Introduction
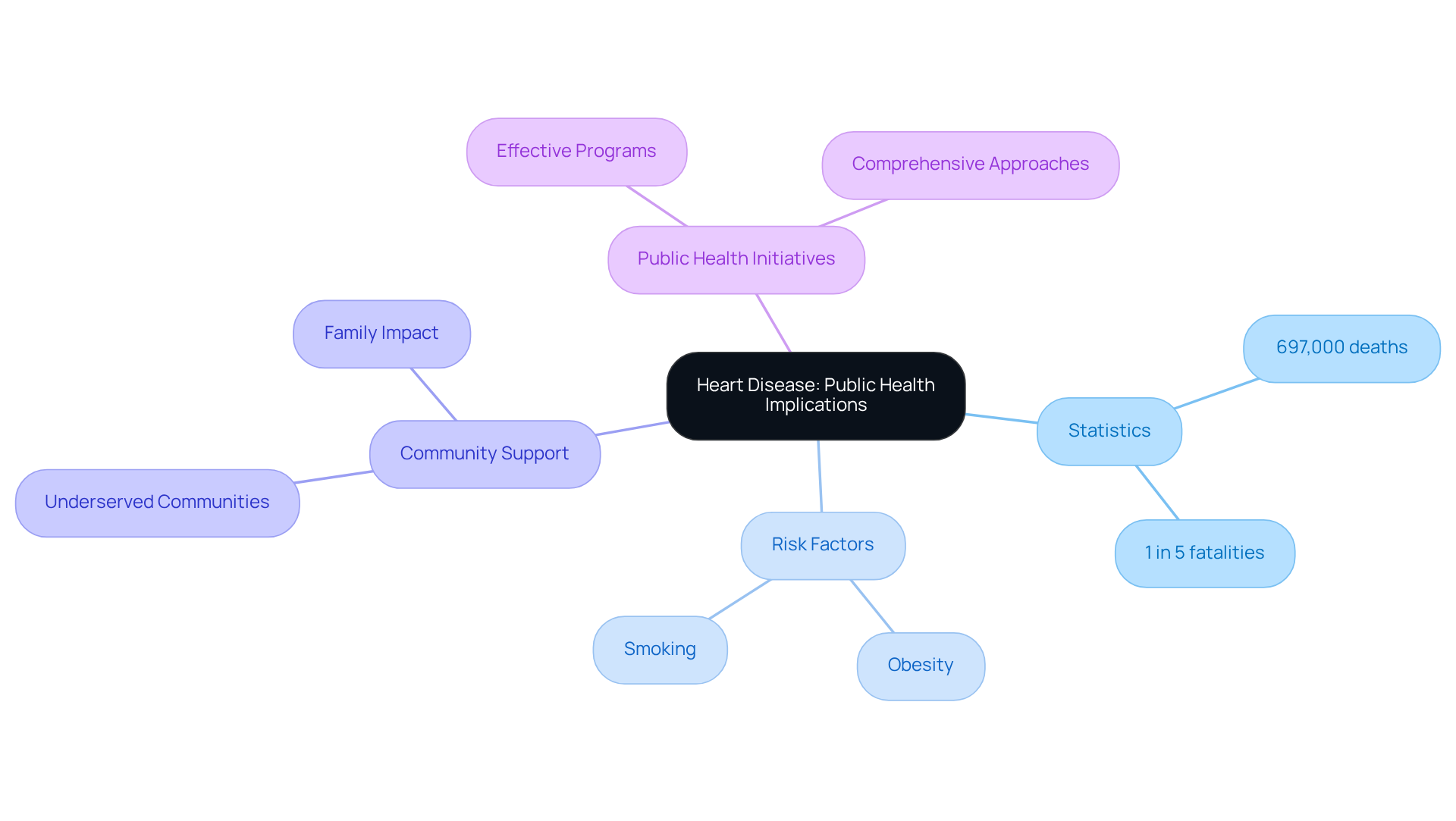
Recognizing cardiac arrest can truly mean the difference between life and death. Yet, many people remain unaware of its critical signs and symptoms. With around 350,000 incidents occurring outside of hospitals each year in the U.S., it’s vital to understand how to identify these warning signs for timely intervention.
What should you do when someone suddenly collapses? How can bystanders respond effectively to maximize survival chances? This article gently explores the essential indicators of cardiac arrest, the vital steps to take during an emergency, and the risk factors that heighten vulnerability. Our goal is to empower you to act decisively when it matters most, ensuring that you feel supported and informed.
Define Cardiac Arrest: Understanding the Medical Emergency
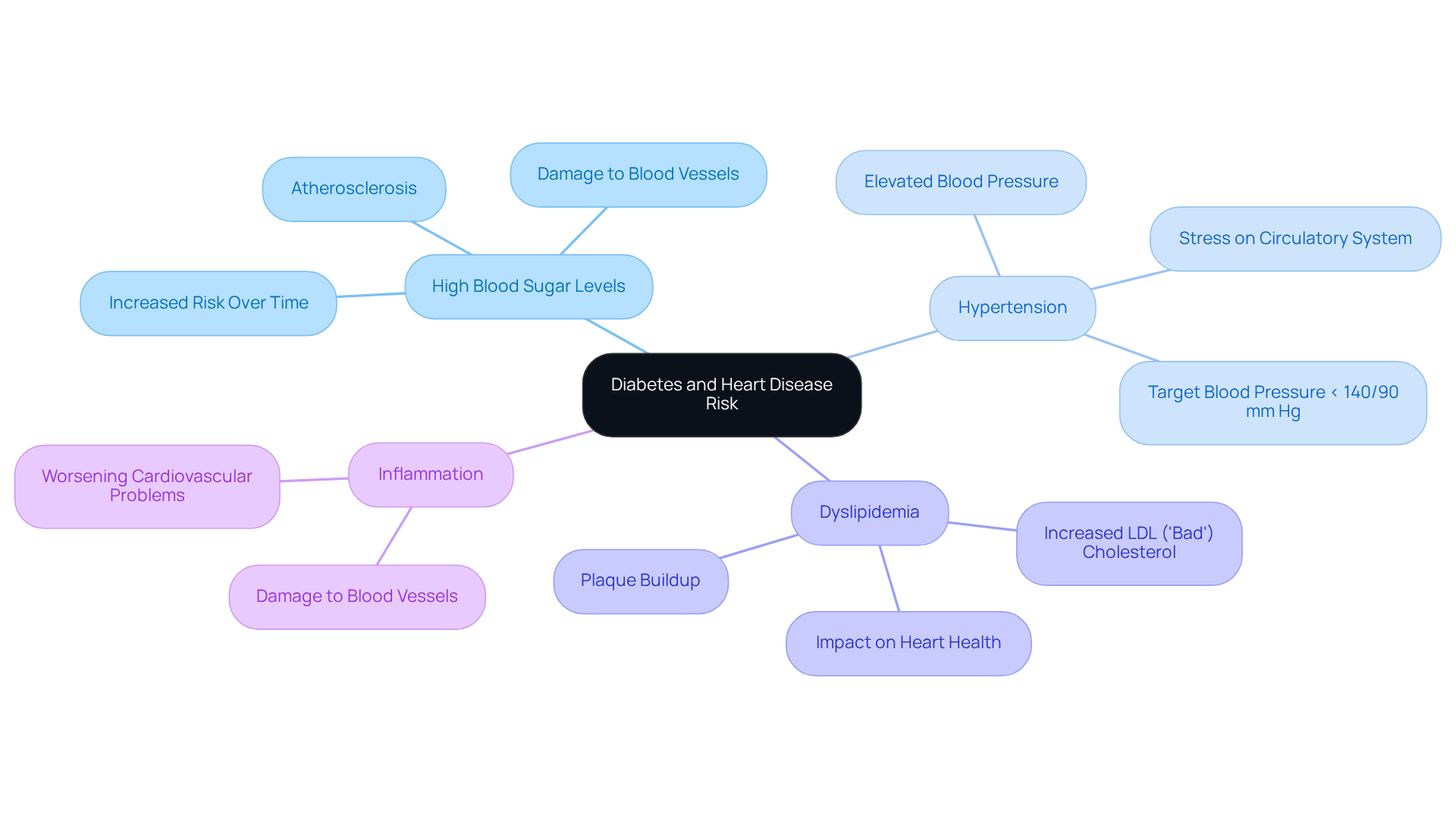
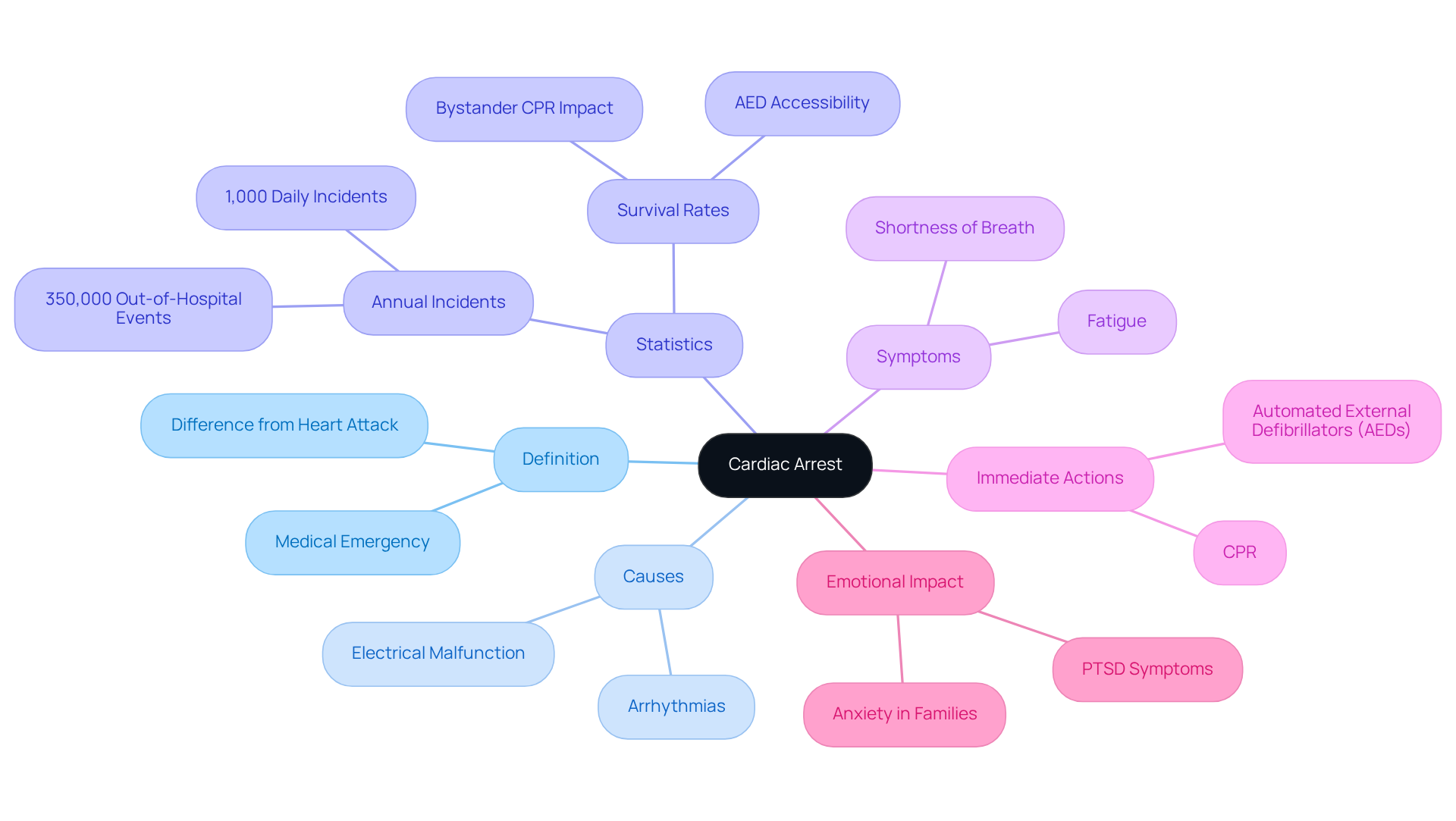
Cardiac failure is a serious medical emergency that can strike suddenly, halting the heart’s ability to pump blood and putting vital organs, including the brain, at risk. This condition can arise unexpectedly, often triggered by an electrical malfunction in the heart that leads to arrhythmias. Unlike a heart attack, which is caused by a blockage in blood flow to the heart muscle, heart failure can affect anyone, regardless of their previous heart health. Recognizing the signs and symptoms of cardiac arrest and acting quickly is crucial, as brain damage can begin within minutes without proper blood flow.
