Introduction
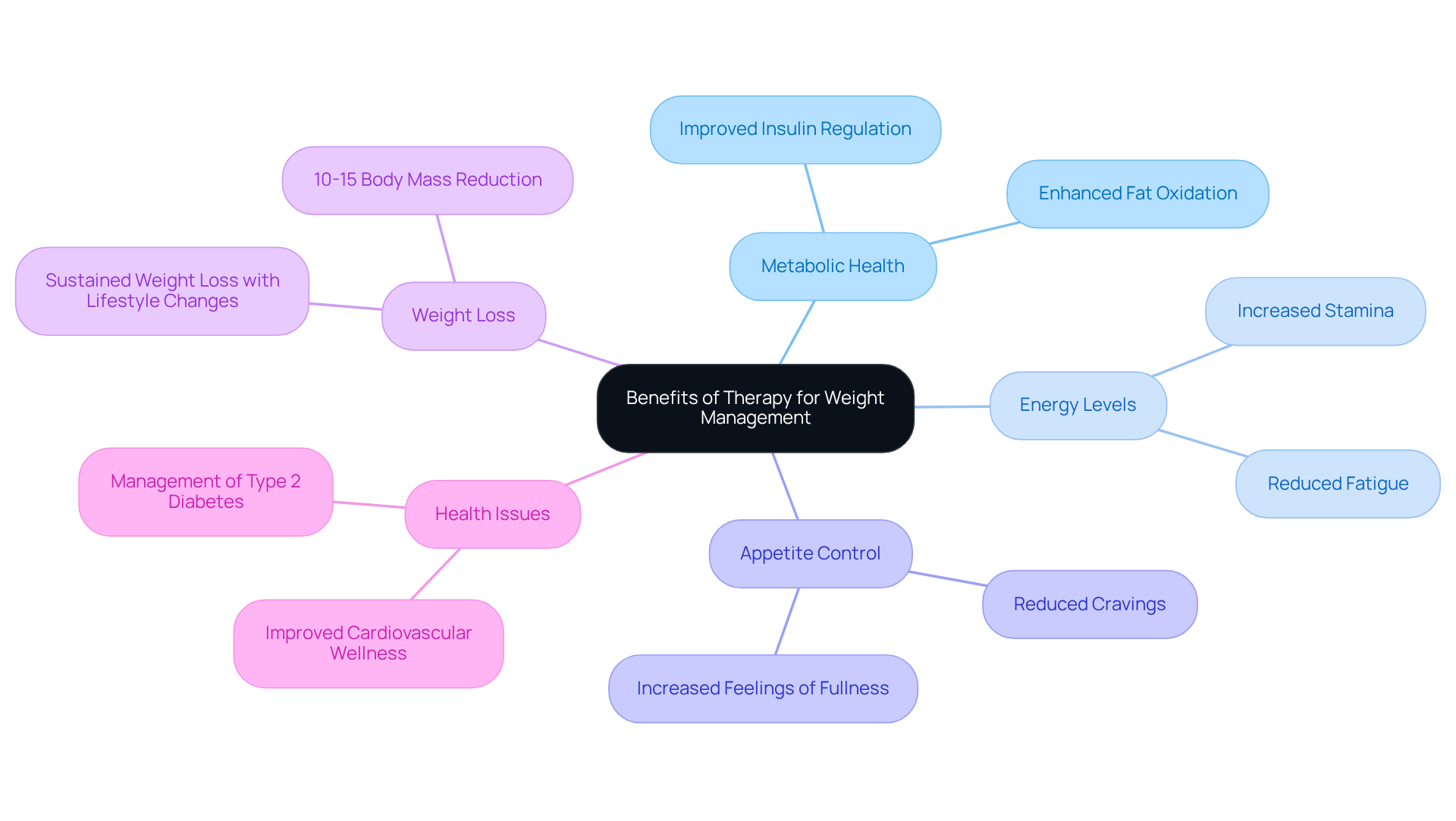
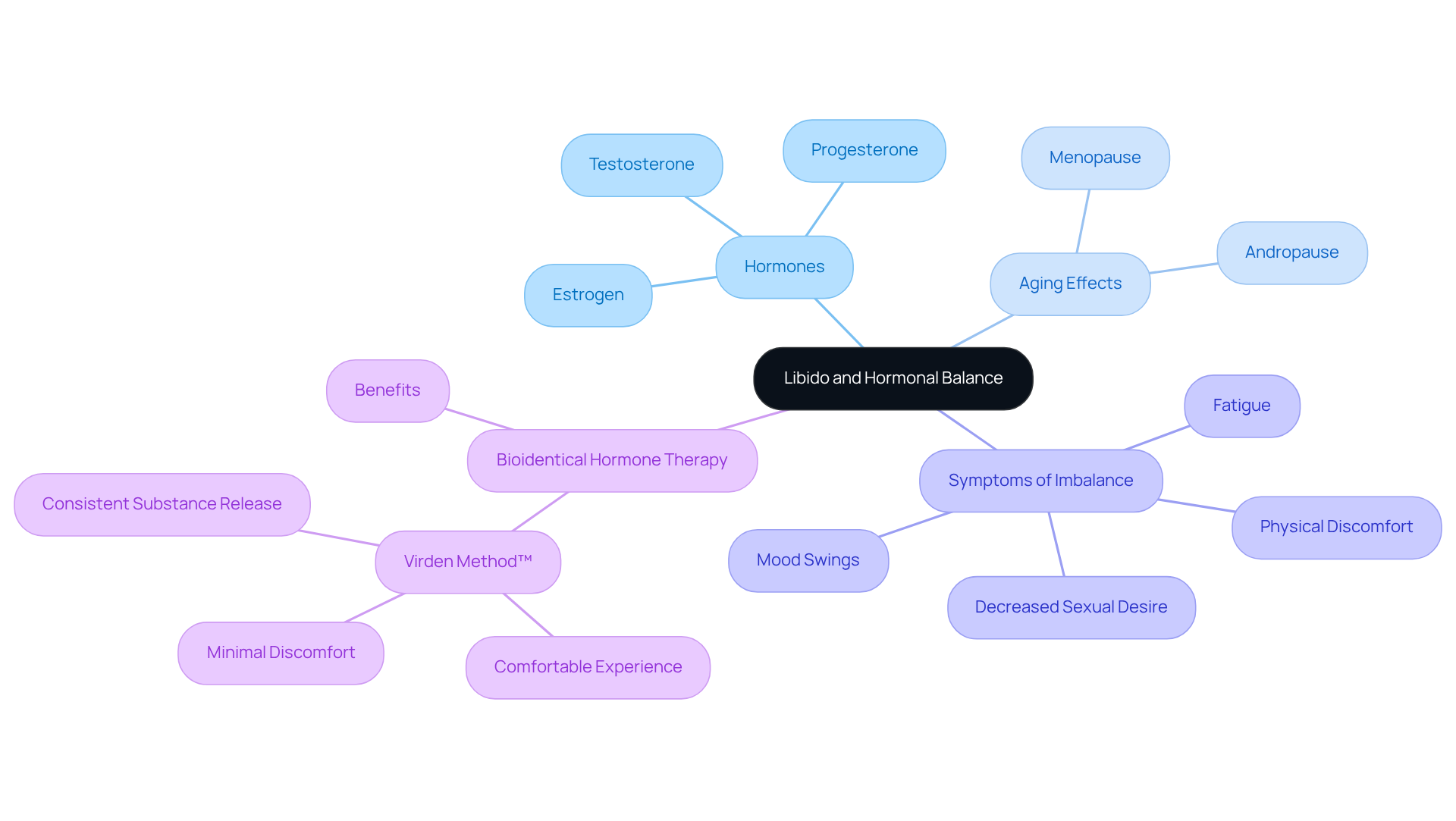
As we age, the quest for optimal health becomes increasingly vital, especially regarding hormonal balance and cardiovascular well-being. Hormone pellet therapy offers a promising solution, providing a range of benefits that can significantly enhance the quality of life for seniors. Yet, many may not realize how this innovative treatment can address common challenges associated with aging.
What if a simple, minimally invasive procedure could restore your energy, improve your mood, and even bolster your heart health? Exploring the potential of hormone pellets reveals not only their direct benefits but also the profound impact they can have on overall well-being in the elderly.
In addition to this, hormone pellet therapy can help alleviate feelings of fatigue and emotional distress, allowing you to enjoy life more fully. Imagine feeling revitalized and more connected to your loved ones. This treatment could be the key to unlocking a happier, healthier you.
If you’re curious about how hormone pellets can support your health journey, know that you’re not alone. Many seniors are discovering the transformative effects of this therapy, and it’s never too late to seek help. Your well-being matters, and there are compassionate professionals ready to guide you on this path.
Amavita Heart and Vascular Health: Personalized Hormone Pellet Therapy for Optimal Balance
At Amavita Heart and Vascular Care, we understand that many older patients face challenges with hormonal imbalances and health issues. Our customized treatment using hormone pellets is designed specifically to restore hormonal equilibrium, addressing your unique medical needs with compassion and care.
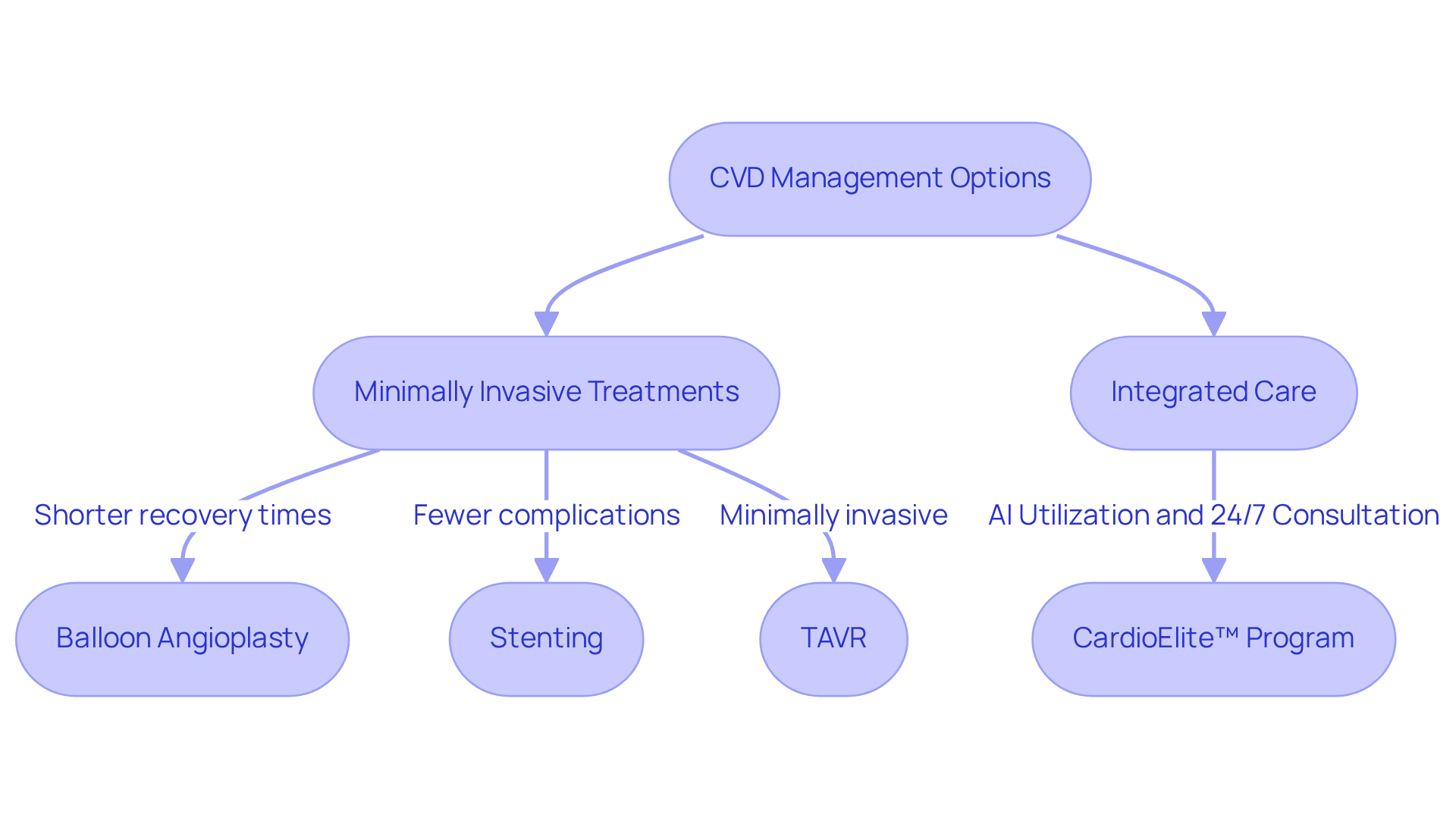
This innovative approach not only targets hormonal imbalances but also integrates seamlessly with traditional therapies through the use of hormone pellets. By doing so, we create a holistic treatment plan that enhances your overall well-being. Research shows that hormone therapy can reduce risks, with studies indicating a 30%-50% decrease in coronary heart disease among users compared to non-users.
