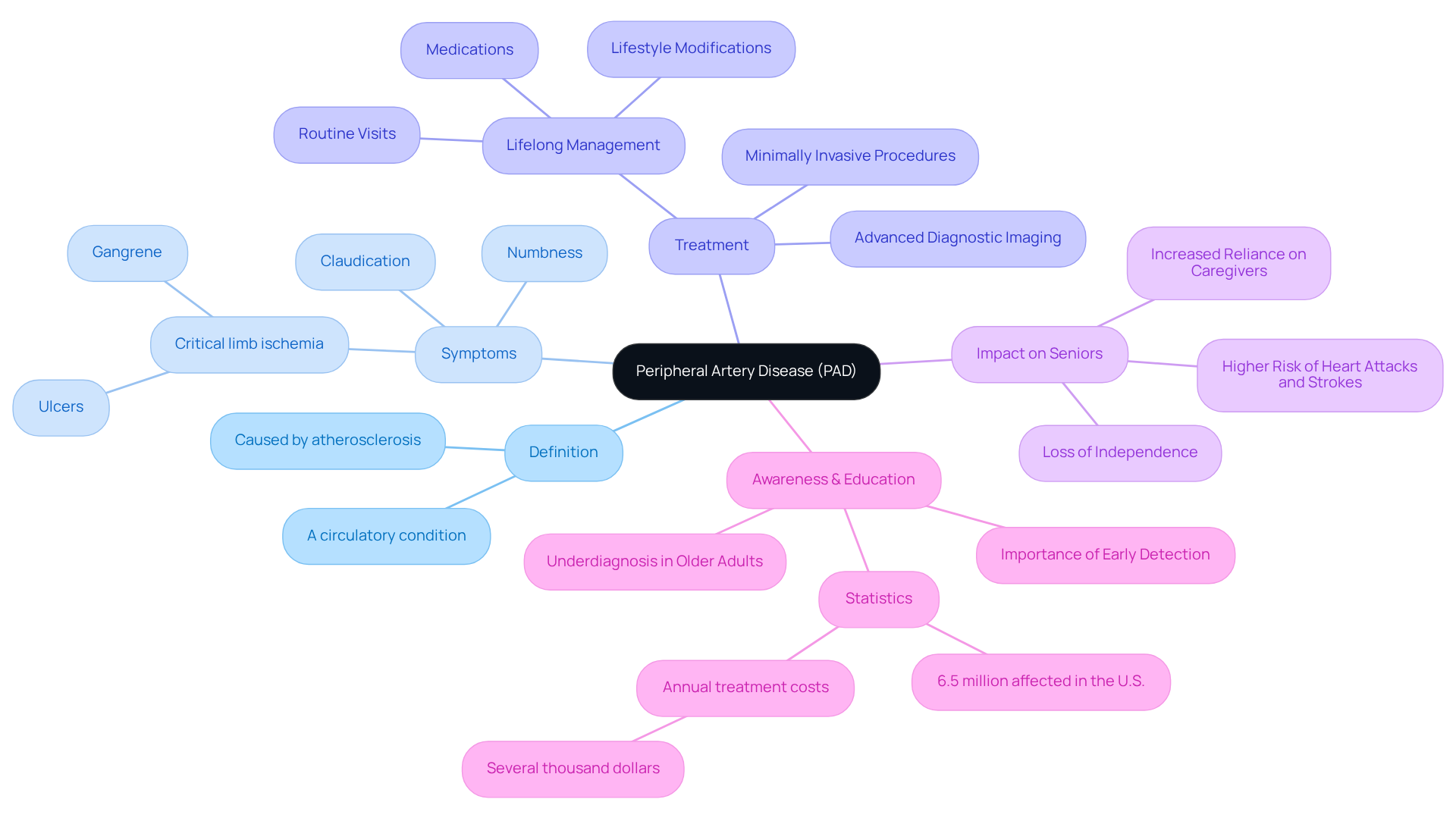
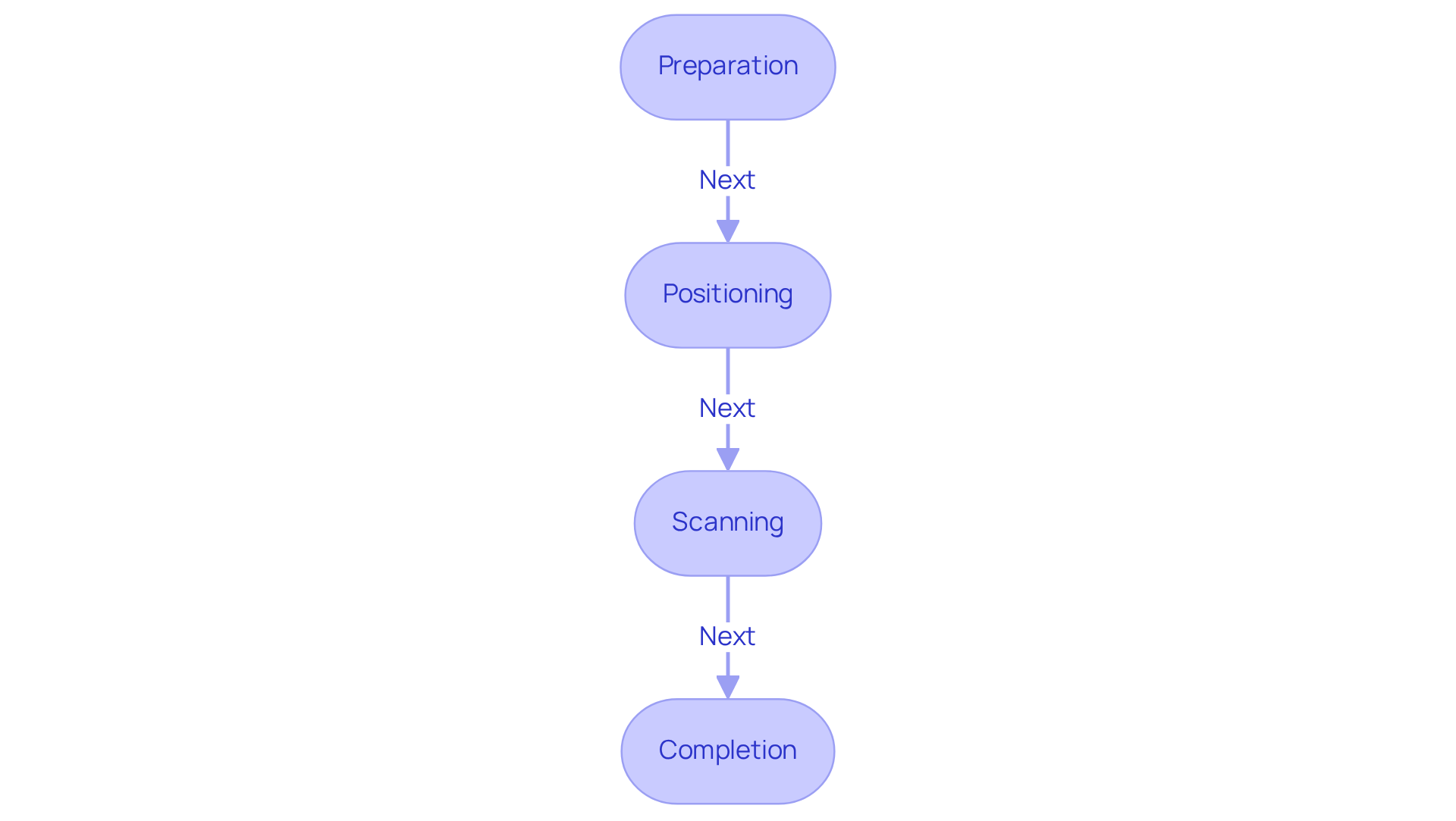
Understanding your heart health is vital, and what does a calcium score show is crucial as it often refers to a coronary artery calcified plaque (CAC) measurement. This test, performed through a specialized CT scan, helps identify mineral deposits in your coronary arteries, providing insight into what does a calcium score show about a condition called atherosclerosis. This condition occurs when arteries become narrowed or blocked due to plaque buildup, and knowing what does a calcium score show can provide valuable insights into your heart health.
