Introduction
Understanding heart health can feel overwhelming, especially for older adults facing complex medical issues. The Automatic Implantable Cardioverter Defibrillator (AICD) is a remarkable solution that monitors heart rhythms and steps in when needed, greatly lowering the risk of sudden cardiac death. This article explores the vital aspects of AICD technology, highlighting its life-saving benefits and the details of the implantation process, while also considering the potential risks involved.
How can elderly patients navigate these challenges to make informed decisions about their heart health? It’s important to remember that you’re not alone in this journey. With the right information and support, you can take proactive steps towards better heart health.
Define AICD: Significance in Cardiology
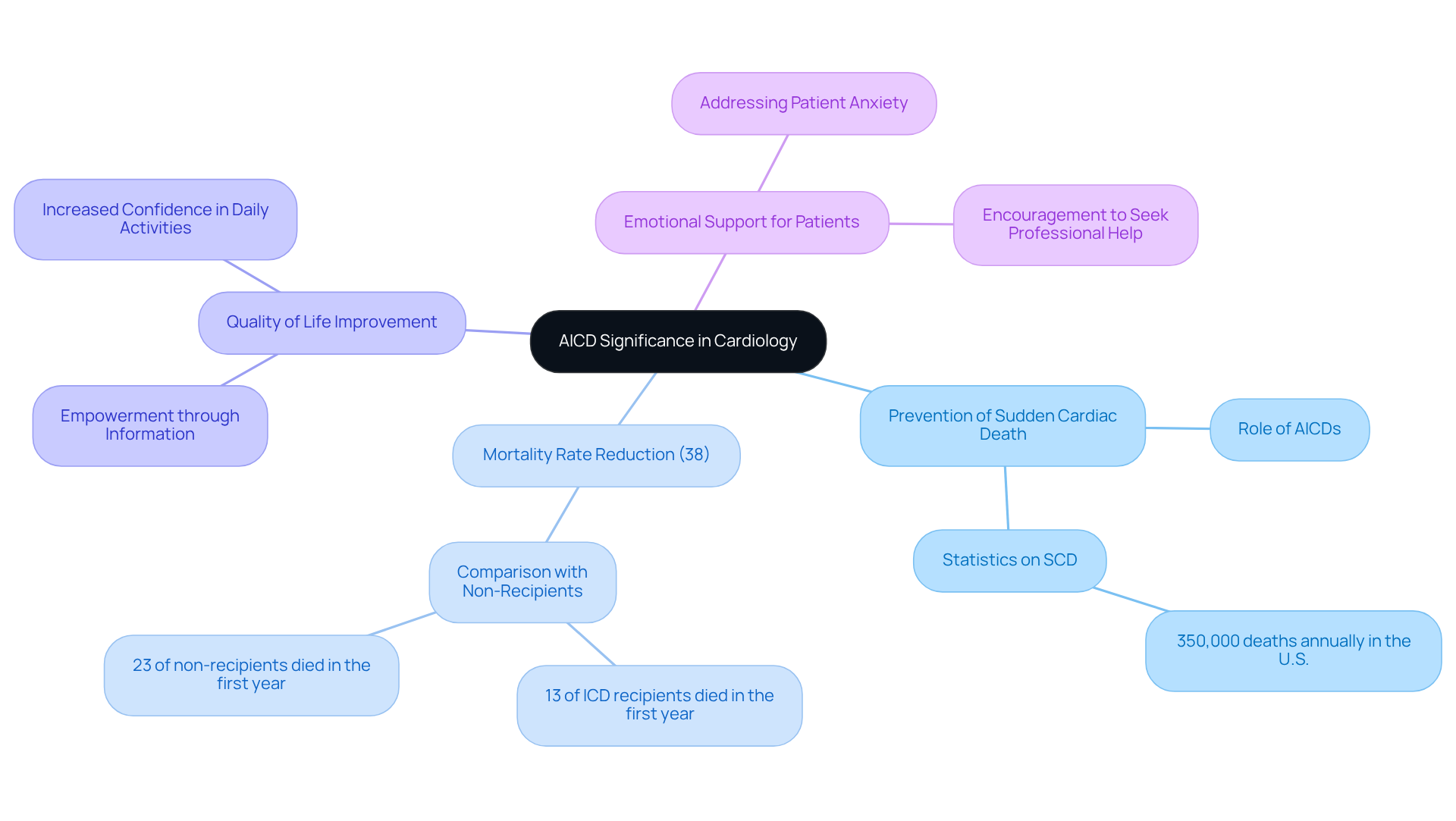
An AICD is a remarkable medical device designed to keep a close watch on your heart rhythms. It steps in when needed to help prevent sudden cardiac death, which can be a real concern, especially for older adults facing conditions like heart failure or a previous heart attack. Did you know that research shows AICDs can reduce mortality by 38% compared to those without this device?