Many patients report feeling more energetic, experiencing mood stabilization, and finding relief from menopausal symptoms, all of which contribute to a better quality of life. For instance, one patient, Michelle, shared how she experienced a remarkable reduction in hot flashes and sleep disturbances, showcasing the effectiveness of our treatment.
We emphasize the importance of this integration, noting that as a treatment option, hormone therapy can enhance heart health by improving vascular function and reducing the risk of cardiovascular incidents. As we continue to advance our therapy using hormone pellet implants, Amavita remains dedicated to providing elderly patients with solutions that not only meet hormonal needs but also promote cardiovascular wellness. Together, we can work towards goals that truly make a difference in your life.
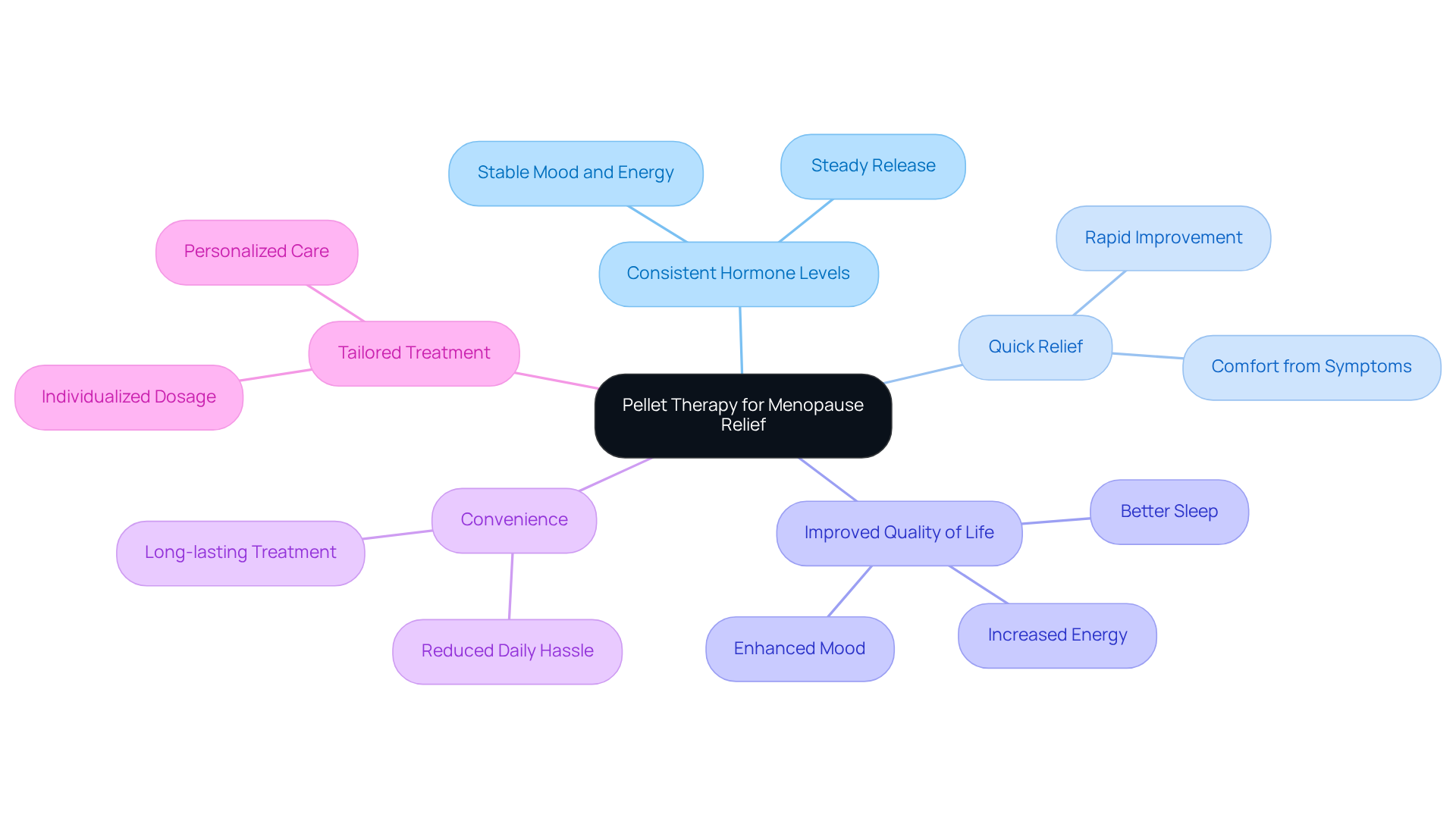
Enhanced Hormonal Balance: How Hormone Pellets Improve Overall Well-Being
provide a gentle solution for those struggling with hormonal imbalances, offering a steady release of essential hormones that help maintain ideal health. Many individuals experience symptoms like fatigue, mood swings, and cognitive decline, which can be distressing. It’s heartening to know that research shows hormone therapy can lead to remarkable improvements. In fact, nearly 90% of seniors report feeling more vibrant and alive after treatment.
In addition to boosting energy, these implants can stabilize mood and enhance mental clarity, which is crucial for enjoying a fulfilling life. Imagine feeling less tired and more mentally sharp, allowing you to engage more fully in daily activities. Testimonials from real people highlight these transformative experiences, with many sharing how treatment has revitalized their energy and mental clarity. They express gratitude for being able to enjoy life more fully and manage their responsibilities with renewed enthusiasm.
If you or a loved one are facing challenges related to hormonal changes, know that help is available. It’s important to reach out and explore options that can lead to a brighter, more energetic future. You deserve to thrive and embrace life with open arms.
Convenient Treatment: The Long-Lasting Effects of Hormone Pellets Over Traditional Therapies
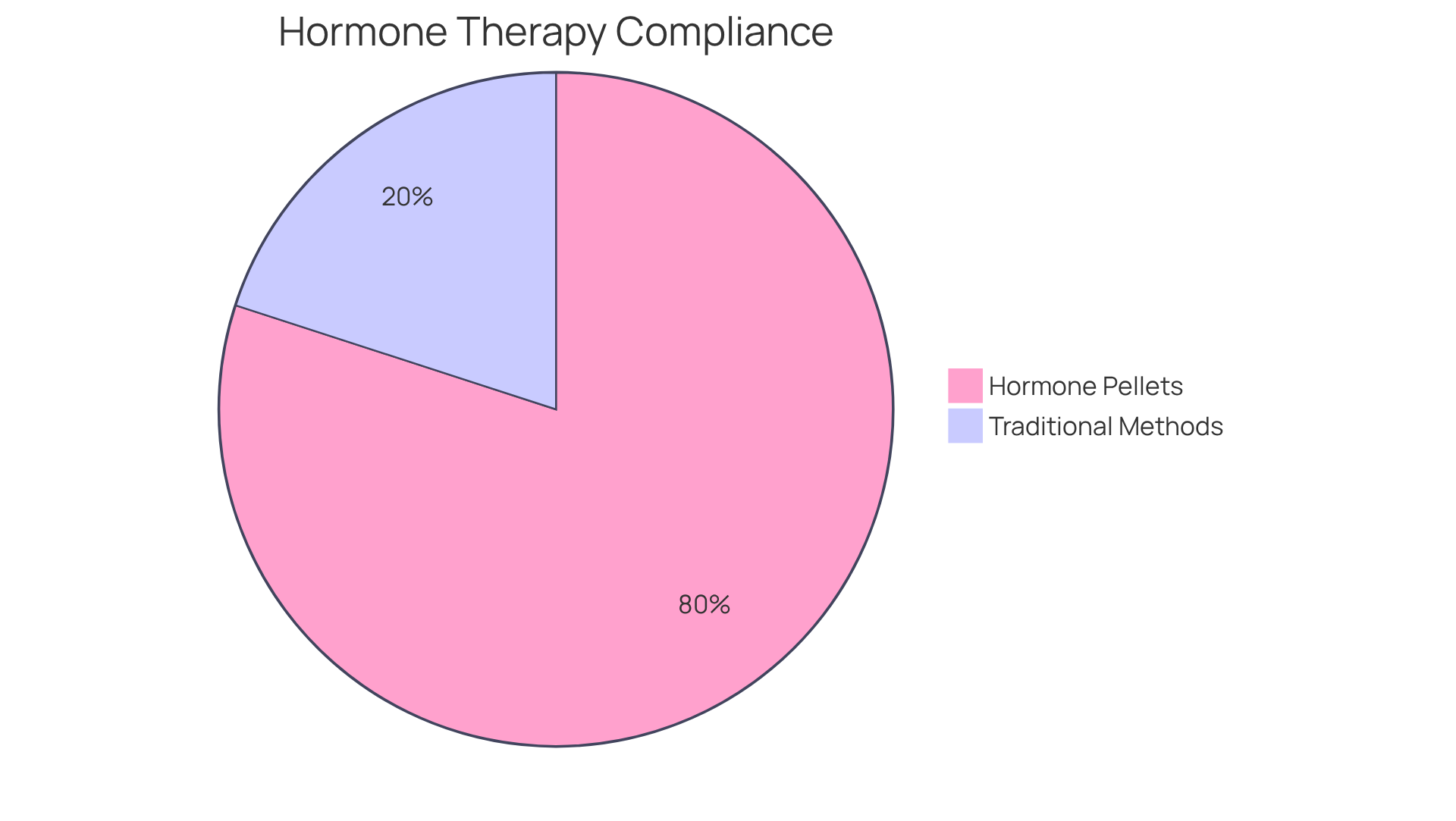
provide a convenient alternative to traditional hormone replacement methods, which often involve daily tablets or regular injections. Imagine not having to remember to take a pill every day! These small doses of hormone pellets, effective for three to six months, eliminate the need for daily administration, making it easier for patients to stick to their treatment plans. In fact, studies show that compliance rates for hormone pellet treatment using hormone pellets for older patients can soar to 80%, compared to lower rates for daily medications.
This long-lasting solution not only simplifies the management of hormone levels but also helps maintain stability, reducing the fluctuations that can occur with other delivery systems, such as injections. Healthcare providers have observed that this ease of use leads to higher adherence rates among elderly patients, who appreciate the relief from the daily burden of medication. As a leading expert wisely noted, “With the exception of vaccines or antibiotics, there’s no treatment that can enhance the well-being of women on a population level more than hormone pellets.”
With hormone pellets, patients can focus on their well-being without the constant reminder of their treatment plan. This ultimately enhances their overall quality of life. If you or a loved one are considering this option, know that support is available to help you navigate your health journey.