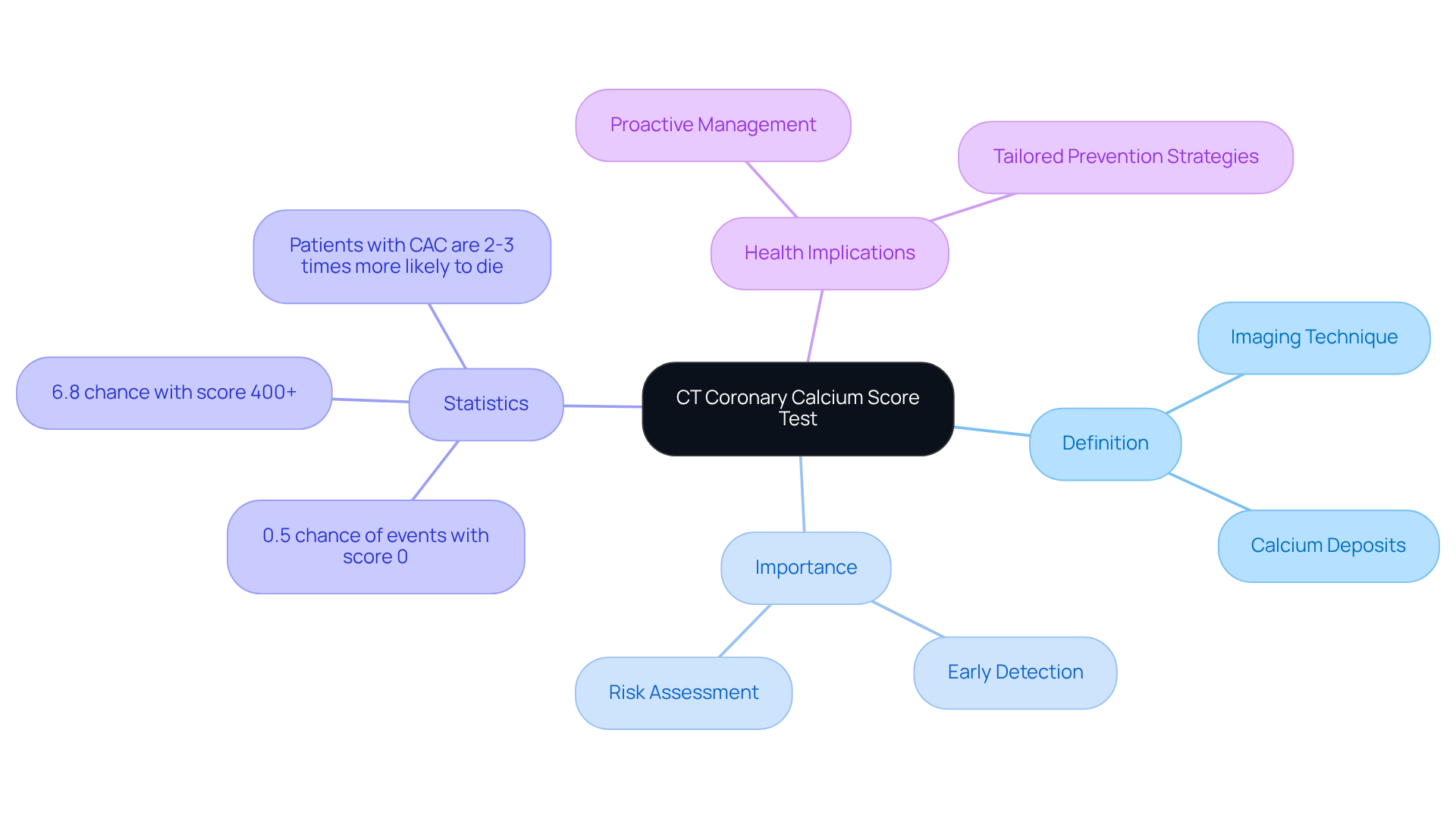
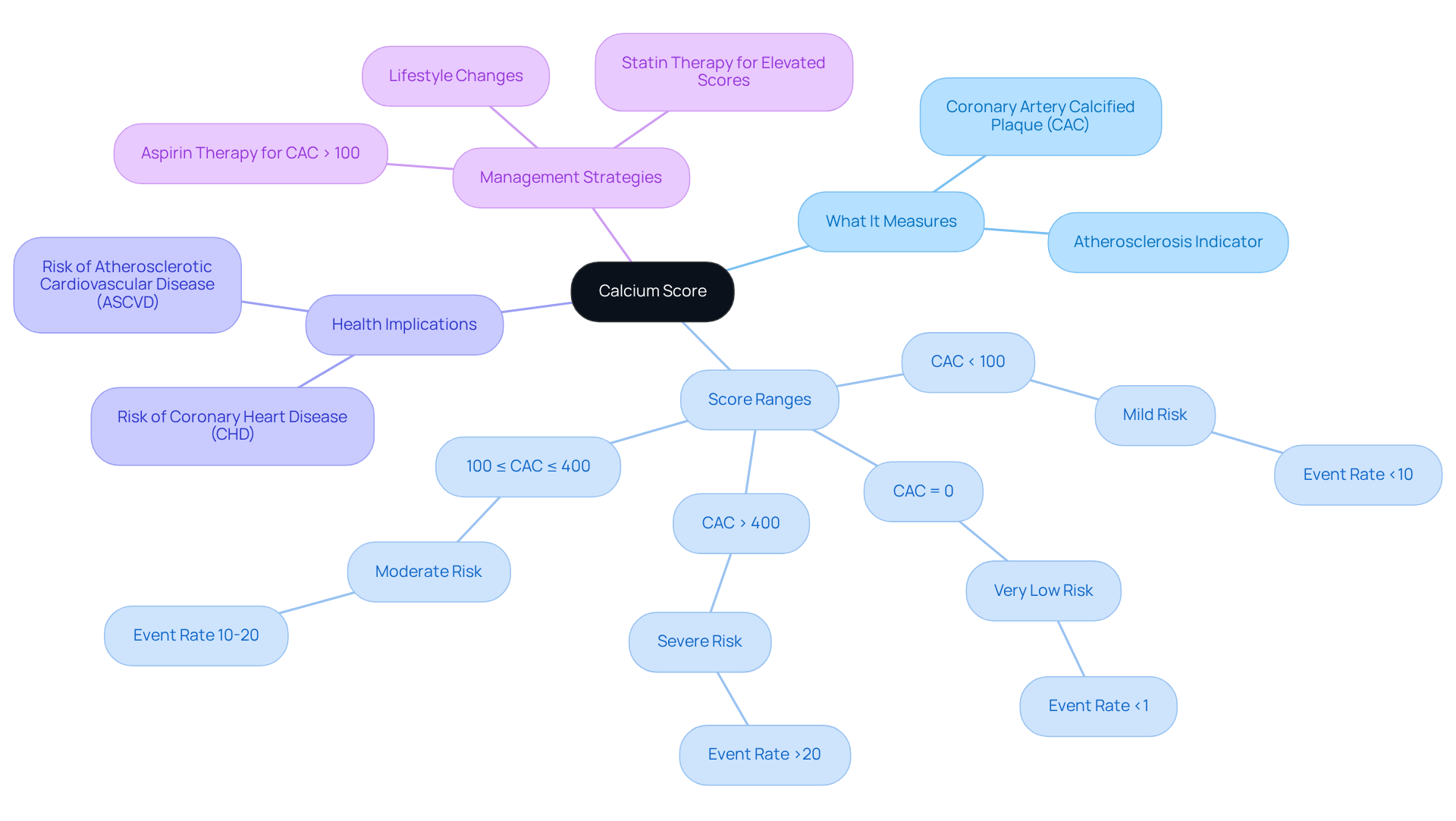
The results of your CAC measurement are categorized into ranges. A score of CAC = 0 means there’s no detectable plaque, suggesting a very low chance of heart disease. Scores below 100 are considered mild, while those between 100 and 400 indicate a moderate risk. If your score exceeds 400, it suggests a severe potential for coronary artery disease (CAD). Understanding what does a calcium score show is essential, as it helps guide healthcare professionals at Amavita Heart and Vascular Health® in making informed decisions about your preventive care and treatment options tailored just for you.
For instance, research shows that individuals with a CAC score of 0 experience a heart event rate of only 0.47% over 50 months. In contrast, those with scores above 100 face significantly higher risks, with a 10-year rate of major coronary heart disease events reaching 17.5%. It’s important to note that the Cardiac Society of Australia and New Zealand (CSANZ) advises against scoring for symptomatic patients, as it may not provide additional value compared to other testing methods.