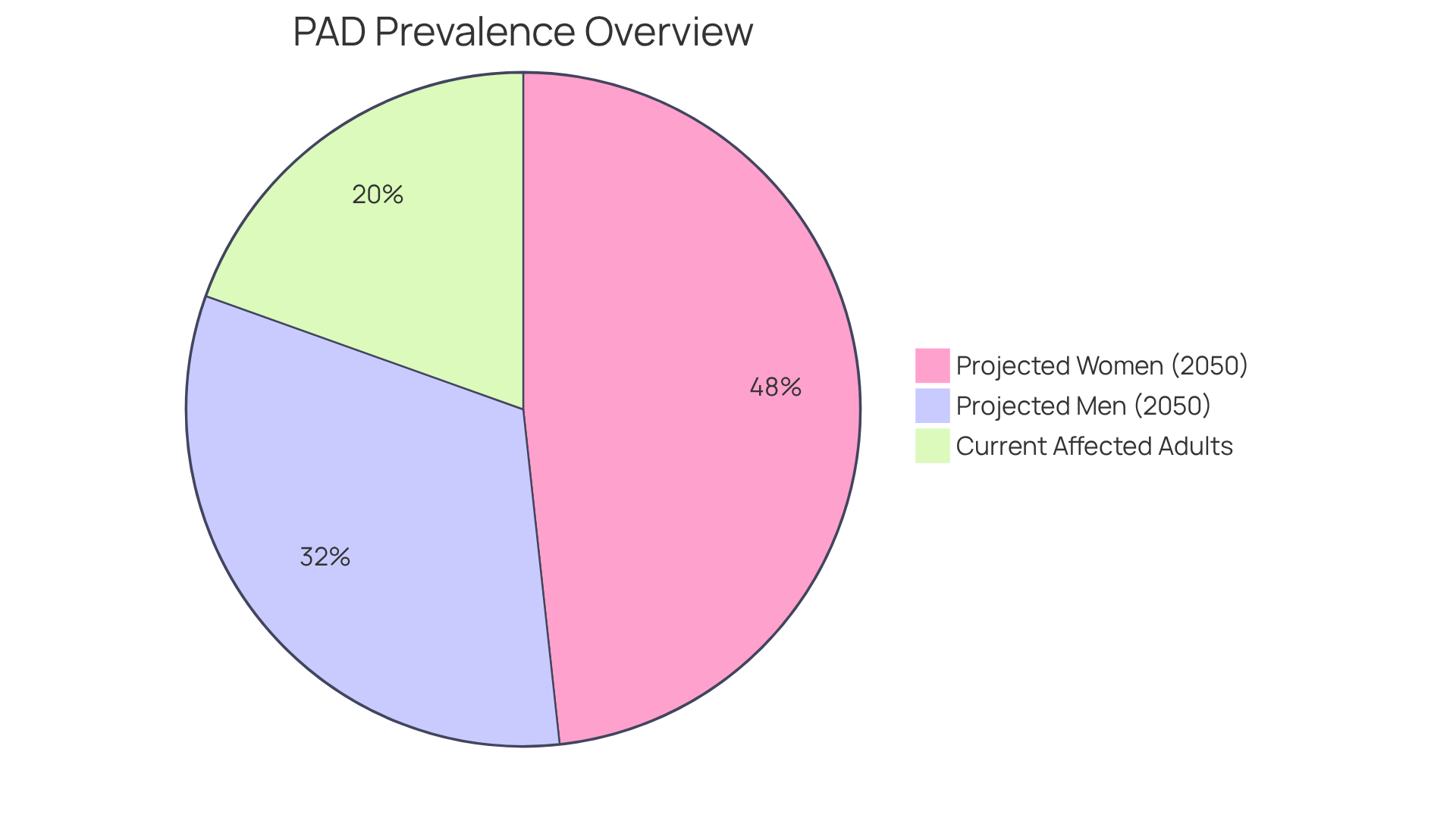
Did you know that around 350,000 out-of-hospital heart failure incidents occur each year in the United States? That’s about 1,000 Americans facing sudden heart events every single day. Recent studies show that many individuals may have warning signs of heart failure, yet the event often happens without warning. Take, for instance, Frank Toro, an 83-year-old veteran who experienced sudden heart failure right after leaving the gym. His story highlights just how unpredictable this condition can be.
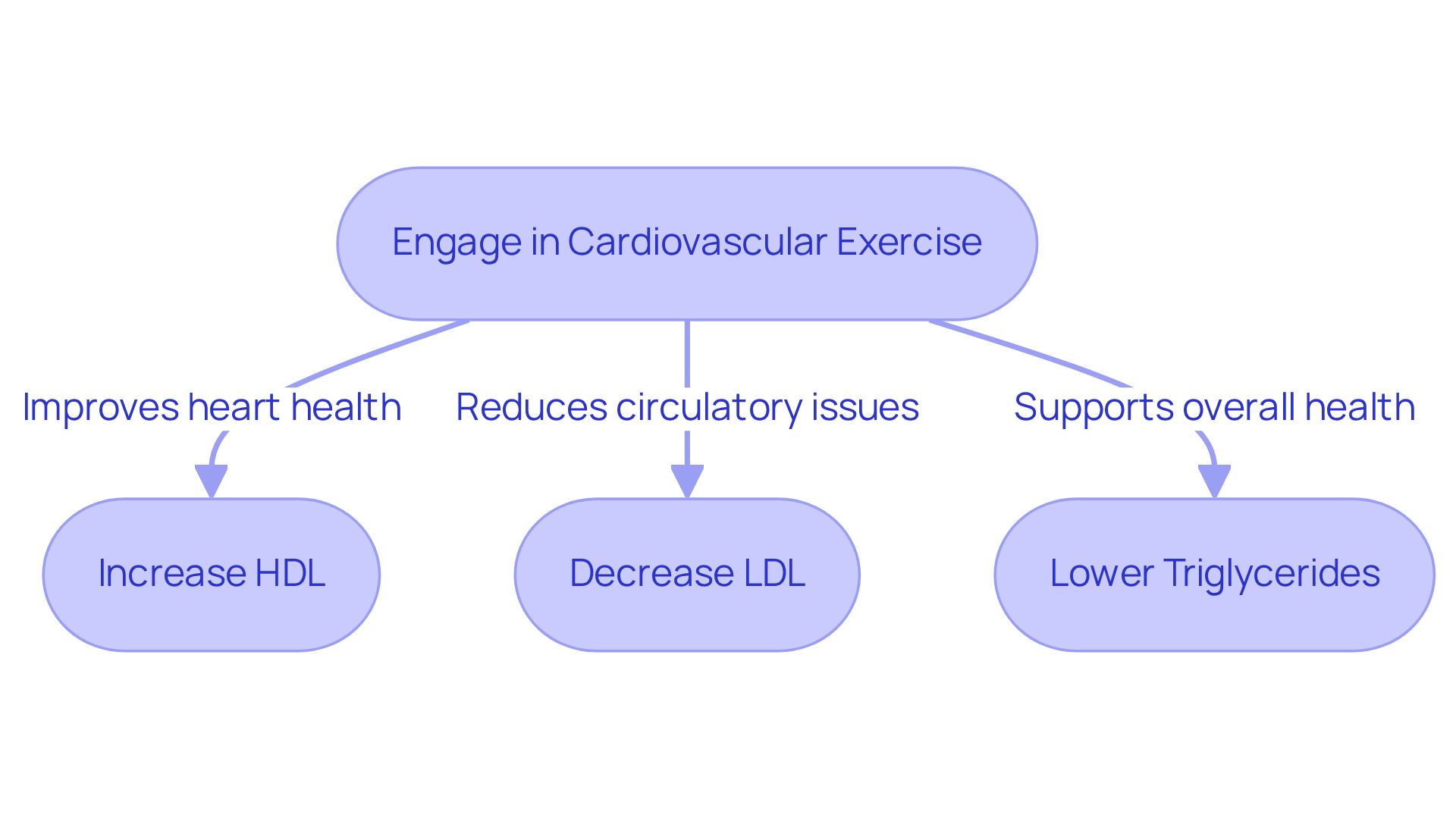
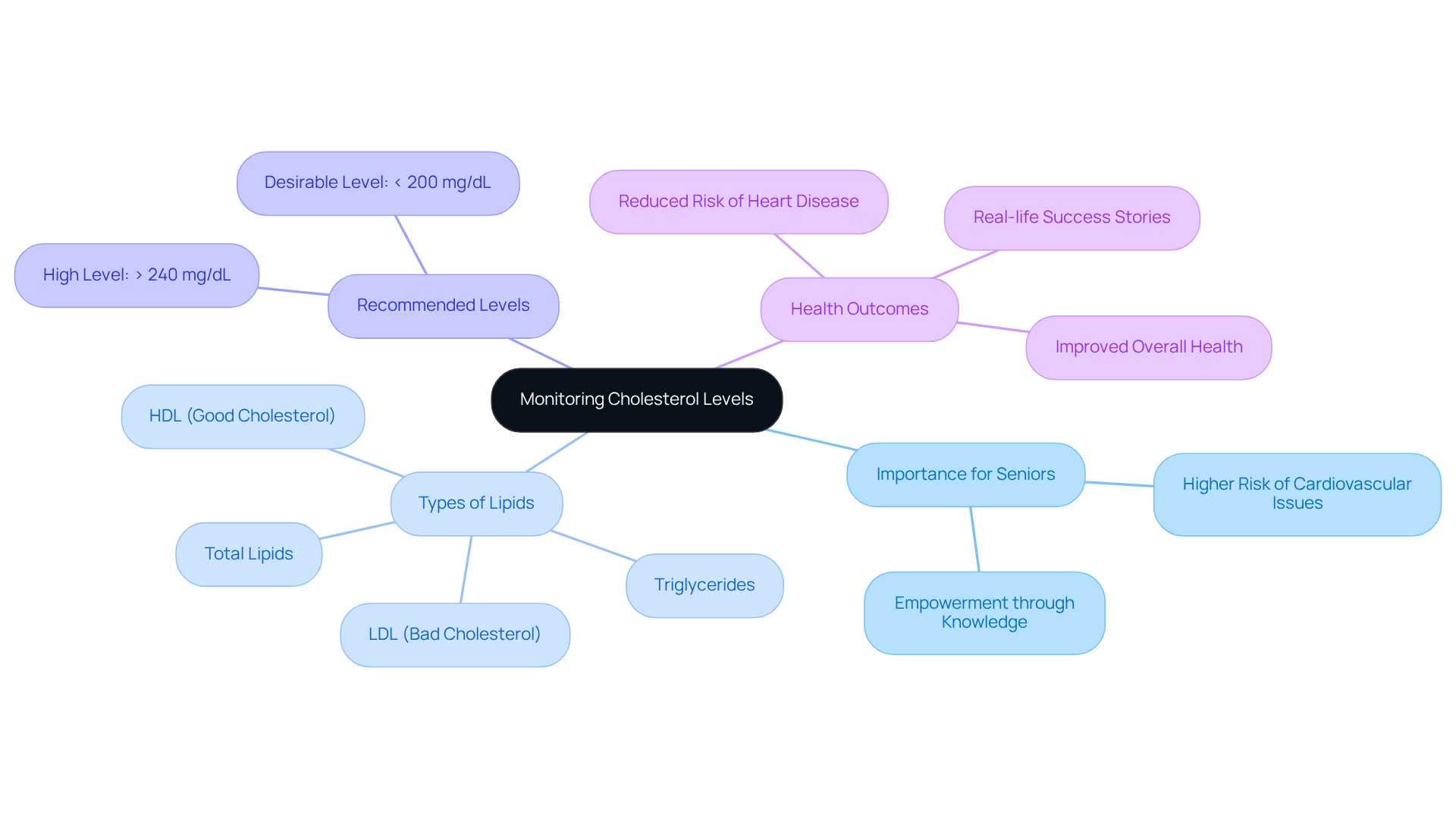
Understanding the signs and symptoms of cardiac arrest is essential for taking prompt action. Immediate CPR and access to automated external defibrillators (AEDs) can significantly improve survival rates. Symptoms like shortness of breath and fatigue during everyday activities may indicate underlying circulatory problems, such as valve disease, which could lead to a sudden heart failure if not addressed.