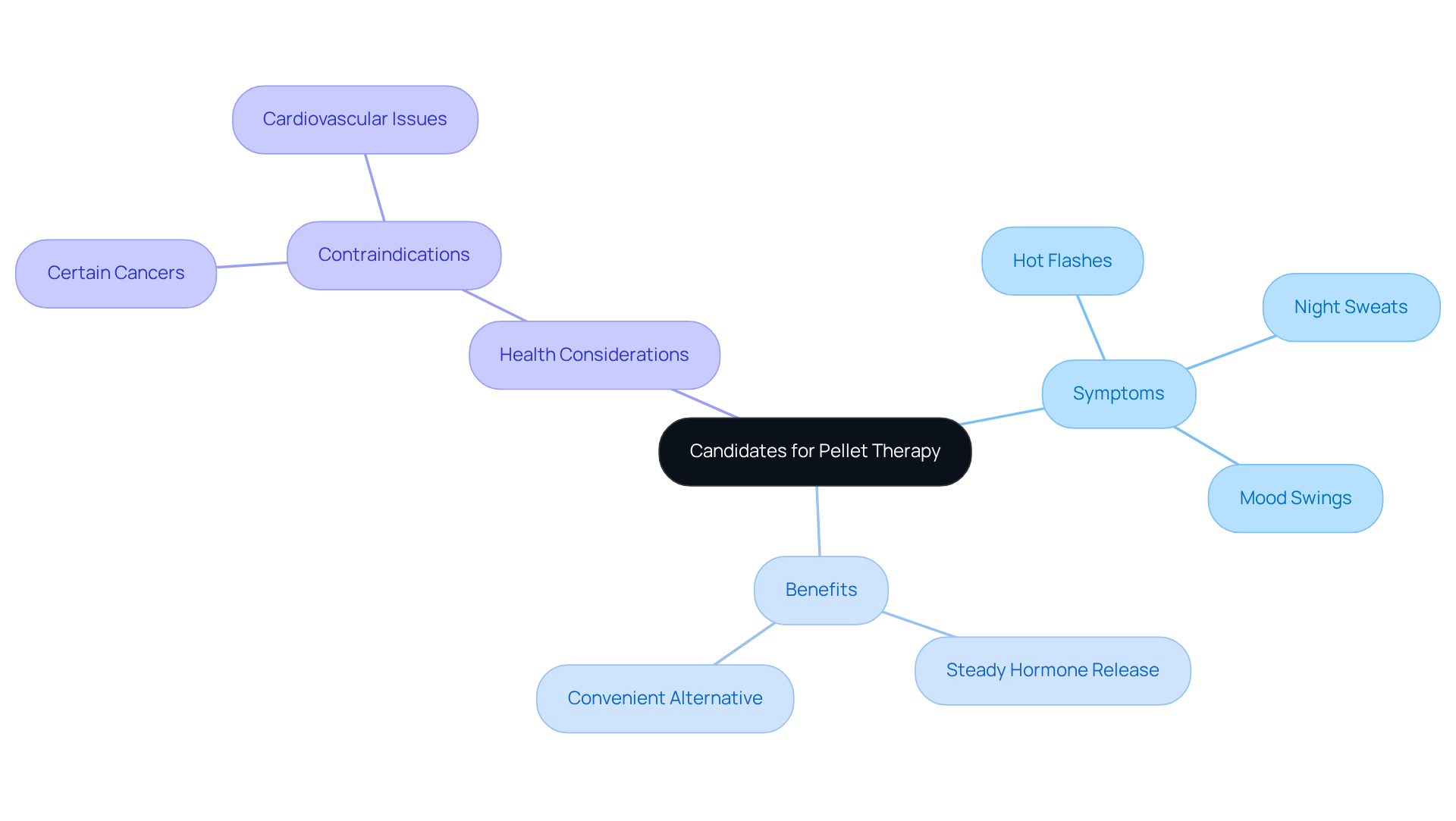
Symptom Relief: Targeting Menopausal and Andropausal Symptoms with Hormone Pellets
provide a compassionate solution for alleviating symptoms related to menopause in women and andropause in men. Many individuals face challenges like hot flashes, night sweats, mood swings, and reduced libido. By effectively addressing these disruptive symptoms, hormone pellet therapy can significantly improve physical and emotional well-being. Have you ever felt a renewed sense of energy and involvement in your daily tasks? Numerous people report just that after beginning treatment.
Recent research suggests that hormonal treatment can lead to improved cognitive ability and emotional balance, especially in older adults. Endocrinologists emphasize that hormone therapy can greatly enhance quality of life, allowing seniors to rediscover their joy and remain actively engaged in social and personal activities. This approach not only alleviates physical discomfort but also nurtures a more positive emotional state, empowering individuals to face the challenges of aging with resilience.
Did you know that many seniors experience hormonal imbalances, yet only 10.5% receive treatment? This highlights the importance of seeking medical help. Furthermore, women may lose as much as 15% of their muscle mass during the first decade of menopause, underscoring the vital role of medical treatment in maintaining overall well-being.
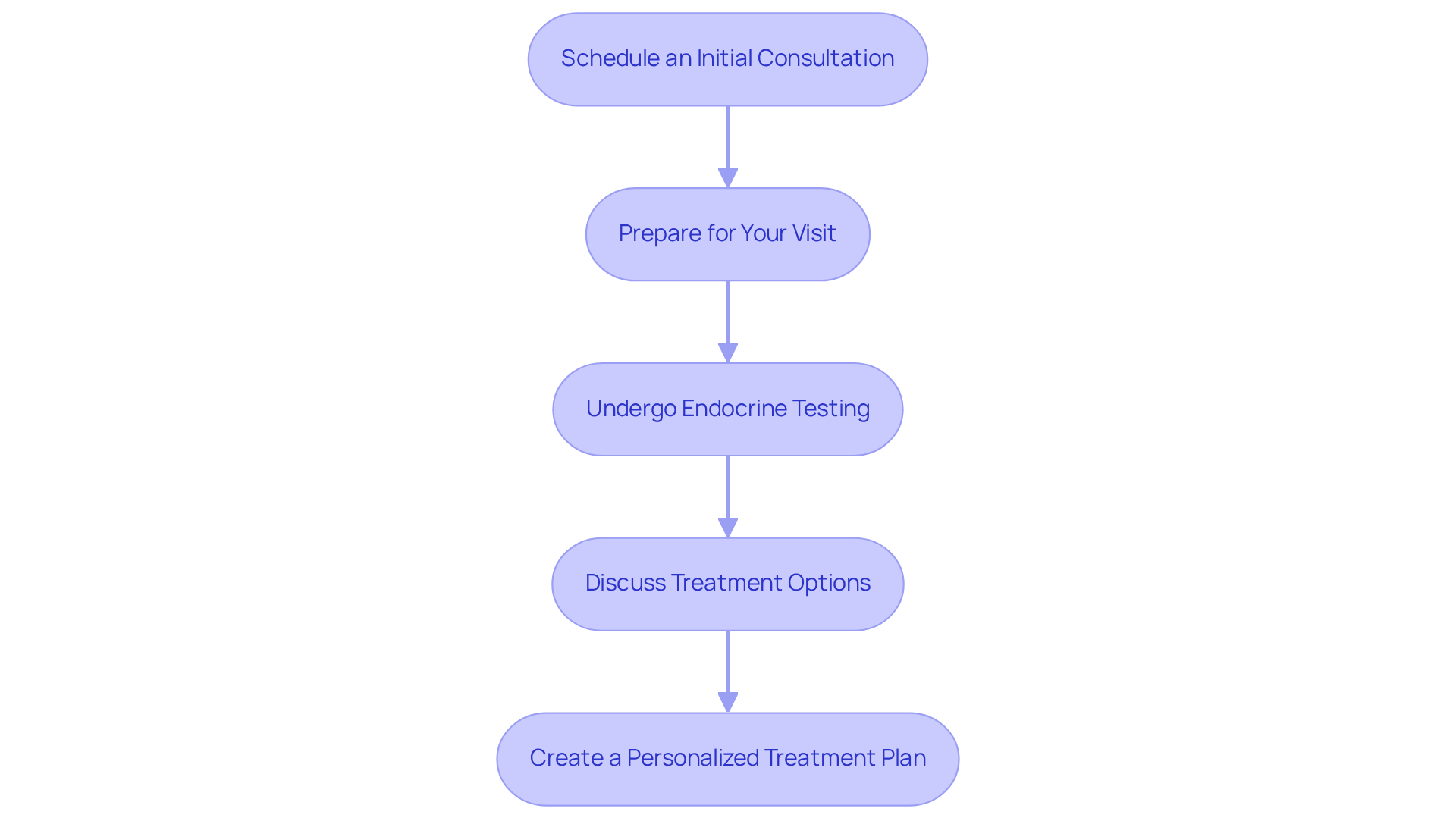
At Amavita, we offer customized treatment plans, which may involve hormone therapy, tailored to meet your individual needs. Our services include:
- Initial consultations
- Assessments
