Introduction
Bradycardia, which means a slower-than-normal heart rate, can be concerning, especially for our elderly loved ones. It often brings about troubling physical symptoms like fatigue, dizziness, and even fainting. Recognizing these symptoms is essential, as they might indicate underlying health issues that need immediate attention. But how can we tell when these signs point to a more serious problem that requires medical help?
As caregivers and family members, it’s vital to stay alert and informed. By understanding the nuances of bradycardia, we can better support our loved ones. What steps can we take to ensure their well-being while navigating these complexities? It’s important to foster an environment where they feel safe discussing their health concerns.
In addition to being observant, we can encourage open conversations about any symptoms they may experience. This not only helps in recognizing potential issues early but also reassures them that they are not alone in this journey. Remember, your support can make a significant difference in their lives.
Define Bradycardia and Its Importance in Heart Health
Bradycardia, or a slower-than-usual pulse rate, typically falls below 60 beats per minute. For older individuals, this condition can be particularly concerning. It may lead to complications, which can cause physical symptoms, including fatigue, dizziness, and fainting. Understanding the symptoms is crucial, as they can indicate underlying issues, including heart disease or other cardiovascular conditions.
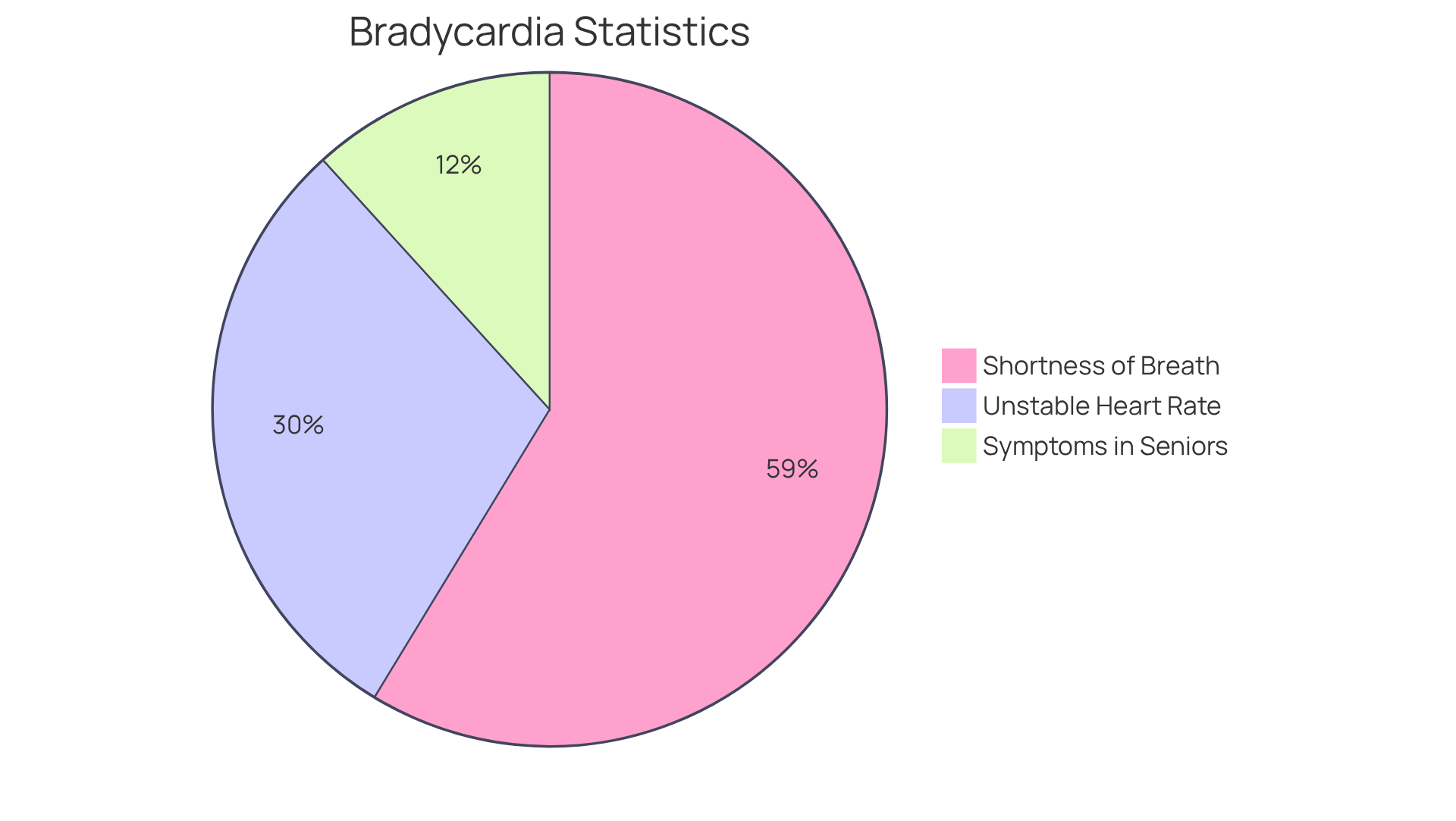
Did you know that about 10% of patients who visit emergency departments show symptoms of a slow heart rate? This statistic comes from a study involving 3,297 individuals. Furthermore, a significant 15.61% of these cases experience an unstable heart rate. Among those with unstable slow heart rates, shortness of breath is the most common symptom, affecting over 31% of people. Alarmingly, 30% of individuals with unstable slow heart rates passed away during hospitalization from causes unrelated to their condition.
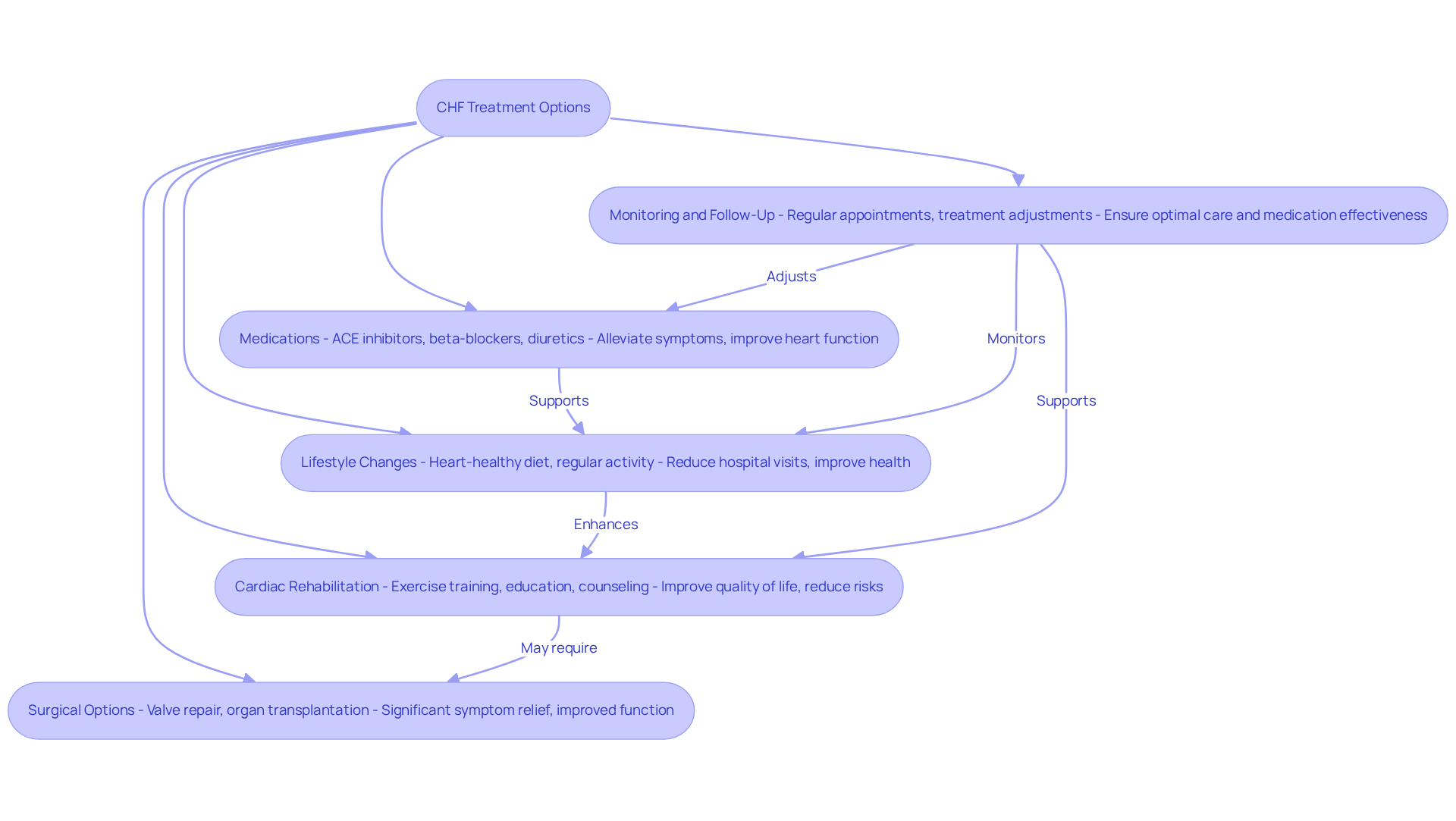
Timely identification and management of bradycardia can improve quality of life. At Amavita Heart and Vascular Health, we prioritize education and preventive strategies to address these concerns. Our dedicated team focuses on innovative, minimally invasive therapies for bradycardia, which can alleviate issues like shortness of breath and fatigue, ultimately enhancing the quality of life for our seniors.
Through our comprehensive programs, we offer a holistic approach to cardiac care, ensuring proactive management and minimizing readmissions. This way, we’re transforming the landscape of cardiac health for those we serve. If you or a loved one are experiencing symptoms, please reach out to us. We’re here to support you every step of the way.