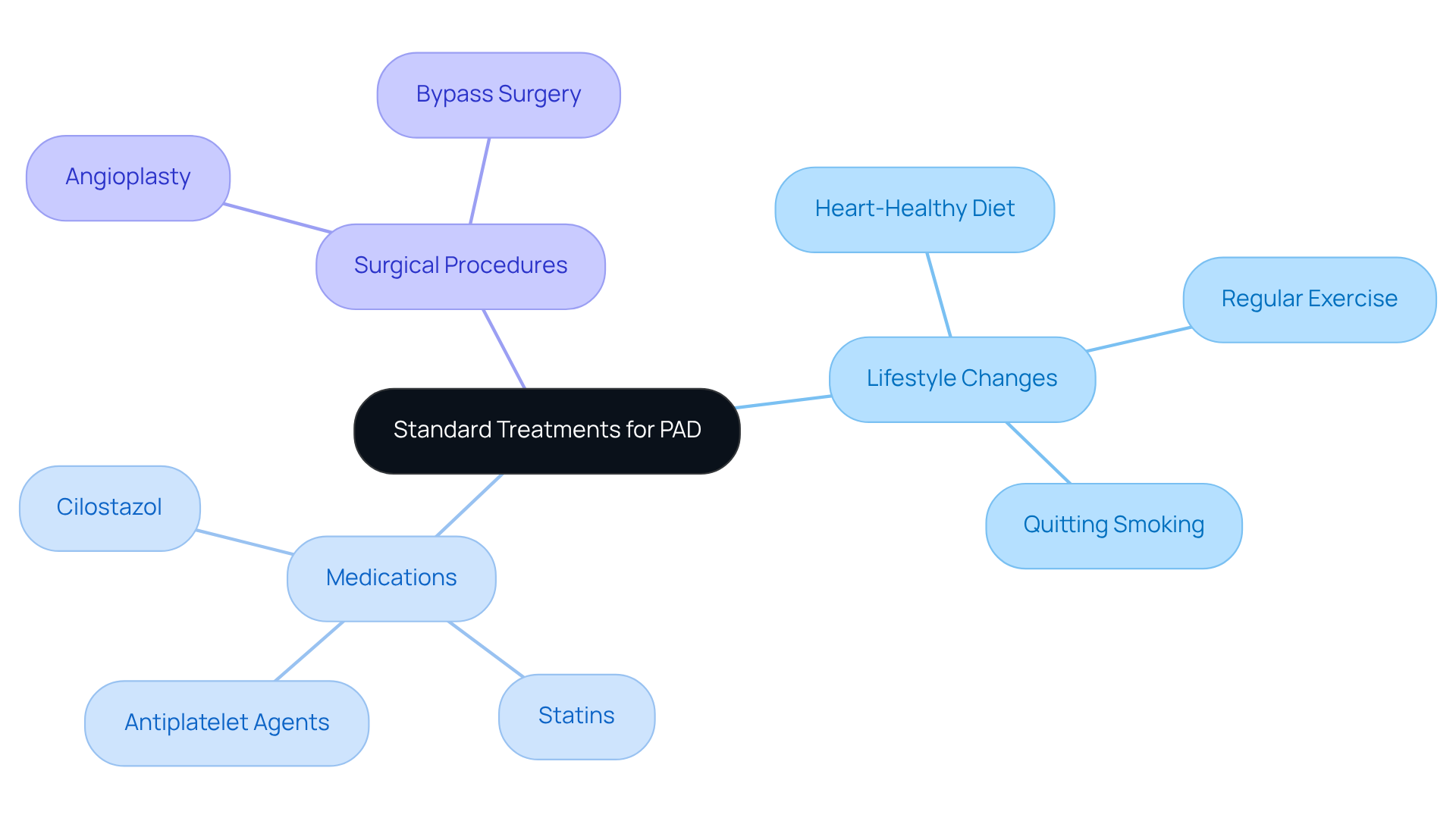
If your CAC measurement indicates higher mineral levels, it’s important to know what does a calcium score show in order to implement proactive management strategies, such as daily aspirin and lifestyle changes, to help reduce future cardiovascular issues. Additionally, incidental findings during calcium scoring may necessitate further evaluations or treatments, emphasizing what does a calcium score show about the broader implications of this assessment.
At Amavita, we prioritize your unique needs through comprehensive cardiac assessments and personalized strategies. Our goal is to support you in effectively lowering your chances of a heart attack, ensuring you feel cared for and valued every step of the way.
Contextualize Calcium Scores: Their Role in Heart Health Assessment