- Various insertion frequencies
This ensures you can achieve optimal balance in your bodily functions and overall health. As one satisfied client shared, “Dr. Martinez-Clark‘s expertise gave me confidence, and the results have been life-changing. I have the energy to excel at work and keep up with the lifestyle I love.”
If you’re ready to explore how our programs can benefit you, please reach out to us today to schedule a consultation. We’re here to support you on your journey to better health.
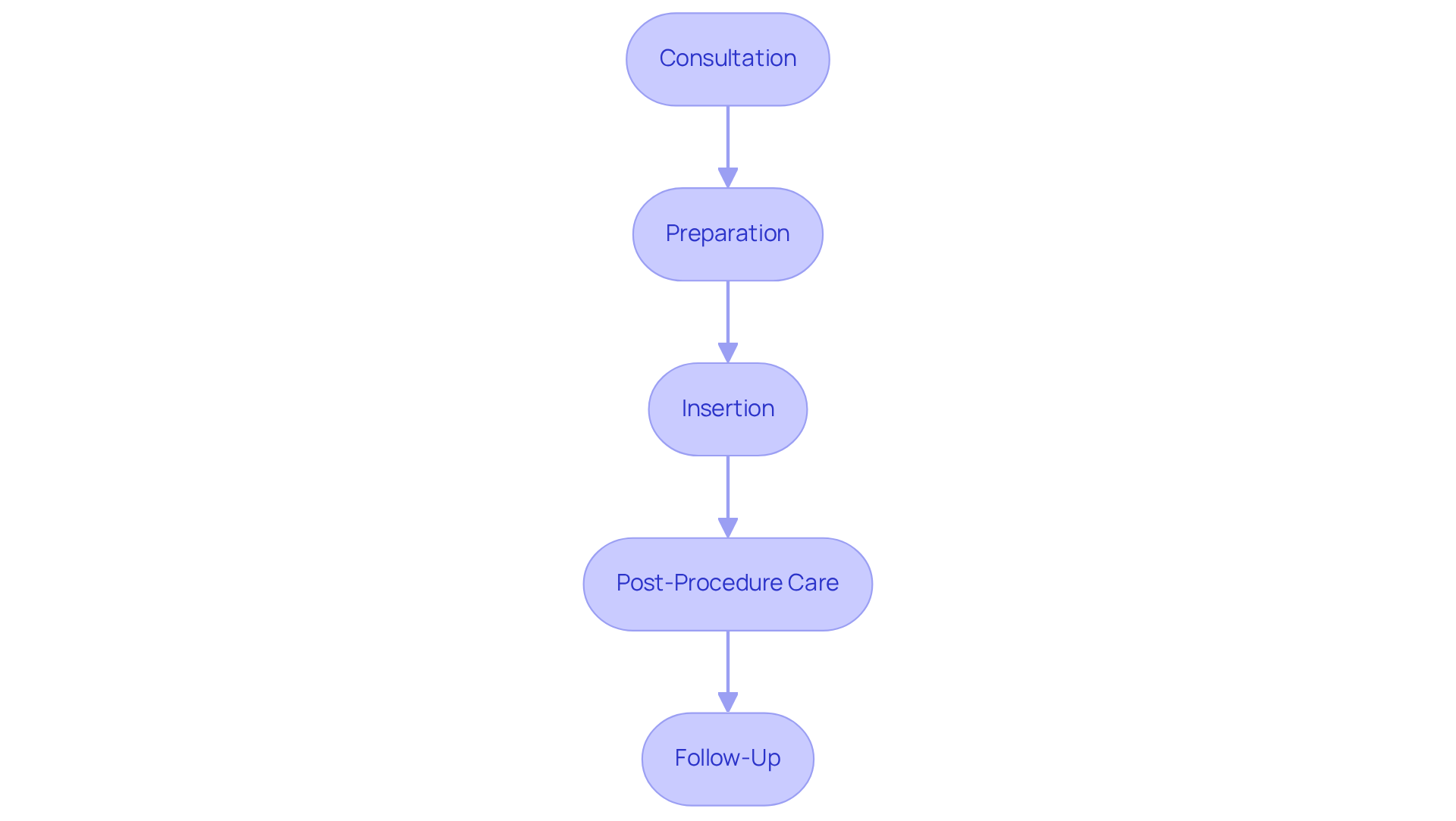
Minimally Invasive Procedure: Understanding the Safety of Hormone Pellet Insertion
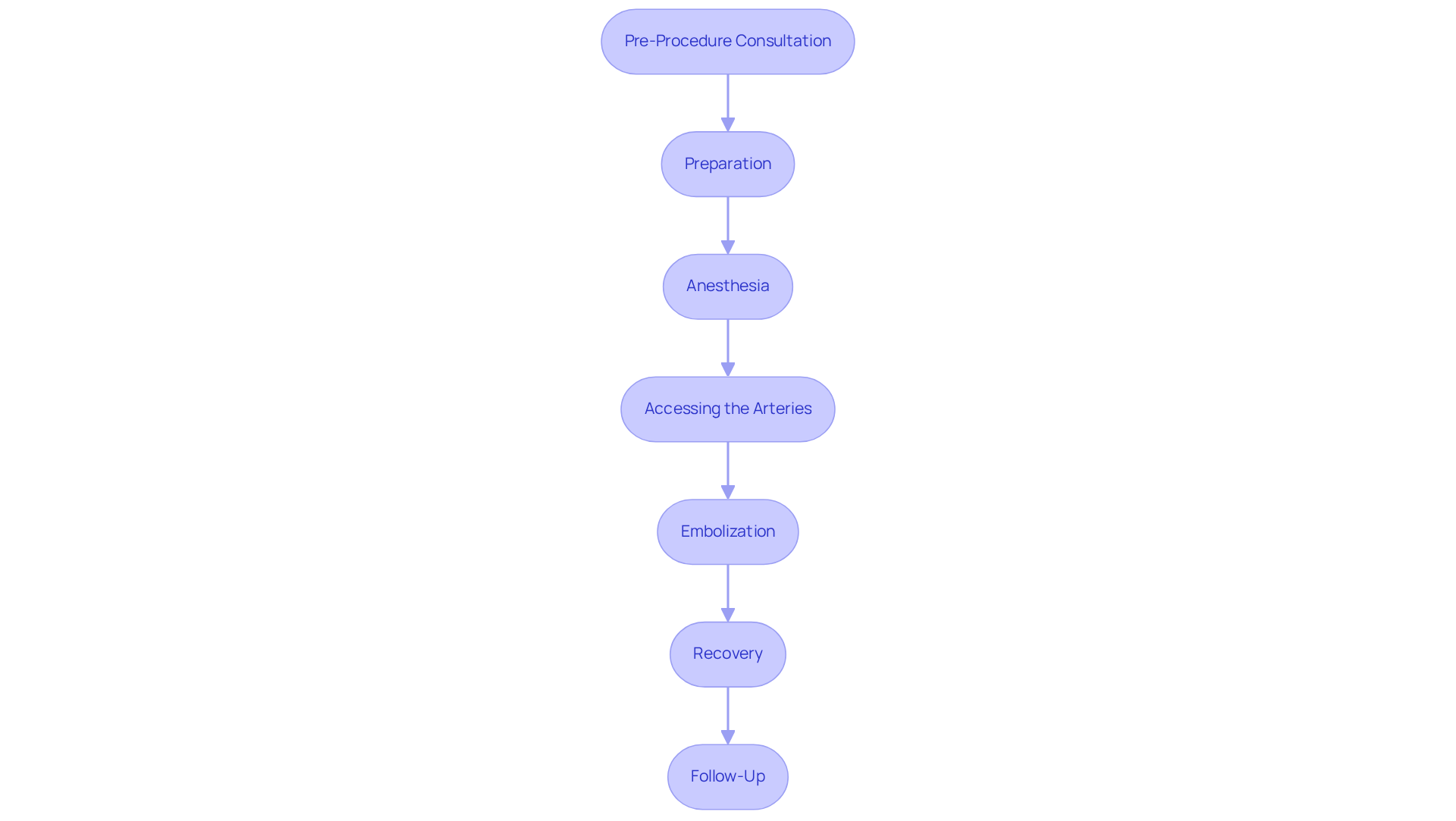
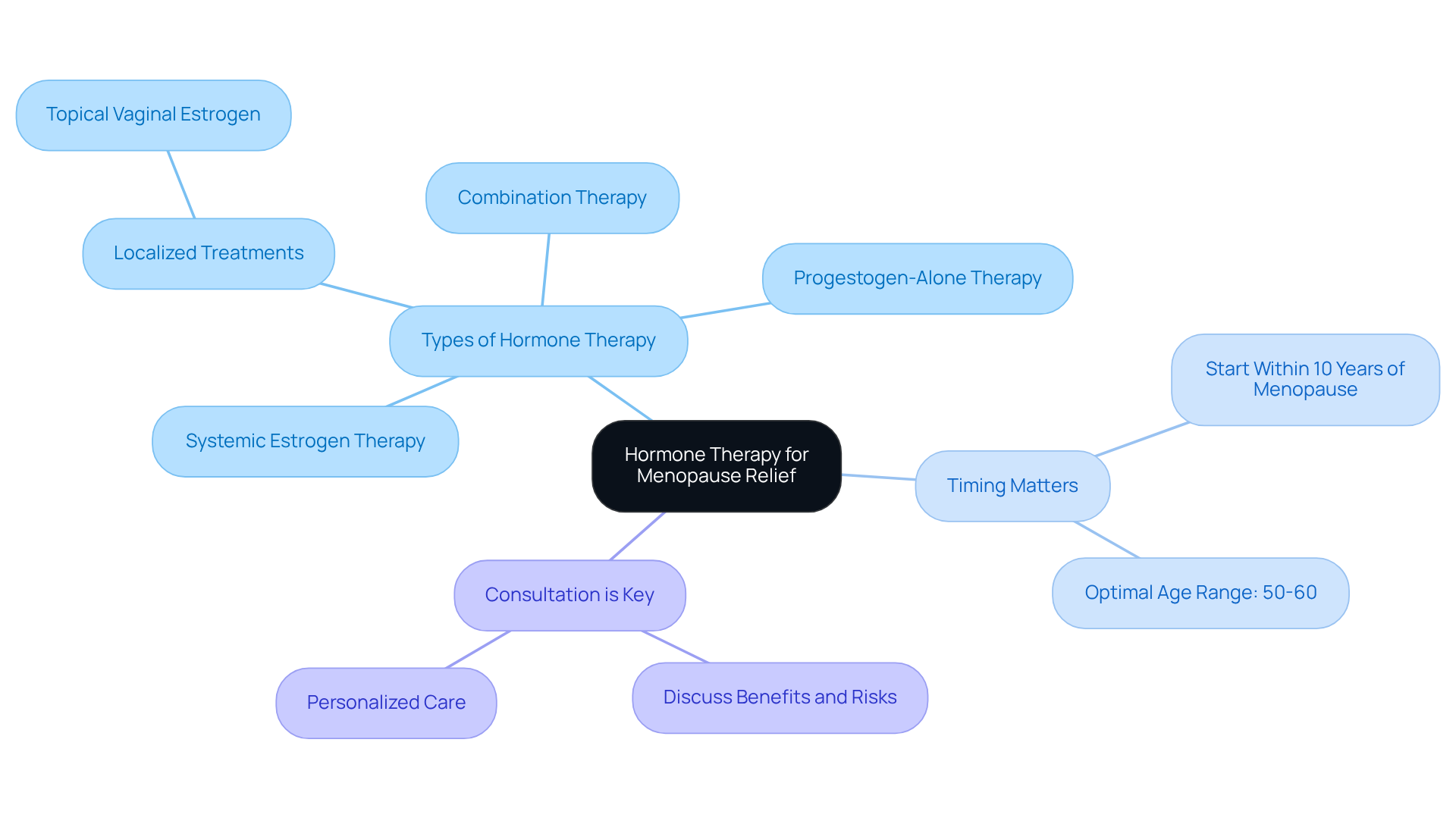
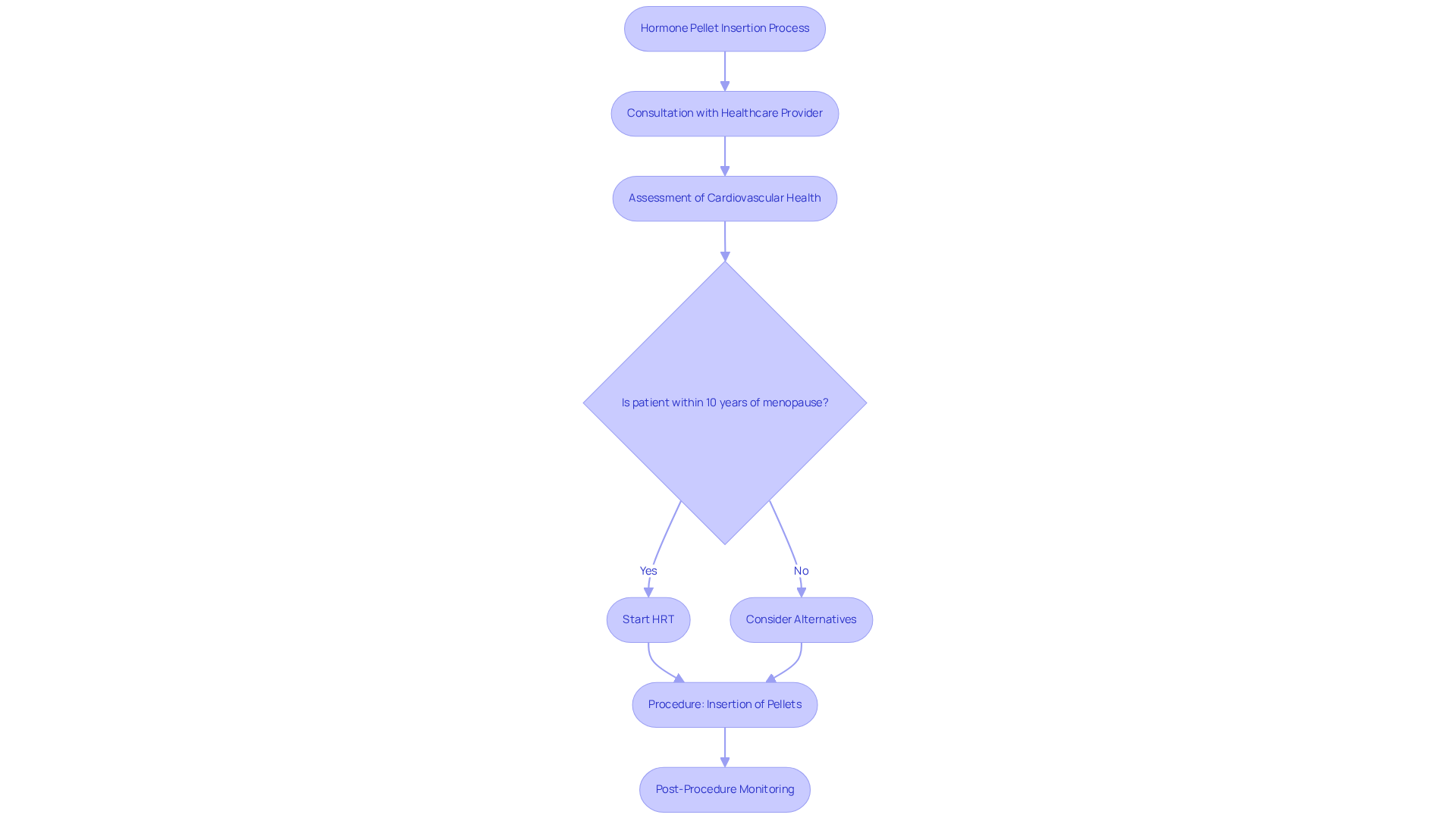
Considering hormone therapy can feel overwhelming, especially for older patients navigating menopause. The placement of endocrine capsules is a minimally invasive technique, typically performed in a medical professional’s office. A small incision allows for hormone pellets to be placed just beneath the skin, often in the hip or buttock area. This quick process usually takes under 30 minutes and carries minimal risks, making it a safe and effective option for those seeking relief from menopausal symptoms.
Recent studies reveal that starting hormone therapy within 10 years of menopause can significantly improve overall health outcomes. In fact, hormone therapy has been shown to notably decrease cardiovascular disease and overall mortality in women under 60. Experts emphasize that these procedures not only alleviate menopausal symptoms but also enhance quality of life, highlighting the importance of timely intervention.