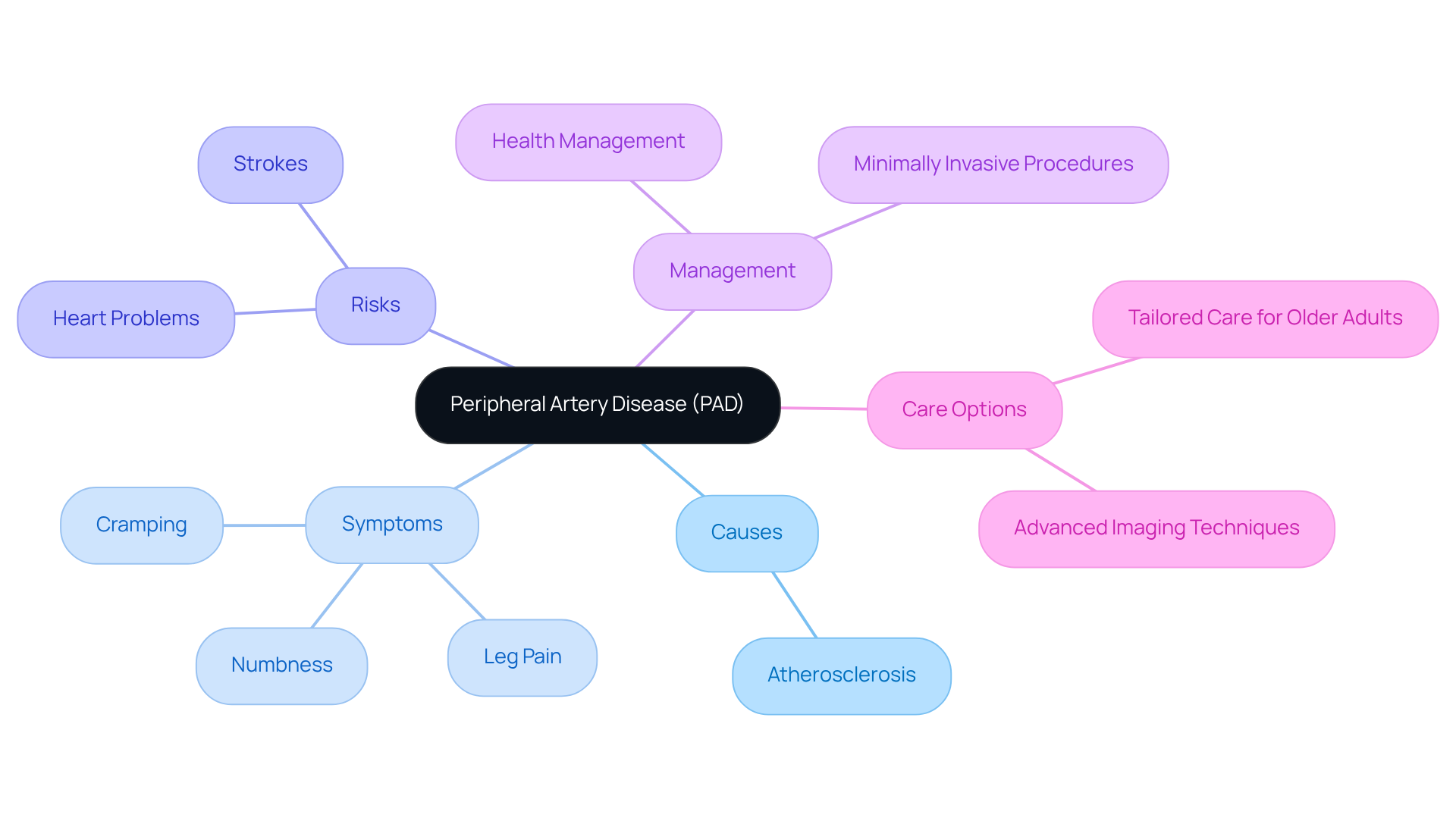
At Amavita, Dr. Pedro Martinez-Clark specializes in minimally invasive treatments tailored to address these cardiovascular issues, ensuring that high-risk patients receive comprehensive care. It’s also important to recognize the emotional toll that heart events can have on families. Many loved ones of heart attack patients experience anxiety and symptoms similar to PTSD, underscoring the need for awareness and preparedness in these situations.
If you or someone you know is experiencing concerning symptoms, don’t hesitate to reach out for support. You’re not alone in this, and there are compassionate professionals ready to help you navigate these challenges.
Identify Signs and Symptoms: Recognizing Cardiac Arrest Early
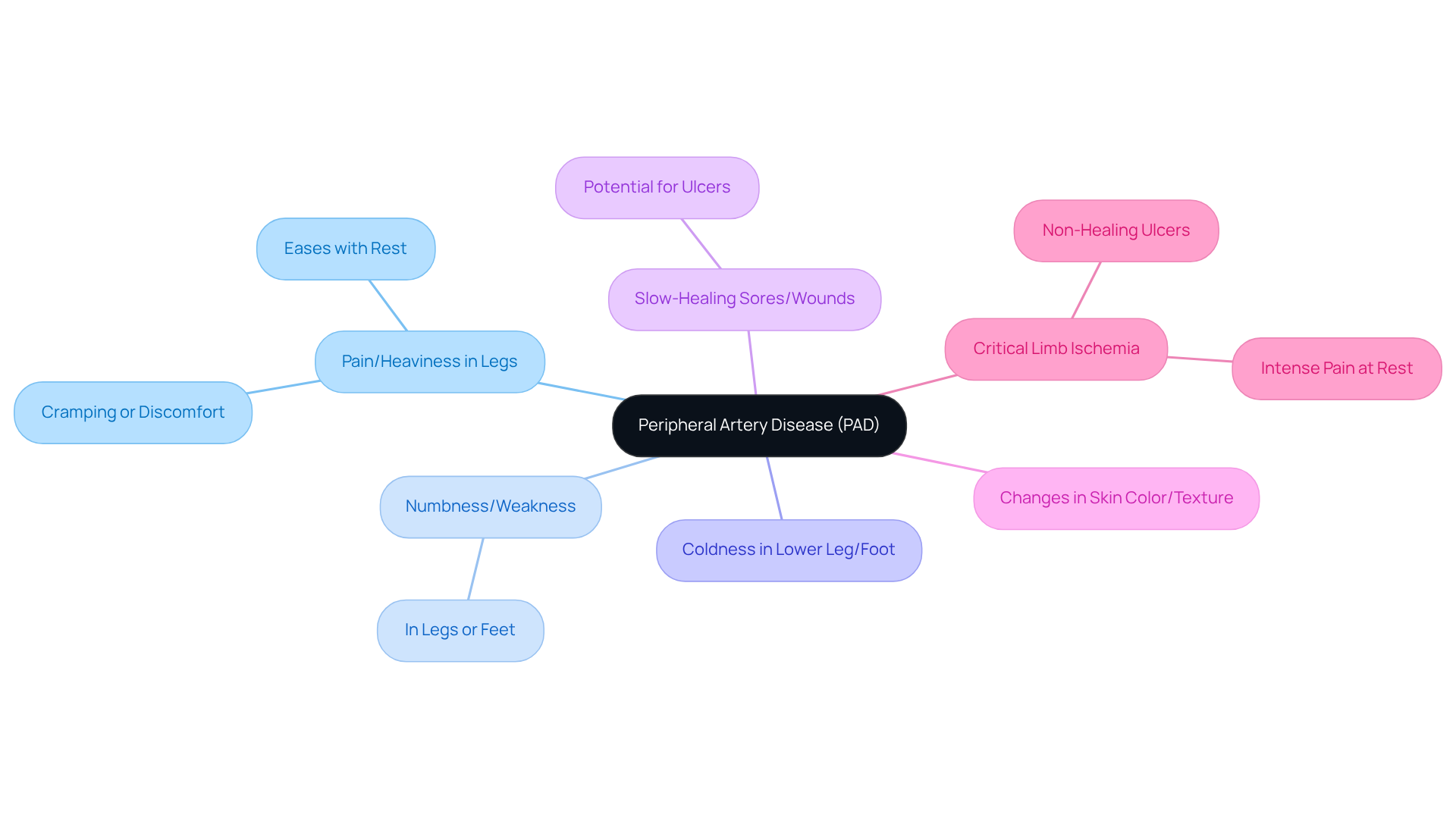
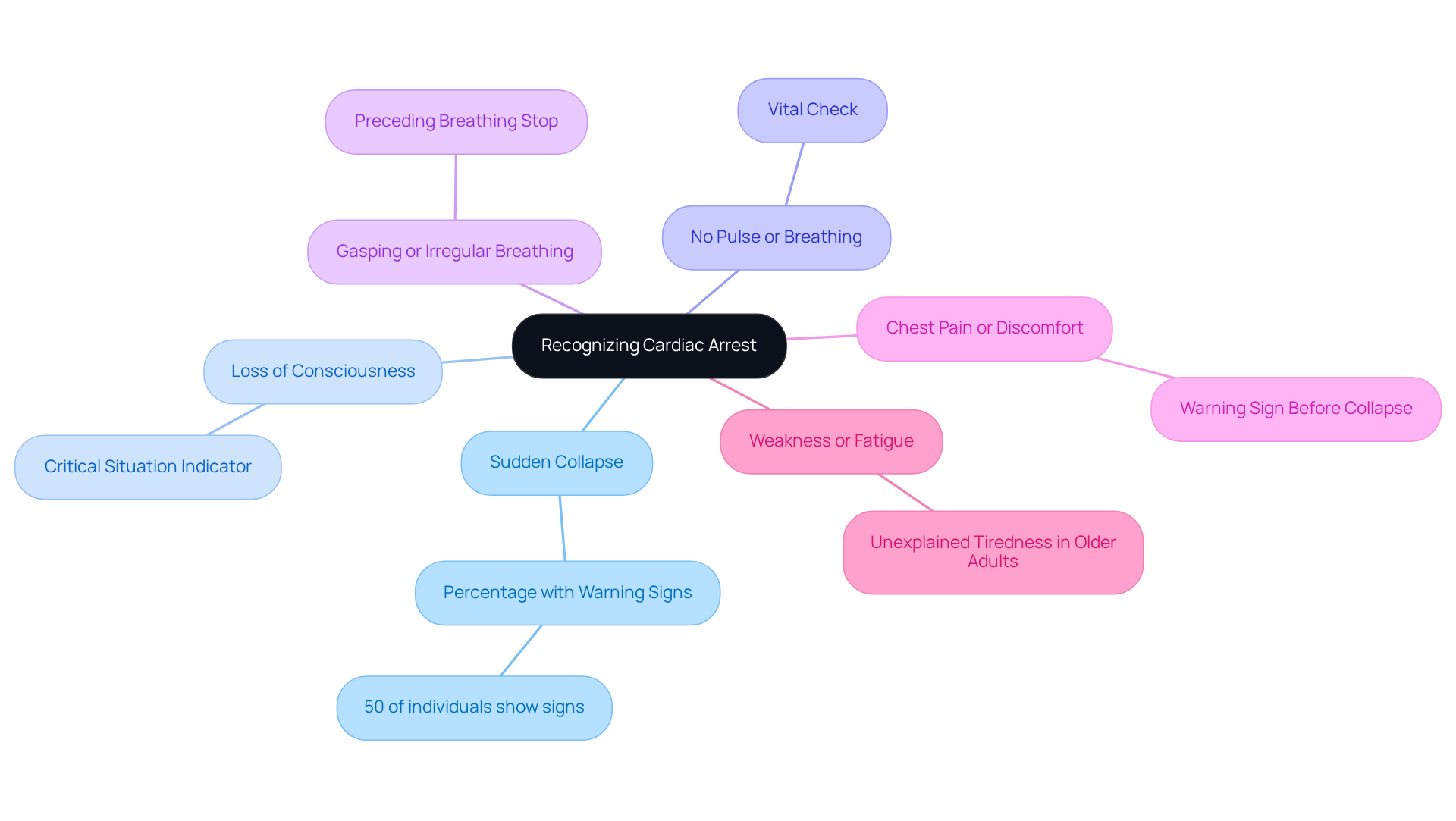
Recognizing the signs of heart failure can truly be lifesaving, especially for those at higher risk, such as individuals with diabetes, hypertension, or a family history of heart conditions. Here are some key indicators to watch for:
- Sudden collapse: If someone falls unexpectedly, it can be alarming and often happens without warning.