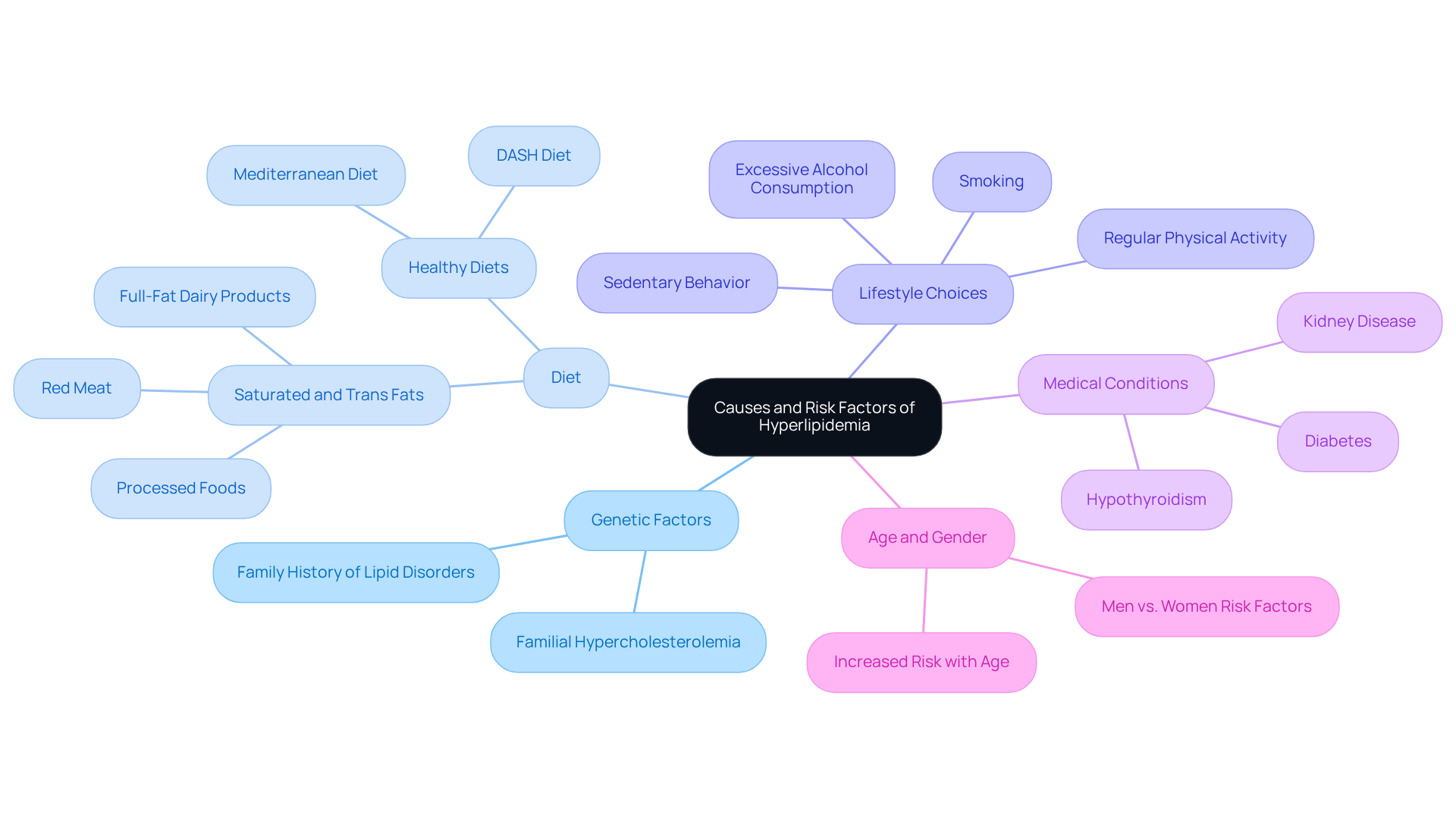
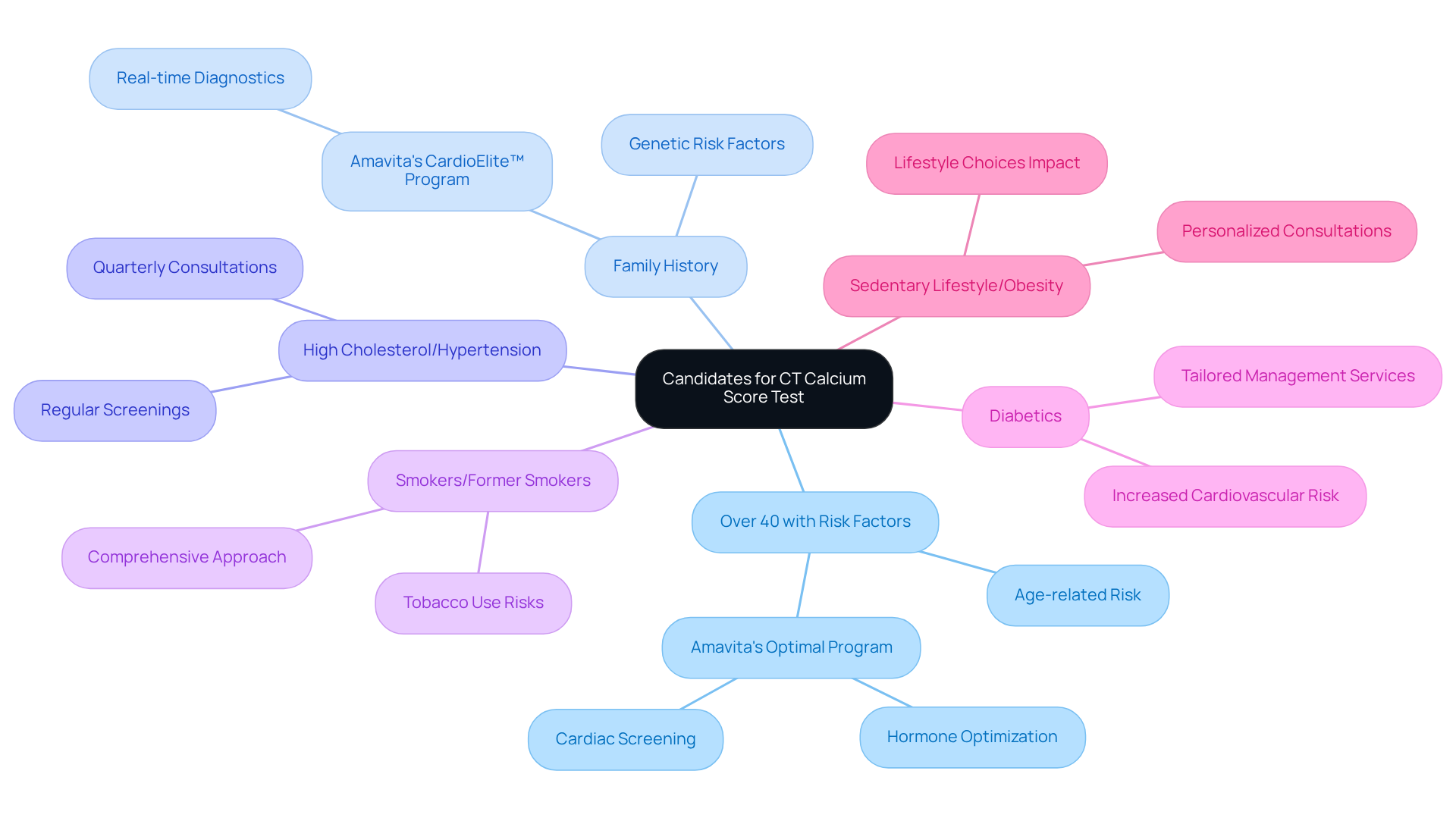
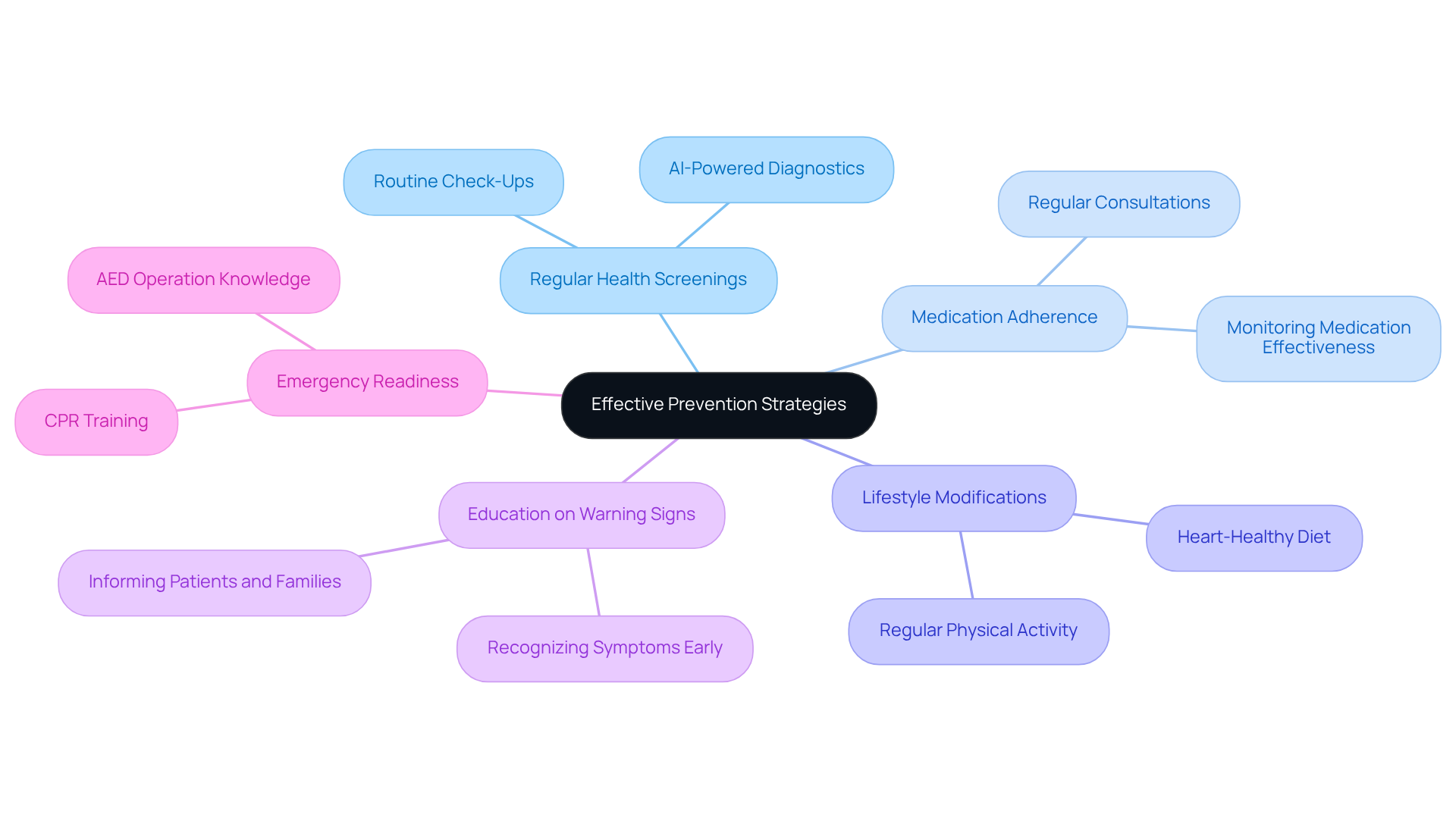
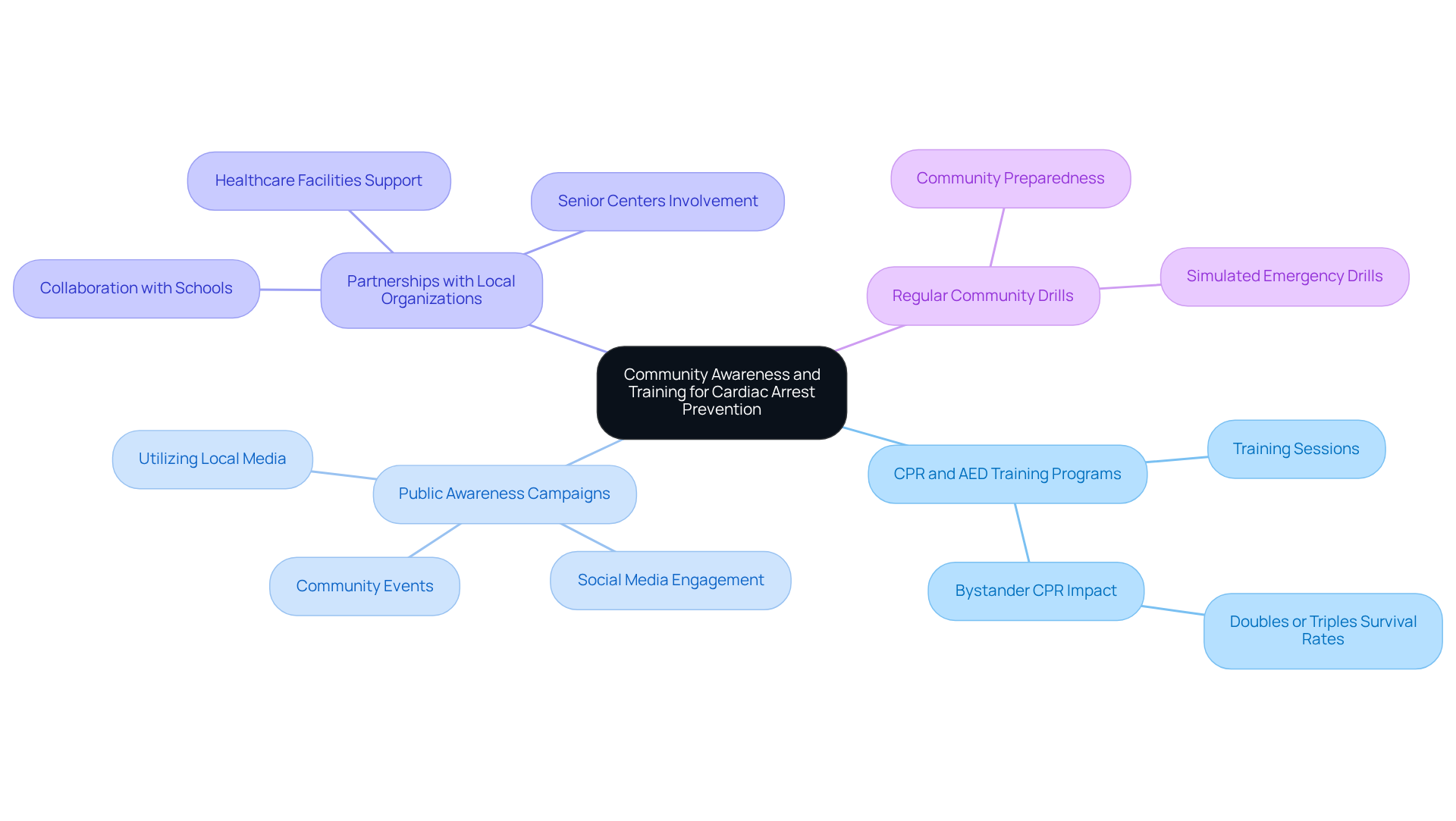
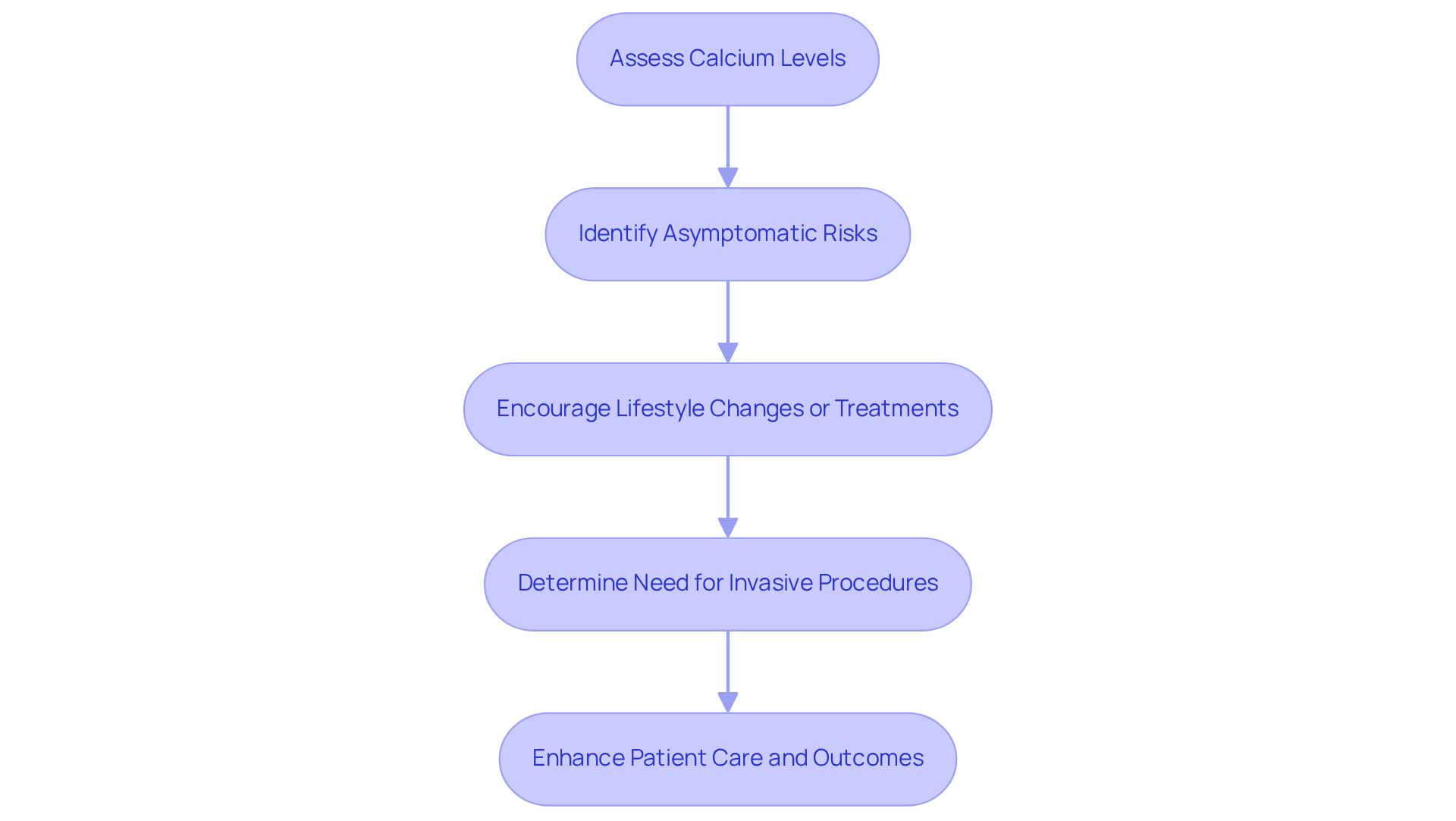
Calcium levels are vital for evaluating heart health, providing a gentle, non-invasive way to check for coronary artery disease. This is especially helpful for those who might not show typical signs of heart issues, like high cholesterol or hypertension. By assessing mineral levels, we can identify individuals who may be at risk but are asymptomatic, allowing for early intervention – an essential part of Amavita’s CardioElite™ program.
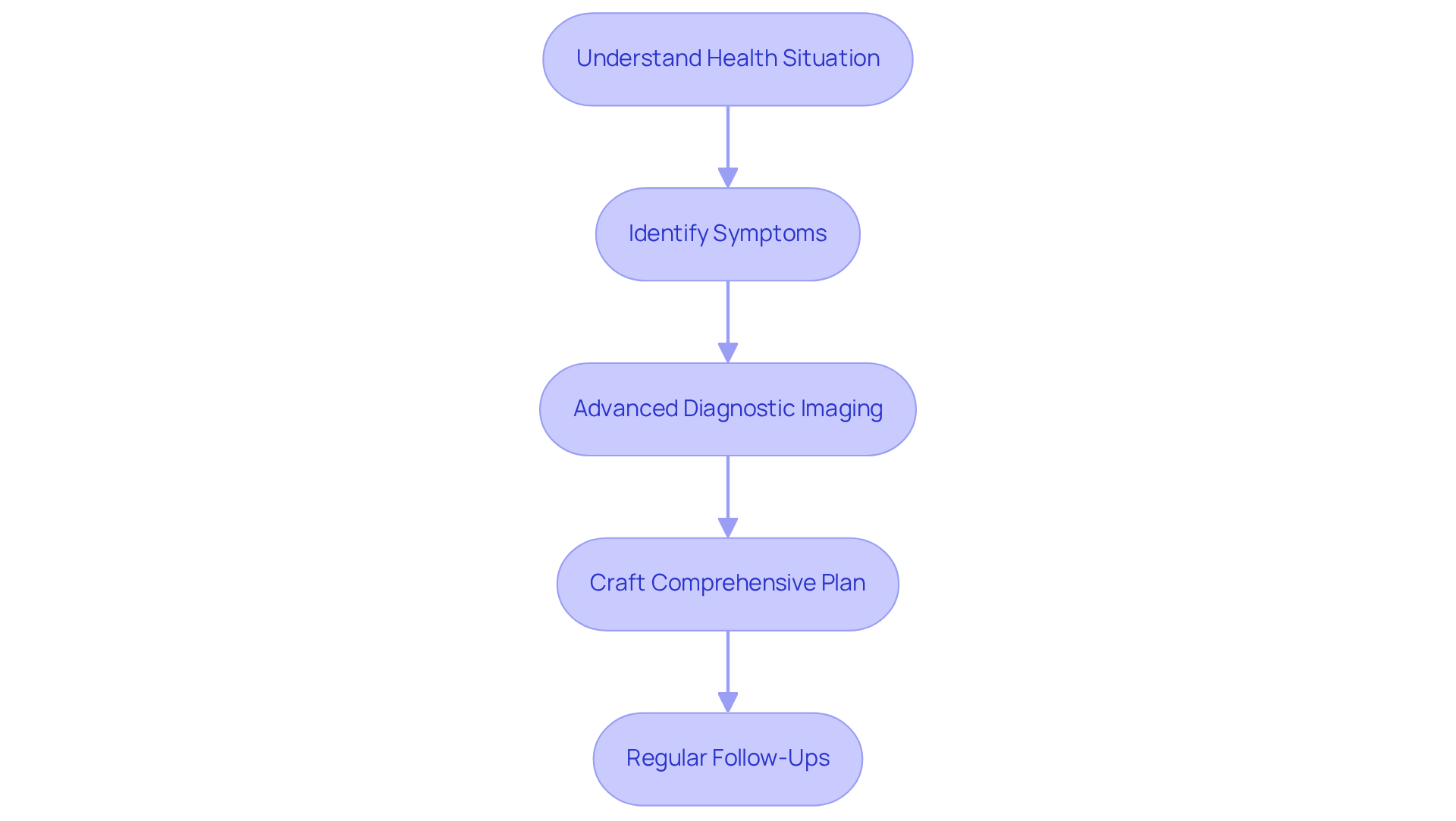
For instance, if a patient has elevated mineral levels, they might be encouraged to make lifestyle changes or start treatments to better manage their heart health. This proactive approach not only helps in recognizing potential risks but also aids healthcare professionals in determining if more invasive procedures, like angiography, are necessary. This thoughtful strategy enhances patient care and optimizes resource use.
By integrating advanced diagnostic tools, such as scoring, with the comprehensive management strategies of the CardioElite™ program – which includes 24/7 cardiology consultations and AI-driven insights – Amavita is dedicated to improving heart health care. Our goal is to reduce hospital readmissions and ultimately enhance patient outcomes. Remember, taking steps towards heart health is a journey we can support you on, and we’re here to help every step of the way.