As Dr. Prudence Hall insightfully notes, these chemical messengers act like the body’s internal software, sending essential instructions that keep every system running smoothly. Furthermore, Dr. G. Thomas Ruiz stresses the importance of initiating hormone replacement therapy within 10 years of menopause to maximize its benefits. At Amavita Heart and Vascular Health, we understand the unique needs of older patients. We offer comprehensive assessments, including blood tests, to ensure that your treatment is tailored to your individual health needs.
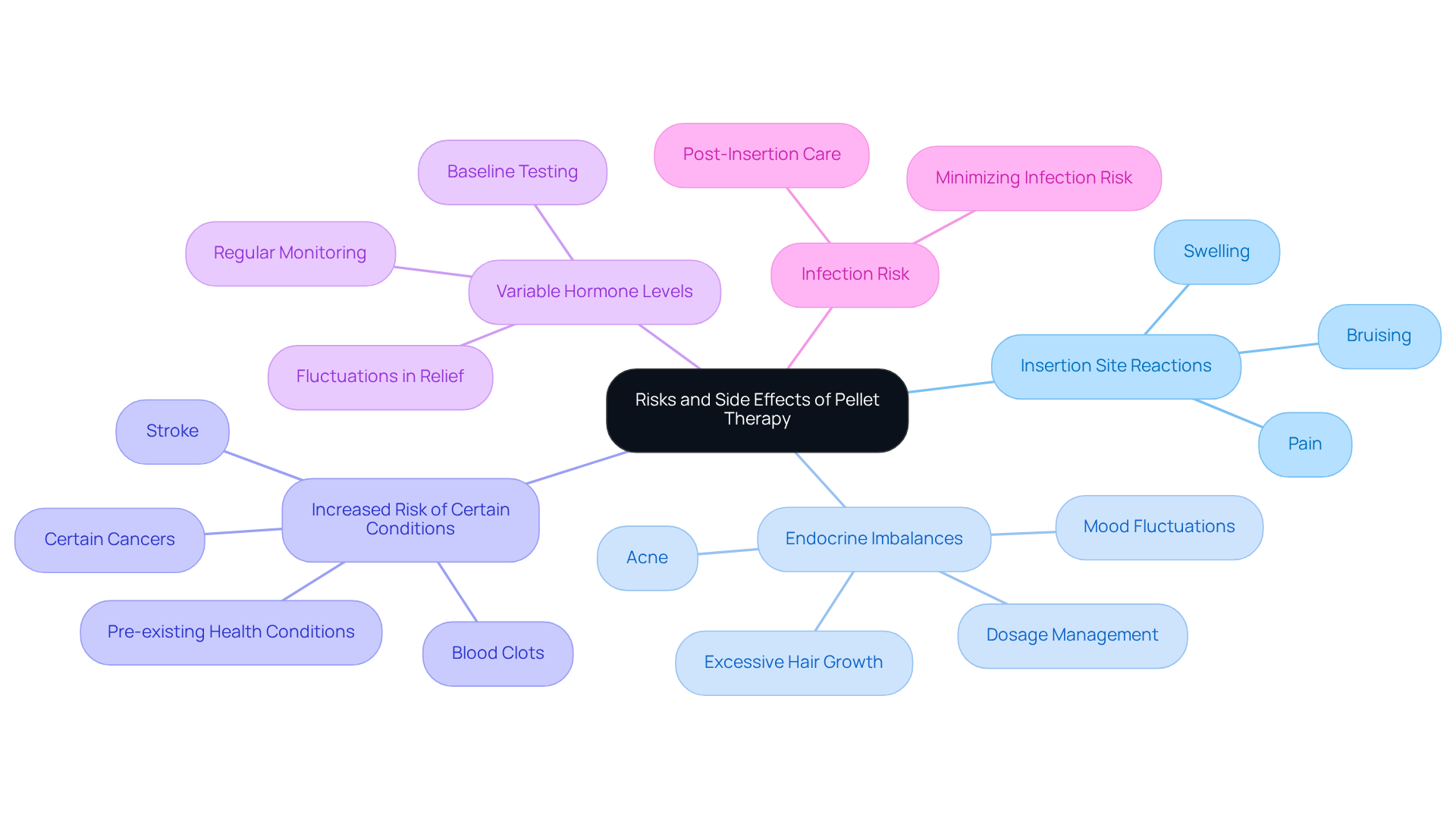
While hormone implants can be beneficial, it’s also important to be aware of potential side effects, such as mood swings, unusual uterine bleeding, and headaches. Discussing these concerns with your healthcare provider is crucial for making informed decisions about your health. Remember, you’re not alone in this journey; we’re here to support you every step of the way.
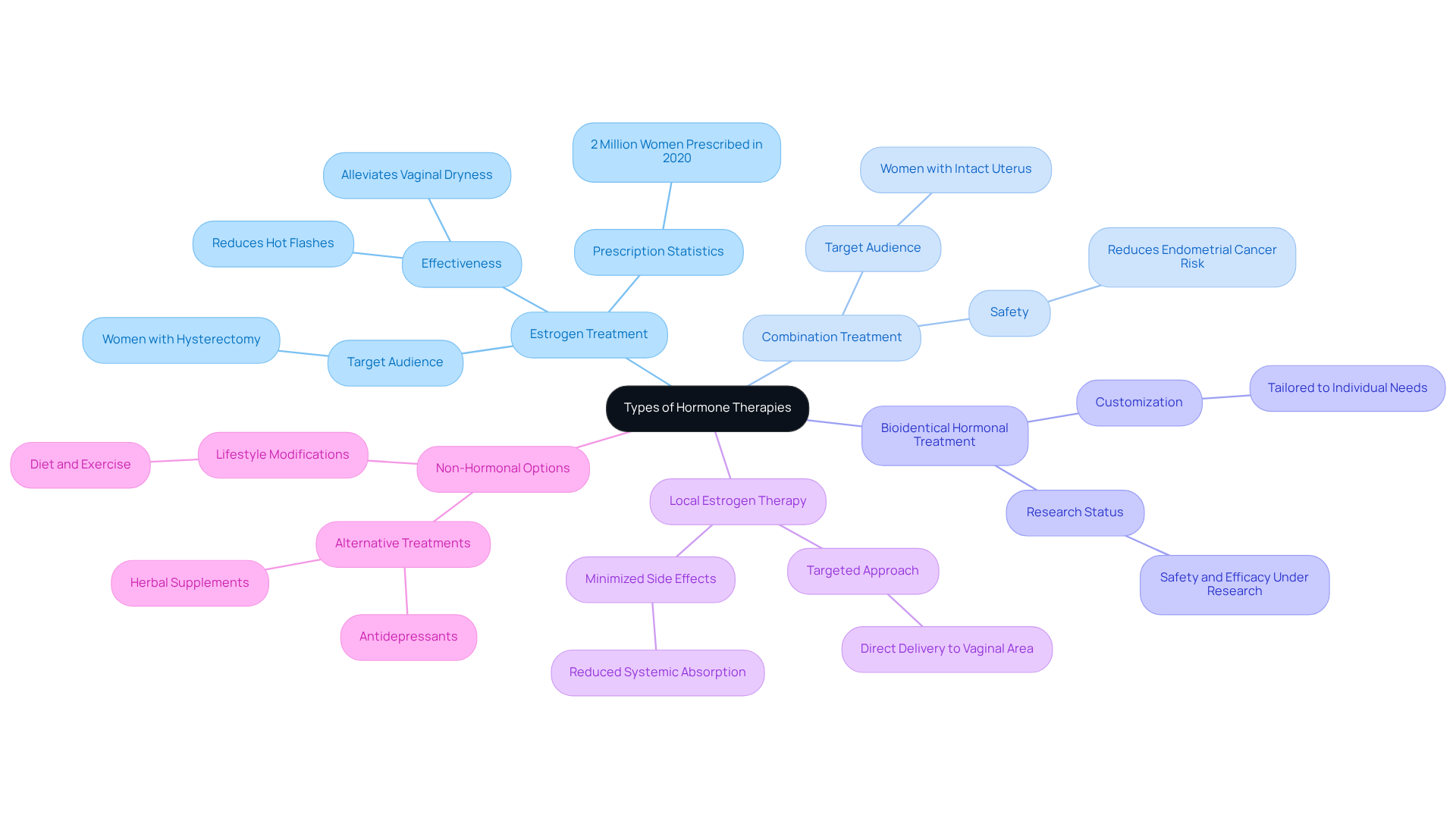
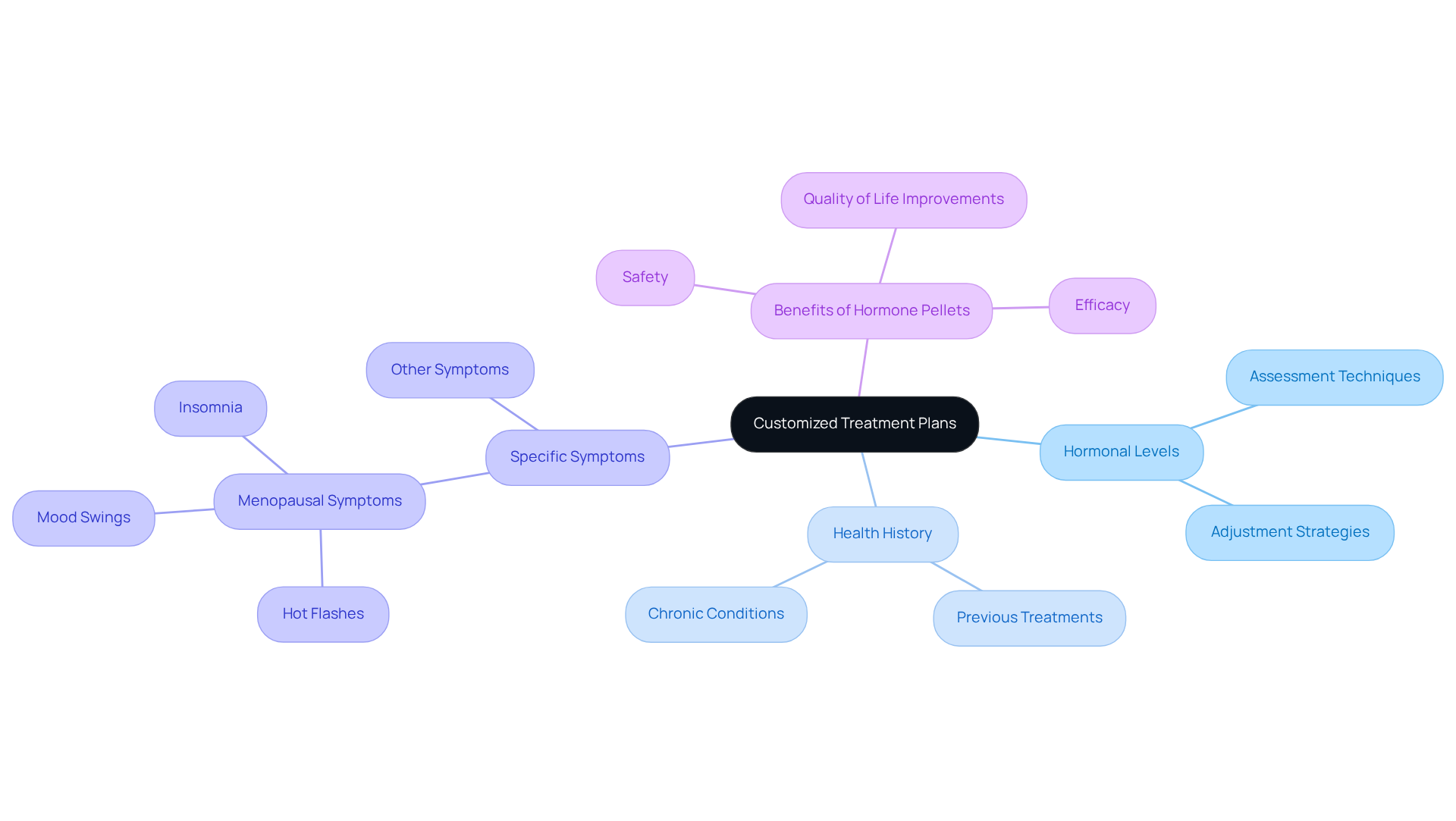
Customized Treatment Plans: Tailoring Hormone Pellets to Individual Needs
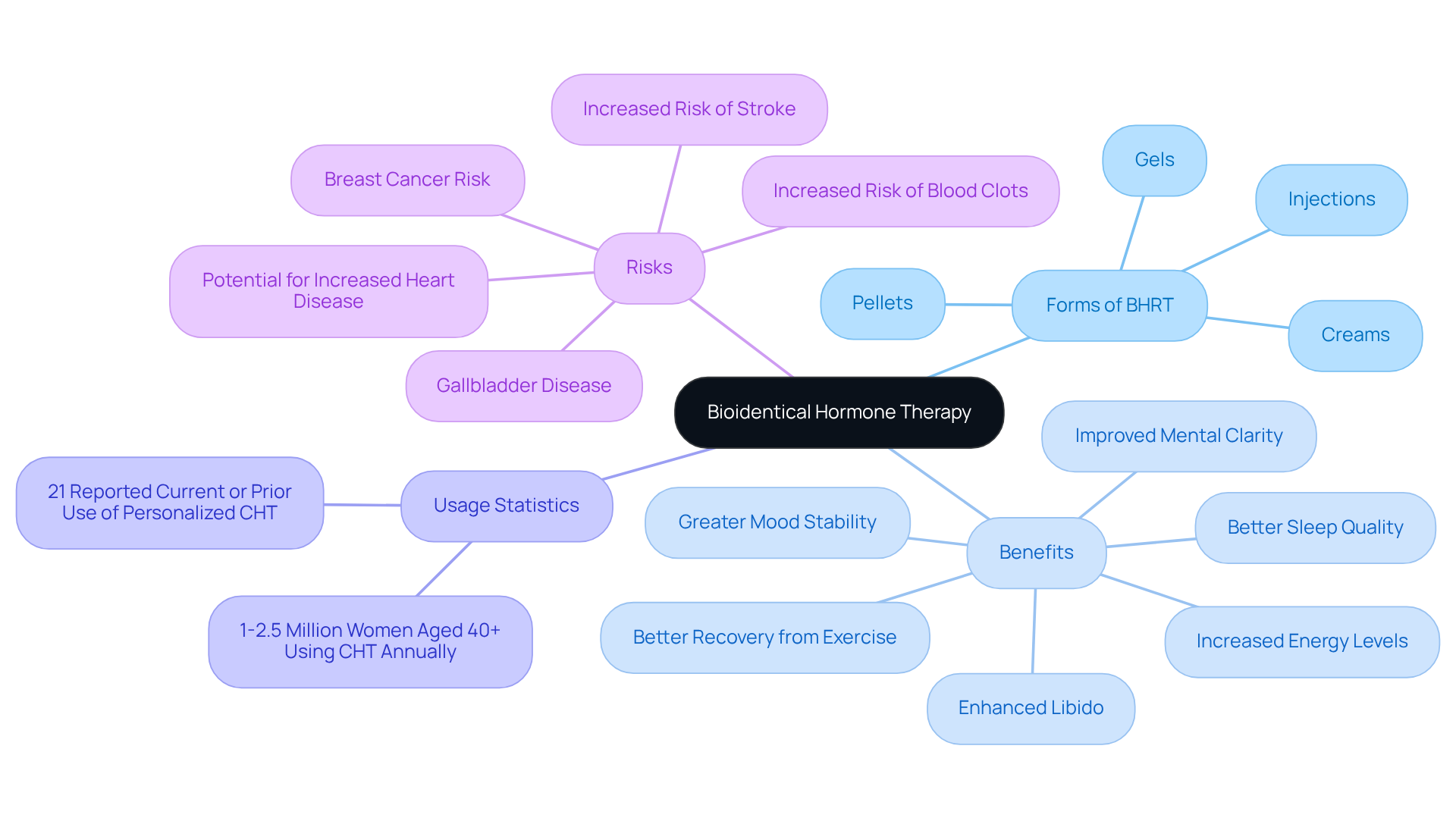
At Amavita, we understand that each individual has unique needs, especially when it comes to health. That’s why our pellet treatment is not a one-size-fits-all solution. Each treatment plan is thoughtfully designed, taking into account your hormonal levels, health history, specific symptoms, and the potential benefits of hormone therapy. This ensures you receive the most effective dosage and type of treatment, enhancing the benefits while minimizing potential side effects.
Have you ever wondered how hormone pellets can truly make a difference? Practical examples show that hormone pellets can lead to significant improvements in managing menopausal symptoms, ultimately enhancing your overall well-being. In fact, a recent survey revealed that 21% of women felt their treatment was tailored to their specific needs, highlighting the effectiveness of personalized care.
The importance of hormone balance is especially crucial as we age. As women grow older, hormone levels can change significantly, necessitating adjustments in treatment to address evolving health concerns. Specialists emphasize that starting therapy with hormone pellets soon after menopause can be most effective, and hormone pellets can help reduce risks associated with hormone replacement.
Endocrine specialists echo this sentiment, noting that a personalized treatment plan not only improves symptom relief but also enhances safety and satisfaction. At Amavita, we are committed to ensuring that you receive the attention and care necessary for optimal health outcomes.