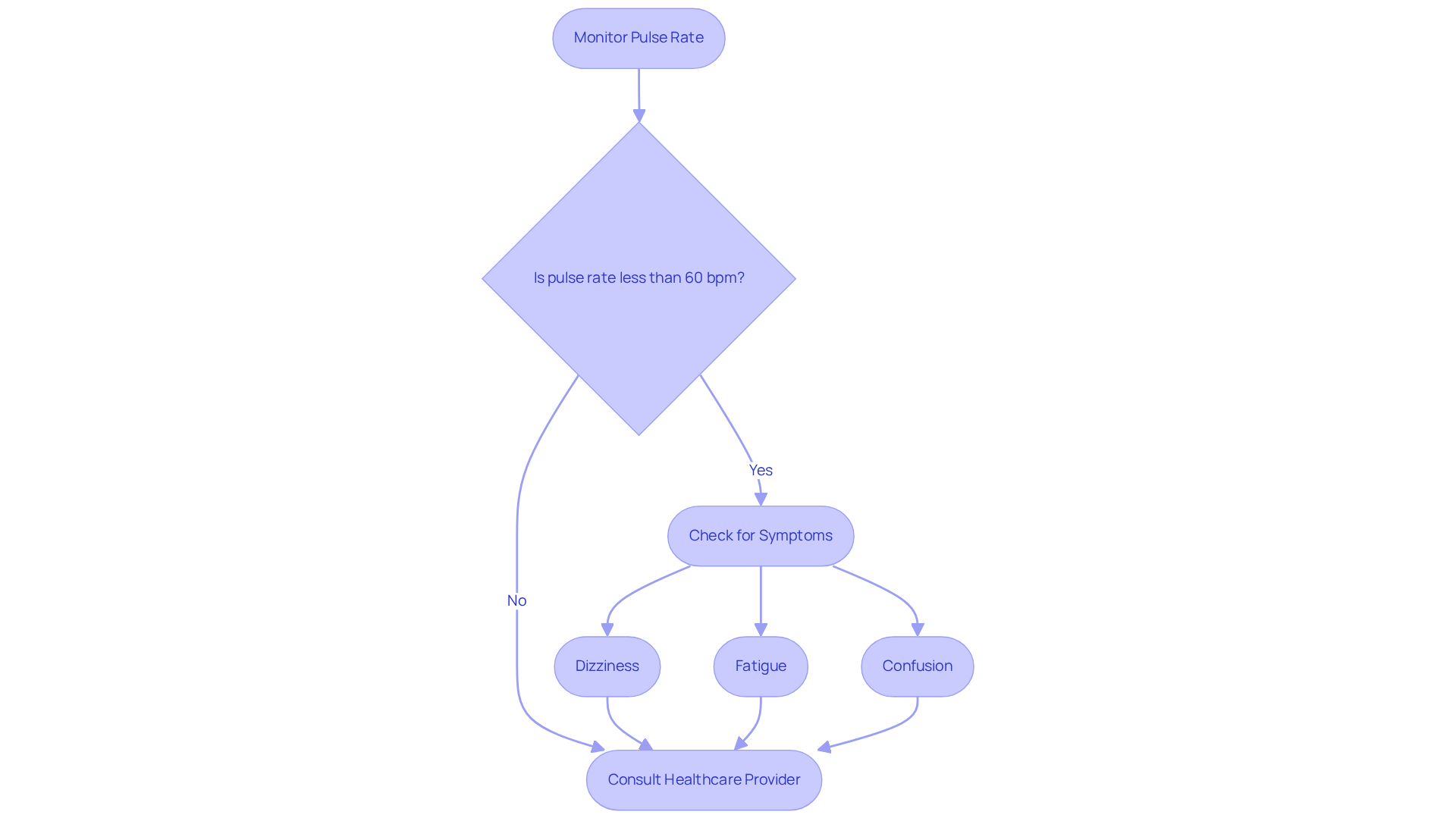
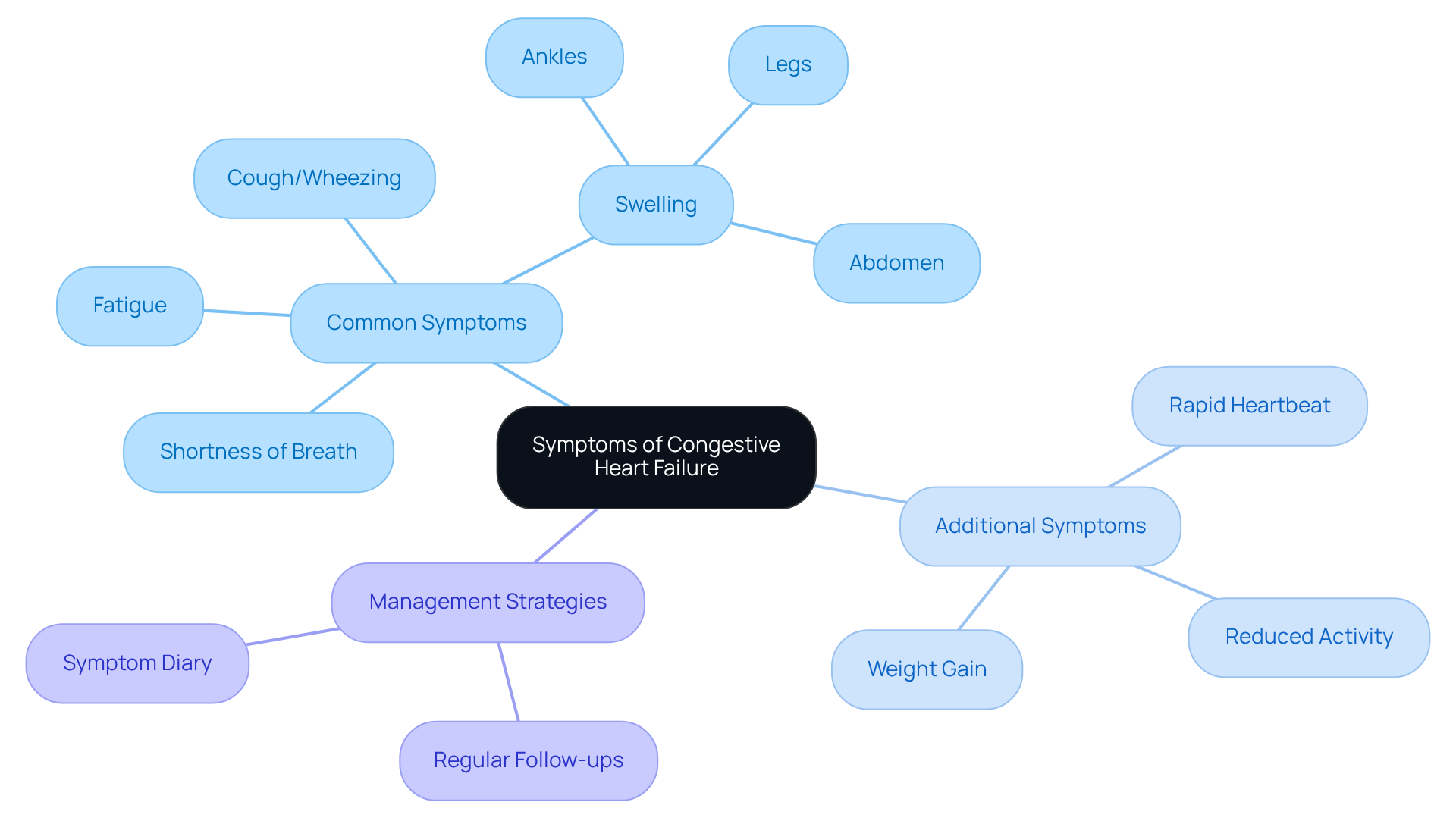
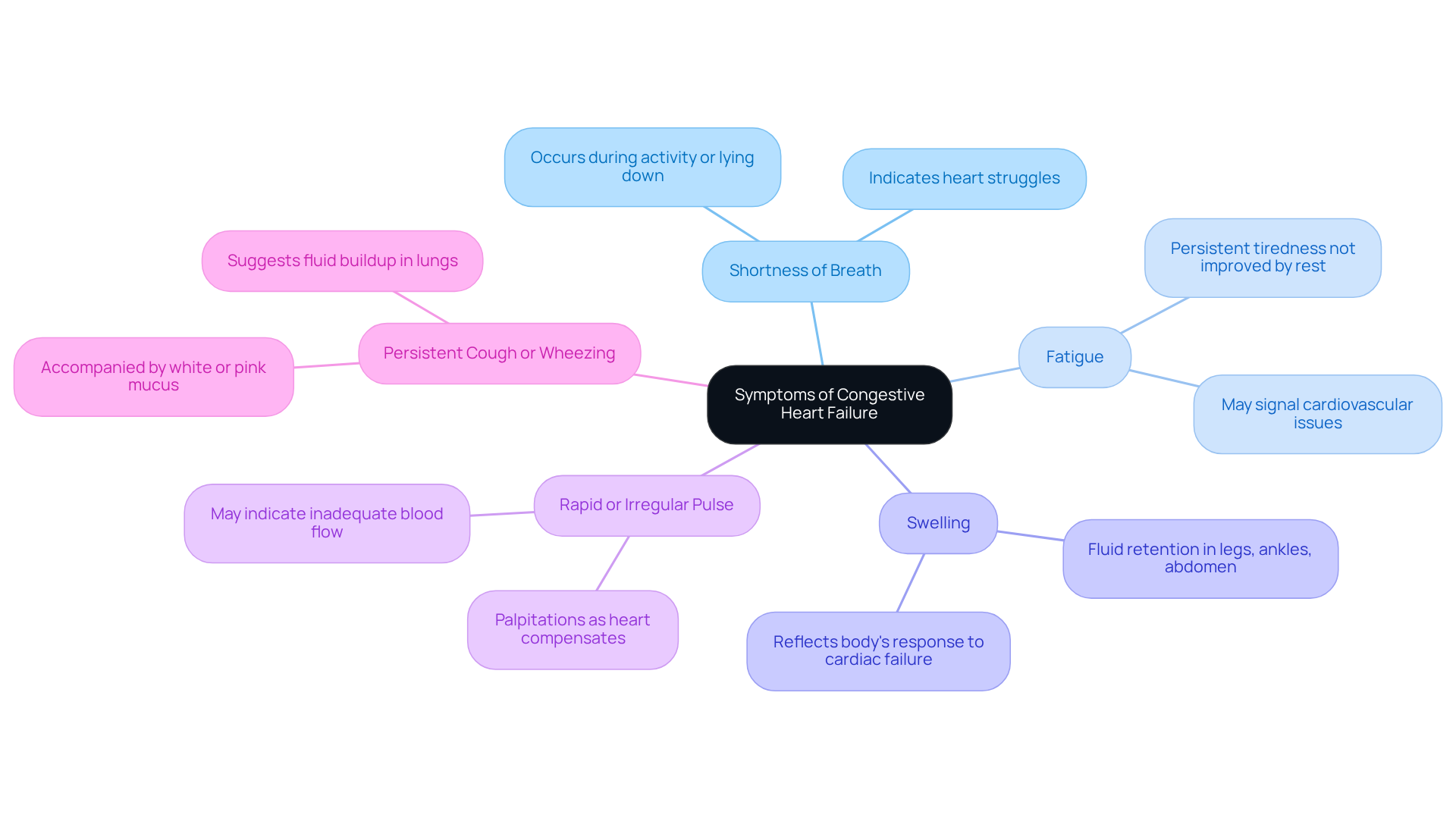
Identify Physical Symptoms of Low Heart Rate
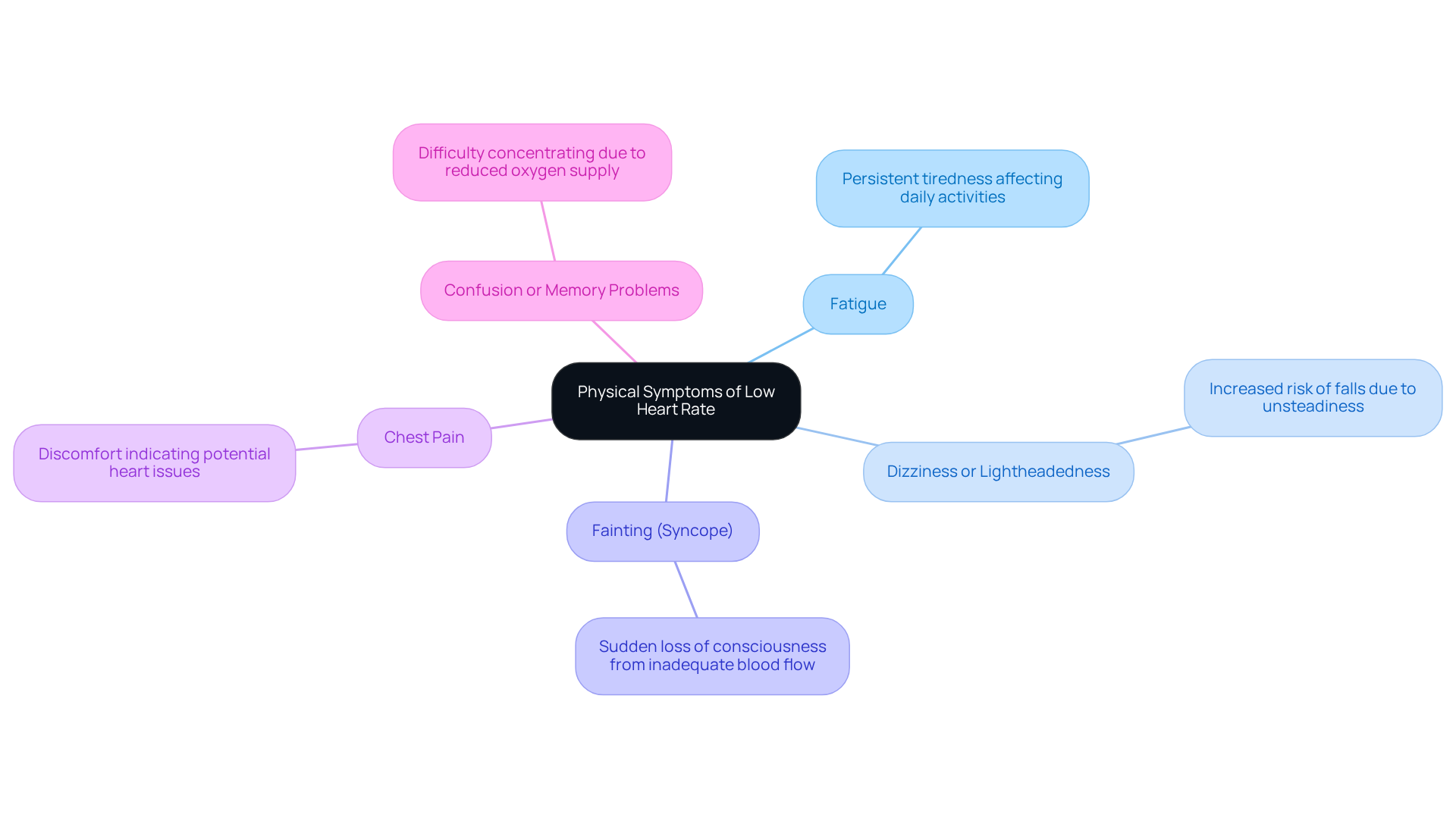
Common symptoms can be concerning, especially for our elderly loved ones. Here are some key physical symptoms:
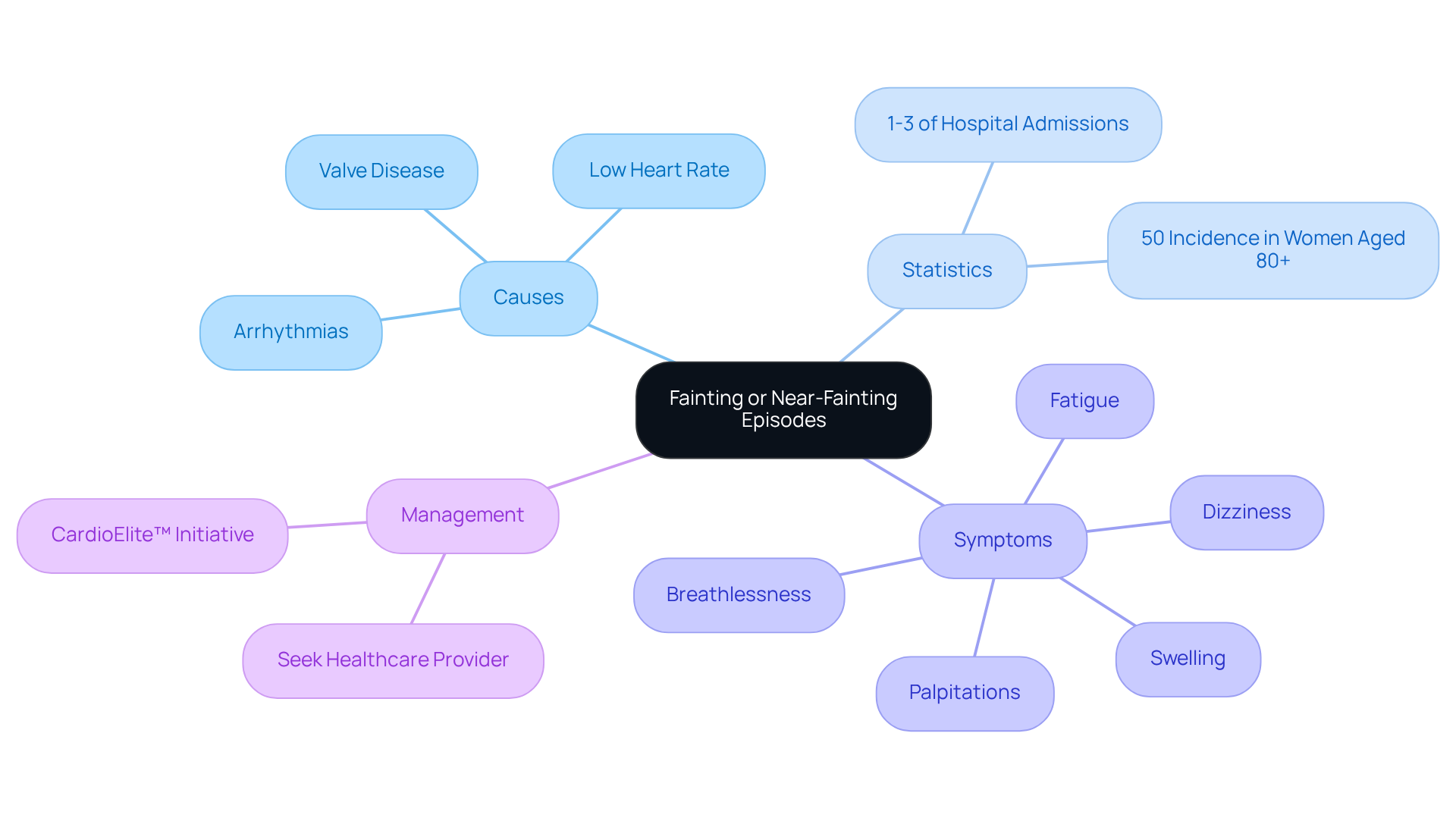
- Fatigue: Many elderly patients often feel persistently tired or low on energy, particularly during physical activities. This overwhelming fatigue can limit daily activities and significantly affect their quality of life.
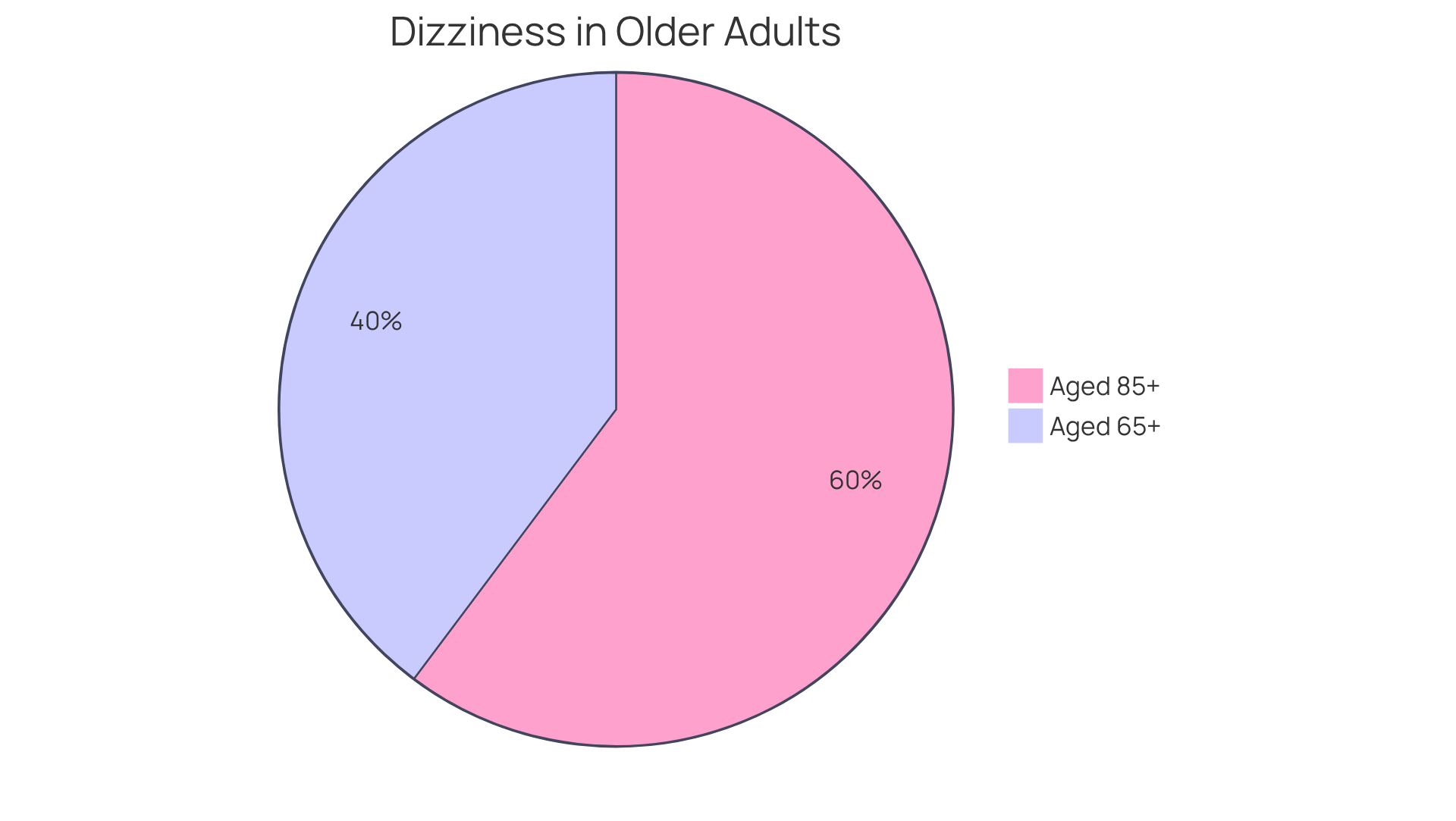
- Dizziness: Feelings of faintness or unsteadiness are common among seniors, increasing the risk of falls. This symptom is particularly alarming, as it can lead to injuries, making careful monitoring essential.