But it’s not just about survival; AICDs can also improve quality of life. Imagine being able to engage in daily activities with more confidence and security. As our population ages, it’s crucial to understand how AICDs can play a vital role in your health management.
If you or a loved one are feeling anxious about AICD implantation, remember that you’re not alone. It’s perfectly normal to have concerns, and seeking information is a great first step. Understanding the benefits of AICDs can empower you to make informed decisions about your health. So, why not reach out to a healthcare professional to discuss your options? You deserve to feel secure and supported in your health journey.
Explain How AICD Works: Mechanisms and Functionality
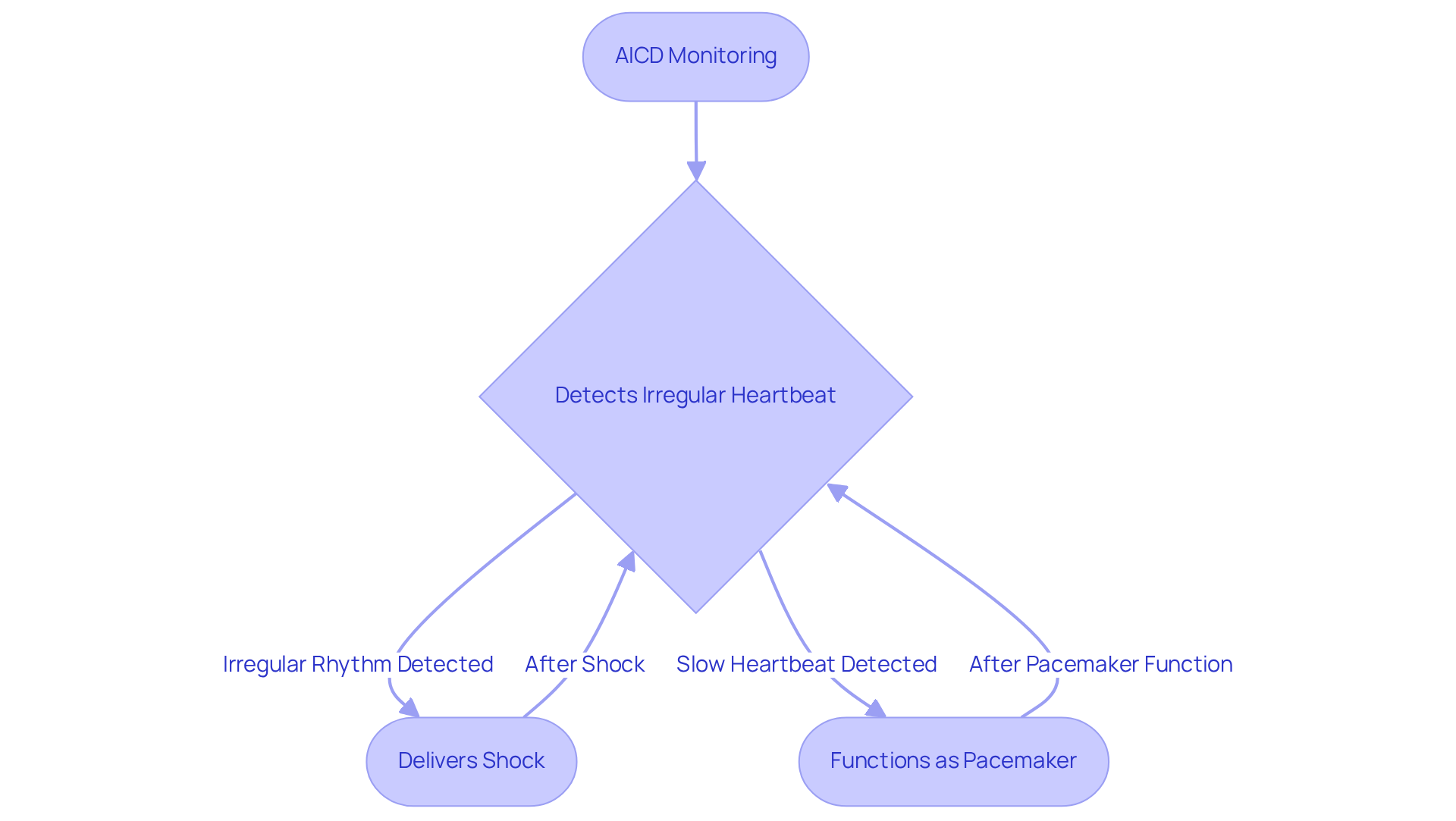
The AICD plays a vital role in cardiology by continuously monitoring heart activity through leads placed in or on the heart. Have you ever worried about a fast or irregular heartbeat? This device is designed to automatically deliver a shock within seconds, restoring a normal rhythm and significantly boosting your chances of survival during a cardiac event. Plus, it can also provide pacing, providing electrical stimulation when your heart beats too slowly. This dual functionality underscores its importance in your treatment plan, offering proactive measures to safeguard your health.