Trace the Evolution: The Development of Calcium Scoring Technology
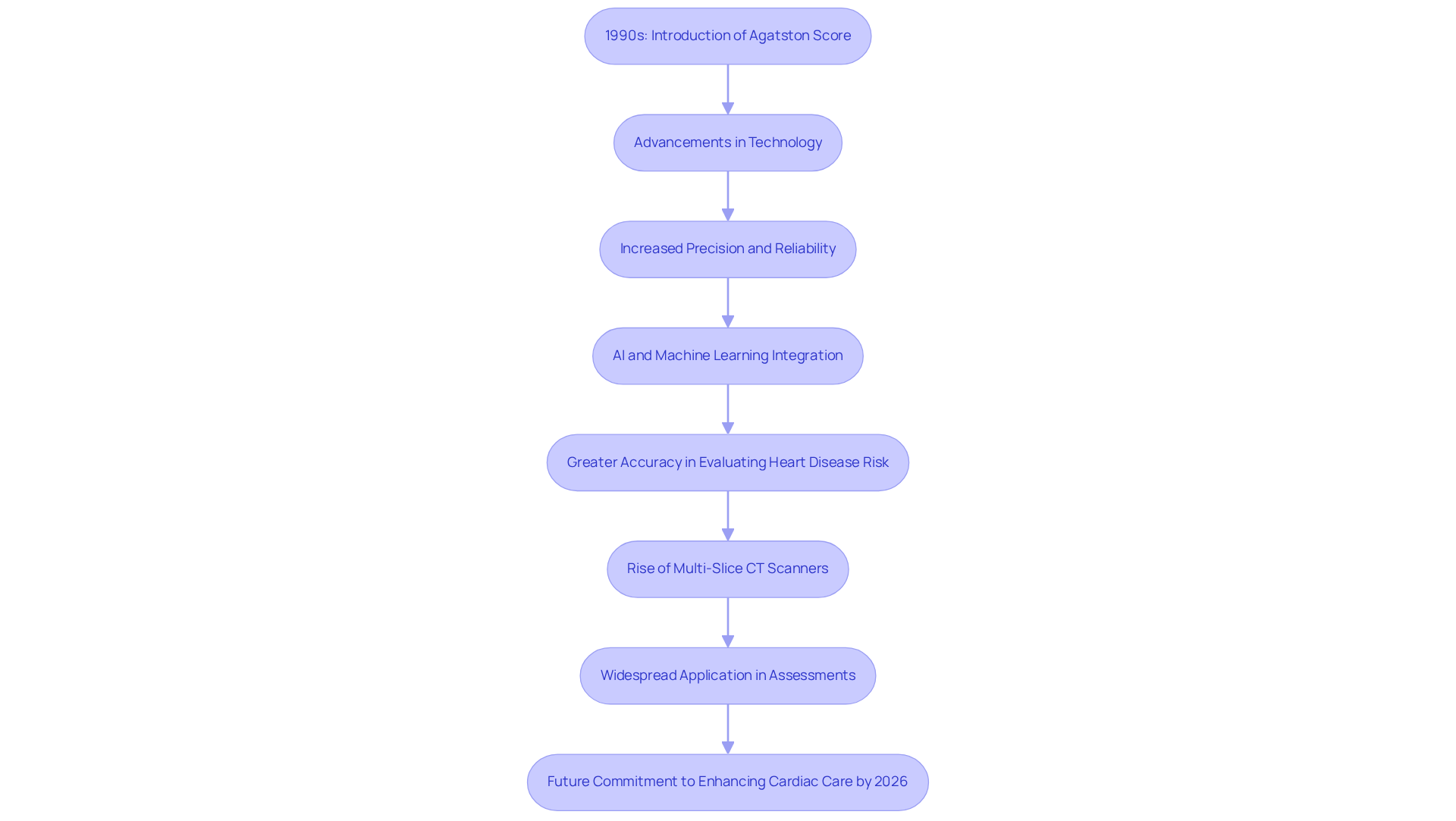
In the early 1990s, a significant breakthrough in heart health emerged with the introduction of mineral scoring by Dr. Arthur Agatston. He developed the Agatston score, a tool designed to measure coronary artery mineral (CAC). This innovative scoring system transformed how we assess cardiovascular health, offering a standardized way to evaluate calcified plaque in the coronary arteries.
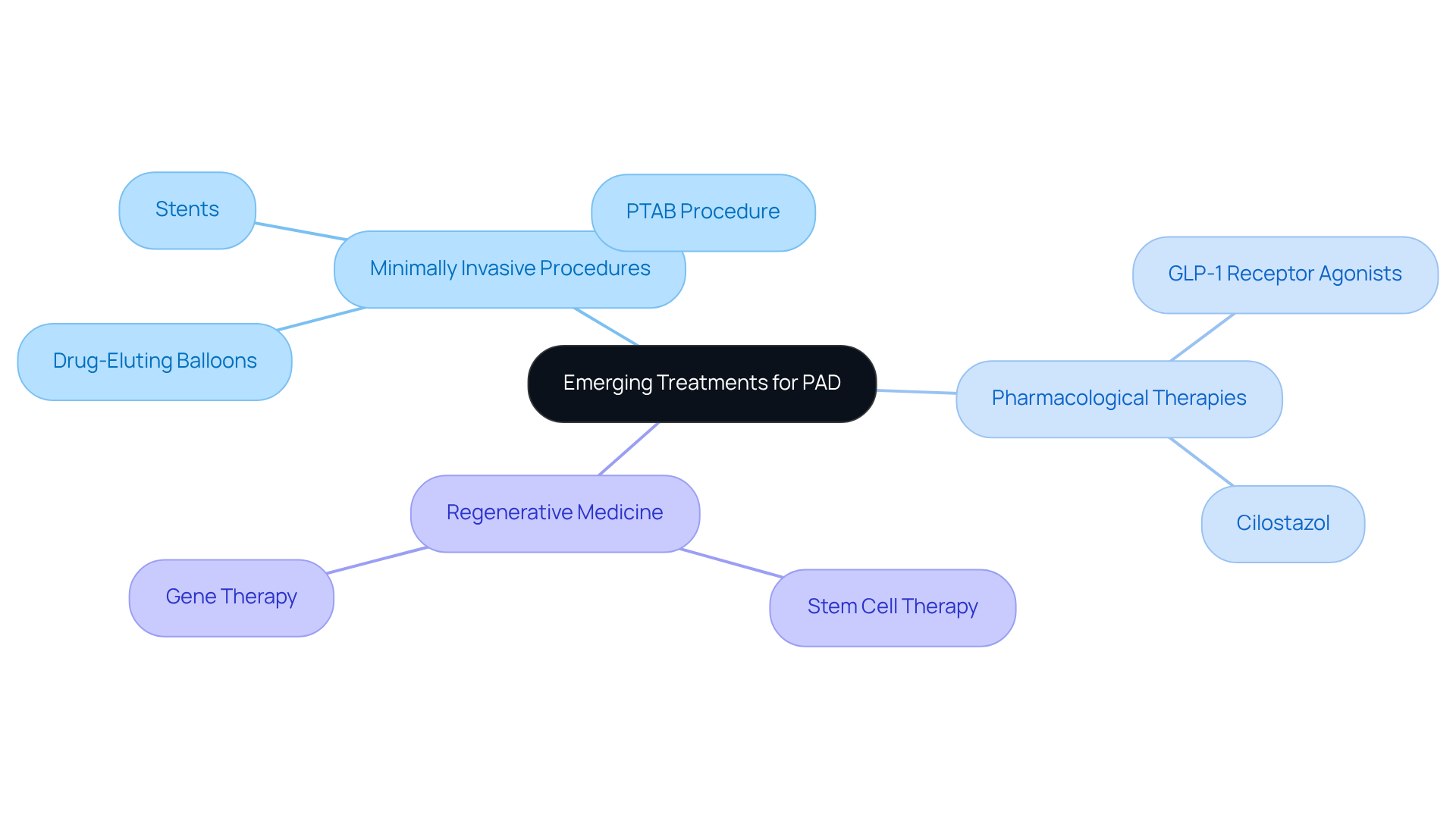
As technology has advanced, so too has the precision and reliability of CAC scoring. Today, it plays a vital role in preventive cardiology, helping healthcare providers identify potential health issues and manage patient care more effectively. Have you ever wondered how these advancements could impact your heart health? Recent developments, including the use of artificial intelligence and machine learning, promise even greater accuracy in evaluating heart disease risk. For example, studies reveal that a CAC score of zero indicates a remarkable 99% negative predictive value for significant stenosis, highlighting its critical role in clinical practice.
Moreover, the rise of multi-slice CT scanners has made CAC scoring more accessible, allowing for widespread application in heart health assessments. At Amavita, we understand that 25% of heart failure patients rely on post-acute care facilities, which underscores the importance of effective predictive tools to prevent complications.
Our CardioElite™ system exemplifies this commitment. It not only offers advanced bedside diagnostics but also supports comprehensive cardiac assessments, enabling early detection of complications before they escalate. As we look ahead to 2026, we remain dedicated to enhancing cardiac care standards through ongoing staff training and certification pathways. Together, we can ensure that patients receive personalized and effective care, fostering a healthier future for all.