- Syncope: A sudden loss of consciousness can happen when blood flow to the brain is inadequate. This can be alarming for both patients and caregivers, so understanding what triggers these episodes is crucial for prevention.
- Chest pain: Discomfort or pain in the chest should never be ignored, as it may indicate underlying heart issues. The intensity of this pain can vary and may come with other signs of distress.
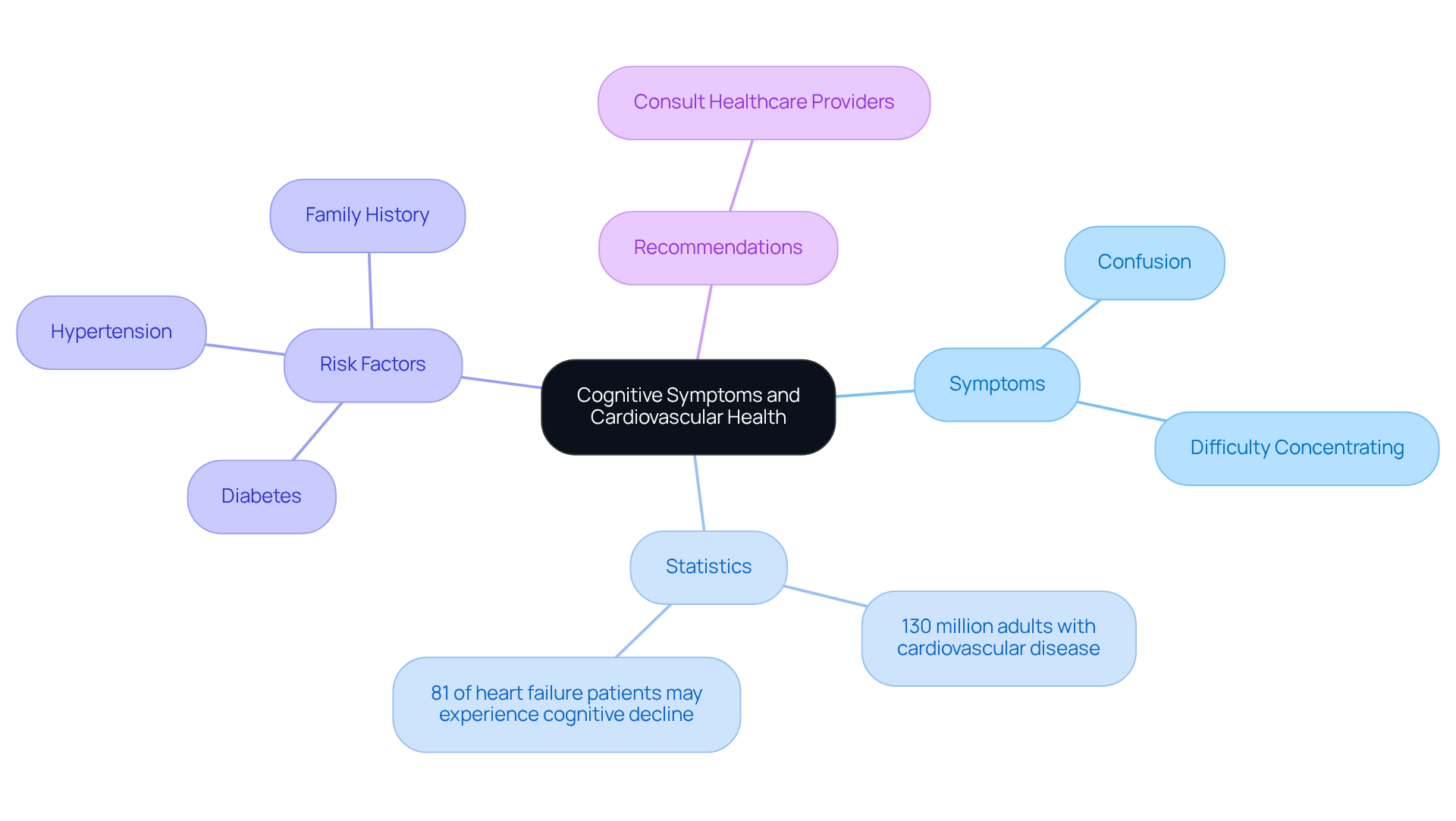
- Cognitive issues: Difficulty concentrating or recalling information often relates to reduced oxygen supply to the brain. This cognitive decline can be distressing for individuals and their families, underscoring the importance of prompt medical evaluation.