- Loss of consciousness: When a person doesn’t respond to verbal or physical cues, it signals a critical situation.
- No pulse or breathing: Checking for a pulse is vital; if it’s absent, the individual may be experiencing cardiac failure.
- Gasping or irregular breathing: This can occur just before breathing stops altogether, sometimes mistaken for normal breathing.
- Chest pain or discomfort: Some may feel chest pain before collapsing, which can serve as an important warning sign.
- Weakness or fatigue: Unexplained tiredness, particularly in older adults, can precede a serious event.
Research indicates that about 50% of individuals who experience sudden heart failure have warning signs beforehand, highlighting the importance of being aware. Recognizing these symptoms quickly can significantly enhance survival rates, potentially doubling them to as much as 50 percent. For instance, when bystander CPR is initiated, the chance of survival to hospital discharge rises to 13.0% for all EMS-treated non-traumatic out-of-hospital heart failures, compared to just 7.6% for those who don’t receive immediate assistance. Most heart failures are linked to existing heart issues, such as previous heart attacks or coronary artery disease, underscoring the need for vigilance.
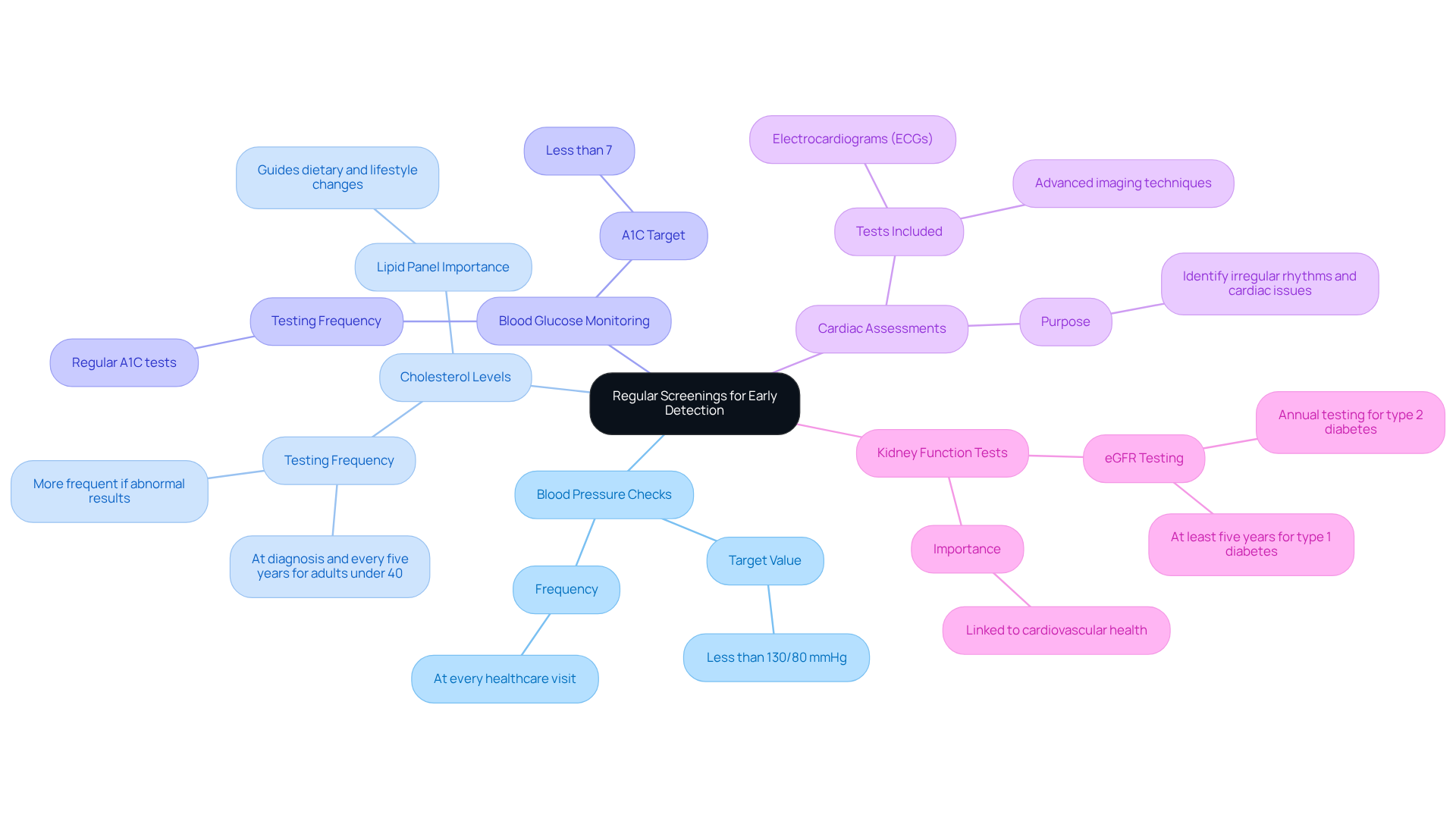
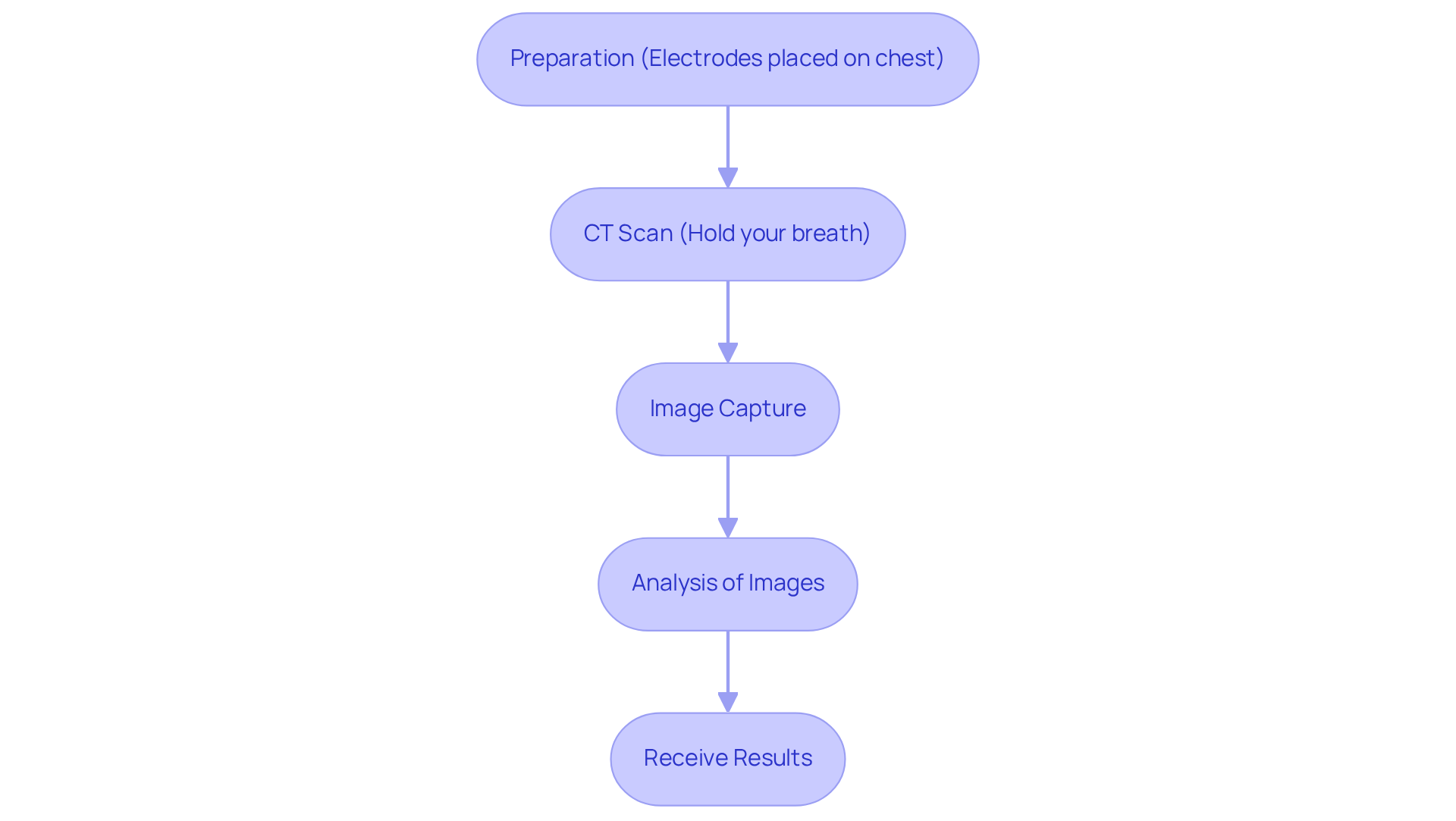
At Amavita Heart and Vascular Health, our healthcare professionals stress that understanding these symptoms enables swift action, which is crucial for survival. With advanced imaging techniques like echocardiograms and CT scans, along with thorough evaluations, we are dedicated to meeting the needs of high-risk patients, ensuring they receive the specialized cardiovascular care essential for better outcomes. Testimonials from experts reinforce the idea that recognizing these signs can truly make a difference, encouraging community members to stay alert and prepared.