Many patients share how comforting it is to have the device. Just imagine the peace of mind that comes from knowing your condition is being monitored and that help is readily available if needed. Understanding how this device works can help you appreciate its vital role in your ongoing care and recovery.
At Amavita Heart and Vascular Health, we recognize the unique challenges faced by older adults, especially those with diabetes, hypertension, or a family history of heart disease. Our team and thorough evaluations ensure that individuals at high risk receive personalized care, enhancing treatment outcomes and reducing hospital readmissions. By integrating sophisticated diagnostic tools into our care plans, we aim to provide a level of cardiovascular care that truly supports you.
If you have concerns about your heart health, don’t hesitate to reach out. We’re here to help you with compassion and understanding.
Outline AICD Implantation Process: Steps and Recovery
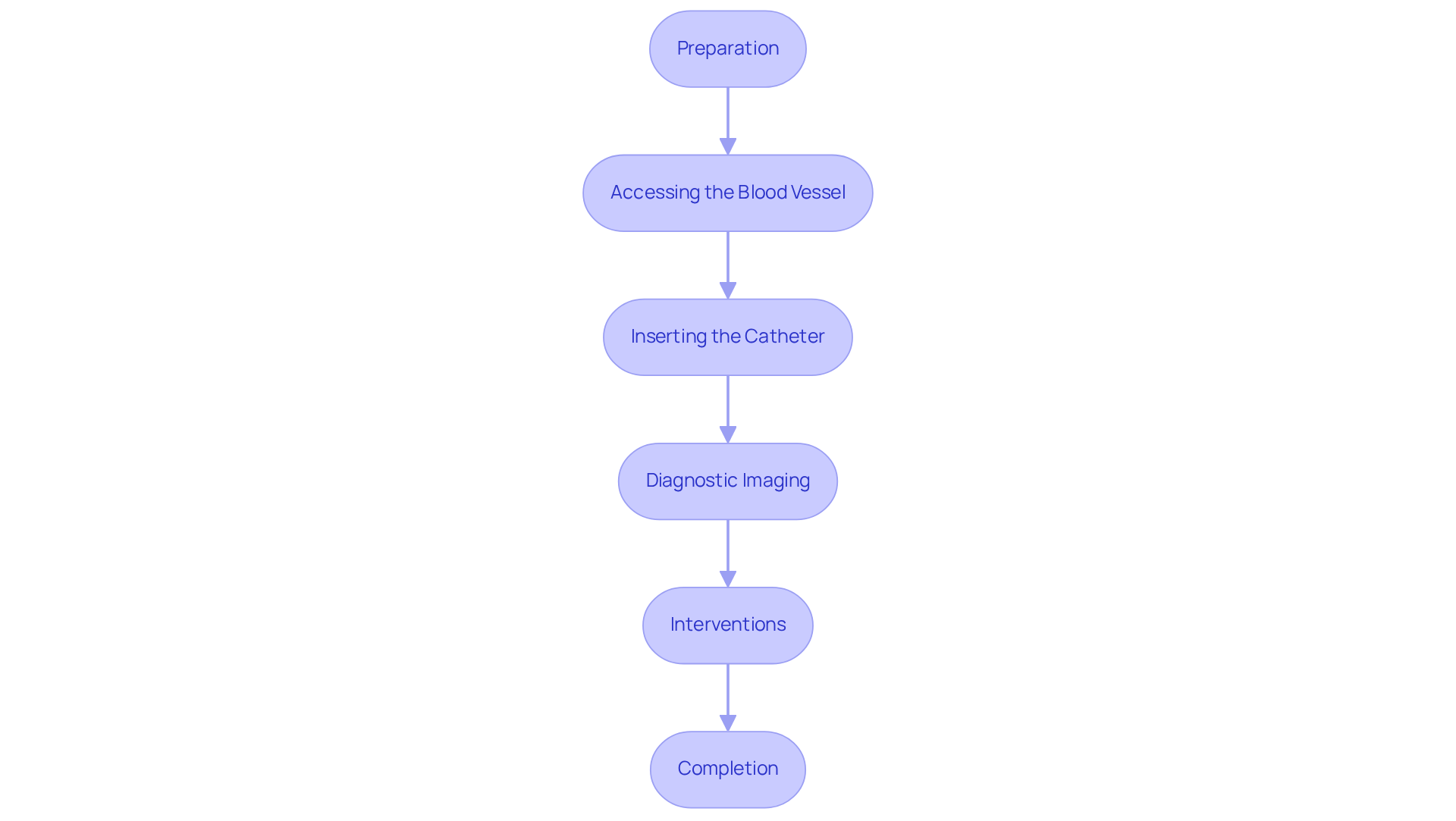
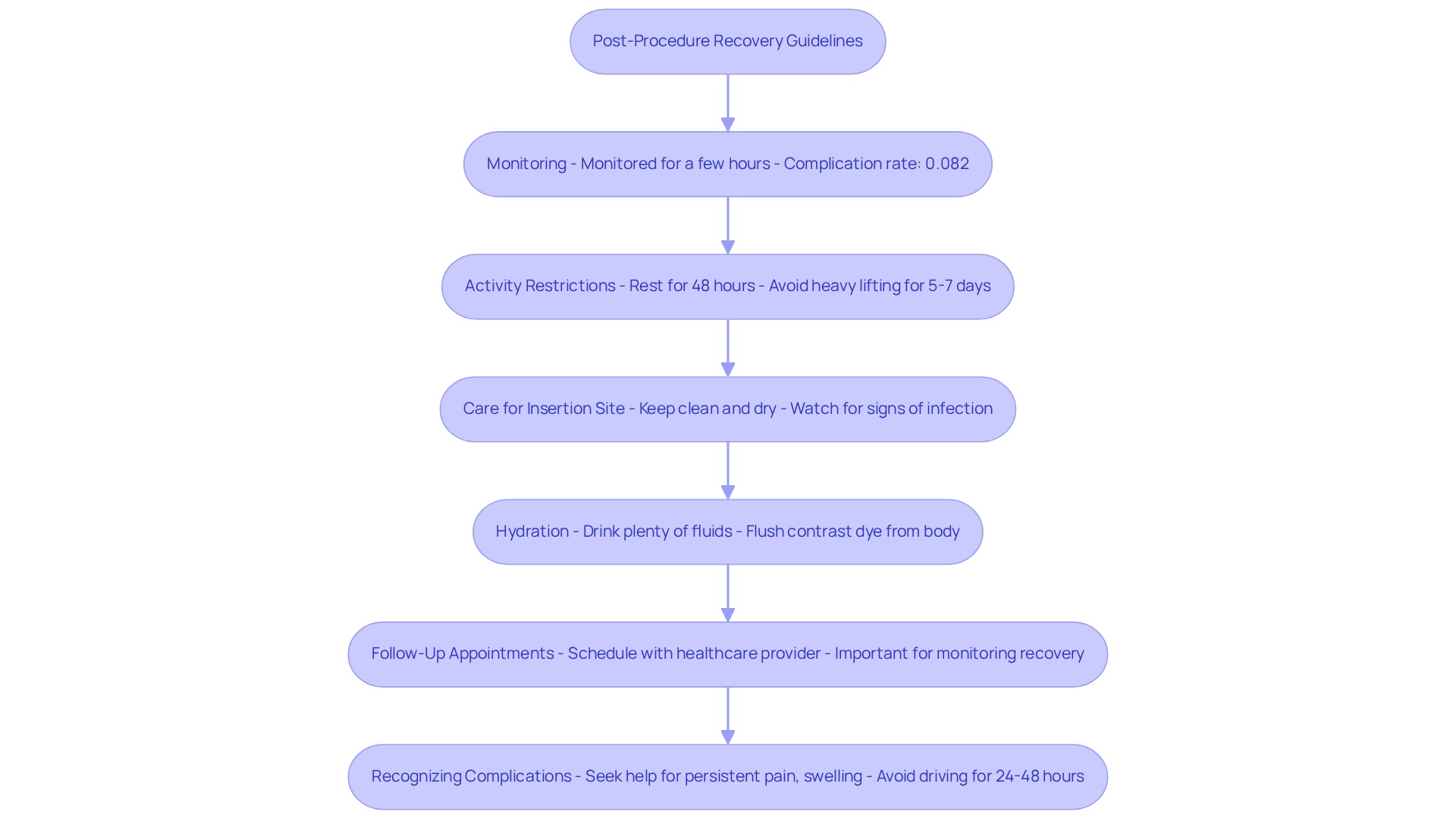
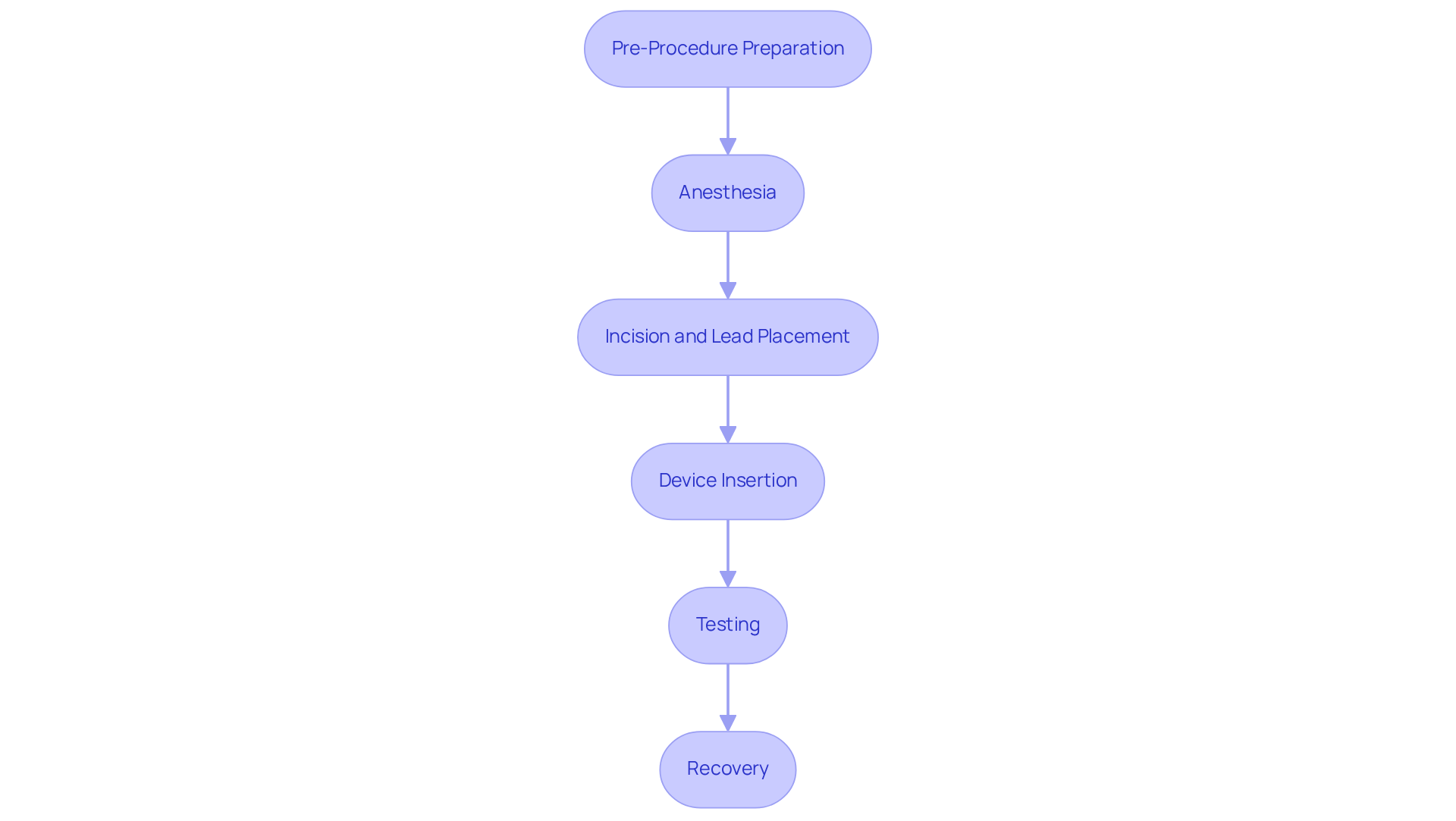
Understanding the implantation of an AICD can help alleviate your worries and prepare you for a journey toward better heart health. Here’s a gentle overview of the key steps involved in the procedure:
- Evaluation: First, a thorough evaluation is conducted. This includes reviewing your medical history and performing a physical examination to ensure you’re a suitable candidate for the procedure.
- Anesthesia: The procedure is performed under local anesthesia, so you can feel comfortable throughout the process.
- Incision and Lead Placement: A small incision is made just below your collarbone, and leads are carefully threaded through a vein to reach your heart.
- Device Insertion: The AICD is positioned beneath your skin, and the leads are connected to the unit, ensuring everything works properly.
- Testing: Before closing the incision, the device is tested to confirm it operates correctly.
- Recovery: Typically, you’ll stay in the hospital for one to two days for monitoring. Full recovery takes time, during which it’s important to avoid heavy lifting and strenuous activities.
Hearing about this procedure can significantly reduce anxiety. Many individuals share positive experiences after AICD cardiology implantation, expressing relief and gratitude for the improved quality of life it provides. One person shared, “I felt it was the best way to give me hope and a prolonged life with my heart problem.” This highlights the importance of making informed decisions and being actively involved in your care.
If you have any questions or concerns, please don’t hesitate to reach out. We’re here to support you every step of the way.