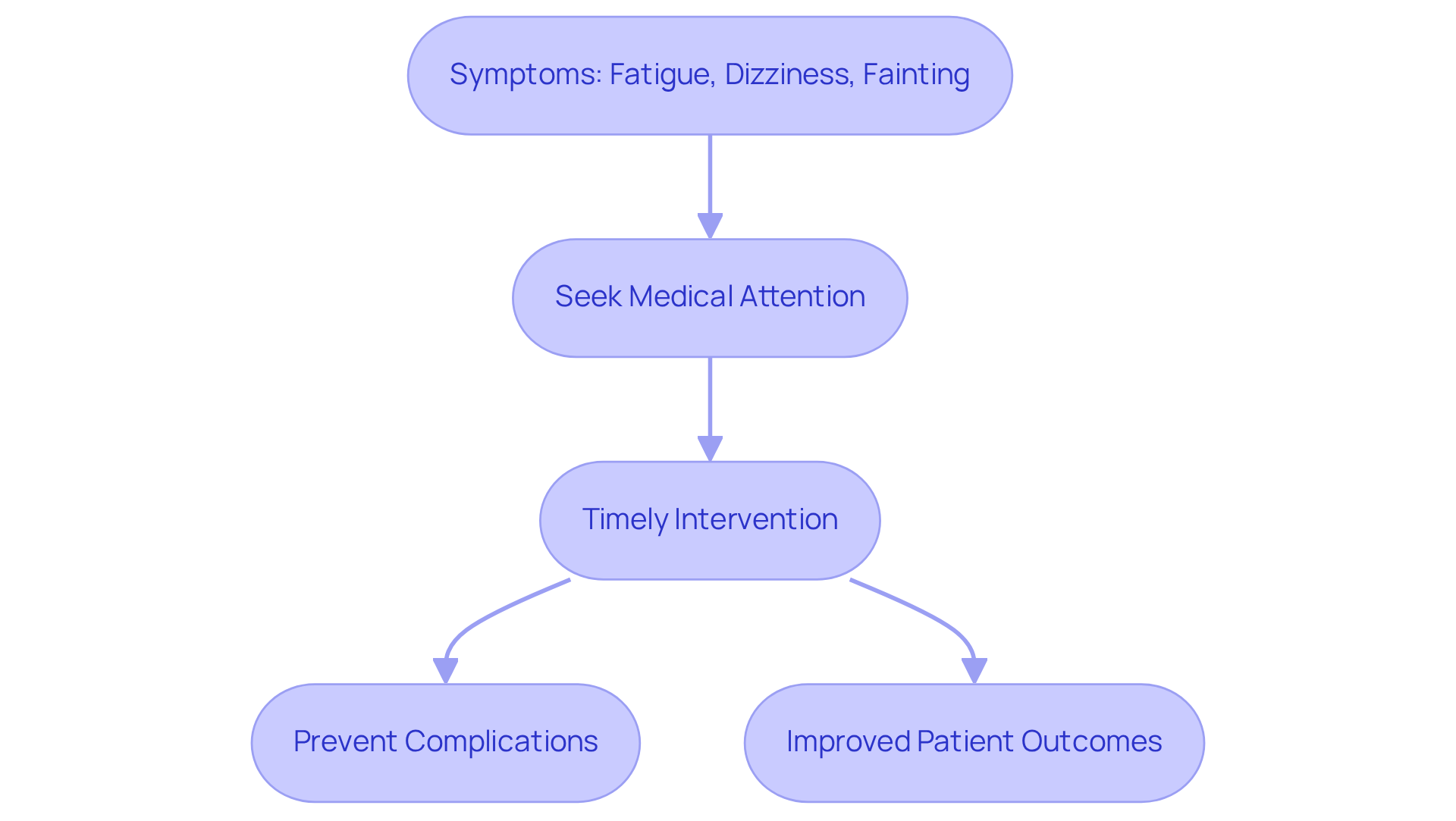
Recognizing these signs is vital for timely intervention. Recent studies indicate that older individuals with slow heart rates often experience symptoms, such as fatigue and dizziness, highlighting the need for awareness and proactive management. For instance, many individuals admitted for unstable bradycardia reported these symptoms, which significantly impacted their daily functioning and overall well-being. By understanding and addressing these physical signs, caregivers and healthcare providers can better support elderly patients in managing their health. If you or a loved one are experiencing these symptoms, please reach out for help. You’re not alone in this journey.
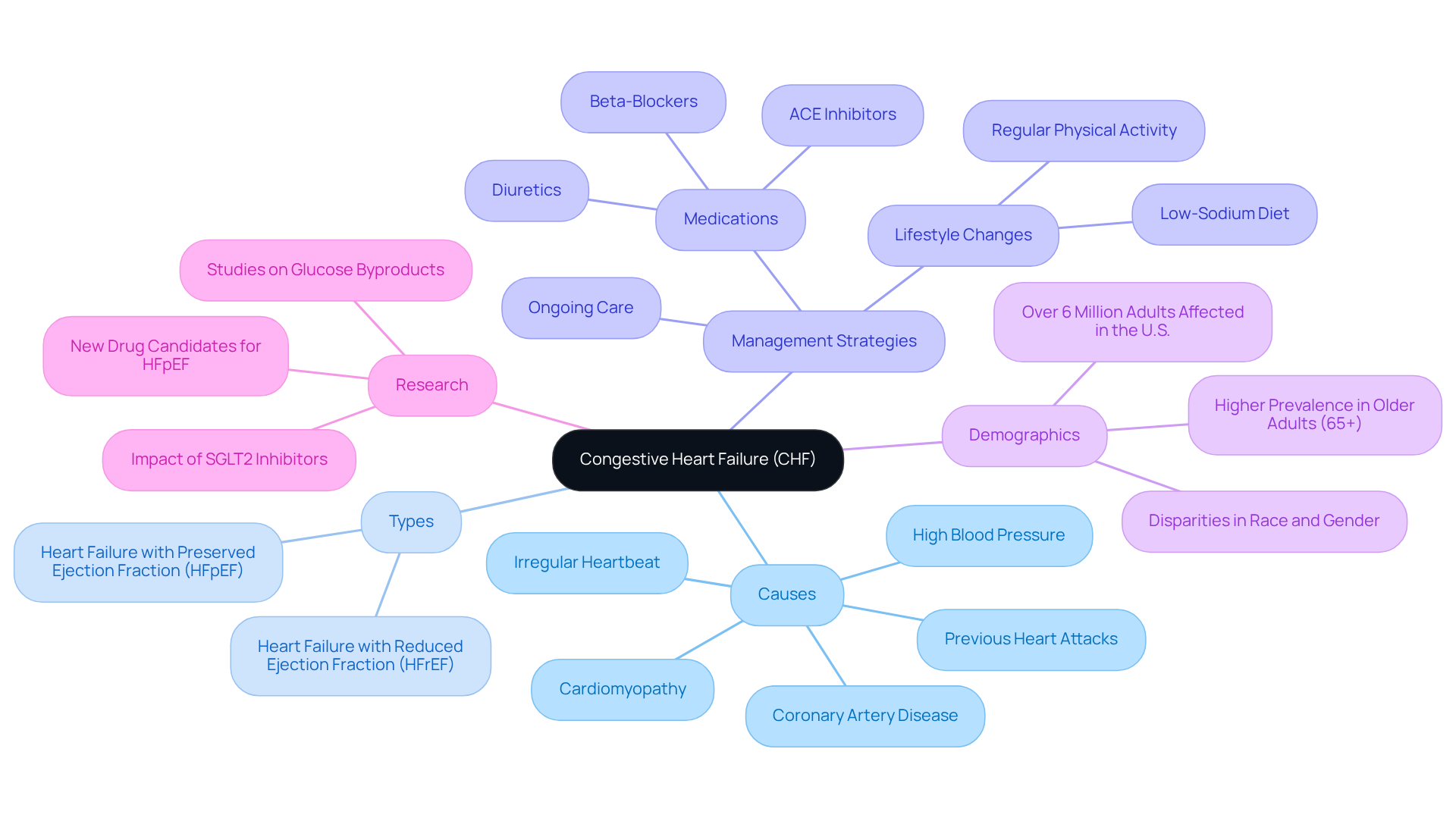
Explore Causes of Bradycardia and Their Impact
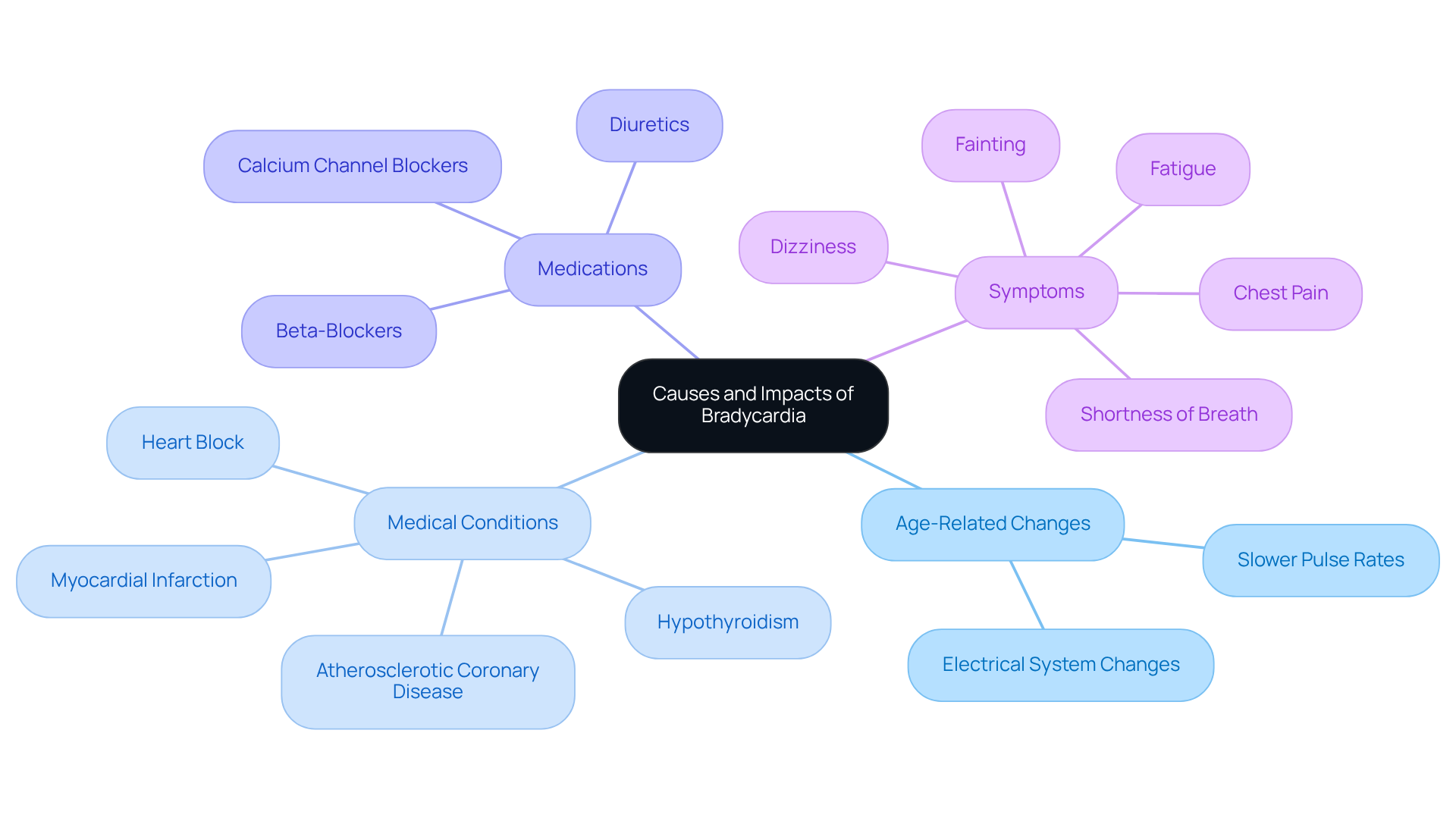
Bradycardia, which means a pulse rate below 60 beats per minute, can be concerning, especially for older adults. As we age, our bodies naturally undergo changes, particularly in the heart’s electrical system, leading to slower pulse rates. This is especially important to consider since studies show that about 85% of people over 50 may face atherosclerotic coronary disease, which can worsen pulse irregularities.