Respond Promptly: Steps to Take During Cardiac Arrest
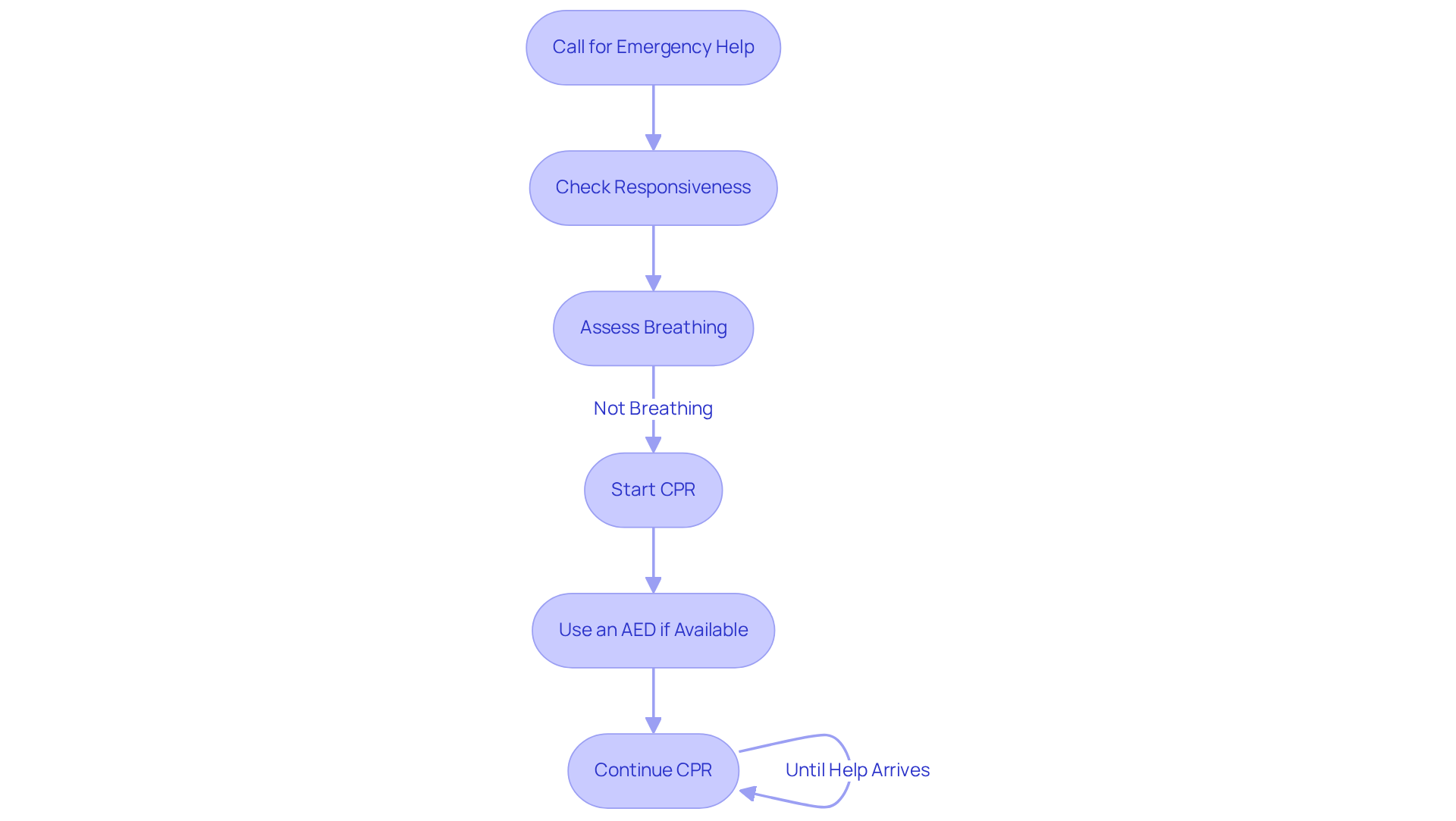
In the event of heart failure, taking swift action is crucial. Here are some essential steps to help maximize the chances of survival:
- Call for emergency help: Please dial 911 or your local emergency number right away. Getting professional assistance on the way is vital.
- Check responsiveness: Gently shake the person and call out to see if they respond. If there’s no response, move on to the next step.
- Assess breathing: Look for signs of normal breathing. If the person isn’t breathing or is only gasping, these are signs and symptoms of cardiac arrest, and it’s time to prepare for CPR.
- Start CPR: Begin chest compressions at a rate of 100-120 per minute. Push hard and fast in the center of the chest, allowing full recoil between compressions to keep blood flowing to vital organs. Remember, prompt CPR can double or even triple the chances of survival for someone experiencing heart failure, underscoring the importance of acting quickly and effectively.
- Use an AED if available: If there’s an Automated External Defibrillator (AED) nearby, turn it on and follow the voice prompts. Early defibrillation can greatly enhance survival rates.
- Continue CPR: Keep performing CPR until emergency personnel arrive or the person shows signs of life, like breathing or movement.
