Introduction
Feeling heart flutters after a meal can be both perplexing and concerning. Many people find themselves wondering what might be causing these sensations. It’s important to know that certain foods, especially those high in sugar, caffeine, or unhealthy fats, can make these fluttering feelings worse, leading to discomfort and anxiety. By understanding which dietary choices might trigger these symptoms, you can take steps toward better heart health.
Have you ever thought that the very foods meant to nourish you could be behind those unsettling palpitations? It’s a common concern, and you’re not alone in feeling this way. In this article, we’ll explore ten specific foods to avoid, empowering you to take control of your cardiovascular well-being. Remember, knowledge is a powerful tool in managing your health, and we’re here to support you every step of the way.
Amavita Heart and Vascular Health: Expert Care for Heart Flutters
At Amavita Heart and Vascular Health, we understand that heart health can be concerning. Guided by the expertise of Harvard-trained Dr. Pedro Martinez-Clark, our team is dedicated to providing comprehensive cardiovascular care tailored to your needs. We utilize advanced technologies that not only enhance the accuracy of our assessments but also help us manage your symptoms more effectively.
In addition to this, we prioritize your comfort through personalized care, significantly reducing anxiety. We believe that your journey towards better health should be as smooth and supportive as possible. Our commitment to excellence ensures that every patient, regardless of background, receives the highest quality of care. We strive to create an environment where you feel acknowledged and supported every step of the way.
Have you been feeling anxious about your heart health? You’re not alone, and we’re here to help. Our compassionate approach means that we listen to your concerns and work with you to find the best solutions. Together, we can navigate your path to improved well-being, ensuring you feel valued and cared for. If you’re ready to take the next step, reach out to us today. Your health is our priority, and we’re here to support you.
Understanding Heart Flutters: What They Are and Why They Happen
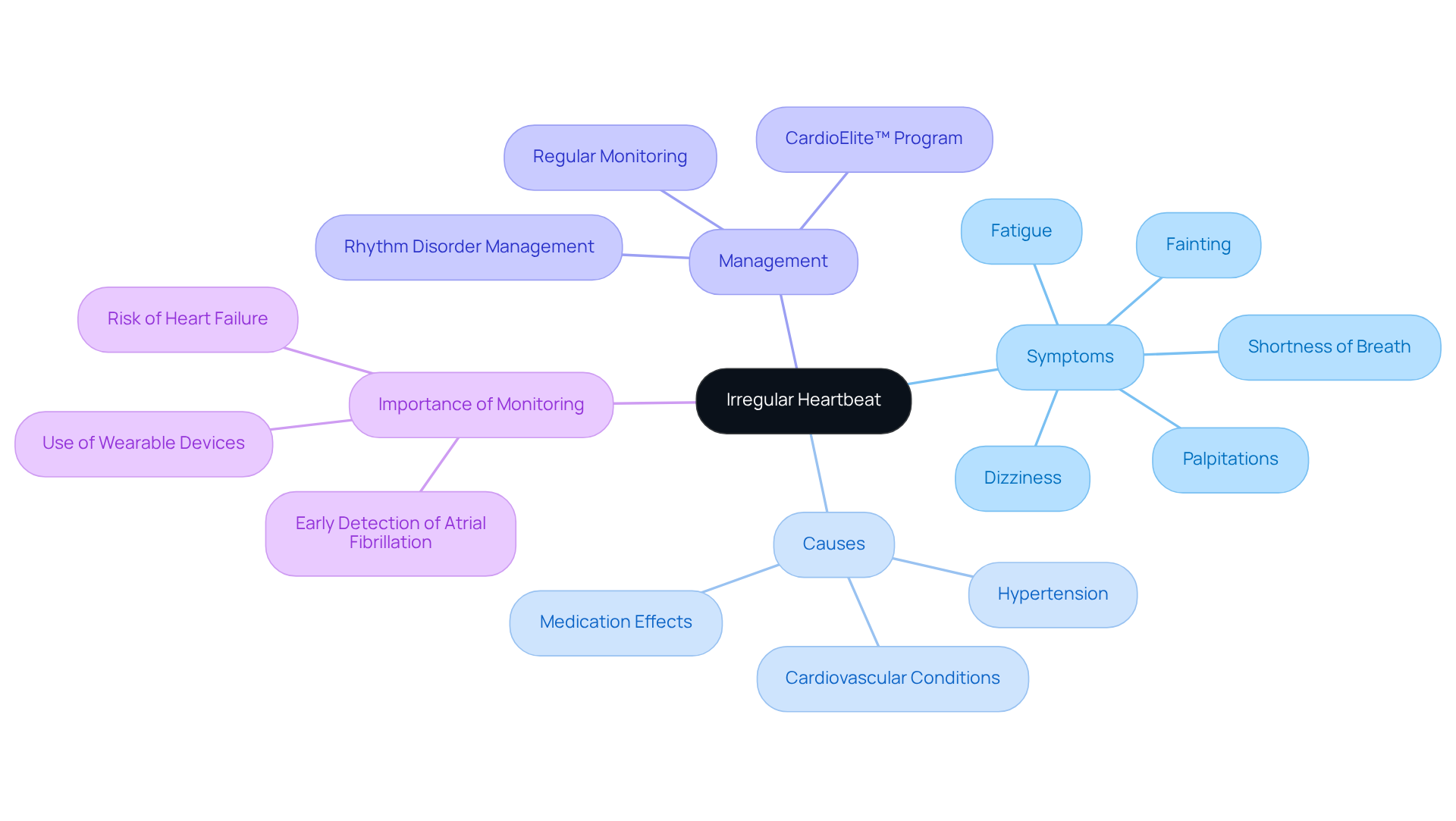
Feeling fluttering sensations or heart palpitations can be concerning. It’s not uncommon to experience moments where your heart seems to race, pound, or skip a beat. These sensations, including irregular heartbeats, can be triggered by various factors such as stress and anxiety. After a meal, your body works hard to digest, which can lead to a heightened awareness of your heartbeat, often resulting in sensations that are more noticeable.
Certain foods can worsen the experience of heart flutters. For instance, dishes high in sugar, sodium, and unhealthy fats can exacerbate the issue. Spicy foods, particularly those containing capsaicin, might activate your nervous system, leading to an increased heart rate. Additionally, caffeine found in coffee and chocolate can trigger palpitations, especially in those who are sensitive to it.
It’s important to pay attention to your diet. Cardiologists often emphasize the benefits of magnesium, potassium, and omega-3 fatty acids, as they can support heart health and potentially reduce irregular heartbeats. Alongside dietary choices, managing stress is crucial. Have you considered mindfulness techniques? They can be incredibly helpful in calming your mind and body.
While many heart flutters are harmless, they can sometimes indicate a more serious issue, especially if accompanied by symptoms like dizziness or chest pain. Understanding these mechanisms is vital for effectively managing your health. Remember, you’re not alone in this journey. If you have concerns, don’t hesitate to reach out for support. Your well-being is important, and there are resources available to help you navigate these feelings.