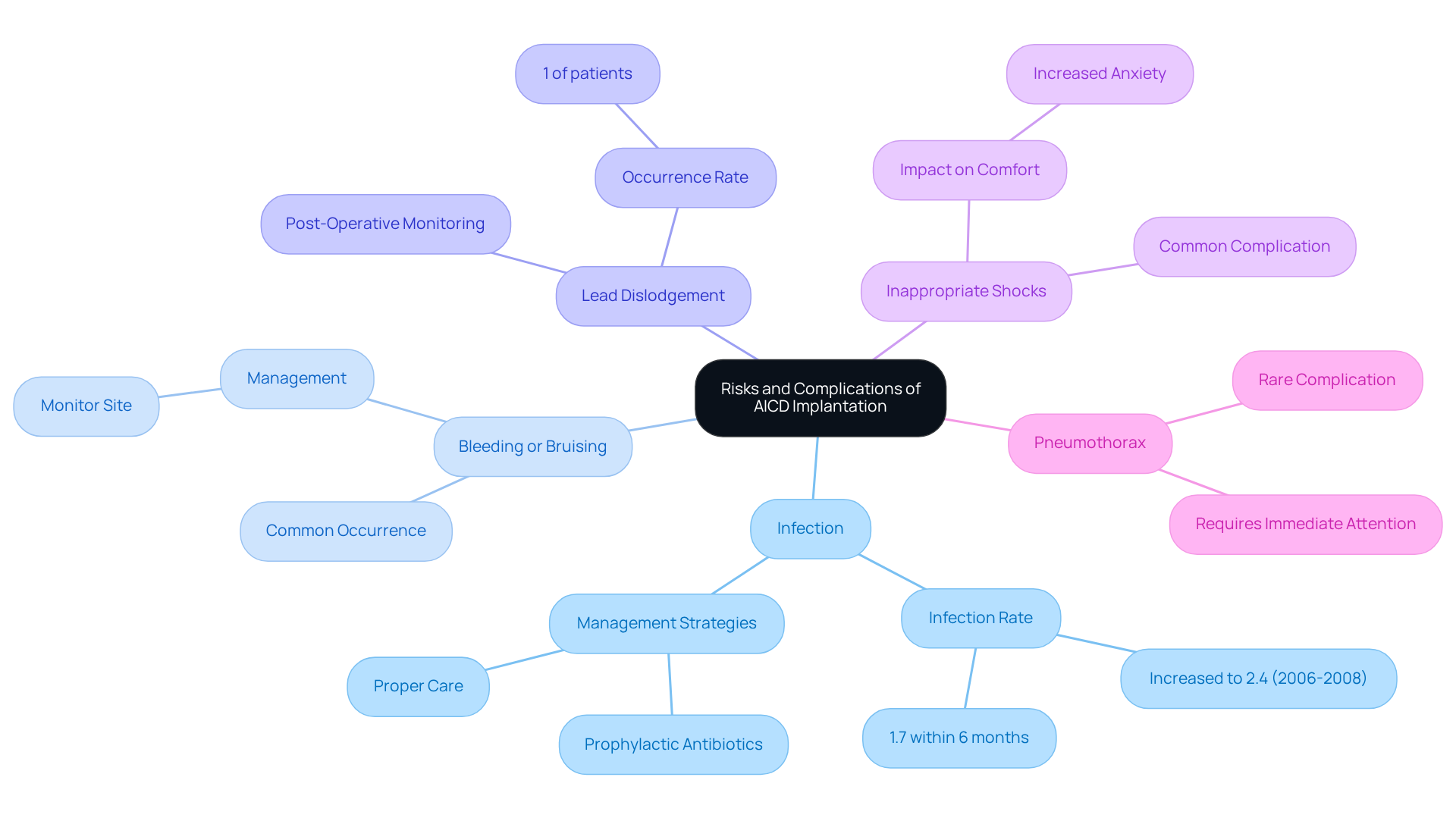
Identify Risks and Complications: What Patients Should Know
While AICD cardiology implantation is generally safe, it’s important for patients to be aware of some risks that may arise.