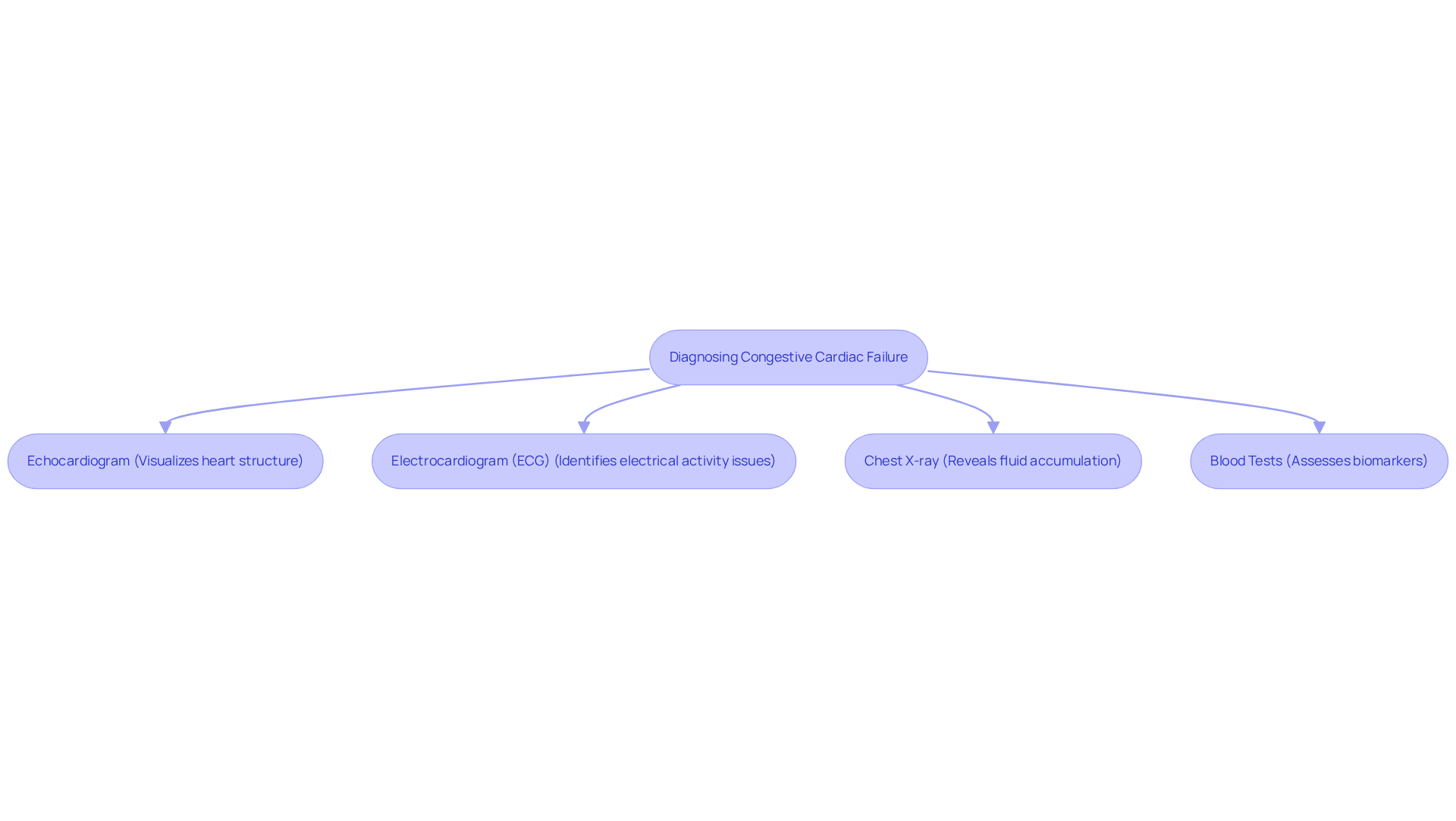
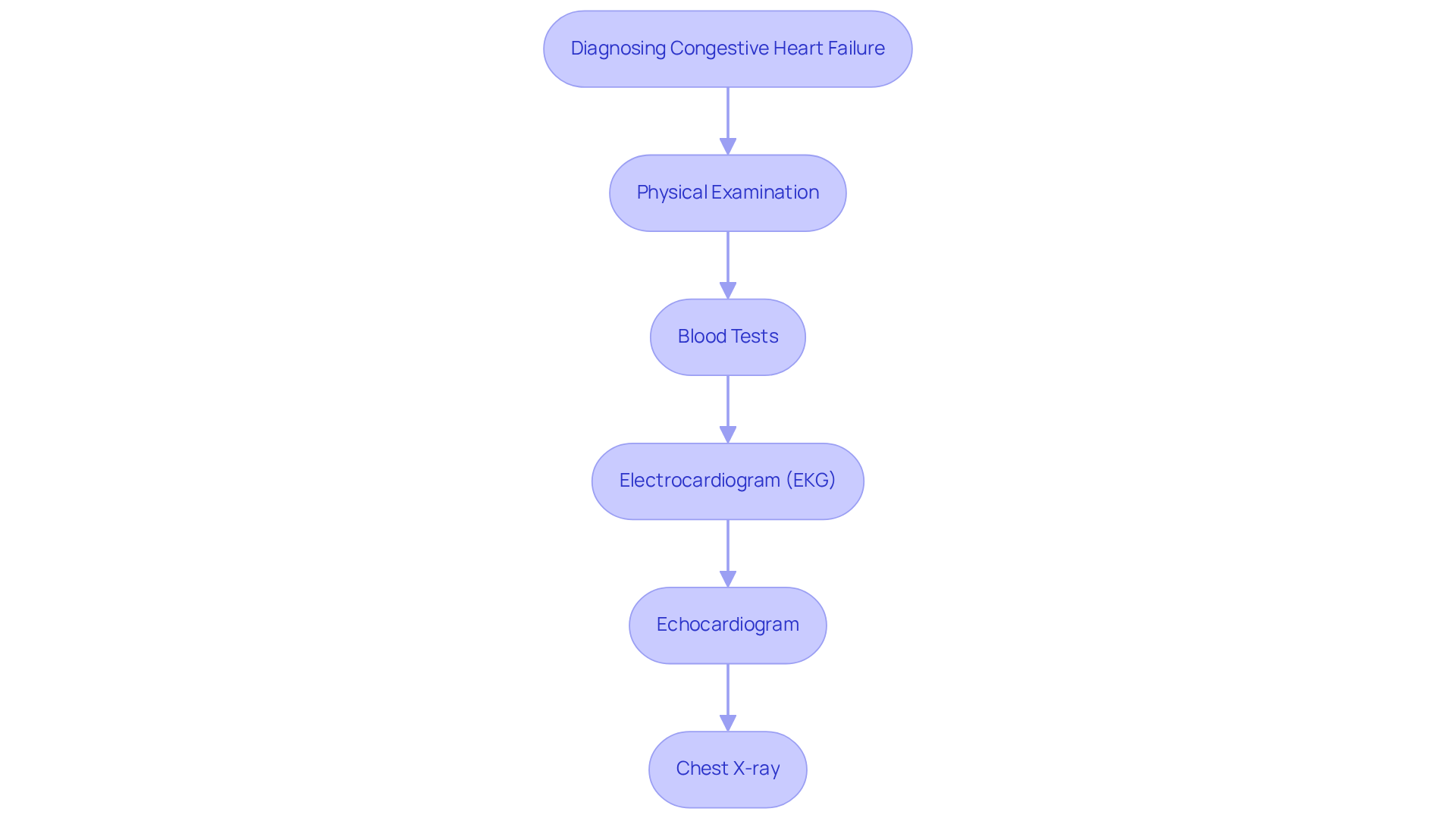
At Amavita Vascular and Cardiovascular Health, we understand the risks associated with chronic conditions, including those with diabetes, hypertension, or a family history of heart issues. Our diagnostic tools, like echocardiograms and cardiac MRI, help us monitor and manage conditions such as bradycardia effectively. We create tailored care plans to meet each patient’s needs, ensuring you feel supported every step of the way. With Dr. Martinez-Clark’s Harvard training and extensive cardiovascular experience, you can trust that these sophisticated tests will be integrated into your comprehensive care plan.
Medications also play a vital role in regulating pulse rates. Some medications, especially beta-blockers and calcium channel blockers, can lower pulse rates as a side effect. For seniors who often take multiple medications, this can lead to complications if not monitored closely.
Heart conditions like heart block, myocardial infarction, or cardiomyopathy can disrupt normal heart rhythms, leading to a slower heart rate. For example, a study found that 39% of patients with heart disease were admitted to the hospital, highlighting the serious implications of these conditions.