So, if you’re feeling uncertain about your health journey, remember that you’re not alone. We’re here to support you every step of the way, providing the compassionate care you deserve.
Boosted Energy Levels: The Impact of Hormone Pellets on Daily Vitality
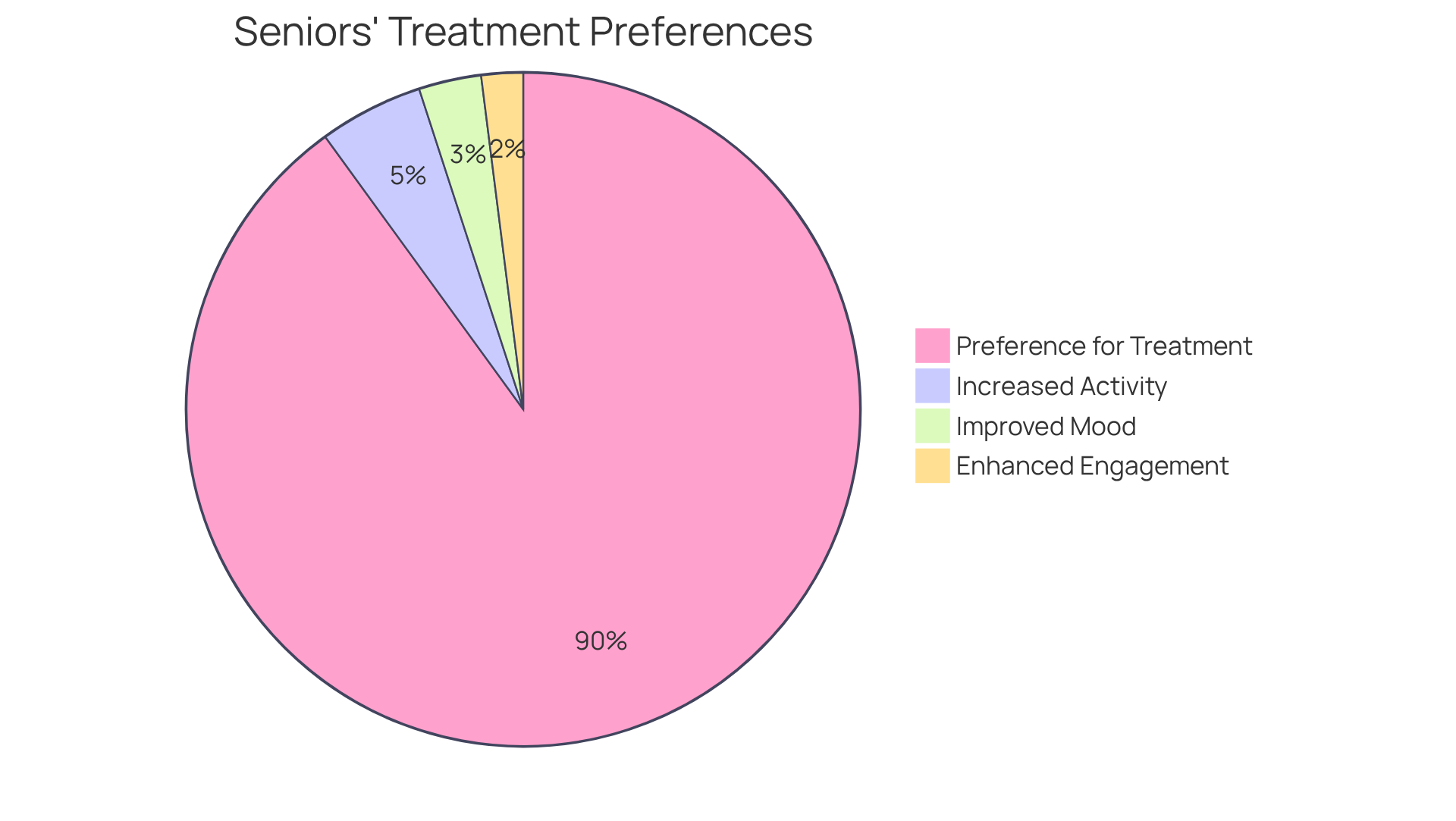
Many patients find a remarkable boost in their energy levels after undergoing endocrine implant treatment. By restoring hormonal balance, hormone pellets help combat fatigue, enabling seniors to engage more actively in their daily lives. Did you know that nearly 90% of seniors prefer hormone pellet therapy? Its simplicity and effectiveness lead to better adherence to care and improved daily functioning.
This surge in energy often means more physical activity, increased social engagement, and an overall enhancement in vitality, contributing to a more fulfilling life. Patients have shared their experiences, highlighting significant improvements in mood and motivation, which reinforces the transformative potential of this treatment. Geriatric specialists emphasize that hormonal treatment, such as hormone pellets, not only alleviates symptoms of imbalance but also plays a crucial role in enhancing quality of life. This makes it an essential component of comprehensive elder care.
If you or a loved one are feeling fatigued or less engaged, consider exploring this option. You deserve to thrive in your daily life.
Improved Mood and Mental Clarity: The Psychological Benefits of Hormone Pellets
The use of hormone pellets in butt can truly make a difference in mood and cognition. By using hormone pellets in butt to stabilize hormone levels, many experience reduced anxiety and enhanced cognitive function, which fosters a greater sense of well-being. For seniors, these benefits are especially important, as they can lead to more fulfilling social interactions and a brighter outlook on life.
Have you ever felt overwhelmed by anxiety? Research shows that hormone therapy can alleviate symptoms. In fact, compared to oral options, hormone pellets provide a more consistent release of hormones. This is reassuring news for those seeking relief.
Mental wellness experts emphasize that maintaining hormonal balance is vital for emotional health. This reinforces the idea that hormone pellets in butt can significantly improve quality of life for senior patients. Remember, you’re not alone in this journey, and support is available to help you navigate these changes.