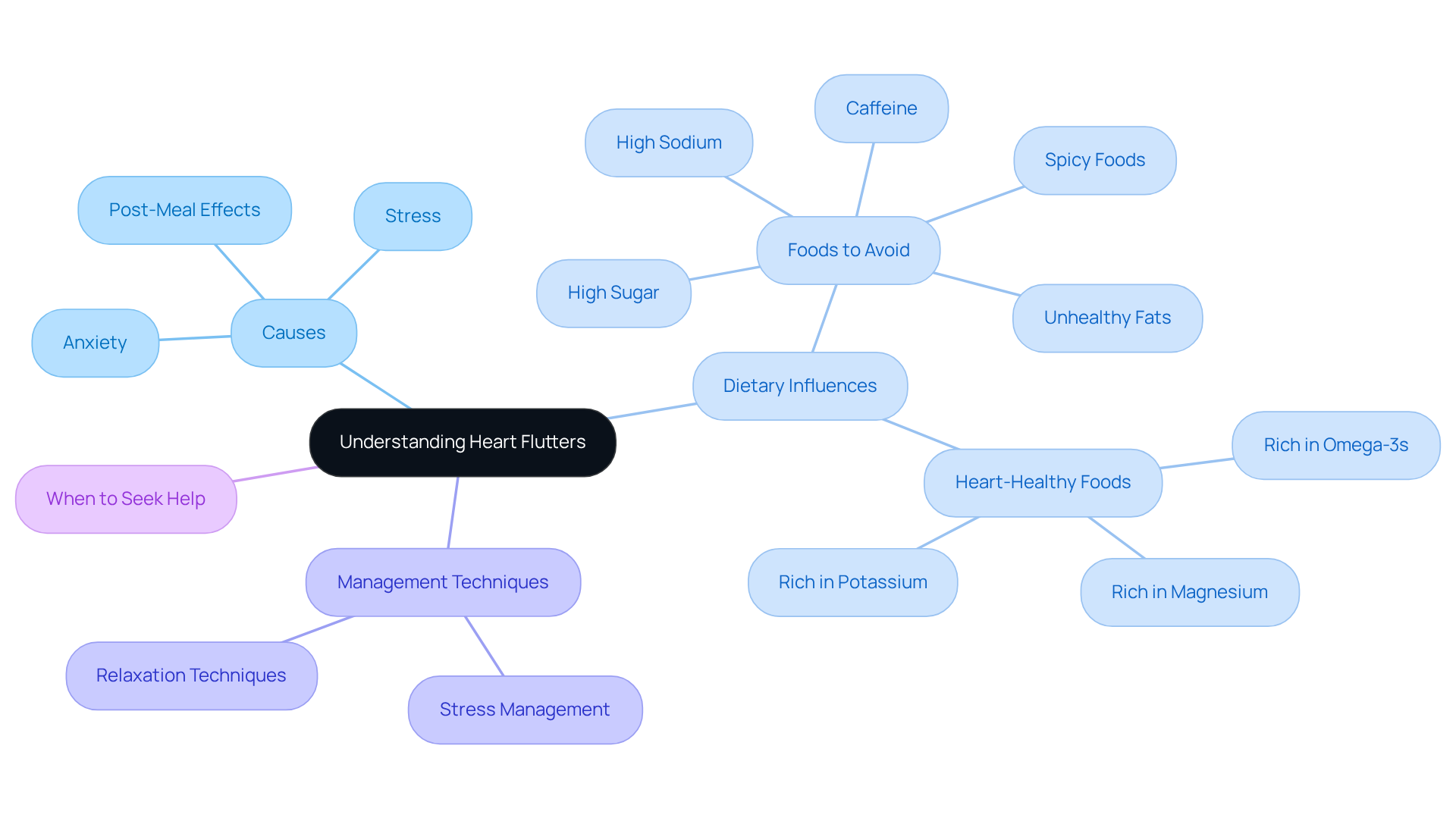
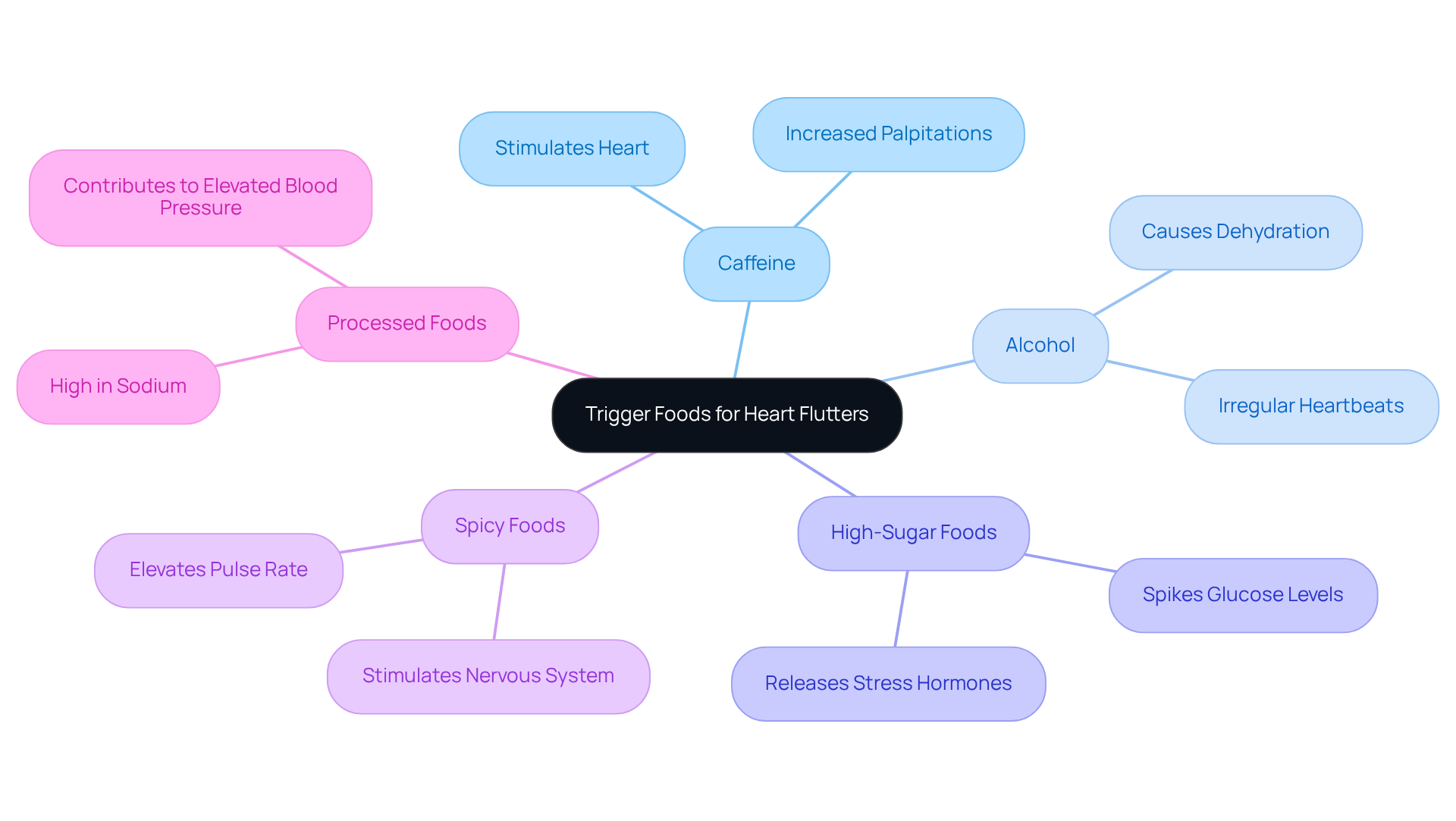
Identifying Trigger Foods: Common Culprits Behind Heart Flutters
Certain foods can trigger heart flutters, and understanding these can help you manage your symptoms more effectively. Let’s explore some common culprits:
- Caffeine: Found in coffee, tea, and energy drinks, caffeine can lead to increased palpitations. While enjoying one or two cups of coffee is generally safe, too much caffeine might provoke fluttering sensations, especially if you’re sensitive to it. Have you noticed how your heart feels after that third cup?
- Alcohol: Excessive drinking can lead to dehydration and electrolyte imbalances, which may worsen fluttering sensations. For women, moderate intake is about one drink per day, while men can have up to two. However, higher consumption, especially during festive occasions, is linked to heart rhythm disturbances. It’s important to be mindful of how alcohol affects you.
- Sugary Foods: Sugary foods can cause rapid spikes and drops in your glucose levels, potentially triggering palpitations. This fluctuation can lead to the release of stress hormones, raising your pulse rate. To maintain stable sugar levels, consider limiting sugary snacks and beverages. How do you feel when you consume sweets?
- Spicy Foods: These can elevate your pulse rate and cause discomfort for some due to capsaicin, which stimulates the nervous system and may lead to adrenaline release. If you notice discomfort after spicy meals, it might be worth cutting back.
- Processed Foods: Often high in sodium and unhealthy fats, these foods can contribute to heart palpitations and rhythm issues, increasing the likelihood of palpitations. Reducing processed snacks can be beneficial for your heart health. Additionally, foods high in tyramine, like aged cheeses and soy sauce, should be avoided as they can trigger spikes in blood pressure.
By being aware of these triggers, you can take steps to protect your heart. Remember, it’s okay to seek help and guidance if you’re feeling uncertain about your health. You’re not alone in managing your heart health.
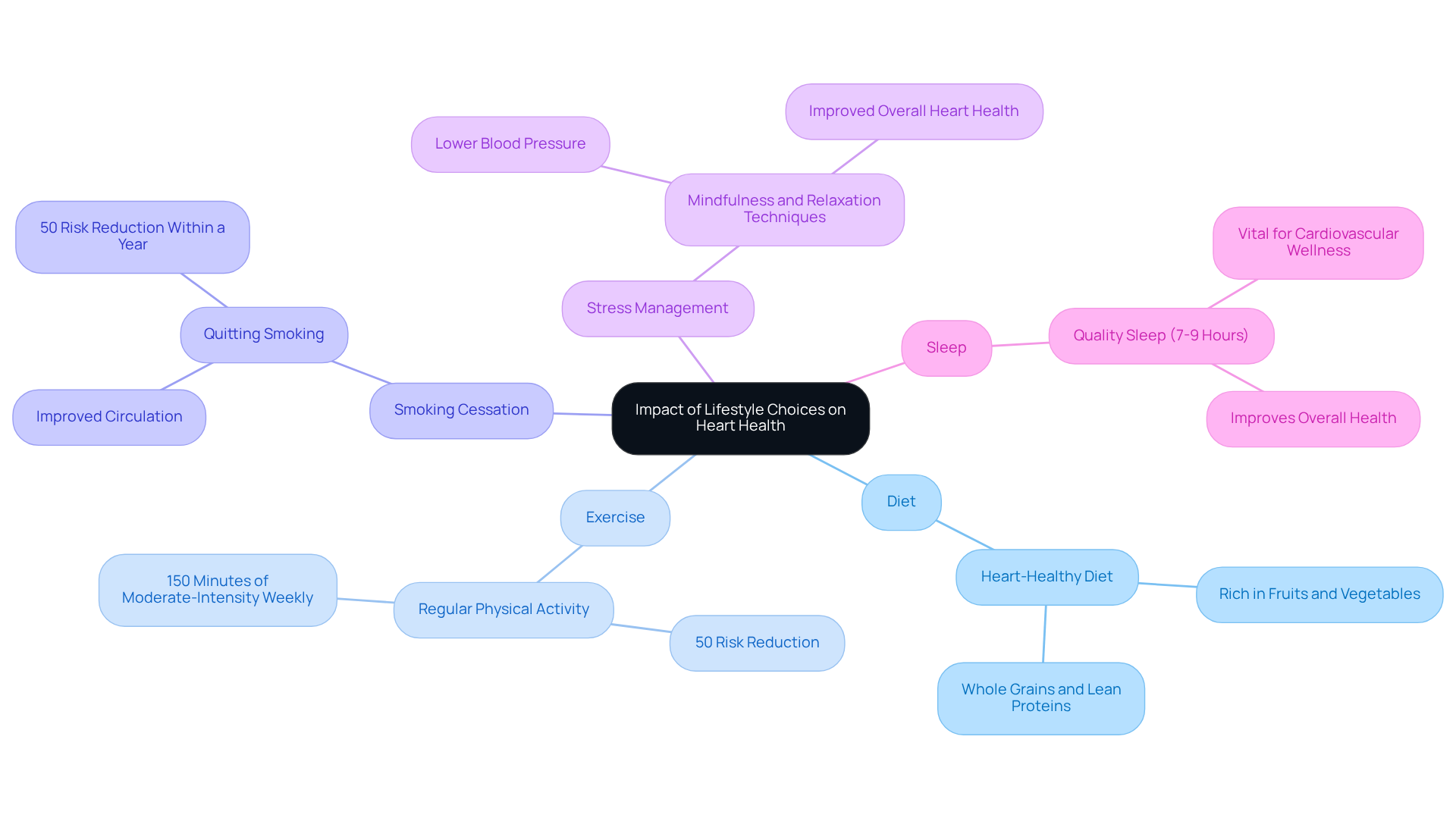
Lifestyle Factors: How Daily Habits Influence Heart Flutters
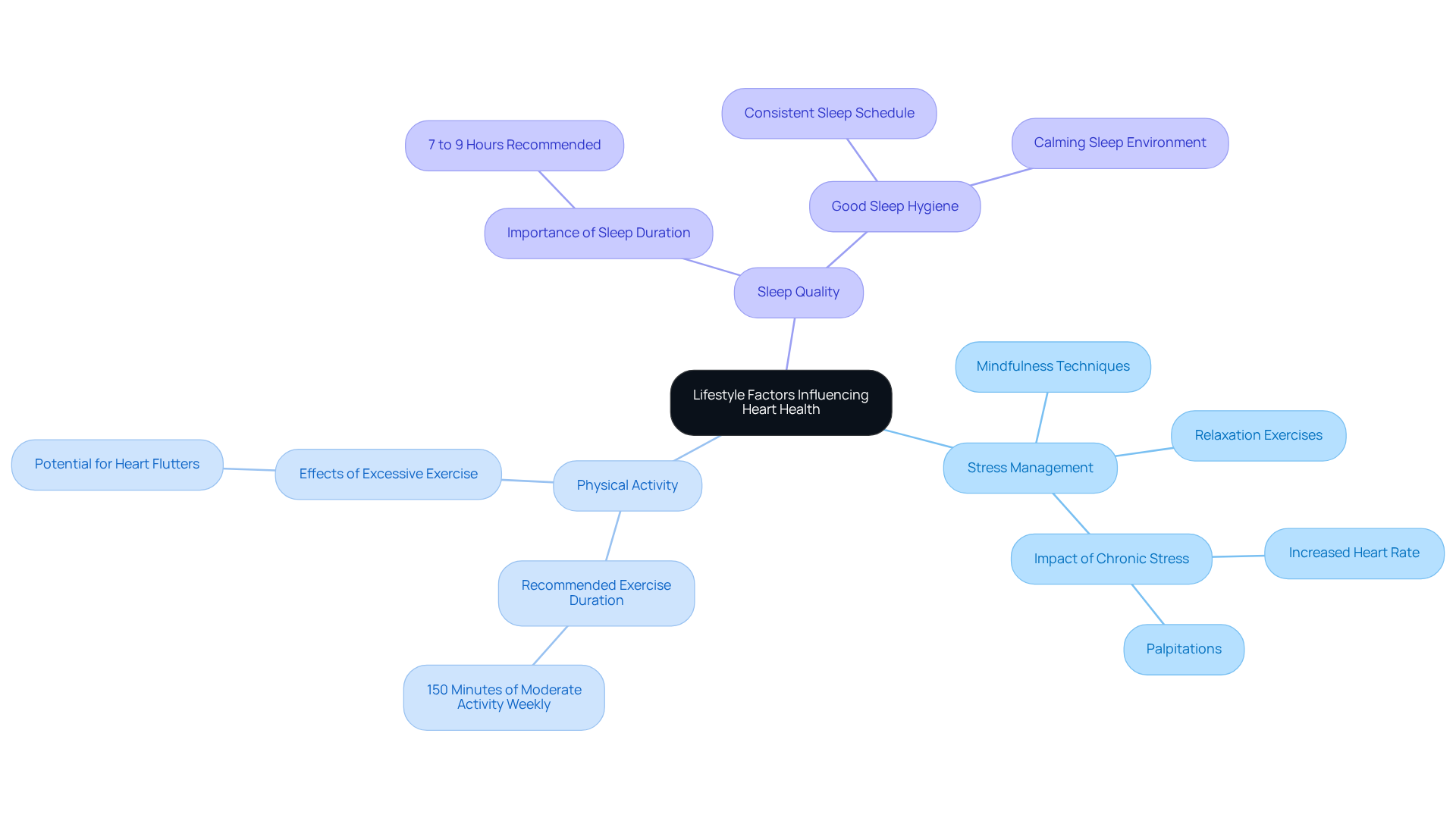
Lifestyle factors play a crucial role in your heart health and can lead to symptoms like heart flutters. Let’s explore some key elements together:
- Stress Management: Have you noticed how stress affects your body? Elevated stress levels can increase your heart rate and lead to palpitations. Research shows that stress can exacerbate heart conditions, especially in older adults. Techniques like mindfulness, deep breathing, and relaxation exercises can effectively reduce stress and improve your heart health. Remember, stress management is vital, as chronic stress can have harmful effects on your cardiovascular system.
- Physical Activity: Engaging in regular exercise and physical activity can help regulate your heart rhythms. The American Heart Association suggests aiming for at least 150 minutes of moderate aerobic activity each week. However, it’s important to be mindful—excessive or intense exercise can sometimes lead to heart issues, particularly if you have underlying cardiovascular issues. Finding a balanced approach to physical activity is essential for maintaining your heart health.
- Sleep Quality: Are you getting enough restful sleep? Poor sleep can exacerbate stress and lead to heart problems. A 2022 study found that insufficient sleep is linked to increased risk of heart disease. Additionally, insufficient sleep is linked to weight gain, high blood pressure, and irregular heartbeat. Prioritizing good sleep hygiene—like keeping a consistent sleep schedule and creating a calming environment—is vital for your overall health.
Taking small steps towards better stress management, staying active, and ensuring quality sleep can make a significant difference in your heart health. Remember, you’re not alone in this journey—support is always available, and it’s okay to reach out for help.
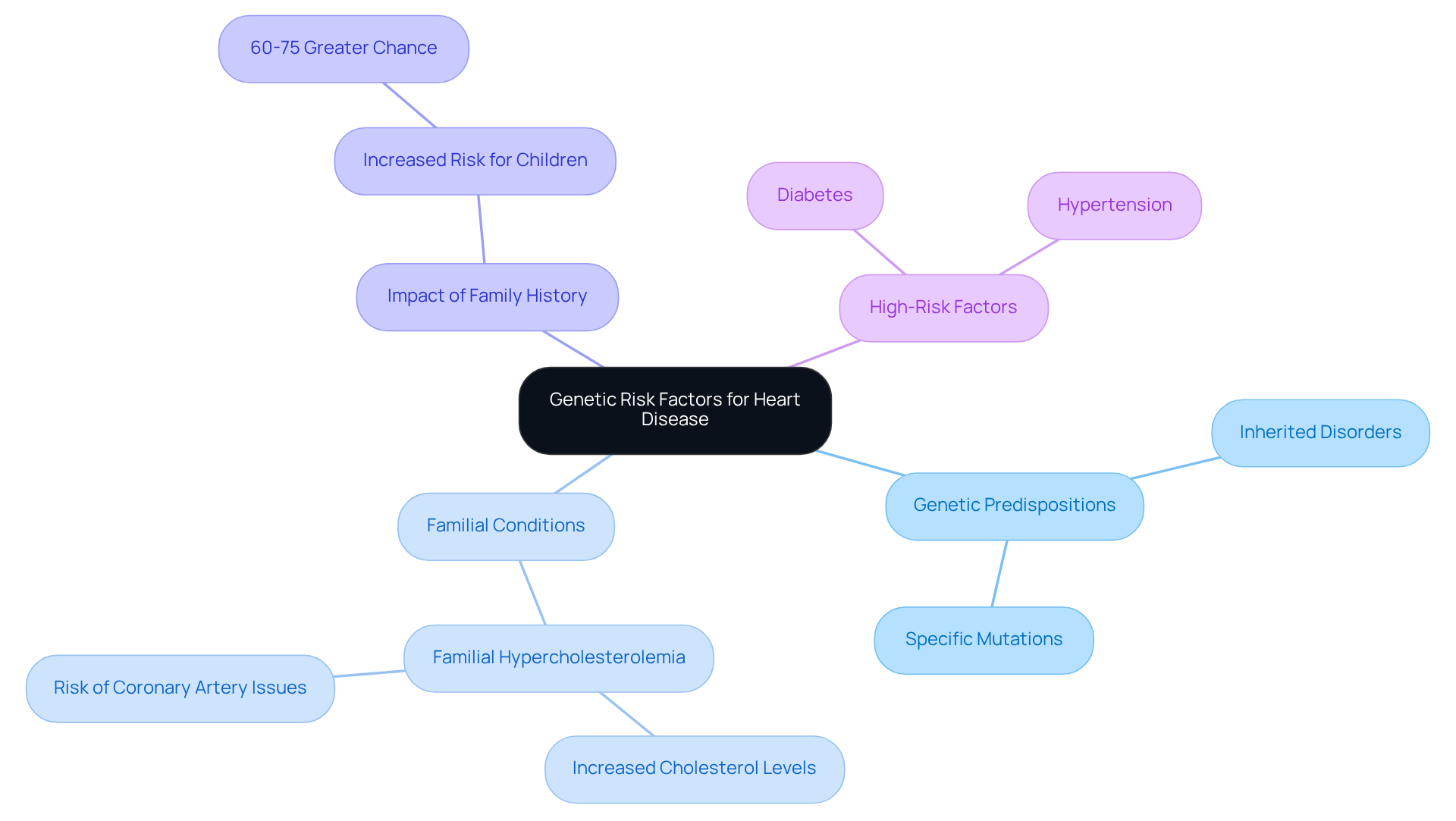
High-Sugar Foods: Their Impact on Heart Flutters
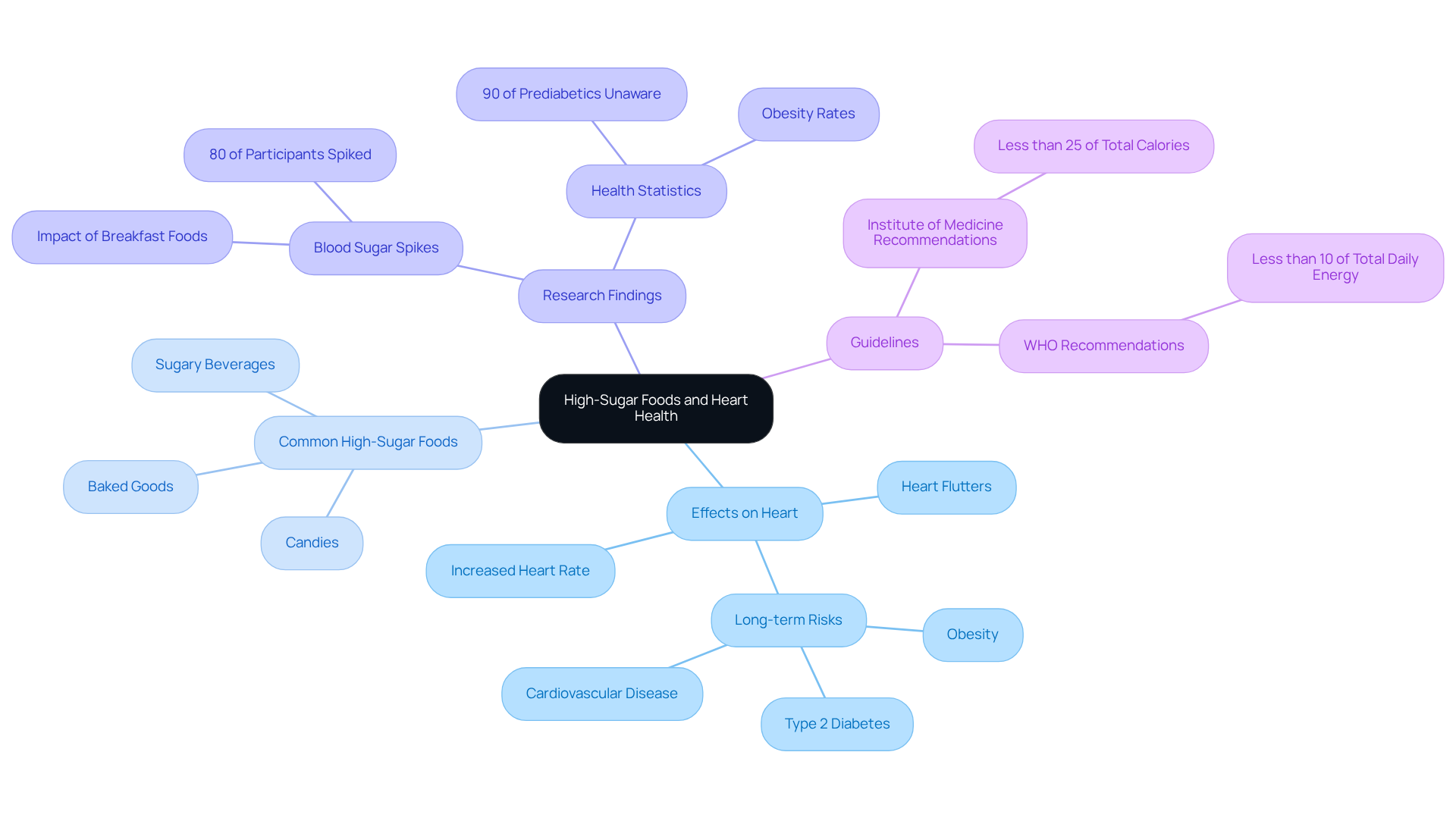
High-sugar foods can cause heart flutters due to rapid fluctuations in sugar levels. When we consume sugar, it triggers an immediate spike in blood sugar, followed by a drop that can create feelings of anxiety and stress, as well as an increased heart rate. This is particularly concerning since nearly 90% of prediabetic individuals are unaware of their condition, potentially leading to serious health issues. It’s crucial to keep track of sugar intake, as diets high in sugar can lead to obesity and type 2 diabetes, both of which heighten the risk of heart disease.