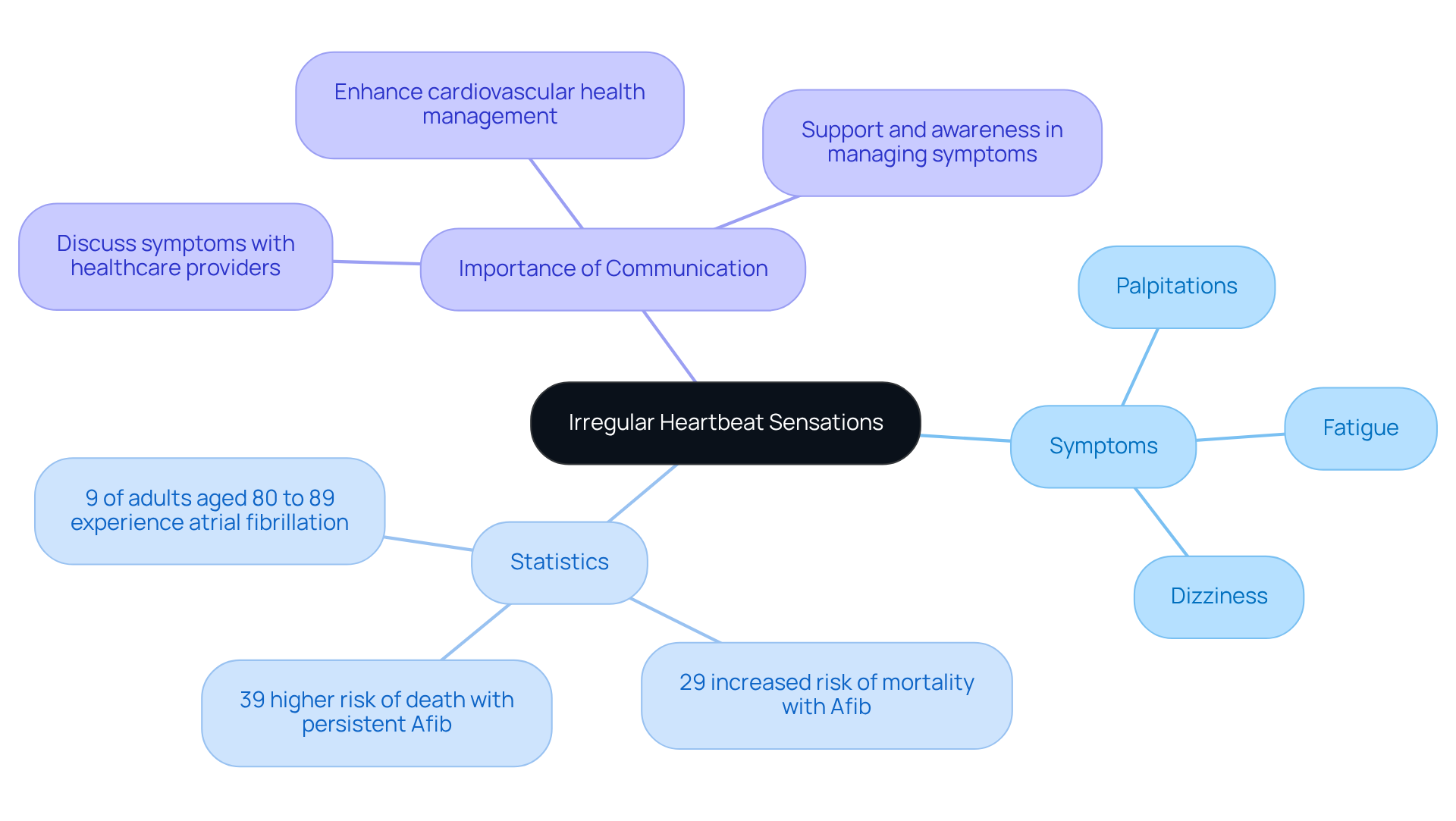
Common physical symptoms of low heart rate include fatigue, dizziness, shortness of breath, fainting, and chest pain. Electrolyte imbalances, particularly low potassium or calcium levels, can significantly impact heart function, resulting in a decreased pulse rate. Additionally, hypothyroidism, which involves reduced thyroid activity, can lower pulse rates, making regular thyroid function evaluations essential for seniors.
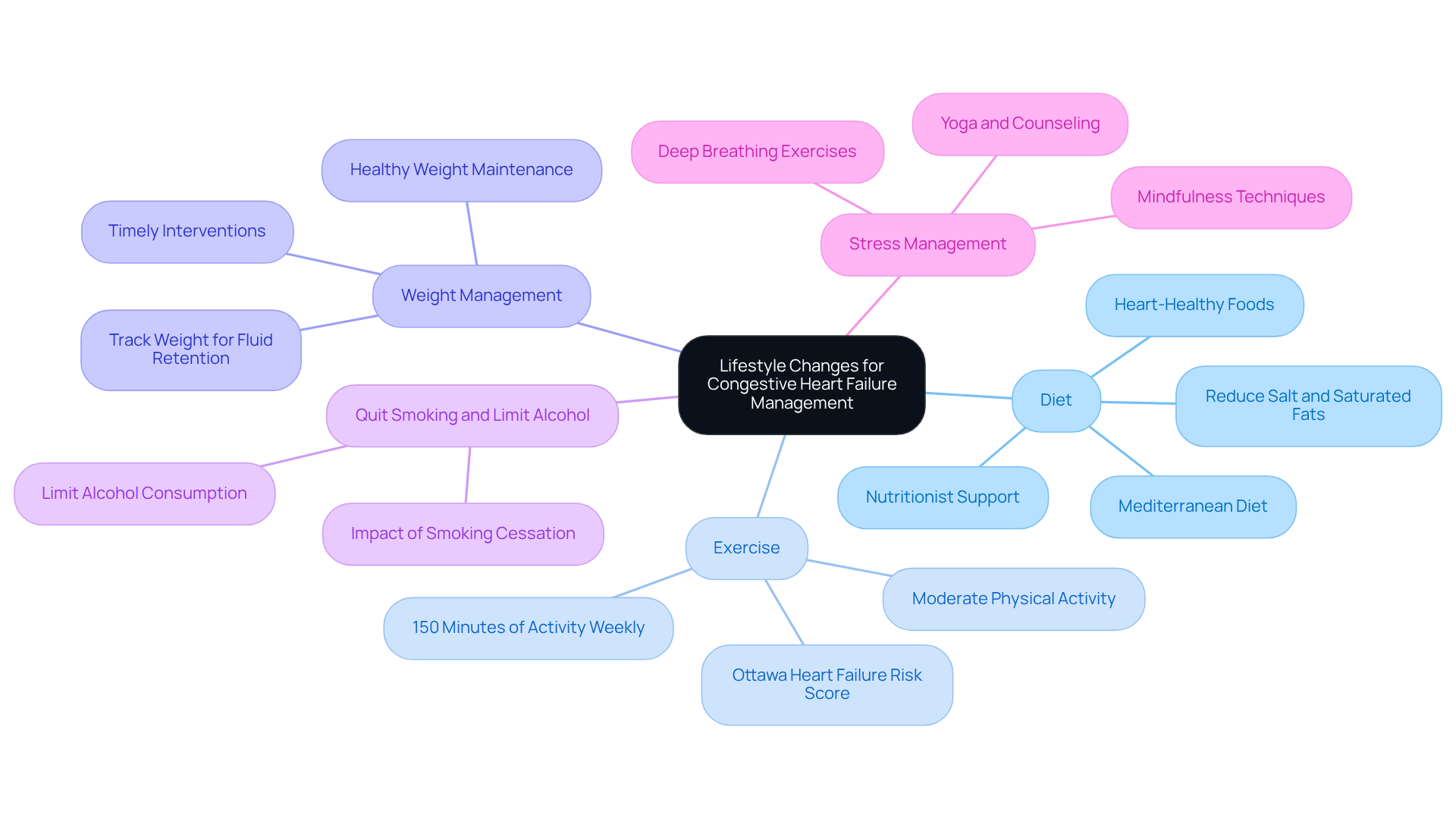
Understanding these factors is crucial for effectively diagnosing and preventing severe complications like heart failure or an increased risk of stroke. Proactive management strategies, including lifestyle changes and regular health assessments at Amavita, can greatly improve outcomes for seniors experiencing low heart rates.
If you have concerns about your heart health, please reach out to us. We’re here to help you navigate these challenges with care and compassion.
Recognize When to Seek Medical Attention for Bradycardia
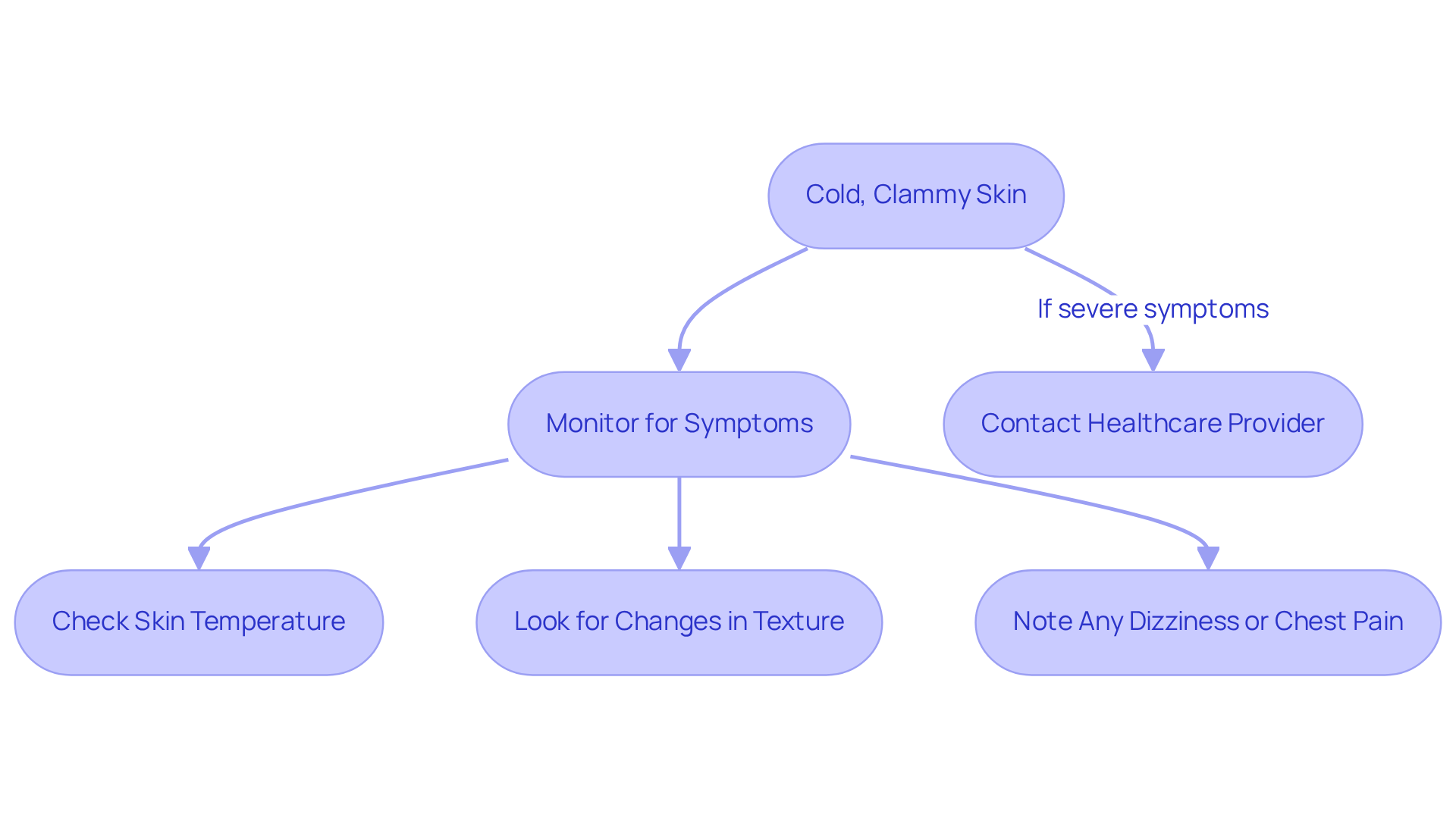
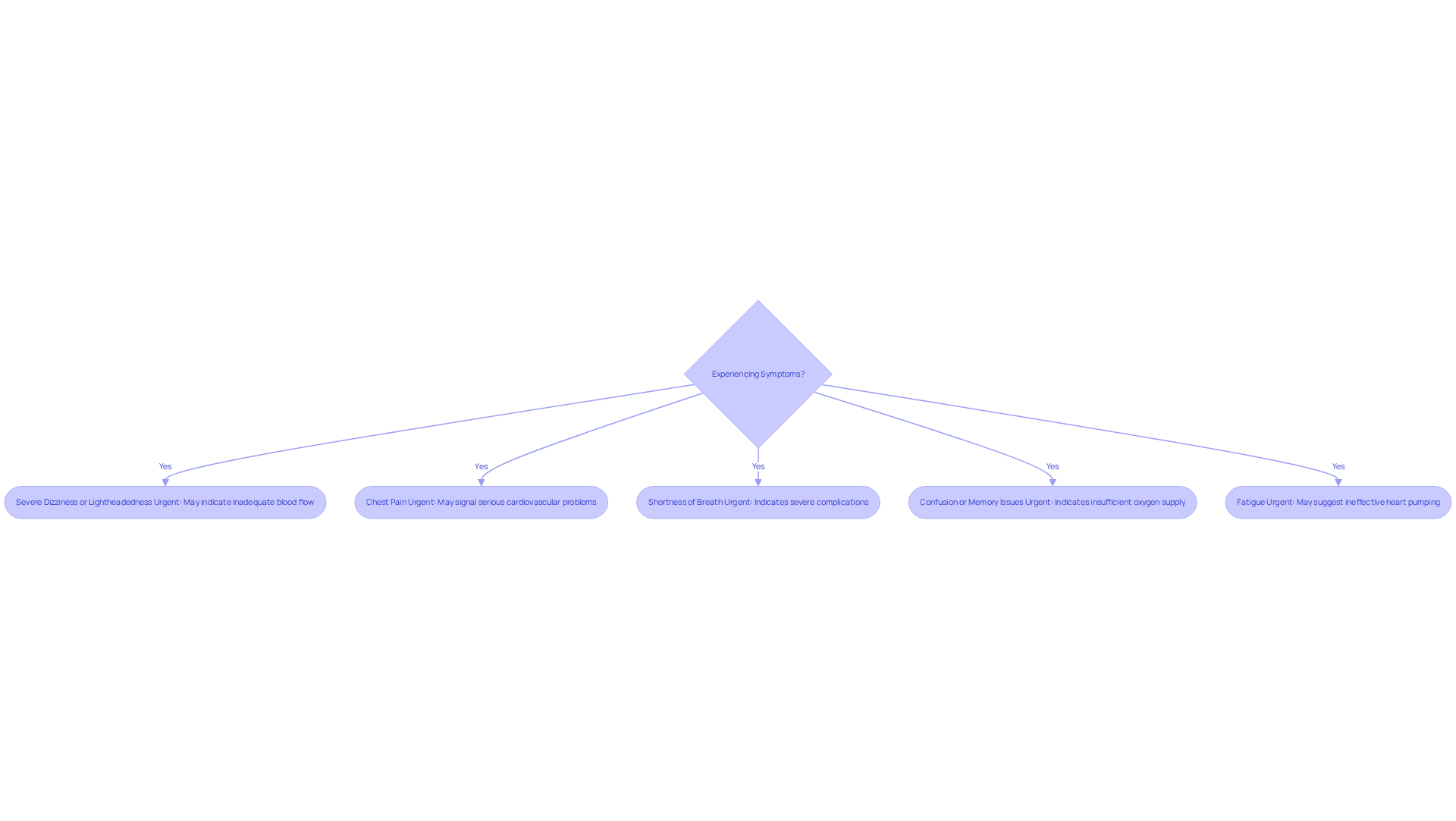
Recognizing when to seek medical attention is crucial, especially for elderly patients. If you or a loved one experiences any of the following symptoms, prompt evaluation is necessary:
- Severe Dizziness or Lightheadedness: This can be particularly concerning if it leads to fainting, as it may indicate inadequate blood flow to the brain.