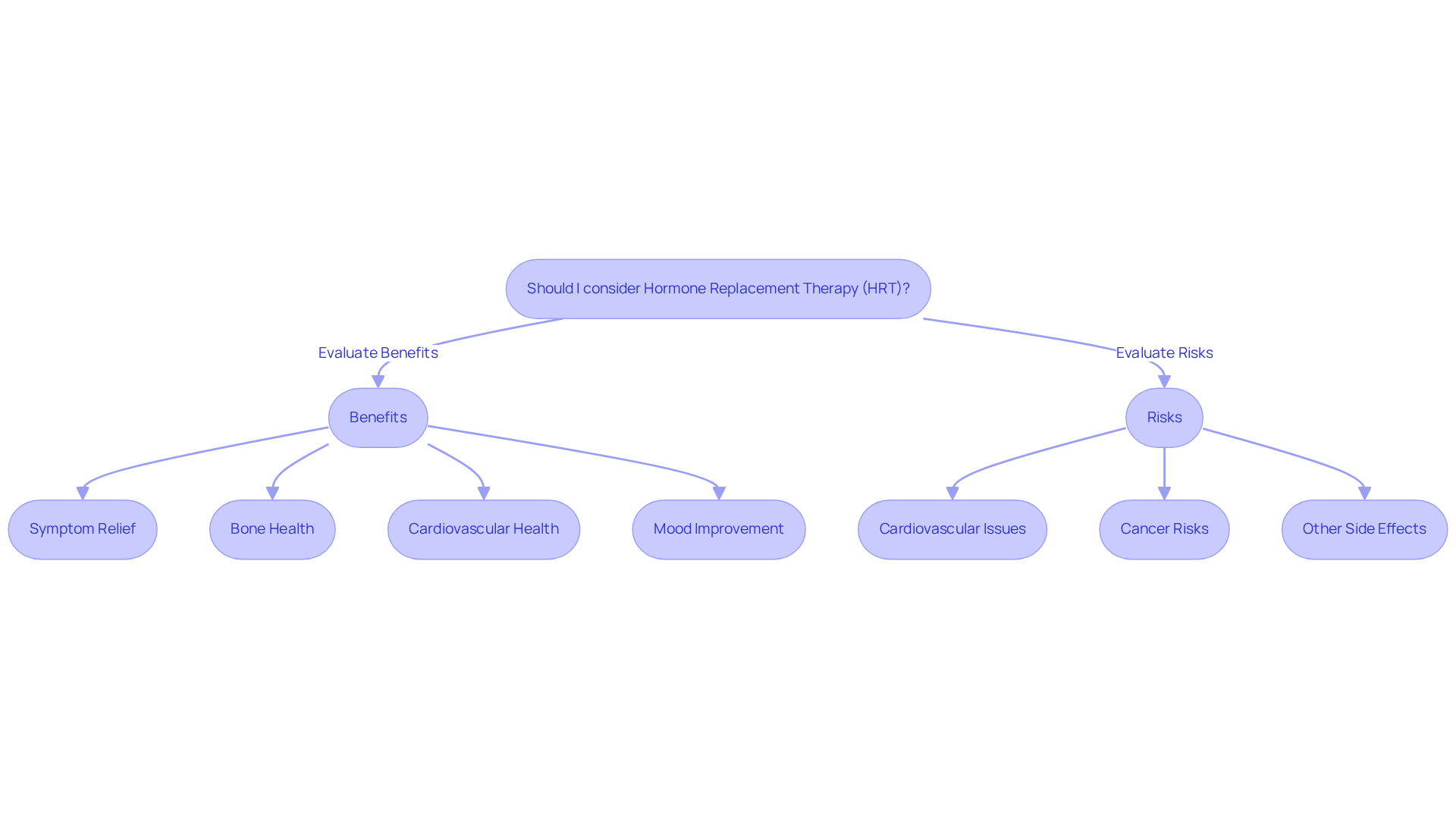
Bone Health Support: How Hormone Pellets Contribute to Osteoporosis Prevention
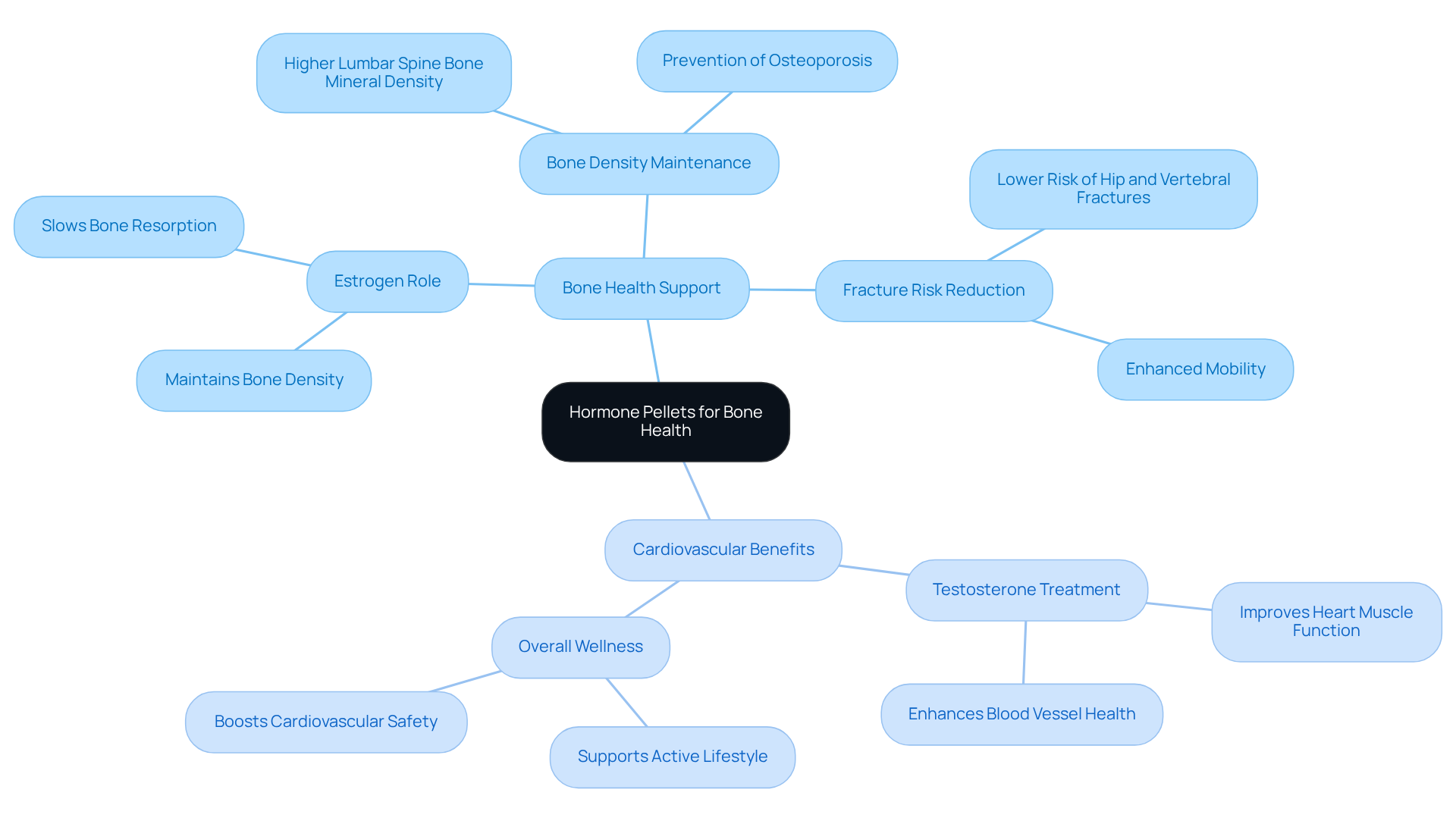
Hormone implants can be a vital ally in preventing osteoporosis and maintaining bone density, especially for our seniors. Research studies and using hormone therapy can help reduce the bone loss that often comes with aging. By supporting bone health, these implants not only lower the risk of fractures but also enhance overall mobility, allowing seniors to lead active, fulfilling lives.
In addition to this, testosterone treatment, part of the hormone therapy regimen, offers proven benefits for heart health. Studies have shown that by improving bone density as much as 6.2% and enhance blood vessel health, which is particularly important for older patients. This comprehensive approach not only supports bone health but also boosts energy levels, ensuring that seniors can enjoy optimal wellness.
Furthermore, Amavita’s unique Virden Method™ and the inclusion of an experienced medical team provide unmatched medical expertise. This reinforces the safety and effectiveness of our treatments, giving you peace of mind. If you have concerns about your health, remember that you’re not alone. We’re here to support you every step of the way.
Innovative Research: The Future of Hormone Pellet Therapy and Its Benefits
Investigations into the use of hormone therapy are moving forward quickly, revealing many benefits for older patients. Recent studies show that the use of hormone pellets can improve cognitive function and overall longevity. For instance, a comprehensive analysis of data from 10 million senior Medicare women has found that hormone therapy can reduce symptoms and enhance quality of life. Specialists emphasize that starting hormonal treatment before the age of 60 yields the best results, particularly in managing and preventing issues like osteoporosis and heart disease.
In addition to this, creative applications of hormone therapy are being explored, focusing on treatments that cater to individual wellness needs. The Menopause Society’s 2022 Position Statement supports the continued use of hormonal treatment for women over 65, provided there is sufficient counseling and risk assessment. This reflects a growing recognition of the subtle benefits of hormonal therapy, which can include symptom relief and improving mental well-being.
Looking ahead, the future of endocrine treatment appears promising, with ongoing clinical trials and studies aimed at refining treatment protocols. Experts advocate for a tailored approach, ensuring that hormone therapy is viewed as a personalized intervention that can lead to significant wellness improvements. As the medical community continues to gather evidence, patients can look forward to more effective and individualized treatment options that enhance their quality of life and overall health outcomes.
Conclusion
The discussion surrounding hormone pellets in the butt highlights their vital role in enhancing the health of our elderly loved ones, especially those facing hormonal imbalances. This innovative therapy not only meets individual hormonal needs but also aligns with cardiovascular care, paving the way for a holistic approach to well-being. By restoring hormonal balance, patients often find themselves experiencing improved energy levels, mood stabilization, and relief from menopausal and andropausal symptoms, ultimately leading to a richer quality of life.
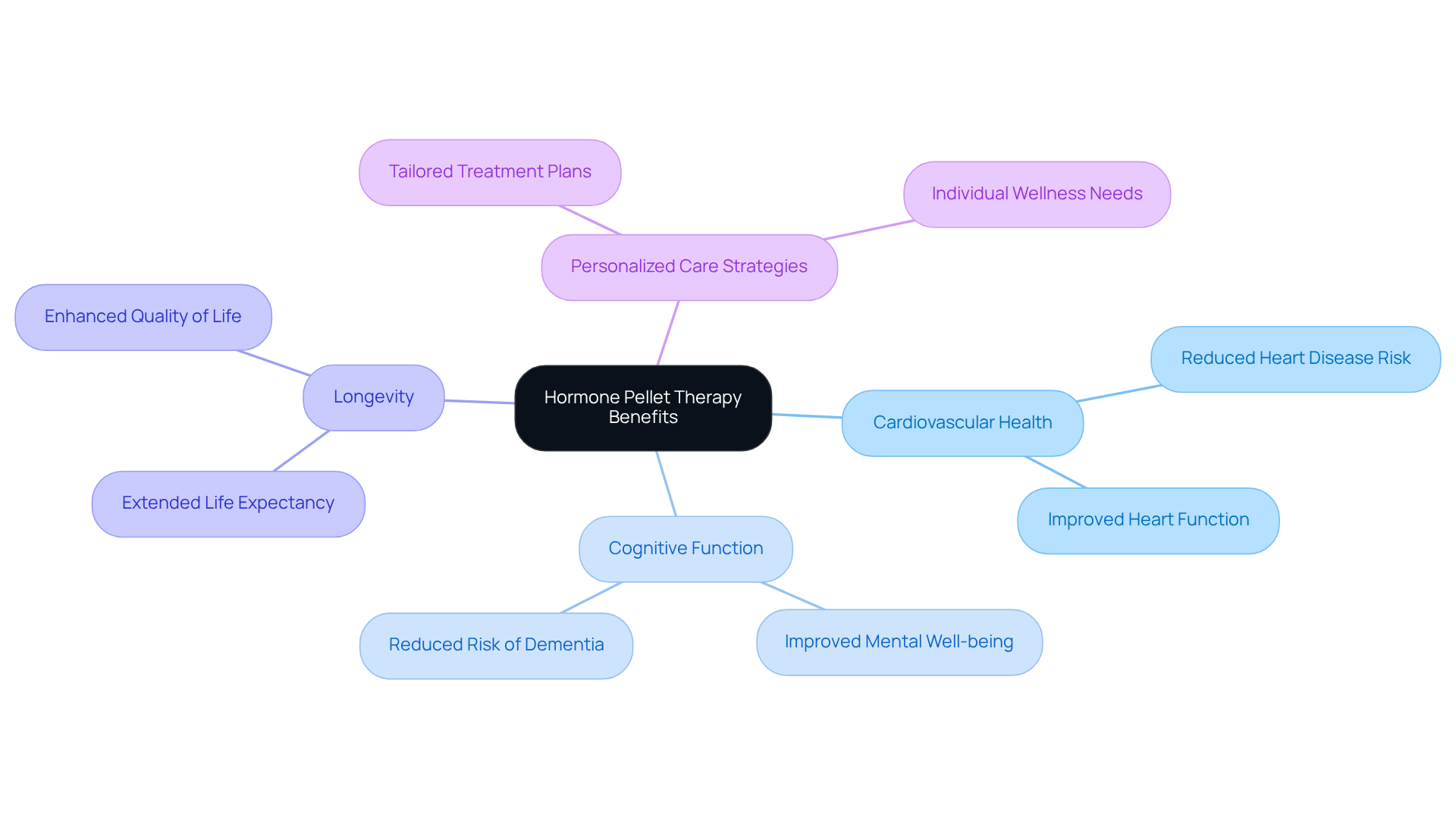
Throughout this article, we’ve explored several key benefits of hormone pellet therapy. These include:
- Enhanced energy and mental clarity
- Improved cardiovascular health
- A convenient treatment method that often surpasses traditional therapies in adherence and effectiveness
Moreover, the personalized nature of hormone pellet treatment ensures that each individual’s unique health profile is taken into account, maximizing the potential for positive outcomes.