These steps are essential for identifying the signs and symptoms of cardiac arrest to maintain blood flow to the brain and other organs until help arrives. As Stacey E. Rosen, M.D., points out, the American Heart Association is working to create a “Nation of Lifesavers” by empowering more individuals to confidently provide CPR when they witness someone in distress. It’s important to remember that around 350,000 people in the U.S. experience out-of-hospital heart failures each year, with a staggering 90% mortality rate. This highlights just how urgent these actions are.
Understand Risk Factors: Who is at Higher Risk for Cardiac Arrest?
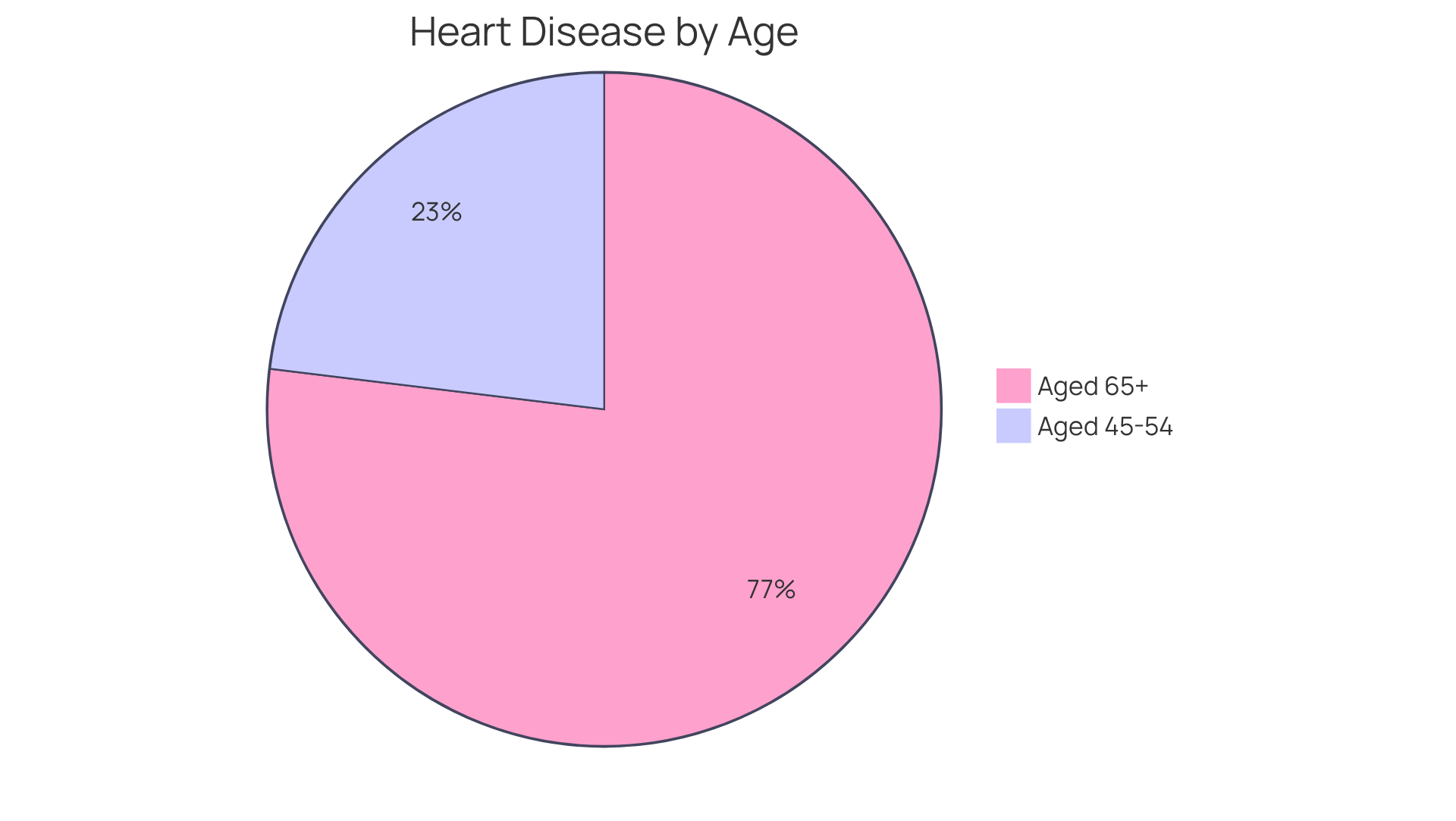
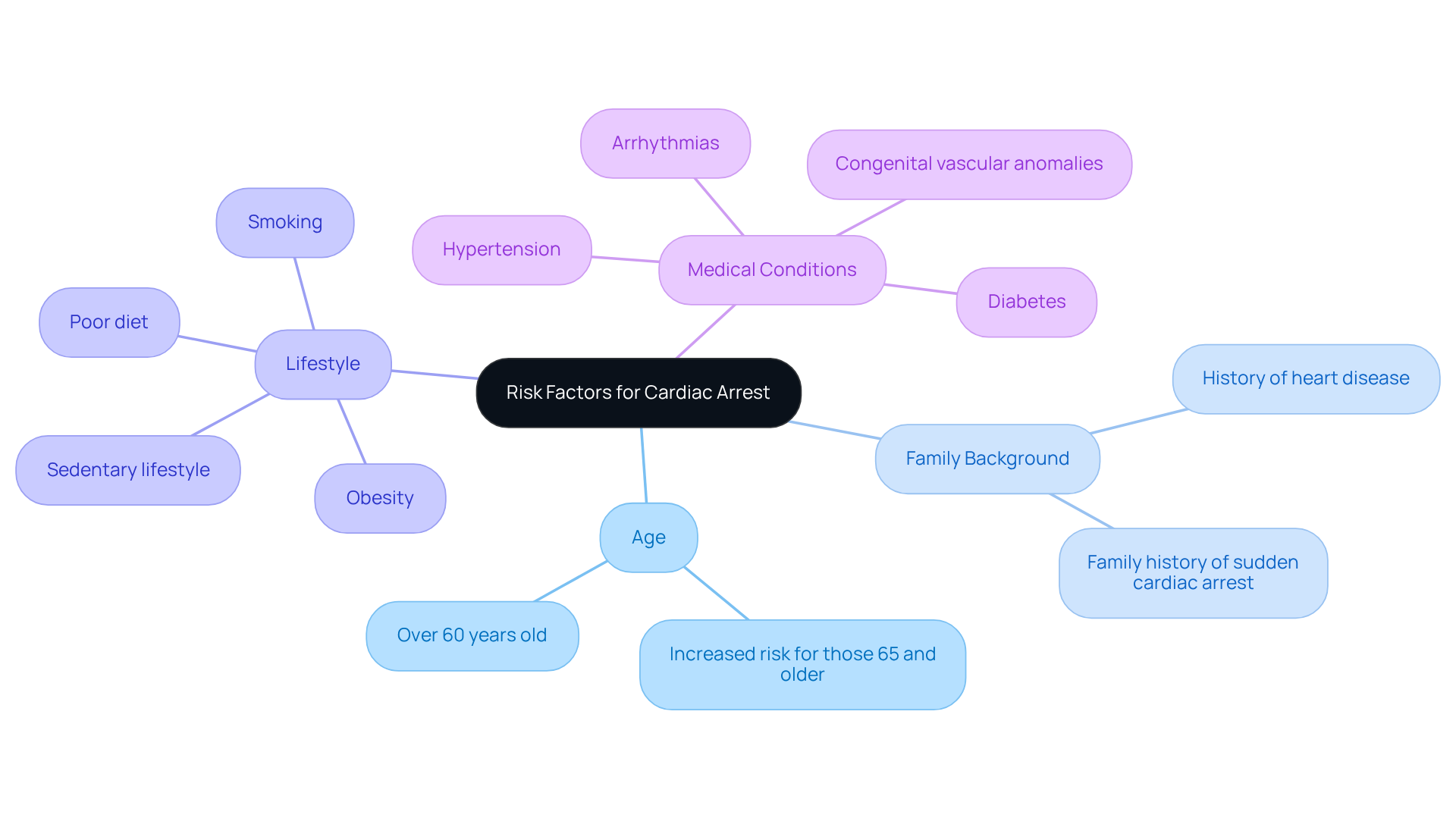
As we age, our hearts can face increased challenges, especially for those over 60. Did you know that about 66% of sudden heart failure incidents occur in this age group? This highlights just how important it is to pay attention to our cardiovascular health. Here are some key risk factors to consider:
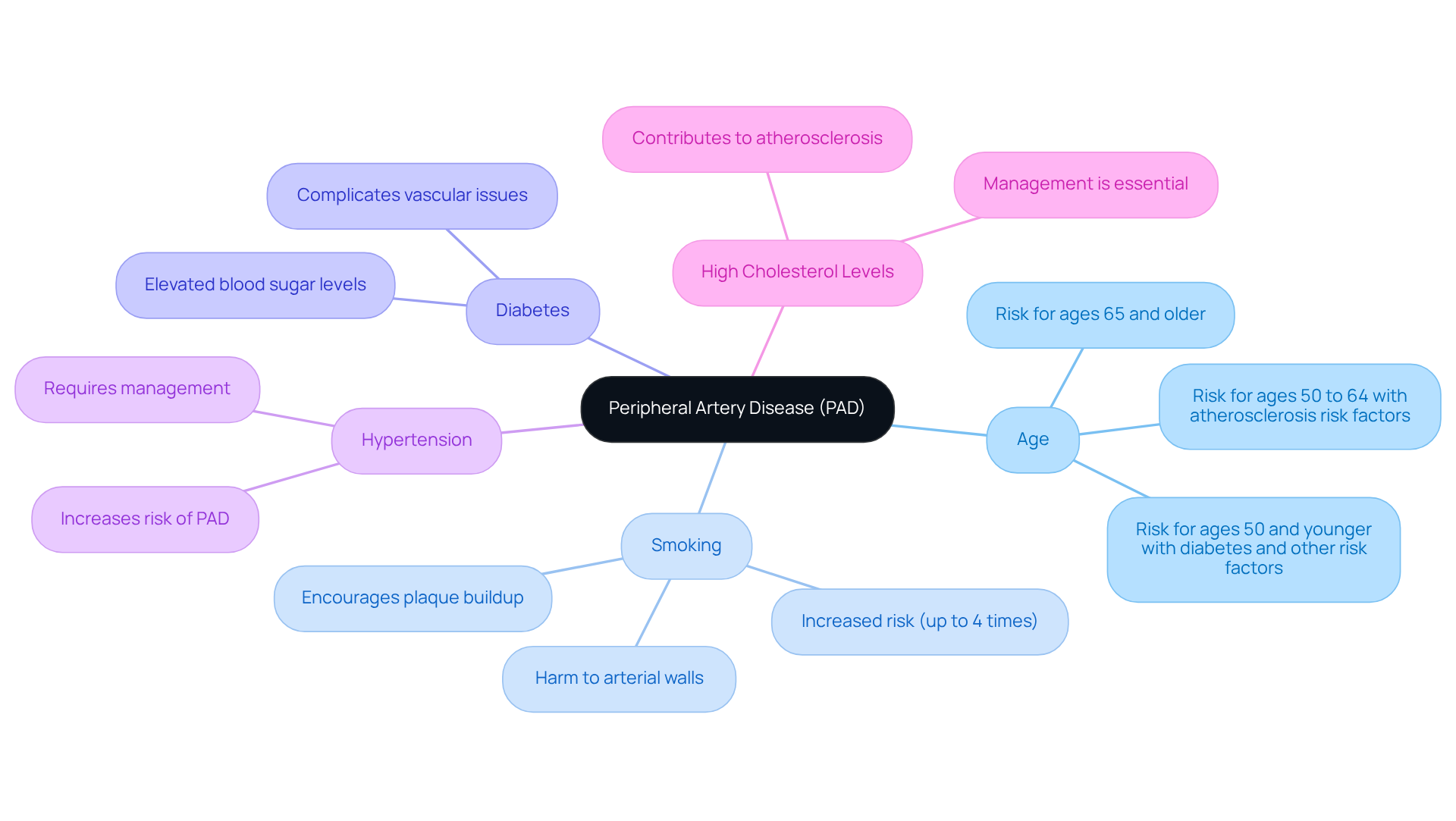
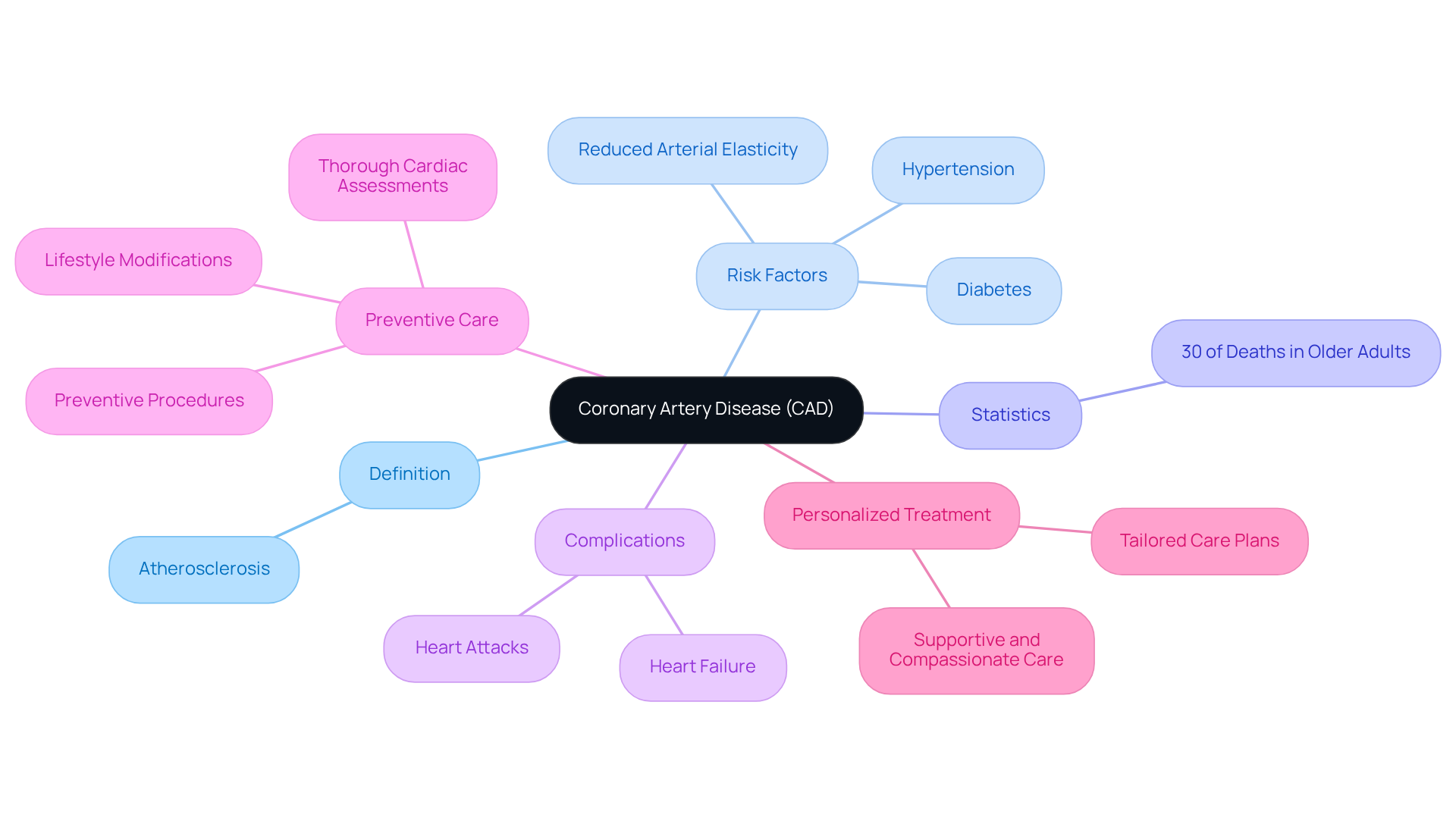
- Age: If you’re 65 or older, your risk for cardiac arrest rises significantly. Having a history of cardiac disease, such as coronary artery disease, heart failure, or previous heart attacks, can greatly increase your risk of developing signs and symptoms of cardiac arrest.
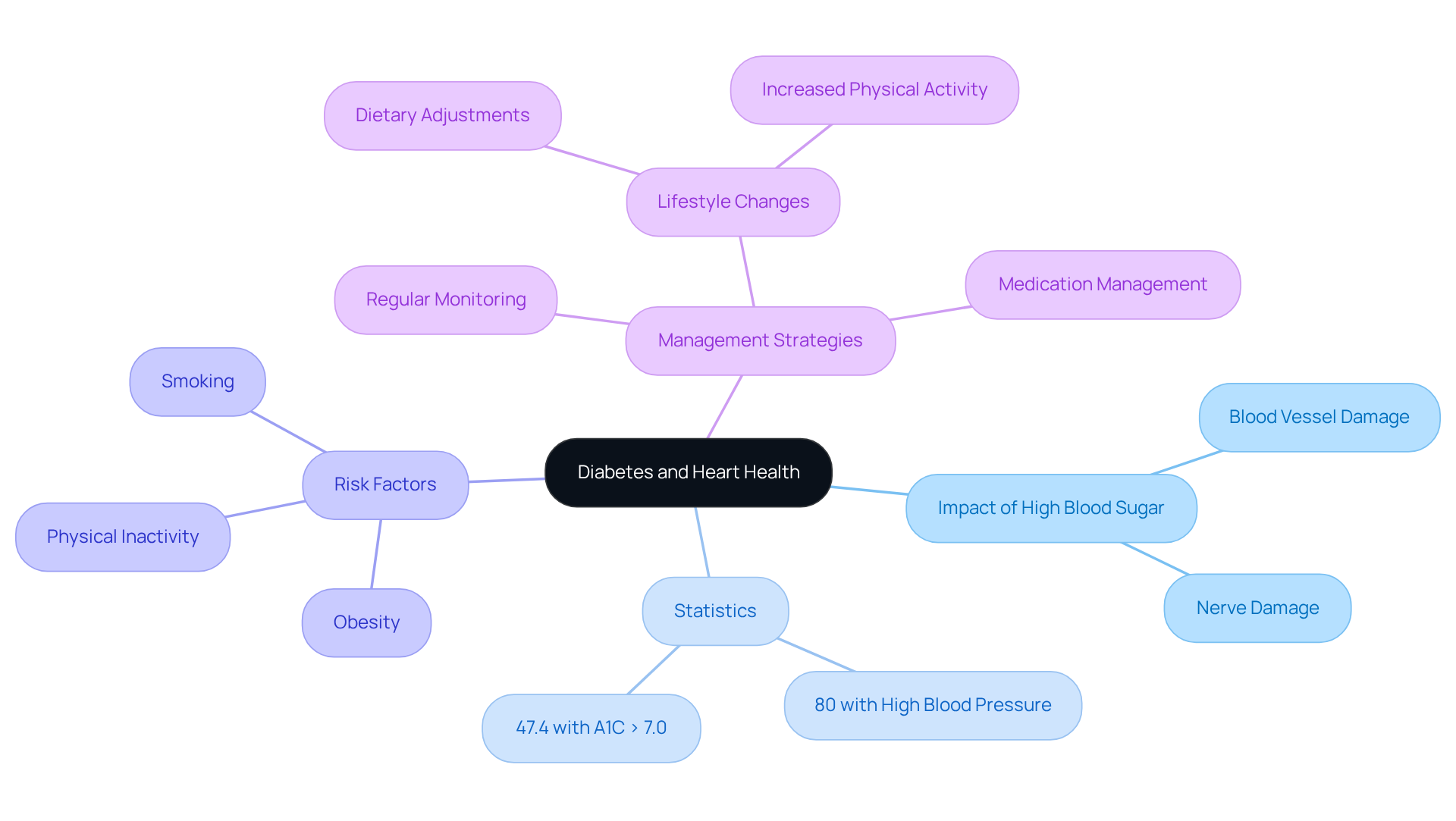
- Family background: If heart disease runs in your family, it’s essential to be aware of your own risk levels. Lifestyle factors such as smoking, obesity, high blood pressure, and diabetes can all contribute to the development of signs and symptoms of cardiac arrest. For instance, hypertension affects over 70% of people aged 70 and above, making it a common concern.