Common trigger foods include:
- Candies and Sweets: They provide a quick burst of energy but can cause significant crashes, leading to jitteriness and palpitations. Beverages like soft drinks and energy drinks are often loaded with sugar, raising blood sugar levels and contributing to dehydration, which can cause heart flutters and worsen anxiety.
- Baked Goods: Pastries and cakes are not only high in sugar but also often contain unhealthy fats, negatively impacting heart health.
Research indicates that excessive sugar intake is linked to various cardiovascular issues, including hypertension, rapid pulse, and arrhythmias. A study found that 80% of participants experienced notable blood sugar increases after eating a bowl of cornflakes and milk, which can cause heart flutters and highlights how even typical breakfast foods can adversely affect heart health. The Institute of Medicine advises that added sugars should comprise less than 25% of total calories, serving as a guideline for safe sugar consumption. Understanding these connections is vital for maintaining heart health and preventing irregular beats.
It’s important for individuals to monitor their diets and consult with healthcare providers to ensure they are making heart-healthy choices. Remember, taking small steps towards a healthier diet can make a significant difference in your overall well-being.
Food Additives: Hidden Triggers for Heart Flutters
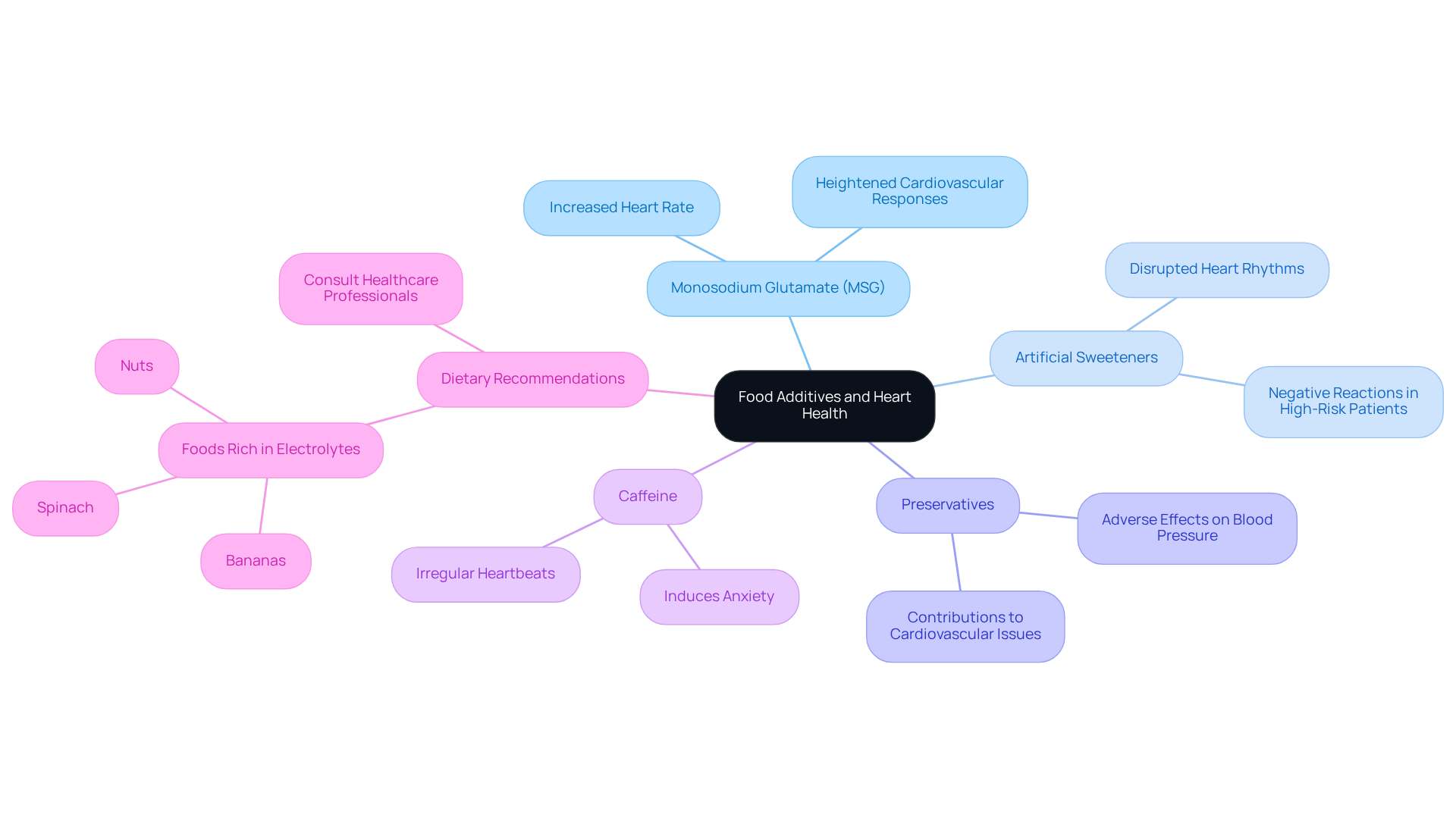
Some food additives can cause palpitations in sensitive individuals, often without them even realizing it. It’s important to be aware of these additives, especially if you’ve experienced heart flutters. Here are some common culprits:
- Monosodium Glutamate (MSG): Often found in processed foods, MSG has been linked to heart palpitations in some people. Recent studies suggest that consuming MSG can lead to heightened sensitivity, particularly for those with existing sensitivities, like patients with diabetes or hypertension.
- Artificial sweeteners: Substitutes such as aspartame and sucralose are frequently used in diet products, but they may lead to negative reactions, including palpitations. Research indicates that these sweeteners can disrupt normal heart rhythms, raising concerns about their long-term health effects, especially for high-risk patients.