As research continues to unveil the myriad benefits of hormone pellets, it’s essential for seniors to consider this option for better health and vitality. The integration of hormone therapy into elder care not only supports physical health but also nurtures emotional well-being, allowing individuals to embrace life with renewed enthusiasm. For those seeking to enhance their quality of life, hormone pellet therapy represents a promising path forward.
Have you thought about how this therapy could improve your daily life? Remember, you’re not alone in this journey. We’re here to support you every step of the way.
Frequently Asked Questions
What is personalized hormone pellet therapy at Amavita Heart and Vascular Care?
Personalized hormone pellet therapy at Amavita is a customized treatment designed to restore hormonal balance in older patients, addressing their unique medical needs while integrating advanced cardiovascular care.
How do hormone pellets improve cardiovascular health?
Research indicates that hormonal treatment using hormone pellets can lead to a significant improvement in cardiovascular health, with studies showing a 30%-50% decrease in coronary heart disease among users compared to non-users.
What benefits do patients experience from hormone pellet therapy?
Patients often report increased energy, mood stabilization, and relief from menopausal symptoms, contributing to an overall better quality of life.
Can you provide an example of a patient’s experience with hormone pellet therapy?
One patient, Michelle, experienced a remarkable reduction in hot flashes and sleep disturbances after receiving treatment, highlighting the effectiveness of the therapy.
What is the duration of effectiveness for hormone pellets?
Hormone pellets are effective for three to six months, eliminating the need for daily administration and simplifying treatment management.
How do hormone pellets compare to traditional hormone replacement methods?
Hormone pellets provide a more convenient alternative to daily tablets or regular injections, leading to higher compliance rates among older patients, which can reach up to 80%.
What overall improvements can patients expect from hormone pellet therapy?
Patients can expect improvements in energy levels, mood stabilization, and cognitive function, allowing them to engage more fully in daily activities.
How can individuals facing hormonal imbalances seek help?
Individuals experiencing challenges related to hormonal imbalances are encouraged to reach out and explore treatment options available to improve their well-being and embrace life more fully.
List of Sources
- Amavita Heart and Vascular Health: Personalized Hormone Pellet Therapy for Optimal Balance
- Patty Vila Media Press Releases
- EIN Presswire – Press Release Distribution Service (https://einpresswire.com/sources/u596103)
- Checking your browser – reCAPTCHA (https://pmc.ncbi.nlm.nih.gov/articles/PMC9178928)
- amavita Heart and Vascular Health® | Top Cardiologist in Miami, FL (https://amavita.health/blog/10-pellet-therapy-reviews-wellness-insights-for-elderly-patients)
- Hormone Pellet Therapy: Why Doctors Are Recommending It – Optimal Medical Group in Fresno, California (https://omgwellnessmd.com/blog/hormone-pellet-therapy)
- Unlocking Hormonal Balance: The Benefits of Pellet Therapy (https://bodylogicmd.com/blog/unlocking-hormonal-balance-the-benefits-of-pellet-therapy)
- Enhanced Hormonal Balance: How Hormone Pellets Improve Overall Well-Being
- US health leaders hailed the benefits of hormone therapy for menopause. Doctors are pushing for balance | CNN (https://edition.cnn.com/2025/11/12/health/fda-hormone-therapy-menopause-balance)
- FDA chief says warning labels deterred women from using menopause hormone therapy: “It’s an American tragedy” (https://cbsnews.com/news/fda-hormone-therapy-marty-makary-interview)
- Why The FDA’s New Move On Hormone Therapy Could Help Women’s Careers (https://forbes.com/sites/kimelsesser/2025/11/11/why-the-fdas-new-move-on-hormone-therapy-could-help-womens-careers)
- amavita Heart and Vascular Health® | Top Cardiologist in Miami, FL (https://amavita.health/blog/10-pellet-therapy-reviews-wellness-insights-for-elderly-patients)
- Convenient Treatment: The Long-Lasting Effects of Hormone Pellets Over Traditional Therapies
- The FDA removes a long-standing warning from hormone-based menopause drugs (https://apnews.com/article/menopause-hormones-warning-fda-drugs-pills-women-f26a8208fd3f5174ec96d61140439561)
- FDA chief says warning labels deterred women from using menopause hormone therapy: “It’s an American tragedy” (https://cbsnews.com/news/fda-hormone-therapy-marty-makary-interview)
- US health leaders hailed the benefits of hormone therapy for menopause. Doctors are pushing for balance | CNN (https://edition.cnn.com/2025/11/12/health/fda-hormone-therapy-menopause-balance)
- Hormone pellets, the ‘miracle’ anti-aging treatment under scrutiny (https://english.elpais.com/health/2025-03-26/hormone-pellets-the-miracle-anti-aging-treatment-under-scrutiny.html)
- HHS Advances Women’s Health, Removes Misleading FDA Warnings on Hormone Replacement Therapy (https://hhs.gov/press-room/hhs-advances-womens-health-removes-misleading-fda-warnings-hormone-replacement-therapy.html)
- Symptom Relief: Targeting Menopausal and Andropausal Symptoms with Hormone Pellets
- FDA chief says warning labels deterred women from using menopause hormone therapy: “It’s an American tragedy” (https://cbsnews.com/news/fda-hormone-therapy-marty-makary-interview)
- The No.1 Menopause Doctor They’re Lying To You About Menopause! Brand New Science! (Men Need To Listen Too!) Mary Claire Haver (https://deciphr.ai/podcast/the-no1-menopause-doctor-theyre-lying-to-you-about-menopause-brand-new-science-men-need-to-listen-too-mary-claire-haver)
- Case Studies: Diseases (https://bio.libretexts.org/Bookshelves/Introductory_and_General_Biology/Supplemental_Modules_(Molecular_Biology)/Case_Studies:_Diseases)
- medicalnewstoday.com (https://medicalnewstoday.com/articles/fda-black-box-warnings-hormone-replacement-therapy-menopause-explainer)
- Hormone replacement therapy will no longer carry a warning label, FDA says (https://nbcnews.com/health/womens-health/hormone-replacement-therapy-no-warning-label-fda-rcna243008)
- Minimally Invasive Procedure: Understanding the Safety of Hormone Pellet Insertion
- medicalnewstoday.com (https://medicalnewstoday.com/articles/fda-black-box-warnings-hormone-replacement-therapy-menopause-explainer)
- Hormone pellets, the ‘miracle’ anti-aging treatment under scrutiny (https://english.elpais.com/health/2025-03-26/hormone-pellets-the-miracle-anti-aging-treatment-under-scrutiny.html)
- Hormone therapy safety: Study finds potential benefits for senior women | Contemporary OB/GYN (https://contemporaryobgyn.net/view/hormone-therapy-safety-study-finds-potential-benefits-for-senior-women)
- Hormones for menopause are safe, study finds. Here’s what changed (https://npr.org/sections/health-shots/2024/05/01/1248525256/hormones-menopause-hormone-therapy-hot-flashes)
- Hormone pellet safety data ‘not very reassuring at all’ for women | MDedge (https://mdedge.com/obgyn/article/241740/menopause/hormone-pellet-safety-data-not-very-reassuring-all-women)
- Customized Treatment Plans: Tailoring Hormone Pellets to Individual Needs
- FDA chief says warning labels deterred women from using menopause hormone therapy: “It’s an American tragedy” (https://cbsnews.com/news/fda-hormone-therapy-marty-makary-interview)
- researchgate.net (https://researchgate.net/publication/272514958_Compounded_bioidentical_hormone_therapy_Identifying_use_trends_and_knowledge_gaps_among_US_women)
- US health leaders hailed the benefits of hormone therapy for menopause. Doctors are pushing for balance | CNN (https://edition.cnn.com/2025/11/12/health/fda-hormone-therapy-menopause-balance)
- HHS Advances Women’s Health, Removes Misleading FDA Warnings on Hormone Replacement Therapy (https://fda.gov/news-events/press-announcements/hhs-advances-womens-health-removes-misleading-fda-warnings-hormone-replacement-therapy)
- Boosted Energy Levels: The Impact of Hormone Pellets on Daily Vitality
- Hormone pellets, the ‘miracle’ anti-aging treatment under scrutiny (https://english.elpais.com/health/2025-03-26/hormone-pellets-the-miracle-anti-aging-treatment-under-scrutiny.html)
- nejm.org (https://nejm.org/doi/full/10.1056/NEJMoa1506119)
- amavita Heart and Vascular Health® | Top Cardiologist in Miami, FL (https://amavita.health/blog/10-pellet-therapy-reviews-wellness-insights-for-elderly-patients)
- Hormone Pellet Therapy — Hancock Women’s Center (https://hancockwomenscenter.net/hormone-pellet-therapy)
- virtua.org (https://virtua.org/articles/tracys-hormone-replacement-therapy-success-story)
- Improved Mood and Mental Clarity: The Psychological Benefits of Hormone Pellets
- embracehealth.com (https://embracehealth.com/blog/50-quotes-about-mental-health)
- 28 Inspiring Mental Health Quotes That Will Empower You (https://positivepsychology.com/mental-health-quotes)
- Sweet spot for HRT may reduce dementia risk by nearly a third, study says | CNN (https://cnn.com/2023/11/02/health/hormone-replacement-dementia-wellness)
- Hormone therapy safety: Study finds potential benefits for senior women | Contemporary OB/GYN (https://contemporaryobgyn.net/view/hormone-therapy-safety-study-finds-potential-benefits-for-senior-women)
- Transdermal hormone therapy linked to lower rates of anxiety, depression in postmenopausal women | Contemporary OB/GYN (https://contemporaryobgyn.net/view/transdermal-hormone-therapy-linked-to-lower-rates-of-anxiety-depression-in-postmenopausal-women)
- Bone Health Support: How Hormone Pellets Contribute to Osteoporosis Prevention
- The Role of Estrogen in Bone Health: Insights for Aging Women (https://hera-health.com/estrogen-in-bone-health)
- Time trend analysis of osteoporosis prevalence among adults 50 years of age and older in the USA, 2005–2018 – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11882656)
- Estrogen and Bone Health: Insights for Aging Women (https://myobgynvegas.com/estrogen-in-bone-health)
- Osteoporosis: Hormone therapy may increase bone mineral density (https://medicalnewstoday.com/articles/hormone-therapy-may-increase-bone-density-prevent-osteoporosis)
- drlouisenewson.co.uk (https://drlouisenewson.co.uk/knowledge/can-hrt-and-testosterone-prevent-osteoporosis)
- Innovative Research: The Future of Hormone Pellet Therapy and Its Benefits
- US health leaders hailed the benefits of hormone therapy for menopause. Doctors are pushing for balance | CNN (https://edition.cnn.com/2025/11/12/health/fda-hormone-therapy-menopause-balance)
- Hormone therapy safety: Study finds potential benefits for senior women | Contemporary OB/GYN (https://contemporaryobgyn.net/view/hormone-therapy-safety-study-finds-potential-benefits-for-senior-women)
- FDA reverses decades-old warning on hormone therapy products for menopause (https://statnews.com/2025/11/10/fda-reverses-hormone-warning-menopause-health)
- HHS Advances Women’s Health, Removes Misleading FDA Warnings on Hormone Replacement Therapy (https://fda.gov/news-events/press-announcements/hhs-advances-womens-health-removes-misleading-fda-warnings-hormone-replacement-therapy)