Understand Key Characteristics: How Calcium Scores Are Calculated and Interpreted
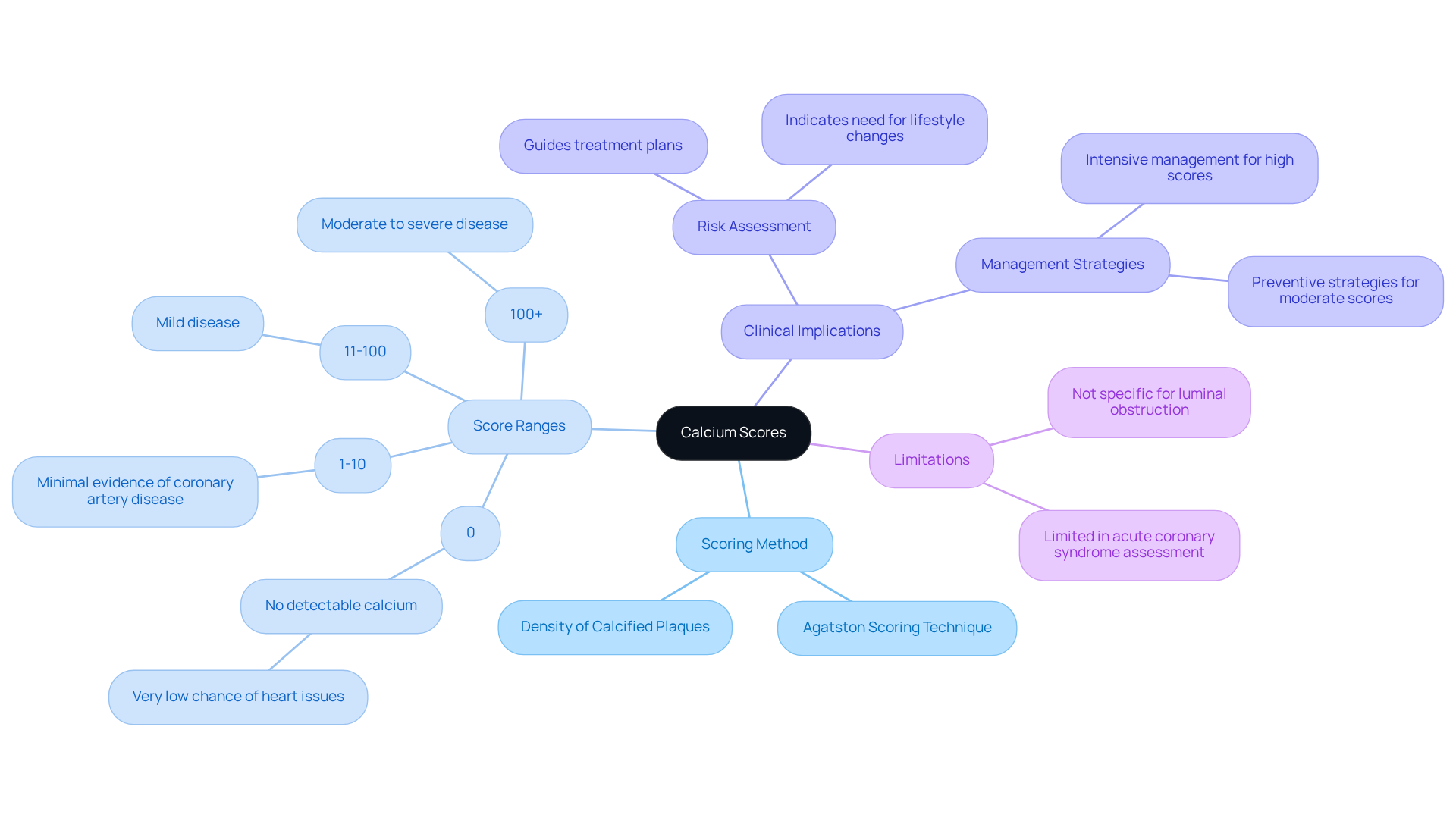
Calcium measurements from a CT scan provide valuable insights into the health of your coronary arteries by quantifying the density and area of calcified plaques. The Agatston scoring technique is a trusted method that assigns points based on the density of these mineral deposits. Denser deposits contribute more significantly to the overall score, reflecting the burden of calcified plaque in your arteries.
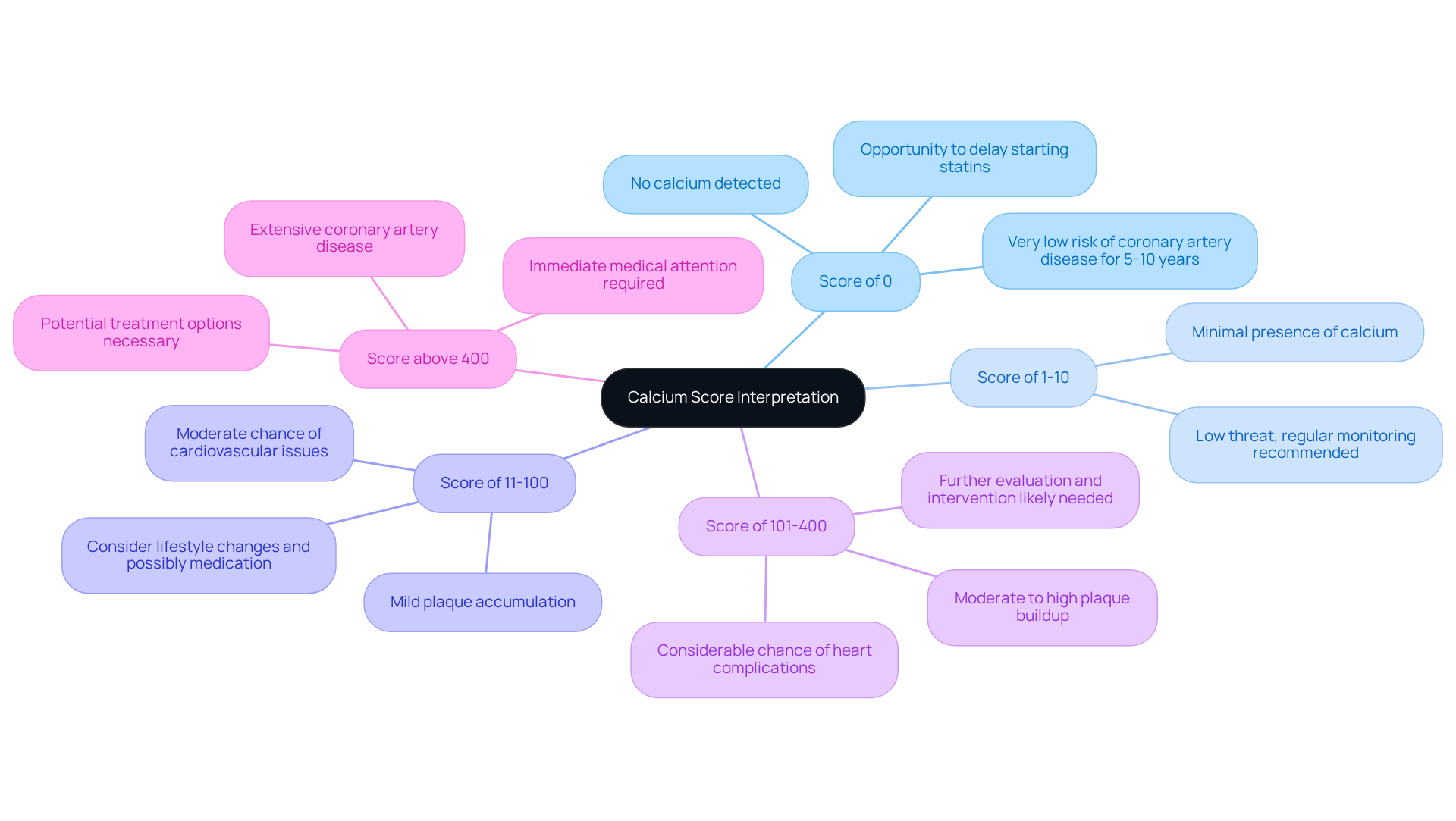
Understanding what does a calcium score show can provide reassurance about your calcium levels. A score of 0 means no detectable calcium, suggesting a very low chance of heart issues. If your score falls between 1-10, it indicates minimal evidence of coronary artery disease. Scores from 11-100 suggest mild disease, while anything above 100 points to moderate to severe disease. These classifications are crucial for your healthcare provider as they assess your risk for future heart-related events and tailor treatment plans just for you.
For instance, if your score exceeds 300, it may signal the need for more intensive management of heart health factors, including lifestyle adjustments and possibly medication. Research shows that individuals with a CAC value between 100-400 face a relative risk of 4.3 for major heart-related events. This underscores the importance of accurately interpreting what does a calcium score show in order to guide clinical decisions. Importantly, a CAC score of zero is a reassuring sign for heart health, providing peace of mind.