- Preservatives: Sodium nitrite and other preservatives commonly found in processed meats can trigger heart flutters. Studies have shown that these additives may contribute to cardiovascular issues, particularly when consumed in large amounts.
- Caffeine: While caffeine isn’t harmful at typical levels, it can induce anxiety and restlessness, potentially causing heart palpitations.
Understanding these additives is essential for managing your heart health. Foods like bananas, spinach, and nuts can help maintain a steady rhythm in your body. At our clinic, we utilize advanced imaging techniques to assess how your dietary choices impact your heart health.
If you’re feeling concerned about your heart health, consulting with healthcare professionals about your dietary choices can help mitigate these risks. It’s crucial to ensure that high-risk patients receive personalized care tailored to their needs. Remember, heart disease remains the leading cause of death in the U.S., but you don’t have to face it alone. We’re here to help.
Dietary Strategies: Managing Heart Flutters Through Food Choices
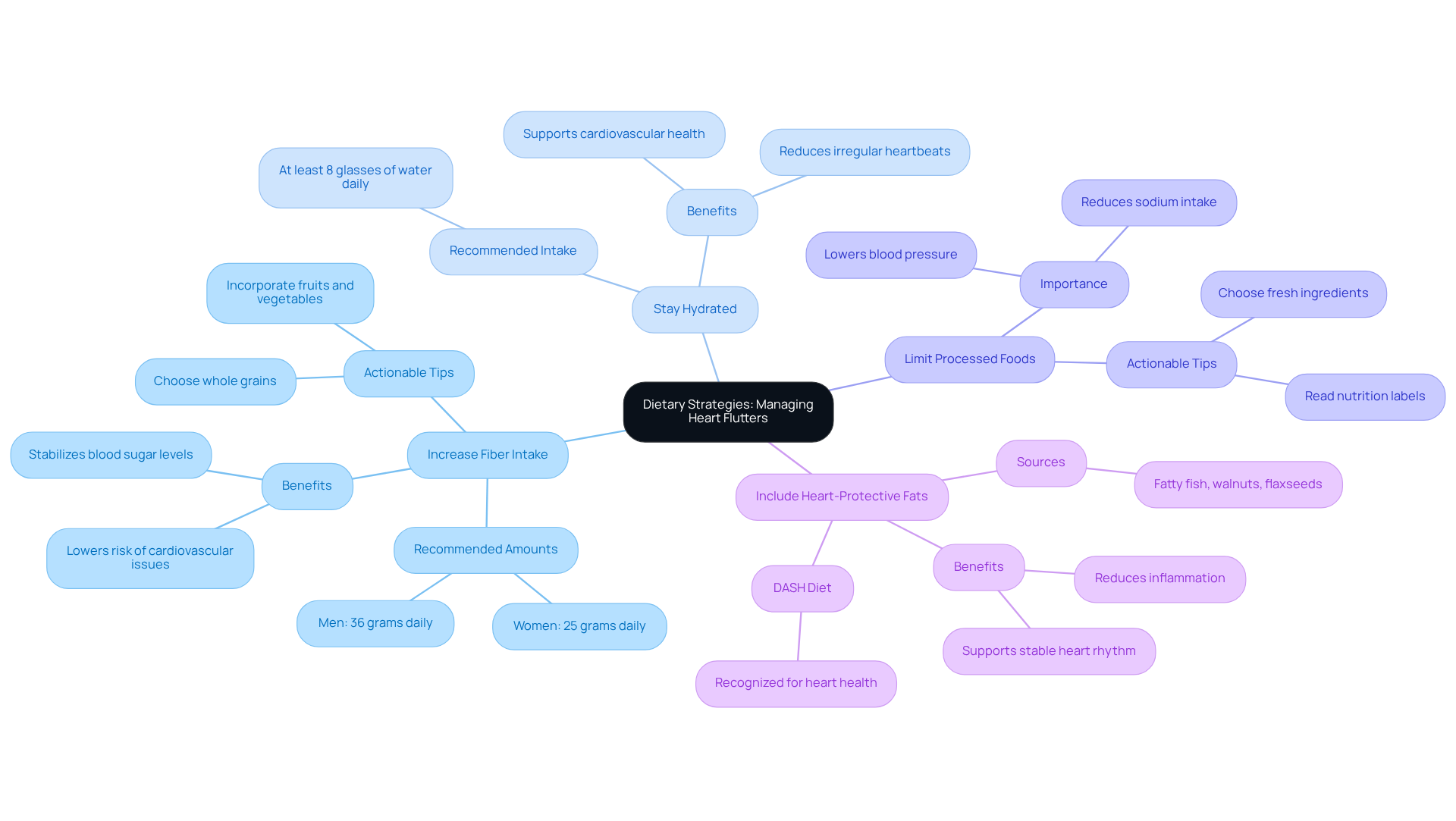
To effectively manage heart flutters, consider these caring dietary strategies:
- Eating foods rich in fiber, like fruits, vegetables, and whole grains, is vital for stabilizing blood sugar levels. Research indicates that increasing fiber can reduce high blood pressure and stroke by up to 20%. For women, aim for about 25 grams daily, while men should target around 36 grams. Remember, small changes can make a big difference in your overall health.
- Keeping hydrated is essential for your heart health. Aim for at least eight glasses of water each day. Proper hydration not only supports overall wellness but can also help reduce irregular heartbeats that might lead to complications after eating. As a nutrition expert wisely notes, “Hydration is essential for preserving cardiovascular wellness and avoiding irregular beats.”
Reducing sodium intake is crucial for lowering blood pressure and reducing the risk of heart flutters after eating, as it helps cut back on high-sodium options. Many adults in the U.S. consume more sodium than recommended, which can worsen heart issues. Making mindful choices can lead to a healthier heart.
- Incorporating foods high in omega-3 fatty acids, such as fatty fish, walnuts, and flaxseeds, can greatly benefit your heart. These healthy fats help reduce inflammation and support overall cardiovascular function, contributing to a more stable heart rhythm. A recent study recognized as one of the best for heart health emphasizes the importance of these dietary choices.
Taking these steps can feel overwhelming, but remember, you’re not alone. Each small change you make can lead to a healthier heart and a more vibrant life. If you have concerns, don’t hesitate to reach out for support.
Deep Breathing and Mindfulness: Techniques to Calm Heart Flutters
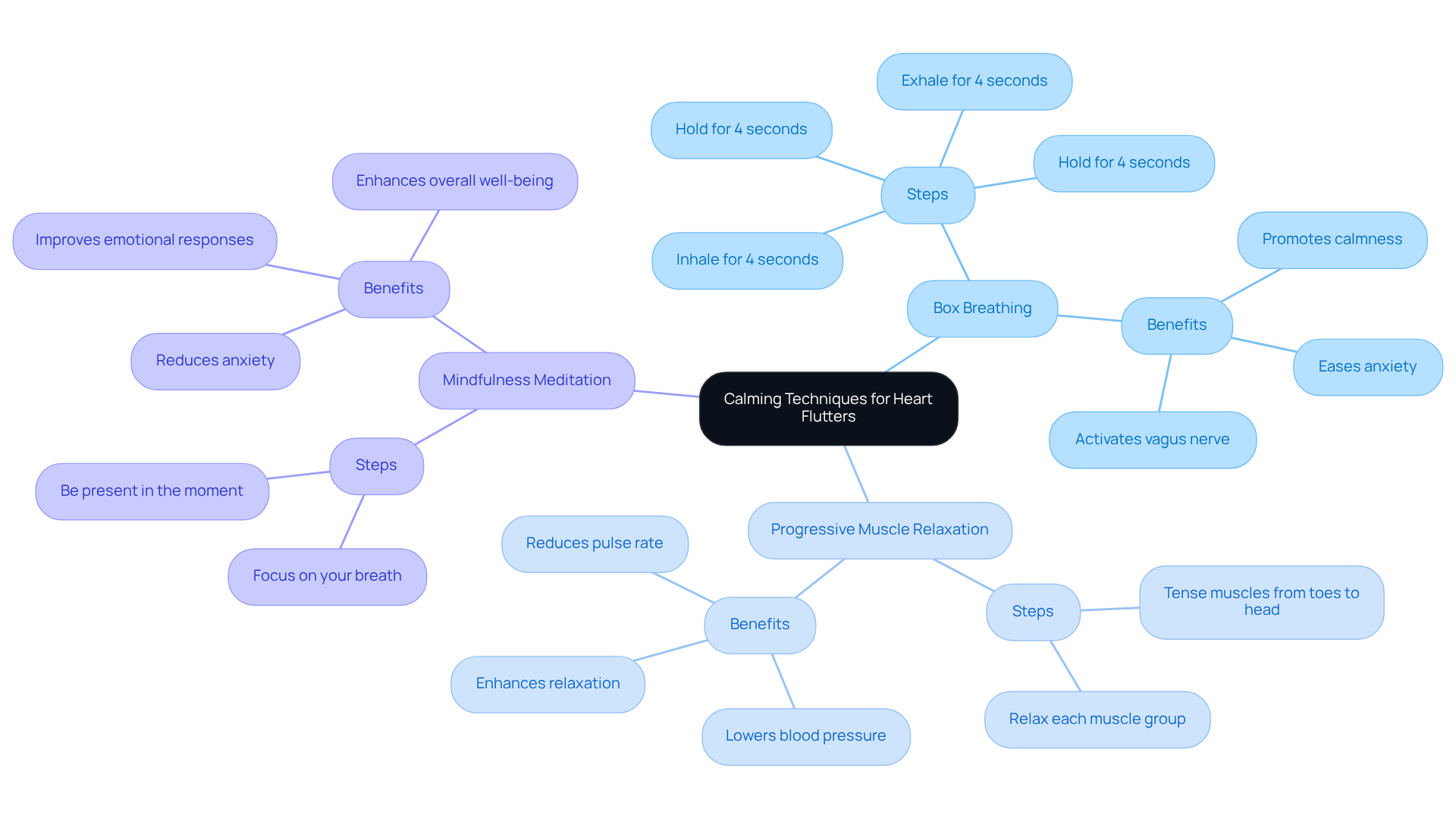
If you’re feeling those unsettling palpitations, know that breathing and mindfulness techniques can truly help. Here are some gentle methods you might find effective:
- Deep breathing: Try inhaling for four seconds, holding for four seconds, exhaling for four seconds, and holding again for four seconds. This simple practice activates the vagus nerve, promoting a sense of calm and easing anxiety, which can help in managing those palpitations.