- Chest Pain: Ongoing discomfort in the chest should always be assessed, as it may signal serious cardiovascular problems.
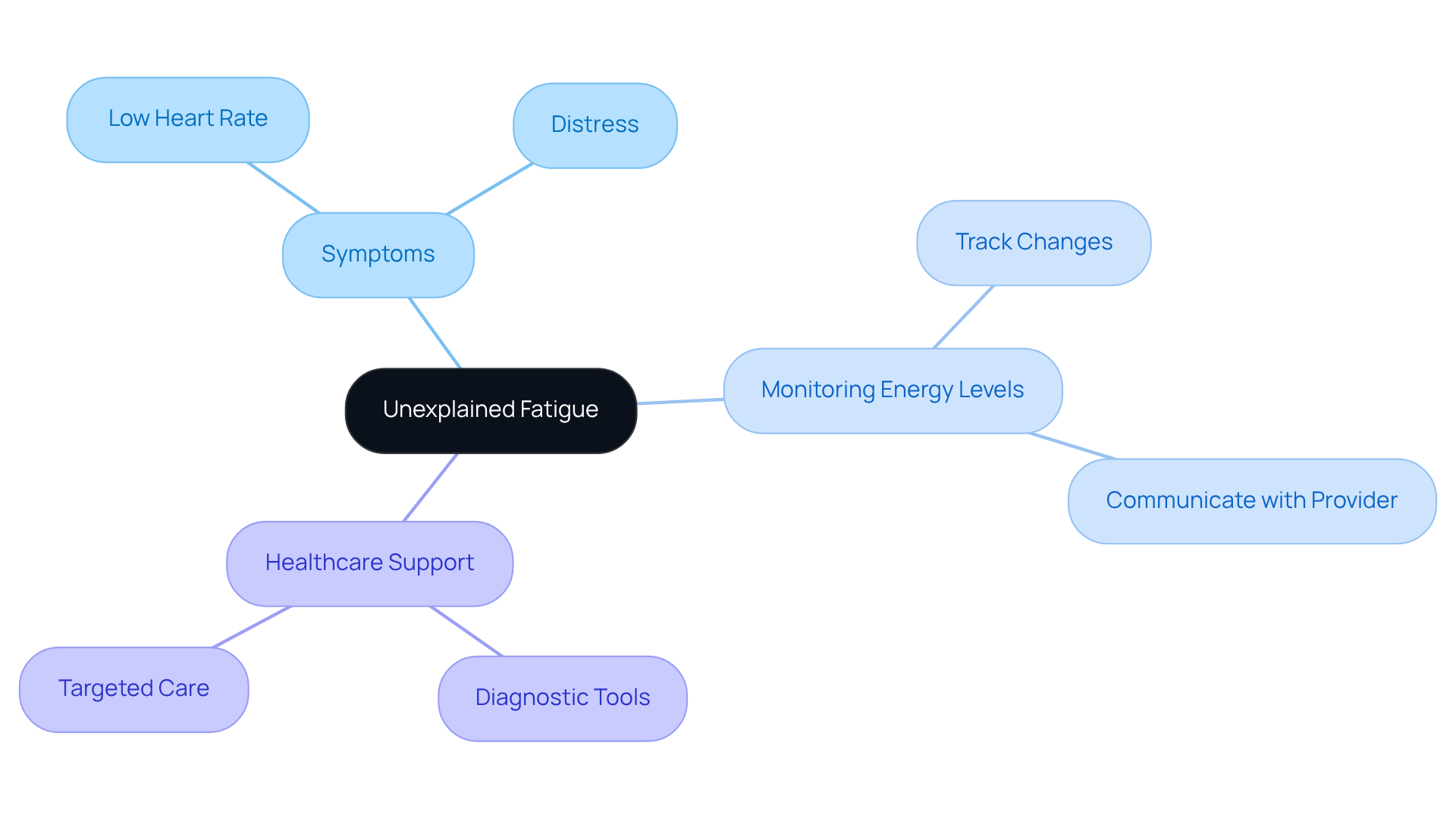
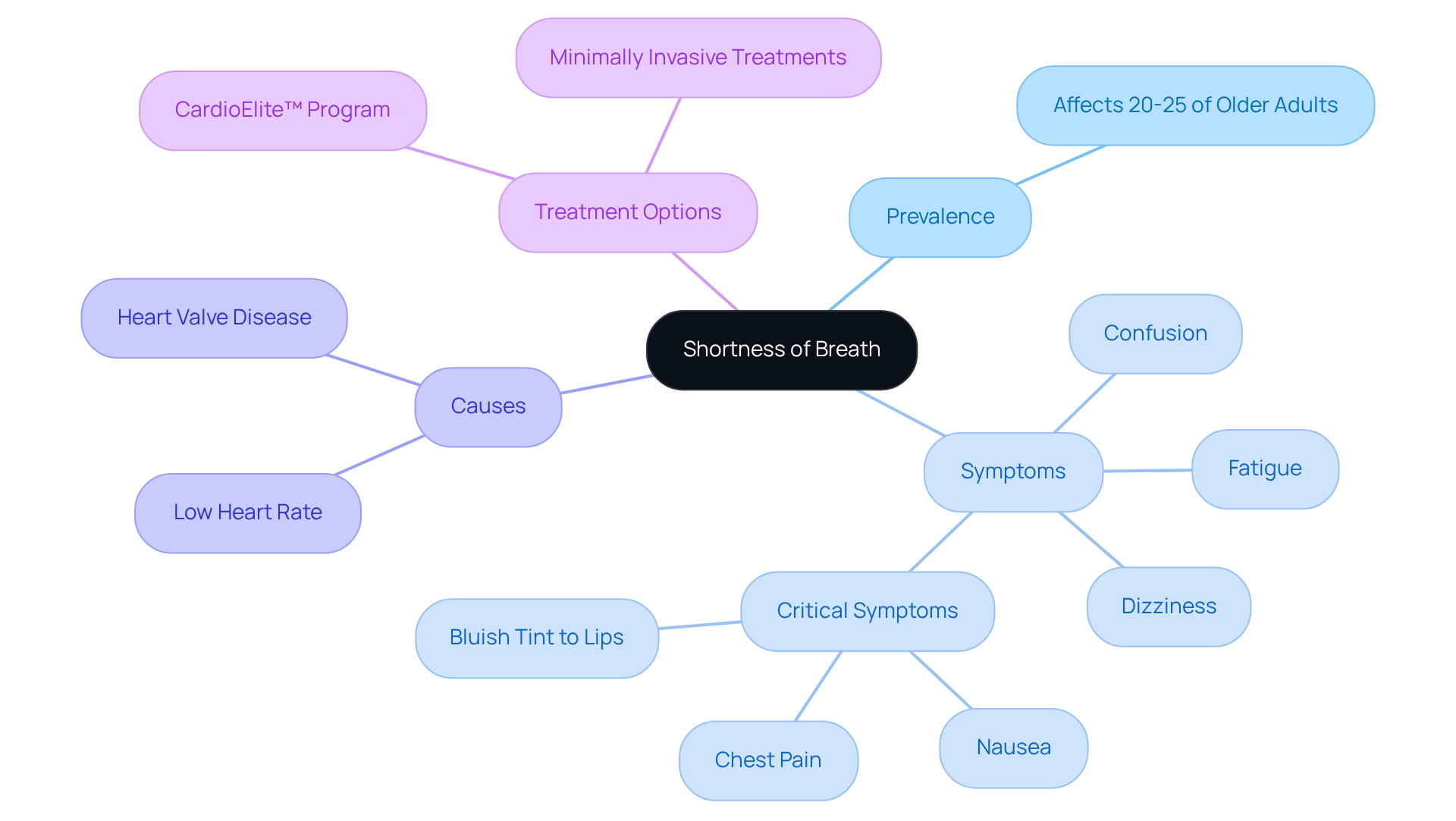
- Shortness of Breath: Difficulty breathing can indicate severe complications related to a slow heart rate, which can manifest as fatigue, potentially pointing to heart failure or other circulatory conditions that require immediate attention. Dr. Martinez-Clark specializes in minimally invasive treatments that can improve breathing and energy levels.
- Confusion: Sudden cognitive changes can indicate insufficient oxygen supply to the brain, necessitating urgent care.
- Fatigue: Unusual tiredness during normal activities may be a warning sign of bradycardia, which can manifest as weakness, suggesting that the heart is not pumping effectively. This fatigue can also indicate various cardiovascular conditions, including heart disease or valve problems.
Data shows that elderly patients often seek care at emergency departments due to these issues, highlighting the importance of awareness and prompt intervention. Understanding these emergency signs can lead to quicker diagnoses and treatment, ultimately preventing complications such as heart failure or sudden cardiac arrest. At Amavita, we offer services to identify the specific causes of these symptoms and create personalized treatment plans. Remember, you’re not alone in this; we’re here to support you every step of the way.
Conclusion
Understanding the physical symptoms of low heart rate, especially in elderly patients, is vital for heart health and overall well-being. Bradycardia, which is when the pulse rate drops below 60 beats per minute, can lead to serious complications if not recognized and managed quickly. Are you or a loved one experiencing fatigue, dizziness, or fainting? Recognizing these signs can greatly enhance the quality of life for older adults and their caregivers.
Throughout this discussion, we’ve highlighted key insights about the prevalence and implications of bradycardia in seniors. Did you know that a significant percentage of elderly patients face symptoms that could lead to severe health issues? This underscores the importance of timely medical intervention. Healthcare providers, like those at Amavita Heart and Vascular Health, play a crucial role in offering thorough evaluations and personalized care plans to effectively address these concerns.