- Sedentary lifestyle: Not staying active can weaken your heart health, so regular exercise is crucial.
- Certain medical conditions: Issues like arrhythmias or congenital vascular anomalies can also put you at risk.
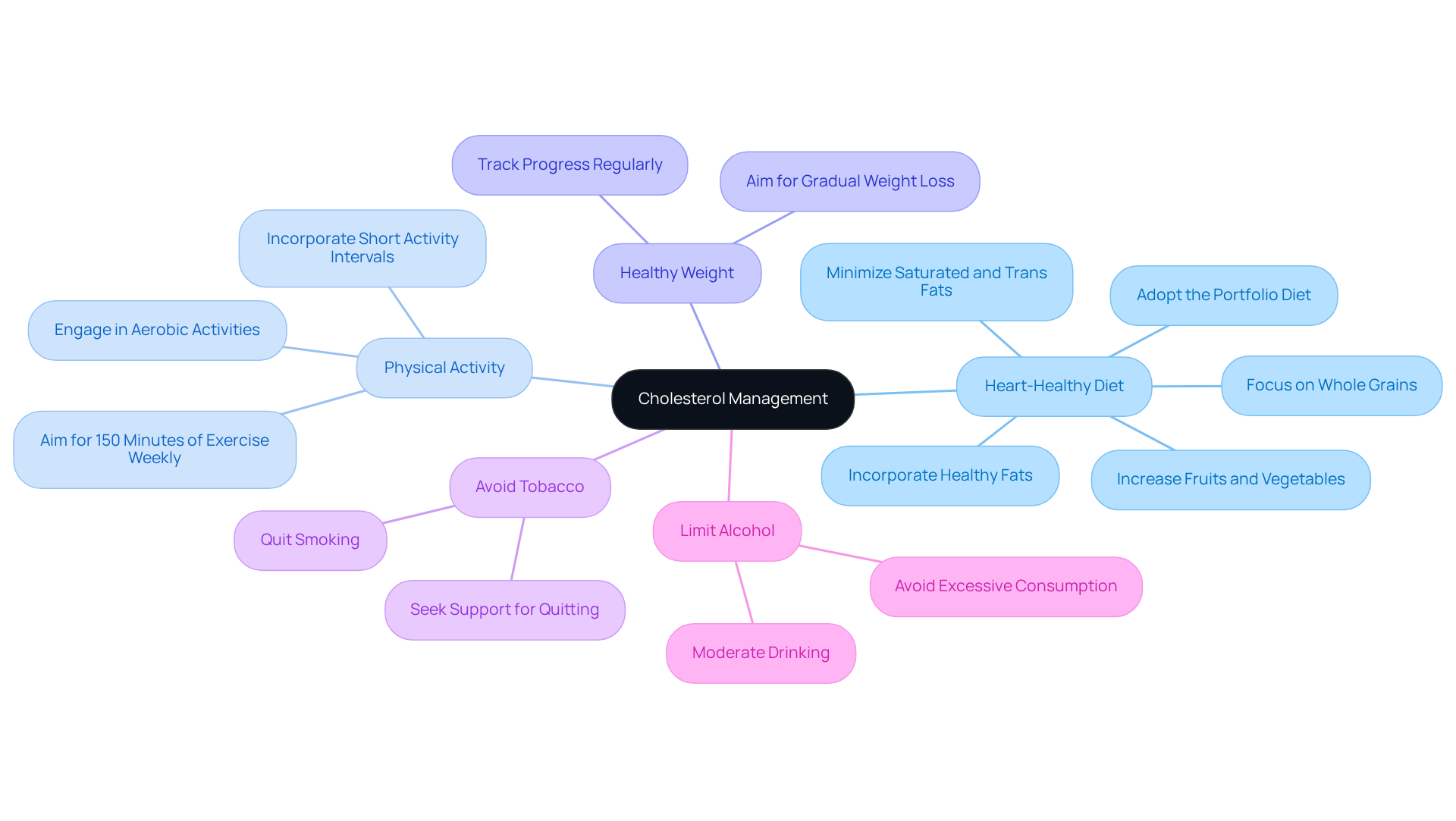
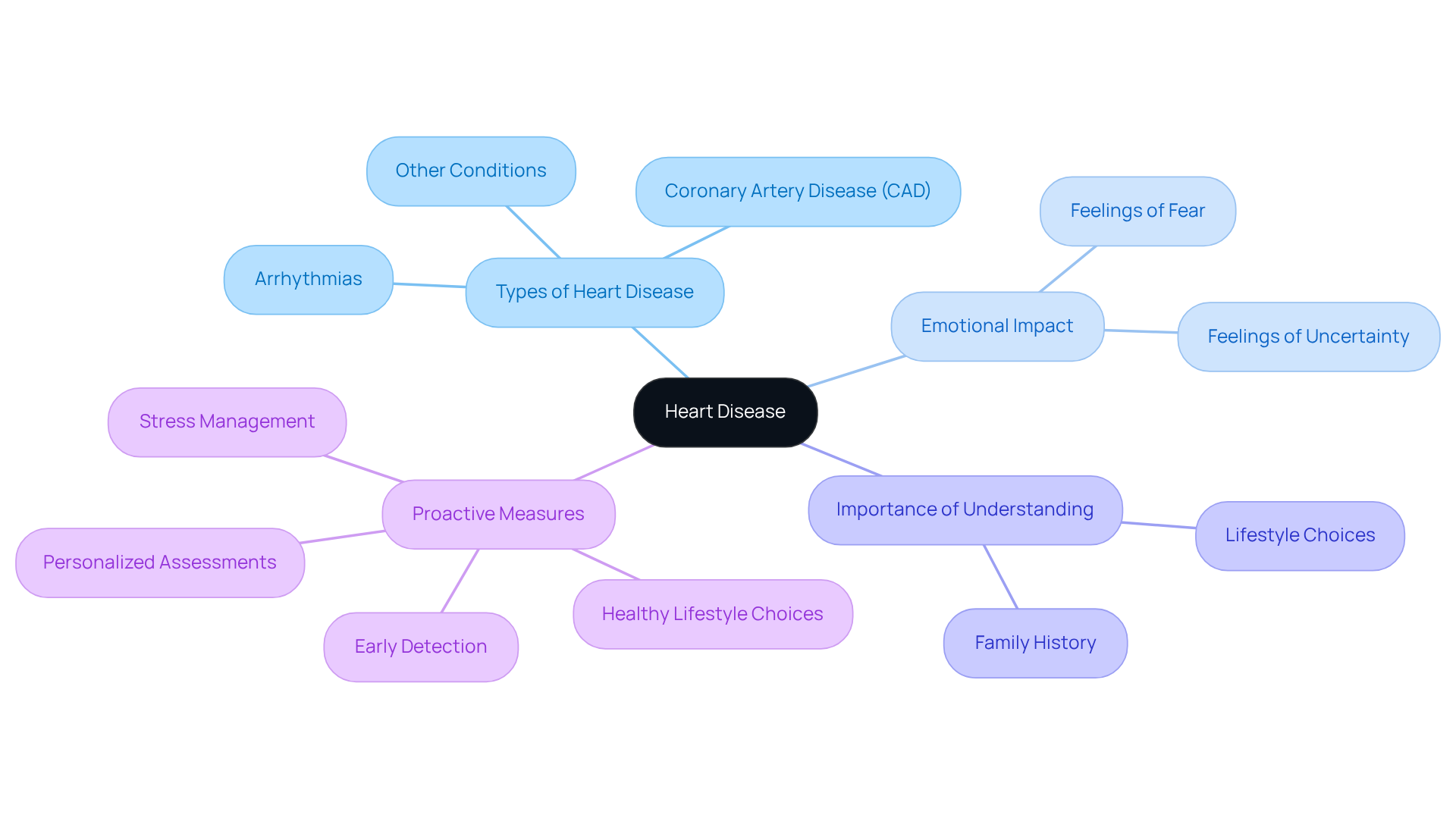
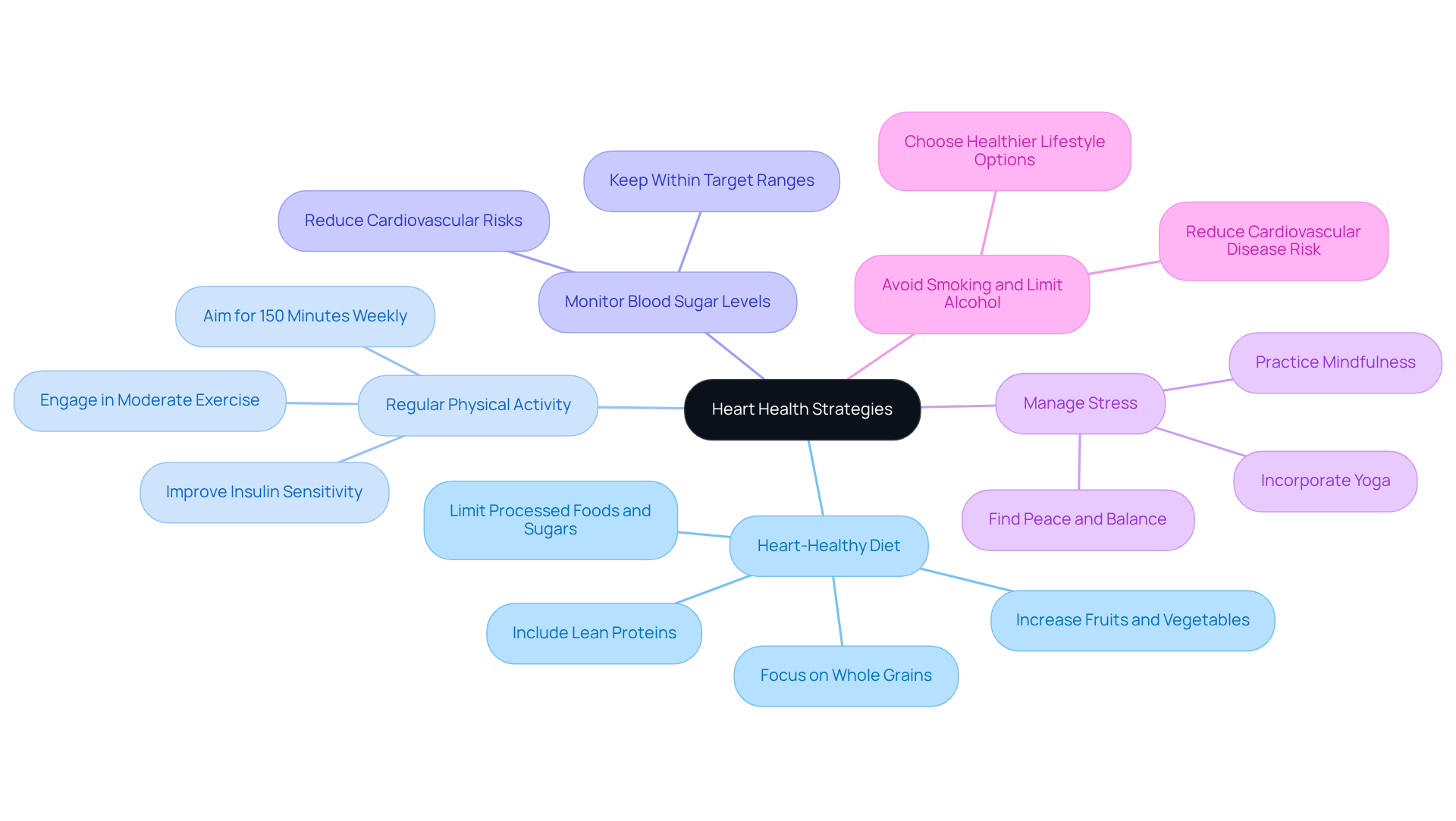
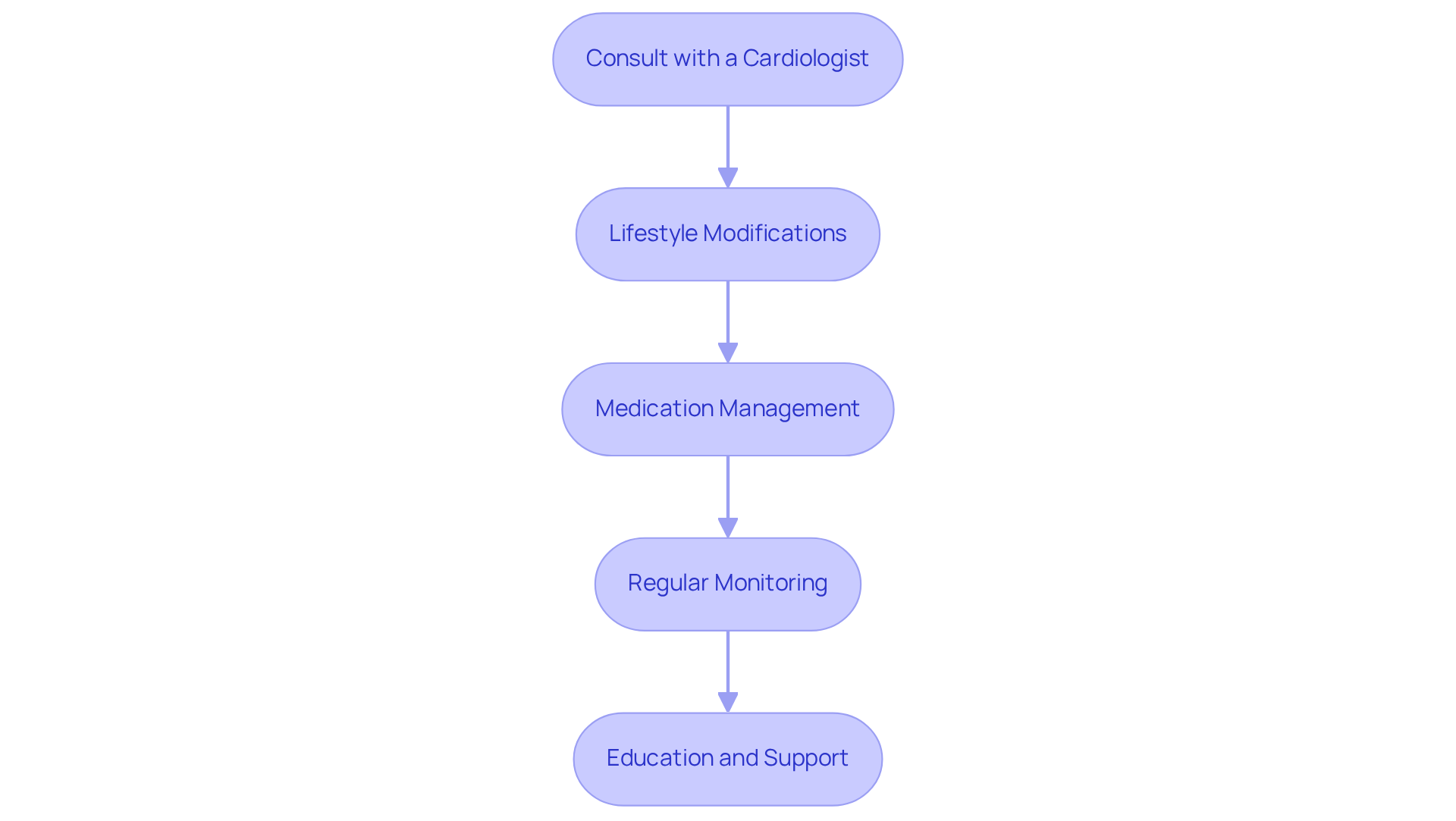
Understanding these factors is vital for managing your heart health effectively. Making lifestyle changes, such as embracing a balanced diet and increasing physical activity, can significantly lower your risk of heart-related events. Programs like Amavita’s Comprehensive and Optimal Programs, along with the CardioElite™ program, offer advanced heart health monitoring and proactive management strategies. These resources ensure that older adults receive the support they need to manage these risks effectively.
The American Heart Association’s Life’s Essential 8 emphasizes the importance of a healthy diet, regular exercise, adequate sleep, and stress management in preventing cardiovascular disease. It’s also crucial to consult with your healthcare provider about your personal risk factors and preventive strategies. Remember, you’re not alone in this journey; there are caring professionals ready to help you enhance your cardiovascular health.
Conclusion
Recognizing the signs and symptoms of cardiac arrest is crucial for ensuring timely intervention in a life-threatening situation. This medical emergency can strike unexpectedly, and understanding its indicators can significantly enhance survival rates. By being aware of critical signs, such as:
- Sudden collapse
- Loss of consciousness
- Absence of pulse or breathing
you can act swiftly and effectively, potentially saving lives.
When faced with a cardiac arrest scenario, immediate action is essential. Key steps include:
- Calling for emergency help
- Assessing the person’s responsiveness and breathing
- Initiating CPR
Remember, nearly half of those who experience sudden cardiac events may show warning signs. This makes awareness and prompt response even more vital. Additionally, understanding risk factors – like age, family history, and lifestyle choices – can empower you to take proactive measures in managing your heart health.
Ultimately, the fight against cardiac arrest is a collective responsibility. By educating yourself and others about the symptoms, risks, and appropriate responses, we can foster a culture of preparedness in our communities. Encouraging conversations about heart health and promoting training in CPR and the use of AEDs can lead to more lifesavers among us. Embracing these actions not only enhances personal safety but also contributes to a broader movement towards reducing the impact of cardiac arrest in our lives.
Frequently Asked Questions
What is cardiac arrest?
Cardiac arrest is a serious medical emergency where the heart suddenly stops pumping blood, putting vital organs at risk due to a lack of blood flow. It can occur unexpectedly, often due to an electrical malfunction in the heart.
How does cardiac arrest differ from a heart attack?
Cardiac arrest occurs when the heart stops pumping blood, while a heart attack is caused by a blockage in blood flow to the heart muscle. Cardiac arrest can affect anyone, regardless of their previous heart health.
What are the signs and symptoms of cardiac arrest?
Signs and symptoms of cardiac arrest can include shortness of breath, fatigue during everyday activities, and other circulatory problems. Recognizing these symptoms is crucial for taking prompt action.
How common is cardiac arrest in the United States?
Approximately 350,000 out-of-hospital cardiac arrest incidents occur each year in the United States, equating to about 1,000 cases every day.