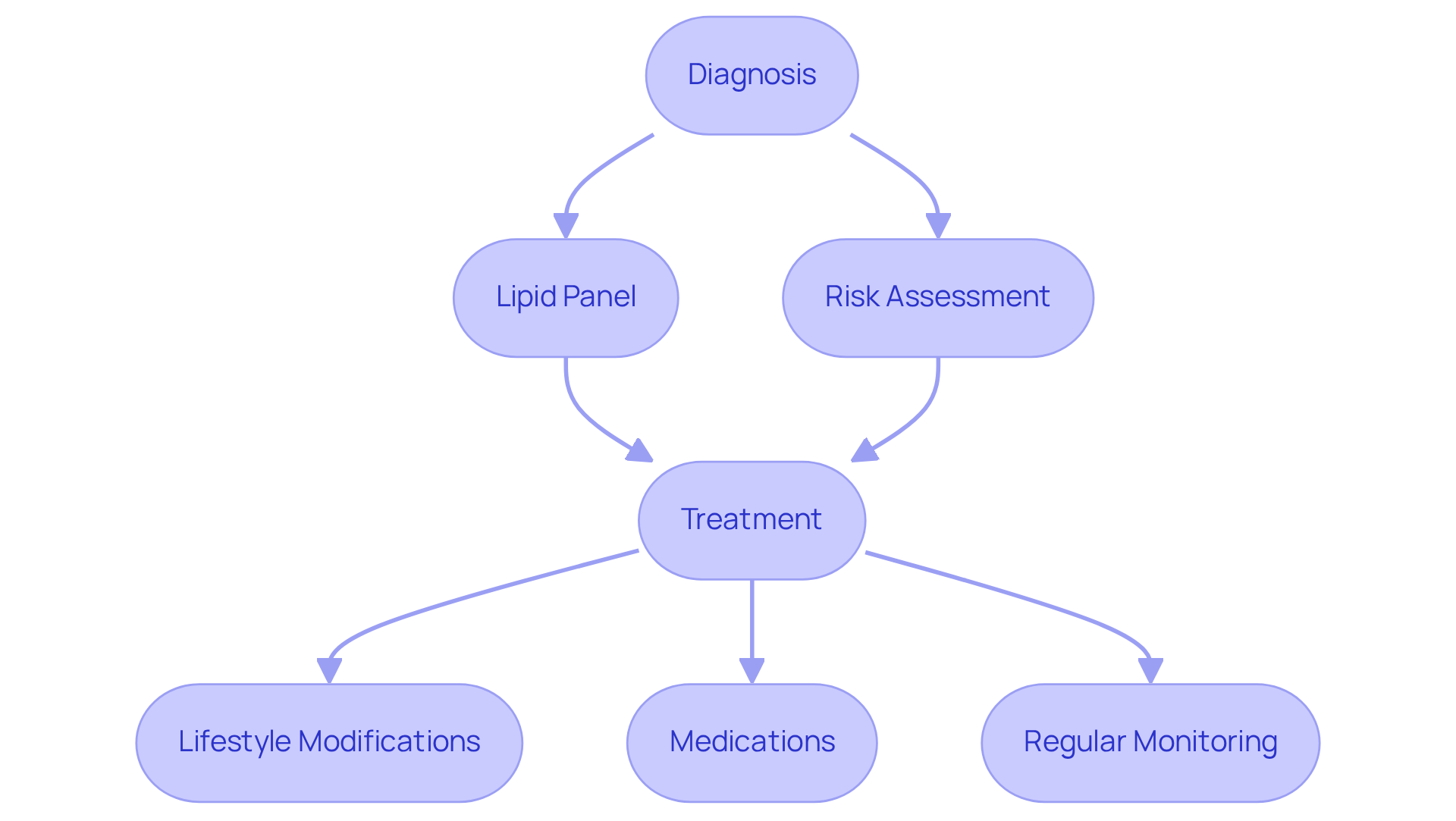
At Amavita Heart and Vascular Health®, we integrate calcium scoring into our standard evaluations, complemented by advanced imaging capabilities. This allows our healthcare providers to enhance assessments and create personalized care plans that truly cater to your needs. Our comprehensive approach aims to improve outcomes in heart health management. We believe in a preventive heart health strategy that combines advanced evaluation tools with tailored interventions, ensuring that high-risk individuals receive focused care.
However, it’s essential to recognize that the CAC score has its limitations, especially when assessing patients with suspected acute coronary syndrome. This highlights the need for a thorough approach to cardiovascular risk assessment. If you have concerns about your heart health, please don’t hesitate to reach out. We’re here to support you every step of the way.
Conclusion
Understanding the implications of a calcium score is vital for anyone concerned about their heart health. This measurement acts as a crucial indicator of coronary artery disease risk, helping both individuals and healthcare professionals make informed decisions about preventive care and treatment strategies. By identifying the presence of calcified plaque in the arteries, a calcium score can provide a clear picture of cardiovascular health and potential risks.
Throughout this discussion, we highlighted key insights, including:
- The significance of different score ranges
- The historical development of calcium scoring technology
- The importance of proactive management strategies for those with elevated calcium levels
A score of zero offers reassurance, while higher scores call for careful monitoring and possible lifestyle changes or treatments to mitigate future cardiovascular issues. The integration of advanced tools and personalized care approaches, such as those offered by Amavita Heart and Vascular Health®, enhances the effectiveness of heart health assessments.
Ultimately, the journey to heart health is a collaborative effort that requires awareness and action. Are you ready to engage with your healthcare provider about calcium scoring and its implications? By understanding what a calcium score indicates, you can take significant steps toward reducing cardiovascular risks and improving your overall health outcomes. Embracing this knowledge not only fosters a proactive approach to heart health but also empowers you to lead a healthier life.
Frequently Asked Questions
What is a calcium score?
A calcium score refers to a measurement of coronary artery calcified plaque (CAC) obtained through a specialized CT scan, which identifies mineral deposits in the coronary arteries and provides insight into heart health.
What does a calcium score indicate about heart health?
A calcium score helps identify the presence of atherosclerosis, a condition where arteries become narrowed or blocked due to plaque buildup, offering valuable insights into the risk of heart disease.
How are calcium score results categorized?
Calcium score results are categorized as follows: a score of 0 indicates no detectable plaque and a very low chance of heart disease; scores below 100 are considered mild risk; scores between 100 and 400 indicate moderate risk; and scores exceeding 400 suggest severe potential for coronary artery disease (CAD).
What are the risks associated with different calcium score ranges?
Individuals with a CAC score of 0 have a heart event rate of only 0.47% over 50 months, while those with scores above 100 face significantly higher risks, with a 10-year rate of major coronary heart disease events reaching 17.5%.
Are there any recommendations regarding calcium scoring for symptomatic patients?
The Cardiac Society of Australia and New Zealand (CSANZ) advises against scoring for symptomatic patients, as it may not provide additional value compared to other testing methods.
What should be done if a calcium score indicates higher mineral levels?
If a calcium score indicates higher mineral levels, it is important to implement proactive management strategies, such as daily aspirin and lifestyle changes, to help reduce future cardiovascular issues.
Can incidental findings during calcium scoring lead to further evaluations?
Yes, incidental findings during calcium scoring may necessitate further evaluations or treatments, highlighting the broader implications of the calcium score assessment.
How does Amavita Heart and Vascular Health® approach calcium scoring and heart health?
Amavita prioritizes unique patient needs through comprehensive cardiac assessments and personalized strategies aimed at effectively lowering the chances of a heart attack while ensuring patients feel cared for and valued.
List of Sources
- Define Calcium Score: What It Measures and Its Importance
- Arterial Plaque Regression: A Case-Based, Integrative Approach to Cardiovascular Risk Reduction | NDNR – Naturopathic Doctor News and Review (https://ndnr.com/arterial-plaque-regression-a-case-based-integrative-approach-to-cardiovascular-risk-reduction)
- Calcium Score Screenings: A Powerful Tool for Preventing Heart Disease (https://uab.edu/news/health-medicine/calcium-score-screenings-a-powerful-tool-for-preventing-heart-disease)
- aafp.org (https://aafp.org/pubs/afp/issues/2022/0700/diagnostic-tests-coronary-artery-calcium-scoring.html)
- Coronary artery calcium in primary prevention (https://www1.racgp.org.au/ajgp/2020/august/coronary-artery-calcium-in-primary-prevention)
- Coronary Artery Calcium Score – A Reliable Indicator of Coronary Artery Disease? – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC8723785)
- Trace the Evolution: The Development of Calcium Scoring Technology
- Coronary Calcium: New Insights, Recent Data, and Clinical Role – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC3551450)
- Coronary Artery Calcium Scoring: A Brief Update and Look to the Future (https://lipid.org/lipid-spin/potpourri-2018/coronary-artery-calcium-scoring-brief-update-and-look-future)
- CAC Scoring Shines at ACC | AI of DBT – The Imaging Wire (https://theimagingwire.com/newsletter/cac-news-at-acc-2025)
- How the Agatston Calcium Score Was Created and its Impact on Heart Attack Prevention (https://dicardiology.com/content/blogs/how-agatston-calcium-score-was-created-and-its-impact-heart-attack-prevention)
- Understand Key Characteristics: How Calcium Scores Are Calculated and Interpreted
- Early detection, lasting prevention: The significance of coronary artery calcium scores (https://bcmj.org/articles/early-detection-lasting-prevention-significance-coronary-artery-calcium-scores)
- Calcium Score CT Scan: Who Needs It in 2026? (https://lakeviewcardiologytexas.com/2026/02/16/calcium-score-ct-scan)
- Coronary Artery Calcium Scores: Current Thinking and Clinical Applications – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC2627524)
- Master Coronary Artery Calcium Score Interpretation for Heart Health (https://amavita.health/blog/master-coronary-artery-calcium-score-interpretation-for-heart-health)
- Coronary artery calcium score: current status – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC5487233)