In conclusion, being aware of the physical symptoms of low heart rate is essential for elderly patients and their families. Proactive management and knowing when to seek medical attention can prevent serious complications, ensuring a better quality of life. As our population ages, it becomes increasingly important to address the impact of bradycardia on cardiovascular health. If you or someone you know is experiencing symptoms, please don’t hesitate to reach out for support and guidance. Remember, timely action can lead to improved health outcomes and peace of mind.
Frequently Asked Questions
What is bradycardia?
Bradycardia is a condition characterized by a slower-than-usual pulse rate, typically falling below 60 beats per minute.
Why is bradycardia important in heart health?
Bradycardia is important in heart health because it can lead to insufficient blood flow to vital organs, causing physical symptoms such as fatigue, dizziness, and fainting.
What are the physical symptoms of low heart rate?
Physical symptoms of low heart rate include fatigue, dizziness, and fainting, which can indicate underlying health issues such as heart disease or other cardiovascular conditions.
How common is bradycardia among seniors?
About 6.2% of seniors aged 60 and above who visit emergency departments show symptoms of a slow heart rate, with 15.61% of these cases experiencing an unstable heart rate.
What is the most common symptom among those with unstable slow heart rates?
The most common symptom among individuals with unstable slow heart rates is shortness of breath, affecting over 31% of people.
What are the risks associated with unstable slow heart rates?
Alarmingly, 30% of individuals with unstable slow heart rates passed away during hospitalization from causes unrelated to their condition.
How can bradycardia be managed?
Timely identification and management of bradycardia can greatly enhance outcomes and improve quality of life. Comprehensive cardiac evaluations and preventive strategies are crucial in addressing this condition.
What services does Amavita Heart and Vascular Health provide for bradycardia?
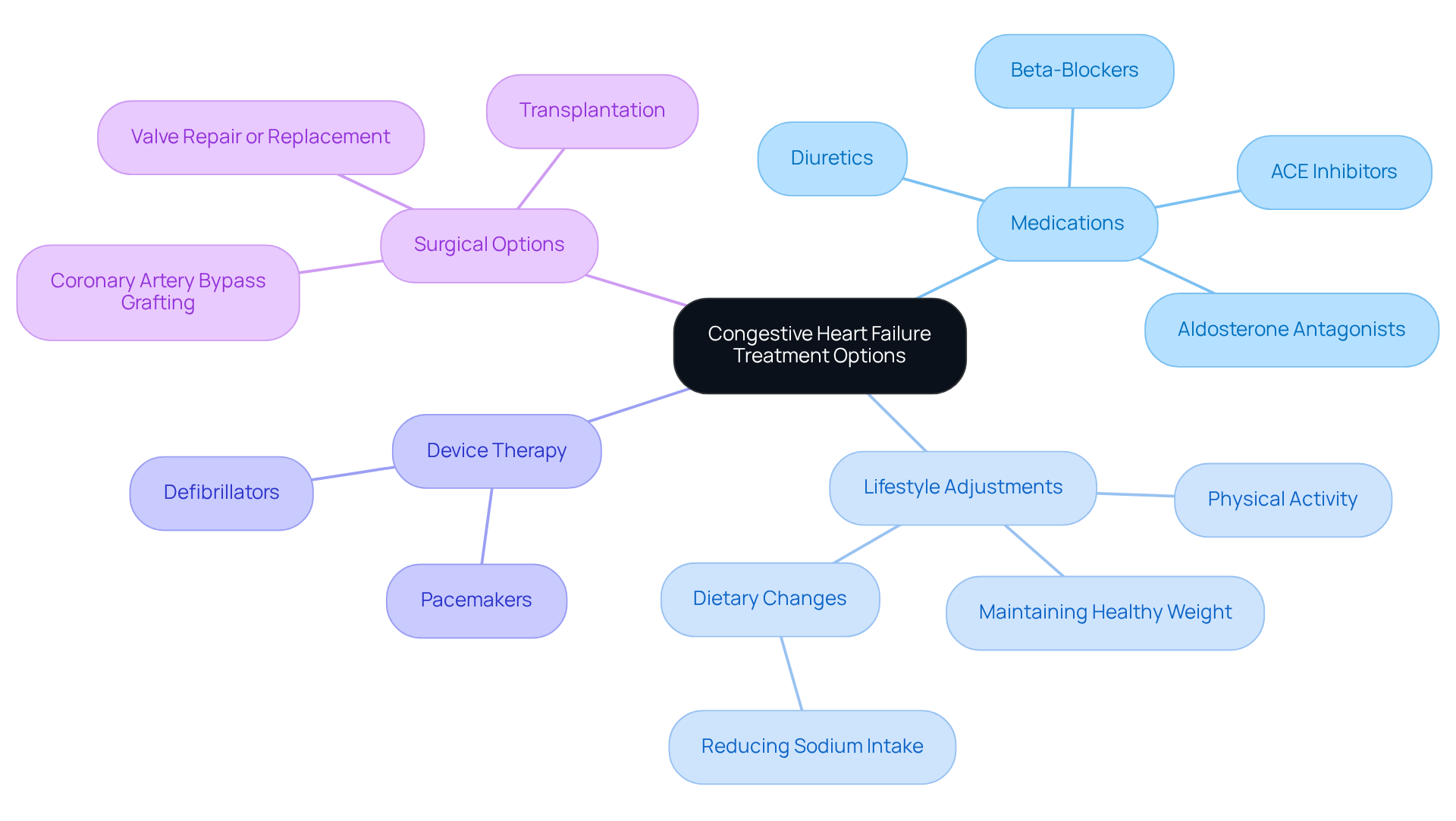
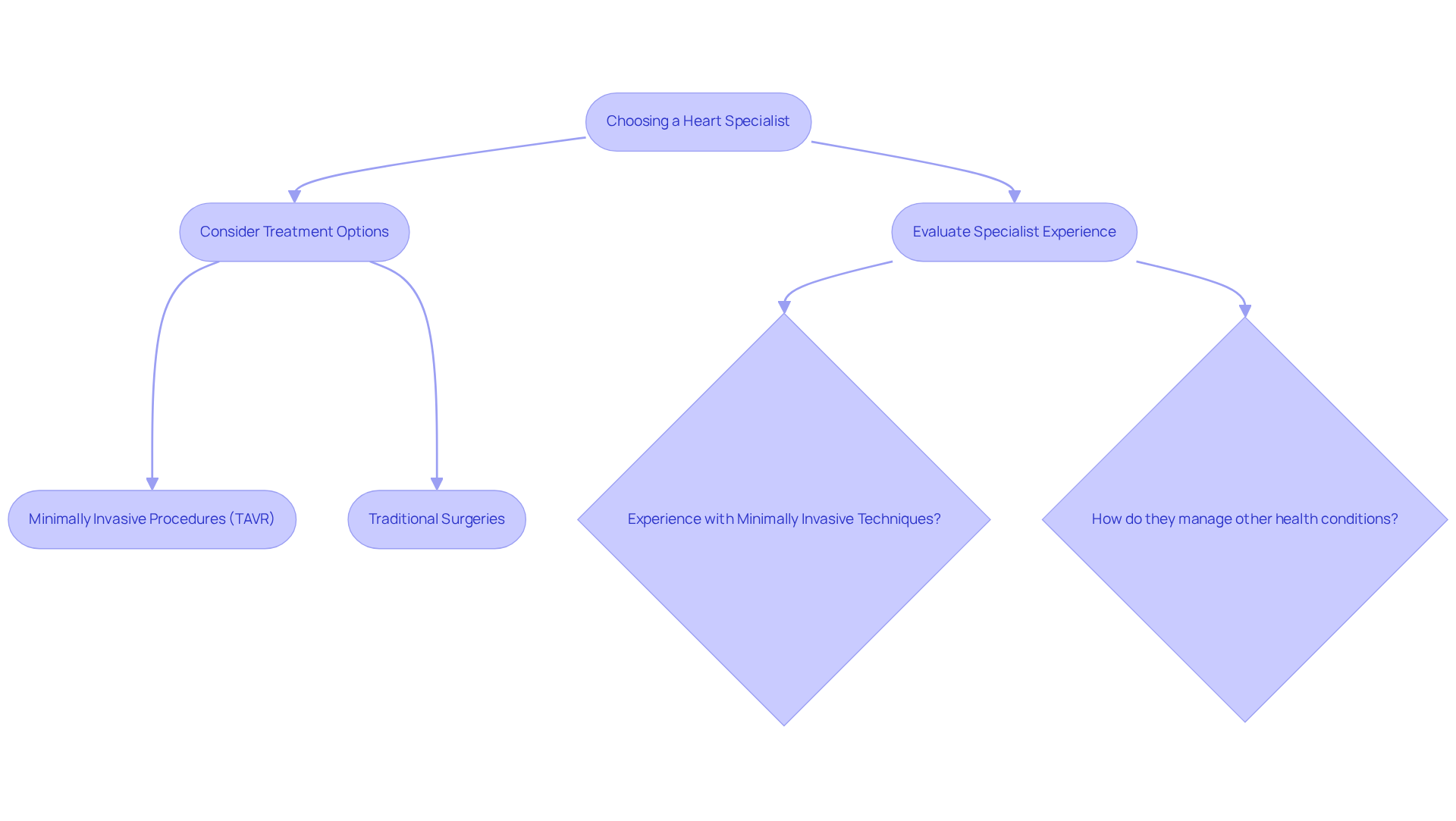
Amavita Heart and Vascular Health offers comprehensive cardiac evaluations and innovative, minimally invasive therapies for heart valve disease, aiming to alleviate issues like shortness of breath and fatigue.
What is the CardioElite™ program?
The CardioElite™ program is a holistic approach to cardiac care offered by Amavita, focusing on proactive management to minimize readmissions and enhance the quality of life for seniors.
What should I do if I or a loved one are experiencing symptoms of bradycardia?
If you or a loved one are experiencing symptoms of bradycardia, it is recommended to reach out to Amavita Heart and Vascular Health for support and evaluation.
List of Sources
- Define Bradycardia and Its Importance in Heart Health
- hrsonline.org (https://hrsonline.org/news/societies-publish-new-guidance-treatment-slow-irregular-heartbeats)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC10689927)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9021000)
- Abnormally slow heart rate associated with xylazine-fentanyl overdose (https://medicalxpress.com/news/2026-01-abnormally-heart-xylazine-fentanyl-overdose.html)
- Significance of Chronic Sinus Bradycardia in Elderly People | Circulation (https://ahajournals.org/doi/10.1161/01.cir.46.5.924)
- Identify Physical Symptoms of Low Heart Rate
- Bradycardia – Symptoms and causes (https://mayoclinic.org/diseases-conditions/bradycardia/symptoms-causes/syc-20355474)
- Roundup: These Adults 65 and Older are Seeing Sharp Declines in Heart Health; and More News (https://baptisthealth.net/baptist-health-news/this-group-of-adults-65-and-older-are-seeing-sharp-declines-in-heart-health)
- Study finds heart health declining in older adults with certain cardiovascular diseases (https://newsroom.heart.org/news/study-finds-heart-health-declining-in-older-adults-with-certain-cardiovascular-diseases)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9021000)
- Explore Causes of Bradycardia and Their Impact
- What Can Cause a Low Heart Rate? Key Insights for Seniors (https://amavita.health/blog/what-can-cause-a-low-heart-rate-key-insights-for-seniors)
- mwhomecare.com (https://mwhomecare.com/aging-in-place-100-quotes-to-make-you-think-differently)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9021000)
- psychologytoday.com (https://psychologytoday.com/us/blog/fulfillment-at-any-age/201201/15-wise-and-inspiring-quotes-about-aging)
- Recognize When to Seek Medical Attention for Bradycardia
- Bradycardia – Symptoms and causes (https://mayoclinic.org/diseases-conditions/bradycardia/symptoms-causes/syc-20355474)
- What Is Bradycardia and When to See a Cardiologist (https://thenyheartcenter.com/blog/1397893-what-is-bradycardia-and-when-to-see-a-cardiologist)