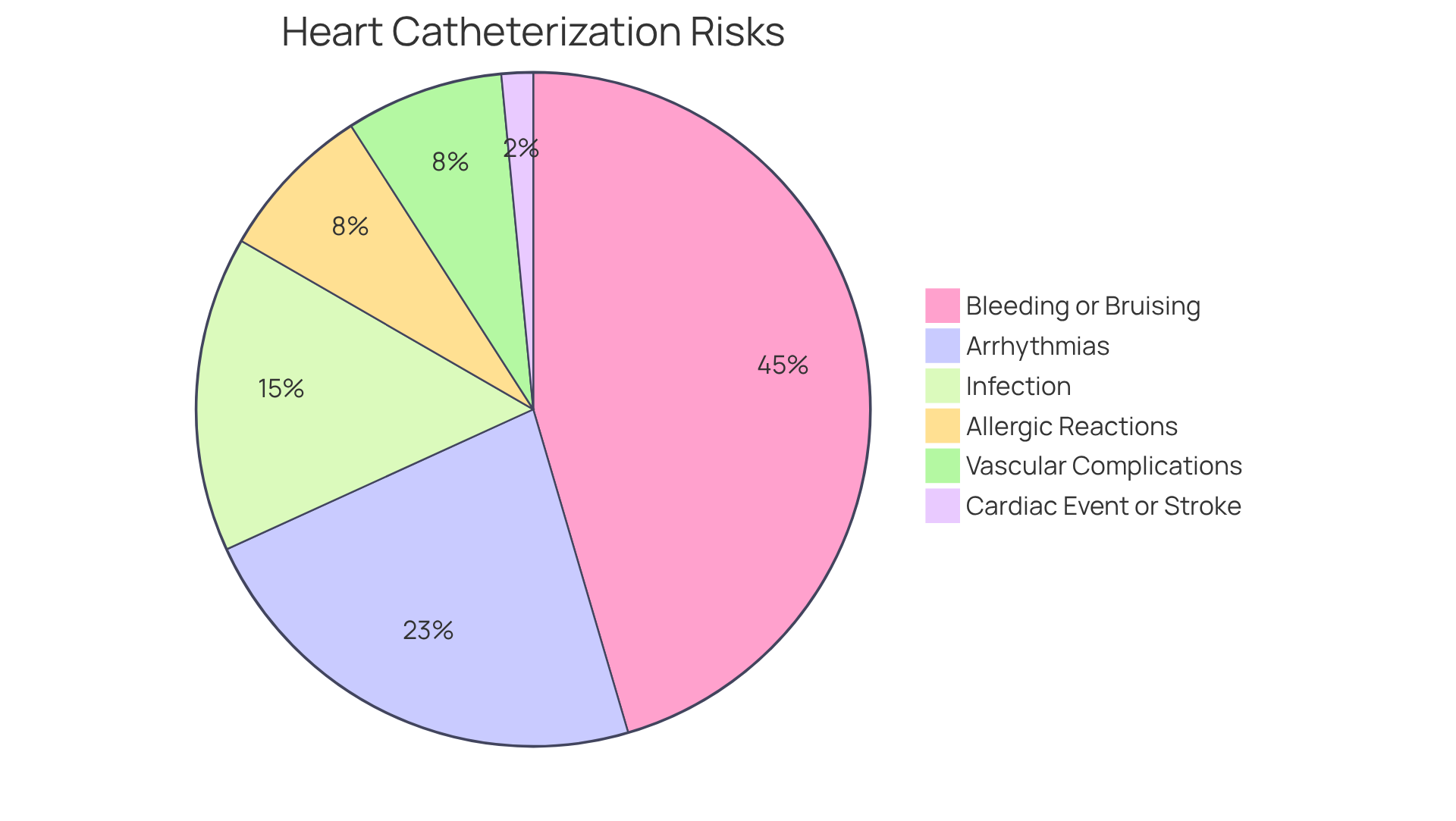
- Infection: One concern is the infection at the incision site. Studies show that the infection rate is about 1%, which has increased to 2.4% from 2006 to 2008. This highlights the need for proper care and the use of prophylactic antibiotics to effectively manage this risk.
- Bleeding or Bruising: Some individuals might notice bleeding or bruising around the implant site. While this is usually manageable, it’s something to keep an eye on.
- Lead Dislodgement: There’s also a chance that the leads may shift from their intended position, which could affect how well the device works. This complication occurs in about 1% of patients, making monitoring essential.
- Inappropriate Shocks: Occasionally, the device may deliver shocks when they aren’t needed, which can be distressing. Reports indicate that this can be uncomfortable, impacting comfort and increasing anxiety levels.
- Pneumothorax: Although rare, the procedure might lead to a pneumothorax, or collapsed lung, due to lead placement. This situation requires immediate medical attention.
Understanding these risks allows individuals to make informed decisions, fostering a proactive approach to their health. As emphasized by Stanford Electrophysiologists, regular monitoring and management of these risks are vital for ensuring patient safety. Remember, you’re not alone in this journey; support is available.
Conclusion
An Automatic Implantable Cardioverter Defibrillator (AICD) is more than just a medical device; it’s a vital lifeline for elderly patients. By significantly reducing the risk of sudden cardiac death, it enhances overall quality of life. For older adults, especially those with heart-related conditions, understanding the role of AICDs in cardiology is crucial. This device not only monitors heart rhythms but also steps in during critical moments, offering peace of mind and empowering patients to engage in daily activities with renewed confidence.
Throughout this article, we’ve shared important insights about how AICDs work, the implantation process, and the potential risks involved. The dual role of AICDs as both defibrillators and pacemakers highlights their importance in managing arrhythmias and ensuring patient safety. From the pre-procedure evaluation to the recovery phase, being informed about each step can help ease anxiety and foster a sense of control over one’s health journey. Additionally, being aware of possible complications, such as infection or inappropriate shocks, allows for proactive discussions with healthcare providers.
Ultimately, embracing knowledge about AICDs can lead to better health outcomes and a more secure future for elderly patients. It’s vital to seek information and support from healthcare professionals to navigate this journey effectively. By doing so, individuals not only enhance their understanding of AICDs but also take an active role in their cardiac care, paving the way for a healthier, more fulfilling life. Remember, you’re not alone in this journey; support is always available.