- Progressive muscle relaxation: Start from your toes and work your way up to your head, tensing and then relaxing each muscle group. This technique has been shown to lower blood pressure and pulse rate, leading to a more relaxed state.
- Mindfulness meditation: Just a few minutes spent focusing on your breath and being present can make a difference. Research indicates that regular practice can reduce common triggers for palpitations. Dr. Rancourt reminds us that mindfulness is about allowing things to be as they are, which can help you manage your emotional responses.
Recent studies have shown that these techniques can be quite effective. Participants often report feeling better emotionally and experiencing fewer palpitations when they incorporate mindfulness and breathing exercises into their daily routines. For example, those who took part in an eight-week mindfulness program noted lower blood pressure and reduced anxiety levels.
Consider setting aside just a few minutes each day to practice these techniques. As you grow more comfortable, you can gradually increase the time you spend on them. Remember, taking these small steps can enhance your overall mental and emotional well-being. You’re not alone in this journey; these practices can make a world of difference.
When to Seek Medical Advice: Recognizing Serious Symptoms
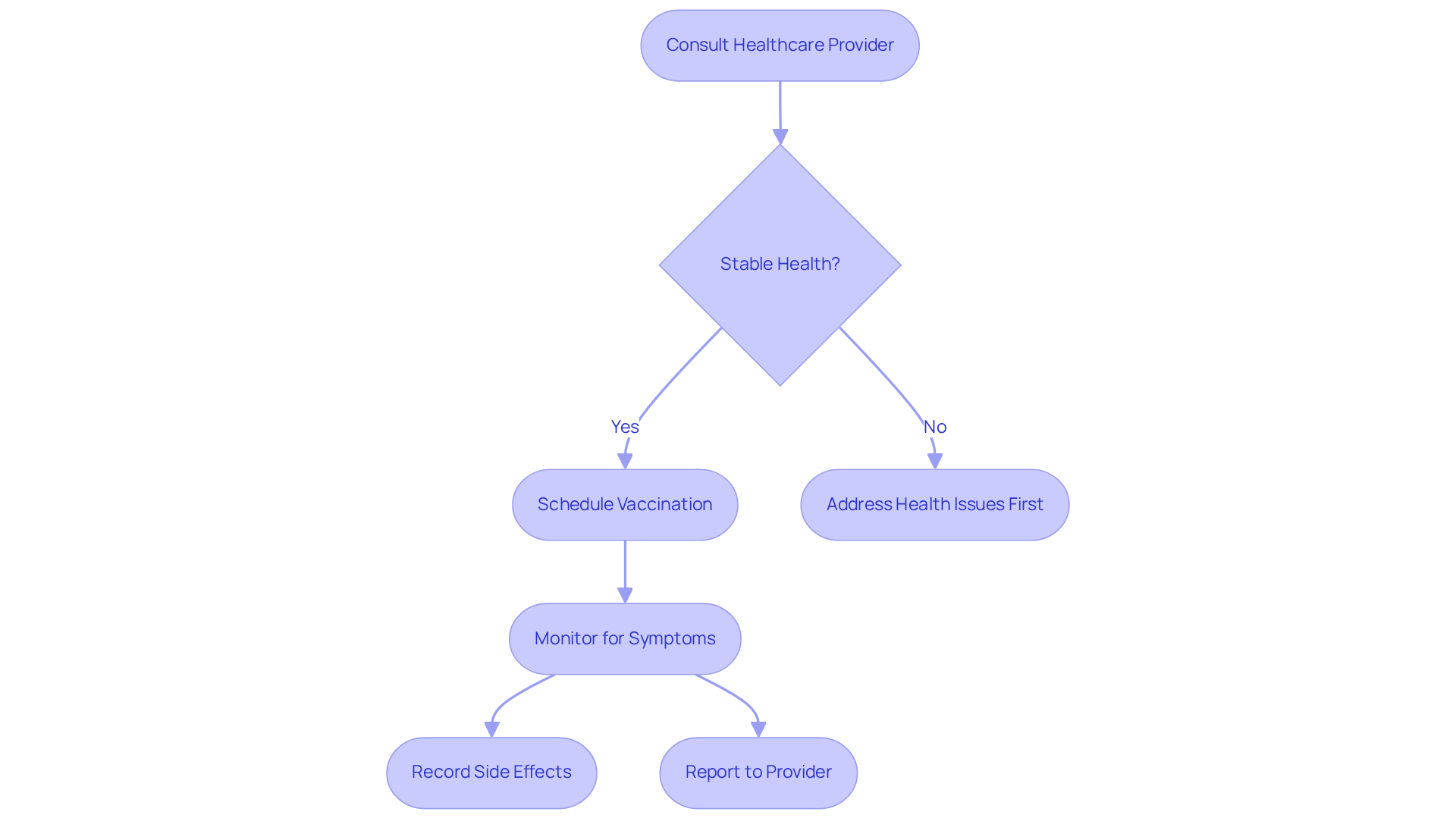
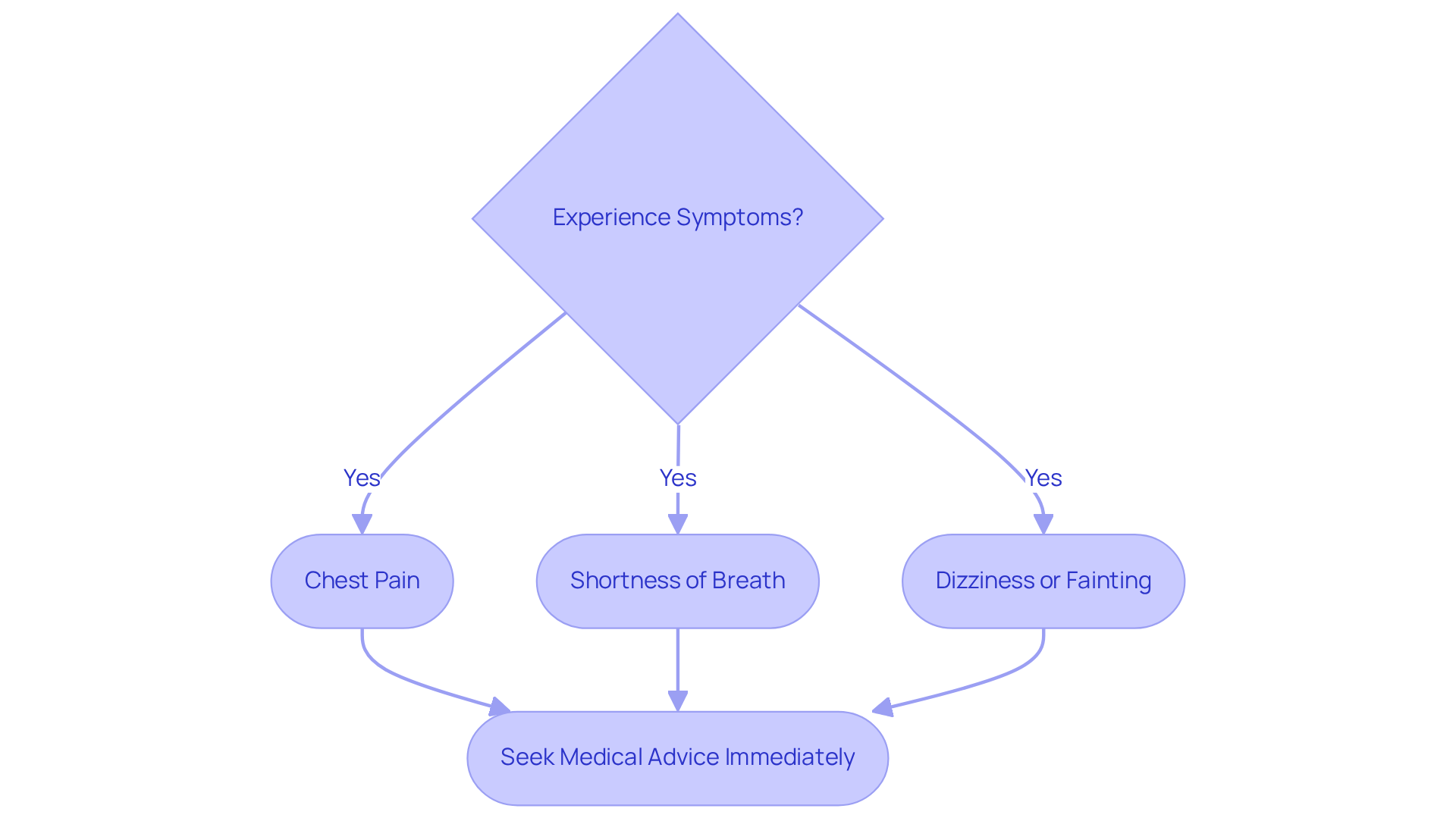
While experiencing heart flutters can often be harmless, it’s important to recognize that certain symptoms may indicate a more serious condition that requires prompt medical attention. If you experience any of the following, please don’t hesitate to seek advice:
If symptoms last more than a few minutes or worsen, it’s essential to consult a healthcare professional to rule out significant health concerns.