What should be done if someone experiences cardiac arrest?
Immediate CPR and access to automated external defibrillators (AEDs) can significantly improve survival rates in cases of cardiac arrest.
What underlying conditions can lead to cardiac arrest?
Underlying circulatory problems, such as valve disease, can lead to sudden cardiac arrest if not addressed.
How can emotional support be important in cases of cardiac arrest?
Families of heart attack patients often experience anxiety and symptoms similar to PTSD, highlighting the importance of emotional support and preparedness in these situations.
Who can help if someone is experiencing concerning symptoms related to cardiac health?
Compassionate professionals, such as those specializing in cardiovascular care, are available to help individuals navigate challenges related to cardiac health.
List of Sources
- Define Cardiac Arrest: Understanding the Medical Emergency
- What is cardiac arrest? Why is it so deadly? (https://newsroom.heart.org/news/what-is-cardiac-arrest)
- CPR Facts and Stats (https://cpr.heart.org/en/resources/cpr-facts-and-stats)
- Sudden cardiac arrest requires luck to survive. Scientists hope to turn those odds around (https://statnews.com/2024/08/14/sudden-cardiac-arrest-research-cardiovascular-risk-factors-improve-survival-rate)
- American Heart Association backs new research that could transform cardiac outcomes for hundreds of thousands of Americans | CWRU Newsroom | Case Western Reserve University (https://case.edu/news/american-heart-association-backs-new-research-could-transform-cardiac-outcomes-hundreds-thousands-americans)
- Latest Statistics (https://sca-aware.org/about-sudden-cardiac-arrest/latest-statistics)
- Identify Signs and Symptoms: Recognizing Cardiac Arrest Early
- CPR Facts and Stats (https://cpr.heart.org/en/resources/cpr-facts-and-stats)
- Watch for Cardiac Arrest Warning Signs (https://virtua.org/articles/watch-for-cardiac-arrest-warning-signs)
- Sudden cardiac arrest: Key warning signs and how to respond (https://uab.edu/news/news-you-can-use/sudden-cardiac-arrest-key-warning-signs-and-how-to-respond)
- Latest Statistics (https://sca-aware.org/about-sudden-cardiac-arrest/latest-statistics)
- Cardiac Arrest Many People Experience Warning Signs the Day Before (https://powershealth.org/about-us/newsroom/health-library/2023/08/30/cardiac-arrest-many-people-experience-warning-signs-the-day-before)
- Respond Promptly: Steps to Take During Cardiac Arrest
- What’s new in the latest CPR guidelines? – Harvard Health (https://health.harvard.edu/heart-health/whats-new-in-the-latest-cpr-guidelines)
- Updated CPR guidelines tackle choking response, opioid-related emergencies and a revised Chain of Survival (https://newsroom.heart.org/news/updated-cpr-guidelines-tackle-choking-response-opioid-related-emergencies-and-a-revised-chain-of-survival)
- Public preparedness key to improving cardiac arrest survival (https://news-medical.net/news/20260212/Public-preparedness-key-to-improving-cardiac-arrest-survival.aspx)
- Understand Risk Factors: Who is at Higher Risk for Cardiac Arrest?
- Heart Disease Facts (https://cdc.gov/heart-disease/data-research/facts-stats)
- Latest Statistics (https://sca-aware.org/about-sudden-cardiac-arrest/latest-statistics)
- Heart attack age: Risk by age group (https://medicalnewstoday.com/articles/heart-attack-age-range)
- Blog : News & Media : Starting Hearts (https://startinghearts.org/news-events/blog.html/article/2024/02/22/sudden-cardiac-arrest-knowing-is-half-the-battle)
- Hidden Triggers of Cardiovascular Disease in Older Adults (https://pcna.net/news/unraveling-the-hidden-triggers-of-cardiovascular-risk-in-older-adults)