Frequently Asked Questions
What is an Automatic Implantable Cardioverter Defibrillator (AICD)?
An AICD is a medical device designed to monitor heart rhythms and intervene when necessary to prevent sudden cardiac death (SCD).
Why is the AICD significant in cardiology?
The AICD is significant because it can lower mortality rates by 38% compared to individuals without the device, making it crucial for patients at risk of heart-related issues.
Who can benefit from an AICD?
Older adults facing heart-related issues, such as heart failure or a history of heart attacks, can benefit from an AICD.
How does an AICD improve quality of life?
An AICD enhances quality of life by allowing individuals to engage in daily activities with more confidence and security.
What should someone do if they have concerns about heart health?
If someone has concerns about heart health, they should reach out to a healthcare professional to discuss their options and gain more information about AICDs and their benefits.
List of Sources
- Define AICD: Significance in Cardiology
- ICDs Are Still an Effective Therapy to Prevent Sudden Cardiac Death in Heart Failure: (https://jacc.org/doi/10.1016/j.jchf.2019.08.001)
- parade.com (https://parade.com/1187612/michelle-parkerton/quotes-about-heart-disease)
- A 60-Year-Old Patient Receives an AICD After a Cardiac Arrest Episode – American College of Cardiology (https://acc.org/education-and-meetings/patient-case-quizzes/a-60-year-old-patient-receives-an-aicd-after-a-cardiac-arrest-episode?w_nav=LC)
- Efficacy and safety of implantable cardioverter-defibrillator implantation in the elderly—The I-70 Study: A randomized clinical trial (https://heartrhythmopen.com/article/S2666-5018(24)00105-3/fulltext)
- Elderly Heart Patients With ICD Devices Live Longer After Heart Failure, Study Shows (https://healthmanagement.org/c/healthmanagement/News/elderly-heart-patients-with-icd-devices-live-longer-after-heart-failure-study-shows)
- Explain How AICD Works: Mechanisms and Functionality
- Appropriateness of implantable cardioverter-defibrillator device implants in the United States (https://sciencedirect.com/science/article/abs/pii/S1547527123030011)
- What is Sudden Cardiac Arrest and How Does an Implantable Defibrillator Help? (https://news.bostonscientific.com/what-is-sudden-cardiac-arrest-implantable-cardioverter-defibrillator)
- Implantable cardioverter-defibrillators (ICDs) – Mayo Clinic (https://mayoclinic.org/tests-procedures/implantable-cardioverter-defibrillators/about/pac-20384692)
- Implantable Defibrillator – StatPearls – NCBI Bookshelf (https://ncbi.nlm.nih.gov/books/NBK459196)
- Implantable cardioverter defibrillators (ICD) | Heart Foundation (https://heartfoundation.org.au/your-heart/automated-implantable-cardioverter-defibrillator)
- Outline AICD Implantation Process: Steps and Recovery
- 80% of older adults survive more than two years after ICD implantation (https://cardiovascularbusiness.com/topics/clinical/heart-rhythm/80-older-adults-survive-more-two-years-after-icd-implantation)
- Case Study: Novel gold-plated implantable cardioverter-defibrillator in a young child with complex long QT syndrome – Norton Healthcare Provider (https://nortonhealthcareprovider.com/news/case-study-novel-gold-plated-implantable-cardioverter-defibrillator-in-a-young-child-with-complex-long-qt-syndrome)
- Decision-Making Experiences of Patients with Implantable Cardioverter-Defibrillators – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC5056835)
- Initial Experience With the Extravascular Implantable Cardioverter-Defibrillator: Procedure Workflow and Patient Selection (https://hmpgloballearningnetwork.com/site/eplab/case-study/initial-experience-extravascular-implantable-cardioverter-defibrillator)
- Case Study: Successful AICD Implantation at Vadamalayan Hospital, Dindigul (https://linkedin.com/pulse/case-study-successful-aicd-implantation-c4y7c)
- Identify Risks and Complications: What Patients Should Know
- Estimates of Implantable Cardioverter-Defibrillator Complications | Circulation (https://ahajournals.org/doi/10.1161/CIRCULATIONAHA.108.841452)
- Rate, Time Course, and Predictors of Implantable Cardioverter Defibrillator Infections: An Analysis From the SIMPLE Trial – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC7499364)
- Risks (https://stanfordhealthcare.org/medical-treatments/i/icd/risks.html)
- Rates of and Factors Associated With Infection in 200 909 Medicare Implantable Cardioverter-Defibrillator Implants | Circulation (https://ahajournals.org/doi/10.1161/circulationaha.114.009081)
- Long-Term Complications Related to Cardiac Implantable Electronic Devices | MDPI (https://mdpi.com/2077-0383/14/6/2058)