Recent studies highlight that frequent palpitations, especially when accompanied by symptoms like chest pain or shortness of breath, should prompt immediate evaluation. Cardiologists emphasize that these symptoms can indicate serious conditions, including arrhythmias, which are more common among older adults. In fact, emergency room visits for chest discomfort and flutters have been on the rise, underscoring the need for awareness and prompt intervention.
Remember, early intervention can significantly improve outcomes and reduce the risk of severe complications. Your health is important, and proactive measures can make all the difference. Don’t hesitate to talk to your doctor about any concerns you may have; they’re there to support you every step of the way.
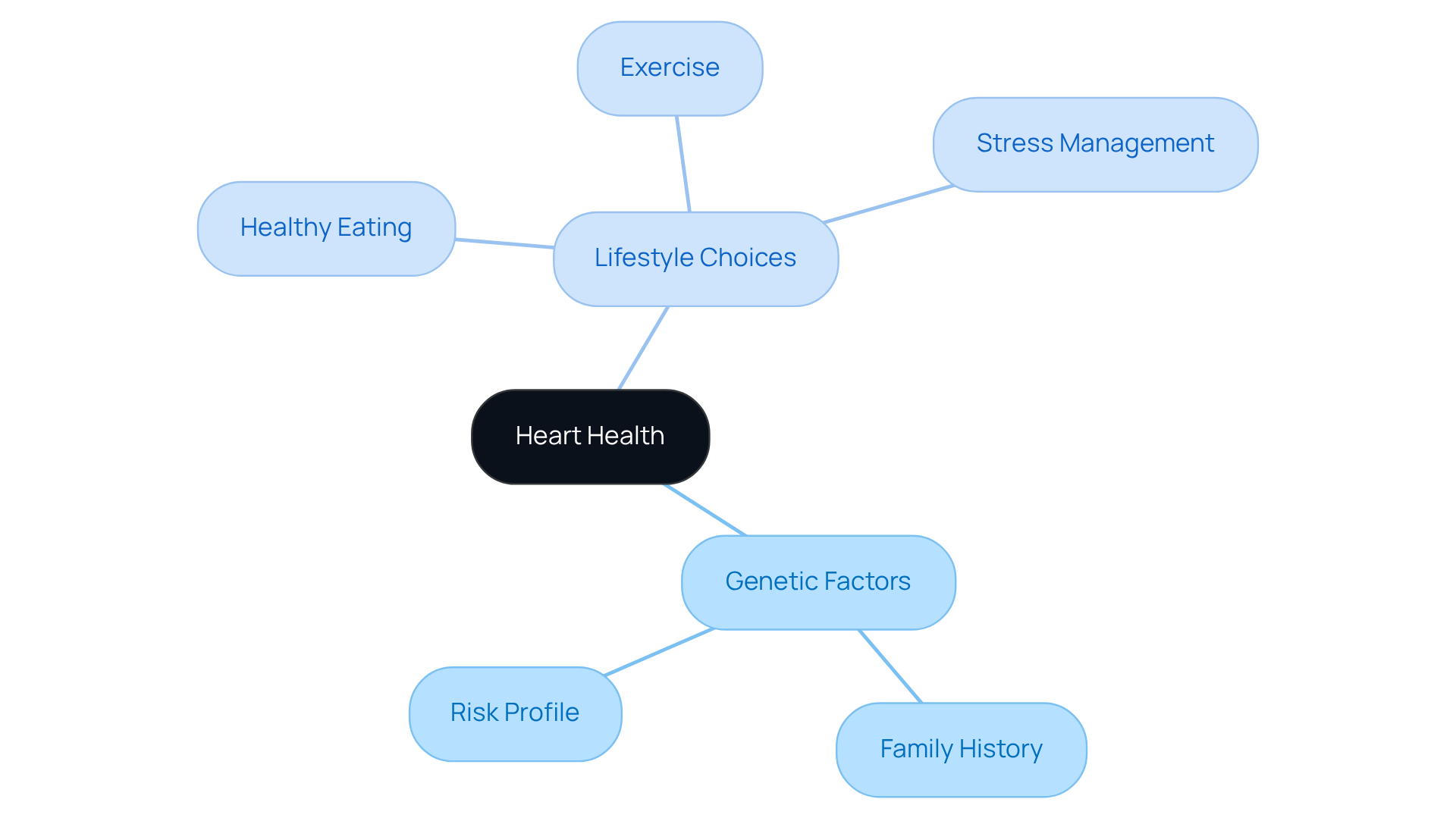
Final Thoughts: Proactive Management of Heart Flutters
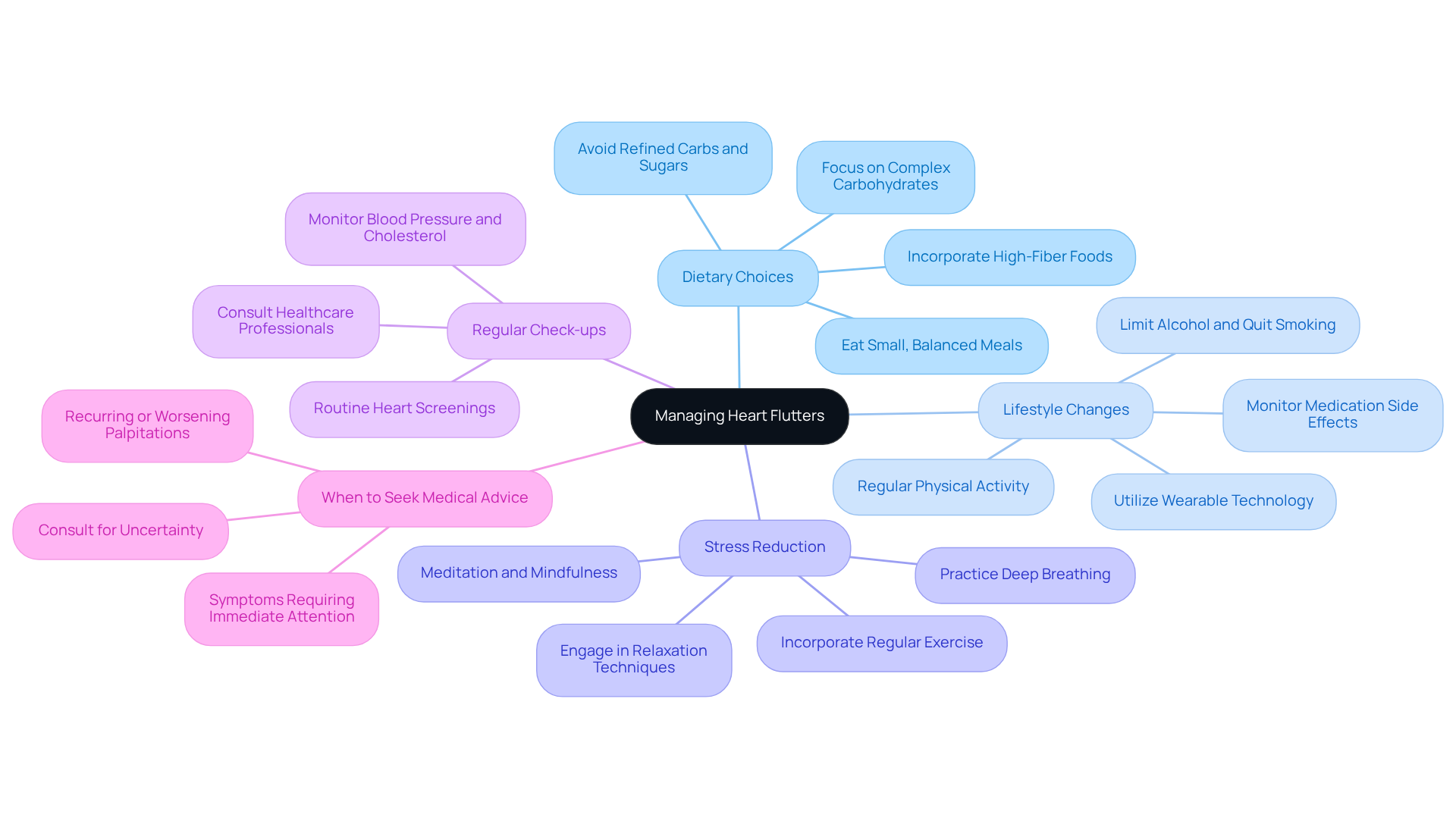
Experiencing heart flutters can be concerning, but there are ways to manage them. By making thoughtful dietary choices, embracing healthy habits, and implementing stress reduction techniques, you can take significant steps toward better heart health, particularly if you experience frequent flutters. Are there certain foods that seem to cause your heart flutters? Being mindful of these factors can influence how my body reacts.
In addition to this, regular check-ups are essential to prevent complications. Medical visits are crucial, especially if you have existing heart conditions. These visits help ensure that you’re on the right track and can prevent potential complications. Remember, you’re not alone in this journey.
At Amavita, we understand the unique needs of our patients, particularly the elderly. That’s why we offer Extensive and Optimal Programs designed for heart health. These programs include:
Our goal is to provide the support you need to maintain your well-being.
Furthermore, it’s important to recognize when to seek medical advice. If you ever feel uncertain about your symptoms, don’t hesitate to reach out for help. We’re here to assist you every step of the way, ensuring you receive the care and attention you deserve. Your well-being is our priority, and together, we can work towards a healthier future.
Conclusion
Experiencing heart flutters after eating can be unsettling, and it’s completely understandable to feel concerned. Recognizing the dietary and lifestyle factors that contribute to this condition is essential for managing your heart health effectively. By identifying trigger foods—like caffeine, alcohol, high-sugar items, and processed foods—you can make informed choices that support your cardiovascular well-being. In addition to this, understanding the importance of stress management, regular physical activity, and quality sleep can significantly enhance heart function and reduce the frequency of palpitations.
While heart flutters are often benign, they can sometimes signal more serious health issues. It’s crucial to remain vigilant and seek medical advice if you experience concerning symptoms like chest pain or shortness of breath. Regular consultations with healthcare professionals, such as those offered by Amavita Heart and Vascular Health, provide valuable support and tailored care to help manage heart flutters and promote overall cardiovascular health.
Taking proactive steps towards healthier eating habits, stress reduction techniques, and lifestyle adjustments can greatly influence heart rhythm stability. By prioritizing your heart health and seeking guidance when needed, you can navigate your journey towards a healthier future with confidence and peace of mind. Remember, you are not alone—there are resources and support available to help ensure your well-being every step of the way.
Frequently Asked Questions
What are heart flutters and what causes them?
Heart flutters are sensations of rapid heartbeats or irregular heart rhythms that can occur due to various factors, including stress, anxiety, and dietary choices. After eating, the body’s digestion process can temporarily increase the pulse rate, leading to noticeable heart flutters.
How can diet affect heart flutters?
Certain foods can trigger heart flutters after eating. High-sugar foods, caffeine, alcohol, spicy foods, and processed foods can exacerbate the issue. Foods rich in magnesium, potassium, and omega-3 fatty acids are beneficial for heart health and may help reduce irregular heartbeats.
What role do stress and anxiety play in heart flutters?
Stress and anxiety can trigger heart flutters by increasing the heart rate and causing palpitations. Managing stress through relaxation techniques can be helpful in calming both the mind and body.
What are some common dietary triggers for heart flutters?
Common dietary triggers include:
- Caffeine: Found in coffee and energy drinks, excessive caffeine can lead to increased palpitations.
- Alcohol: Excessive drinking can cause dehydration and electrolyte imbalances, worsening fluttering sensations.
- High-sugar foods: These can cause rapid fluctuations in glucose levels, triggering palpitations.
- Spicy foods: Capsaicin in spicy foods can stimulate the nervous system and elevate heart rates.
- Processed foods: High in sodium and unhealthy fats, these can contribute to elevated blood pressure and rhythm issues.
When should I be concerned about heart flutters?
While many heart flutters are harmless, they can sometimes indicate a more serious issue, especially if accompanied by symptoms like dizziness or chest pain. It’s important to consult a healthcare professional if you have concerns about your heart health.
What kind of care does Amavita Heart and Vascular Health provide?
Amavita Heart and Vascular Health offers comprehensive cardiovascular care tailored to individual needs, utilizing advanced diagnostic techniques and minimally invasive procedures to enhance patient comfort and reduce recovery times.
How does Amavita support patients from diverse backgrounds?
Amavita prioritizes culturally aware communication to ensure that every patient, regardless of background, receives high-quality care in an environment where they feel acknowledged and supported.
What should I do if I am feeling anxious about my heart health?
If you are feeling anxious about your heart health, it is important to reach out for support. Amavita Heart and Vascular Health offers compassionate care and listens to your concerns to help find the best solutions for your cardiovascular health.
List of Sources
- Amavita Heart and Vascular Health: Expert Care for Heart Flutters
- wric.com (https://wric.com/business/press-releases/ein-presswire/862601624/amavita-heart-vascular-health-launches-cardiologist-led-testosterone-therapy)
- amavita.health (https://amavita.health/news/aisap-amavita-heart-and-vascular-health-expand-cardiac-diagnostics-in-underserved-florida-communities)
- Roundup: Heart Disease Still No. 1 Cause of Death as Risk Factors Rise Post-COVID; and More News (https://baptisthealth.net/baptist-health-news/heart-disease-still-top-cause-of-death-as-risk-factors-rise)
- Heart and Stroke Statistics (https://heart.org/en/about-us/heart-and-stroke-association-statistics)
- Understanding Heart Flutters: What They Are and Why They Happen
- my.clevelandclinic.org (https://my.clevelandclinic.org/health/diseases/22416-heart-palpitations-after-eating)
- my.clevelandclinic.org (https://my.clevelandclinic.org/health/diseases/17084-heart-palpitations)
- bswhealth.com (https://bswhealth.com/blog/heart-palpitations-after-eating)
- Why Am I Having Heart Palpitations? (https://webmd.com/heart-disease/atrial-fibrillation/ss/slideshow-heart-palpitations-causes)
- northwell.edu (https://northwell.edu/news/insights/heart-palpitations-after-eating)
- Identifying Trigger Foods: Common Culprits Behind Heart Flutters
- 8 Foods To Avoid Eating Frequently if You Have Heart Palpitations | Carda Health (https://cardahealth.com/post/foods-to-avoid-if-you-have-heart-palpitations)
- Foods to Avoid If You Have Heart Palpitations (https://sugarlandcardiologyspecialist.com/blog/heart-palpitations-foods-to-avoid)
- harleystreet.sg (https://harleystreet.sg/blog/foods-to-avoid-if-you-have-heart-palpitations)
- bswhealth.com (https://bswhealth.com/blog/heart-palpitations-after-eating)
- Foods to Avoid if You Have Heart Palpitations (https://southdenver.com/foods-to-avoid-if-you-have-heart-palpitations)
- Lifestyle Factors: How Daily Habits Influence Heart Flutters
- Lifestyle changes for heart disease prevention (https://uhc.com/news-articles/healthy-living/lifestyle-changes-for-heart-disease-prevention)
- sciencedirect.com (https://sciencedirect.com/science/article/pii/S2772487524000709)
- timesofindia.indiatimes.com (https://timesofindia.indiatimes.com/life-style/health-fitness/cardiologist-with-25years-of-experience-lists-4-lifestyle-factors-behind-most-heart-issues/articleshow/125124145.cms)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC8578196)
- High-Sugar Foods: Their Impact on Heart Flutters
- A High-Sugar Diet Consumption, Metabolism and Health Impacts with a Focus on the Development of Substance Use Disorder: A Narrative Review – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9323357)
- Diabetic-level glucose spikes seen in healthy people (https://med.stanford.edu/news/all-news/2018/07/diabetic-level-glucose-spikes-seen-in-healthy-people.html)
- cdc.gov (https://cdc.gov/nutrition/php/data-research/sugar-sweetened-beverages.html)
- newsroom.heart.org (https://newsroom.heart.org/news/california-study-finds-drinking-sugary-drinks-daily-may-be-linked-to-higher-risk-of-cvd-in-women)
- Food Additives: Hidden Triggers for Heart Flutters
- crestline.com (https://crestline.com/c/slogans-for-american-heart-month)
- (PDF) Artificial Intelligence, Machine Learning and Reasoning in Health Informatics—Case Studies (https://researchgate.net/publication/346113079_Artificial_Intelligence_Machine_Learning_and_Reasoning_in_Health_Informatics-Case_Studies)
- ucfhealth.com (https://ucfhealth.com/our-services/cardiology/how-to-stop-heart-palpitations-after-eating)
- foodunpacked.com (https://foodunpacked.com/health/health-effects-of-substances)
- parade.com (https://parade.com/1187612/michelle-parkerton/quotes-about-heart-disease)
- Dietary Strategies: Managing Heart Flutters Through Food Choices
- heart.org (https://heart.org/en/news/tag-nutrition-news)
- newatlas.com (https://newatlas.com/heart-disease/dietary-fiber-gut-microbes-cardioprotection-scfas)
- nhlbi.nih.gov (https://nhlbi.nih.gov/news/2025/nih-supported-dash-diet-named-best-heart-healthy-diet-and-best-diet-high-blood-pressure)
- healthieru.unl.edu (https://healthieru.unl.edu/news/fibers-impact-heart-health)
- mplsheart.org (https://mplsheart.org/news/eating-heart-health-teachings-registered-dietitian-nutritionists)
- Deep Breathing and Mindfulness: Techniques to Calm Heart Flutters
- Effectiveness of deep breathing exercises on anxiety, depression and sleep quality in patients undergoing coronary artery bypass surgery – Scientific Reports (https://nature.com/articles/s41598-025-12481-x)
- heartandstroke.ca (https://heartandstroke.ca/articles/mindfulness-for-a-healthier-heart)
- today.com (https://today.com/health/mind-body/cardiologist-tip-lower-heart-rate-box-breathing-rcna228741)
- journals.lww.com (https://journals.lww.com/md-journal/fulltext/2023/11240/effect_of_slow_breathing_exercise_and_progressive.112.aspx)
- journals.lww.com (https://journals.lww.com/hhmi/fulltext/2024/08040/mindfulness_in_cardiovascular_disease_patients_.11.aspx)
- When to Seek Medical Advice: Recognizing Serious Symptoms
- Five Heart Disease Symptoms You Should Never Ignore (https://nyulangone.org/news/five-heart-disease-symptoms-you-should-never-ignore)
- Heart palpitations: When to visit the doctor or ER (https://medicalnewstoday.com/articles/when-to-be-concerned-about-heart-palpitations)
- Frequency of Cardiac Rhythm Abnormalities in a Half Million Adults – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC6051725)
- When Should You Worry About Heart Palpitations? (https://healthliteracy.tuftsmedicine.org/about-us/news/when-should-you-worry-about-heart-palpitations)
- Global surge in serious heart rhythm disorders sparks urgent call to action from experts: 1 in 3 people at risk (https://escardio.org/The-ESC/Press-Office/Press-releases/global-surge-in-serious-heart-rhythm-disorders-sparks-urgent-call-to-action-from)
- Final Thoughts: Proactive Management of Heart Flutters
- int.livhospital.com (https://int.livhospital.com/7-essential-facts-about-flutter-disease-symptoms-risks-and-treatment)
- The Importance of Routine Heart Check-ups | AMS Cardiology (https://amscardiology.com/the-importance-of-routine-heart-check-ups)
- doralhw.org (https://doralhw.org/lifestyle-changes-to-reduce-palpitations)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC10460604)
- Recent Advancements Make it Easier to Live Well with Atrial Fibrillation (https://uabmedicine.org/news/recent-advancements-make-it-easier-to-live-well-with-atrial-fibrillation)